Page 4: Human Antimicrobial Use Report – 2014 - Physician Diagnosis Data
Physician Diagnosis Data
The Canadian Disease and Therapeutic Index (CDTI) dataset was purchased from IMS Health Canada Inc. and analysed by the Government of Canada. This dataset provides information about the patterns and treatments of disease encountered by office-based physicians (specialists and general practitioners, including those with offices in hospitals) and includes those treatments recommended during hospital rounds. These data are presented over three geographic regions in Canada: West (British Columbia, Alberta, Saskatchewan, and Manitoba); Central (Québec and Ontario), and East (New Brunswick, Newfoundland and Labrador, Nova Scotia, and Prince Edward Island).
The sample of physicians represents all major specialties across Canada. The data is collected using a two-stage stratified design, first stratifying by region and then by physician specialty. Data from 652 physicians were available in 2014, and projection methods were used to extrapolate data to a universe of approximately 57,218 physicians in Canada.
The information contained in this analysis is for drugs for which a physician has provided a recommendation and does not represent actual antibiotics consumed by the patient. Recommendations are not necessarily tied to a prescription as the patient may have been against receiving an antimicrobial prescription, may have not filled out a prescription due to physician orders to wait a period of time, may have chosen not to fill the prescription, the physician may have provided a sample or it represented the continuation of previous prescription renewals. These data do not include patient visits to a primary care nurse. Furthermore, diagnoses or recommendations do not translate into the total number of patients, as some patients visited multiple times for the same reason, or were diagnosed with multiple diseases at a single visit. This information does not look at recommendations provided for multiple antibiotics to treat the individual diagnoses.
Due to the methods of data collection and extrapolation, the sample size may be considered too small for decision making purposes. Furthermore, although data are presented at the per-inhabitant level, these measures do not reflect every inhabitant; they are average values across the entire Canadian population. However, data from these analyses are included to provide a view of antimicrobial recommendation practices in Canada, and to allow experts and data users identify areas where further research may be required.
More detailed information on IMS Health Canada Inc. data collection and the Government of Canada's analytic methods are described in Appendix A.
National diagnosis data
In 2014, Canadian physicians saw patients for more than 297 million diagnoses and provided more than 23 million antimicrobial recommendations for these diagnoses (Table 1.1). This was an increase of approximately 4 million diagnoses between 2013 and 2014, but a decrease of 0.8 million antimicrobial recommendations during this same time frame. In 2014, there were approximately 8.4 diagnoses made per inhabitant in Canada similar to that observed in 2013. Although a similar diagnosis rate was observed in 2014 compared to 2013, the percentage of diagnoses resulting in an antimicrobial recommendation decreased from 8.1% to 7.7%.
Similar to what was observed in 2013, the diagnostic classes with the greatest number of antimicrobial recommendations were upper respiratory tract infections (RTI) (10% of inhabitants receiving a recommendation), lower urinary tract infections (UTI) or cystitis (9% of inhabitants receiving a recommendation) and diseases of the ear (6% of inhabitants receiving a recommendation) (Table 1.1). This is not surprising as these were the 3 most common diagnoses. Therefore, it is expected that the raw number of recommendations would be high for these classes. These classes may be areas to target for further research to assess the appropriateness of antibiotic recommendations. However, it should be noted that the data displayed here are not patient-level data, and therefore cannot be used to determine the proportion of appropriate or inappropriate recommendations.
The diagnostic rates of acute sinusitis, acute bronchitis, and pneumonia were much lower than the upper RTI, UTI, and diseases of the ear (Table 1.1 and Figure 1.1). However, these 3 conditions were the classes most likely to receive an antimicrobial recommendation upon diagnosis. This is likely due to severity of the patient presentation, and the potential for complications.
Figure 1.1: Number of specific diagnoses per inhabitant and the percentage of those diagnoses with recommendations for an antimicrobial in 2014
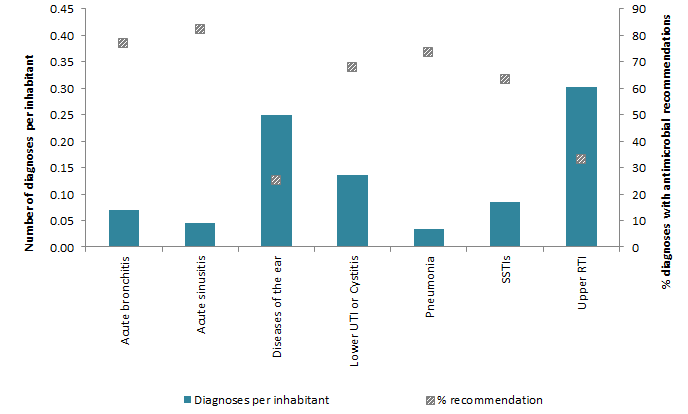
Figure 1.1 - Text Description
| Diagnostic Class | Diagnoses per inhabitant | % diagnoses with recommendations |
|---|---|---|
| Acute bronchitis | 0.07 | 76.79 |
| Acute sinusitis | 0.05 | 82.35 |
| Diseases of the ear | 0.25 | 25.12 |
| Lower UTI or Cystitis | 0.14 | 67.65 |
| Pneumonia | 0.03 | 73.62 |
| SSTIs | 0.08 | 63.32 |
| Upper RTI | 0.30 | 33.19 |
| TOTAL | 8.37 | 7.73 |
Antimicrobial recommendations by diagnostic class
| Diagnostic Class | Total diagnoses | Number of diagnoses per inhabitant | Number of antimicrobial recommendations | Antimicrobial recommendations per 100 inhabitants | % diagnoses with antimicrobial recommendations |
|---|---|---|---|---|---|
Diagnostic classes were removed from this table if they represented < 1% (230,000) of antimicrobial mentions in 2014. These classes were: complications of pregnancy, childbirth, and puerperium; congenital anomalities; diseases of the central nervous system; diseases of the circulatory system; diseases of the sense organs; endocrine, nutritional, metabolic, and immunity diseases; musculoskeletal diseases; perinatal conditions; supplementary classifications; and upper UTI or pyelonephritis. |
|||||
| Acne | 2,070,210 | 0.06 | 410,590 | 1.16 | 19.83 |
| Acute bronchitis | 2,495,160 | 0.07 | 1,915,950 | 5.41 | 76.79 |
| Acute sinusitis | 1,594,820 | 0.05 | 1,313,390 | 3.71 | 82.35 |
| Chronic bronchitis | 1,119,540 | 0.03 | 786,330 | 2.22 | 70.24 |
| Chronic sinusitis | 1,373,910 | 0.04 | 820,100 | 2.32 | 59.69 |
| Disease of the gastrointestinal system | 20,896,550 | 0.59 | 1,101,390 | 3.11 | 5.27 |
| Diseases of the ear | 8,808,200 | 0.25 | 2,212,860 | 6.25 | 25.12 |
| Injuries and poisonings | 12,707,970 | 0.36 | 420,130 | 1.19 | 3.31 |
| Lower UTI or Cystitis | 4,798,090 | 0.14 | 3,245,770 | 9.16 | 67.65 |
| Neoplasms | 9,577,270 | 0.27 | 159,450 | 0.45 | 1.66 |
| Other diseases of the genitourinary system | 14,608,320 | 0.41 | 1,366,290 | 3.86 | 9.35 |
| Other respiratory tract infections | 16,169,390 | 0.46 | 1,183,150 | 3.34 | 7.32 |
| Other skin and soft tissue infections | 17,093,200 | 0.48 | 773,210 | 2.18 | 4.52 |
| Pneumonia | 1,225,990 | 0.03 | 902,620 | 2.55 | 73.62 |
| SSTIs | 2,977,890 | 0.08 | 1,885,520 | 5.32 | 63.32 |
| Symptoms and ill-defined conditions | 22,702,870 | 0.64 | 326,580 | 0.92 | 1.44 |
| Upper respiratory tract infections | 10,697,470 | 0.30 | 3,550,440 | 10.02 | 33.19 |
| TOTAL | 297,468,080 | 8.37 | 23,003,450 | 64.72 | 7.73 |
In 2014, the diagnostic class with the largest decrease in the percentage of diagnoses receiving an antimicrobial recommendation was pneumonia, decreasing from 85% in 2013 to 74% in 2014 (Table 1.2 and Figure 1.2). Although the percentage of upper UTI or pyelonephritis diagnoses resulting in an antimicrobial recommendation decreased from 97% in 2007 to 93% in 2014, there was an increase from 2013 to 2014 (85% to 93%). Similarly, the percentage of chronic sinusitis diagnoses resulting in an antimicrobial recommendation increased from 52% in 2013 to 60% in 2014. Over the 2007 – 2014 time frame acne had the greatest reduction in the percentage of diagnoses resulting in an antimicrobial recommendation, from 27% in 2007 to 20% in 2014 (Table 1.2 and Figure 1.2).
| Diagnostic Class | 2007 | 2008 | 2009 | 2010 | 2011 | 2012 | 2013 | 2014 | RankTable 1.2 - Footnote * |
|---|---|---|---|---|---|---|---|---|---|
| Acne | 26.5 | 21.0 | 21.7 | 25.2 | 18.3 | 25.0 | 20.4 | 19.8 | 11 |
| Acute bronchitis | 78.9 | 77.3 | 80.9 | 85.1 | 82.1 | 77.0 | 77.9 | 76.8 | 3 |
| Acute sinusitis | 86.7 | 87.6 | 83.7 | 81.6 | 86.7 | 87.8 | 83.5 | 82.4 | 2 |
| Chronic bronchitis | 68.7 | 70.1 | 68.6 | 59.5 | 74.5 | 71.3 | 67.0 | 70.2 | 5 |
| Chronic sinusitis | 58.0 | 58.2 | 56.7 | 51.9 | 48.8 | 51.3 | 51.7 | 59.7 | 8 |
| Disease of the gastrointestinal system | 4.6 | 4.8 | 5.1 | 5.3 | 5.0 | 5.9 | 5.7 | 5.3 | 14 |
| Diseases of the ear | 26.8 | 29.2 | 27.6 | 25.5 | 25.2 | 26.8 | 25.7 | 25.1 | 10 |
| Diseases of the sense organs | 2.4 | 3.5 | 3.3 | 1.6 | 2.2 | 2.2 | 1.9 | 3.5 | 16 |
| Lower UTI or Cystitis | 73.5 | 73.3 | 76.0 | 69.3 | 68.3 | 67.3 | 68.9 | 67.6 | 6 |
| Other diseases of the genitourinary system | 6.4 | 6.9 | 6.6 | 10.3 | 9.8 | 9.7 | 9.9 | 9.4 | 12 |
| Other respiratory tract infections | 8.4 | 8.5 | 7.2 | 8.6 | 7.1 | 6.6 | 7.4 | 7.3 | 13 |
| Other skin and soft tissue infections | 2.7 | 3.1 | 2.9 | 4.4 | 3.7 | 4.1 | 4.6 | 4.5 | 15 |
| Pneumonia | 75.0 | 80.9 | 77.3 | 84.8 | 76.6 | 82.1 | 84.5 | 73.6 | 4 |
| SSTIs | 58.6 | 59.9 | 64.9 | 62.1 | 60.6 | 65.2 | 64.5 | 63.3 | 7 |
| Upper respiratory tract infections | 35.1 | 32.1 | 31.2 | 31.5 | 33.3 | 32.8 | 32.6 | 33.2 | 9 |
| Upper UTI or Pyelonephritis | 97.0 | 74.0 | Table 1.2 - Footnote - | 97.6 | 81.1 | 77.4 | 84.5 | 93.0 | 1 |
Figure 1.2: Percent of diagnoses that received an antimicrobial recommendation by community physicians in Canada, 2007, 2010, 2013 and 2014Footnote 1

Figure 1.2 - Text Description
| Disease Classification | 2007 | 2008 | 2009 | 2010 | 2011 | 2012 | 2013 | 2014 |
|---|---|---|---|---|---|---|---|---|
| Upper RTIs | 35.1 | 32.1 | 31.2 | 31.5 | 33.3 | 32.8 | 32.6 | 33.2 |
| Upper UTI | 97.0 | 74.0 | 119.0 | 97.6 | 81.1 | 77.4 | 84.5 | 93.0 |
| SSTIs | 58.6 | 59.9 | 64.9 | 62.1 | 60.6 | 65.2 | 64.5 | 63.3 |
| Pneumonia | 75.0 | 80.9 | 77.3 | 84.8 | 76.6 | 82.1 | 84.5 | 73.6 |
| Lower UTI | 73.5 | 73.3 | 76.0 | 69.3 | 68.3 | 67.3 | 68.9 | 67.6 |
| Diseases of the ear | 26.8 | 29.2 | 27.6 | 25.5 | 25.2 | 26.8 | 25.7 | 25.1 |
| Chronic sinusitis | 58.0 | 58.2 | 56.7 | 51.9 | 48.8 | 51.3 | 51.7 | 59.7 |
| Chronic bronchitis | 68.7 | 70.1 | 68.6 | 59.5 | 74.5 | 71.3 | 67.0 | 70.2 |
| Acute sinusitis | 86.7 | 87.6 | 83.7 | 81.6 | 86.7 | 87.8 | 83.5 | 82.4 |
| Acute bronchitis | 78.9 | 77.3 | 80.9 | 85.1 | 82.1 | 77.0 | 77.9 | 76.8 |
| Acne | 26.5 | 21.0 | 21.7 | 25.2 | 18.3 | 25.0 | 20.4 | 19.8 |
Diagnostic classes were removed from this table if they represented < 1% of antimicrobial mentions in 2014. These classes were: complications of pregnancy, childbirth, and puerperium; congenital anomalities; diseases of the central nervous system; diseases of the circulatory system; diseases of the sense organs; endocrine, nutritional, metabolic, and immunity diseases; musculoskeletal diseases; perinatal conditions; supplementary classifications; and upper UTI or pyelonephritis.
The total number of antimicrobial recommendations per 10,000 inhabitants decreased from 7,587 recommendations in 2007 to 6,494 recommendations/10,000 inhabitants in 2014 (data not shown). In particular, the lowest recommendation rates were observed in 2014 for acute bronchitis, acute sinusitis, diseases of the ear, lower UTI or cystitis, pneumonia and upper respiratory tract infections. These decreases could be due to a number of factors, including changes in the diagnoses provided by physicians or reduction in office visits by patients for those specific diagnoses.
The particular antimicrobial drugs recommended varied by the class of diagnosis (Table 1.3). These data display that for the majority of the diagnostic classes (e.g., diseases of the ear, upper RTI) a single antimicrobial was recommended at a much higher rate than others. This was an exception for acute bronchitis and lower UTI or cystitis, where the majority of the recommendations were for two specific antimicrobials – clarithromycin and azithromycin for acute bronchitis and ciprofloxacin and nitrofurantoin for lower UTI or cystitis (Table 1.3). Between 2013 and 2014 recommendation rates for azithromycin for treating acute bronchitis decreased from 1.4% to 0.8% of inhabitants, while amoxicillin and enzyme inhibitor recommendations increased from 0.2% to 0.4% of inhabitants receiving recommendations. Other changes between 2013 and 2014 observed included increases among recommendation rates of amoxicillin and enzyme inhibitor for treatment of chronic bronchitis (0.2% to 0.4% of inhabitants receiving recommendations), while decreases among norfloxacin for treatment of lower UTI or cystitis (0.4% to 0.2%) and azithromycin for treating pneumonia (0.5% to 0.2%) were observed (Table 1.3).
| Diagnostic Class | Antimicrobial Recommended | Number of antimicrobial recommendations per 10,000 inhabitants | |||||||
|---|---|---|---|---|---|---|---|---|---|
| 2007 | 2008 | 2009 | 2010 | 2011 | 2012 | 2013 | 2014 | ||
| Acne | Minocycline | 110 | 83 | 80 | 89 | 54 | 82 | 62 | 50 |
| Doxycycline | 10 | 8 | 19 | 12 | 15 | 18 | 17 | 19 | |
| Cephalexin | 9 | 13 | 13 | 9 | 10 | 16 | 13 | 17 | |
| Tetracycline | 43 | 22 | 19 | 29 | 18 | 19 | 14 | 13 | |
| Cefadroxil | NR | NR | 2 | 2 | NR | 2 | 3 | 3 | |
| Other antimicrobials | 19 | 26 | 28 | 18 | 17 | 18 | 19 | 13 | |
| TOTAL | 190 | 151 | 160 | 159 | 114 | 155 | 129 | 116 | |
| Acute bronchitis | Clarithromycin | 265 | 252 | 269 | 270 | 280 | 196 | 213 | 195 |
| Azithromycin | 125 | 125 | 97 | 123 | 141 | 156 | 162 | 134 | |
| Amoxicillin | 115 | 133 | 103 | 93 | 95 | 88 | 135 | 77 | |
| Moxifloxacin | 70 | 86 | 65 | 73 | 70 | 60 | 53 | 46 | |
| Amoxicillin and enzyme inhibitor | 8 | 12 | 6 | 11 | 14 | 8 | 15 | 37 | |
| Other antimicrobials | 113 | 77 | 93 | 73 | 62 | 57 | 54 | 52 | |
| TOTAL | 694 | 685 | 634 | 643 | 661 | 566 | 632 | 541 | |
| Acute sinusitis | Amoxicillin | 105 | 111 | 111 | 107 | 125 | 121 | 155 | 131 |
| Clarithromycin | 149 | 176 | 161 | 157 | 138 | 112 | 77 | 78 | |
| Amoxicillin and enzyme inhibitor | 31 | 34 | 35 | 24 | 43 | 25 | 35 | 52 | |
| Azithromycin | 49 | 51 | 38 | 26 | 34 | 41 | 29 | 26 | |
| Moxifloxacin | 55 | 46 | 48 | 51 | 50 | 54 | 33 | 23 | |
| Other antimicrobials | 134 | 103 | 123 | 91 | 91 | 59 | 62 | 61 | |
| TOTAL | 522 | 521 | 515 | 454 | 482 | 412 | 392 | 371 | |
| Chronic bronchitis | Clarithromycin | 82 | 84 | 86 | 64 | 71 | 55 | 68 | 70 |
| Azithromycin | 84 | 91 | 60 | 66 | 46 | 57 | 43 | 46 | |
| Amoxicillin | 67 | 65 | 44 | 33 | 31 | 58 | 42 | 36 | |
| Moxifloxacin | 37 | 39 | 30 | 30 | 42 | 33 | 25 | 31 | |
| Amoxicillin and enzyme inhibitor | 5 | 8 | 6 | 6 | 7 | 8 | 13 | 16 | |
| Other antimicrobials | 36 | 52 | 55 | 16 | 42 | 30 | 21 | 21 | |
| TOTAL | 312 | 339 | 282 | 214 | 239 | 242 | 213 | 222 | |
| Chronic sinusitis | Amoxicillin | 51 | 47 | 75 | 51 | 57 | 62 | 45 | 75 |
| Amoxicillin and enzyme inhibitor | 31 | 30 | 39 | 19 | 16 | 25 | 19 | 41 | |
| Clarithromycin | 63 | 70 | 72 | 56 | 61 | 45 | 42 | 39 | |
| Azithromycin | 46 | 32 | 16 | 19 | 15 | 21 | 22 | 29 | |
| Cefuroxime | 7 | 9 | 17 | 8 | 8 | 6 | 12 | 15 | |
| Other antimicrobials | 69 | 60 | 62 | 41 | 39 | 36 | 34 | 33 | |
| TOTAL | 268 | 248 | 282 | 194 | 196 | 195 | 174 | 232 | |
| Diseases of the ear | Amoxicillin | 306 | 394 | 384 | 377 | 366 | 391 | 436 | 394 |
| Clarithromycin | 114 | 123 | 109 | 113 | 111 | 101 | 62 | 48 | |
| Amoxicillin and enzyme inhibitor | 51 | 42 | 33 | 39 | 31 | 45 | 35 | 46 | |
| Cefprozil | 77 | 82 | 60 | 56 | 67 | 72 | 67 | 44 | |
| Azithromycin | 46 | 71 | 71 | 58 | 48 | 60 | 55 | 30 | |
| Other antimicrobials | 98 | 85 | 85 | 49 | 45 | 32 | 56 | 63 | |
| TOTAL | 692 | 796 | 743 | 692 | 669 | 700 | 711 | 625 | |
| Lower UTI or Cystitis | Ciprofloxacin | 472 | 465 | 476 | 458 | 442 | 470 | 431 | 418 |
| Nitrofurantoin | 278 | 282 | 290 | 320 | 297 | 324 | 342 | 343 | |
| Amoxicillin | 35 | 39 | 37 | 27 | 33 | 34 | 42 | 43 | |
| Sulfamethoxazole and trimethoprim | 175 | 171 | 146 | 42 | 7 | 15 | 12 | 20 | |
| Norfloxacin | 67 | 53 | 77 | 36 | 26 | 20 | 41 | 19 | |
| Other antimicrobials | 72 | 52 | 55 | 69 | 80 | 53 | 66 | 72 | |
| TOTAL | 1099 | 1061 | 1081 | 953 | 884 | 916 | 935 | 916 | |
| Pneumonia | Clarithromycin | 114 | 97 | 98 | 116 | 103 | 107 | 95 | 83 |
| Moxifloxacin | 73 | 72 | 78 | 87 | 88 | 91 | 48 | 54 | |
| Amoxicillin | 11 | 15 | 23 | 29 | 35 | 34 | 24 | 27 | |
| Levofloxacin | 26 | 37 | 25 | 13 | 25 | 10 | 28 | 22 | |
| Azithromycin | 31 | 60 | 19 | 35 | 31 | 38 | 52 | 20 | |
| Other antimicrobials | 63 | 83 | 77 | 73 | 52 | 63 | 57 | 49 | |
| TOTAL | 317 | 365 | 320 | 353 | 334 | 342 | 303 | 255 | |
| SSTIs | cephalexin | 204 | 202 | 207 | 174 | 232 | 203 | 199 | 227 |
| Amoxicillin | 26 | 33 | 33 | 50 | 36 | 44 | 50 | 54 | |
| Cloxacillin | 74 | 91 | 70 | 79 | 60 | 65 | 60 | 43 | |
| Clindamycin | 26 | 19 | 40 | 47 | 27 | 23 | 38 | 40 | |
| Amoxicillin and enzyme inhibitor | 20 | 25 | 25 | 36 | 34 | 30 | 21 | 28 | |
| Other antimicrobials | 162 | 158 | 188 | 137 | 128 | 149 | 151 | 140 | |
| TOTAL | 513 | 530 | 562 | 524 | 516 | 514 | 519 | 532 | |
| Upper UTI or Pyelonephritis | Ciprofloxacin | 11 | 12 | 19 | 8 | 12 | 15 | 15 | 7 |
| Ceftriaxone | 3 | 3 | NR | 5 | 6 | 4 | 2 | 3 | |
| Cephalexin | 2 | NR | NR | NR | NR | 2 | NR | 2 | |
| Trimethoprim | NR | NR | NR | NR | NR | NR | NR | 1 | |
| Amoxicillin | NR | NR | 3 | NR | NR | 1 | 2 | NR | |
| Other antimicrobials | 8 | 2 | 9 | 10 | 3 | 5 | 2 | NR | |
| TOTAL | 24 | 18 | 31 | 23 | 21 | 26 | 21 | 12 | |
| Upper respiratory tract infections | Amoxicillin | 602 | 528 | 573 | 525 | 567 | 500 | 543 | 505 |
| Clarithromycin | 200 | 159 | 176 | 158 | 133 | 120 | 169 | 136 | |
| Azithromycin | 145 | 155 | 131 | 116 | 146 | 153 | 121 | 118 | |
| Penicillin v | 183 | 170 | 142 | 147 | 129 | 131 | 120 | 111 | |
| Amoxicillin and enzyme inhibitor | 15 | 30 | 32 | 19 | 28 | 26 | 36 | 38 | |
| Other antimicrobials | 189 | 155 | 138 | 112 | 139 | 128 | 84 | 94 | |
| TOTAL | 1334 | 1197 | 1192 | 1076 | 1142 | 1058 | 1073 | 1002 | |
Recommendations by age group and gender
The rate of antimicrobial recommendations varied in 2014 by age and gender of the patient (Table 1.4). As expected, the highest numbers of diagnoses per inhabitant were seen at the lowest and highest age groups. Although 15.4 diagnoses per inhabitant were observed in the 65+ age group, this group was the least likely to receive an antimicrobial recommendation; likely due to an increased number of diagnoses for chronic conditions not requiring antimicrobial treatment. Children aged 0-2 had a slightly lower diagnosis rate (11.3 diagnoses per inhabitant), but were the age group most likely to receive an antimicrobial recommendation; nearly 9 out of 10 inhabitants in this age group received a recommendation in 2014. In contrast, children aged 3-9 had a diagnosis rate half that of the 0-2 age group and were slightly less likely to receive an antimicrobial recommendation (3 out of 4 inhabitants in this age group receiving a recommendation).
In 2014, the number of diagnoses per individual decreased among all age groups with the exceptions of adults between the ages of 40 and 59 years (3% increase) and 60-64 years (2% increase). Simultaneous reductions were observed in the number of antimicrobials recommended per inhabitant, with the highest decreases observed among the 0-2 (29% decrease), 3-9 (13% decrease) and 10-19 (9%) age groups. A 2% decrease was observed in the percentage of diagnoses among the 0-2 and 3-9 age groups resulting in an antimicrobial recommendation.
| Demographic | Diagnoses per inhabitant | Number of antimicrobial recommendations per inhabitant | Percentage of diagnoses with antimicrobial recommendations |
|---|---|---|---|
| Age Group | |||
| 0-2 | 11.3 | 0.9 | 7.8 |
| 3-9 | 5.6 | 0.8 | 13.5 |
| 10-19 | 4.9 | 0.5 | 10.3 |
| 20-39 | 6.6 | 0.6 | 9.6 |
| 40-59 | 9.5 | 0.6 | 6.1 |
| 60-64 | 13.7 | 0.7 | 5.1 |
| 65+ | 15.4 | 0.7 | 4.5 |
| Unspecified | N/A | N/A | 6.3 |
| Gender | |||
| Female | 10.4 | 0.8 | 7.2 |
| Male | 8.1 | 0.5 | 6.4 |
| Unspecified | N/A | N/A | 7.9 |
The choice of antimicrobial recommended varied by age of the patient in 2014 (Figure 1.3), as in previous years of surveillance. Children aged 0 to 19 years were more likely to receive a recommendation for a penicillin than any other antimicrobial class. While penicillins were among the most common recommendations for adults (20+), adults were more likely to receive a quinolone or "other antibacterials" recommendation than children. Recommendations for macrolides, second-, and third-generation cephalosporins were relatively similar among the age groups (Figure 1.3).
From 2013 to 2014, recommendation rates for the 0-2 age group changed (data not shown); large reductions occurred for the second-generation cephalosporins (10% to 1.6% of the population in this age group receiving a recommendation) and third-generation cephalosporins (3.2% to <1%), while increases were observed for penicillins (58.6% to 68.2%). Recommendation rates for second-generation cephalosporins increased among the 60-64 age group over the same time frame (1.3% to 3.1% of the population in this age group receiving a recommendation) while recommendations for first-generation cephalosporins (9.1% to 7.3%) decreased during this time period (Figure 1.3).
Figure 1.3: Number of antimicrobial recommendations per 10,000 inhabitants provided by office-based physicians in Canada, by age and antimicrobial classification, 2014Footnote 1
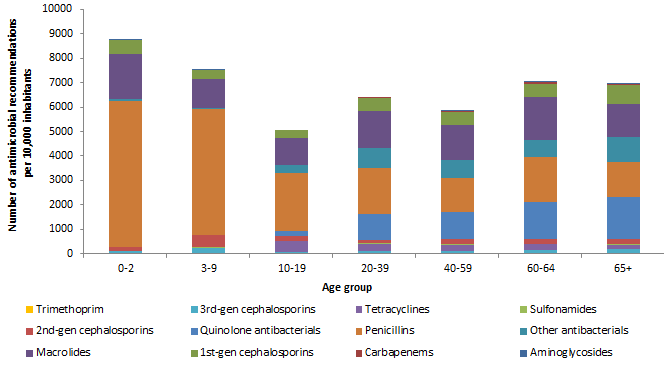
Figure 1.3 - Text Description
| 0-2 | 3-9 | 10-19 | 20-39 | 40-59 | 60-64 | 65+ | |
|---|---|---|---|---|---|---|---|
| "Other antibacterials" include: daptomycin, fidaxomicin, fosfomycin, fusidic acid, linezolid, metronidazole, metronidazole and nystatin, nitrofurantoin, and vancomycin. |
|||||||
| Aminoglycosides | 22 | 7 | 0 | 0 | 18 | 49 | 10 |
| Carbapenems | 0 | 0 | 0 | 3 | 13 | 75 | 21 |
| 1st-generation cephalosporins | 596 | 357 | 339 | 511 | 542 | 514 | 814 |
| Macrolides | 1829 | 1159 | 1109 | 1507 | 1440 | 1785 | 1333 |
| Other antibacterials | 77 | 60 | 329 | 828 | 709 | 668 | 1020 |
| Penicillins | 5981 | 5157 | 2344 | 1891 | 1393 | 1858 | 1452 |
| Quinolone antibacterials | 0 | 10 | 239 | 1042 | 1129 | 1497 | 1683 |
| 2nd-generation cephalosporins | 147 | 494 | 170 | 134 | 186 | 216 | 226 |
| Sulfonamides | 0 | 43 | 15 | 30 | 32 | 0 | 52 |
| Tetracyclines | 0 | 0 | 431 | 301 | 264 | 235 | 129 |
| 3rd-generation cephalosporins | 97 | 211 | 92 | 113 | 110 | 153 | 205 |
| Trimethoprim | 23 | 7 | 0 | 0 | 2 | 8 | 9 |
Recommendations by region
The diagnosis rate, antimicrobial recommendation rate and percentage of diagnoses with antimicrobial recommendations varied by region in Canada during 2014 (Table 1.5). The eastern region had a higher diagnosis rate compared to the central and western regions, consistent with previous years, but a lower percentage of diagnoses resulting with an antimicrobial recommendation than the central region. Over time, a consistent decrease in the percentage of diagnoses with an antimicrobial recommendation has been observed in the central region, while maintaining a constant diagnosis rate (Figure 1.4). These changes may reflect an increase in the diagnosis of chronic (non-infectious) conditions, and/or a move towards more prudent use.
In 2014, the eastern region had a much smaller diagnosis rate for acute bronchitis (2.8% of inhabitants receiving a diagnosis) compared to central (7.6% of inhabitants) and western Canada (6.8% of inhabitants). However, the eastern region had the highest percentage of acute bronchitis diagnoses resulting with an antimicrobial recommendation (Table 1.5). In contrast, the eastern region has a higher diagnosis rate for diseases of the ear (4.4% of the population) but a lower percentage of these diagnoses resulting with an antimicrobial recommendation (20%) (Table 1.5).
The "preferred" antimicrobial drug recommended for treating the different diagnoses seemed consistent across the regions, with the exception of acne, acute bronchitis, and chronic sinusitis (Table 1.6). While both the central and western regions most commonly recommend the use of minocycline for the treatment of acne, the eastern region most commonly recommended the use of amoxicillin or amoxicillin and enzyme inhibitor for treatment, both of which are not reported to be used in the other regions. Azithromycin was the preferred drug for treatment of acute bronchitis in both western and eastern regions, while clarithromycin is the most recommended antimicrobial in the central region, with azithromycin coming in second (Table 1.6). Although not used for treatment of acute sinusitis in the western and central regions, ciprofloxacin is the preferred antimicrobial used in the eastern region, representing more than half of the recommendations provided in that region.
Figure 1.4: Number of diagnoses and percentage of diagnoses with antimicrobial recommendations by region, 2007 to 2014
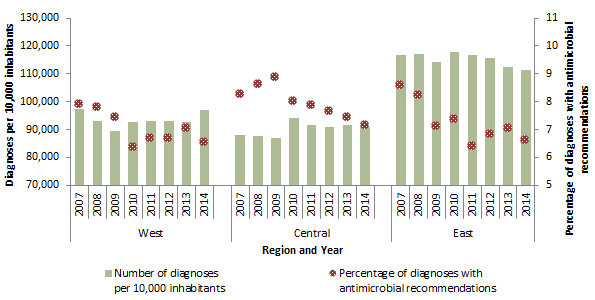
Figure 1.4 - Text Description
| area | year | Number of diagnoses per 10,000 inhabitants |
Percentage of diagnoses with antimicrobial recommendations |
|---|---|---|---|
| West | 2007 | 97305.12 | 7.89 |
| 2008 | 92924.24 | 7.78 | |
| 2009 | 89521.11 | 7.41 | |
| 2010 | 92828.36 | 6.36 | |
| 2011 | 93008.96 | 6.66 | |
| 2012 | 93047.45 | 6.68 | |
| 2013 | 92592.26 | 7.05 | |
| 2014 | 96849.23 | 6.53 | |
| Central | 2007 | 87968.36 | 8.26 |
| 2008 | 87619.98 | 8.63 | |
| 2009 | 86958.58 | 8.86 | |
| 2010 | 94229.34 | 8.01 | |
| 2011 | 91572.57 | 7.85 | |
| 2012 | 90984.56 | 7.66 | |
| 2013 | 91563.37 | 7.42 | |
| 2014 | 90713.42 | 7.15 | |
| East | 2007 | 116732.32 | 8.59 |
| 2008 | 117259.77 | 8.21 | |
| 2009 | 114292.86 | 7.10 | |
| 2010 | 117974.90 | 7.35 | |
| 2011 | 116667.48 | 6.40 | |
| 2012 | 115522.44 | 6.82 | |
| 2013 | 112288.30 | 7.05 | |
| 2014 | 111487.94 | 6.60 |
| Diagnostic Class | Region | Number of diagnoses per 10,000 inhabitants | Number of antimicrobial recommendations per 10,000 inhabitants | Percentage of diagnoses with antimicrobial recommendations |
|---|---|---|---|---|
| Acne | Central | 609 | 116 | 19 |
| East | 810 | 93 | 11 | |
| West | 488 | 120 | 25 | |
| Acute bronchitis | Central | 762 | 589 | 77 |
| East | 278 | 227 | 82 | |
| West | 681 | 514 | 75 | |
| Acute sinusitis | Central | 509 | 436 | 86 |
| East | 428 | 351 | 82 | |
| West | 340 | 247 | 73 | |
| Chronic bronchitis | Central | 290 | 216 | 74 |
| East | 771 | 527 | 68 | |
| West | 270 | 170 | 63 | |
| Chronic sinusitis | Central | 361 | 242 | 67 |
| East | 569 | 401 | 70 | |
| West | 401 | 175 | 44 | |
| Diseases of the ear | Central | 2,433 | 653 | 27 |
| East | 4,358 | 873 | 20 | |
| West | 2,194 | 517 | 24 | |
| Lower UTI or Cystitis | Central | 1,283 | 893 | 70 |
| East | 1,273 | 788 | 62 | |
| West | 1,513 | 988 | 65 | |
| Pneumonia | Central | 363 | 290 | 80 |
| East | 315 | 226 | 72 | |
| West | 319 | 192 | 60 | |
| SSTIs | Central | 776 | 493 | 63 |
| East | 937 | 690 | 74 | |
| West | 946 | 576 | 61 | |
| Upper respiratory tract infections | Central | 3,113 | 996 | 32 |
| East | 2,276 | 1,044 | 46 | |
| West | 2,995 | 1,005 | 34 |
| Diagnostic Class | Antimicrobial Recommended | Antimicrobial recommendations per 10,000 inhabitants | ||
|---|---|---|---|---|
| West | Central | East | ||
| Acne | Minocycline | 48.0 | 56.2 | - |
| Cephalexin | 26.5 | 11.9 | 25.4 | |
| Tetracycline | 21.4 | 10.5 | - | |
| Doxycycline | 20.3 | 18.9 | 8.6 | |
| Clindamycin | 1.9 | - | - | |
| Amoxicillin | - | - | 25.4 | |
| Amoxicillin and enzyme inhibitor | - | - | 24.9 | |
| Other antimicrobials | 1.7 | 18.9 | 8.2 | |
| Acute bronchitis | Azithromycin | 144.1 | 129.5 | 125.6 |
| Clarithromycin | 137.5 | 237.2 | 76.3 | |
| Amoxicillin | 87.4 | 80.6 | - | |
| Amoxicillin and enzyme inhibitor | 59.7 | 29.3 | - | |
| Moxifloxacin | 29.5 | 58.6 | - | |
| Cefuroxime | 16.0 | 18.3 | - | |
| Doxycycline | 15.5 | 2.7 | - | |
| Cephalexin | 5.4 | - | 25.4 | |
| Other antimicrobials | 18.5 | 32.5 | - | |
| Acute sinusitis | Amoxicillin | 118.9 | 142.7 | 75.2 |
| Azithromycin | 37.4 | 20.8 | 25.4 | |
| Clarithromycin | 37.0 | 98.3 | 75.8 | |
| Amoxicillin and enzyme inhibitor | 16.2 | 74.0 | 24.9 | |
| Doxycycline | 16.0 | - | - | |
| Moxifloxacin | 5.2 | 34.8 | - | |
| Ciprofloxacin | - | - | 125.0 | |
| Cefixime | - | 18.9 | - | |
| Other antimicrobials | 16.0 | 46.6 | 24.9 | |
| Chronic bronchitis | Clarithromycin | 65.8 | 61.4 | 175.9 |
| Azithromycin | 34.1 | 49.4 | 75.2 | |
| Amoxicillin | 21.2 | 34.2 | 125.6 | |
| Cefuroxime | 18.7 | - | - | |
| Amoxicillin and enzyme inhibitor | 10.6 | 21.0 | - | |
| Moxifloxacin | - | 42.2 | 75.8 | |
| Cefixime | - | - | 74.7 | |
| Other antimicrobials | 19.2 | 7.3 | - | |
| Chronic sinusitis | Amoxicillin | 47.7 | 86.0 | 101.2 |
| Clarithromycin | 37.0 | 30.3 | 125.6 | |
| Azithromycin | 27.0 | 25.4 | 74.7 | |
| Cefuroxime | 20.7 | 13.2 | - | |
| Amoxicillin and enzyme inhibitor | 10.4 | 55.5 | 49.8 | |
| Other antimicrobials | 32.4 | 31.4 | 49.8 | |
| Diseases of the ear | Amoxicillin | 325.0 | 418.0 | 503.4 |
| Amoxicillin and enzyme inhibitor | 55.4 | 38.2 | 75.2 | |
| Clarithromycin | 47.7 | 50.1 | 25.4 | |
| Cephalexin | 38.2 | 13.8 | - | |
| Azithromycin | 18.7 | 27.4 | 101.2 | |
| Moxifloxacin | 5.4 | 4.2 | 25.4 | |
| Cefprozil | 5.2 | 63.8 | 49.8 | |
| Ciprofloxacin | 5.2 | 12.9 | 38.4 | |
| Other antimicrobials | 15.7 | 24.7 | 54.4 | |
| Lower UTI or Cystitis | Ciprofloxacin | 427.4 | 415.5 | 401.6 |
| Nitrofurantoin | 361.6 | 340.6 | 285.5 | |
| Amoxicillin | 57.2 | 40.9 | - | |
| Sulfamethoxazole and trimethoprim | 47.7 | 8.1 | - | |
| Cephalexin | 35.1 | 8.2 | - | |
| Cefuroxime | 5.4 | 1.2 | 50.9 | |
| Norfloxacin | 5.2 | 25.8 | 25.4 | |
| Cefprozil | - | 2.8 | 24.9 | |
| Other antimicrobials | 48.7 | 50.4 | - | |
| Pneumonia | Clarithromycin | 75.5 | 87.2 | 75.8 |
| Azithromycin | 28.3 | 13.2 | 50.3 | |
| Levofloxacin | 27.0 | 22.1 | - | |
| Moxifloxacin | 23.8 | 71.8 | 25.4 | |
| Amoxicillin | 10.8 | 38.3 | - | |
| Cefixime | - | 2.7 | 24.9 | |
| Cefuroxime | - | 5.5 | 24.9 | |
| Ciprofloxacin | - | 10.1 | 24.9 | |
| Other antimicrobials | 26.7 | 39.0 | 0.0 | |
| SSTIs | Cephalexin | 323.1 | 163.0 | 367.9 |
| Clindamycin | 81.0 | 21.1 | 25.4 | |
| Amoxicillin and enzyme inhibitor | 37.4 | 26.4 | - | |
| Amoxicillin | 28.5 | 56.2 | 149.9 | |
| Ceftriaxone | 16.2 | 9.4 | 25.4 | |
| Cloxacillin | 10.8 | 61.0 | 25.4 | |
| Minocycline | 10.4 | - | 24.9 | |
| Ciprofloxacin | 5.4 | 25.0 | 24.9 | |
| Cefadroxil | - | 44.4 | - | |
| Other antimicrobials | 63.6 | 86.3 | 46.5 | |
| Upper respiratory tract infections | Amoxicillin | 493.0 | 496.4 | 638.6 |
| Clarithromycin | 201.1 | 112.7 | 49.8 | |
| Azithromycin | 83.3 | 121.3 | 251.2 | |
| Penicillin v | 71.9 | 143.6 | - | |
| Amoxicillin and enzyme inhibitor | 50.4 | 30.2 | 50.3 | |
| Cefuroxime | 16.0 | 7.9 | 15.5 | |
| Clindamycin | 10.6 | 10.1 | 38.4 | |
| Other antimicrobials | 78.8 | 74.2 | - | |
References
Page details
- Date modified: