Rapid emergence of methicillin-resistant Staphylococcus aureus (MRSA) among children and adolescents in northern Manitoba, 2003-2006
15 January 2007
Volume 33
Number 02
L Larcombe, PhD (1), J Waruk, BSc (1), J Schellenberg, MSc (1), and M Ormond, RN (2)
1 Department of Medical Microbiology, University of Manitoba, Winnipeg, Manitoba
2 Ormond Consulting Inc., Winnipeg, Manitoba
The global spread of community-associated methicillin-resistant Staphylococcus aureus (CA-MRSA) since the mid-1990s is a major public health concern. The epidemiology of CA-MRSA differs from that of health-care-associated MRSA (HCA-MRSA), and this is reflected at the genetic level 1. Resistance to beta-lactams is encoded in the mecA gene, which is carried, along with resistance determinants for other antibiotics, on the staphylococcal chromosomal cassette (SCC). CA-MRSA typically carries a type IV SCC, which is smaller and encodes resistance to fewer antibiotics than the SCC of HCA-MRSA clones1. This may help to explain the ecologic success of CA-MRSA in the community setting and may facilitate horizontal transfer of type IV SCC into other methicillin-sensitive strains1.
CA-MRSA is common in many urban and rural communities in the United States. It has been associated with fatal necrotizing pneumonia in four children in Minnesota and North Dakota2, severe sepsis in 13 adolescents in Texas, three of whom died3, and 14 cases of necrotizing fasciitis in Los Angeles4. The increasing incidence of MRSA infections among Canadian First Nations and in northern communities has received attention from public health authorities1,5,6, although comprehensive measures to determine the infection dynamics and prevent spread have yet to be implemented in affected areas.
Whole-genome fingerprints of CA-MRSA strains isolated in northern Manitoba and Saskatchewan have been generated using pulsed field gel electrophoresis1,6. Most strains in these studies had a fingerprint indistinguishable from the strain responsible for pediatric deaths in Minnesota and North Dakota1,6. The majority of CA-MRSA strains carry the lukF-PV-lukS-PV genes encoding Panton-Valentine leukocidin, a virulence factor that is associated with severe primary skin infections and necrotizing pneumonia7. As the number of CA-MRSA infections increase in these regions, the risk of life-threatening sequelae is also greater. This heightened risk is of particular concern in remote communities where access to emergency health care can be significantly delayed.
Methods
Observations of MRSA infections in clinical situations by nursing staff in several First Nations communities in 2005 and 2006 stimulated an analysis of monthly infectious disease report8. The reports provided information about the total number of MRSA infections and made no distinction between CA- and HCA-MRSA. Data were broken down by age, sex and regional health authority (RHA; see Figure 1A). Crude rates of MRSA infection per 10,000 population were calculated using data from the 2004 Manitoba Health Population Report 9.
Figure 1A. Rising levels of MRSA reported in northern Manitoba over the last 3 years – geography and population size of Manitoba's regional health authorities (RHAs)

*2006 third quarter (Q3) results are the average of July and August only.
Results
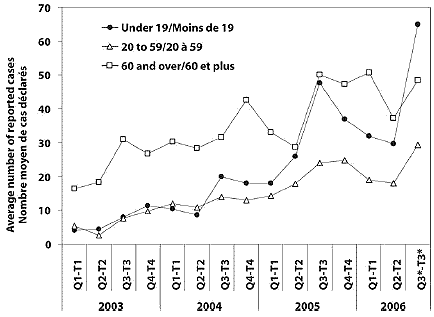
Reported cases of MRSA in the northern RHAs of Burntwood and Norman (Figure 1A) have increased dramatically since 2003, showing spikes in the crude rates reported during the summer months (Figure 1B). These rising rates and seasonal trends are observed in all age groups but especially in young people aged ≤ 19 (Figure 1C). Interpretation of the observed trends is limited because the available data do not distinguish between CA- and HCA-MRSA, and the extent of potential inconsistencies in reporting is unknown. Nonetheless, the available evidence suggests that the recent expansion of MRSA is concentrated among those aged < 20 residing in the First Nations communities of Burntwood and Norman.
Discussion
Observed increases in cases of MRSA among young people in northern health regions over the past 4 years, along with annual seasonal peaks, suggests that a unique combination of factors may be contributing to this novel infection pattern.While rates in southern regional health authorities, including Winnipeg, have remained relatively consistent, observed increases among children and adolescents in the summer months deserve close investigation. Seasonality has not been previously reported as a characteristic of MRSA, and it is not clear whether the observed pattern is related to the genetics of the pathogen, host behaviours or patterns of activity in the community and/or nursing stations. The number of cases associated with insect bites and skin abrasions in one community may partially explain observed seasonal trends.
Figure 1B. Rising levels of MRSA reported in northern Manitoba over the last 3 years – average (3-month) crude rates of MRSA reported to Manitoba Health, by RHA
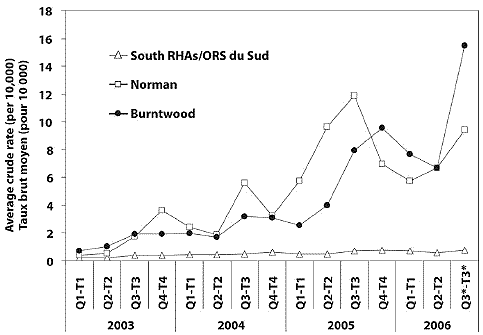
Figure 1C. Rising levels of MRSA reported in northern Manitoba over the last 3 years – average (3-month) reported cases of MRS in Manitoba by age group
Risk factors for CA-MRSA remain largely undefined, but socioeconomic factors, crowded housing conditions and limited access to health care have been implicated1. In a case-control study involving an Alaskan Native population, frequency of antibiotic use in the previous 12 months correlated with MRSA infection in a dose-dependent manner10. In a recent study of MRSA infections in patients without established risk factors in Baltimore, Atlanta and Minnesota, a large proportion of cases were associated with underlying health conditions (smoking, diabetes, asthma and non-infectious skin conditions such as eczema), crowded households (defined in this study as more than one person per bedroom), antibiotic use in the previous year and contact with health care settings (visiting a doctor's office, working in a health care setting or living with someone in contact with a health care setting)11. These findings suggest a range of factors that may be relevant in First Nations communities, where rates of diabetes are high, homes are crowded and nursing stations are the only point of contact with a formal health care system. Accurate epidemiologic data, safety guidelines, contact information, demographic data, diagnosis, strain identification and treatment are critical in managing hospital outbreaks of MRSA12,13 , but resources for these activities in First Nations communities are limited. An important first step towards defining MRSA outbreaks should be separate reporting of CA- and HCA-MRSA infections, as previously recommended 1. Other measures might include reduction in antibiotic use, optimization of water supplies, and improved hand washing by health care providers, as recently recommended by the Canadian Paediatric Society14.
A case-control study is currently under way in neighbouring Saskatchewan (M. Mulvey, Head, Hospital Infections, National Microbiology Laboratory: personal communication, 2006). This effort might be expanded to communities in Manitoba and should focus on suspected risk factors for CA-MRSA, such as recent antibiotic use, contact with health care facilities (nursing stations, MediVac air transport, hospitals in The Pas, Thompson andWinnipeg), crowded housing (according to the Canadian definition of > 0.4 persons per room15), non-infectious skin diseases, smoking and chronic conditions such as diabetes. In the meantime, community members and health care providers must be informed in order to respond rapidly to emergencies that result from invasive MRSA infections, particularly among young people in remote communities.
Acknowledgements
The authors would like to thank the Dr. M. Mulvey, Head, Hospital Infections, National Microbiology Laboratory, Public Health Agency of Canada, Winnipeg, Manitoba, Dr. J. Wylie, Manitoba Health, Cadham Provincial Laboratory, Winnipeg, Dr. P. Orr, Department of Medical Microbiology, University of Manitoba and the University of Manitoba's CIHR/ICID National Training Program in Infectious Diseases for their helpful comments on this paper. Any errors are the responsibility of the authors.
References
1. Wylie J, Nowicki D. Molecular epidemiology of communityand health care-associated methicillin-resistant Staphylococcus aureus in Manitoba, Canada. J Clin Microbiol 2005;43:2830-6.
2. Centers for Disease Control and Prevention. Four pediatric deaths from community-acquired methicillin-resistant Staphylococcus aureus – Minnesota and North Dakota, 1991-1999. MMWR 1999;48:701-10.
3. Gonzalez BE, Martinez-Aguilar G, Hulten KG et al. Severe staphylococcal sepsis in adolescents in the era of communityacquired methicillin-resistant Staphylococcus aureus. Pediatrics 2005;115:642-8.
4. Miller LG, Perdreau-Remington F, Rieg G et al. Necrotizing fasciitis caused by community-associated methicillin-resistant Staphylococcus aureus in Los Angeles. N Engl J Med 2005;352:1445-53.
5. Ofner-Agostini M, Simor AE, Mulvey M et al. Methicillinresistant Staphylococcus aureus in Canadian Aboriginal people. Infect Control Hosp Epidemiol 2006;27:204-7.
6. Mulvey MR, MacDougall L, Cholin B et al. Community associated methicillin-resistant Staphylococcus aureus, Canada. Emerg Infect Dis 2005;11:844-50.
7. Chambers HF. Community-associated MRSA – resistance and virulence converge. N Engl J Med 2005;352:1485-7.
8. Communicable Disease Control Unit, Manitoba Health, Winnipeg. Surveillance & epidemiology: Monthly summary of communicable diseases. URL: <http://www.gov.mb.ca/health/ publichealth/cdc/surveillance/index.html#summary>. Accessed 21 February, 2006.
9. Manitoba Health. Population report: June 1, 2004. URL: <http://www.gov.mb.ca/health/population/2004/ index.html>. Accessed 21 Feb, 2006.
10. Baggett HC, Hennessy TW, Rudolph K et al. Communityonset methicillin-resistant Staphylococcus aureus associated with antibiotic use and the cytotoxin Panton-Valentine leukocidin during a furunculosis outbreak in rural Alaska. J Infect Dis 2004;189:1565-73.
11. Fridkin SK, Hageman JC, Morrison M et al. Methicillin-resistant Staphylococcus aureus disease in three communities. N Engl J Med 2005;352:1436-44.
12. Centers for Disease Control and Prevention. Community associated MRSA: Information for clinicians. URL: <http://www. cdc.gov/ncidod/dhqp/ar_mrsa_ca_clinicians.html#4>. Accessed 24 February, 2006.
13. Harbarth S, Pittet D. Methicillin-resistant Staphylococcus aureus. Lancet Infect Dis 2005;5:653-63.
14. Canadian Paediatric Society. Methicillin-resistant Staphylococcus aureus in First Nations communities in Canada. Position Statement: FNIH 2005-02. Paediatr Child Health 2005;10:557-9.
15. Indian and Northern Affairs Canada. Highlights from the report of the Royal Commission on Aboriginal Peoples: People to people, nation to nations. URL: < http://www.ainc-inac.gc.ca/ ch/rcap/rpt/index_e.html>. Accessed 3 October, 2005.
Outbreak of Escherichia coli O157:H7 gastroenteritis associated with consumption of beef donairs, Edmonton, Alberta, May - June 2006
L Honish, MSc, CPHI(C) (1), I Zazulak, CPHI(C) (1), R Mahabeer, BA, BEH(AD), CPHI(C) (1), K Krywiak, BSc, CPHI(C) (1), R Leyland, BSc, CPHI(C) (1), N Hislop, MSc CPHI(C) (1), L Chui, PhD (2)
1 Capital Health - Public Health Division, Edmonton, Alberta
2 Provincial Public Health Laboratory, Edmonton, Alberta
Twelve cases of laboratory-confirmed Escherichia coli O157:H7 intestinal infection were identified through notifiable disease surveillance in the Capital Health Region (metro Edmonton, Alberta) in May 2006. During the previous 5 years, the average annual incidence in the region had been 51 cases and the average during the month of May 5.2 cases. Initial follow-up (i.e. administration of a standard E. coli O157:H7 exposure questionnaire to cases) by Capital Health - Environmental Public Health Services (EPHS) revealed no epidemiologic links. Enhanced surveillance methods were employed, which resulted in the identification of an outbreak associated with consumption of beef “donairs” (see Discussion) from one local restaurant chain. This enhanced surveillance and the subsequent outbreak investigation are summarized here.
Methods
Demographic analysis of E. coli O157:H7 cases reported in the region during May and June 2006 revealed that most cases were males aged 19 to 26 years. An enhanced hypothesis-generating questionnaire, including items on exposures thought to be common in this particular age/sex group, was developed and administered to cluster cases. At the time of the outbreak, a local professional hockey team was involved in a playoff tournament, during which informal postgame celebrations, involving several thousand participants, frequently occurred in Edmonton along an approximately 10-cityblock strip with a high density of drinking and eating establishments. Outbreak cases were asked about participation in these festivities; a hockey game schedule for the team obtained from an Internet Website was used to assist recall. Several cases reported taking part in the hockey celebrations, and when prompted about food history during the festivities these cases also reported consumption of beef donairs from one Edmonton restaurant specializing in this food product. Other outbreak cases also recalled that during the incubation period they had consumed donairs from a different Edmonton location of the same restaurant chain.
This information prompted an investigation of the implicated donair restaurant chain and a source meat processing facility. The investigation included inspections of the implicated facilities and interviews with the facility operators, collection of representative food samples and collection of stool specimens from employees of an implicated restaurant. Food samples and stool specimens were submitted to Alberta's Provincial Public Health Laboratory (PPHL) for microbiologic analysis. All human E. coli O157:H7 isolates identified in the health region are subject to pulsed-field gel electrophoresis (PFGE) profiling by the PPHL. A predominant PFGE pattern was identified among case isolates in the May-June E. coli O157:H7 cluster, which was used to refine the case definition. This pattern was also compared with a PPHL database containing all E. coli O157:H7 PFGE patterns observed in the province since 1998. Other provincial and federal health and food safety agencies were advised of the outbreak in order that they could assist with the investigation.
Results
Case definition
The case definition was restricted to residents of or visitors to the Capital Health Region who were positive for E. coli O157:H7 national PFGE pattern ECXAI 0.1455 (or a different PFGE pattern if epidemiologically linked to a pattern ECXAI 0.1455 case) in stool collected between 1 May and 30 June, 2006. A total of nine cases met this definition - eight cases were infected with an isolate of provincial PFGE pattern ECXAI 0.1455, and a ninth case was infected with an isolate of pattern ECXAI 0.1468. Both PFGE patterns had not been previously observed in Alberta. There were nine additional laboratory-confirmed E. coli O157:H7 cases reported in the Capital Health Region during this same period that did not meet the case definition.
Demographic information
Six cases (67%) were male. The mean and median ages were 23.7 and 22.0 years respectively, with a range of 2 to 45. Six cases (67%) were aged 19 to 26 years. All but one case were residents of the Capital Health Region; one case resided in another health region of Alberta.
Disease presentation
The predominant symptoms reported were diarrhea (100%) and bloody diarrhea (56%). None of the cases was hospitalized as a result of infection, and there were no known resultant cases of hemolytic uremic syndrome. Dates of onset ranged between 13 May and 19 June, 2006; all but one of the cases reported onset during the month of May (Table 1). An incubation period was estimated for three cases that reported the exact date of consumption of the implicated food; these were 3, 5 and 9 days. Other cases could recall only a date range within their incubation period during which the implicated food was consumed.
Table 1. Donair-associated Escherichia coli O157:H7 outbreak cases in the Capital Health Region, May and June 2006, with reported onset date, donair consumption date/range and location of donair purchase
| Case number | Onset date* | Donair consumption date/range* | Location of donair purchase |
|---|---|---|---|
| 1 | 13-May | May 6-13 | Location B |
| 2 | 27-May | May 19-21 | Location A |
| 3 | 28-May | 25-May | Location A |
| 4 | 28-May | May 18-27 | Location A |
| 5 | 28-May | 19-May | Location A |
| 6 | 29-May | May 19-27 | Location B |
| 7 | 19-Jun | 14-Jun | Location A |
| *All dates are during the calendar year 2006. | |||
Food/exposure histories
Of the nine outbreak cases, seven (78%) reported consumption of a beef donair during the incubation period. This food item was purchased at one of two locations of an Edmonton restaurant chain specializing in the food product (Table 1). The two cases that did not report donair consumption had not been administered the enhanced exposure questionnaire (lost to follow-up). There were six locations (designated A-F) of the implicated restaurant chain in the Capital Health Region at the time of the outbreak. Of those cases that reported donair consumption, five (71%) purchased the donair at restaurant location A, and two (29%) at restaurant location B. Location A is located in the area of Edmonton where the hockey post-game celebrations, discussed earlier, took place. There were no other significant epidemiologic links identified among cases.
Investigation of the implicated restaurant chain
Beef donair at the implicated restaurants was prepared by adding spices to ground beef, mixing with a food processor until the meat was more finely ground, then shaping the meat into a “cone” on a rod. Cones were then covered with plastic wrap, and frozen. All locations reported that frozen beef donair cones were then placed directly onto a rotisserie without thawing and heated on the rotisserie until they appeared cooked; meat was then sliced off the cone to order. Beef sliced from donair cones was placed into a pita with processed cheese, tomatoes, lettuce and sauce (canned evaporated milk, sugar, vinegar) and then served. All locations except location B reported that meat sliced from the cone was additionally cooked on a grill before being served (location A and three other locations reported that the meat was always cooked on a grill, one location reported that meat was cooked on a grill only if the color of the meat made it appear undercooked after slicing off the cone). Location B reported that donair meat was cooked on the rotisserie only. Thermometers were rarely or never used to verify donair meat cooking temperatures; meat colour was used as a guide. At all locations, the unused portions of donair cones were usually placed in a refrigerator or freezer at the end of the business day and placed on the rotisserie the following day.
Spices for donair cones served at locations A and B were obtained from different suppliers, but vegetables and processed cheese for beef donairs were obtained from the same supplier. Ground beef for donair cones served by locations A and B and two additional locations (C and D) originated from the same small specialty meat supplier, located in the Edmonton area. Locations A and D received cones prepared at location C; location B prepared cones on site. The remaining locations (E and F) also prepared cones on site but received ground beef for donair cones from suppliers different from each other and from locations A, B, C and D.
Food sample results
There was no beef available for analysis from the same lot as was served to outbreak cases; however, five beef samples were collected as part of the investigation. Four were donair beef samples from location A (two cooked donair cone surface cuts, one deep cut that appeared undercooked) or location B (one sample of raw donair beef). One raw ground beef sample was collected from the meat facility from which ground beef originated for donair meat served by locations A, B, C and D. All beef samples were negative for E. coli O157:H7.
Employee stool specimen results
The last case identified in the outbreak reported consumption of a beef donair from location A on 14 June, i.e. 18 days following donair consumption in the previously last case identified and following review of the donair cooking procedures by EPHS. Food handling employees of location A were investigated as a possible outbreak source. The two food handling employees of location A were screened for E. coli O157:H7 in stool (collected 29 June); both were negative. Locations A and B reportedly had no employees in common.
Case finding
On 9 June, to facilitate case finding, an alert was posted on CIOSC (Canadian Integrated Outbreak Surveillance Centre), a secure Web-based system through which outbreak alerts are distributed to local, provincial and national enteric disease surveillance professionals nationwide. The prominent PFGE profile was also posted on PulseNet USA and PulseNet Canada, the National Molecular Subtyping Network for Foodborne Disease Surveillance, by PPHL. Case finding methods resulted in the identification of one case outside of the Capital Health Region.
Discussion
Donairs (and similar products called doner kebabs, gyros, shawirmas and chawarmas) are specialty foods of Middle Eastern origin that have been served by Canadian retail food facilities for over 30 years, typically prepared by placing meat (usually spiced ground beef that has been formed into a conical shape) onto a rotisserie on which it is cooked, sliced and placed into a pita wrap with vegetables and condiments1. A Calgary, Alberta, outbreak of E. coli O157:H7 in 2004 involving 43 cases was associated with consumption of beef donairs2. Similar foods have been associated with outbreaks of Salmonella infection3,4 . It was reported in a 2006 Turkish study that over 25% of cooked doner kebab beef samples were contaminated with E. coli O157:H7(5). Improper handling of such products has long been known to be a potential foodborne illness risk 6,7.
This investigation confirms that an outbreak of E. coli O157:H7 infection occurred in the Capital Health Region in May and June 2006: eight cases infected with this pathogen of PFGE pattern not previously observed in Alberta (and one case epidemiologically linked to these cases) occurred during this period. The availability of PFGE pattern information for all E. coli O157:H7 cases during the outbreak was critical in developing a specific outbreak case definition. This allowed the investigators to detect background cases and focus the investigation on exposures among outbreak cases. A predominant PFGE pattern is also consistent with one specific food association among outbreak cases - isolates of an indistinguishable PFGE pattern collected from different individuals suggests a common source8.
There is strong epidemiologic evidence linking consumption of beef donairs from one of two locations of a restaurant chain and infection in outbreak cases: seven of nine cases reported this exposure, and there was no other significant epidemiologic link identified among the cases. The two implicated restaurant locations received ground beef for donair cones from the same small specialty supplier, consistent with the hypothesis that ground beef (frequently implicated in E. coli O157:H7 outbreaks in Canada 9) was the source ingredient. Food (ground beef) samples collected as part of the investigation were all negative for E. coli O157:H7, and thus the source of this outbreak was not laboratory confirmed; however, there were no beef samples available from the same lot as was served to outbreak cases, and thus it cannot be determined whether the beef served to cases was truly contaminated. Neither could it be determined whether other donair ingredients (such as lettuce and tomatoes) were contaminated with the pathogen, nor whether food handlers may have been the source, as it is not known whether they were shedding the pathogen at the time the implicated food was prepared. The lack of employees common to both implicated locations means that multiple employees would have to have been infected during the outbreak period for this to be the source.
There was evidence of mishandling of ground beef at the implicated restaurants, which may have been a contributing factor in this outbreak. Processes that may have resulted in pathogenic survival or growth in donair meat included the use of unreliable methods to confirm the thoroughness of ground beef cooking, and the re-heating and serving of donair meat that had been kept on a rotisserie the previous day and then refrigerated or frozen whole. The likelihood of donair beef undercooking may have been further increased by high customer volume reportedly observed during post-hockey game celebrations in the vicinity of one implicated location and the possible resultant reduction in the length of time that donair beef was cooked on the rotisserie in response to this increased demand.
Conclusion
The risks associated with the potential mishandling of donairs have been identified previously in Canada, and at the time of this outbreak, local, provincial and federal health and food safety agencies were working collaboratively to devise strategies to reduce the risk1. This outbreak has demonstrated the importance of the continuation of this work, to help ensure that this food product is safe in Canada.
Acknowledgements
The authors thank the following for their assistance: D. Everett, Alberta Health and Wellness, Edmonton, Alberta; C. Assen, Canadian Food Inspection Agency - Food Safety and Fair Labeling (Alberta North), Edmonton; C. Munroe, Alberta Agriculture, Food and Rural Development-Regulatory Services Division, Edmonton; A. Jessome, Northern Lights Health Region, Fort McMurray, Alberta; J. Fuller, Provincial Public Health Laboratory, Edmonton; V. Mah, C. Galbraith, D. Langier-Blythe, P. Wagner, K. Shaw and G. Predy, Capital Health - Public Health Division, Edmonton.
References
1. Health Canada. Issue identification paper: Donairs (and similar products), June 2006 draft. Ottawa: Health Canada, 2006.
2. Currie A. Outbreak of E. coli O157:H7 infections in Calgary Health Region, September to October, 2004: Summary report. Calgary: Calgary Health Region, 2005.
3. Evans MR, Salmon RL, Nehaul L et al. An outbreak of Salmonella typhimurium DT170 associated with kebab meat and yogurt relish. Epidemiol Infect 1999;122:377-83.
4. Synnott M, Morse DL, Maguire H et al. An outbreak of Salmonella mikawasima associated with doner kebabs. Epidemiol Infect 1993;111:473-81.
5. Ulukanli Z, Cavli P. Detection of Escherichia coli O157:H7 from beef doner kebabs sold in Kars. G U J Sci 2006;19:99-104.
6. Todd ECD, Szabo R, Spiring F. Donairs (gyros) – potential hazards and control. J Food Prot 1986;49:369-77.
7. Bryan FL, Standley SR, Hendersen WC. Time-temperature conditions of gyros. J Food Prot 1980;43;346-53.
8. Harrington SM, Bishai WR. Molecular epidemiology and infectious diseases. In: Nelson KE, Willams CM, Graham NMH, eds. Infectious disease epidemiology: Theory and practice. Gaithersburg, MD: Aspen Publishers Inc., 2001;205.
9. Todd ECD. Escherichia coli O157:H7 infections associated with ground beef and their control in Canada. CCDR 2000:26(13):111-6.
Page details
- Date modified:
