The Chief Public Health Officer's Report on the State of Public Health in Canada 2013 – Antimicrobial resistance – A shared responsibility
Antimicrobial Resistance—A Shared Responsibility
Highlights
- Antimicrobial resistance is inevitable, but can be delayed.
- Antimicrobial-resistant micro-organisms are not restricted to healthcare facilities.
- Inappropriate use of antimicrobial agents and limited research into and development of new agents have helped accelerate antimicrobial resistance.
- Treatment of diseases caused by antimicrobial-resistant organisms takes more time, uses more resources and is more costly.
- Managing antimicrobial use is everyone's responsibility.
- The World Health Organization has recognized antimicrobial resistance as one of the most serious public health threats to the treatment of infectious diseases worldwide.
The discovery of penicillin by Alexander Fleming in the 1920s and its development as therapy by Howard Florey in the 1940s are generally accepted as the start of the modern antimicrobial revolution.Footnote 1 With the advent of antimicrobial agents (antimicrobials), the chances of recovering from an infection have increased considerably.Footnote 2-Footnote 5 However, the overuse and misuse of antimicrobials among people, in animals and for crops, as well as the innate adaptability of micro-organisms have made these drugs less effective.Footnote 3, Footnote 4, Footnote 6-Footnote 8
Antimicrobials are natural, semisynthetic or synthetic substances that destroy or inhibit the growth of micro-organisms.Footnote 11, Footnote 12
Antibiotics are either produced by micro-organisms or are semisynthetic substances derived from micro-organisms. They are used to treat infections caused by bacteria.Footnote 7
A mutation is a permanent and heritable change in an organism's DNA that may lead to the creation of new traits or characteristics.Footnote 13
Horizontal gene transfer is "the process of swapping genetic material between neighbouring bacteria".Footnote 13
Multidrug-resistant (MDR) micro-organisms have "acquired non-susceptibility to at least one agent in three or more antimicrobial categories."Footnote 14
Extensively drug-resistant (XDR) micro-organisms are not susceptible to at least one agent in all but two or fewer antimicrobial categories.Footnote 14
Pandrug-resistant (PDR) micro-organisms are not susceptible to all agents in all antimicrobial categories.Footnote 14
Development and transmission
That micro-organisms develop resistance to antimicrobials is inevitable.Footnote 7, Footnote 8 They multiply quickly and mutate and adapt to hostile environments.Footnote 7,Footnote 9, Footnote 10 Micro-organisms have existed on earth for more than 3 billion years, and have developed over time a natural ability to become resistant to antimicrobials in order to survive, which is one of the main reasons the most resilient micro-organisms thrive.Footnote 7, Footnote 9
Antimicrobials are natural, semisynthetic or synthetic substances that destroy or inhibit the growth of micro-organisms.Footnote 11Footnote 12
Antibiotics are either produced by micro-organisms or are semisynthetic substances derived from micro-organisms. They are used to treat infections caused by bacteria.Footnote 7
A mutation is a permanent and heritable change in an organism's DNA that may lead to the creation of new traits or characteristics.Footnote 13
Horizontal gene transfer is the process of swapping genetic material between neighbouring bacteria .Footnote 13
Multidrug-resistant (MDR) micro-organisms have acquired non-susceptibility to at least one agent in three or more antimicrobial categories. Footnote 14
Extensively drug-resistant (XDR) micro-organisms are not susceptible to at least one agent in all but two or fewer antimicrobial categories.Footnote 14
Pandrug-resistant (PDR) micro-organisms are not susceptible to all agents in all antimicrobial categories.Footnote 14
Antimicrobials, such as antivirals, antibiotics, antifungals and antiparasitics, kill or slow the growth of most micro-organisms (i.e. viruses, bacteria, fungi and parasites, respectively).Footnote 7, Footnote 11, Footnote 12, Footnote 15 However, those micro-organisms with greater resistance survive and continue to infect their host, illustrating Darwin's principle of survival of the fittest. Footnote 8, Footnote 16
Antimicrobial resistance is the ability of micro-organisms to resist the effects of antimicrobials.Footnote 7, Footnote 13, Footnote 17 The micro-organisms change in a way that reduces or eliminates the effectiveness of drugs, chemicals or other agents designed to cure or prevent infections and/or disease caused by the micro-organism.Footnote 7, Footnote 13, Footnote 17 Bacteria may be naturally resistant or insensitive to antimicrobial agents (intrinsic resistance) or may become resistant after being exposed to antimicrobial agents (acquired resistance); alternatively, a combination of both intrinsic and acquired resistance may counter the effects of antimicrobial agents.Footnote 12, Footnote 13 The majority of strains of bacterial species can show intrinsic resistance; acquired resistance can occur through mutation, horizontal gene transfer or a combination of each.Footnote 13, Footnote 18 Unlike intrinsic resistance, acquired resistance is less common, existing only in some bacterial strains and species sub-populations.Footnote 13 A bacterium can make antimicrobials ineffective by modifying or degrading parts of the antimicrobial, expelling the antimicrobial, or changing its own structure so as to reduce the antimicrobial's ability to bind or attach to the bacterium.Footnote 13, Footnote 19
While antimicrobials do not themselves create resistance, they can create the environments in which resistant bacteria flourish.Footnote 12, Footnote 20 This happens because they kill only susceptible bacteria, leaving resistant strains to survive and multiply.Footnote 12, Footnote 13, Footnote 20 Over time, this can lead to strains that are resistant to multiple drugs, and in extreme cases, resistant to all drugs.Footnote 13, Footnote 14, Footnote 21 Common diseases with strains that are resistant to at least one antimicrobial agent include salmonellosis, gonorrhea, tuberculosis and influenza.Footnote 22, Footnote 23 For example, gonorrhea, once easily treated using first-line antibiotics, currently has 32 different antibiotic-resistant strains.Footnote 24-Footnote 26 Multidrug-resistant strains may account for as many as 60% of gonorrhea cases worldwide each year.Footnote 23
Antibiotic use and research
Antimicrobials are widely used in many sectors of society (see Figure 1), and their effects on people, animals and the environment can be far-reaching, contributing both directly and indirectly to the development of antimicrobial resistance.Footnote 18, Footnote 27, Footnote 28 As such, the decision to use antimicrobials needs to take the potential antimicrobial risks into consideration.Footnote 7, Footnote 12, Footnote 17, Footnote 29, Footnote 30
Figure 1 Sectors impacted by antimicrobial useFootnote 7, Footnote 27, Footnote 31
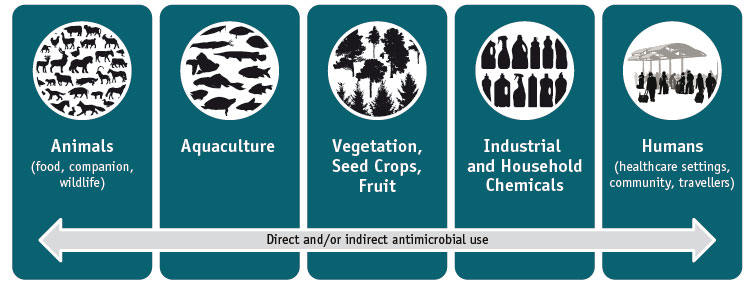
Text Equivalent - Figure 1
This figure describes how antimicrobials used in many sectors contribute to the emergence and spread of resistant micro-organisms in various settings. Each of these are linked through direct and indirect pathways (e.g. Direct pet to human contact or indirect from water or food consumption).
Note: Modified after Linton, A.H. (1977) and Irwin, R. (2007).
Animals
In Canada, more than three-quarters of antimicrobials are used in animals.Footnote 32 Of the antimicrobials used in animals, approximately 90% are used to promote growth or to guard against disease and infection (prophylaxis).Footnote 7, Footnote 33 The development of antimicrobial-resistant pathogens in animals can pose risks to public health when they are transmitted as food-borne or water-borne contaminants.Footnote 32 Between 2003 and 2011, the Canadian Integrated Program for Antimicrobial Resistance Surveillance (CIPARS) tested 26,428 human Salmonella samples caused from exposure to contaminated food products.Footnote 34 Of these, 28% of the Salmonella strains were resistant to one or more antimicrobials.Footnote 34 In 2011, CIPARS observed consistently high levels of resistance to a specific antimicrobial, ceftiofur, in Salmonella isolates found in retail chicken products, as well as in Salmonella causing human infections.Footnote 35 This antimicrobial resistance was attributed to the use of antibiotics in chicken hatcheries.Footnote 36 Once the use of antimicrobials ceased, a significant decrease in antibiotic resistant Salmonella was seen in both retail chicken and humans.Footnote 36
Antimicrobials are also often used in companion animals, for example, dogs, cats, horses and other pets.Footnote 37-Footnote 39 Unfortunately, available information regarding antimicrobial resistance and antimicrobial use is generally lacking for companion animals.Footnote 37, Footnote 38 Given that more than one-half of Canadian households share their homes with at least one dog or cat, better information about antimicrobial use and resistance in this group of animals is important.Footnote 40
Aquaculture
In Canada, antimicrobial agents are also used in the farming of aquatic organisms, or aquaculture.Footnote 12 Although publicly available information about antimicrobial resistance and use in aquaculture is limited, the use of antimicrobials has steadily decreased in British Columbia since 1995.Footnote 12, Footnote 41-Footnote 43 Increased use of vaccination in aquaculture has decreased the need to use antimicrobials to guard against disease.Footnote 12 The majority of antimicrobials (97%) that are administered for aquaculture are given to young, non-market fish.Footnote 12
Plants
Antibiotics have been used since the 1950s to control certain bacterial diseases (e.g. fire blight and bacterial spot) that affect fruits, vegetables and ornamental plants.Footnote 44 In the United States, antibiotics applied to plants account for less than 0.5% of total antibiotic use.Footnote 12, Footnote 44
Industrial and household chemicals
Antibiotic-like substances and antibacterial agents are now common in various household products such as clothing, cosmetics, toothpaste, cleansers and detergents.Footnote 7, Footnote 12, Footnote 21, Footnote 45-Footnote 47 Despite the fact that they do not significantly reduce infections or microbial contamination–and may contribute to the development of antibiotic resistance– the number of products containing antibacterial agents continues to increase.Footnote 47-Footnote 50 In 1993, there were 23 common household products containing antibacterial agents in the United States; less than a decade later, there were more than 700.Footnote 21, Footnote 51
Humans
Antibiotics have revolutionized medicine: healthcare providers can prescribe a wide range of treatments for their patients who are, as a result, less likely to die or to suffer serious outcomes.Footnote 7, Footnote 23 However, bacteria may become resistant if prescribed antibiotics are used inappropriately or are not completed.Footnote 7, Footnote 12, Footnote 30, Footnote 52 Healthcare providers frequently have to depend on partial or imperfect information to diagnose an infection and decide on treatment.Footnote 30 Antimicrobials may be given "just in case," or broad-spectrum antimicrobials may be prescribed when narrow spectrum antibiotics might be sufficient.Footnote 7, Footnote 30 In addition, some patients demand a prescription for antibiotics when they are not needed, to the point of seeking out healthcare providers who will prescribe the antibiotics they want.Footnote 20, Footnote 53, Footnote 54
The number of oral antimicrobial prescriptions for humans has decreased since 2000. Despite this, for every 1,000 Canadians, more than 670 prescriptions for oral antimicrobials were filled by retail pharmacies in 2009 (see Figure 2).Footnote 55 In addition, estimates suggest that one-half of all patients do not complete their prescribed courses of medication, including antibiotics, making a person more vulnerable to resistant bacteria.Footnote 56 Not completing the prescribed antibiotic therapy can create an environment in which resistant bacteria can flourish.Footnote 7, Footnote 17
Healthcare settings often have to deal with antimicrobial resistance since antibiotics are frequently used.Footnote 28, Footnote 30, Footnote 57 Resistant micro-organisms can spread quickly and easily through institutions when prevention and control procedures are inadequate or nonexistent (see "Healthcare-Associated Infections–Due Diligence").Footnote 57, Footnote 58 Methicillin-resistant Staphylococcus aureus (MRSA), vancomycin-resistant enterococci (VRE) and carbapenemase-producing Enterobacteriaceae (CPE) are examples of increasingly common pathogens that can cause multidrug-resistant healthcare-associated infections (HAIs).Footnote 59-Footnote 62 In 2009, more than 2,000 confirmed infections and more than 4,500 confirmed colonizations of healthcare-associated MRSA were reported to the Canadian Nosocomial Infection Surveillance Program (CNISP); between 1998 and 2005, more than 3,000 new cases of VRE were identified.Footnote 60, Footnote 61
Antimicrobial-resistant infections, such as tuberculosis and community-acquired MRSA (CA-MRSA), can also be transmitted from person to person outside of healthcare settings.Footnote 17, Footnote 59, Footnote 63-Footnote 65 In 2011, of the 139 tuberculosis isolates that were drug-resistant, 18 were classified as MDR and one as XDR in Canada (see "Tuberculosis–Past and Present").Footnote 66 Between 1995 to 1999 and 2004 to 2007, the percentage of Canadian patients with CA-MRSA increased from 6% to 23%.Footnote 67 Poor hygiene practices, such as inadequate handwashing, may spread the bacteria more easily.Footnote 65
Research
Fewer new antimicrobials are being developed for a number of reasons.Footnote 9, Footnote 10, Footnote 68-Footnote 70 The overall success rate of antimicrobials and low return on investment makes them less profitable for drug companies.Footnote 9, Footnote 68, Footnote 69 Since antibiotics are generally used as short-course therapies (1 to 2 weeks) for a targeted disease, therapies for chronic diseases tend to be more profitable.Footnote 9, Footnote 68 Between 1983 to 1987 and 2008 to 2011, approval of new systemic antibacterial agents by the United States Food and Drug Administration decreased by 87% compared to the period from 1983 to 1987 (see Figure 3).Footnote 9, Footnote 71 In 2004, only five new antibiotics were listed as under development by the largest pharmaceutical companies; in the same year, four new drugs to treat erectile dysfunction were listed as under development.Footnote 9
Figure 2 Total number of prescriptions per 1,000 population for oral antimicrobials dispensed by retail pharmacies in Canada, 2000 to 2009Footnote 55
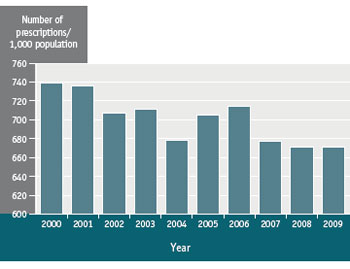
Text Equivalent - Figure 2
| Year | Number of prescriptions per 1,000 population |
|---|---|
| 2000 | 739.0 |
| 2001 | 735.6 |
| 2002 | 706.6 |
| 2003 | 710.9 |
| 2004 | 677.9 |
| 2005 | 705.0 |
| 2006 | 714.5 |
| 2007 | 677.4 |
| 2008 | 670.8 |
| 2009 | 671.1 |
Figure 3 Number of new systemic antibacterial agents approved by the United States Food and Drug Administration per 5-year period, 1983-1987 to 2008-2011Footnote 71
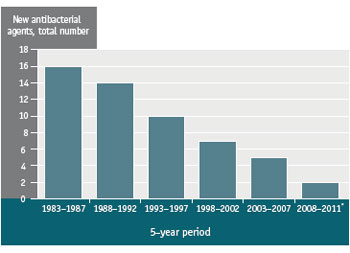
Text Equivalent - Figure 3
Number of new systemic antibacterial agents approved by the United States Food and Drug Administration per 5-year period. New molecular entities are considered. Data are accurate through February 2011.
Note: New molecular entities are considered.
Impacts of antimicrobial resistance
Antimicrobial resistance has a great impact on human health.Footnote 7, Footnote 19, Footnote 72 Antimicrobial-resistant infections are associated with a greater risk of death, more complex illnesses, longer hospital stays and higher treatment costs.Footnote 7, Footnote 17, Footnote 72, Footnote 73 The people most likely to be affected are the most vulnerable–the elderly, the very young, critical care patients, those who are immune-compromised, those being treated with immune-suppressing drugs and those who have had antimicrobial-resistant infections before.Footnote 7 Also at risk are those who are frequently exposed to antimicrobial-resistant pathogens (via healthcare institutions, consumption of contaminated food/water or through direct contact with infected animals).Footnote 7, Footnote 17
Antimicrobial resistance is also an issue in hospitals, where patients are given antibiotics to fight off many types of infections.Footnote 20 When treatment is unsuccessful, patients are able to spread the resistant strain for longer periods of time.Footnote 7, Footnote 17, Footnote 74 Heavy antibiotic use can lead to the development of drug-resistant strains that may be untreatable, even by the strongest available antibiotics.Footnote 17, Footnote 20, Footnote 74 In hospitals patterns of resistance can vary, underlining the need for accurate records of antibiotic use and outcomes in order to define the scope of the problem and identify populations and areas at greatest risk.Footnote 20
In addition to being more difficult to treat, antimicrobial-resistant infections are more costly to treat. If first-line medicines are ineffective, more expensive therapies may be needed, probably for longer, with more adverse effects.Footnote 7, Footnote 17, Footnote 20, Footnote 74 A Canadian study estimated the annual hospital costs of MRSA to be between $42 million and $59 million, while an American study found the treatment costs associated with antimicrobial-resistant infections to be about $6,000 to $30,000 more per patient compared with the treatment costs of antimicrobial-susceptible infections.Footnote 75-Footnote 77
Mitigation strategies
Antimicrobial resistance is increasing around the world.Footnote 9, Footnote 57 Managing the effects of using antimicrobials is not a problem that can be solved by any one city, country or continent.Footnote 28, Footnote 57 The following discussion outlines strategies to manage antimicrobial use.
Surveillance
Surveillance of both antimicrobial use and antimicrobial resistance would help monitor trends and patterns, and measure the effectiveness of policies and interventions.Footnote 7, Footnote 57, Footnote 78, Footnote 79 Such surveillance needs to take place in different environments (in the community and in institutions, on the farm and along the food supply chain) locally, nationally and internationally.Footnote 7, Footnote 57, Footnote 78
Many countries, including Canada, have developed systems to measure the extent and distribution of both antimicrobial use and the associated resistance. CIPARS was established in 2002 to monitor antimicrobial use and antimicrobial resistance of specific bacteria across the food supply chain.Footnote 80 The program is based on several integrated surveillance components that are linked to examine the relationship between antimicrobials used both in food animals and in people and the associated health impacts.Footnote 81 This information is used to support the development of evidence-based policies to control antimicrobial use in hospitals, the community and agricultural settings so as to make these drugs more effective, and to identify appropriate measures to slow the emergence and spread of resistant bacteria between animals, food and people.Footnote 32, Footnote 81 CIPARS is coordinated by the Public Health Agency of Canada's Centre for Food-borne, Environmental and Zoonotic Infectious Diseases, Laboratory for Foodborne Zoonoses and National Microbiology Laboratory, in partnership with the Canadian Food Inspection Agency, the Veterinary Drugs Directorate of Health Canada and provincial health and agriculture ministries.Footnote 32
CNISP was established in 1994 to gather information on HAIs in Canadian healthcare facilities.Footnote 82 These data allow clinicians and policy makers to compare rates (benchmarks) and trends and gather information for the development of national guidelines on clinical issues.Footnote 82 CNISP is a collaboration between the Canadian Hospital Epidemiology Committee, a subcommittee of the Association of Medical Microbiology and Infectious Disease Canada and the Centre for Communicable Diseases and Infection Control of the Public Health Agency of Canada.Footnote 82 At present, 54 sentinel hospitals from 10 provinces participate in the CNISP network.Footnote 82 CNISP conducts surveillance for MRSA, Clostridium difficile infection (CDI), VRE and CPE, among others.Footnote 83, Footnote 84
Internationally, the Danish Integrated Antimicrobial Resistance Monitoring and Research Programme (DANMAP) was established in 1995 by the Danish Ministry of Food, Agriculture and Fisheries and the Danish Ministry of Health.Footnote 85 The program monitors the amount of antimicrobials consumed by people and food animals, as well as the number of antimicrobial-resistant organisms in food animals, food of animal origin and people.Footnote 85 DANMAP also studies associations between consumption of antimicrobials and resistance and identifies the pathways by which antimicrobial resistance spreads.Footnote 85 Antimicrobial resistance is monitored in human and animal pathogens, zoonotic bacteria and indicator bacteria.Footnote 85
The National Antimicrobial Resistance Monitoring System (NARMS) is a collaboration between three United States agencies: the Centers for Disease Control and Prevention (CDC), the Food and Drug Administration (Center for Veterinary Medicine) and the Department of Agriculture (Agricultural Research Service).Footnote 86 NARMS data have been collected continually since the system was established in 1996, making it possible to analyze trends as well as provide useful information about patterns of emerging resistance that arise from animal and food sources and their impact on public health.Footnote 87 The data may also be used to investigate outbreaks.Footnote 87
Stewardship
The development of new drugs will not be enough to address the growing resistance problem as micro-organisms will change in ways to reduce their effectiveness.Footnote 7, Footnote 88 For this reason it is important to use existing drugs judiciously.Footnote 52, Footnote 88 Antimicrobial stewardship has been defined as "the optimal selection, dose, and duration of an antimicrobial that results in the best clinical outcome for the treatment or prevention of infection, with minimal toxicity to the patient and minimal impact on subsequent resistance."Footnote 89, Footnote 90 To achieve this, everyone must adopt attitudes and practices that mitigate the spread of antibiotic resistance–by using antibiotics appropriately, through targeted education and awareness programs and by re-establishing common preventive hygiene measures.Footnote 20
Regulations and practical measures could help to lessen the external pressures on bacteria to become resistant.Footnote 57 Antibiotics should be given only to those who stand to benefit and avoided for viral illnesses such as colds or many sore throats.Footnote 20 Well-targeted antibiotic therapy (which depends on an accurate diagnosis) reduces the need for sequential, hit-and-miss courses of antibiotics and the consequent risk of developing antibiotic resistance.Footnote 20 In some instances, combining multiple antibiotics may improve the chances of curing a bacterial infection more quickly, and thereby reduce the possibility of resistance.Footnote 20 Programs such as Alberta's Do Bugs Need Drugs? aim to educate healthcare professionals and the general public on their roles in managing antimicrobial use and mitigating antimicrobial resistance (see the textbox "Antimicrobial stewardship: Do Bugs Need Drugs?").Footnote 91
Antimicrobial stewardship: Do Bugs Need Drugs?
Do Bugs Need Drugs? (DBND) is a community education program about washing hands and the responsible use of antibiotics.Footnote 91 DBND materials, available for healthcare professionals and the general public, explain why antibiotic resistance is an issue and how to prevent antibiotic resistance from developing.Footnote 91 Teaching correct handwashing is a key component of DBND materials because handwashing prevents many infections and the need for treatment.Footnote 91
The DBND program started as a small six-month pilot in Grande Prairie, Alberta, Canada, in 1998-1999.Footnote 91 It is now a provincial program in Alberta and in British Columbia, and elements of the program are used in other parts of Canada, the United States and elsewhere.Footnote 91 Programs are available for physicians, pharmacists, nurses, teachers, schools, daycare centres, preschools, early childhood educators, occupational health nurses, human resources personnel, older adults, parents, children and the general public.Footnote 91 Annual evaluations of the program have shown decreases in prescription rates for ear infections and sore throats as well as a decrease in overall antibiotic consumption.Footnote 92, Footnote 93
Similarly, using antibiotics in animals should be limited to treating infection and not for long-term mass medication for growth promotion or guarding against disease.Footnote 94 Limiting antibiotics could help reduce the development of resistance in animals and the transmission to other animals and to people.Footnote 33 In addition to having no official guidelines or policies to manage antimicrobial use in animals, Canada is one of the few industrialized countries that allows over-the-counter sale of antimicrobials for use in food animals.Footnote 95, Footnote 96 To help veterinarians assist their clients in creating and implementing sound antimicrobial programs, the Canadian Veterinary Medical Association has created a set of guidelines for beef cattle, dairy cattle, poultry and swine.Footnote 97 They recommend using targeted drug therapies only when needed and only within the confines of a valid veterinary-client-patient relationship.Footnote 97
Increasing public awareness of the issues associated with antimicrobial resistance is vital.Footnote 20, Footnote 98 Studies have shown that when people are told the reasons why appropriate antimicrobial use is important and given related guidance, behaviours can be modified to reflect more positive use.Footnote 20, Footnote 98 Good handwashing and hand hygiene techniques remain the best protection against the spread of infections and antibiotic-resistant micro-organisms.Footnote 99-Footnote 101
Commitment and cooperation
Health risks due to antimicrobial resistance are a global concern.Footnote 28, Footnote 57 Mobilizing the necessary expertise and resources to prevent and control antimicrobial resistance depends on the commitment and cooperation of policy makers and decision makers and the global medical and veterinary community.Footnote 57
The World Health Organization (WHO) has been advocating for better coordination to promote infection control and appropriate antimicrobial use, to help fill knowledge gaps and to develop new drugs and vaccines more effectively.Footnote 28, Footnote 57 At the 51st World Health Assembly in 1998 and in the subsequent report, Overcoming Antimicrobial Resistance, WHO stated its concern "about the rapid emergence and spread of human pathogens resistant to available antibiotics" and urged member states to implement policies to address the problem of antimicrobial resistance.Footnote 102 In 2001, the WHO Global Strategy for Containment of Antimicrobial Resistance emphasized the need for member states to address a number of principles and actions for reducing and containing the problem of antimicrobial resistance.Footnote 28 Further, in 2008 the WHO Advisory Group on Integrated Surveillance of Antimicrobial Resistance (WHO-AGISAR) was established to help minimize the public health impact of antimicrobial resistance associated with animal, food and human sectors.Footnote 103, Footnote 104 As part of the 2011 World Health Day, which focused on antimicrobial resistance, policy packages were developed to help countries and governments reduce inappropriate use of antimicrobials in people and animals and stop the spread of antimicrobial resistance.Footnote 105, Footnote 106
Within Canada, the Public Health Agency of Canada coordinates national efforts to prevent and control infectious diseases, including those due to antimicrobial-resistant organisms; Health Canada regulates antimicrobials for sale for people and animals; the Canadian Institutes of Health Research promotes research in all aspects of infectious disease including antimicrobial resistance and strategies to combat it; and the Canadian Food Inspection Agency, in addition to working with the Public Health Agency of Canada and Health Canada to monitor antimicrobial resistance through CIPARS, also verifies that medicated livestock feeds meet federal standards.Footnote 6, Footnote 107-Footnote 109 Provincial and territorial ministries of health and agriculture and various professional organizations (the Canadian Veterinary Medical Association, the Association of Medical Microbiology and Infectious Disease Canada, Ontario Medical Association) and non-governmental organizations (the Canadian Bacterial Surveillance Network, the Canadian Antimicrobial Resistance Alliance and the Northern Antibiotic Resistance Partnership) are all involved in the control of antimicrobial resistance, through education and the setting of standards and guidelines.Footnote 110-Footnote 114
Actions for success
Antimicrobial resistance will continue to occur. The challenge is to limit unnecessary pressures that promote the development of antimicrobial resistance and to continue to develop solutions to manage current and future problems.
- The appropriate use of antimicrobial agents in both human and veterinary medicine only as needed is key to reducing the development of antimicrobial resistance.
- Robust monitoring of antimicrobial use in hospitals and the community, as well as agriculture and aquaculture, can enrich resistance and disease surveillance data.
- The search for new, effective antimicrobials is essential to keep infectious diseases from becoming a major cause of morbidity and mortality.
Page details
- Date modified: