A Primer to Reduce Substance Use Stigma in the Canadian Health System

Download the alternative format
(PDF format, 2.06 MB, 30 pages)
Organization: Public Health Agency of Canada
Date Published: January 2020
Related links
Table of contents
- Introduction
- How to use this primer
- The need to reduce substance use stigma in the health system
- The role of key players across the health system
- Promising system-level interventions
- Conclusion
- Related links
- Annex 1: Substance Use Stigma Pathways to Health Outcomes Model
- References
Introduction
Stigma is increasingly recognized as a pressing public health problem. The Chief Public Health Officer’s (CPHO) 2019 annual report on addressing stigma illustrates how the range of stigma drivers and practices ultimately contribute to social and health inequities (Public Health Agency of Canada, 2019). The report also draws attention to the large increase in opioid-related deaths in Canada since 2000, and how substance use stigma in the health system represents a barrier to good health and wellbeing among people who use substances. These issues have galvanized public health leaders across the country.
The purpose of this primer is to mobilize health professionals and other health system stakeholders (e.g., hospital administrators, regional health authorities, governments, etc.) to take action to reduce substance use stigma across the health system by applying evidence-informed interventions. While the CPHO’s report examines numerous stigmas (e.g., such as those associated with racism, homophobia, sexism, etc.), as well as their intersections, and describes stigma interventions at various levels (i.e., population, institutional, interpersonal and individual levels), this resource focuses on systemic stigma related to substance use and promising practices for interventions within the health system.
This primer centres on 3 key messages:
- Substance use stigma is prevalent throughout the health system and contributes to poorer quality of care and negative health outcomes.
- Creating a stigma-free health system will require collaborative action and sustained commitment of key players across the health system.
- Efforts to reduce substance use stigma within the health system must also acknowledge and address intersecting stigmas, including through initiatives not traditionally labelled as “anti-stigma interventions”.
How to use this primer
This primer can be used in 3 ways. First, it can support health professionals and other stakeholders to advocate within their professional communities for a collective response to reduce substance use stigma in the health system. This primer helps to illustrate why substance use stigma is a problem for all health professionals, regardless of discipline, and how stigma adversely impacts the quality of clinical practice and the health and wellbeing of patients.
Second, this primer can be used to demonstrate the need for system-level changes within the health system to mitigate substance use stigma. This primer illustrates how stigma is embedded in many aspects and practices of the health system, often in subtle ways. While education and training are common strategies for addressing stigma, they are limited in their effectiveness when not supported by broader changes to the ways institutions are set up and how they serve people who use substances.
Thirdly, the primer can direct health system leaders and decision makers to evidence-informed interventions that can help to reduce substance use stigma within the health system. The primer provides an overview of tangible areas for action and uses evidence to describe how they can help prevent or mitigate stigma. However, this primer is not an implementation guide. Stakeholders should consult and use other resources (e.g., toolkits, training courses, etc.), as necessary, for specific guidance and tools on how to implement intervention approaches.
The need to reduce substance use stigma in the health system
Key message 1: Substance use stigma is prevalent throughout the health system and contributes to poorer quality of care and negative health outcomes.
Substance use is a cross-cutting theme across the Canadian health system, and for various reasons. Most Canadians use substances (medical and/or non-medical) in one form or another and in diverse contexts. Many Canadians access care settings for treatment or management of health conditions related to substance use, including substance use disorders and infectious and chronic diseases for which substance use is a risk factor. Patients’ substance use often is discussed during routine medical history taking within various health settings. Further, health professionals commonly prescribe substances to their patients to treat and manage pain and other health conditions. Despite these realities, substance use stigma is salient within the health system (see Text box 1 ).
Text box 1: Substance use stigma in the health system
Substance use stigma can be reflected within policies, practices, training and work culture in the health system. Examples include institutional policies that require patients to be abstinent from substances before they can receive certain health services, services that don’t reflect the diverse needs of people who use substances, and the limited formal training opportunities for students and practicing health professionals on substance-related topics. These are examples of systemic stigma.
Systemic stigma reinforces and is reinforced by public stigma. Key drivers of public stigma include the widespread views that substance use and its related harms are the result of individual choice, weakness, immorality or a lack of willpower. This stigma can be expressed through various stigma practices like avoidance, blame and judgment of people who use substances, including by health professionals.
Stigma can also be internalized among people who use substances, leading to shame, decreased self-efficacy and social avoidance, which are manifestations of self-stigma. Self-stigma can affect both patients and health professionals who use substances.
Impacts on patient-provider interactions and accessibility and quality of services
At the provider/patient interface, expressions of substance use stigma have a direct, negative impact on communication and relationships, and create barriers that reduce access to timely, appropriate and compassionate care for individuals who use substances. On the provider’s end, barriers to care can arise from implicit or explicit bias against people who use substances. Implicit bias can manifest as health professionals spending less time with patients who use substances or other subtle avoidance behaviours (e.g., reduced eye contact, closed off body language, etc.), while explicit bias is evident in deliberately coarse interactions (e.g., rude behaviour reflecting prejudice, being treated unfairly as a security threat, etc.) with patients who use substances and refusal to offer medical interventions to these patients for other illnesses or pain management. These barriers reflect systemic and/or public stigma.
On the patient’s end, barriers may include feelings of unease, distrust and fear, which may manifest as defensive or evasive behaviour or a lack of disclosure about their substance use or other relevant details of their medical history. These barriers reflect anticipated or self-stigma (e.g., feeling ashamed, inferior, responsible for their disorder, etc.). For example, research demonstrates that many individuals prescribed long-term opioid therapy for management of chronic pain report not disclosing their personal concerns about their opioid use to health professionals, fearing changes in their treatment (particularly, discontinuation) and being labeled an “addict” (Larance et al., 2018). In scenarios such as these, stigma may interfere with early identification, prevention and/or appropriate management of potential opioid use disorder among those who use medically-indicated prescription opioids.
Impacts on patient outcomes
Substance use stigma within the health system contributes to poorer outcomes among people who use substances. For example, Canadian research highlights how opioid-related stigma within the health system negatively impacts patients’ quality of life, leads to avoidance of care settings and increases the likelihood of risky self-medication (e.g., through use of diverted opioids) (Voon et al., 2018). Among people with substance use disorders, self-stigma is associated with greater physical, social, intrapersonal, and interpersonal problems related to their condition (Kulesza et al., 2017). Although we count on the health system to provide care and support health and well-being, substance use stigma within health settings can perpetuate various harms linked to substance use.
Impact on social and health inequities
Beyond these negative impacts on individual-level outcomes, stigma contributes to population-level social and health inequities. Some populations (e.g., Indigenous peoples, people experiencing homelessness, poverty and/or unemployment, etc.) are disproportionately affected by substance-related harms (Feng et al., 2013; Buchanan, 2006). These harms (and others) are exacerbated when systems are not set up to meet the needs of these groups, as reflected in varied system-level barriers to services and opportunity (e.g., restricted hours of operation, failure to account for linguistic or literacy differences, requirements of proof of address, cost, etc.). These barriers are expressions of systemic stigma that extend beyond substance use stigma, and limit the accessibility of housing, employment, social support networks, income and social and health services. As a result, systemic stigma can create and widen inequities among people who use substances and members of other groups that have experienced stigma and marginalization. The dynamic links between social and health inequities, stigma and substance use are shown in Figure 1.
Figure 1 - Text description
The figure is composed of 3 elements: “social and health inequities,” “stigma” and “substance use,” which are aligned from left to right respectively. Each element is interconnected to the other by arrows, illustrating the linkages between them.
For a detailed illustration of how substance use stigma undermines the health of individuals and contributes to health inequities, see the Stigma Pathways to Health Outcomes Model (Annex 1).
The role of key players across the health system
Key message 2: Creating a stigma-free health system will require collaborative action and sustained commitment of key players across the health system.
Commitment and collaboration across the health system is required to meaningfully reduce substance use stigma at the system-level. This will require close evaluation of and efforts to improve the rules, policies, procedures, cultural norms and values of health-related institutions and how they impact people who use substances. Collectively, professionals working within the health system have many levers to help reduce systemic substance use stigma, including the design of training and professional development programs, decisions on which programs and services are funded, policies that govern how health settings operate, the time service providers can spend with patients, how facilities are designed and decorated, the content and tone of communication materials published by health organizations, service providers’ everyday practice and interactions with patients.
Promising system-level interventions
Key message 3: Efforts to reduce substance use stigma within the health system must also acknowledge and address intersecting stigmas, including through initiatives not traditionally labelled as “anti-stigma interventions”.
This section details promising intervention approaches for reducing substance use stigma, their supporting evidence and illustrations of what these approaches “look like” in the health system. These intervention approaches fall into 3 broad categories:
- Efforts to explicitly address social and health inequities among people who use substances and other populations who experience stigma and marginalization;
- Efforts specifically designed to reduce stigma that have been applied to mitigate a wide range of stigmas, including those related to mental health, weight, suicide, etc.; and
- Efforts to enhance care and supports for people who use substances.
Social and health inequities
1. Equity-oriented interventions
Background: “Equity-oriented interventions” seek to make institutions and systems more accessible, compassionate and safer for individuals to better meet their diverse needs and help prevent harms. Given the many ties between substance use stigma and social and health inequities (described above), equity-oriented interventions represent a relevant approach to mitigating the numerous forms of stigma experienced by people who use substances. There are specific examples of equity-oriented interventions that are proven to be effective at reducing stigma, including: trauma- and violence-informed (TVI) policy, programs and practice, cultural safety, and harm reduction oriented services and supports. It is important to note that these interventions could be used independently or in combination (see Text box 2).
i. Trauma-and violence-informed policy, programs and practice
Background: Trauma begins with one or more event/experience that overwhelms a person’s normal coping mechanism. Traumatic experiences can be both interpersonal and/or systemic and are unique to individuals, including events such as natural disasters, witnessing acts of violence and/or structural policies (such as the Indian Act and/or the Residential Schooling System). Traumatic experiences are unique to individuals, and what is traumatic to one person may not be to another person. There are physical and psychological reactions in response to trauma; both reflect normal reactions to abnormal, extreme and/or unjust situations (Covington, 2008). TVI approaches acknowledge that experiences of trauma and violence - both interpersonal and systemic - are common and can have a lasting impact on development and behaviour.
Intervention objectives: TVI approaches aim to prevent harms and avoid re-traumatizing individuals by creating safe spaces, fostering compassion and collaboration, and building on strengths to support coping and resilience.
Impacts on substance use stigma: TVI approaches can mitigate substance use-related stigma by shifting the thinking from “what’s wrong with you?” to “what happened to you?” This strategy is beneficial in reducing the blaming and shaming of individuals for their situation and focuses on providing safe, and compassionate care that may improve patient outcomes (Knaak et al., 2019).
Examples of intervention approach:
- Anybody can cultivate a TVI setting, and implementing these approaches does not require being a specialized trauma worker. TVI practices can be applied universally in service settings (i.e., as opposed to strictly in cases where trauma is suspected). Examples of TVI approaches include recognizing potentially re-traumatizing services or practices in health services settings that may be triggering and/or cause panic or fear among patients that may have experienced trauma (e.g., the use of mouth props in dental offices, restraints and seclusion in in-patient psychiatric settings, being in a physically vulnerable position during an examination, etc.), and efforts to provide alternatives where possible.
- TVI approaches also could involve relatively simple strategies like patient/client-centred communication (e.g., asking what can be done to make the patient/client more comfortable, using the “tell-show-do” strategy to explain to a patient/client what a procedure will entail to potentially alleviate their anxiety of the unknown, etc.) and efforts to make the built environment less austere, more calming and inviting (Raja et al., 2014; Muskett, 2014).
ii. Cultural safety
Background: Cultural safety was catalyzed as a model of care by Indigenous health professionals in New Zealand. This model is especially important for patients who identify as Indigenous but is recognized as relevant for other priority populations, including transgendered individuals and members of racialized communities (Kellet & Fitton, 2017; Bailey et al., 2017). Culturally safe models of care reflect a recognition of and efforts to counter systemic racism and the power imbalances that exist within health systems along the lines of cultural differences.Culturally safe care is a practice of care that aims to address forms of discrimination, such as inequitable power relations, and interpersonal and institutionalized racism against non-Western cultures (e.g., Indigenous) that has had lingering effects because of historical and current health inequities (Browne et al., 2015).
Intervention objectives: The goal of cultural safety is to ensure that all individuals who interact with a service provider or institution are able to do so in a way that makes them feel respected and physically, emotionally, socially and spiritually safe, regardless of their expressed or assumed culture or identities.
Impacts on substance use stigma: When health professionals embrace a culturally safe model of care, they can work towards validating a person’s cultural identity, create mutual trust and empathy, and counter power imbalances. Understanding how culture intersects with the other aspects of ones life (including substance use, mental health diagnosis) can inform the creation of a unique care plan that will help increase patient outcomes and wellness.
Examples of intervention approach:
- Examples of specific cultural safety interventions include, hiring and supporting Indigenous health professionals, education for health professionals on cultural humility (i.e., health professionals becoming aware of their own biases and awareness of power imbalance surrounding culture (Muise, 2019)), efforts to support the legitimacy and effectiveness of traditional healing (which may include prayer, smudging, energy work, healing circles, etc.), and providing clients appropriate resources and referrals to access these cultural services.
iii. Accessible harm reduction-oriented services and supports
See the substance use section for more information on harm reduction-oriented services and supports.
Text box 2: Comprehensive Equity-Oriented Intervention
The Research to Equip Primary Healthcare for Equity (EQUIP) is a system-level intervention that encompasses multiple strategies to ensure equitable care, including trauma- and violence-informed care, cultural safety and harm reduction (as outlined above) (Ford-Gilboe et al., 2018). By doing so, EQUIP has created an intervention designed to build the capacity of primary health care clinics to adopt and sustain equity-oriented care (Browne et al., 2015). The intervention utilizes education modules to enhance staff knowledge of equity-informed care at an organizational level, and capacity to shift policies and practices.
2. Initiatives to prevent and manage trauma-related stress and burnout among health professionals
Background: Health professionals are at risk of facing trauma-related stress and/or burnout when working in environments that subject them to high-stress situations. Trauma-related stress (i.e., vicarious trauma, secondary traumatic stress and compassion fatigue) is related specifically to working with patients who share traumatic experiences, and burnout is a more general phenomenon that may occur within any health service setting as a result of chronic stress (long shifts, insufficient staff). These types of stress are related but distinct that can co-occur, and both adversely impact the health and well-being of health professionals and diminish quality of care.
Intervention objectives: Initiatives to prevent and manage trauma-related stress and burnout among health professionals aim to support health providers in different capacities to ensure the health provider is able to provide the best care to their patients/client’s.
Impacts on substance use stigma: The links between trauma-related stress, burnout and stigma are particularly salient in the context of the current opioid crisis. Recent Canadian research illustrates how burnout, compassion fatigue and vicarious trauma among first responders and health professionals and with patients/clients experiencing substance-related harms contribute to emotional and behavioural distancing, disconnection and apathy, all of which have negative consequences for care (Knaak et al., 2019). Research identifies other manifestations of trauma-related stress and burnout, including anger and irritability, reduced ability to feel sympathy and empathy, a diminished sense of enjoyment or satisfaction with work, increased absenteeism and an impaired ability to make decisions and care for patients (Mathieu, 2007; Patel et al., 2019). Trauma-related stress and burnout interventions can better enable health professionals to provide compassionate support that meets the demands of their job.
Examples of intervention approach:
- Ongoing system inadequacies, including resource limitations, poor working conditions (e.g., long shifts), understaffing and inadequate access to treatment and care for patients, can heighten health professionals’ risk of trauma-related stress and burnout (Knaak et al., 2019). The risks and impacts of trauma-related stress and burnout can be mitigated through a variety of organizational-level interventions. These include those focused on workplace mental health and resiliency, training in TVI care and practice (supporting service providers in managing their vicarious trauma and other stressful experiences) and organizational supports and culture that support health professionals’ mental health and well-being (Knaak et al., 2019).
- A recent meta-analysis found that structural/organizational-level interventions within health settings (e.g., shortened resident shifts, various changes to clinical work processes, etc.) are far less common, though equally as effective, as those at the individual-level (e.g., self-care training, mindfulness training, etc.), and suggested both approaches are needed (West et al., 2016). It is important that direct service providers and educators understand the risk factors and symptoms associated with trauma-related stress and burnout in order to identify, prevent, and/or minimize their effects. This information can be infused into curricula for trainees and included as a part of training for health professionals already working in the field.
3. Availability of comprehensive wrap-around services
Background: Wrap-around service is a comprehensive model of care that aims to address the client’s unique and individual care needs as a whole. This model of care quite literally “wraps around” the client to address many aspects of their life to ensure they have the best care for their unique needs. While core services directly related to diagnosis and treatment of substance use-related health conditions are critical (withdrawal management services, psychotherapy), wrap-around services allow for several other intersections (childcare, child and family services, nutrition programming, housing assistance, cultural services, supports for women experiencing intimate partner violence, HIV testing and primary medical services) of the patient/client’s needs to be met.
Intervention objectives: Wrap-around services seek to manage patient’s co-occurring problems as a whole and enhance well-being, patient outcomes and empowerment concurrently.
Impacts on substance use stigma: Decades of research evidence demonstrate that access to wrap-around services for those seeking care for their substance use-related problems is associated with better patient/client engagement and retention and better, more sustained patient/client outcomes (Marsh, Smith, & Bruni, 2011; McLellan et al., 1998; Marsh, D’Auno, & Smith, 2000). A recent study identified that health services settings are often more responsive to certain clients’ unique needs for wrap-around services (e.g., women, adolescents, survivors of trauma, etc.) than others (e.g. those referred from the criminal justice system) (Paino, Aletraris, & Roman, 2016). This research underscores the importance of health systems being sensitive and responsive to the wrap-around needs of all clients/patients, particularly the most marginalized. Given the barriers that people who use substances encounter related to care, wrap-around services offer a holistic method of care that can help reduce self stigma in patients by alleviating feelings of being “just an addict” and encouraging self-reflection as a whole person.
Examples of intervention approach:
- Wrap-around services can be implemented at various facilities (i.e., primary health care, addiction treatment centres, walk-in clinics) to provide clients/patients a “one-stop shop” for their care. These facilities would offer support for many intersections of one’s life, including medical care, mental health, childcare, family, educational, vocational, housing/transportation, financial and legal issues. The specific services a patient/client receives or is connected to are reflective of the individual’s particular needs and context.
Stigma
1. Contact-based interventions
Background: Contact-based programming involves interventions where people with lived or living experience of a stigmatizing condition (such as substance use disorder or mental illness diagnosis) interact with the public or specific groups (such as health professionals) who do not have experience with the stigmatizing condition to describe their challenges and stories of success (National Academies of Sciences, Engineering, and Medicine, 2016) as a means to de-stigmatize their conditions (Shera, 1996).
Intervention objectives: Contact-based interventions aim to facilitate positive interaction and connection between people with and without stigmatized identities to overcome negative attitudes engendered by lack of contact and/or opportunity to view people as unique, whole beings. These interventions enable people with lived/living experience to interact with the public or specific groups and share their challenges and stories of success via in-person or digital means.
Impacts on substance use stigma: Meta-analytic evidence demonstrates contact-based interventions’ effectiveness at reducing self and public stigma related to mental illness, as well as its superiority to traditional education efforts (Corrigan et al., 2012). Though these approaches have not yet been broadly applied to address substance use stigma, their application in the mental health context serves as a relevant reference point (Stuart, 2019), and the available evidence points to contact-based approaches as a promising practice to counter stigma related to substance use (National Academies of Sciences, Engineering, and Medicine, 2016).
Examples of intervention approach:
- Contact-based approaches are most often applied via public education efforts, and as a means of addressing social stigma. An example is the Mental Health Commission of Canada’s (MHCC) Opening Minds anti-stigma initiative, which is aimed at changing negative attitudes and behaviours Canadians may have towards people with mental illnesses. MHCC leveraged contact-based programming via educational sessions where people with experience living with mental illnesses share their personal stories of how they were living in recovery from their mental illness or are managing their mental illnesses (Stuart et al., 2014). This intervention has demonstrated favourable outcomes across a number of populations, including youth, workers, media and health professionals (Stuart et al., 2014).
- Contact-based interventions can also be subtly imbedded in institutional processes, such as through inclusion of people with lived/living experience in policy/program planning and evaluation, curricula for health professional trainees and peer support services (see below).
2. Peer support services
Background: Peer support services involve including people with lived/living experience of a stigmatized condition (e.g., substance use disorder, mental illness, homelessness) as part of a larger health service provisions team. Peer support services aim to provide self-efficacy, improved engagement with social supports, healthy coping skills and reduce self-stigma (Tracy & Wallace, 2016; Reif et al., 2014; Morgenstern et al., 1997; Greer et al., 2016). Peer support workers can also offer a unique perspective of firsthand experience to patients that may enhance treatment, reduce self and structural stigma by allowing people with lived/living experience a voice in policies and procedures surrounding their well-being, and increase self-efficacy (Reif et al., 2014; Tracy & Wallace, 2016).
Intervention objectives: Peer support workers aim to provide support to patients who use substances by offering empathy, suggesting coping strategies and challenging self-stigma and other stigmas related to belonging to a marginalized population (Bassuk et al., 2016; Krawczyk et al., 2018).
Impacts on substance use stigma: Peer support services incorporate contact-based interventions into day-to-day practice. Peer supporters draw from their experiential knowledge (and oftentimes, formal training) to provide non-clinical support to assist others in initiating and maintaining recovery and in enhancing the quality of personal and family life. Peer support services benefit those seeking services for substance use-related issues and those acting in a peer role. These services are associated with significant improvements in a range of substance use and recovery outcomes (e.g., related to re-hospitalization, housing stability, treatment completion, etc.) among patients with substance use disorders (Bassuk et al, 2016). For the peer supporter, the role can offer personal growth (e.g., in terms of enhanced self-esteem, ability to manage their own condition, sense of empowerment and hope) and professional growth (e.g., by enhancing job skills and professional/social networks) (Solomon, 2004).
Example of peer support services:
- In the United States, Veterans Affairs (VA) is working to integrate peer support services within their case management team as a part of their strategy to address stigma towards people with mental illnesses. The results have been positive, with a slight increase in patient activation; and peer support workers have also developed strong relationships with veterans and assisted with case management duties (Chinman et al., 2015).
3. Use of non-stigmatizing language and depictions of substance use/people who use substances
Background: There are many stigmatizing substance use-related terms and expressions, including those that describe people who use substances (e.g., “drug abuser”, “addict”, “junkie”, etc.). This type of language implies that substance use and related harms solely reflect a personal choice, moral failing and a defining characteristic of an individual. Use of stigmatizing language and images can drive negative implicit or explicit prejudice among the general population (Kelly, Saitz, & Wakeman, 2016), as well as health professionals, influencing their perceptions of patients’ culpability and need for treatment (Kelly & Westerhoff, 2010; Kelly, Dow, & Westerhoff, 2010).
Intervention objectives: Using non-stigmatizing language and depictions of substance use/people who use substances aims to combat stigma by viewing the individual as a person first and not solely defined by the fact that they use substances.
Impacts on substance use stigma: Research identifies that health professionals’ language around substance use-related health conditions (e.g., FASD, substance use disorders, etc.) tends to be deficit- versus strength-based. Language that emphasizes possibility (versus tragedy) within the context of a diagnosed substance use-related condition can increase individuals’ agency and hope (Choate & Badry, 2019). Deliberate use of non-stigmatizing language and images, both in interactions with patients and through web and print publications in health and social settings can prevent or mitigate these prejudices and may help create conditions that make people who use substances feel safe, respected and cared for when seeking services.
Example of intervention approach:
- Recently, the Canadian Centre on Substance Use and Addiction (CCSA) and the Canadian Public Health Association (CPHA) published language resources to help the public reduce their use of stigmatizing language. The Public Health Agency of Canada (PHAC) has also recently published a resource for health professionals to communicate about substance use in compassionate, safe and non-stigmatizing ways. Each of these resources includes a list of stigmatizing language to avoid, an explanation of why the language is stigmatizing and a list of alternative non-stigmatizing language to use (Canadian Centre on Substance Use and Addiction, 2019; Canadian Public Health Association, 2019; Public Health Agency of Canada, 2019).
Refer to our related links for these language resources.
4. Education initiatives
Background: Education initiatives are a common strategy to mitigate stigma since they can reach a wide audience (e.g., through mass media campaigns), as well as deliver targeted, localized messages to specific groups (e.g., health professionals, law enforcement personnel, social service providers, those working in communications/media, employers, landlords, etc.) (National Academies of Sciences, Engineering, and Medicine, 2016; Griffiths et al., 2014). There are numerous education initiatives that can be effective in alleviating stigma, including public service announcements, movies, podcasts and videos (Corrigan et al., 2012).
Intervention objectives: Education and awareness initiatives can mitigate stigma by including messages that correct misinformation and counter prejudices about people who belong to a stigmatized population.
Impacts on substance use stigma: There is mixed evidence for the effectiveness of education initiatives on reducing stigma (Corrigan et al., 2012), suggesting they be used as only one component of a more comprehensive effort to address stigma. These initiatives are most effective at countering stigma when they feature positive stories that emphasize hope and treatability and/or effective management of substance use-related health conditions (e.g., featuring individuals with substance use disorders “living their best life”) and do not include “scare tactics” with the goal of scaring people away from using substances (Choate & Badry, 2019; McGinty et al., 2015).
Example of intervention approach:
- The Association of Faculties of Medicine of Canada (AFMC) has created e-learning tools for undergraduate medical education students to educate them on numerous topics related to addiction. The resources include a primer (e-textbook), podcast series and virtual patients (Association of Faculties of Medicine of Canada, 2017).
- Similarly, the AFMC conducted an environmental scan across Canada to review the curricula regarding opioid prescribing and/or pain management. The scan resulted in a robust source of best practices and education information for opioid prescribing and/or pain management that will be disseminated and shared on the AFMC website (Association of Faculties of Medicine of Canada, 2017a).
5. Policy/practice changes to reduce stigma
Background: Systemic stigma is embedded in various parts of the health system, including policies and practices and built environment characteristics. Structural changes can be made to health systems to expand opportunities and spaces for patients’ health and well-being (Blankenship et al., 2000). Structural changes can also include efforts to discourage the use of stigma as a tool to encourage behaviour change or prevent substance use-related behaviours. Indeed, public health practice and messaging that leverage stigma in this way can increase negative social and health outcomes among people who use substances by encouraging non-disclosure of substance use, delays in seeking care and avoidance of care settings. The same is true of the prevailing beliefs that equate “recovery” with “abstinence” (i.e., which stigmatizes those with recurrent substance use and/or cannot abstain from substance use), rather than focusing on reducing harms and enhancing well-being. Health professionals are encouraged to empower their patients by sharing accurate and up-to-date information on potential substance-related harms in a non-judgmental manner and providing compassionate, contextualized patient/client-centred advice and support in decision-making (Zizzo & Racine, 2017).
Intervention objectives: Efforts to reduce stigma embedded within policies/practice aim to deliberately reflect and correct prevalent policies and practice as they pertain to people who use drugs.
Impacts on substance use stigma: Stigma reduction initiatives that focus on institutional change in policy or practice directly impact systemic stigma and reflect structural interventions. Structural interventions modify social, economic and political environments that, in turn, shape and constrain individual, community and societal social and health outcomes (Blankenship et al, 2000).
Example of intervention approach:
Structural interventions can be leveraged to ensure people who use substances are not subject to explicit/conscious bias and/or implicit/subconscious bias.
- Examples of explicit/conscious bias in practice include disqualification from accessing certain services, use of stigmatizing language in policy/practice, invalidating substance use as a medical condition, etc. Interventions designed to address explicit/conscious bias in health systems include education, contact and skill building among health professionals, as well as institutional-level changes to service availability, accessibility and delivery and the physical and social environment.
- Examples of implicit/subconscious bias in practice include health professionals deprioritizing the care of individuals who use substances in a busy waiting room, attributing health problems to substance use and not assessing other potential contributors, etc. Interventions designed to address implicit/subconscious bias in health systems include training related to perspective-taking (i.e., consciously assessing an interaction from a patient/client’s perspective) and individuation (i.e., consciously focusing on specific, known information about an individual rather than assumptions).
Substance use
1. Accessible harm reduction-oriented services and other supports
Background: Harm reduction-oriented services provide supports to patients that focus on reducing the harm(s) (e.g., Sexually Transmitted and Blood-borne Infections, overdoses) associated with substance use. Harm reduction services can include strategies on reducing or abstaining from substance use, even though these are not ends in themselves. Central to harm reduction is the importance of “meeting people where they are at”, and recognizing that many people are unable or unwilling to abstain from substance use for various reasons.
Intervention objectives: Harm reduction services aim to reduce the potential negative consequences and harms related to substance use, without requiring abstinence.
Impacts on substance use stigma: Fostering harm reduction-oriented services helps to mitigate the stigma widely associated with substance use. When health professionals are dedicated to working collaboratively with clients to reduce harms related with substance use instead of pushing abstinence, clients may feel less judged and criticized for their choices to use substances. There is clear evidence that harm reduction services and other supports prevents substance use-related harms and enhances the well-being of individuals who use substances. As specific examples, harm reduction efforts have averted thousands of opioid-related deaths in British Columbia (Irvine et al., 2019) and are associated with reduced use of alcohol among expectant parents who cannot abstain during pregnancy (Choate & Badry, 2019). Harm reduction-oriented health services increase opportunities to connect patients to a wide variety of supports and forms of care. For example, programs and services intended to reduce harms associated with alcohol use during pregnancy represent opportunities to engage expectant parents in medical care, nutritional support, mental health and parenting preparation (Choate & Badry, 2019). Conversely, services that exclusively focus on abstinence may marginalize expectant parents who are unable or unwilling to abstain from alcohol use and reduce the accessibility of these other supports.
Example of intervention approach:
- The mere availability of harm reduction supports in health systems is insufficient; health professionals must also acknowledge harm reduction as a legitimate public health goal and mitigate potential barriers to accessing these harm reduction services and supports for people who need them. Among these barriers is substance use stigma, which significantly undermines harm reduction efforts, even those that are well-designed (Tam, 2018).
- While supervised consumption sites, needle exchange programs, free naloxone kits, managed alcohol programs and education on lower-risk substance use are all examples of initiatives very explicitly aimed at reducing substance-related harms, harm reduction principles can be integrated into a wider range of services and supports in more subtle ways. For example, harm reduction extends to relatively simple initiatives that can mitigate alcohol-related harms, including enabling access to safe, supportive physical spaces and water and food for people who are inebriated.
2. Evidence-based training on substance use topics, including those related to treatment and recovery of individuals who use substances
Background: Research points to a significant training gap for most health professions on addiction, substance use disorders and other substance-related issues/co-morbidities (Klimas, 2015; McKee, 2017). This training gap contributes to a lack of understanding of substance use, which may foster prejudices about individuals who use substances and misconceptions about substance use disorder (i.e., that they are not legitimate medical conditions) and a lack of knowledge and skills for working with these patient populations, leading to suboptimal care (Ayu et al., 2015; van Boekel et al., 2015).
Health professionals may demonstrate unease or frustration when interacting with patients with concurrent disorders due to lack of training and knowledge on client’s needs (Staiger et al., 2011). These reactions may reflect concerns about “staying in one’s lane”, feeling like the care these patients need is beyond their expertise, as well as feeling like their usual care approach is “complicated” by the presence of the other condition(s). Concurrent conditions necessitate unique approaches to diagnosis, treatment and management compared to stand-alone conditions (e.g., due to symptoms of one condition masking or mimicking another), which is complicated by the existing silos between mental health and substance use within health systems (Ayu et al., 2013). Canadian data demonstrates how these silos in care can create unmet needs among those with concurrent conditions. A nationally-representative study identified that nearly 90% of those with concurrent mental health and substance use disorders reported having a need for mental health care (most often counseling), and that these individuals were significantly more likely to report that these needs were only partially, rather than fully, met (Sunderland & Findlay, 2013). Likewise, health professionals often lack training on the management of complex pain, which may impede their confidence and ability to appropriately prescribe, monitor and/or wean patients off opioids for treatment of chronic pain (Glowacki, 2015).
Intervention objectives: Training for health professionals on substance use topics, both among trainees and ongoing professional development for those already working in the field, aims to effectively reduce health professionals’ negative attitudes (stigma) towards patients who use substances and improve clinical skills for working with this population (Livingston, 2013; Ayu et al., 2015).
Impacts on substance use stigma: When health professionals are knowledgeable and have a deep understanding of substance use topics, they can work towards acknowledging the legitimacy of substance use as a medical condition and help combat substance use related stigma. Having a deeper understanding of substance use disorder (i.e., prognosis, range of service/care options), health providers can work to better support their patients instead of perpetuating harms.
Example of intervention approach:
- A recent study on barriers to care patients face when pursuing opioid tapering highlighted ways to overcome potential anxiety and uneasiness often associated with tapering (Kennedy et al., 2014). These mechanisms included training on empathizing with patients, working with patients to plan and prepare for the tapering, as well as supportive guidelines and institutional policies (Kennedy et al., 2014).
Conclusion
Substance use-related stigma is prevalent in the health system and both reflects and contributes to social and health inequities among individuals that use substances. Given the pervasiveness of stigma, comprehensive approaches that comprise multiple, complementary intervention efforts are needed to meaningfully and sustainably address this pressing public health problem. These efforts can include those that focus on enhancing equity and improving care and services for individuals who use substances, as well as those that counter stigma directly. Health professionals and other key actors in the health system are well-poised to prevent and mitigate substance use stigma through system-level changes to policy, programs, training, organizational culture and service provision.
Related links
Other resources in this series
- Reducing Substance Use Stigma in the Canadian Health System (one pager)
- Communicating About Substance Use in Compassionate, Safe and Non-Stigmatizing Ways: A Resource for Canadian Health Professional Organizations and their Membership
Related reading from the Government of Canada
- The Chief Public Health Officer’s Report on the State of Public Health in Canada 2019. Addressing Stigma: Towards a More Inclusive Health System
- Stigma around substance use
Related external reading
- Canadian Centre on Substance Use and Addiction
- Changing the Language of Addiction (fact sheet)
- When it Comes to Substance Use Disorders, Words Matter (infographic)
- Canadian Public Health Association: Sexually Transmitted and Blood-borne Infections and Related Stigma (resource series)
- EQUIP Health Care: Health Equity Toolkit for Health Care Providers and Institutions (toolkit)
- Mental Health Commission of Canada: Stigma and the Opioid Crisis (PDF, report)
Annex 1: Substance Use Stigma Pathways to Health Outcomes Model
The diagram below is an adaptation of the Stigma Pathways to Health Outcomes Model, which can be found in the CPHO Report on the State of Public Health in Canada 2019: Addressing Stigma – Towards an Inclusive Health System. The model above highlights examples of substance use stigma pathways. For a detailed model and references, please see the CPHO report.
The extent to which substance use is stigmatized varies by the particular substance and context of use. Much of the literature on substance use stigma focuses on substance use-related health conditions (e.g., substance use disorders) or use of substances in ways that might be harmful (e.g., drinking alcohol during pregnancy), though other contexts of substance use are also subject to stigma.
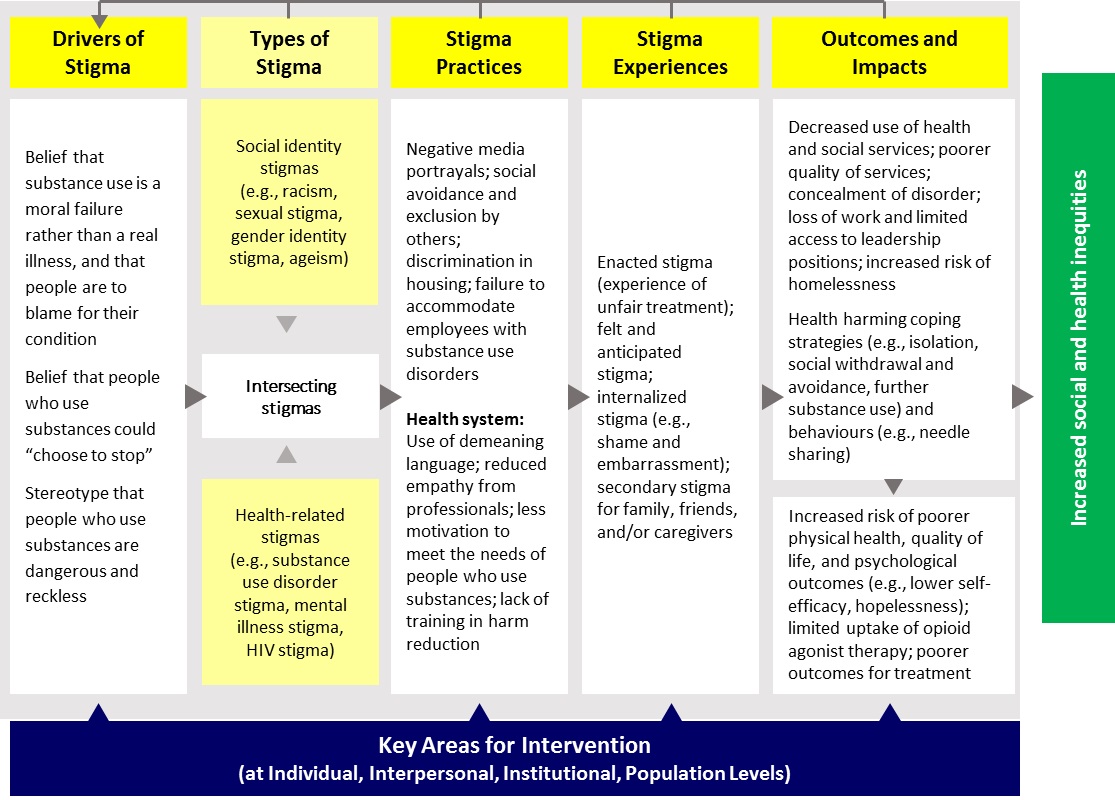
Figure 2 - Text description
This figure depicts an adaptation of the Stigma Pathways to Health Outcomes Model. The model works from left to right, describing the following components that flow into one another:
- drivers of stigma
- types of stigma
- stigma practices
- stigma experiences
- outcomes and impacts
Drivers of stigma can include:
- beliefs that substance use is a moral failure rather than an illness or people who use substances could “choose to stop”
- stereotypes (e.g., people who use substances are dangerous and reckless)
Drivers lead to different types of stigma that include those targeting:
- social identity stigmas (e.g., racism, sexual stigma, gender identity stigma, ageism)
- health-related stigmas (e.g., substance use disorder stigma, mental illness stigma, HIV stigma)
These can also be intersecting stigmas.
Stigma practices include:
- negative media portrayals
- social avoidance and exclusion by others
- discrimination in housing
- failure to accommodate employees with substance use disorders
There are stigma practices that are observed in the health care system:
- use of demeaning language
- reduced empathy from professionals
- less motivation to meet the needs of people who use substances
- lack of training in harm reduction
Stigma experiences include:
- enacted stigma (which is the experience of unfair treatment)
- felt and anticipated stigma
- internalized stigma (e.g., shame and embarrassment)
- secondary stigma experienced by family, friends or caregivers
Outcomes for affected populations include:
- decreased use of health and social services
- poorer quality of services
- concealment of the disorder
- loss of work and limited access to leadership positions
- increased risk of homelessness
- health harming coping strategies and behaviours (e.g., isolation, social withdrawal, avoidance and further substance use)
Ultimately these lead to:
- increased social and health inequities
- poorer physical health, quality of life, and psychological outcomes (e.g., lower self-efficacy, hopelessness)
- limited uptake of opioid agonist therapy
- poorer outcomes for treatment
Key areas for intervention would target:
- stigma drivers
- stigma practices
- stigma experiences
- outcomes for affected populations
These interventions would happen at the individual, interpersonal, institutional or population level.
References
Association of Faculties of Medicine of Canada (2017). Addiction E-Learning. AFMC Primer on Biopsychosocial Approach to Addiction. Available from https://afmc.ca/medical-education/addiction-e-learning/e-textbook-primer
Association of Faculties of Medicine of Canada (2017a). AFMC’s Response to The Opioid Crisis. Available from https://afmc.ca/publications/educationmatters/vol-1-issue-1-december-2017/afmc%E2%80%99s-response-opioid-crisis
Ayu, A. P., Schellekens, A. F., Iskandar, S., Pinxten, L., & De Jong, C. A. (2015). Effectiveness and organization of addiction medicine training across the globe. European addiction research, 21(5), 223-239.
Bailey, Z. D., Krieger, N., Agénor, M., Graves, J., Linos, N., & Bassett, M. T. (2017). Structural racism and health inequities in the USA: evidence and interventions. The Lancet, 389(10077), 1453-1463.
Bassuk, E. L., Hanson, J., Greene, R. N., Richard, M., & Laudet, A. (2016). Peer-delivered recovery support services for addictions in the United States: a systematic review. Journal of substance abuse treatment, 63, 1-9.
Blankenship, K. M., Bray, S. J., & Merson, M. H. (2000). Structural interventions in public health. Aids, 14, S11-S21.
Browne, A. J., Varcoe, C., Ford-Gilboe, M., & Wathen, C. N. (2015). EQUIP Healthcare: An overview of a multi-component intervention to enhance equity-oriented care in primary health care settings. International journal for equity in health, 14(1), 152.
Buchanan, J. (2006). Understanding Problematic Drug Use: A Medical Matter or a Social Issue, British Journal of Community Justice, Vol. 4. No. 2 pp.387–397
Canadian Centre on Substance Use and Addiction. (2019). Overcoming Stigma Through Language. A Primer. Available from https://www.ccsa.ca/sites/default/files/2019-09/CCSA-Language-and-Stigma-in-Substance-Use-Addiction-Guide-2019-en.pdf
Canadian Public Health Association. (2019). Language Matters. Using Respectful language in relation to sexual health, substance use, STBBI's and intersecting sources of stigma. Available from: https://www.cpha.ca/sites/default/files/uploads/resources/stbbi/language-tool-e.pdf.
Chinman, M., Oberman, R. S., Hanusa, B. H., Cohen, A. N., Salyers, M. P., Twamley, E. W., & Young, A. S. (2015). A cluster randomized trial of adding peer specialists to intensive case management teams in the veterans health administration. The Journal of Behavioral Health Services & Research, 42(1), 109-121. doi:10.1007/s11414-013-9343-1
Choate, P., & Badry, D. (2019). Stigma as a dominant discourse in fetal alcohol spectrum disorder. Advances in Dual Diagnosis, 12(1/2), 36-52.
Corrigan, P. W., Morris, S. B., Michaels, P. J., Rafacz, J. D., & Rüsch, N. (2012). Challenging the public stigma of mental illness: a meta-analysis of outcome studies. Psychiatric services, 63(10), 963-973.
Covington, S. S. (2008). Women and addiction: A trauma-informed approach. Journal of psychoactive drugs, 40(sup5), 377-385.
Feng, C., DeBeck, K., Kerr, T., Mathias, S., Montaner, J., & Wood, E. (2013). Homelessness independently predicts injection drug use initiation among street-involved youth in a Canadian setting. Journal of Adolescent Health, 52(4), 499-501.
Ford‐Gilboe, M., Wathen, C. N., Varcoe, C., Herbert, C., Jackson, B. E., Lavoie, J. G., Pauly, B.B., Perrin, N.A., Smye, V., Wallace, B., Wong, S.T., & Browne, A.J. (2018). How Equity‐Oriented Health Care Affects Health: Key Mechanisms and Implications for Primary Health Care Practice and Policy. The Milbank Quarterly, 96(4), 635-671.
Glowacki, D. (2015). Effective pain management and improvements in patients’ outcomes and satisfaction. Critical care nurse, 35(3), 33-41.
Greer, A. M., Luchenski, S. A., Amlani, A. A., Lacroix, K., Burmeister, C., & Buxton, J. A. (2016). Peer engagement in harm reduction strategies and services: A critical case study and evaluation framework from British Columbia, Canada. BMC Public Health, 16(1), 452-452. doi:10.1186/s12889-016-3136-4
Griffiths, K. M., Carron‐Arthur, B., Parsons, A., & Reid, R. (2014). Effectiveness of programs for reducing the stigma associated with mental disorders. A meta‐analysis of randomized controlled trials. World psychiatry, 13(2), 161-175.
Irvine, M. A., Kuo, M., Buxton, J., Balshaw, R., Otterstatter, M., Macdougall, L., Milloy, M.J., Bharmal, A., Henry, B., Tyndall, M., Coombs, D., & Gilbert, M. (2019). Modelling the combined impact of interventions in averting deaths during a synthetic‐opioid overdose epidemic. Addiction.
Kellett, P., & Fitton, C. (2017). Supporting transvisibility and gender diversity in nursing practice and education: embracing cultural safety. Nursing inquiry, 24(1), e12146.
Kelly, J. F., Dow, S. J., & Westerhoff, C. (2010). Does our choice of substance-related terms influence perceptions of treatment need? An empirical investigation with two commonly used terms. Journal of Drug Issues, 40(4), 805-818.
Kelly, J. F., Saitz, R., & Wakeman, S. (2016). Language, substance use disorders, and policy: the need to reach consensus on an “addiction-ary”. Alcoholism Treatment Quarterly, 34(1), 116-123.
Kelly, J. F., & Westerhoff, C. M. (2010). Does it matter how we refer to individuals with substance-related conditions? A randomized study of two commonly used terms. International Journal of Drug Policy, 21(3), 202-207.
Kennedy, L. C., Binswanger, I. A., Mueller, S. R., Levy, C., Matlock, D. D., Calcaterra, S. L., Koester, S., & Frank, J. W. (2017). “Those conversations in my experience don’t go well”: A qualitative study of primary care provider experiences tapering long-term opioid medications. Pain Medicine, 19(11), 2201-2211.
Klimas, J. (2015). Training in addiction medicine should be standardised and scaled up. Bmj, 351, h4027.
Knaak, S., Christie, R., Mercer, S., & Stuart, H. (2019). Harm Reduction, Stigma and the Problem of Low Compassion Satisfaction. Journal of Mental Health and Addiction Nursing, 3(1), e8-e21.
Krawczyk, N., Negron, T., Nieto, M., Agus, D., & Fingerhood, M. I. (2018). Overcoming medication stigma in peer recovery: A new paradigm. Substance abuse, 39(4), 404-409.
Kulesza, M., Watkins, K. E., Ober, A. J., Osilla, K. C., & Ewing, B. (2017). Internalized stigma as an independent risk factor for substance use problems among primary care patients: Rationale and preliminary support. Drug and alcohol dependence, 180, 52-55.
Larance, B., Campbell, G., Moore, T., Nielsen, S., Bruno, R., Lintzeris, N., Cohen, M., Hall, W., Mattick, R., O’Donnell, C., & Degenhardt, L. (2018). Concerns and help-seeking among patients using opioids for management of chronic noncancer pain. Pain medicine, 20(4), 758-769.
Livingston, J. D., Milne, T., Fang, M. L., & Amari, E. (2012). The effectiveness of interventions for reducing stigma related to substance use disorders: a systematic review. Addiction, 107(1), 39-50.
Marsh, J. C., D'Aunno, T. A., & Smith, B. D. (2000). Increasing access and providing social services to improve drug abuse treatment for women with children. Addiction, 95(8), 1237-1247.
Marsh, J. C., Smith, B. D., & Bruni, M. (2011). Integrated substance abuse and child welfare services for women: A progress review. Children and youth services review, 33(3), 466-472.
Mathieu, F. (2007). Running on empty: Compassion fatigue in health professionals. Rehab & Community Care Medicine, 4, 1-7.
McGinty, E. E., Goldman, H. H., Pescosolido, B., & Barry, C. L. (2015). Portraying mental illness and drug addiction as treatable health conditions: effects of a randomized experiment on stigma and discrimination. Social Science & Medicine, 126, 73-85.
McKee, S. A. (2017). Concurrent substance use disorders and mental illness: Bridging the gap between research and treatment. Canadian Psychology/Psychologie Canadienne, 58(1), 50.
McLellan, A. T., Hagan, T. A., Levine, M., Gould, F., Meyers, K., Bencivengo, M., & Durell, J. (1998). Supplemental social services improve outcomes in public addiction treatment. Addiction, 93(10), 1489-1499.
Morgenstern, J., Labouvie, E., McCrady, B. S., Kahler, C. W., & Frey, R. M. (1997). “Affiliation with alcoholics anonymous after treatment: A study of its therapeutic effects and mechanisms of action.” Journal of Consulting and Clinical Psychology, 65(5), 768-777. doi:10.1037/0022-006X.65.5.768
Muise, G. M. (2019). Enabling cultural safety in indigenous primary healthcare. Healthcare Management Forum, 32(1), 25-31.
Muskett, C. (2014). Trauma‐informed care in inpatient mental health settings: A review of the literature. International journal of mental health nursing, 23(1), 51-59.
National Academies of Sciences, Engineering, and Medicine. (2016). Ending discrimination against people with mental and substance use disorders: The evidence for stigma change. National Academies Press.
Paino, M., Aletraris, L., & Roman, P. (2016). The relationship between client characteristics and wraparound services in substance use disorder treatment centers. Journal of studies on alcohol and drugs, 77(1), 160-169.
Patel, R. S., Sekhri, S., Bhimanadham, N. N., Imran, S., & Hossain, S. (2019). A Review on Strategies to Manage Physician Burnout. Cureus, 11(6).
Public Health Agency of Agency of Canada (2019). The Chief Public Health Officer’s Report on the State of Public Health in Canada 2019. Addressing Stigma: Towards a More Inclusive Health System. Accessible from: https://www.canada.ca/en/public-health/corporate/publications/chief-public-health-officer-reports-state-public-health-canada/addressing-stigma-toward-more-inclusive-health-system.html.
Raja, S., Hoersch, M., Rajagopalan, C. F., & Chang, P. (2014). Treating patients with traumatic life experiences: providing trauma-informed care. The Journal of the American Dental Association, 145(3), 238-245.
Reif, S., Braude, L., Lyman, D. R., Dougherty, R.H., Daniels, A.S., Ghose, S.S., Salim, O., & Delphine-Rittmon, M.E. (2014). Peer recovery support for individuals with substance use disorders: Assessing the evidence. Psychiatric Services, 65(7), 1.
Shera, W. (1996). Managed care and people with severe mental illness: Challenges and opportunities for social work. Health and Social Work, 21(3), 196.
Solomon, P. (2004). Peer support/peer provided services underlying processes, benefits, and critical ingredients. Psychiatric rehabilitation journal, 27(4), 392.
Staiger, P. K., Thomas, A. C., Ricciardelli, L. A., Mccabe, M. P., Cross, W., & Young, G. (2011). Improving services for individuals with a dual diagnosis: A qualitative study reporting on the views of service users. Addiction research & theory, 19(1), 47-55.
Stuart, H. (2019). Managing the stigma of opioid use. In Healthcare management forum (Vol. 32, No. 2, pp. 78-83). Sage CA: Los Angeles, CA: SAGE Publications.
Stuart, H., Chen, S. P., Christie, R., Dobson, K., Kirsh, B., Knaak, S., Koller, M., Krupa, T., Lauria-Horner, B., Luong, D., Modgill, G., Patten, S.B., Pietrus, M., Szeto, A., & Whitley, R. (2014). Opening minds in Canada: background and rationale. Canadian journal of psychiatry. Revue canadienne de psychiatrie, 59(10 Suppl 1), S8–S12. doi:10.1177/070674371405901s04
Sunderland, A., & Findlay, L. C. (2013). Perceived need for mental health care in Canada: results from the 2012 Canadian community health survey-mental health (pp. 3-9). Ottawa: Statistics Canada.
Tam, T. (2018). Commentary-Building the evidence base for sustained public health response to the opioid epidemic in Canada. Health promotion and chronic disease prevention in Canada: research, policy and practice, 38(6), 221.
Tracy, K., & Wallace, S. P. (2016). “Benefits of peer support groups in the treatment of addiction.” Substance Abuse and Rehabilitation, 7, 143-154. doi:10.2147/SAR.S81535
van Boekel, L. C., Brouwers, E. P., van Weeghel, J., & Garretsen, H. F. (2015). Stigma among health professionals towards patients with substance use disorders and its consequences for healthcare delivery: systematic review. Tijdschr Psychiatr, 57(7), 489-497.
Voon, P., Greer, A. M., Amlani, A., Newman, C., Burmeister, C., & Buxton, J. A. (2018). Pain as a risk factor for substance use: a qualitative study of people who use drugs in British Columbia, Canada. Harm reduction journal, 15(1), 35.
West, C. P., Dyrbye, L. N., Erwin, P. J., & Shanafelt, T. D. (2016). Interventions to prevent and reduce physician burnout: a systematic review and meta-analysis. The Lancet, 388(10057), 2272-2281.
Zizzo, N., & Racine, E. (2017). Ethical challenges in FASD prevention: Scientific uncertainty, stigma, and respect for women’s autonomy. Canadian Journal of Public Health, 108(4), 414-417.