Archived Committee Report – Public Health Approach November 28-29 2018
Chemicals Management Plan Science Committee
Public health approach to chemicals management in Canada
On this page
- Introduction and overview of process
- Charge Question 1
- Charge Question 2
- Charge Question 3
- Conclusions
- Glossary
- References
- Appendix
Introduction and overview of process
Health Canada (HC) and Environment and Climate Change Canada (ECCC) (the departments) through the Chemicals Management Plan (CMP) are exploring the development of a roadmap for implementing a public health/population health approach to support chemical risk assessment and management in Canada. It is recognized that such an approach would take significant resources and time to move forward. We define a public health approach as an "approach [that] would attempt to tie increased risk of specific diseases or outcomes to chemical management actions (i.e. research, monitoring and surveillance, priority setting, risk assessments, risk management)."
As part of this effort, the CMP Science Committee (SC) was requested to consider opportunities and challenges associated with such an approach, including offering suggestions about which foundational elements could be appropriate to help build a roadmap to advance it.
The SC agreed that a successful outcome of such an initiative would better anchor chemicals management within a population health approach, and is fundamentally linked to an ecosystem approach as exemplified by the "One Health" concept as well as other similar approaches (Aguirre et al., 2016; OHC, 2019). "One Health" is among several similar initiatives that include "ecohealth," which is supported by Canada's International Development Research Centre (IDRC, 2010) and "planetary health" by the United States (U.S.)-based Rockefeller Foundation (Planetary Health, 2019). A "public health" or "population health" approach with an environmental health component can be seen to be more holistic than other chemical management approaches that focus only on chemical exposures or only on disease outcomes, because public health sciences focus on the full range of disease determinants and links between exposures and diseases, with the aim of improving disease prevention and control through diverse interventions (for example, with targets ranging from the level of individuals through to whole populations). In a complementary way, "One Health" aims to achieve optimal health for "people, animals and our environment" (American Veterinary Medical Association, One Health, 2008). These approaches may assist in shaping the federal government's efforts to address the renewal of the Canadian Environmental Protection Act, 1999 (CEPA 1999) (Parliament of Canada, 2017) and might allow improved articulation of the form and direction of the post-2020 phase of the CMP.
The SC was asked to consider a broad framing of the CMP within a public health approach in Canada. The SC's consideration was shaped by 3 Charge Questions posed by the departments. This report summarizes the outcome of a 2 day meeting held in Ottawa to discuss these Charge Questions.
Charge Question 1
Could the CMP SC provide considerations related to the opportunities and challenges for the development of a public health approach to chemicals management in Canada?
Many opportunities were identified and discussed:
- The SC discussed the opportunities presented by enriching the current chemicals management paradigm that considers chemical risk. That enrichment would be moving from a chemical-by-chemical and chemical grouping approach to include a more holistic approach based on multiple determinants of health, where 1 or more of those determinants is chemical exposure. By addressing the real-world context (for example, complexities of multiple exposures to multiple stressors, not just chemical stressors, throughout the life course), a public health lens would aim to establish links between the risk of disease or early markers of adverse effects and chemicals management actions, and further to allow early screening for unanticipated exposure effects and other environmental (including social) and genetic factors relating to adverse health outcomes.
- The addition of a public health approach noted above could be developed from existing health-based approaches by adding, as appropriate, public health-associated competencies and technologies into an enhanced chemicals management approach, where problem solving includes analyses of the endpoints (for example, disease states) and seeks to determine the contribution of chemical insult as a causal agent. This approach might result in a shift from the direct causal or deterministic approach of "A causes B" towards adopting a "probability of causation" (PoC) approach for chemicals management, which would subsequently inform preventative risk management actions. A PoC approach acknowledges the uncertainties and the statistical probability (including stochasticity) inherent in drawing a causal connection between A and B. PoC has been used in legal decisions, occupational health rulings, and toxicological decisions (for example, Pearl, 1999; Robins and Greenland, 1989). Arguably, in the context of environmental factors and public health, a PoC approach could consider the strength and uncertainties of causality using a weight of evidence approach, whose use is mandated in CEPA 1999. The approach would need to explicitly consider multiple uncertainties, noting that the basis of the approach lies in estimating probabilities. The concept of considering a PoC approach is discussed further under Charge Question 3a.
- Another element of incorporating a public health approach comes in recognizing "One Health" and similar concepts, as noted above. "One Health" is a transdisciplinary concept that incorporates multi-sector expertise to ensure the health of humans, animals, and ecosystems (for example, One Health Commission). Within this report, the SC uses the term holistic in this general sense. Further, the "One Health" approach seeks optimal health for human and ecosystem populations-from local to global scales-by embracing transdisciplinary and inter-sectoral approaches (Aguirre et al., 2016). The term "One Health" is relatively new, but the fundamental concepts underlying the approach were first proposed by Hippocrates over 2,000 years ago. The "One Health" approach is being explored by various government programs in the U.S., Europe, and elsewhere, as well as by prominent global organizations such as the World Health Organization (WHO) and the Food and Agriculture Organization (FAO) of the United Nations. This approach recognizes and promotes the value of ecosystem protection in and of itself. In addition, the approaches take a more inclusive stance that could provide for early warning indicators of causative agents by considering impacts on any sensitive ecosystem population as an indicator of adverse health effects that could impact other species, including the human population. While recognizing that the approach must evolve rather than being adopted as a single change, an opportunity exists in Canada to explore such an approach given the existing expertise in ecosystem and human health population studies, particularly in academia and government, as well as ongoing communication and partnerships between these communities.
Realizing a paradigm shift of including a public health approach comes with identifying expertise and opportunities. As listed under Charge Question 2b, Canada has numerous existing resources and expertise, including human and ecological surveillance and monitoring programs and platforms that could be accessed and leveraged. Canadian health care systems are repositories of considerable data. The country also has several established prospective cohort studies, including the Canadian Partnership for Tomorrow Project (CPTP), which has the design and scale that yields the potential to advance the understanding of environmental chemical effects (see Charge Question 2b). Additionally, Canada is in a strong position to link data systems, which include environmental, socio-demographic, and health systems data. New "big data analytics" offer opportunities for linking such data sets. Further, public health education in Canada is undergoing significant growth, with strong programs in toxicology, exposure science, epidemiology, and data science, including training in new technologies and approaches [for example, computational toxicology, "omics," new approach methodologies (NAMs)]. It is anticipated that a readily available expert group will emerge over the next generation to help shape the direction of an enhanced and more comprehensive chemicals management program. This could include experts from various governments, academics, and research organizations. It could include re-evaluating and updating previous decisions.
The SC recognized that other public health-focused groups, including those in Canada (such as federal and provincial public health agencies and academics), are studying and monitoring the patterns and determinants of health and disease via different and more comprehensive approaches that include the surveillance of known pathogens and potentially harmful exposures. The SC saw the opportunity to acknowledge and potentially link with such groups. The SC observed numerous "roadmaps" or frameworks that would accompany each group's effort, and that there is an opportunity to build bridges between roadmaps and foster collaborative opportunities internationally. Further, this initiative can learn from other initiatives such as that of the U.S. National Institute of Environmental Health Sciences (NIEHS) for which their strategic plan takes a public health approach (Birnbaum, 2018; Pattibone et al., 2018), although the degree to which this has been implemented is uncertain. Lessons can be learned from other examples such as those mentioned in the introduction.
The SC discussed the well-established public health approach for pathogen discovery as a useful example. By illustration, the SC noted genomic-based advances in modern molecular microbiology as applied in public health have demonstrated how new methods, used within surveillance programs, can enable outbreaks (in other words, disease states) to be characterized and controlled. Such an approach applied to chemicals management would initially focus on currently available hazard data. Subsequently, the results of high-throughput toxicity and exposure screening could also be used for prioritization purposes.
Further, a public health approach would emphasize that sizable economic costs of inaction exist and that win-win solutions could be sought in which sound and inter-sectoral chemicals management decisions can be taken. Together, these not only improve the environment and health but also the economy (Landrigan et al., 2018).
In summary, working towards a public/population health or a more multidimensional approach would have numerous and important long-term advantages. A multidimensional process to create such an approach will be required, comprising numerous incremental steps, as discussed under Charge Question 3a.
Similarly, many challenges were also identified and discussed:
As previously noted, taking a population health approach involves taking a transdisciplinary as well as inter-sectoral view, which necessarily requires coordination and some level of integration across multiple teams. A clear challenge to moving forward is dealing with multiple institutional barriers in terms of cooperation and information sharing (see Charge Question 2). Such barriers can be broken down and resolved by various means to create partnerships, which takes willingness, considerable effort and patience, and resources (such as, time and funding). Practically, the SC discussed the need for greater data availability, engagement with the health research and health systems communities, and cross-government coordination (for example, Health Canada, public health agencies, Statistics Canada).
First, the paradigm shift discussed above requires the aspiration and commitment to build capacity to enable the shift. Then, significant theoretical and methodological advances must be identified and promoted. One clear issue is that adopting a "disease causation" scheme in chemicals management must consider the latency that often exists between exposure and the outcome of an adverse effect, which is one reason why the long-term prospective cohort studies are instrumental. Sustained data collection and surveillance-based approaches to track the health of populations are of importance. Traditionally, this was demonstrated in public health where infectious disease pathogens were known or suspected. The same methods are now routinely applied to track long-term effects that lead to chronic diseases (for example, tobacco smoke and cancer). As an example, the SC discussed several ideas that build on existing surveillance and research approaches to investigate childhood cancers. Further, in some cases, ecosystem species can be harbingers of chemical-related adverse effects before they become apparent in human populations (in other words, the argument for taking the "One Health" or a similar approach).
Another theoretical advancement is needed to relate a disease state with a chemical agent while recognizing that the disease state may have multiple causative agents, including non-chemical stressors. This challenge is compounded by recognizing the latency of disease while identifying multiple stressors that are changing over time. Examples of such non-chemical stressors include socioeconomic status and multiple impacts from a changing climate. In response to this challenge, the SC commented that ambiguities in establishing a causal relationship can, in part, be addressed by using indicators of endpoints upstream of apical effects within the broader context of adverse outcome pathways (AOPs) (Tollefsen et al., 2014). Teasing apart contributions from multiple stressors, including non-chemical stressors, will be complicated and require long-term and sustained monitoring data across the Canadian population; it would likely be best investigated by taking a systems analysis approach.
In terms of chemicals management decisions and actions, questions exist about the level of proof that would be required if a public health paradigm was built into the chemicals management program. What would the acceptable level of uncertainty for making decisions on chemicals' management within a public health-based approach be? Are current processes and practices within the CMP sufficiently robust and precautionary? Are data availability and their quality and quantity sufficient for taking a public health approach? Given that these issues are problematic today, the challenge would be even greater considering a broader program driven by data.
It was noted that surveillance programs that detect no effects are as important and informative as those that identify an adverse impact-both provide directional clues in forging links between chemical exposures and population impacts. Positive results are more straightforward to react to, and conclude that "X causes Y." Negative data, particularly from well-designed and large-scale surveillance programs, also provide the benefits associated with the reassurance that adverse effects are not occurring, along with evidence to support priority setting.
Moving in a public health direction could be facilitated by the expansion of existing and recently created tools, including those of surveillance such as existing biomonitoring programs [for example, to expand existing programs to include long-term prospective cohorts such as the Canadian Health Measures Survey (CHMS 2019), the National Health and Nutrition Examination Survey (NHANES 2019), Great Lakes monitoring program (ECCC 2017)], plus new analytical methods and an organizational framework to assemble all the data streams for assessments (Basu and Lanphear, 2019). The need for long-term, stable funding in governmental and research organizations and having the funding to develop the necessary new infrastructure and methods are key challenges for meeting the need for adding a public health approach. The SC noted that these will be costly. However, the cost of building such a program needs to be weighed against the public health and ecosystems costs incurred by not taking such an approach.
Another challenge identified by the SC was communicating the complexities (including risk outcomes) to decision makers and the public.
Finally, to include a public health approach, weighing the benefits associated with a specific chemical identified as potentially being associated with a health or environmental risk will need to be considered.
Charge Question 2
The SC broke down this question into its 3 components. Based on the data and tools currently available, what gaps exist that would create a barrier to the implementation of a public health approach to chemicals management in Canada? What other data and tools would be required to move this approach forward? Are there certain disease states that have a clearer link to chemical exposure that should be focused on for generation of data and tools?
Charge Question 2a
Based on the data and tools currently available, what gaps exist that would create a barrier to the implementation of a public health approach to chemicals management in Canada?
The SC addressed this question in 3 distinct groupings:
1. Knowledge gaps
Numerous knowledge gaps must be filled in order to understand the health effects of chemicals within a population health paradigm. These gaps may be accentuated for those chemicals management programs that do not have explicit minimum data requirements and for which data is not readily publicly available (for example, chemicals that are not a pesticide, a food/deliberate food additive, or a drug, and therefore have minimal reporting requirements). These gaps must be identified and organized into a logical and accessible framework. A sound framework, consistent with a public health approach, would allow us to move from "known knowns" to "known unknowns," and finally to include current "unknown unknowns." Such a knowledge base needs to capture not only the general population but also vulnerable groups and ecosystems. An option could be building the framework under the auspices of the "One Health" (or similar) approach (in other words, combine resources, data, methods, etc. from the human and ecosystem communities). Within this framework, scoping could begin on what data exist and what data are needed. Then the gaps can be clearly identified, along with the agencies and other organizations most likely able to fill those gaps.
Additional gaps are likely to become evident as part of efforts to scale up from what is relevant and required on the small scale and that is available today (and possibly being done extremely well), to what is required on a large scale and in the future (in other words, in a screening or surveillance mode).
The SC discussed specific knowledge gaps that include data availability and accessibility (not only for the research community but also for the broader public who have a right to know). Here, it was noted that the U.S. and Canada [for example, Statistics Canada and provincial health organizations such as the Institute for Clinical Evaluative Sciences (ICES) in Ontario] are creating data centres to facilitate data sharing, which include technical details such as issues of data compatibility. Such issues were raised by the SC in previous reports where the SC discussed data sharing with international partners (CMPSC, 2015; CMPSC, 2017).
2. Gaps in availability of resources
Measurement and ongoing monitoring of a large number of chemicals and biomarkers in the human population and other species invariably require a sustained and significant investment. The need for financial resources must not be underestimated. The SC noted the opportunity to align infrastructure investment with the needs of a public health/"One Health" approach.
From a data-sharing perspective, the Government of Canada's Open Data policy still does not apply to data that would be useful for this approach [for example, the Canadian Health Measures Survey (CHMS, 2014) raw data, due to Statistics Canada Act restrictions, that may only be accessed via data centres, which creates a barrier to stakeholders and especially to the public]. Overall, steps need to be taken to make relevant data accessible and interpretable to all stakeholders.
The SC suggested that an analysis of data gaps should distinguish between the need for detailed, in-depth data collection versus less detailed, population-scale data collection. Core exploratory programs could be developed where centralized labs exist to perform specific types of research. Databases could be maintained in core centres and accessed by smaller research labs that would otherwise be unable to do this type of research due to financial limitations. The U.S. has funded the creation of such data centres to facilitate access to data from specific cohorts, but this effort is largely research-based. Health Canada has initiated discussions with Statistics Canada to develop a similar model [for example, the Canadian Census Health and Environment Cohort (CanCHEC)], which could be set up from the outset to be more surveillance based.
To fill the data gaps discussed, the collection and analysis of environmental biomarkers requires complex infrastructure and highly specialized expertise. For example, the CHMS relies heavily on the expertise of a limited number of laboratories such as the Institut national de santé publique du Québec (INSPQ), one of few labs in the country with the required expertise to conduct this highly specialized work. Internal capacity has also been established within Health Canada at other laboratories to undertake sample analysis of a select number of analytes. As noted above, funding to pursue this endeavour (for both capital and operating costs) would need to come from a realignment and expansion of existing programs. Predictive models could be used to address uncertainty in exposure information and data gaps could be monitored to offset some of this cost.
3. Institutional barriers
The SC noted several times the importance of institutional barriers. These barriers range from data access (in other words, access to information must become much easier than it is at present), to privacy concerns about data sharing and ownership across organizations and investigators, to jurisdictional issues. The barriers currently hamper efforts to integrate biomonitoring, ecological monitoring, and modelling efforts, including geospatial modelling, aimed at better characterizing exposure and effects. In addition, the SC commented on financial and professional considerations for access to data curated by others. The lack of available institutional data to the general public can be highly problematic in creating and communicating information within a population health framework; knowledge is lacking on which data gaps exist when access to the data is limited. Again, the creation of partnerships would minimize the problem of institutional barriers, which would take time, goodwill, and significant effort.
Charge Question 2b
What other data and tools would be required to move this approach forward?
The SC discussed at length the type of data and tools that could advance a public health approach. Some of the responses to Charge Question 2b also address Charge Question 3b about a suitable case study/studies. Several possibilities exist in response to Charge Question 2b:
- One focus should be on more highly exposed populations. An example here would be Indigenous Peoples exposed to country/traditional foods that could contain elevated levels of certain contaminants (notable studies exist, such as the First Nations Food, Nutrition and Environment Study as well as various population studies funded via the Northern Contaminants Program). Other examples are populations exposed occupationally to various classes of chemicals such as industrial chemicals, pharmaceuticals, or pesticides. Military personnel were discussed as another example, given the records that are kept that could allow for reconstructing potential exposures that may have occurred. These groups could be broadly considered to be "vulnerable populations" in Canada due to an increased exposure to specific chemicals. A shortcoming of many occupational studies is that they are retrospective and do not or have not collected biological samples. However, this shortcoming could be addressed by immediately expanding ongoing epidemiological studies and large prospective cohorts to include such sampling and baseline evaluations. Again, numerous institutional barriers may exist here, which would take some time to work through.
- The SC heard about existing cohorts, notably the CPTP, which itself is an assemblage of several provincial cohort studies (Dummer et al., 2018; see Appendix). There is much to be said for engaging with existing cohorts to realize a pan-Canada public health approach: it is achievable because it builds on current programs and activities and yet allows elements of a more generic framework to be identified and honed. However, the SC recognizes that this suggestion would require significant analysis and investment plus the recruitment of relevant subpopulations with appropriate exposure profiles.
- Canada has several bio-banks for ecosystem populations [for example, the National Wildlife Research Centre (NWRC) Specimen Bank, (NWRC Specimen Bank, ECCC, 2010)] that might be open to expanding chemical analyses. These could be useful sources of data due to the longevity of these programs, their spatial coverage, and the opportunity to realize a "One Health" approach using such data.
- A complication with most of the SC's suggestions is that for any individual for whom chemical information becomes available under a public health framework, the collection of non-chemical information (diet, health status) is necessary in order to derive as much value as possible. It was noted that this limitation is one reason why a large prospective cohort such as the CPTP has been launched in Canada.
- The SC discussed other tools that could be useful. It was agreed that non-targeted testing (for both exposures and outcomes) is a useful tool and that suspect screening could be incorporated into ongoing prospective cohort studies in order to identify which chemicals can be identified in particular populations (for example, through methods being discussed under the exposome concept). Exposure models can complement monitoring programs and address data gaps (Bonnell et al., 2018; Cowan-Ellsberry et al., 2009; Ring et al., 2019). In addition, within these same cohorts one may apply emergent "omics" technologies (for example, metabolomics, proteomics, transcriptomics, and exposomics), which promise to expand our understanding of health status and environmental exposures.
- Another tool is geospatial analyses and databases that are allowing better estimates of burden of disease (BoD) in specific areas, including geographic "hot spots" and vulnerable populations. These approaches allow for increasing granularity (for example, smaller geographic areas) and can allow for matching geospatially related exposure data with BoD to better understand the relationships. Platforms exist that can be adapted to be fit-for-purpose, which in early days should be mostly focused on prioritization [see EJSCREEN (U.S. EPA, 2014); EnviroAtlas (U.S. EPA, 2015)]. At the same time, studies with a more inclusive design (see the opportunities section under Charge Question 1) can be taken across the country to better pinpoint a national BoD from which decisions can be taken and progress tracked.
Charge Question 2c
Are there certain disease states that have a clearer link to chemical exposure that should be focused on for generation of data and tools?
Certain disease states are more likely to have a clear and direct link to chemical exposure than others. States with a high "signal to noise" (better defined as having a higher prevalence in a population related to a stressor of interest) are clearly those upon which to focus initially. For chronic diseases such as most cancers, identifying a meaningful biomarker or other interim biological response is obviously of greater value than relying on the final endpoint.
Disease states of higher concern with possibly clearer links to chemical exposure include those associated with brain development, given the research conducted on neurobehavioural toxicants [for example, adverse cognitive outcomes from lead exposure (Landrigan et al., 2018)]. The second suggestion related to cardiovascular outcomes. Neurobehavioural outcomes are a moving target with regards to changing and evolving technologies and recognition/measurement of impacts. Understanding clear causative agents of cardiovascular effects is complicated by the contributions from many other factors (for example, diet, lifestyle). Here, the question needs to be asked: What is the relative contribution (or relative risk) of the chemical exposure under consideration with respect to the other factors/stressors? These concerns were carried forward in the proposed elements of a roadmap in Charge Question 3.
The SC also discussed, but did not seek agreement on, other possible disease states of potentially higher interest, including those related to endocrine-disrupting compounds (EDCs). For example, some neurobehavioural adverse outcomes could be produced through an EDC pathway. It was noted that a focus on disease outcomes with AOPs associated with non-EATS (non-Estrogen receptor, Androgen receptor, Thyroid hormone pathways, and Steroidogenesis) pathways (CMP SC, 2018) might prove to be fruitful. A BoD approach may also help identify which disease states are of greatest concern in the country.
As noted above, the SC discussed the need to diagnose an effect upstream of the apical endpoint [for example, somewhere between a molecular-initiating event (MIE) and an apical effect]. An AOP approach might be useful here. An AOP is a conceptual framework that portrays existing knowledge concerning the linkage between 2 anchor points - the MIE and an adverse outcome (AO) - connected by a chain of key events (KEs) and the relationships between them. To enable the scientific community, in 1 central location, to share, develop, and discuss AOP-related knowledge, the Organisation for Economic Co-operation and Development (OECD) launched a project to develop the "Adverse Outcome Pathway Knowledge Base" (AOP-KB). The collaborative development of AOP descriptions and evidence is available through the AOP-Wiki.
The SC agreed that future work should build on the foundation of what is well described now and adopt the best ideas that are currently in place while ensuring that the framework is capable of adapting to constant change and "upgrades" that will continue to take place.
Charge Question 3
Charge Question 3a
With a focus on post-2020 chemicals management, could the CMP SC identify elements that should be considered as part of a roadmap to develop a public health approach to chemicals management in Canada that would be required in the short to medium term (for example, 5-10 years)?
The SC endorsed a number of existing and developing elements that would help to realize a public health/"One Health" approach within the CMP and to augment the current chemical-by-chemical risk-based approach. One goal of the overall public health approach is to establish links between disease risk and chemicals management actions. Other goals are to provide early screening for unanticipated exposures and impacts and thus enable a preventative and precautionary response. The value of such a program could be to increase recognition in the general public. The SC agreed that both aspects - human and ecosystem health - should be considered simultaneously as much as possible.
The conceptual model for a public health perspective presented by Gwinn and colleagues (2017) was seen as a useful starting point for identifying key elements that should be considered. The SC suggested that this conceptual model be more inclusive of human and ecological coverage and to add a focus on surveillance. The centre of this conceptual model is the goal of improved public health. The model illustrates the elements that go into achieving this goal, that build on elements used in a traditional risk assessment (which allows for past and future work conducted under CMP), and those currently used in taking a public health approach. The Gwinn et al. model identifies the need to assemble and connect multiple data sources to identify and implement appropriate prevention strategies.
One major element would be the emerging world of "omics" data, as discussed under Charge Questions 1 and 2, the increasing availability and applicability of which is a major enabling technology for this initiative. A well-designed comparative toxicogenomic and exposomic database would have links between chemicals, genes, outcomes, and exposures. Yet, to be effective, the framework has to be driven by health/disease outcomes and vulnerable populations rather than specific chemicals.
As previously discussed, existing prospective studies (see Appendix) might be early candidates to adopt elements of the framework.
The SC went further to propose elements of a "fit-for-purpose" framework that encapsulates the "One Health" and probability of causation approaches along with identifying key elements to achieve the proposed framework. These are illustrated in Figures 1 and 2 and in Table 1.
As illustrated in Figure 1, the framework would consider single and multiple chemical exposures to humans and health through a progression of levels of organization, starting from the cell, moving through to tissue, organs, and so forth, through to individuals, populations, and communities. Whereas a traditional risk assessment would relate the exposure(s) to a disease state, a public health and "One Health" approach would work backwards from the disease state towards the chemical exposure. This overall approach also acknowledges the multiple stressors (chemical and non-chemical) that can cause the disease state, not just the chemical exposure.
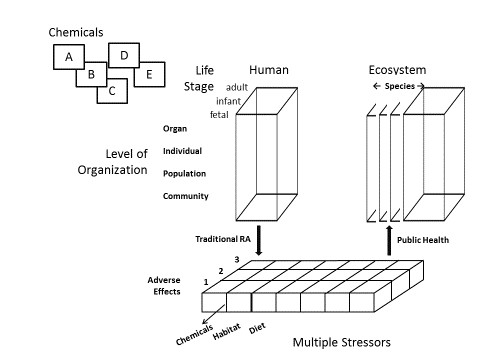
Figure 1 - Text description
The diagram shows proposed elements of a "fit-for-purpose" framework that encapsulates the "One Health" approach with identifying key elements to achieve the proposed framework. Single and multiple chemical exposures are represented by the letters A,B, C and D that are standalone and grouped together. The general framework includes Human and Ecosystem components. In the forward direction, work flow shows how currently chemical exposures are considered at the fetal, infant and adult stages starting from the cell and moving to tissue, organs, through to individuals, populations, and communities. In contrast, the "One Health" public health approach would work backwards from the disease state and ecosystem communities towards the chemical exposure. This overall approach also acknowledges the multiple stressors (chemical and non-chemical) that can cause the disease state, not just the chemical exposure.
In the forward direction, the workflow follows that of a traditional risk assessment. In the reverse direction, the workflow follows a public health/"One Health" approach.
To operationalize the general approach illustrated in Figure 1, the SC outlined a process that could be followed to arrive at a PoC, as shown in Figure 2. Linking to the adverse effect or disease state identified in Figure 1, the process would consider both toxicological and epidemiological evidence through a systematic review process (Figure 2). This consideration would or could use an expert panel to evaluate the consistency of evidence to arrive at a consensus outcome of a PoC. The process would involve developing a probabilistic exposure-response relationship that would relate to the BoD. The SC noted that Bayesian statistical methods have been used in this context.
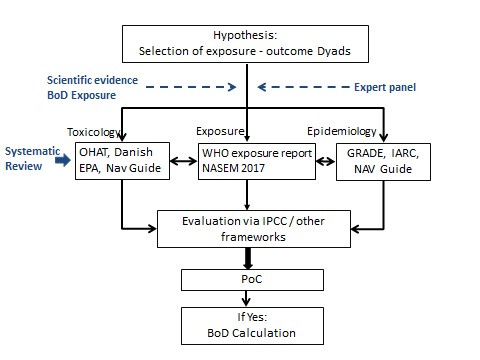
Figure 2 - Text description
BoD calculation. The process begins with the selection of the exposure-outcome Dyads, followed by consideration of BoD exposure data including WHO exposure report and NASEM 2017. Linking to the adverse effect or disease state identified in Figure 1, the process would next consider both toxicological (i.e. OHAT, Danish EPA and Nav Guide) and epidemiological evidence (i.e. GRADE, IARC and NAV Guide) through a systematic review process. This consideration could use an expert panel to evaluate the consistency of evidence via IPCC or other frameworks to arrive at a consensus of a PoC. The process would involve developing a probabilistic exposure-response relationship that would relate to the final BoD calculation outcome.
The end result of the workflow is a consensus statement of the PoC derived by considering toxicological and epidemiological evidence using a systematic review method. Elements with "Toxicology", "Exposure," and "Epidemiology" are given as examples. The final outcome would be an estimate of the BoD.
Table 1 presents key elements of a roadmap that would enable a public health approach to chemicals management. Capacity would be further developed and directed to focus surveillance, testing, and assessment on priority health outcomes and vulnerable groups that ultimately drive public and ecosystem health concerns.
| Capacity | Priority health outcomes + vulnerable groups |
|---|---|
Partnerships Canadian data sources
Technology (cores)/NAMs
Cohorts
Environmental surveillance platform
Data centres
Training/academics Adverse outcomes (chemical and intrinsic) Systems integration |
Common metrics/markers
|
Signals/evidence in real time (surveillance)
|
|
Multiple lines of evidence
|
|
Assessment process
|
|
Policy
|
Lastly, the SC noted that economic and policy aspects of public health decisions should be included in the framework, although no further discussion was held on how to achieve this.
Charge Question 3b
Could the CMP SC recommend a reasonable Canadian case study (in other words, disease of focus that has existing data available) that could be used as a "proof of concept" to validate the recommended roadmap elements to develop a public health approach to chemicals management? What data sources exist for the recommended case study? How would you measure that the "proof of concept" is a success?
The SC initially discussed applying current knowledge to 3 types of case studies that could be used as a proof of concept: (1) one where causality is settled ("known knowns") and for which a regulatory mandate exists (for example, mercury and brain development, under the auspices of the Minamata Convention); (2) working with an emerging contaminant of concern ["known unknowns"; for example, a suspected EDC and neurodevelopmental/reproductive concerns, or organophosphate pesticides and attention deficit hyperactivity disorder (ADHD)]; and (3) a current unknown hazard ("unknown unknown"). After discussion, the SC preferred to create criteria for consideration that would guide the choice of a case study/studies by the departments (see below). This decision was taken in part because the choice of case study was influenced by many considerations, including identifying a disease state of concern using situations where exposures are well characterized, reflecting the situation where all relevant confounders (in other words, other stressors) are well characterized, to a focus on available cohorts [for example, the Maternal-Infant Research on Environmental Chemicals (MIREC) study], and/or targeting case studies on ecological issues [such as bird populations, given the Canadian expertise in avian toxicology, long-lived cetaceans (whales), etc.].
The SC settled on the following case study/framework criteria to guide the selection of appropriate case studies by the departments:
- Availability of a high-quality cohort. An ongoing prospective study is preferred over a retrospective study, although this is not critical if there is the potential to reconstruct dose usage (for example, modelling approaches).
- Potential to impact diseases of concern.
- Availability of sources of relevant and necessary information, in addition to cohorts (environmental monitoring data/banked environmental specimens).
- Potential to incorporate emerging new approach methodologies (NAM) activities (for example, AOPs, exposomics/toxicogenomics).
- A high-priority regulatory or societal concern with a clear potential for successful intervention, so that the outcome has high value for translation into further adoption of "public health approaches" to chemicals management in addition to validation and acceptance by stakeholder communities.
Conclusions
- The SC discussed adopting a comprehensive and multidimensional public health approach to complement the current chemical-by-chemical and chemical grouping approaches. A public health approach could offer opportunities to advance early screening and precaution to minimize adverse impacts from chemical stressors.
- The SC supported broadening a public health approach to encompass a "One Health" or similar paradigm that simultaneously considers the health of the human population and ecosystems. The SC noted that some of the foundations and expertise for adopting a public health and "One Health" approach are now available but would require a significant realignment of priorities and resources. Adopting such an approach would entail dealing with significant challenges.
- The SC discussed approaches and frameworks that could enable the implementation of this approach. Again, the SC saw that the departments could make use of existing approaches, such as using a probability of causation method underpinned by a weight of evidence approach. Such a concept will require detailed analysis and review.
- The SC discussed how this approach could be implemented by noting the need, for example, for:
- expertise and capacity
- resources (time and money)
- improved data availability and linkages
- overcoming institutional barriers.
- One or more case studies could be undertaken in order to explore the feasibility of taking a public health approach:
- Consider 3 conditions of a "known known" (a known disease state caused by a known chemical stressor such as mercury), a "known unknown" [for example, a chemical stressor with known endocrine disruption activity and neurobehavioural, reproductive, or cardiovascular adverse outcome(s)], and then an "unknown unknown" (with uncertainty in the chemical stressor and adverse effect). The SC noted that this consideration could also be framed by referencing and incorporating current knowledge-to-action-cycle paradigms.
- Consider highly exposed human and/or ecosystem populations.
- Use existing cohorts and biobanks, as well as emerging and established tools such as non-target and suspect screening, geospatial analyses, and "omics."
Glossary
ADHD - attention deficit hyperactivity disorder
AO - adverse outcome
AOP - adverse outcome pathway
BoD - burden of disease
CanCHEC - Canadian Census Health and Environment Cohort
CHMS - Canadian Health Measures Survey
CMP - Chemicals Management Plan
CPTP - Canadian Partnership for Tomorrow Project
EATS - Estrogen receptor, Androgen receptor, Thyroid hormone pathways, and Steroidogenesis
ECCC - Environment and Climate Change Canada
EDC - endocrine-disrupting compound
HC - Health Canada
ICES - Institute for Clinical Evaluative Sciences
IDRC - International Development Research Centre
INSPQ - Institut national de santé publique du Québec
KE - key event
MIE - molecular-initiating event
MIREC - Maternal-Infant Research on Environmental Chemicals study
NAMs - new approach methodologies
NWRC - National Wildlife Research Centre
OECD - Organisation for Economic Co-operation and Development
PoC - probability of causation
SC - science committee
U.S. NIEHS - United States National Institute of Environmental Health Sciences
References
Aguirre A. A., Beasley V. R., Augspurger T., et al. 2016. One Health-transdisciplinary opportunities for SETAC leadership in integrating and improving the health of people, animals, and the environment.Environ Toxicol Chem, 35(10): 2383-2391. doi:10.1002/etc.3557.
American Veterinarian Medical Association. 2008. One Health Initiative Task Force: Final Report. July 15, 2008. One Heath: A New Professional Imperative. Available at: www.avma.org/KB/Resources/Reports/Documents/onehealth_final.pdf.
[AOP-Wiki]. Collaborative Adverse Outcome Pathway Wiki. Available at: https://aopwiki.org/.
Basu N., Lanphear B. P. 2019. The challenge of pollution and health in Canada. Canadian J Public Health, 110(2): 159-164. Available at: https://link.springer.com/article/10.17269%2Fs41997-019-00175-7.
Birnbaum L. S. 2018. Moving NIEHS forward for the next five years. Environ Health Perspect, 126(9):91001. Available at: https://doi.org/10.1289/EHP4356.
Bonnell M. A., Zidek A., Griffiths A., et al. 2018. Fate and exposure modeling in regulatory chemical evaluation: New directions from retrospection. Environ Sci Proc Impacts, 20(1): 20-31. doi:10.1039/C7EM00510E.
[CanCHEC] Canadian Research Data Centre Network. CanCHEC (Canadian Census Health and Environment Cohort). Available at: https://crdcn.org/datasets/canchec-canadian-census-health-and-environment-cohort.
[CHMS] Government of Canada, Statistics Canada. 2019. Canadian Health Measures Survey (CHMS). Available at: www.statcan.gc.ca/eng/survey/household/5071.
[CMPSC 2015] Chemicals Management Plan Science Committee. 2015. "Meeting Record June 2-3, 2015-Chemicals Management Plan Science Committee. Available at: www.canada.ca/en/health-canada/services/chemical-substances/chemicals-management-plan/science-committee/meeting-records-reports/meeting-record-june-2-3-2015.html.
[CMPSC 2017] Chemicals Management Plan Science Committee. 2017. Committee Report-November 16-17, 2016. Available at: www.canada.ca/en/health-canada/services/chemical-substances/chemicals-management-plan/science-committee/meeting-records-reports/committee-report-november-16-17-2016.html.
[CMPSC 2018] Chemicals Management Plan Science Committee. 2018.
Committee Report. Meeting #7, July 18-19, 2018. Advancing Consideration of Endocrine-Disrupting Chemicals under the Canadian Environmental Protection Act, 1999. In press.
Cowan-Ellsberry C. E., McLachlan M. S., Arnot J. A., et al. 2009. Modeling exposure to persistent chemicals in hazard and risk assessment. Integr Environ Assess Manage, 5(4): 662-679. Available at: https://doi.org/10.1897/IEAM_2008-084.1.
[CPTP] Canadian Partnership for Tomorrow Project. Available at: www.partnershipfortomorrow.ca/.
Dummer T. J. B., Awadalla P., Boileau C., et al.; with the CPTP Regional Cohort Consortium. 2018. The Canadian Partnership for Tomorrow Project: A pan-Canadian platform for research on chronic disease prevention. Canadian Med Assoc J, 190 (23): E710-E717. Available at: https://doi.org/10.1503/cmaj.170292.
[ECCC] Government of Canada, Environment and Climate Change Canada. 2017. Great Lakes Surveillance Program. Available at: www.ec.gc.ca/scitech/default.asp?lang=en&n=3F61CB56-.
Guyatt, G. H., Oxman, A. D., Schünemann, H. J., et al. 2011. GRADE guidelines: A new series of articles in the Journal of Clinical Epidemiology. J Clinical Epidemiol 64: 380-382. Available at: www.jclinepi.com/article/S0895-4356(10)00329-X/fulltext.
Gwinn M.R., Axelrad D.A., Bahadori T., Bussard D., Cascio W. E., Deener K., Thomas R. S., Kavlock R. J., Burke T. A., 2017. Chemical Risk Assessment: Traditional vs Public Health Perspectives. AJPH, 107(7): 1032-1039. doi: 10.2105/AJPH.2017.303771.
[HC ECCC CMP SC] Health Canada Environment and Climate Change Canada Chemicals Management Plan Science Committee. 2018. Combined government discussion paper and science committee report on informed substitution. Available at: www.canada.ca/content/dam/hc-sc/documents/services/chemical-substances/chemicals-management-plan/science-committee/meeting-records-reports/cmp-eng.pdf.
[IDRC] International Development Research Centre. 2010. Ecohealth: Improving the health of people and the environment. Available at: http://www.idrc.ca/en/research-in-action/ecohealth-improving-health-people-and-environment.
[IOM]. Institute of Medicine. 2011. National Academies of Science. Finding What Works in Health Care: Standards for Systematic Reviews. Available at: www.nationalacademies.org/hmd/~/media/Files/Report%20Files/2011/Finding-What-Works-in-Health-Care-Standards-for-Systematic-Reviews/Standards%20for%20Systematic%20Review%202010%20Insert.pdf.
Landrigan P. J., Fuller R., Acosta, N. J. R., et al. 2018. The Lancet Commission on pollution and health. The Lancet Commissions, 391: 462-512.
MIREC. Maternal-Infant Research on Environmental Chemicals. Available at: www.mirec-canada.ca/en/.
[NTP] National Toxicology Program. 2019. U.S. Department of Health and Human Services. OHAT Systematic Review. Available at: https://ntp.niehs.nih.gov/pubhealth/hat/review/index-2.html.
[NHANES] Centers for Disease Control and Prevention, National Center for Health Statistics. 2019. National Health and Nutrition Examination Survey. Available at: www.cdc.gov/nchs/nhanes/index.htm.
[NWRC Specimen Bank, ECCC] Environment and Climate Change Canada. 2010. Laboratories and research support: National Wildlife Specimen Bank. Available at: www.canada.ca/en/environment-climate-change/services/wildlife-research-landscape-science/laboratories-support/national-wildlife-specimen-bank.html.
Parliament of Canada. 2017. Standing Committee on Environment and Sustainable Development. Healthy Environment, Healthy Canadians, Healthy Economy: Strengthening the Canadian Environmental Protection Act, 1999. 42ndParl., 1st sess. Available at: www.ourcommons.ca/Content/Committee/421/ENVI/Reports/RP9037962/envirp08/envirp08-e.pdf.
[OHC] One Health Commission. 2019. Available at: www.onehealthcommission.org/.
Pearl, J. 1999. Probabilities of causation: Three counterfactual interpretations and their identification. Synthese, 121: 93-149. Available at: https://ftp.cs.ucla.edu/pub/stat_ser/r260-reprint.pdf.
Planetary Health. 2019. Safeguarding both human health and the natural systems that underpin it. The Rockefeller Foundation. Available at: www.rockefellerfoundation.org/our-work/initiatives/planetary-health/.
Ring C. L., Arnot J. A., Bennett D. H., et al. 2019. Consensus modeling of median chemical intake for the U.S. population based on predictions of exposure pathways. Environ Sci Technol, 53(2): 719-732. doi: 10.1021/acs.est.8b04056.
Robins J., Greenland S., 1989. The probability of causation under a stochastic model for individual risk. Biometrics, 45: 1125-1138. Available at: www.ncbi.nlm.nih.gov/pubmed/2611320.
Tollefsen, K. E., Scholz, S., Cronin, M. T., Edwards, S. W., de Knecht, J., Crofton, K., Garcia-Reyero N., Hartung T., Worth A., Patlewicz G. 2014. "Applying Adverse Outcome Pathways (AOPs) to Support Integrated Approaches to Testing and Assessment (IATA)." Regulatory Toxicol Pharmacol, 70(3): 629-640. Available at: http://www.sciencedirect.com/science/article/pii/S0273230014002141.
[U.S. EPA] United States Environmental Protection Agency. 2014. EJSCREEN: Environmental justice screening and mapping tool. Available at: www.epa.gov/ejscreen.
[U.S. EPA] United States Environmental Protection Agency. 2015. EnviroAtlas. Available at: https://www.epa.gov/enviroatlas
Woodruff, T. J., Sutton, P. 2014. The navigation guide systematic review methodology: A rigorous and transparent method for translating environmental health science into better health outcomes. Environ Health Perspect, 122(10): 1007-1014. Available at: https://ehp.niehs.nih.gov/doi/pdf/10.1289/ehp.1307175.
[WHO] World Health Organization. 2019. International Programme on Chemical Safety. Available at: www.who.int/ipcs/methods/harmonization/areas/exposure/en/.
Appendix
Ongoing Canadian cohort studies (examples)
| Canadian cohort study | Number of participants |
|---|---|
| CPTPTable Footnote 1 (Canadian Partnership for Tomorrow Project) | >320,000 |
| CLSA (Canadian Longitudinal Study on Aging) | ~50,000 |
| CHILD (Canadian Healthy Infant Longitudinal Development Study) | 3,455 |
| MIREC (Maternal-Infant Research on Environmental Chemicals) | 2,001 |
|
|
These are examples of major research platforms that are active in Canada and that consist of prospective (longitudinal) designs with informed consent that permits linkage to stored medical and health system databases. Study sizes at present indicate that the Canadian Partnership for Tomorrow Project is Canada's largest prospective cohort study with a biorepository and linkage to provincial health systems data.
Examples of alternative platforms
(for example, repeated, cross-sectional surveys)
| Alternative platform | Number of participants |
|---|---|
| CHMS (Canadian Health Measures Survey): 5 surveys | ~29,000 |
| CCHS (Canadian Community Health Survey): survey every other year | ~65,000 |
Footnotes
- Footnote 1
-
Abbreviations in Figure 2: GRADE: Grades of Recommendation, Assessment, Development, and Evaluation (a series of guidelines for systemic review in epidemiology; Guyatt et al., 2011); IARC, International Agency for Research on Cancer; IPCC, Intergovernmental Panel on Climate Change; NASEM, U.S. National Academies of Sciences, Engineering, and Medicine (IOM, 2011); Nav Guide, Navigation Guide Systematic Review Methodology (Woodruff and Sutton, 2014); OHAT, U.S. National Toxicology Program's Office of Health Assessment and Translation (NTP, 2019).