Chapter 4: The Chief Public Health Officer's Report on the State of Public Health in Canada, 2009 – Social and physical influences on health
Chapter 4 - Social and Physical Influences on Health
Many factors contribute to the health outcomes experienced by Canadian children. Outcomes can be influenced by environments, experiences, cultures and other factors (the determinants of health). In addition, the ability to learn and to be resilient, and developmental growth in areas such as social skills and emotional maturity, are all influenced by a combination of factors in early life.footnote 161 Economic and social determinants such as income, education, social connectedness and behaviour have both direct and indirect bearings on health.footnote 216
Socio-economic status
While many Canadian children are experiencing the conditions necessary for positive outcomes, such as adequate income, food security and acceptable housing, it is more difficult for some families and communities to provide these conditions. The socio-economic environment in which a child lives can create circumstances of advantage or disadvantage for the child.footnote 161
A family's income level and level(s) of individual education in the household, combined with other social factors, establish their SES. Inequalities in SES have been shown to be linked to subsequent inequalities in health outcomes.footnote 220
Children born into a low SES environment tend to have a higher than average likelihood of being born at low birth weight and experiencing disability and disease, as well as behavioural problems and mental health disorders that can lead to a lifetime of poor health.footnote 221 In fact, inequalities in health outcomes exist at every level of the socio-economic scale, with those in each income quintile lower than the highest often experiencing worse health outcomes than those in the quintile(s) above. In this sense, it can be said that disparities in health affect those at every level of the economic gradient to some extent, and not just those considered to be worst off.30 For example, birth data from Quebec neighbourhoods over a 10-year period show a relationship between household income and birth outcomes. Figure 4.1 shows that the greater the percentage of households with income below the low-income cut-off in a neighbourhood, the higher the percentage of babies born prematurely or small for their gestational age.footnote 222
Socio-economic status (SES) refers to an individual's or group's position within society. It is dependent on a combination of variables, including occupation, education, income, wealth and place of residence.footnote 217 SES and health status share a close relationship, where generally health improves as SES rises and deteriorates as SES falls. Poverty, which can be measured by income and consumption, is a term which many use interchangeably with low SES, however, references to poverty often fail to encompass the greater scope of challenges and obstacles that accompany a lower status within society.footnote 30 footnote 218 This includes social exclusion or the ability to be a part of society.footnote 30 footnote 218 Social exclusion is a “short-hand term for what can happen when people or areas face a combination of linked problems such as unemployment, discrimination, poor skills, low incomes, poor housing, high crime, bad health and family breakdown” creating a cyclical pattern of disadvantage.footnote 219
From infancy through to adulthood, low SES is an important influence for some of the most common chronic diseases, including coronary heart disease, Type 2 diabetes and chronic obstructive pulmonary disease.footnote 23 Other risk factors associated with disease – such as diet during pregnancy, infant feeding and indoor/outdoor air quality – are conditions to which those with lower SES are also known to be more vulnerable.footnote 23
For those who experience low SES, the timing and duration of those experiences also matter, with the earliest years of a child's life being critical.footnote 223 footnote 224 One reason is that childhood is the period when physical, emotional and cognitive patterns are established – including the value we place on ourselves and others, and the way we behave. Negative patterns are more likely to persist into adulthood if there is no change in SES variables or no intervention to mitigate the effects of low income.footnote 23
| Value | Description | Year | |
|---|---|---|---|
| Socio-economic status | |||
| Children living in low-income (after tax)Footnote 1.1 | 12.4 | percent of population aged 0 to 11 years | 2006 |
| People reporting food insecurityFootnote *Footnote 1.2 | 10.4 | percent of households with children in the previous year | 2004 |
| Unable to access acceptable housingFootnote *Footnote 1.3 | 12.7 | percent of households | 2006 |
| Parental educationFootnote *Footnote 1.6 | 96.1 | percent of households with the highest level of education being high school or greater | 2007 |
| Home, school and community | |||
| Family functioningFootnote *Footnote 1.5 | 8.7 | percent of children aged 0 to 5 years in families with high levels of dysfunction | 2004–2005 |
| Parental depressionFootnote *Footnote 1.5 | 10.0 | percent of children aged 0 to 5 years whose primary care giver exhibits high levels of depression | 2004–2005 |
| MaltreatmentFootnote *Footnote 1.6 | 22.1 | substantiated cases per 1,000 population, birth to 11 years, excluding Quebec | 2003 |
| Regular family physicianFootnote *Footnote 1.6 | 92.1 | percent of households with children aged 0 to 11 years | 2007 |
| Low on at least one school readiness domainFootnote *Footnote 1.4 | 27.5 | percentage of national cohort of senior kindergarten-level children | 2006 |
| Neighbourhood cohesionFootnote *Footnote 1.5 | 13.6 | percent of children aged 0 to 5 years living in neighbourhoods with low neighbourhood cohesion | 2004–2005 |
| Neighbourhood safetyFootnote *Footnote 1.5 | 22.3 | percent of children aged 0 to 5 years living in neighbourhoods with low neighbourhood safety | 2004–2005 |
| Healthy behaviours | |||
| Adult behaviours | |||
| Breastfeeding (initiation)Footnote *Footnote 1.6 | 90.3 | percent of women who gave birth in the past 5 to 14 months | 2006–2007 |
| Breastfeeding (6+ months)Footnote *Footnote 1.6 | 53.9 | percent of women who gave birth in the past 5 to 14 months | 2006–2007 |
| Smoking during last 3 months of pregnancyFootnote *Footnote 1.6 | 10.5 | percent of women who gave birth in the past 5 to 14 months | 2006–2007 |
| Alcohol consumption during pregnancyFootnote *Footnote 1.6 | 10.5 | percent of women who gave birth in the past 5 to 14 months | 2006–2007 |
| Child behaviours | |||
| Physical activity (7+ hours per week)Footnote 1.1 | 84.3 | percent of children aged 6 to 11 years | 2004 |
| Screen time (less than 1 hour per day)Footnote 1.1 | 20.9 | percent of children aged 6 to 11 years | 2004 |
| Fruit and vegetable consumption (5+ times per day)Footnote 1.1 | 41.3 | percent of children aged 2 to 17 years | 2004 |
Note: More detailed information can be found in Appendix E: Definitions and Data Sources for Indicators. |
|||
Figure 4.1 Percentage of adverse birth outcomes by neighbourhood quintile, Quebec, 1991 to 2000 footnote 222
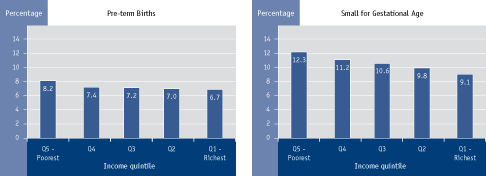
Textual Equivalent - Figure 4.1
Summary: The percentage of pre-term births in Quebec from 1991 to 2002 ranged from 8.2 in the poorest neighbourhood quintile to 6.7 in the richest. The percentage of births where the child was small for their gestational age in Quebec from 1991 to 2002 ranged from 12.3 in the poorest neighbourhood quintile to 9.1 in the richest.
Source: Luo, Z.-C., Wilkins, R., & Kramer, M. S. (2006).
| Birth outcome | Quintile 5, Poorest |
Quintile 4 | Quintile 3 | Quintile 2 | Quintile 1, Richest |
|---|---|---|---|---|---|
| Preterm | 8.2 | 7.4 | 7.2 | 7.0 | 6.7 |
| Small for gestational age | 12.3 | 11.2 | 10.6 | 9.8 | 9.1 |
Footnote:
Q - population divided into fifths based on the percentage of the population in their neighbourhood below the low-income cut-offs.
Source: Luo, Z.-C., Wilkins, R., & Kramer, M. S. (2006).
Adequate income
Although poverty is a concept that extends beyond income, in the absence of a standardized indicator to measure the complex mix of factors that define it, income indicators are often used as proxy measures of poverty. The most commonly used indicator within Canada is the low-income cut-off (LICO), which considers a family's portion of income spent on food, clothing and footwear, and shelter relative to other families of the same size and geographic location.footnote 229 footnote 230
Based on the LICO, an estimated 12% of Canadian children under the age of 12 were living in poverty in 2006.footnote 230 Although this is an improvement over rates estimated to be as high as 20% in the 15-year period between 1991 and 2006 (see Figure 4.2), it still represents a significant proportion of children in this age group and demonstrates that the problem of inadequate income persists in Canada.
Poverty as defined by the United Nations is “a human condition characterized by the sustained or chronic deprivation of the resources, capabilities, choices, security and power necessary for the enjoyment of an adequate standard of living and other civil, cultural, economic, political and social rights.”footnote 225
Figure 4.2 Estimated proportion of children, aged 0 to 11 years, living in low-income households, Canada, 1991 to 2006 footnote 227
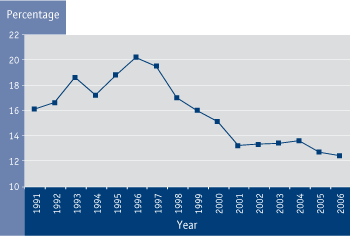
Textual Equivalent - Figure 4.2
Summary: Between 1991 and 1996 the percentage of children aged 0 to 11 years living in low-income households increased from 16% to 20%. Between 1996 and 2006 the percentage of children aged 0 to 11 years living in low-income households has decreased to 12%.
Source: Statistics Canada.
| Year | Proportion |
|---|---|
| 1991 | 16.1 |
| 1992 | 16.6 |
| 1993 | 18.6 |
| 1994 | 17.2 |
| 1995 | 18.8 |
| 1996 | 20.2 |
| 1997 | 19.5 |
| 1998 | 17.0 |
| 1999 | 16.0 |
| 2000 | 15.1 |
| 2001 | 13.2 |
| 2002 | 13.3 |
| 2003 | 13.4 |
| 2004 | 13.6 |
| 2005 | 12.7 |
| 2006 | 12.4 |
Source: Statistics Canada.
LICO-based poverty rates have been estimated to be even higher among certain Canadian populations, including children living with disabilities (one in four), children in families who have recently immigrated to Canada (one in two) and Aboriginal children living inside and outside First Nations communities (1 in 4 and 1 in 2.5 respectively).footnote 229 A 2006 survey showed significant differences between Aboriginal and non-Aboriginal children under the age of six living in urban areas as defined by census metropolitan areas (CMAs). While more than 20% of non-Aboriginal children in CMAs were living in low-income families, rates for Aboriginal children were higher (57% of First Nations, 45% of Inuit and 42% of Métis children).footnote 185
Internationally, a measure which considers a family's income after tax and transfers relative to the median income of similar-sized families within a country is often used to compare poverty rates between countries. Using this indicator, a 2007 study ranked Canada 15 out of 24 OECD countries in terms of children living in relative poverty. The countries with the lowest relative child poverty rates were Denmark, Finland and Norway.footnote 230–footnote 232 The study also showed that between 1994 and 2000 Canada saw only a minimal decrease (0.4%) in its poverty rate.footnote 230 231
In addition to the persistence of poverty among Canadian children, the gap between families with the highest and lowest incomes has been increasing over time. (see Figure 4.3).
Figure 4.3 Ratio of richest and poorest deciles*, families raising children in Canada, 1976 to 2004 footnote 233
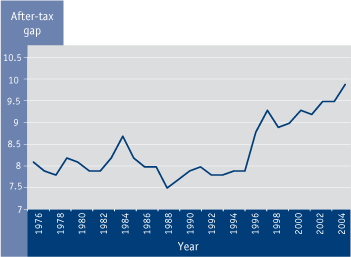
Textual Equivalent - Figure 4.3
Summary: Fluctuations in the gap between the 10% of families with the highest after-tax income and the 10% of families with the lowest after-tax income can be seen during the 20-year period between 1976 and 1996, while remaining fairly constant on average. However, since a sudden increase in 1996, a steady rise in the gap can be noted that is partially attributed to the wealthiest families benefiting disratioately from a strong economy.
Source: Yalnizyan, A. (2007).
| Year | Ratio |
|---|---|
| 1976 | 8.1 |
| 1977 | 7.9 |
| 1978 | 7.8 |
| 1979 | 8.2 |
| 1980 | 8.1 |
| 1981 | 7.9 |
| 1982 | 7.9 |
| 1983 | 8.2 |
| 1984 | 8.7 |
| 1985 | 8.2 |
| 1986 | 8.0 |
| 1987 | 8.0 |
| 1988 | 7.5 |
| 1989 | 7.7 |
| 1990 | 7.9 |
| 1991 | 8.0 |
| 1992 | 7.8 |
| 1993 | 7.8 |
| 1994 | 7.9 |
| 1995 | 7.9 |
| 1996 | 8.8 |
| 1997 | 9.3 |
| 1998 | 8.9 |
| 1999 | 9.0 |
| 2000 | 9.3 |
| 2001 | 9.2 |
| 2002 | 9.5 |
| 2003 | 9.5 |
| 2004 | 9.9 |
Footnote:
*Deciles refer to the division of families raising children in Canada into tenths based on their after-tax income.
Source: Yalnizyan, A. (2007).
Figure 4.3 represents the gap between the 10% of families with the highest after-tax income and the 10% of families with the lowest after-tax income. Fluctuations in the gap can be seen during the 20-year period between 1976 and 1996, while remaining fairly constant on average. However, since a sudden increase in 1996, a steady rise in the gap can be noted that is partially attributed to the wealthiest families benefiting disproportionately from a strong economy.233 In 2004, families with incomes in the highest 10% after tax were earning 10 times the after-tax income of families with incomes in the lowest 10% after tax. This difference is significant because larger gaps are associated with greater differences in the health of a population.234 Given what is known about the relationship between income and health, we could expect that this widening gap will perpetuate and further increase existing inequalities in health and developmental opportunities between children in low- and high-income households.
Influence of Income on Childhood Development
Canadian researchers have reported that family income plays a significant role in influencing child development.228 Of 27 factors identified as having an impact on child development, up to 80% were seen to improve as family income increases.228 Compared to children living in higher-income families, research has shown children in low-income families to be:
- twice as likely to be living in poorly functioning families (i.e. in terms of family stability, supportive relationships and protection);
- more likely to live in substandard housing and problem neighbourhoods (i.e. those where negative activities such as drug use/dealing, burglaries and unrest due to cultural differences are common);
- more likely to demonstrate high levels of indirect aggression;
- over two and a half times more likely to have a problem with one or more basic abilities such as vision, hearing, speech or mobility;
- more likely to exhibit delayed vocabulary development; and
- less likely to participate in organized sport (a measure of cultural and recreational activities within their communities).228
Food security
One of the possible repercussions of living in relative poverty is being food insecure. Someone is food insecure if he or she does not have physical and economic access to sufficient, safe and nutritious foods to meet the needs of a healthy and active life.footnote 235 In 2004, 10% of Canadian households with children reported being food insecure at some point in the previous year as a result of financial challenges. Although in many cases it was the adults in those households who experienced food insecurity, in 5% of all households with children, one or more of the children themselves were food insecure. Among children in Aboriginal households, 23% reported experiencing food insecurity.footnote 236
When children go to school hungry or poorly nourished, their energy levels, memory, problem-solving skills, creativity, concentration and behaviour are all negatively impacted. As a result of being hungry at school, these children may not reach their full developmental potential – an outcome that can have health impacts throughout their lives.
Housing and water
Shelter is a basic need for optimal health. Inadequate housing can result in numerous negative health outcomes, ranging from respiratory disease and asthma due to moulds and poor ventilation, to mental health impacts associated with overcrowding.237–footnote 239 The issue of overcrowding is especially true for First Nations and Inuit populations in Canada.footnote 132 footnote 240 In 2006, an estimated 15% of the First Nations population were living in overcrowded homes, a rate five times higher than the non-Aboriginal population.footnote 132
The Canada Mortgage and Housing Corporation defines acceptable housing as that which is “adequate in condition, suitable in size, and affordable” (see Appendix E).footnote 241 Although the number of children, or families with children, living in unacceptable housing is unknown, data shows that 13% of all Canadian households were unable to access acceptable housing in 2006.footnote 241
Access to safe drinking water is also important. In March 2008, 1,766 cities, small towns and neighbourhoods in Canada were under boil water advisories, as were 93 First Nations communities.footnote 242 Parasites found in some water supplies, such as Giardia and Cryptosporidium, can cause stomach cramps, nausea, fever, as well as vomiting and diarrhea that can lead to dehydration.footnote 243 E. coli., another bacteria associated with boil water advisories, is known to cause a specific type of kidney failure, hemolyticuremic syndrome (HUS), in 10% to 15% of infected children.footnote 244
Home, school and community environments
While children's health and social outcomes are associated with family income and other basic needs, living in poverty is also about “poverty of opportunity”.footnote 228 Nurturing caregivers, positive learning environments, access to health care, good nutrition and social interaction with other children all contribute to early physical and social development in ways that can positively affect health and well-being over a lifetime.footnote 30 footnote 161 The origin of these influences is the home or family environment, with the broader social and school environments playing an increasing role as children grow. If the experiences in these environments are positive and a child's needs are being met to a degree necessary for optimal development, it can be expected that this will set the child on a path toward positive health outcomes, especially since supportive environments have been shown to mitigate the negative effects associated with low income.
Family influences
Preschool-age children spend the majority of their time with family. The functioning of both the parents and the family as a whole can influence the health of the children in the family. For example, the mental health of a child's parent or primary caregiver can directly impact the care of that child and therefore the child's health. The majority of Canadian children are reported to live in well-functioning families and do not have a parent who suffers from a mental illness.footnote 14 However, the 2004/05 National Longitudinal Survey of Children and Youth (NLSCY) found that 10% of children aged 0 to 5 years had a parent who exhibited high levels of depression.footnote 14 The same survey found that 9% of children in that age group were living in families with high levels of dysfunction as measured in terms of problem solving, communication, roles, effective responsiveness and behaviour.footnote 14 These children are more likely to experience relationship, behavioural and emotional problems than their peers in functional families.footnote 14 In an earlier analysis of NLSCY data, anxiety in children aged 2 to 5 years was more likely in dysfunctional families and those with a depressed parent.245 Children in this age group who had a parent suffering from depression were also more likely to show higher levels of aggressive behaviour.footnote 245
Abuse and neglect
Child maltreatment includes direct and indirect acts that can harm a child, including physical abuse and neglect, emotional abuse and neglect, sexual abuse and exposure to family violence.footnote 246 Childhood abuse and neglect is a worrisome problem in Canada. According to the Canadian Incidence Study of Reported Child Abuse and Neglect (CIS), case numbers doubled between the 1998 and 2003 datacollection cycles. Some of this growth may be attributable to changes in awareness, legislation, data collection and/ or increases in maltreatment rates.footnote 246 In 2003, there were more than 75,000 substantiated cases of maltreatment among Canadian children aged 0 to 11 years – equivalent to 22 cases per 1,000 population for that age group (see Figure 4.4). The majority involved exposure to domestic violence and neglect as the primary form of abuse, and in almost all cases the perpetrator (or at least one, if there was more than one perpetrator) was a relative of the child.footnote 246 Most at risk of maltreatment are those living in households with a single or disabled parent, low income, low levels of education or high unemployment, or overcrowding. In many cases, more than one of these factors is present.footnote 246–footnote 249 Evidence shows that maltreatment can have adverse repercussions in childhood, later in life and across generations. Not only can maltreatment result in physical injuries, sexually transmitted infections and emotional disorders, but research now shows that experiencing maltreatment in childhood is linked to illnesses in adulthood such as fibromyalgia, irritable bowel syndrome, chronic lung disease and cancer.footnote 250
In 2003, just over 9% of all substantiated cases of maltreatment among children aged 0 to 11 years involved those in their first year of life.footnote 246 Even before birth, a child can be at risk. It is estimated that 6% of women in Canada are physically abused during pregnancy.footnote 251footnote 252 Outcomes for the fetus following severe blunt force trauma to the abdomen of a pregnant woman can include: skull fractures, intracranial hemorrhage and bone fractures; placental abruption; pre-term labour and delivery; spontaneous abortion; and fetal death.footnote 253footnote 254
Abuse and neglect can have immediate and long-term repercussions. In childhood, factors that contribute to a child's development (having a sense of control, being loved and feeling socially connected) can become compromised.footnote 22 footnote 30 When relatives are perpetrators of the abuse and neglect, a child's sense of trust, dependency and protection can be threatened.footnote 255
Research shows that adverse childhood experiences may disrupt neurodevelopment with lasting effects on overall brain structure and function.footnote 22 footnote 256 As the number of adverse experiences increases, these impacts may be compounded and the risk of later health and social issues rises.footnote 22 256 Child maltreatment has been associated with low school grades, school failure and dropping out.footnote 257 According to the Street Youth in Canada survey, 30% of street youth, aged 15 to 24 years, have experienced some form of neglect in their past.footnote 258 There is also an association between severe and habitual physical punishment by parents or guardians and the development of violent behaviour patterns in children and youth subjected to this punishment.footnote 259
Exposure to family/domestic violence is one of the most common forms of maltreatment experienced by Canadian children. Exposure to family violence can have long-lasting negative effects on children, including an increased likelihood to exhibit hyperactive behaviour, have emotional disorders and be physically aggressive.footnote 260 Girls who have been exposed to or experienced abuse in childhood sometimes continue the cycle as victims of partner/spousal abuse, whereas boys who have been exposed to or experienced a form of abuse are more likely to become abusers in adolescence and adulthood.footnote 259 It is important to note, however, that among individuals who have experienced child abuse many do not go on to abuse others. Factors such as receiving emotional support from a non-abusive parent during childhood, receiving therapy at any point during their lives, and having a stable, emotionally supportive and satisfying relationship with a partner in adulthood, may serve to prevent them from being abusive toward their own children and partners.footnote 261
Bullying among peers is also a problem in Canada. In 2000, 12% of children aged 10 and 11 years reported being bullied “at least some of the time” at school. Children in families with lower incomes (below $40,000 per year), experience higher rates of bullying than children in higher-income households – 20% compared to 9% respectively.footnote 262 With increased Internet use, some bullying (known as cyber-bullying) is now being done online as well as in the school yard. In 2001, 25% of young Canadian Internet users, aged 9 to 17 years, reported receiving e-mails containing hateful messages about others.footnote 263
In terms of health outcomes, both aggressors and victims of childhood bullying are at greater risk for experiencing emotional, social and psychiatric problems that can persist into adulthood.footnote 262 footnote 264 Research indicates that playground bullying can be an indicator of future negative behaviours such as sexual harassment, workplace harassment, dating and marital aggression, and child and elder abuse.footnote 262 And although cyber-bullying is a relatively new phenomenon, a recent international report indicated that cyber-bullying contributes negatively to the psychosocial functioning of children.footnote 265
Figure 4.4 Substantiated maltreatment cases by primary category and sex, Canada excluding Quebec, 2003 footnote 141 footnote 246
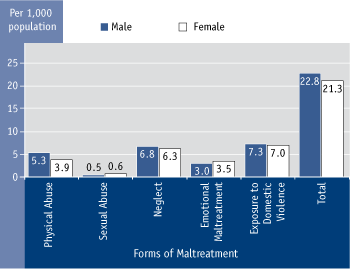
Textual Equivalent - Figure 4.4
Summary: In 2003 the number of substantiated maltreatment cases per 1,000 population aged 0 to 11 years in Canada, excluding Quebec, associated with physical abuse were 5.3 for males and 3.9 for females; sexual abuse were 0.5 for males and 0.6 for females; neglect were 6.8 for males and 6.3 for females; emotional maltreatment were 3.0 for males and 3.5 for females; exposure to domestic violence were 7.3 for males and 7.0 for females; and total substantiated cases of maltreatment were 22.8 for males and 21.3 for females.
Source: Public Health Agency of Canada.
| Form of maltreatment | Cases per 1,000 population, male | Cases per 1,000 population, female |
|---|---|---|
| Physical Abuse | 5.3 | 3.9 |
| Sexual Abuse | 0.5 | 0.6 |
| Neglect | 6.8 | 6.3 |
| Emotional Maltreatment | 3.0 | 3.5 |
| Exposure to domestic Violence | 7.3 | 7.0 |
| Total | 22.8 | 21.3 |
Source: Public Health Agency of Canada.
Early care and development
Parents who spend time away from their children, for work, education or other reasons, rely on others to provide positive environments for their children in their absence. Options that provide opportunities for early learning and social interaction with other children can contribute to early physical and social development in ways that can positively affect a child's health and wellbeing over a lifetime.footnote 22 footnote 161
Canadian parents make use of various forms of both regulated and non-regulated child care. Concrete measures of need and unmet need for such care in Canada are not available, but some information on availability of regulated child care spaces and the use of different child care options exists. Data from 2002–03 shows that 54% of Canadian children between the ages of six months and five years were in some form of non-parental care (both regulated and non-regulated). The most common forms of care were with a non-relative outside the home, excluding daycare centres (30%), with a relative either inside or outside the home (30%) and in a daycare centre (28%).footnote 266 Although there has been some recent growth in Canada's regulated child care, there were enough regulated spaces for only 17% of all Canadian children aged 0 to 12 years in 2006.footnote 267
While these care options supplement and complement each other, it is difficult to determine whether all needs are being met and, in particular, whether quality care is universally available. The general quality of both formal and informal child care centres is unclear, although some indicators of quality have been established to help evaluate regulated, formal child care centres in Canada. These include measurements such as staff training, wages, funding and care. Data on these factors, along with past studies on Canadian child care, show that the quality is generally rated as mediocre.footnote 268–footnote 270
Additionally, barriers to care may exist due to financial limitations or developmental relevance. Although all provinces and territories provide subsidies to offset the costs of regulated child care, the level of those subsidies, the programs for which they apply and eligibility criteria differ across jurisdictions.footnote 271 As a result, some parents in need of financial support may still face considerable out-of-pocket expense, while others will incur no personal costs, creating financial barriers and inequalities in access.footnote 271 Barriers also exists for access to culturally and developmentally relevant care. It is estimated that 90% of Aboriginal families with children do not have access to regulated infant development or early childhood programs with an Aboriginal component.footnote 18 footnote 272 Data from British Columbia also shows that after-school programming for older children (aged 9 to12 years) is not meeting the needs of that age group.footnote 273 Parents of those children reported barriers to care and developmentally appropriate activities for their children in the hours outside of school, with one in five reporting that such programs were not available in their community.footnote 273 More than 10% of the children in the British Columbia study reported being in unsupervised or self-care between the hours of 3:00 p.m. and 6:00 p.m.footnote 273
Recognizing the importance of early childhood services to child development, the United Nations Children's Fund (UNICEF) has developed a set of 10 benchmark indicators to determine the level of these services in affluent OECD countries. The benchmarks fall into four broad categories of policy framework, access, quality, and supporting context. In UNICEF's first related report, which considered childhood services in 25 countries, Sweden met all ten benchmarks and Iceland met nine, while Canada and Ireland were the only two countries reported to meet the minimum standard for only one out of the ten benchmarks.274 These first results must be interpreted with caution due to limitations in the data and indicators, such as the measurement of minimum standards rather than level of quality, the lack of inclusion of informal home-based or neighbourhood daycare, no account of other services for children at risk, and no measure of parental involvement.footnote 274 However, the implication that Canada is behind other countries in providing key services for positive early childhood development remains.
Access to primary care
When families have access to primary health care, they may access preventative, diagnostic and treatment options which may otherwise be unavailable. The vast majority of children in this country have access to such care. In Canada, 92% of surveyed families with children under the age of 12 reported that they had access to a general practitioner in 2007.footnote 275 However, this number does not account for those families who may be the most vulnerable to access barriers (i.e. those living in situations or locations that prevent them from being included in the survey due to a lack of phone access or permanent address). Additionally, barriers such as language, physical inaccessibility, remoteness or cost of non-insured health services (such as eye or dental care) may prevent families and children from accessing necessary services.276 footnote 277 Aboriginal peoples and recent immigrants have been known to face such barriers in Canada.footnote 276 footnote 278
Access to dental care is equally important to the health of children. Dental health established in childhood affects not only the immediate health of a child, but also continues to impact oral and overall health in adulthood.footnote 279 The pain associated with tooth decay can affect a child's sleep, behaviour and eating, which in turn can affect their overall health.footnote 280 Healthy baby teeth are necessary for the healthy development of adult teeth.footnote 279 If poor dental health persists into adulthood, there is the possibility of serious health consequences such as respiratory disease, diabetes, heart disease, and experiencing pre-term births and lower birth weights.footnote 281 While there is no data to show the number of Canadian children who are not receiving dental care, information exists that suggests that access varies across the country. Dental care is not universally covered under the Canada Health Act and is therefore privately funded for the most part. In addition to limited public funding for dental screening and treatment programs, other barriers to dental health include the availability of services, stigma associated with accessing dental services through social assistance, cultural barriers, and additional costs associated with travel and time off work.footnote 282
School readiness
One way to consider the degree to which early childhood education and developmental opportunities benefit a child, a community or even a country is to look at the number of children who are "school ready" upon reaching kindergarten age. This measurement is based on levels of knowledge, skills, maturity, language and cognitive development, and can be interpreted as representative of the cumulative effects of many early influences on a child's life. It also offers a discrete way to describe the complex interactions of events, influences and outcomes contributing to a child's overall health.
The early development instrument (EDI) is one means of assessing school readiness in children. This instrument, used within several Canadian provinces as well as internationally, measures a child's development in each of five domains: physical health and well-being; social competence; language and cognitive development; emotional maturity; and communication skills and general knowledge.footnote 283 In 2006, a national cohort of more than 100,000 children at the senior kindergarten-level in seven provinces (average age of 5.7 years) was assessed using the EDI. Over one-quarter (28%) were classified as "vulnerable" on at least one domain, meaning they scored in the lowest 10% of children at their site for that domain, and almost 14% were vulnerable in two or more domains.footnote 284
Results for the national cohort also showed statistically significant differences in mean domain scores among different groups of children. For all five domains:
- Aboriginal children, on average, had lower mean scores than non-Aboriginal children;
- children who had attended an organized part-time preschool or nursery school had higher mean scores than those who had not; and
- those who had attended junior kindergarten had higher mean scores than those who had not.footnote 283 footnote 284
The data also suggest that children who are not school ready by kindergarten level will continue to perform below their peers as they move through the school system. It was found that the greater the number of numeracy or reading EDI vulnerabilities identified in kindergarten children, the more likely they were to fail the standardized Foundation Skills Assessment in Grade 4.footnote 285 Given that education is a foundation for improved lifelong health prospects, children who are ill-prepared for school are more likely to experience poorer health along their lifecourse than their more well-prepared peers.footnote 16
Neighbourhood characteristics
Defining a safe neighbourhood as one where a child is protected from violence, abuse, exploitation, injuries and neglect at home, school and in the community, it is difficult to determine whether or not a child's neighbourhood is safe.footnote 286 However, even the perception that it is unsafe can lead to health consequences. For example, the perceived safety of a child's neighbourhood can influence levels of physical activity (e.g. less use or availability of bicycle paths, parks and other recreational spaces) with resulting health outcomes for children.footnote 287 footnote 288 One study found that children living in a neighbourhood that their parents perceived to be unsafe were more likely to be overweight at age seven (the impact of the built environment on overweight/obesity is discussed in Chapter 5).footnote 289 Although most primary caregivers surveyed for the 2004/05 NLSCY indicated that they felt their neighbourhoods were safe, more than one-fifth (22%) of those with children between the ages of 0 and 5 years felt they lived in neighbourhoods with a low degree of safety.footnote 14 Neighbourhood cohesion is an indicator of a person's perception of their neighbours and the sense of support they feel from those neighbours. The 2004/05 NLSCY data also showed 14% of primary caregivers of children aged 0 to 5 years report low neighbourhood cohesion. This indicator has been linked to higher levels of conduct disorder, hyperactivity, emotional disorder and non-sports related injuries among children aged 4 to 11 years.footnote 290
Environmental exposures
Children are at risk from harmful exposures during the early years of life (e.g. air pollution, prolonged exposure to ultraviolet radiation from the sun). While many environmental exposures are not well documented, there is enough information available to highlight a number of areas. One adverse exposure for which there are prevalence data and evidence of health impact is environmental tobacco smoke. In 2007, 7% of Canadian children aged 0 to 11 years were reported to be exposed to second-hand smoke at home.footnote 291 These children are more likely to die from SIDS or to develop health conditions such as asthma, ear infections or lower respiratory tract problems than unexposed children. It has also been shown that a child's cognitive abilities may be affected by exposure to second-hand smoke.footnote 292
For other exposures, some knowledge of the negative health outcomes associated with them exists but the extent to which children in Canada are exposed is unknown. Exposure to mould is a concern because it can contribute to allergic reactions and respiratory diseases. In fact, symptoms of asthma can be worsened by exposure to a range of contaminants, including mould, found in indoor and outdoor air.footnote 293–295 Young children are also affected by exposure to even very low levels of lead, which can cause learning disabilities and other harmful effects on their development.293 footnote 296 footnote 297 There is also evidence that parental occupational exposure to pesticides may be associated with certain childhood cancers.footnote 298–301 For both developing fetuses and young children, there are negative health risks associated with exposure to methyl mercury through either direct consumption or maternal consumption of fish.footnote 302 Currently, the Government of Canada is moving forward with proposed regulations to prohibit the advertisement and importation of polycarbonate plastic baby bottles that contain bisphenol A, as well as preventing the use of six types of phthalate chemicals in manufacturing soft vinyl toys and child-care products given their potential for negative health effects.footnote 303–306
Healthy behaviours
Behaviours on the part of both parents and children can have an impact on child health. Parental behaviour, whether negative or positive, can have a corresponding influence on a child's health from conception, through critical fetal development periods and infancy, to later childhood.
Adult behaviours
Breastfeeding
Maternal practices such as breastfeeding can positively influence an infant's start in life. The benefits to children of breastfeeding include a reduced risk of asthma, obesity and fewer cases of ear infections.footnote 307–309 Canada's breastfeeding initiation rates have increased dramatically over the last four decades (25% of mothers initiated breastfeeding in 1965 compared to 90% of mothers in 2006-07).footnote 310 footnote 311 Breastfeeding initiation rates vary among populations, however, and are generally lower for younger mothers (76% of those aged 15 to 19 years), single mothers (78%), Aboriginal off-reserve mothers (82%) and First Nations on-reserve mothers (63%), and higher among immigrant mothers (92%).footnote 275 footnote 312 Breastfeeding exclusively for a minimum of six months is recommended for healthy full-term infants by the Public Health Agency of Canada, Health Canada and the Canadian Paediatric Society.footnote 312 footnote 313 In 2005, just over half of Canadian mothers reported breastfeeding for six months or more, but only 14% did so exclusively.footnote 311 footnote 314
Smoking
While efforts to reduce the smoking rates of parents during pregnancy have had an impact in recent years, there are still some parents in Canada who smoke while pregnant.footnote 311 footnote 315 In 2006–07, 11% of Canadian women reported smoking during the last three months of their pregnancy and nearly 17% reported smoking during the first year after birth.footnote 311 In 2002–03, more than one-third (37%) of First Nations mothers on reserve reported smoking during pregnancy.footnote 50 footnote 316 Health risks are present with maternal exposure to second-hand smoke during pregnancy as well. About 25% of women who gave birth in 2006–07 reported living with someone who smoked during their pregnancy.footnote 311 Evidence shows that the shortterm health impacts and complications associated with this behaviour include higher rates of miscarriage, preterm birth and SIDS.317 Longer-term impacts for children include increased risk of ear and respiratory infections, asthma and learning difficulties.footnote 50 footnote 317 footnote 318
Alcohol and drugs
As with smoking, alcohol consumption during pregnancy has declined in recent years.footnote 312 In 2006–07, the Maternal Experiences Survey (MES) asked women about their drinking habits during pregnancy. Nearly 11% percent of women who had been pregnant reported drinking some amount of alcohol during their last pregnancy.footnote 311 Of these women, 1% consumed alcohol more than once a week.footnote 311 A serious consequence of consuming alcohol during pregnancy is giving birth to a child with Fetal Alcohol Spectrum Disorder (FASD). Approximately 1% of all babies in Canada (more than 3,000 per year) are born with FASD.footnote 319 This estimate is thought to be low since the signs and symptoms associated with FASD are often hard to detect and may very well go unnoticed until later on in life.footnote 320 FASD in children has been linked to learning difficulties and behavioural issues, such as not understanding the consequences of actions and difficulties in social settings.footnote 319 footnote 321–323
As measured by the 2006–07 MES, the use of street drugs (marijuana, cocaine, heroin, ecstasy, sniffing glue, gasoline or other solvents) three months prior to pregnancy is estimated to be 7%, but drops substantially to 1% once the pregnancy is recognized.footnote 311 footnote 324 Prenatal use of drugs, such as heroin and cocaine, can lead to neonatal abstinence syndrome, where the newborn begins life with an addiction to the drug to which he or she was prenatally exposed.footnote 325 This causes immediate withdrawal symptoms after birth, which may include sleep problems, fever, sweating and poor feeding habits.footnote 325 Prenatal cocaine exposure has also been linked to conditions such as oppositional defiant disorder and ADHD.footnote 326
Sexually transmitted infections
Some sexually transmitted infections (STIs) are on the rise among young women in Canada, including human immunodeficiency virus (HIV), syphilis and chlamydia infections, increasing the potential risk of vertical (mother-to-child) transmissions of these infections.footnote 327 footnote 328 For example, cases of congenital syphilis have increased over the past decade from two cases or less to eight cases per year nationally.footnote 329 footnote 330 Although the number of cases of vertical transmission of STIs and viral diseases is small, this type of adverse exposure can threaten the immediate and long-term health of the fetus and newborn.footnote 331 A congenital syphilis infection can lead to miscarriage, still or premature birth, and low birth weight.footnote 148 footnote 332 Over the lifecourse, babies with congenital syphilis may experience hearing loss, developmental delays, and skin and bone abnormalities.footnote 332 footnote 333 Chlamydial infections have been increasing in recent years and are known to cause intrauterine fetal death, low birth weight, eye infections and pneumonia.footnote 334–336
Child behaviours
After children are born, their own behaviours begin to have an impact on their health, although their actions are determined (to a great extent) by their social and physical environment. Physical activity levels, for example, reflect parental behaviours, access to safe play areas and the opportunity to participate in organized sports. Likewise, nutritional behaviours are the result of what foods are available to children in their home. Children who experience poor nutrition and a lack of daily physical activity are more likely to have excess body weight.
Physical activity
While the majority of Canadian children regularly participate in physical activities, 16% of children aged 6 to 11 years are physically active less than seven hours per week, which is less than recommended under Canada's Physical Activity Guidelines for Children and Youth.footnote 179 footnote 337 Research shows that each hour a child spends being sedentary significantly increases their risk of being overweight. In 2004, children aged 6 to 11 years who reported spending more than two hours a day in front of the television or computer were almost twice as likely to be overweight or obese (35%) as their peers who spent an hour or less (18%).footnote 179
Nutrition
Findings on nutritional practices from the 2004 Canadian Community Health Survey indicate that 70% of children aged 4 to 8 years do not meet the minimum recommended daily servings of fruits and vegetables, more than onequarter do not meet the daily minimum grain servings, and more than one-third of those aged 4 to 9 years do not consume the recommended daily minimum servings of milk products or substitutes.footnote 338 footnote 339 Survey results also suggest that 7% of children, aged 4 to 8 years, exceed the suggested percentage of total calories from fat.footnote 338 An increased intake of carbohydrates and simple sugars, larger portion sizes and an increased consumption of high calorie fast foods have all contributed to higher risks for childhood obesity.footnote 188 footnote 340–342 Food affordability also comes into play in making food choices. A greater proportion of Aboriginal families are faced with food affordability issues than non-Aboriginal families, especially in the North where transportation costs factor into higher prices for healthy perishable foods such as milk and fresh fruits.footnote 160 footnote 343 footnote 344
Summary
Most Canadian children experience the conditions necessary for healthy outcomes, such as adequate income, food security, acceptable housing, access to early and late childhood education, and strong connections to family and community. However, certain social and physical influences can have negative impacts on their health. These outcomes may be apparent in childhood and some may persist over the lifecourse, while others may not appear until later in life. For the purposes of this report, three of these factors – SES and developmental opportunities, abuse and neglect, and prenatal risks – will be further examined in Chapter 5 along with three key health issues highlighted in Chapter 3 (mental health and disorders, obesity and unintentional injuries). These six issues represent areas in which there is potential to make a significant difference in the health of Canadian children through interventions to address persistent or worsening trends and to prevent serious long-term negative health outcomes.
Page details
- Date modified: