Conference to Develop a Federal Framework on Lyme Disease May 15-17, 2016: Conference Summary Report

Download the alternative format
(PDF format, 1.36 MB, 30 pages)
Organization: Public Health Agency of Canada
Published: 2016-10-20
This Report was prepared for information purposes only. It aims to provide an overview of the key messages expressed by presenters and participants who attended the conference, the majority being patients who shared their personal experiences (see Figure 1). The key messages and ideas summarized in this report are not intended to indicate a consensus of opinion or agreement across patient groups and the medical and scientific communities on these topics. The opinions and views expressed at this Conference are those of the presenters and participants and do not necessarily reflect the opinions and views of the Government of Canada.
1. Introduction
As mandated by the Federal Framework on Lyme Disease Act, the Public Health Agency of Canada, on behalf of the Minister of Health, held a conference in May of 2016 in Ottawa, Canada. Participants included patients, representatives of provincial and federal health ministries, researchers, patient groups, health care professionals or other interested Canadians. Conference attendees participated both on-site and through an online interface.
Figure 1: Summary of total attendance (in person and online)
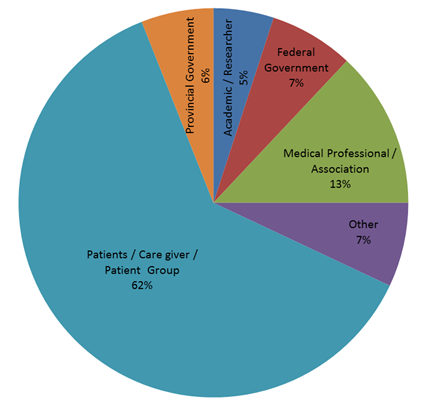
Figure 1: Summary of total attendance (in person and online) - Text Description
This figure shows how many participants attended the Conference to Develop a Federal Framework on Lyme Disease. Participants included patients, their care givers and patient groups, provincial and federal government representatives, academics/researchers, members of the medical community, as well as other interested Canadians.
Provincial Government
- 6 % of the participants were representatives from a provincial government
Academic / Researcher
- 5% of the participants were academics or researchers
Federal Government
- 7% of the participants were from the Federal Government
Medical Professional / Association
- 13% of the participants were medical professionals or members of a medical association
Patients / Caregiver / Patient group
- 62% of participants were Lyme disease patients, their caregivers or representatives of a Lyme disease patient group
Other
- 7% were interested Canadians
The three-day conference included a Public Forum on Day 1 that provided the opportunity for patients, caregivers and health professionals to share their experiences. Opening remarks at the Public Forum were provided by Dr. Gregory Taylor, Chief Public Health Officer for the Public Health Agency of Canada, Mr. Jim Wilson, President of the Canadian Lyme Disease Foundation and Dr. Daniel Gregson, Past President of the Association of Medical Microbiology and Infectious Disease Canada.
Day 2 of the conference began with opening remarks by the Honourable Jane Philpott, Minister of Health and Green Party leader and Member of Parliament Elizabeth May (whose private member's Bill C-442 lead to the Act). During Days 2 and 3, domestic and international Lyme disease experts provided information and insight on current understanding, concerns and research related to Lyme disease surveillance, treatment, prevention, identification and management, as well as education and awareness. In breakout and plenary sessions during Days 2 and 3, participants had the opportunity to provide ideas for consideration in the development of the Federal Framework for Lyme Disease.
The conference focused on the three areas aligned with the Act:
- Medical Surveillance, including incidence rates and associated economic costs.
- Education and Awareness, including standardized education materials for use by Canadian public health providers and to increase national awareness.
- Guidelines and Best Practices for clinicians, data collectors and analysts, public health practitioners and policy-makers.
2. Public Forum
2.1 Tri-Chairs Opening Remarks
Dr. Gregory Taylor, Chief Public Health Officer, Public Health Agency of Canada, welcomed participants to the Public Forum portion of the conference. He noted that the Public Forum is an opportunity for those most directly affected to share their personal experiences with Lyme disease, and "these stories will shape and influence discussions during the conference." He indicated that the goal of the conference is to seek direction and guidance on improving existing efforts in surveillance, education and awareness, treatment guidelines and best practices, all of which are pillars in the approach to preventing and reducing the risk of Lyme disease for all Canadians. He also mentioned that there are unanswered questions about Lyme disease that require further research and analysis, and the stories told will provide valuable insight that will help determine how those questions should be answered. He said that this conference is one step in a much broader process of consultation that is essential for the framework's development. There have been opportunities to provide views prior to the conference, and as the framework develops there will be additional opportunities to provide feedback. His closing message was that the ultimate goal is to build a framework for action that contributes to a better understanding of Lyme disease so that fewer Canadians suffer from its effects.
Mr. Jim Wilson, President, Canadian Lyme Disease Foundation, extended his appreciation to Elizabeth May, MP, and all other members of Parliament and the Senate who brought the Federal Framework on Lyme Disease Act into law. He noted that it has been 27 years since the first Lyme disease patient group was formed in Canada. He said, "It has taken too long, but we are here now. The Public Forum and the conference are significant steps in moving forward." He proposed that Canada has no idea of how many people now or in the past decades have contracted Lyme disease due to flawed testing protocols, and that this conference is the beginning of transparent, patient engaged, ethical scientific discussion. He also stressed that policy on Lyme disease in Canada must be a made-in-Canada policy, not an imported policy.
Dr. Daniel Gregson, Past President, Association of Medical Microbiology and Infectious Disease Canada (AMMI), noted that his colleagues at AMMI are committed to ensuring that Canadians are protected as much as possible from infections and that physicians have the tools to properly diagnose and treat patients when they do get infected. He said that the scientific evidence that will be presented during the conference will help guide the federal government in forming policies for Lyme disease in Canada. He reinforced that the Public Forum, however, is about patient experiences. "We are here to listen to your stories. As we learned from HIV/AIDS, patient participation in research and clinical trials is crucial to making scientific progress and developing better treatments. We need your continuing involvement, and we thank you for sharing your stories with us."
2.2 Public Forum Key Messages
Over 500 participants from across Canada participated over the 3 days which began with 100 speakers at the Public Forum who shared their personal experiences either in person or online. Speakers included patients, their families and caregivers and health care professionals.
A number of common key messages emerged from the speakers' personal experiences:
- Canada's medical system has failed Lyme disease patients.
- There is a great deal of physical, mental and financial suffering as the result of Lyme disease.
- There is a general lack of awareness of Lyme disease and ticks within the medical community.
- Misdiagnosis is common. Lyme disease symptoms overlap with those of other complex chronic diseases, such as fibromyalgia, chronic fatigue and depression.
- Misdiagnosed Lyme disease and/or improper or inadequate treatment have ruined lives, families and careers.
- Many patients have been frustrated by the need to see multiple specialists rather than receiving a holistic approach to treatment of this chronic disease.
- Many patients feel disrespected and not listened to by the medical community - Lyme disease is stigmatized.
- Many patients have had to seek treatment out of Canada at great personal expense.
- Early detection is essential - the burden of the disease increases if not treated early and adequately.
- Current diagnostic tests are inadequate, leading to both false positive and false negative results.
- Lyme disease is under-reported - many more Canadians may be suffering from Lyme disease.
- Co-infection and multiple strains need to be acknowledged and tested for.
- Canadians and the medical community need to be more aware of Lyme disease prevention and symptoms.
3. Opening Remarks
The Honourable Jane Philpott, Minister of Health, welcomed participants to the conference, noting that attendees from across the country are participating in-person and online. She thanked fellow parliamentarian Elizabeth May for her tireless work and leadership in bringing the Federal Framework on Lyme Disease Act forward.
Minister Philpott said that Lyme disease is a serious illness that is spreading across Canada. The voices of patients, scientists, medical practitioners, policy makers and others will help ensure that the framework is guided by their needs and concerns. "There is no doubt that we need much more research to better guide diagnoses. We need better surveillance and we need more education and awareness to inform both the public and practitioners about this infectious disease."
She explained that, three years ago, the Public Health Agency of Canada implemented an action plan to address prevention, diagnosis and treatment of Lyme disease. In cooperation with the provinces and territories, Canadians received information to protect themselves. Health professionals have been told to be vigilant in diagnosing Lyme disease and reporting cases to the local health authorities. The Canadian Institutes for Health Research (CIHR) over the past five years has invested more than $2.8 million toward Lyme disease research projects.
In closing, Minister Philpott noted that this conference is an essential and important step in continuing to build on this work. "All of the information, feedback, ideas, and opinions that are generated at this conference will be fully considered as this federal framework for Lyme disease is developed. Ultimately, the outcomes of this conference are going to help protect the health and well-being of all Canadians."
Ms. Elizabeth May, MP, Green Party of Canada, thanked all those who shared their deeply moving stories about their suffering during the Public Forum portion of the conference. She also thanked all the parliamentarians who helped drive the Act forward, calling Lyme disease "the ultimate non-partisan issue." She noted that the goal of the Act is a Federal Framework on Lyme disease with a focus on the patient. She encouraged all participants and stakeholders to work together: patients, Health Canada, the Public Health Agency of Canada, provincial and territorial departments of health, medical doctors, research agencies, and the official accrediting bodies for doctors.
She noted her personal goals for the framework: "We must put an end to the status quo in which sick Canadians are forced to go to the US for treatment at their own expense, losing homes, savings and pensions. Our Canadian health care system has to take care of everyone. No one with Lyme disease should be stigmatized anymore." She acknowledged that Lyme disease presents enormous challenges. But, "I have faith in the framework development process and am confident that it will remain transparent and inclusive."
Mr. Jim Wilson, President, Canadian Lyme Disease Foundation, thanked Minister Philpott, Elizabeth May and all others who helped bring Bill C-442 into law. He noted that this conference is the starting point for moving forward. He remarked that the number of Canadians affected by Lyme disease needs to be identified, along with an accounting of the burden of the disease. Better diagnosis and treatment protocols are needed. Canada must stop imposing US policy and guidelines on Canadians. He said, "Canada is a large country and we have at least as many Lyme strains as elsewhere in the world."
Mr. Wilson emphasized that patients and their experts must be seen as equal partners in all aspects of the framework development process, including guideline writing for diagnostics, treatment, prevention, surveillance and research. He said, "With patients as equal partners at the table, we can make a difference for Canadians. The time for action on Lyme disease is finally here."
Dr. Daniel Gregson, Past President, Association of Medical Microbiology and Infectious Diseases Canada (AMMI), stated that he had been "moved by the people at the Public Forum who shared their stories of their physical, financial and psychological suffering." He noted that he represents AMMI members, who include approximately 500 specialists and scientists involved with research, diagnostics, treatment and care of patients who have been affected by infections of all types. AMMI members offer expert advice to patients, other members of the medical community and the government on how to manage and control infections that affect the health of Canadians. Association members evaluate new diagnostic tests to ensure the diagnoses patients receive for all infectious processes are the best available based on the best evidence. Members introduce new treatments, deal with emerging infections such as Ebola, and manage chronic diseases from infections, such as Hepatitis C and HIV.
Dr. Gregson noted that this conference brings together patients, delegates and experts to help the Public Health Agency of Canada develop a Federal Framework on Lyme disease. He said, "It is a very important meeting for finding common ground. AMMI members see this conference as a major opportunity for the development of an evidence- and science-based framework to deal with this important health issue."
4. Overview of Lyme Disease
Presentations
A Brief History of Lyme Disease and a Review of the U.S. Clinical Trials
Brian Fallon, MD MPH, Professor of Psychiatry, Director, Lyme and Tick-borne Disease Research Center, Columbia University Medical Center - Director, Center for the Study of Neuroinflammatory Disorders and Biobehavioral Medicine, New York State Psychiatric Institute
Lyme Disease from the Perspective of a General Physician in Active Clinical Practice
Ralph Hawkins, MD LLM FRCPC, Clinical Associate Professor of Medicine, University of Calgary, South Health Campus Hospital Site Lead for Division of General Internal Medicine
Laboratory Diagnostics of Lyme Disease - Past, Present, Future
Raymond J. Dattwyler, MD, Professor of Microbiology/Immunology and Medicine, School of Medicine, New York Medical College
Lyme Disease Diagnosed by Alternative Methods and Similar Syndromes: Research Approaches to Take us Forward
David Patrick, MD, FRCPC MHSc, Professor and Director, School of Population and Public Health, University of British Columbia
Presenters' Key Messages Summary
The following suggestions were brought forward by the presenters for consideration in the development of the Federal Framework for Lyme disease.
Research
- Well-structured research projects are needed to better understand Lyme disease (leading to a better case definition).
- Research needs to look at the full array of Borrelia and other pathogens in ticks.
Surveillance
- Joint collaboration between the US and Canada should be expanded (increased data sharing among researchers, scientific meetings and conferences).
- Better surveillance is needed.
- Include Lyme disease question on the Canadian Community Health Survey.
- Create a national Lyme disease biobank (collect and store samples from patients).
Treatment
- Antibiotic use:
- Need for more clinical trials to support the notion that repeated antibiotic treatment is helpful.
- Antibiotic treatment must be weighed against risks (resistance, reactions, and changes in the human biome).
5. Focus on Surveillance
Presentations
Lyme Disease Surveillance in Canada
Nick H. Ogden, BVSc DPhil, Senior Research Scientist, National Microbiology Laboratory, Public Health Agency of Canada
The Ecological, Epidemiological and Molecular Aspects of Borrelia Burgdorferi Sensu Lato: Consequence of Diversity, Distribution and Genome Variations of Lyme Borreliosis Spirochetes
Nataliia Rudenko, PhD, Biology Centre, Institute of Parasitology of Czech Academy of Sciences, Ceske Budejovice, Czech Republic
Comparing Results and Predictions of Different Surveillance Approaches for Lyme Borreliosis: Canine Seroprevalence in New Brunswick as a Case Study
Vett Lloyd, PhD, Professor, Department of Biology, Mount Allison University
Ontario's Lyme Disease Surveillance Program
Curtis Russell, PhD, Senior Program Specialist, Enteric, Zoonotic and Vector-borne Diseases Unit, Communicable Diseases, Emergency Preparedness and Response, Public Health Ontario
Surveillance Key Messages Summary
The following key messages were expressed by participants and presenters:
Surveillance Scope
- Ongoing, coordinated surveillance efforts are needed in all provinces to track blacklegged ticks and other tick species. Worldwide, there are about 10 different tick species capable of transmitting Lyme disease. The movement of migratory birds (i.e. movement of ticks from the US to Canada) is also to be considered.
- Surveillance must track the various species of Borrelia.
- There is a need to track Lyme disease infections that occurred outside of Canada; especially those infected prior to Lyme disease becoming a reportable disease in 2009.
- A One Health approach (human health and animal health) that includes the involvement of veterinarians is important.
- Information/data must be precise enough to allow patients, communities and health care practitioners to make informed choices.
- Regional and community-level data is essential. For example, information on the prevalence of ticks at a provincial level is misleading and "almost meaningless."
- The BC Centre for Disease Control has a model that may be useful for displaying PHAC data by region.
- More resources are needed to provide the suggested improvements to the scope of surveillance.
Surveillance Best Practices
- Look to other jurisdictions for best practices.
- Risks maps must be continuously updated.
- There is understandably a lag between data collection and production of a risk map, but the shorter the span, the better and more useful the surveillance map will be.
- Integrated data, from both passive and active sources, are important.
Collaboration and Information Sharing
- The surveillance system is driven by the collaboration of the provinces/territories and federal government. This highlights the need for ongoing, systematic surveillance efforts in all provinces and territories.
- The multiple levels of health care authorities (federal, provincial, local) must ensure information sharing.
Community Involvement
- Community involvement in surveillance should be leveraged:
- Community involvement increases awareness of the disease.
- Care must be taken to ensure the safety of collectors.
- Precise and common collection methodologies must be used to ensure consistency of data.
Dissemination and Use of Surveillance Data
- The limitations of surveillance data need to be recognized:
- Identification of "high risk/endemic areas" gives impression that other areas are risk/tick free.
- A disclaimer should be included on surveillance maps.
- Some of the relevance and implications of surveillance data, as well as their utility, can be lost or altered as messages move from researcher to health care practitioners to informed public and general public.
- Some of the risk maps are being used inappropriately, for example to prevent testing and diagnosis or to deny insurance coverage.
6. Focus on Guidelines and Best Practices
Presentations
Evidence-based, Patient-centered Guidelines for the Diagnosis and Treatment of Lyme Disease
Elizabeth Maloney, MD, President, Partnership for Healing and Health, Minnesota
Treatment of Lyme Disease
William Bowie, MD, Professor Division of Infectious Diseases, Faculty of Medicine, University of British Columbia
Current State of Lyme Diagnostics in Canada
Todd F. Hatchette, MD FRCPC, Chief, Division of Microbiology, Department of Pathology and Laboratory Medicine, Nova Scotia Health Authority Professor, Department of Pathology, Dalhousie University
Challenges of Post-Treatment Lyme Disease Syndrome (PTLDS): Will Persister Drugs Help to Cure PTLDS?
Ying Zhang, MD, PhD, Department of Molecular Microbiology and Immunology, Bloomberg School of Public Health, Johns Hopkins University
Guidelines and Best Practices Key Messages Summary
The following key messages were raised by participants and presenters:
Lyme Disease
- The bacterium that causes Lyme disease, Borrelia burgdorferi, is a complex organism that changes over time. This makes studying it, working with it, and healing it very difficult.
- Co-infections that cause Lyme-like symptoms are not well understood, leading to further confusion.
- Other tick-borne infections also need to be tested for.
- Other modes of infection other than ticks need to be fully explored, as well as multiple tick species.
- Even though there are similarities, there are many differences among cases.
- There are different needs at different stages of the disease, with severe issues in the later stages.
Patients
- Patients want to be heard and included: they understand the risks and want to work with doctors on the best solutions for them.
- There is a sense of urgency: relief is needed now.
- The disease causes excessive strain and emotional impact:
- Patients need validation and emotional support.
- The burden of cost to patients needs to be acknowledged.
- Lyme disease needs to be recognized as a disability.
- Most patients are willing to help with research, participate in clinical trials, provide blood samples - do whatever it takes to fix the current situation.
- A holistic approach is needed that includes alternative practitioners.
- Progress is happening too slowly for those living with Lyme disease. Interim solutions for improved diagnostics and testing are needed while the science advances.
- Physicians who treat Lyme disease patients outside the existing treatment guidelines should be protected from sanctions from their licensing organization.
Researchers
- Researchers are constrained because their science must be evidence based.
- Qualitative data (patient experience) is not considered enough. There is an abundance of information that should be used to benefit Lyme disease research.
- Must avoid doing research in silos.
- There is promising research being done. For example, in vitro experiments are showing that use of a combination of drugs can be effective.
- More research is needed on diagnostics and testing, not just treatment.
Medical Community
- Doctors are constrained by the current guidelines and, in many cases, lack awareness of the disease.
- The guidelines are not flexible enough.
- The guidelines are more effective in the early stages of the disease but not at later stages.
- The two-tier testing approach under the guidelines is only effective in some cases; diagnostics are not 100% accurate.
- There is a need for more Lyme-literate doctors (LLDs), able to effectively diagnose and treat the disease.
- Need to consider patient's symptoms more than serology results.
- The issues of antibiotic resistance and the need for responsible stewardship cannot be dismissed, as well as the risks to patients of long-term antibiotic use.
7. Focus on Education and Awareness
Presentations
Creation of Standardized Educational Material for Public Health Care Providers Regarding the Prevention, Identification, Treatment and Management of Lyme Disease: Educational Gaps
Liz Zubek, BSc Med MD CCFP FCFP, Family Physician, Shepherd's Hill Medical Clinic, Maple Ridge, BC
Alison C. Bested, BSc MD FRCPC, Associate Professor, Department of Medicine, University of British Columbia
Lyme Disease in KFLA: Health Care Professional Communication Strategy
Kieran Moore, MD CCFP(EM) FCFP MPH DTM&H FRCP(C), Associate Medical Officer of Health, Program Director of Public Health and Preventative Medicine, Professor of Emergency and Family Medicine, Queen's University
Tick-borne Disease Educational Materials and Methods from the Centers for Disease
Control and Prevention
Christina Nelson, MD MPH FAAP, Medical Epidemiologist, Division of Vector-borne Diseases at the Centers for Disease Control and Prevention, Atlanta, GA
Education and Awareness Key Messages Summary
The following key messages were raised by participants and presenters:
Current Situation
- There is a patchwork of poor, misleading and incorrect information and conflicting messages.
- Public awareness is low.
- Lyme disease and Lyme disease patients are stigmatized.
- Focus is too often only on acute infection.
- Physicians are not being educated about Lyme disease; they lack needed information (for example, diagnostic criteria, rate of presentation of "classic" rash, which tests to order, etc.).
- Many physicians don't know if they are in an endemic/high-risk area.
Education and Awareness within the Medical Community
- Educate physicians about Lyme disease in medical schools.
- Ensure physicians have easily accessible, up-to-date information to make a clinical diagnosis.
- Take a holistic approach: focus on all health care professionals (paramedics, pharmacists, nurses, etc.) and alternative medicine practitioners.
- To reach physicians and health professionals, use newsletters, guides, reference manuals, exhibits at well-attended conferences, and webinars that provide credits.
- Innovative ideas for reaching the medical community included:
- Create a "Lyme Corps" - use medical students and residents who are Lyme savvy to get the message out.
- Create a Lyme app (with information on diagnosing, treatment, prevention tips, etc.).
- Messaging aimed at the medical community:
- Surveillance activities and results need to be communicated to physicians (e.g., tick prevalence in their area).
- Clinical diagnosis, testing and treatment guidelines and best practices.
- Information on both tick-borne infections and co-infections.
- Chronic aspects - not only acute.
- Good ethics and communication to eliminate the stigma.
- Some examples of recommended messages: be alert to the potential for Lyme disease, don't rely on or wait for the test results, treatment must be individual and evolve with the disease, use combination therapy, don't give up on your patient.
Education and Awareness for the Public
- Persistent and consistent information/education is needed.
- A cross-country campaign using multiple mass and other media (TV, radio, internet, social media, signs on trails, parks, campgrounds, recreation facilities).
- Need to focus on prevention (avoiding tick bites), how to remove ticks, how transmission occurs, what Lyme disease does to your health, symptoms and associated risks, and what to do if you think you are infected.
- Use age-appropriate approaches (e.g., comics for children) and culturally appropriate messaging and images to reflect the Canadian mosaic.
Monitoring and Evaluation
- For both the medical community and the public, education and awareness efforts must be evaluated to determine if behaviours are changing.
8. Advice and Ideas for Consideration for the Development of a Federal Framework
8.1 Focus on Surveillance
What might success look like?
- A systematic Lyme disease surveillance approach is in place in all provinces and territories.
- The surveillance system provides timely, accessible information about risk and how the risk evolves over time.
- The system has shifted from a static surveillance approach to one that is predictive.
- Researchers representing patients have been involved in the development of surveillance protocols and methodology.
Ideas for Consideration
Lyme Disease Surveillance System
- Clear and common surveillance objectives for use by all relevant provincial/territorial and federal government departments need to be developed.
- The system requires transparent and effective governance.
- A better case definition is needed (separate objectives for diagnosis and surveillance).
- Baseline levels and sentinel sites need to be established.
- New technologies need to be leveraged, and best practices applied.
- The system should facilitate data sharing and use across federal and provincial lines, with data and collection standards for compatibility.
- Coordination, funding and resources are available to carry out appropriate surveillance.
- Engage veterinarians: testing of ticks at no charge, tracking of tick areas. (Some veterinarians require education on Lyme disease and its vectors.)
- Tick testing capacity needs to be increased.
- Provide information to the public about surveillance activities (where surveillance is done, what is being tracked (i.e., what tick species, what strains of Borrelia, other bacteria, etc.)).
- Ticks don't recognize borders: surveillance information changes constantly - we have to accept that Lyme disease is here and blacklegged ticks and other ticks carry the disease. No surveillance system can keep up.
Risk Communication
- "Low risk" does not mean "no risk."
- Risk communication goal: to drive behaviour change and support informed decision-making.
- Need to define how risk information maps are drawn; a topographical approach is more realistic.
- Risk information maps are misleading - ticks are mobile.
- Need standards for signage and identification of targeted locations for signage.
- To lessen misuse of risk maps, add a disclaimer that they are for research purposes.
- Use a notification system similar to the Amber Alert program (announcements on television and radio to convey information on high-risk areas).
Research
- Develop a surveillance research agenda, with appropriate funding.
- Leverage existing and prior research.
- Short-term research project: collate/integrate existing risk maps.
- Research question: Are certain people more susceptible to tick bites and Lyme disease, for instance due to their HLA haplotype?
- Study chronic Lyme disease patients, for example how Lyme disease affects different areas of the body.
Surveillance of Lyme Disease in Humans
- Need for closer/better patient monitoring, recognizing limits imposed by privacy needs.
- Physician reporting needs improvement.
- All Borrelia strains and all co-infections to be monitored.
- Include patients with a positive test result from an outside lab: create a "count me in" program.
- Use patient tick bite history to help identify areas for tick surveillance.
- Integrate both passive surveillance (reporting of positive test results) and active surveillance (areas where clusters of people are being tested, regardless of test results, areas where ticks are prevalent).
8.2 Focus on Guidelines and Best Practices
What might success look like?
- There is patient liaison and advocacy.
- Patient experience is characterized by respect, transparency and inclusion.
- There is trust in the medical system.
- There is timely, accurate and effective diagnosis and treatment.
- Doctors are free to diagnose and treat based on clinical observation as well as test results.
- Research includes qualitative and quantitative evidence.
- There is recognition and understanding of the evolution of the disease in its acute and chronic aspects.
- Lyme disease is recognized and acknowledged by employers, insurers and provincial health care plans.
- There is adequate funding for research.
- Clinical practice guidelines are regularly reviewed and updated.
- There is a holistic approach to patient care that includes traditional, alternative and social science practitioners.
Ideas for Consideration
Immediate/Short-term Actions
- Action is needed now to relieve suffering and to begin longer-term research and other activities, such as surveillance and education.
- Build a business case (cost analysis):
- Determine costs associated with treating later stages of Lyme disease (costs to the health care system, out-of-pocket costs to patients, costs related to lost productivity, etc.).
- Determine how much money is saved by early and appropriate treatment and use cost savings for Lyme disease research, treatment and patient support.
- Create a multidisciplinary centre(s) of excellence and innovation for Lyme disease research and treatment:
- Would enable direct exposure for researchers to patients.
- Involve the Canadian Medical Association, medical colleges, and provincial governments.
- Create databases of tick areas, symptoms, treatments and their outcomes, patient experience, etc.
- Enable sharing of best practices across Canada among the whole spectrum of health care practitioners.
- Review the guidelines and best practices of other countries.
- Create a list of physicians treating Lyme disease.
Patients
- Revise the Health Care Act to improve access to care and prevent out-of-pocket expenses.
- Reimburse patients/families for past and ongoing expenses not covered by their provincial health plans, such as travel for treatment, supplements, complementary care providers, diagnostic tests, homecare and equipment.
- Provide compassionate loans/grants for people in immediate need.
- Create an online help centre/forum for Lyme disease patients or those suspecting they may have been infected.
- Create a database of patient experience.
- Hold regular annual conferences to engage patients, provide support, review latest research and treatment options, and build networks.
- Have a part-time disability category to accommodate those who can manage some work.
- Disability to be based on functionality not diagnosis.
- Provide retraining, alternative jobs. Hire Lyme patients for Lyme disease education.
Diagnosis, Testing and Treatment
- Promote diagnosis based only on clinical symptoms.
- Enable ethical, open and transparent access to test results for patients:
- Allow more thorough reporting on serology - not just positive or negative. Patients should be able to see the "fine print."
- Release banding data from all past Western blot tests for Lyme disease.
- Automatic testing of spouses of Lyme disease patients.
- Lift restrictions on prescribing antibiotics for Lyme disease.
- Enable antibiotics to be prescribed as a precaution when someone suspects a tick bite.
Medical Community
- Need to create Lyme-literate doctors.
- Establish specialists in vector-borne diseases.
- Impose an immediate five-year moratorium on penalties/professional consequences for physicians diagnosing and treating Lyme disease.
- Impose some form of penalty on any medical college that persists in prosecuting physicians who treat Lyme disease patients.
- Reinstate doctors who lost their medical licenses due to treating Lyme disease.
- Coroners to be required to submit tissue samples, especially of patients with diseases that for which Lyme disease is frequently misdiagnosed (e.g., Parkinson's, Alzheimer's), to a biobank.
Holistic Approach
- Patients and doctors work together.
- Facilitate and encourage traditional and naturopathic practitioners to work together with openness and respect.
- A holistic approach to mental wellness is important (suicide prevention, treatment for long-term trauma). Need to recognize the psychological and psychiatric dimensions - not psychosomatic but somatic-psychic (physical symptoms causing psychological problems).
- Recognize the importance of nutrition and health of the personal and community microbiome as part of Lyme disease treatment:
- Registered holistic nutritionists and other holistic health care providers to be considered part of the integrative health care team, with their services covered by provincial health care plans.
- If services are not covered by provincial health care plans, ensure they are tax deductible to the patient.
Research
- Funding is needed for Lyme disease research.
- Need to look at research that has been done in other countries (e.g., U.S. research on agents that attack the biofilm).
- Research topics/areas:
- Properly define the disease, including strains, co-infections and modes of infection.
- Human-to-human transmission: congenital, breast milk, sexual, blood supply, organ donation.
- Presence of Borrelia burgdorferi, Lyme disease strains or spirochetes in patients with other diagnoses such as Parkinson's and Alzheimer's.
- Other vectors and birds have implication for surveillance.
- Vaccine development.
- Environmentally protective eradication/control of ticks and other vectors.
- Better products to protect against ticks that are safe for humans, pets, and the environment.
Development, Monitoring and Evaluation of the Federal Framework for Lyme Disease
- Do not develop the Federal Framework in isolation - look at the practices, guidelines and policies of other countries.
- Refer to the U.S. National Academies Institute of Medicine's standards for the development of trustworthy clinical practice guidelines when developing the framework.
- A process of evaluation and accountability needs to be established to monitor change.
8.3 Focus on Education and Awareness
What might success look like?
- There is one source of factual information on Lyme disease for Canada.
- Information and tools are readily available to all.
- All education and awareness materials reflect all Canadians and are available in many languages to meet community needs.
- Media coverage of Lyme disease is factual.
- Children are fully educated on Lyme disease.
- The entire medical community is fully educated and aware of Lyme disease and all its aspects and issues.
- Physicians know what to do and where to get information.
- Every family doctor knows how to treat tick bites, Lyme disease symptoms (acute and chronic) and transmission risk factors (vaginal/semen secretions, etc.).
- Specialists are knowledgeable about Lyme disease.
- Multidisciplinary teams, including naturopathic doctors, work together with openness and respect.
- Awareness campaigns are year-round (not only seasonal).
- The stigma of Lyme disease has been erased through education and awareness.
- Education and awareness efforts are monitored and evaluated for use of recommendations, information materials, and behaviour change.
Ideas for Consideration
General Public
- Accurate and current information is provided in pamphlets and posters available in medical offices, pharmacies, veterinarian clinics, etc.
- Need to know the risks (including that Lyme disease can be fatal) and how to prevent infection, what to do if you suspect infection.
- Need a broad description of Lyme disease and its co-infections.
- Need photos of ticks and rashes (all not just bull's eye, also state that there may not be any rash).
- Promote awareness through a national Lyme Disease Awareness Day.
- Use all forms of media to get the message out.
- Use a celebrity champion that the general public would relate and listen to.
- Target employers and workplaces to generate understanding for co-workers who have Lyme disease.
- A patient-centered conference is held annually to transfer new knowledge and provide support.
Children
- Goal is to reduce or eliminate contraction, but without creating fear (use Red Cross swimming education as a model).
- Reach children through schools and daycare centres and through those who work with children (coaches, club leaders, etc.).
- Use age appropriate messaging and delivery vehicles (role play, comics, etc.).
- Create campaigns similar to anti-bullying; "lime green t-shirt day" at schools.
- Tick removal kits should be provided to all schools and school boards should have a tick/Lyme policy.
- Suggestions for such a policy included a protocol for the school to seek immediate medical attention for a child that has been bitten and formal notification to parents to seek medical attention if there is suspected exposure.
Recreation and Outdoor Audiences
- Signs at parks, trails, golf courses and campgrounds: notification of tick prevalence, identification of ticks, tick removal, bite prevention, action to take if bitten.
- Tick removal kits for summer camps, sports coaches, club leaders, etc.
- Advertisements/advertorials in outdoor magazines (hunting, camping, RVing, hiking) and local and regional papers.
- Posters and pamphlets at sporting goods/outdoor stores.
- Need to reach outdoor workers (hydro, military, camps, landscapers, tree planters, etc.).
- Need to reach weekend gardeners and cottagers.
Medical Community
- Need to provide "Lyme basics" (how to remove a tick, visual signs of different rashes, symptoms, antibiotic guidelines for acute and chronic) to the whole spectrum of health care practitioners, including general practitioners, specialists, alternative practitioners, nurses, medical students and pharmacists.
- Need to reach and engage veterinarians.
- Survey health care practitioners to determine their current knowledge and practices on Lyme disease (will provide baseline data for future evaluation of progress/change).
- Deliver information through medical journals.
- Ensure key information sources, such as UpToDate, have current information (e.g., the International Lyme and Associated Diseases Society (ILADS) guidelines or those of the National Guideline Clearing House). It was noted, however, that UpToDate will only publish what it considers to be evidence-based information.
- Ongoing education is done through compulsory continuing education requirements; various levels are available, leading to accreditation as a Lyme literate practitioner.
- Database of Lyme-literate doctors for referring patients.
- Promote how to become a Lyme-literate doctor.
Public Health Agencies
- At the federal, provincial/territorial, regional and community levels: need mechanisms to ensure information is correct and delivered to appropriate parties.
- Existing Lyme disease information on public health websites needs to be reviewed for accuracy: false information is just as bad as no information.
- Public health agencies to acknowledge and communicate that all provinces have Lyme disease.
- Provide public access to tick testing and information on where to take ticks for testing.
- Establish time-based billing codes for complex cases to ensure patients are given adequate attention.
- Mandatory training on Lyme disease basics in medical schools and mandatory yearly updating of training for licensed practitioners. Pay physicians to attend accredited training for physicians (e.g., BC Practice Support Program).
- Hire summer students for public education.
- Yearly conference to raise awareness within public health agencies, including information on blood and organ donation by Lyme disease patients.
Media
- Need all the correct information, from ticks to treatment to transmission.
- Consider a big media campaign (e.g., Bell mental health awareness; promote the "Take a Bite out of Lyme" social media challenge).
- Use creativity and humour to get attention.
Parliamentarians and Members of Legislative Assemblies
- Promotion of a Canada-wide strategy for ministers of health that would include factual information on Lyme disease, co-infections, prevention, awareness and surveillance.
- Create provincial laws to protect medical professionals who treat Lyme disease.
- Promote funding for research.
Pest Control Industry and Regulators
- Engage the national and provincial associations and regulators (e.g., Pest Management Regulatory Agency of Canada) on tick control and bite prevention.
- The industry also needs to be better educated about Lyme disease.
- Need to improve consumer information on pest control and bite prevention products, (e.g., length of effectiveness).
9. Tri-chair Closing Remarks
Dr. Daniel Gregson, Past President, Association of Medical Microbiology and Infectious Disease Canada thanked participants for sharing their stories and offering many good ideas. He said, "Many of you are suffering, and that is difficult for me as a doctor." He noted that he has concerns about some of the physician/patient interactions and will be taking those stories back to his colleagues.
Dr. Gregson observed that there are a lot of unanswered questions about Lyme disease. When the next conference on Lyme disease is convened, there will hopefully be fewer unanswered questions and changes will have been made. To do that, a number of things need to happen. He suggested that improvements are needed in how people with Lyme disease are classified and how patient experience is captured. Data needs to better reflect the number of Canadians affected whether they have had positive Lyme tests in Canada or not, as well as those who had Lyme disease and got better and the outcomes of treatment. He noted that observational studies are needed along with a better understanding of the complexity of multiple symptoms and manifestations of the illness and a better process than sending patients to multiple specialists.
In closing, he said, "My hope as we move forward with the Federal Framework is that we can identify the issues that we can all agree on, and that we can communicate those issues to the public and the government. With agreement we can have forward motion; if we are divided we can't."
Mr. Jim Wilson, President, Canadian Lyme Disease Foundation, noted that much has been said over the short period of the conference. He observed that the global shift that happened for HIV/AIDS is poised to happen now for Lyme disease, noting that, "The momentum and opportunity are here. The stage is set for the cooperation that will make the difference that will find the research funding and create multiple centres of excellence." He noted that opposing opinions are not to be avoided: science, to become evidence, requires open and transparent debate by all stakeholders.
Mr. Wilson observed that what is most important is the involvement of patients and their experts as equal partners in all matters of Lyme disease policy. He noted that the Canadian Institutes of Health Research clearly states that patient involvement at health policy design and planning stages yields the best outcomes and that this must be the foundation from this point forward and the legacy of this conference. He emphasized that, "We [patients] are equal partners."
Dr. Gregory Taylor, Chief Public Health Officer, Public Health Agency of Canada, said that he has experienced "an incredible learning experience" over the course of the conference. He thanked participants for sharing their moving stories openly and honestly and for taking the risk to do so. He said, "I have seen the pain and the anger in many people. But I have seen a shift to hope. People are here to make things better." He observed that the goal of the Public Health Agency of Canada is also to make things better for people. "If we are not helping individual Canadians, if we are not making a difference in their lives, then we are not doing our job."
Dr. Taylor observed that Canadians are natural collaborators. Some of the common messages of the conference include:
- We need better surveillance.
- We need better education and more awareness.
- We need to prevent this disease from affecting more Canadians.
- And we need improved treatment guidance and best practices.
He noted that while the Act states that the Public Health Agency of Canada is to produce a Federal Framework on Lyme Disease, for it to be effective it must be a "roadmap for action", and that this is the Agency's intent.
In closing, he noted that the ongoing engagement of participants and all Canadians is important to the framework development process. As the Federal Framework is developed, there will be opportunities for review and input. He said that the conference "is not the end. We need to and will engage on an ongoing basis."
Page details
- Date modified: