ARCHIVED - Incidence of Invasive Pneumococcal Disease After Introduction of the Universal Infant Immunization Program, British Columbia (2002-2005)
15 July 2006 Volume 32 Number 14
Introduction
In North America, Streptococcus pneumoniae has long been a leading cause of meningitis, bacteremia, and bacterial pneumonia in children. In 2001, a 7-valent pneumococcal conjugate vaccine (PCV-7) was licensed for use in children in Canada. This vaccine is effective against the serotypes that are responsible for > 80% of invasive disease in children < 5 years of age in Canada (1). In order to reduce the incidence of invasive pneumococcal disease (IPD) in British Columbia (BC), a selective immunization program of high-risk and Aboriginal children aged 2 to 59 months was implemented in April 2003, and a universal immunization program was introduced in September 2003. Children are offered a four-dose schedule administered at age 2, 4, 6, and 18 months. They are offered three doses if vaccination is initiated after 6 months of age, two doses if initiated after 12 months of age, and one dose if initiated after 2 years of age. All children born on or after July 2003 are eligible for vaccination.
In addition to high-risk patients, all persons aged ≥ 65 years in BC have been offered a 23-valent polysaccharide pneumococcal vaccine (PPV-23) since 1998.
The expectation is that within 5 years the new universal infant PCV-7 immunization program will prevent 112 cases of pneumococcal meningitis or sepsis annually in children < 5 years of age (2) . We present the latest surveillance data for IPD in BC dating from 2002 to 2005.
Methods
IPD is a reportable condition in BC and has been monitored by the British Columbia Centre for Disease Control (BCCDC) since 1999. IPD cases are defined by the isolation of S. pneumoniae from a sterile body site, usually blood or cerebrospinal fluid.
Data on IPD cases were extracted from the integrated Public Health Information System (iPHIS), a database that contains a range of information, including age at presentation, sex, type of infection, health authority, and year of case. Annual cumulative incidence rates were calculated using the P.E.O.P.L.E. 30 (Population Extrapolation for Organization Planning with Less Error, run cycle 30, BC STATS). Data management and calculations were performed using Microsoft® Excel software. Trends over time were explored with the chi-square test for trend, using the StatCalc calculator in EpiInfo 6. Trends were considered statistically significant if the p value was < 0.05.
Immunization coverage in BC is reported at the second birthday. To date, information on pneumococcal immunization coverage is available for children born between 1 July and 31 December, 2003. These statistics are calculated using immunization records in iPHIS and exclude regions not using the immunization registry portion of iPHIS (Vancouver, Richmond, and North Shore/Coast Garibaldi).
Results
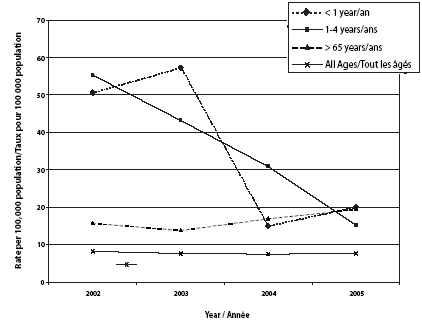
British Columbia had a population of 4.2 million people, including 203,435 children < 5 years of age, in 2005. In 2002, the year before universal vaccine introduction, 343 cases of IPD were reported in BC (8.3 cases/100,000 population). Figure 1 shows that 114 reports were in children < 5 years of age (53 cases/ 100,000 population), of whom 55 were between 12 and 23 months of age (135 cases/100,000 population); 20 cases were < 1 year old (51 cases/100,000 population); and 87 cases were in the age group > 65 years (16 cases/100,000 population).
It was estimated that 64% of the first group of infants offered pneumococcal vaccine (those born between 1 July and 31 December, 2003) were up to date for pneumococcal vaccination by 2 years of age, according to the schedule appropriate for the age at which they started their series (outlined earlier) (BCCDC, unpublished data).
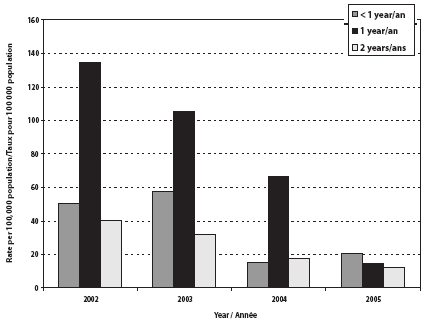
In the last 2 years we have witnessed a steady decline in the rate of IPD among children < 5 years of age. In 2005, the incidence in this age group was 18 cases/100,000 population, a 67% reduction from the 2002 rates. When smaller age categories were examined, the data demonstrated a statistically significant trend (÷ 2 =9.9; p = 0.002) of decreasing incidence of IPD among children < 1 year old (Figure 2), from 20 cases in 2002 (51 cases/100,000 population) to eight cases in 2005 (20 cases/100,000 population). In children aged 12 to 23 months, the number of IPD cases significantly decreased from 55 cases in 2002 (135 cases/100,000 population) to six cases in 2005 (15 cases/100,000 population) (÷ 2 = 39.9; p < 0.001). There was also a significant decrease in IPD incidence among 2-year-olds (40 to 12 cases/100,000 population; ÷ 2 = 7.9; p = 0.005) and 4-year-olds (22 to seven cases/ 100,000 population; ÷ 2 = 3.9; p = 0.049) but no significant change in incidence among 3-year-olds (28 to 27 cases/100,000 population; ÷ 2 = 0.007; p = 0.934). No significant decrease was observed in the 5 to 9-year age group. As for those aged 10 top 14, there was a reduction in reported IPD rates; however, the total number of reported cases was small (five cases in 2002 and two in 2005), and the decrease was not statistically significant (÷ 2 = 2.1; p = 0.147).
Figure 2. Incidence of reported IPD in children < 3 years of age
The rate of IPD for all ages combined has not changed signifi-cantly since 2002 and has remained between seven and eight cases/100,000 population. The rate of IPD in the ≥ 65-year age group has slightly increased, from 87 cases in 2002 to 115 cases in 2005 (16 to 20 cases/100,000 population); however this change was not statistically significant (÷ 2 = 3.7, p = 0.06).
Discussion
This report provides the first insight into the impact of the PCV-7 universal immunization program started in BC in 2003. The program appears to have been well received by the general public. However, the coverage rate for the first group of eligible 2-year-olds was relatively low, at 64%. This figure represents only the first two measurable quarters after the initiation of the program and may reflect a slow start. Coverage with pneumococcal conjugate vaccine is likely to improve in subsequent reports.
The dramatic reduction of IPD in the < 5-year age group observed in the United States (US) following the implementation of the PCV-7 program in 2000 was similarly observed in BC. In the US, the baseline IPD rate in 1998 among those < 5 years was 96 cases/100,000 population (3). This rate decreased by 59% to 40 cases/100,000 population in 2001, just over 1 year after the start of the immunization program. In BC, the baseline IPD rate among children < 5 years of age was lower than in the US (53 cases/100,000 population in 2002). The incidence of IPD in this age group has decreased by 67% to 18 cases/100,000 population 2 years following the implementation of the universal program. This is compatible with the initial aim to reduce the annual burden of disease due to IPD by 90% within 5 years.
In parallel with the US experience, the most dramatic reduction was seen in the 1-year-olds. The baseline 1998 US rate of 208 cases/100,000 seen in the 12 to 23-month age group decreased by 68% to 66 cases/100,000 population in 2001. Similarly, in BC the rate in this age group decreased from 135 cases/100,000 population in 2002 to 67 cases/100,000 population in 2004 and to 15 cases/100,000 population in 2005. This represents an 89% reduction in this age group. The reports in infants < 1 year also confirmed an important reduction of IPD, by 60%. Furthermore, significant declines in incidence were observed among 2- and 4-year-olds but not 3-year-olds. The epidemiologic reasons behind these particular results are unclear. Unlike in the US, the BC vaccination program has no catch-up schedule for children born before 1 July, 2003; children born earlier would not receive the vaccine. Therefore, this partial decrease of invasive disease in the 3- to 5-year-olds could represent the appearance of herd immunity.
The IPD rate in the population as a whole has been constant over the last 3 years. No significant difference was noted in any of the age groups > 5 years old. This is not in line with the US experience, which was of a quite significant decrease in IPD rates in the general population after the introduction of the universal vaccination program (3,4). Indeed, although the initial US reports showed no change of rate in the 5 to 19-year age range, statisti-cally significantly lower rates of IPD occurred in all older age groups, especially in the > 65 age group. In contrast, the IPD rate in BC among > 65-year-olds has not changed significantly over the last 3 years.
A previous report from Alberta by Kellner et al. (5) might explain the absence of an effect in the > 65-year age group. Two years after the initiation of the universal immunization program in Alberta in 2002, they observed no statistically significant decline in the rate of IPD among individuals > 65 years of age. Upon analysis of the serotypes, it was determined that there was a statistically significant decline in PCV-7-associated serotypes accompanied by a statistically significant rise in serotypes not included in either the PCV-7 vaccine or the PPV-23 vaccine. This finding raises the potential of serotype replacement as the cause of inva-sive disease in the > 65-year age group.
It is also interesting to note that the baseline rate of IPD in the US population aged > 65 was 60 cases/100,000 population versus 16 cases/100,000 population in BC. The reason for this difference in disease rate is not entirely clear, but it might be partially related to the difference in reporting, which has been active (with the use of sentinel sites) in the US versus passive reporting in most of Canada, including BC.
Conclusion
This report emphasizes the success of the PCV-7 universal immu-nization program in British Columbia. The rate of invasive pneumococcal disease among children < 5 years has been dramatically reduced within 2 years of the start of the program. However, the herd immunity phenomenon observed in the older age groups after vaccination in the US has yet to be been seen in British Columbia.
References
-
National Advisory Committee on Immunization (NACI). Statement on recommended use of pneumococcal conjugate vaccine. CCDR 2002;28(ACS-2):1-32.
-
British Columbia Centre for Disease Control. Annual burden of disease due to pneumococcus. Communicable Disease Policy Discussion Paper. 15 July, 2005.
-
Whitney CG, Farley MM, Hadler J et al. Decline in invasive pneumococcal disease after the introduction of protein-polysaccharide conjugate vaccine. N Engl J Med 2003;348(18):1737-46.
-
Lexau CA, Lynfield R, Danila R et al. Changing epidemiology of invasive pneumococcal disease among older adults in the era of pediatric pneumococcal conjugate vaccine.JAMA 2005;294(16):2043-51.
-
Kellner JD, Church DL, MacDonald J et al. The result of a large effectiveness study showed sharp reductions in the number of invasive infections among children. Can Med Assoc J 2005;173(10):1149-51.
Source: S Paulus, MD, DTM&H, FAAP, Division of Immunological and Infectious Diseases, British Columbia Children’s Hospital; ST David, MHSc, W Tang, BSc, M Winters, BSc, J Buxton, MBBS, MHSc,FRCPC,B Henry,MD,MPH,FRCPC,DPatrick,MD, MHSc, FRCPC, Department of Epidemiology Services, British Columbia Centre for Diseases Control, Vancouver, British Columbia.
Page details
- Date modified:
