ARCHIVED - Self-exclusion behaviours of people with gastrointestinal illness who work in high-risk settings or attend daycare
15 August 2006 Volume 32 Number 16
K Thomas, MSc (1), S Majowicz, MSc, PhD (1), P Sockett, PhD (1), V Edge,MSc (1), J Flint,MPH (1), K Doré, MHSc (1), L MacDougall, MSc (2), S Atashband, MHSc (2), M Fyfe, MD, MSc, FRCPC (3), S Henson, MSc, PhD (4), S Kovacs, MSc (5), A Jones, DVM, PhD (6)
-
Foodborne, Waterborne and Zoonotic Infections Division, Public Health Agency of Canada, Guelph and Ottawa, Ontario, Canada
-
British Columbia Centre for Disease Control and Prevention, Vancouver, British Columbia, Canada
-
Vancouver Island Health Authority, Victoria, British Columbia, Canada
-
Department of Agricultural Economics and Business, University of Guelph, Guelph, Ontario, Canada
-
Western University of Health Sciences, Pomona, California, USA
-
Division of Community Health Faculty of Medicine, Memorial University of Newfoundland, St. John's, Newfoundland and Labrador, Canada
Introduction
Understanding the behaviour of people with acute gastrointestinal illness (GI) who choose to continue to work in high-risk settings or attend daycare is useful for creating appropriate education and intervention programs to help reduce secondary transmission. High-risk settings include those where the nature of the environment or the worker's duties increase the likelihood of transmission of GI to others. These include food preparation duties, especially handling of ready to eat foods, working in acute care or long-term care facilities and working in or attending daycare. There is a lack of literature specifically investigating the actions of employees in high-risk settings when ill with infectious disease. This paper describes behaviours and practices of those working in high-risk settings or of parents of children attending daycare, including self-exclusion practices (i.e. of their own accord, opting not to go to work or attend daycare because of illness) or reasons for working while ill, as compared to those experiencing GI who do not work in high-risk settings or attend daycare.
Methods
In June 2002, a retrospective, cross-sectional telephone survey entitled “Magnitude of enteric illness in the province of British Columbia: A population telephone survey” was conducted. The objective of the survey was to estimate the magnitude and describe the distribution of self-reported GI in British Columbia (BC)1,2.
The study area consisted of three regions, chosen to be representative of the socio-economic structure of BC, and therefore included one urban, one mixed, and one rural public health authority area. The sampling frame consisted of a randomized list of residential telephone numbers obtained from a commercial database (SelectPhoneTM, InfoUSA, Inc.). Once telephone contact was made, the individual from the household whose birthday fell next was randomly selected to participate in the survey. The survey tool was developed using the Hamilton survey tool3, which had been created through modifying other existing validated questionnaires4-6.
To identify individuals with acute, self-reported GI, respondents were asked if they had experienced any vomiting or diarrhoea in the 28 days prior to the interview. Proxy respondents were used for children < 12 years of age or for those between the ages of 12 and 17 if preferred by the parent/guardian. Respondents who did not report symptoms of GI, as well as those identified as having chronic GI, were included in the non-case category. Chronic GI included symptoms attributed to pregnancy, medication use, food allergy and/or medical condition previously diagnosed by a doctor, e.g. colitis, diverticulitis, Crohn's disease, irritable bowel syndrome etc.
Additional survey questions explored daycare attendance, occupation, and demographic characteristics. If the individual was employed in a high-risk setting (a food handler, daycare worker or health care worker) or attended daycare, additional questions concerning exclusion were asked, including whether they stayed home while ill, whether this decision was made by themselves or by an employer or doctor, reasons for not staying home while ill and whether they were symptom-free upon return to work or daycare.
Data analysis was performed using SAS version 9.1 (SAS Institute Inc., Cary, NC, USA). TheWilcoxon rank sum test was used to test for significant differences in the number of days taken off work due to illness.
Results
Respondents ≥ 19 years of age
There were 3,709 adult respondents ≥ 19 years of age; 354 (9.5%) were cases, of whom 223 (63%) responded ‘yes' to the question ‘Are you employed?'. Of those adults employed, 6% (n = 4), 1% (n = 2) and 10% (n = 22) were employed as food handlers, daycare workers and health care workers respectively (Figure 1). Several workers continued to work while experiencing symptoms of acute GI (Figure 1). Half of food handlers and nearly one quarter of healthcare workers continued to work while experiencing symptoms; however, none of the daycare workers reported continuing to work while experiencing symptoms of acute GI.
Figure 1. Breakdown of employed adult cases of gastrointestinal illness by type of employment and whether they continued to work while experiencing symptoms of acute gastrointestinal illness
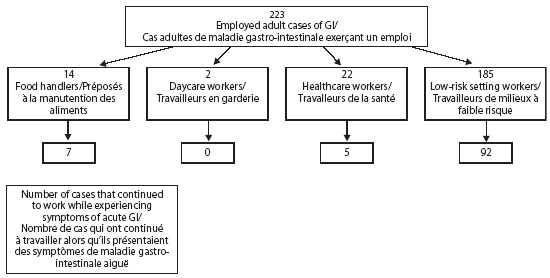
Employees who worked in high-risk settings were 1.4 (95% confidence interval (CI): 1.1 - 1.8) times more likely to discontinue working while ill than employees who worked in low-risk settings. When broken down by type of high-risk setting, health care workers and daycare workers were 1.5 (95% CI: 1.2 - 2.0) and 2.0 (95% CI: 1.7 - 2.3) times more likely to discontinue working while ill than employees in low-risk settings, respectively. Food handlers were neither more nor less likely to discontinue working while ill compared to employees in low-risk settings (relative risk = 1.0, 95% CI: 0.6 - 1.7).
Of those employed in high-risk settings who were scheduled to work but took time off because of illness (n = 17), 14 decided for themselves, as they were self-employed, two cases were excluded by a physician, and one case did not indicate who had made the decision. However, of these 17 adult cases, two food handlers, one day care worker and five health care workers returned to work while still experiencing symptoms of acute GI.
For those working in high-risk settings, the elapsed time from onset of symptoms to the decision to stay home from work ranged from 1 to 10 days, with a median of 1 day. The number of days taken off work due to illness was not significantly different (p = 0.63) between those working in high-risk settings (0.5 to 12 days) and employees in low-risk settings (1.5 hours to 8 days). Cases working in high-risk settings most commonly reported the following reasons for not taking time off work while sick: “Did not think their illness was serious enough to stay home”, “Unable to afford to take time off work”, and “Employer depends on them / no one else would be able to cover for them”.
Respondents < 19 years of age
Of the respondents < 19 years of age (n = 600), 15% (n = 90) were cases, two of whom were employed as food handlers; however, they were not scheduled to work during the time of their illness and thus their responses are not analysed here.
Eleven of the 142 children in the survey aged < 4 years of age attended daycare, four of whom were cases. All four children were kept out of daycare; however one child did return to daycare while still experiencing symptoms. The elapsed time from onset of symptoms to when the children began to stay home from daycare ranged from 1 to 3 days with a median of 1 day. The number of days absent from daycare for illness ranged from 1 to 3 days.
Discussion
Though this analysis is based on a small sample, it does provide insight into self-exclusion practices of those with acute GI who work in high-risk settings or attend daycare. We found that 17% of all employed adult cases worked in high-risk settings (i.e. food handlers, daycare and health care workers), which could represent a considerable public health risk of secondary disease transmission. Numerous reports link ill food handlers with foodborne disease outbreaks7-9; other reports link contact with ill people working or attending daycare centres with daycare centre outbreaks of GI10-13. Furthermore, many ill workers continued to work for a period of time before deciding to stay home, increasing the likelihood of secondary transmission. This potential public health risk needs to be addressed, and a better understanding of the magnitude of the problem is critical.
A greater proportion of food handlers continued to work while ill compared to daycare and health care workers. Similarly, daycare and health care workers were statistically more likely to discontinue working while ill compared to those working in low-risk settings, whereas food handlers were not. It is possible that educational programs addressing disease transmission aimed at daycare and health care workers, or incorporated within their professional training, are more successful than those used to educate food handlers. However, according to the Food Premises Regulation of the BC Health Act14, every operator of a food service establishment must hold a certificate from a food safety-training program such as ‘Food Safe'15, and they must ensure that while the operator is absent from the premises, at least one employee holds such a certificate. Although this training program includes a section explaining why workers should not work when ill or infected, it appears investigation into the effectiveness of educational and training programs is needed.
Many workers in high-risk settings stated they continued to work while ill because they could not afford to take the time off, or felt that no one else would be able to do their job while they were away. These results are supported by those found by Aronsson et al.16, who suggested that a worker's perceived level of replaceability as well as income level were significant in the occurrence of sickness “presenteeism” (sickness “presenteeism” is “the phenomenon of people, despite complaints and ill health that should prompt rest and absence from work, still turning up at their jobs”16). In the Aronsson study, those who felt they would have to ‘re-do' most of the work they missed if absent from work and those in lower income brackets were more likely to exhibit sickness presenteeism behaviours. Interestingly, the study found the highest sectors experiencing sickness presenteeism were education and care and welfare sectors, including child minders, pre-primary educationalists, nursing home aides, assistant nurses, and registered nurses. Within the restaurant service workers sector, cooks and waiters had the highest odds ratio of sickness presenteeism.
From a business perspective, sickness presenteeism represents an indirect cost associated with reduced productivity17. It is thought that illness in general can affect the quantity and quality of performed work17-19. A study investigating the loss in productive time due to pain found that sickness presenteeism accounted for four times more lost productive time than absenteeism18,19. Increased understanding of reasons for sickness presenteeism in Canada is needed, as it may represent a risk to public health and the indirect costs associated with reduced productivity. In turn, this may indicate the need for improvements in employee health benefits to promote self-exclusion of employees when ill.
Conclusion
This paper highlights some of the self-exclusion behaviours and practices of people with acute GI working in high-risk settings or attending daycare, helping to fill the void in this area of research. Further investigation is warranted to determine the need for intervention and education strategies aimed at employees working in high-risk settings and parents of children attending daycare. Changes in health coverage benefits may help to reduce sickness presenteeism, which may in turn not only reduce potential disease transmission but also improve overall employee productivity.
Acknowledgements
The authors would like to thank the other members of the British Columbia National Studies on Acute Gastrointestinal Illness (NSAGI) team, and in particular V. Remple (British Columbia Centre for Disease Control, Vancouver British Columbia), for their contribution to the overall project; the staff of the Centre for Evaluation of Medicines (St. Joseph's Hospital, Hamilton) for their expert interviewing; the Health Service Delivery Areas of Vancouver, Northern Interior and East Kootenay for their overall support of this project; and the residents of British Columbia for their participation. This project was funded by the Public Health Agency of Canada.
References
-
Health Canada. An Introductory Letter in Advance of a Telephone Survey may Increase Response Rate. CCDR 2004;30(13):121-3.
-
Thomas MK, Majowicz SE, MacDougall L et al. Epidemiology of acute gastrointestinal illness in British Columbia: Population incidence, distribution, and burden. 2006. (In press).
-
Majowicz SE, Dore K, Flint J et al. Magnitude and Distribution of Acute, Self-Reported Gastrointestinal Illness in a Canadian Community. Epidemiol Infect 2004;132:607-17.
-
Herikstad H, Yang S, Van Gilder TJ et al. A population-based estimate of the burden of diarrhoeal illness in the United States: FoodNet, 1996-7. Epidemiol Infect 2002;129:9-17.
-
de Wit MAS, Koopmans MPG, Kortbeek LM et al. Sensor, a population-based cohort study on gastroenteritis in the Netherlands, incidence and etiology. Am J Epidemiol 2001;154:666-74.
-
Wheeler JG, Sethi D, Cowden JM et al. Study of infectious intestinal disease in England: rates in the community, presenting to general practice, and reported to national surveillance. Br Med J 1999;318:1046-50.
-
Kimura AC, Palumbo MS, Meyers H et al. A multi-state outbreak of Salmonella serotype Thompson infection from commercially distributed bread contaminated by an ill food handler. Epidemiol Infect 2005;133:823-8.
-
Parashar UD, Dow L, Fankhauser RL et al. An outbreak of viral gastroenteritis associated with consumption of sandwiches: Implications for the control of transmission by food handlers. Epidemiol Infect 1998;121:615-21.
-
Anderson AD, Garrett VD, Sobel J et al. Multistate outbreak of Norwalk-like virus gastroenteritis associated with a common caterer. Am J Epidemiol 2001;154:1013-9.
-
Venczel LV, Desai MM, Vertz PD et al. The role of child care in a community-wide outbreak of hepatitis A. Pediatrics 2001;108:E78.
-
Al-Jader L, Salmon RL, Walker AM et al. Outbreak of Escherichia coli O157 in a nursery: Lessons for prevention. Arch Dis Child 1999;81:60-3.
-
Galanis E, Longmore K, Hasselback P et al. Investigation of an E. coli O157:H7 outbreak in Brooks, Alberta, June-July 2002: The role of occult cases in the spread of infection within a daycare setting. CCDR 2003;29(3):21-8.
-
Gouveia S, Proctor ME, Lee MS et al. Genomic comparisons and Shiga toxin production among Escherichia coli O157:H7 isolates from a day care center outbreak and sporadic cases in southeastern Wisconsin. J Clin Microbiol 1998;36:727-33.
-
British Columbia Health Act, Food Premises Regulation. B.C. Reg 210/99, 2. 2004. Victoria, British Columbia, Queen's Printer. 2004. (http://www.qp.gov.bc.ca/statreg/reg/H/Health/210_99.htm).
-
The Province of British Columbia. FOODSAFE Training for FoodserviceWorkers & Managers, 2005. (http://www.foodsafe.ca/).
-
Aronsson G, Gustafsson K, Dallner M. Sick but yet at work. An empirical study of sickness presenteeism. J Epidemiol Community Health 2000;54:502-9.
-
Hemp, P. Presenteeism: At work - but out of it. Harvard Business Review. Oct, 2004. Harvard Business School Publishing Corporation.
-
Stewart WF, Ricci JA, Chee E et al. Lost productive time and cost due to common pain conditions in the US workforce. JAMA 2003;290:2443-54.
-
Stewart WF, Ricci JA, Chee E et al. Cost of lost productive work time among US workers with depression. JAMA 2003;289:3135-44.
Page details
- Date modified:
