Tackling Antimicrobial Resistance and Antimicrobial Use: A Pan-Canadian Framework for Action

Download the alternative format
(PDF format, 1.42 MB, 44 pages)
Organization: Public Health Agency of Canada
Date published: 2017-09-05
Executive Summary
Antimicrobial-resistant infections are becoming more frequent and increasingly difficult to treat. The rapid emergence and spread of antimicrobial-resistant infections is exacerbated by the widespread use of antimicrobials in human and veterinary medicine and in the agriculture industry.
Antimicrobials are an essential tool against infections in both humans and animals, but they are losing their effectiveness more quickly than we are identifying and developing new drugs or other treatments. These developments have significant consequences for human health, animal health and welfare, food safety, the environment and the economy. Canada must take coordinated action domestically and globally to slow the rising trend of antimicrobial resistance (AMR), to minimize its impact and to preserve the effectiveness of existing and future antimicrobials.
Canada is actively engaged in global efforts to fight AMR and has committed multisectoral support to the implementation of the World Health Organization’s (WHO) Global Action Plan on AMR, as well as to develop and implement its own domestic plan to address the issue. This document, Tackling Antimicrobial Resistance and Antimicrobial Use: A Pan-Canadian Framework for Action outlines the context and the foundation to guide a pan-Canadian approach.
The Framework is grounded in a One Health approach, which recognizes the interconnectedness of humans, animals and the environment. The complexity of AMR underscores the need for coordinated action by the many actors in Canada who are responsible for it such as governments, private and public partners and the public across the human, animal and environmental sectors. To ensure cross-sectoral collaboration and accountability, the Framework was developed with input from federal, provincial and territorial (F/P/T) governments, academics, non-governmental organizations, industry and subject matter experts representing human health, animal health and agriculture sectors at all levels. Its development was facilitated through a dedicated governance structure composed of a Deputy Minister Champions Committee, an F/P/T Steering Committee of senior government representatives, and task groups with subject matter experts.
The overarching goal of the Framework is to strengthen Canada’s ability to combat the risks of AMR in a coordinated, multisectoral and effective manner.
Although all types of antimicrobials (e.g. antifungal, antivirals, antiparasitics) are critical for treating infections, the primary focus of the Framework is on bacterial resistance to antibiotics. This issue is of the utmost concern and warrants urgent action due to the significant threat it presents to human and animal health. The human and animal health aspects of the One Health approach are the initial focus of the Framework. As work advances in these areas, the environmental aspect will be considered.
The Framework consists of four components:
- Surveillance;
- Infection prevention and control;
- Stewardship;
- Research and innovation.
The Framework builds upon the AMR work that is already underway in the human and animal health sectors and strives to connect all these pieces together. Implementation of the Framework will require continued engagement and committed actions by governments, industry and stakeholders in each of the four components to enable a sustainable and effective pan-Canadian response to AMR. The Framework provides the foundation to spur further action and collaboration among partners in human and animal sectors to minimize the impact of AMR, and to ensure that antimicrobials will continue to be an effective tool in protecting the health of Canadians. These actions will be identified through the subsequent development of the pan-Canadian action plan, which will lay out the details of concrete deliverables, measurable outcomes and timeframes.
Table of Contents
- Executive Summary
- 1 Introduction
- 2 The pan-Canadian approach to address Antimicrobial Resistance and Antimicrobial Use
- 3 Core Components
- 4 Implementation
- 5 Conclusion
- Annex I: Roles and Responsibilities in Canada relating to Antimicrobial Resistance
- Annex II: Glossary
- References
1. Introduction
1.1 Defining the Problem
Antimicrobial-resistant infections are becoming more frequent and increasingly difficult to treat. As a result, antimicrobial resistance (AMR) is now recognized as a growing health threat in Canada and around the world.Footnote 1 Left unchecked, AMR could cause a return to a pre-antibiotic era in which common infections could once again become incurable, with grave consequences to the health of Canadians and populations world-wide.
Antimicrobials are natural or synthetic substances that can kill or block the growth of microorganisms.
Antibiotics are a type of antimicrobial used to treat infections caused by bacteria.
AMR occurs when microbes (e.g. bacteria, viruses, fungi and parasites) evolve in ways that reduce or eliminate the effectiveness of antimicrobial medicines (e.g. antibiotics, antivirals, antifungals and antiparasitics) to treat infections by killing or slowing microbial growth. When microbes are exposed to antimicrobials, they adapt and become more resistant. This contributes to increased AMR in humans, animals, crops and in the environment (e.g. water, soil)Footnote 2 through exposure to waste water, consumer products and animal manure. There are also many social and environmental factors that contribute to rising rates of AMR including poor hygiene, inadequate infection prevention and control (IPC) practices, lack of awareness and education about AMR and appropriate antimicrobial use (AMU), insufficient access to health services, overcrowded housing conditions and a lack of clean water.
Since their introduction in the 1940s, antimicrobials have revolutionized modern medical treatment of infectious diseases in humans, animals and plants. Furthermore, the application of antimicrobials has enabled more intensive production of food animals to feed an increasing global demand for animal protein. Over the past decades, however, antimicrobials have become less effective in treating infections world-wide, particularly antibiotics used to treat bacterial infections. Due to their widespread use in human and veterinary medicine, and agriculture settings, antimicrobials have become a major contributor in accelerating the development and spread of AMR. AMR infections are outpacing the development of new drugs, alternative therapies or tools, and are creating a serious challenge. Urgent action by Canada and the international community must take place to counter the potentially devastating effects of the emergence and spread of AMR.
Between 1935 and 1968, fourteen new classes of antibiotics were created for human use, yet since then, only five new classes have been introduced. The need to limit AMU to conserve antimicrobial effectiveness makes their development less commercially desirable and this, combined with their expensive and lengthy research, development and commercialization process, has led to few new products entering the market.
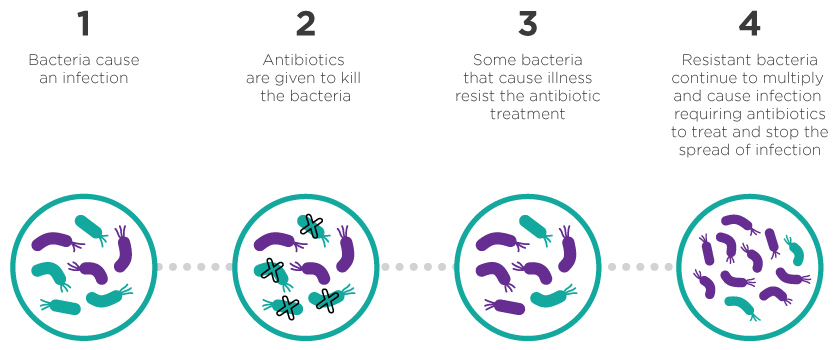
Figure 1 - Text Description
Figure 1 represents how: 1) bacteria cause an infection 2) antibiotics are given to kill the bacteria 3) some bacteria that cause illness resist the antibiotic treatment 4) resistant bacteria continue to multiply and cause infection requiring antibiotics to treat and stop the spread of infection.
Without effective antimicrobials, our ability to fight infectious diseases will significantly decline. Serious infections will become untreatable, illnesses will become longer and more severe, treatments will become more expensive and toxic, and the risk of death will increase. If infections cannot be prevented or treated, procedures such as organ transplants, cancer chemotherapy and major surgeries (e.g. caesarean deliveries or hip and knee replacements) may become so risky that they may not be readily available.Footnote 1
The Organisation for Economic Co-operation and Development estimates that up to 50% of human infections in G7 countries may be resistant to routinely used antibiotics and notes that patients with resistant infections have two to three times higher mortality and risks of complications.Footnote 3 The World Bank predicts that by 2050, severe AMR impacts could reduce the global gross domestic product by 3.8% and cause an additional 24 million people to fall into povertyFootnote 4 if concerted action is not taken.
AMR infections have far-reaching implications for human and animal health and potentially the economy. The economic burden of AMR includes impacts on healthcare systems and labour force productivity due to the increased costs of treating patients, longer illness and higher death tolls.Footnote 5 Individuals sick with drug-resistant infections are often not able to work and as a result, they suffer income loss and this contributes to an overall decline in productivity.
The United Kingdom Review on AMR economic analysis estimates that worldwide 700,000 people die from AMR infections every year. By 2050, this is forecasted to increase to 10 million lives lost annually. A cumulative $100 trillion USD of global economic output is at risk due to the rise of drug-resistant infections.Footnote 6
The appropriate use of antimicrobials in agriculture (e.g. in animals and crop settings) plays a key role in safeguarding the health of food-producing animals, and also promotes the health of the Canadian population by improving access to healthy and safe food at competitive prices. Since the international trade of animal products and food by-products is a critical component of Canada’s agriculture industry, continued alignment with international standards and regulatory measures to address AMR and AMU is crucial for governments and industry in Canada. Some evidence has emerged that several infection-causing animal microorganisms are developing resistance to commonly used antimicrobials, posing a risk to the health and welfare of animals.Footnote 7
Increasing market and social pressures are driving Canadian livestock producers to use fewer antimicrobials to respond to the changing international market requirements, meet consumer demand and support public health. In response, Canada’s animal industry is already making commitments to demonstrate socially responsible AMU practices. To address the challenges of AMR, effective treatments and management approaches must be further implemented to demonstrate appropriate use of antimicrobials in order to ensure the health and welfare of animals, preserve and ensure a safe food supply and keep livestock producers competitive.
Case Story: Last resort antibiotic has side effect complications
A patient in their 40s with leukemia was treated for five weeks with broad spectrum antibiotics since their condition made them more susceptible to infections. Nevertheless, they developed resistant skin and soft tissue infections and were treated with colistin, an antibiotic of last resort. Colistin can be toxic to the kidneys, and the patient developed kidney failure but eventually recovered and was able to return home after an additional four weeks in hospital.
(AMR cases are based on true stories of Canadian patients. Patient information has been altered so as to preserve anonymity.)
1.2 The Global Response to Antimicrobial Resistance
No country is immune to the effects of AMR. Drug-resistant organisms that emerge in a single country can quickly spread across national borders due to migration, travel, medical tourism and the global trade of animals and foods. This was demonstrated in 2008 when a Swedish patient traveled to India and became sick with a newly identified multidrug-resistant infection containing the NDM-1 enzyme (New Delhi metallo-beta-lactamase-1) that enables resistance to critically important last resort antibiotics. This resistance has since spread across multiple countries, including Canada. This case demonstrates how a resistant infection acquired by one individual abroad can easily be brought back to their community and spread across the world.
Given its enormous societal and economic costs, AMR is too great a burden for any one country to bear alone. As such, it must be addressed through a global approach. AMR requires a coordinated One Health approach across domestic and international boundaries that results in shared solutions for an effective, comprehensive response. A One Health approach acknowledges the interconnection between the health of humans, animals and the environment and the need for collaborative efforts across sectors to improve health for all.
The global community is mobilizing through international initiatives to protect human and animal health, conserve antimicrobial medicines and develop innovative responses to mitigate the risk of AMR before the situation worsens. Nations are working together to find ways to share their experience, learn from each other, partner on initiatives and pool resources.
In 2015, the WHO Global Action Plan (GAP) on AMR was endorsed at the World Health Assembly by Member States and acknowledged by heads of state and government at the United Nations General Assembly (UNGA) Meeting on AMR in 2016 as the blueprint for action on AMR. As international AMR infection rates continue to riseFootnote 1, the global community is taking action under the leadership of the WHO, the World Organisation for Animal Health (OIE) and the Food and Agriculture Organization of the United Nations (FAO). Both the OIE and FAO have passed resolutions encouraging Member States to combat AMR and to promote prudent use of antimicrobials in animals and agriculture. In line with the GAP on AMR, Codex Alimentarius has recently established an Ad hoc Intergovernmental Task Force on Antimicrobial Resistance to develop guidelines on integrated surveillance and to review and revise the Code of Practice to Minimize and Contain Antimicrobial Resistance to address the entire food chain. International collaboration and commitments on AMR are also occurring among organizations such as the G7, G20 and the Global Health Security Agenda to strengthen domestic and international capacities.
Canada is actively engaging and collaborating with partners in these venues to support global coordinated actions on AMR and to identify best practices and initiatives that can be leveraged to support domestic action.
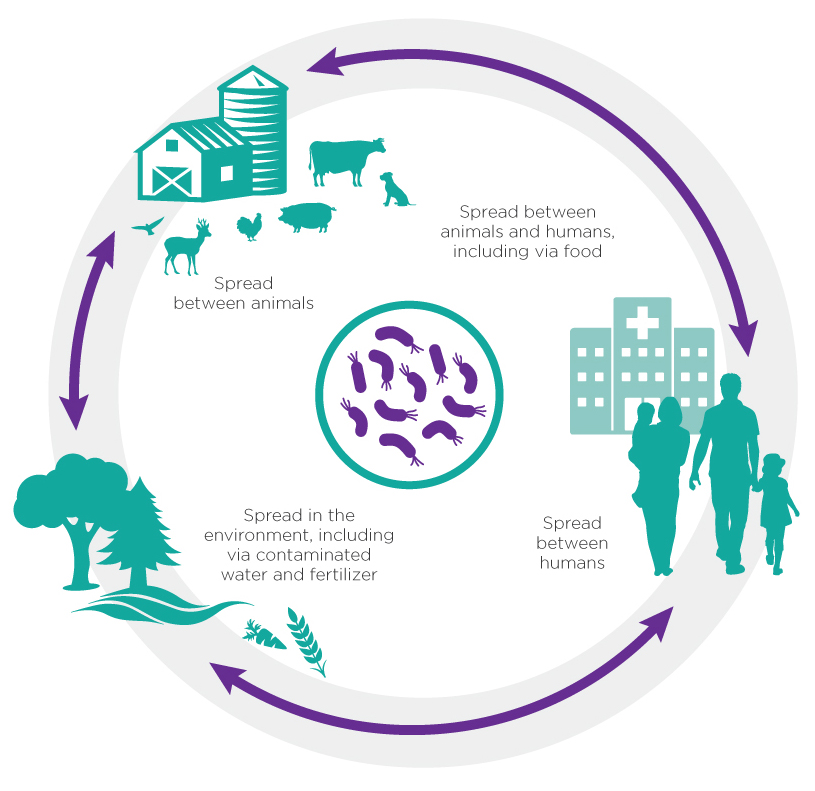
Figure 2 - Text Description
Figure 2 represents how human health, animal health,and the environment are all linked to the issue of AMR. In a continuous circle, you can see how AMR is spread between: 1) humans 2) animals and humans including via food 3) animals 4) the environment, including via contaminated water and fertilizers.
1.3 The State of Antimicrobial Resistance in Canada
Human health
In Canada, rates of most AMR infections are stable and in some cases there has been a decline in the infection rates of select drug-resistant organisms. However, even these reduced rates continue to exceed those of the early 2000s. For example, although infection rates of methicillin-resistant Staphylococcus aureus (MRSA) in hospitals are down by 25 percent since 2008 and rates of vancomycin-resistant Enterococci (VRE) have declined since 2012, these levels remain higher than before 2007 when the increase in resistance began. Rates of Neisseria gonorrhoea, a community-acquired infection, have increased by 43.1% over the past decade and now require stronger and more complex antibiotic treatment. Over 50% of gonorrhoea cases are resistant to at least one antibiotic.Footnote 8
Drug-resistant infections within hospital settings levy a significant cost on Canada’s healthcare system.Footnote 9 Approximately 4.2% of hospitalized patients will become infected with MRSA.Footnote 10 Seventy percent of Canadians fear acquiring an infection in healthcare settings particularly since 1 in 16 patients admitted to Canadian hospitals will develop an infection from a multidrug-resistant organism.Footnote 11
Animal health and food-borne AMR
Canada is a major producer of food animals for domestic and international markets, and there are approximately 19 times more food animals than humans in Canada.Footnote 8 Antimicrobials are used in livestock to treat, control and prevent bacterial disease, improve feed efficiency, promote growth, and to maintain animal health and welfare. Rates of AMU and AMR can fluctuate in agricultural settings due to changing AMU practices among animal species and in agriculture. In Canada, bacteria that harm animals have rarely been studied for AMR. Limited existing information suggests that resistance is present in some, but not all of these bacterial organisms.Footnote 12
AMU in animals
The majority (73%) of antimicrobials distributed for use in animals belong to the same classes as those antimicrobials used in human medicine.Footnote 8
In addition, bacterial infections in animals, such as Salmonella, that can cause food-borne infections in humans have been found to be multidrug-resistant and resistant to antibiotics that are critical to human medicine.Footnote 13
Antimicrobials are also used in companion animals (e.g. dogs and cats) to treat disease. While they account for less than 1% of all antimicrobials used in animals, many of the antimicrobials used to treat companion animals are of critical importance to human health.Footnote 8 Given the close contact between humans and their companion animals, AMR risks must be considered to protect the welfare of animals since resistant organisms can easily be spread between them.
1.4 Addressing Antimicrobial Resistance in Canada
The complexity of AMR is enormous, and addressing it is beyond the capability and responsibility of any one government, agency or organization. Canada must be prepared to respond to the threat of AMR in order to lessen the health risks to Canadians in the face of rising rates of drug-resistant infections around the world. Like their international counterparts, F/P/T governments in Canada are employing a One Health approach to tackle AMR. Together with F/P/T governments, public and private sector partners, including professional associations, industry, academia and the public (Annex I) who have a role to play in AMR must collaborate, coordinate and leverage actions being taken across sectors to minimize duplication and to move in the same direction in an effective and sustained manner.
There are already numerous actions underway that address AMR in Canada by those in the public health, healthcare and agriculture sectors. However, many of these actions have been isolated and uncoordinated, creating an important opportunity to knit them together through improved cross-sectoral coordination and collaboration at all levels for a coherent pan-Canadian response to AMR. Leadership on AMR at all levels of governments and by human and animal health stakeholders taking actions within their spheres of responsibility is required to successfully accomplish this.
At the federal level, the Government of Canada has developed a Federal Framework and Federal Action Plan on AMR to coordinate among federal departments and to initiate and take action within their respective mandates and sectors in the areas of surveillance, stewardship and innovation. Provinces and territories (P/Ts) are undertaking multiple initiatives to combat AMR, including surveillance, public and health professional awareness raising and hospital-based programs to reduce antibiotic use, and immunization programs to prevent and control infections and the spread of infectious diseases. Likewise, stakeholder organizations such as the National Farmed Animal Health and Welfare Council, the Canadian Veterinary Medical Association, the Association of Medical Microbiology and Infectious Disease Canada and other health sector non-governmental organizations have established plans and initiatives to support the appropriate use of antibiotics in human and animal health settings. These documents serve as a starting point from which to build a broader, pan-Canadian approach.
In some cases, Canadian livestock industries have taken the lead in banning or reducing the use of medically important antibiotics as growth promoters or as a preventative treatment for the production of farm animals. For example, in 2014, the Canadian poultry industry eliminated the preventative use of Category 1 antibiotics, which are considered to be of high importance to human medicine.
In the health sector, a team of Canadian physicians is leading Choosing Wisely Canada, a campaign to engage physicians and patients in conversations about overuse of unnecessary tests, treatments and procedures and to help physicians and patients make smart and effective choices to ensure high-quality care. One of the key recommendations of the campaign is to decrease the use of unnecessary antibiotics.

Figure 3 - Text Description
Figure 3 shows the groups who play a key role in addressing AMR in Canada. These groups include: the federal government, provincial and territorial governments, academia, human and animal stakeholders, industry, public and health professionals.
2. The pan-Canadian Approach to Address Antimicrobial Resistance and Antimicrobial Use
2.1 Vision
The health of humans, animals and the environment is protected through comprehensive and coordinated action to conserve the effectiveness of antimicrobials now and into the future.
2.2 Scope
This Framework lays the foundation for collaborative actions to be taken by all sectors to address the effects of antibiotic resistant bacteria on humans, animals and the environment in Canada. The Framework will first focus on the human and animal health aspects of AMR. As actions advance in these areas, the environmental aspect will be considered to fully reflect the One Health approach.
2.3 Purpose
To establish a coherent approach to guide collective efforts in addressing AMR and AMU in Canada with a focus on four key components: surveillance, infection prevention and control, stewardship, and research and innovation.
2.4 Desired outcome
To strengthen ability in Canada to reduce the risks of AMR in a coordinated and effective manner.
2.5 Strategic goals
The Framework is anchored by four overarching goals that support this outcome:
- Strengthen governance structures to generate knowledge and information on AMR and AMU in humans, agriculture and animals through the monitoring, detection and tracking of resistant organisms to develop and monitor interventions.
- Promote, facilitate and measure appropriate AMU in humans and animals to conserve the effectiveness of antimicrobials that are critical to human and animal health, and to limit the development and spread of resistant organisms within and among populations.
- Reduce the need for antimicrobial treatment by promoting infection prevention and control practices to decrease infection rates in healthcare, community and animal settings.
- Support the advancement of research and innovative approaches for the identification, characterization and real time detection of microorganisms including resistant bacteria, the treatment and prevention of infections as well as basic and behavioural research.
2.6 Principles underpinning the Framework
- Collaboration. Working individually will yield some results but real change requires collaborative action by all jurisdictions, sector partners and the public to better coordinate and respond to AMR.
- Integrated approach. The adoption of an integrated One Health approach that recognizes the interconnectedness between humans, animals, and the environment, and for coordinated actions by all implicated actors.
- Sustainability. Implementation of the Framework requires sustained engagement and collaboration across jurisdictions and sectors to reduce the emergence and spread of AMR.
- Information sharing. A concerted response demands that information and best practices are shared and leveraged across jurisdictions and sectors for a cohesive pan-Canadian approach to AMR and AMU.
- Flexibility. Progress on the implementation of the Framework requires a flexible and incremental approach that is adaptable and recognizes that AMR activities and capacities are variable across governments and sectors.
- Global cooperation. Canada’s response to AMR is inextricably linked to global efforts and solutions. It is necessary to align with international efforts to better position and leverage domestic actions that maximize contribution and benefits to Canada in the global context.
- Measuring success. Collaborate across jurisdictions and sectors to develop common indicators and benchmarks to measure the effectiveness of priority actions under the Framework.
3. Core Components
Component 1: Surveillance
Strong, integrated surveillance systems are needed to provide a comprehensive picture of AMR and AMU in Canada.
Background
Surveillance systems are essential to detect, track and monitor emerging and re-emerging resistant organisms, drug-resistant infections and AMU in humans and animals. These systems provide key information and data to identify gaps for actionable outcomes and to better understand the magnitude of drug-resistant infections, AMU, and their impacts. Human health and veterinary medicine professionals, public health authorities, livestock producers, and policy makers at all levels of government rely on high quality data from these systems to inform policy decisions, implement and evaluate stewardship and IPC activities, set research priorities and conduct analyses (namely economic analyses) of the burden of AMR.
AMR and AMU data generated from surveillance systems can be enhanced with the further implementation of an integrated One Health approach to surveillance in Canada, as recommended by the WHO and the OIE, outlined in guidelines from the WHO Advisory Group on Integrated Surveillance of Antimicrobial Resistance and adopted by other G7 countries. This approach creates a full picture of AMR emergence and spread, improves understanding of how and where antimicrobial drugs are being used, provides evidence to show how use is affecting resistance and identifies areas requiring action.
Enhancing surveillance successfully requires coordination and cooperation among governments, non-governmental organizations, industry stakeholders, veterinarians, farmers, healthcare professionals and academia, to share and analyse AMR and AMU data in a timely manner to guide action. Surveillance at all levels depends on this type of partnership and collaboration to be effective. In Canada, there are multiple surveillance systems at different levels of government that collect data on AMR and AMU in human and animal settings such as hospitals, community settings and farms. These systems are not all connected and this hinders good integration of AMR and AMU data.
Canada has several pan-Canadian surveillance systems led by the Public Health Agency of Canada, with input from P/Ts, to track AMR and AMU in healthcare, community settings, veterinary and on-farm/agriculture settings. The Canadian Antimicrobial Resistance Surveillance System (CARSS) reflects an integrated approach to AMR and AMU surveillance. It compiles and synthesizes information from various surveillance systems to provide an integrated, pan-Canadian picture of AMR and AMU across all settings. Pan-Canadian surveillance systems include the Canadian Integrated Program for Antimicrobial Resistance Surveillance (CIPARS) and the Canadian Nosocomial Infection Surveillance Program (CNISP). CIPARS monitors trends in AMR and AMU in selected bacterial organisms from humans, animals and the food supply in order to better understand how resistant bacteria in food and food animals can contribute to resistant illness experienced by humans. CNISP collects information on resistant organisms and monitors AMU in hospitalized patients. These systems are complemented by public and private laboratories across Canada that are engaged in AMR surveillance. Canada’s National Microbiology Laboratory (NML), for example, provides diagnostic testing and reference services to identify and characterize existing and emerging resistant organisms across the One Health continuum. Collaboration with other government and private laboratories is an integral part of NML’s work.
Veterinary diagnostics and surveillance are supported by the Canadian Animal Health Surveillance Network, a collaborative federal-provincial-academic network that links veterinary laboratories across the country to collect animal surveillance data and serves as a surveillance system for animal disease threats to animal and human health and the security of the food supply.
Canada’s pan-Canadian surveillance systems could benefit from better integration and coordination to capture the various factors contributing to AMR. This will improve cooperation on data sharing and collection, particularly in regions of the country where public health laboratories do not exist, to enable proper assessment of the impact of AMR and AMU, to generate data that are comparable across sectors, jurisdictions and internationally, and to align with international surveillance standards and systems such as the Global Antimicrobial Resistance Surveillance System.
The Canadian Public Health Laboratory Network is a national association of public health laboratory professionals which acts as a unified voice for federal and provincial member laboratories. Its AMR Working Group focuses on laboratory requirements and promotes a harmonized approach across Canadian laboratories for AMR surveillance and analysis.
Challenges in surveillance
While pan-Canadian surveillance systems are producing useful, reliable data on AMR and AMU, there are still significant knowledge gaps in measuring the extent of AMR and AMU in humans and animals. These gaps include limited information for certain settings (e.g. community), the need for benchmarking to assess trends in AMR and AMU and an increased need for the standardization of laboratory and data collection methods, case definitions and improved timeliness of reporting.
In order to focus surveillance efforts, Canada has established a list of priority microorganisms that pose a risk to human health. However, there is limited information collected on the resistance of a number of other priority microorganisms of concern to the health of Canadians such as E.coli, MRSA and other multidrug-resistant bacteria. There are also gaps in AMR data collection from community and long-term care settings. In the area of AMU, comprehensive surveillance is needed to support targeted stewardship interventions and research in healthcare and community settings to address AMR. There is a lack of information on antibiotic prescribing patterns in hospitals, community settings and rural and northern healthcare settings.
AMR surveillance data for animals are restricted to specific bacterial organisms (e.g. Salmonella) in specific livestock (e.g. cattle, poultry and swine) while no data are collected for other animal species group (e.g. sheep and companion animals). There is currently minimal systematic surveillance of AMR in microorganisms of primary concern to the health of livestock or other domestic animal species. There are also gaps in data collection across Canada that must be addressed to ensure sampling is representative across target animal species and bacterial organisms.
AMU surveillance gaps in animal health and agriculture settings are also present. In veterinary settings, there is no pan-Canadian systematic data collection on prescribing patterns of veterinarians or on the quantity of antimicrobials prescribed versus those dispensed. Farm-level AMU data are currently limited to select farms (which are few in number and location and are insufficient for benchmarking) to identify trends and antimicrobial usage patterns. In addition, existing surveillance systems do not monitor the type and quantity of antimicrobials imported for own use or as active pharmaceutical ingredients for use in animals and feed.
There is very little data regarding AMR in the environment (e.g. soils, waterways, wildlife) or on AMR or AMU in plant agriculture.
Research and innovation and surveillance are linked. Research and innovation enable better understanding of the emergence of resistant organisms and to identify innovative approaches to monitor and detect resistant organisms. They also enable us to continually adapt our surveillance programs and to ensure their relevance through changes in trends of resistant organisms. More research and innovation are needed on the mechanisms of how AMR develops and spreads, and on tools and methodologies that support the detection and analysis of resistant organisms. In turn, AMR and AMU surveillance supports the identification of research priorities by identifying trends in AMR, AMU and emerging resistant organisms, and provides the data and platforms required to conduct the research and evaluate the effectiveness of IPC and stewardship interventions.
The vast complexity of data collection from healthcare, community, agriculture and veterinary settings poses a major challenge. Surveillance is a shared jurisdictional responsibility in Canada and there are variations in how data are collected, managed and reported by multiple systems at the local, provincial, territorial and federal levels. In addition, resource and infrastructure capacity to collect and analyze data varies. Within this fragmented landscape, comprehensive data comparison and analysis of AMR and AMU becomes extremely challenging.
That said, these surveillance gaps create opportunities to explore actions to better integrate the work of existing surveillance systems, access new AMR and AMU surveillance data, and to develop a robust pan-Canadian AMR and AMU surveillance system. Canada has laid the foundation for an integrated surveillance approach with the establishment of CARSS. However, to truly enhance the integration of AMR data and information, surveillance will require partnership and collaboration between F/P/T governments and relevant stakeholders so that all levels of surveillance systems can be strengthened and made more effective to best monitor and report on AMR and AMU in Canada.
Surveillance opportunities for action:
- Engage with stakeholders to ensure coordination at all levels to move towards robust and comprehensive surveillance systems with defined objectives and the required capacity for AMR and AMU data collection.
- Establish coordinated platforms and mechanisms to link AMR and AMU data, in particular from human health, animal health and agriculture sectors.
- Enhance coordinated technical guidance for data collection, collation and comparison, including developing standardized definitions of AMR and priority microorganisms in humans and animals.
Component 2: Infection Prevention and Control
To contain the spread of resistant organisms and reduce AMR and AMU, standardized infection prevention and control approaches, programs and policies must be in place.
Background
IPC is critical to combatting infectious diseases. IPC focuses on non-antimicrobial strategies that prevent infections in human healthcare, community, veterinary and agriculture settings. It includes elements such as infrastructure, policies, guidelines, practices and procedures.
IPC must figure prominently in any AMR strategy. Well established and consistent IPC measures and practices in all relevant settings can reduce infections and prevent the spread of harmful bacteria, reducing the need for AMU. IPC measures also mitigate the risk of infections spreading from and between humans and animals by helping to reduce the transmission of resistant microorganisms between food animals and food processors, along the food chain, between companion animals and their owners, and between humans in the community and places where healthcare is delivered.
In order to successfully limit the emergence and spread of infections, IPC activities in human and animal settings must be carried out in parallel with activities that reinforce antimicrobial stewardship. In addition, timely and useful surveillance data that link AMR and AMU in all settings is a key factor in implementing and measuring the success of IPC.
Canada has established many important IPC measures for infectious diseases, some of which are commonly applied in human and animal settings. Key IPC measures and practices used in healthcare, community, veterinary and agriculture settings include good biosecurity practices, hand and respiratory hygiene, environmental hygiene and sanitation, sterilization and disinfection of equipment, proper food handling and processing, education, training, immunization and infectious disease outbreak management. These measures are all important to protect the work force in human and animal health and food production settings.
The role of immunization cannot be understated as a crucial IPC measure to prevent infectious disease. As a first line of defence, biosecurity and immunization contribute to the health and well-being of humans and animals by preventing infections and controlling the transmission of disease. Immunization programs and strategies must continue to underpin efforts to control AMR and reduce AMU.
Governments at all levels in Canada and all affected stakeholders, including animal industry groups, medical and veterinary professionals and associations, play a fundamental role in promoting good IPC practice. Establishing partnerships among these actors across jurisdictions and sectors to integrate and align approaches to IPC should be considered where possible.
IPC is essential to prevent the spread of infections in healthcare settings (e.g. hospitals, long-term care facilities, dentist's and physician’s offices). Healthcare workers and patients count on effective IPC measures in hospitals to protect their health and safety. IPC programs are particularly important in hospitals because of the risk of acquiring healthcare-associated infections such as MRSA, multidrug-resistant Enterobacteriaceae and VRE. Hospitalized individuals frequently share rooms and bathroom facilities and can be exposed to equipment that is used on multiple patients. These practices make for the easy spread of microorganisms and resistant genes in the hospital environment between healthcare workers and patients if IPC measures are not in place.
Accreditation Canada’s Qmentum Program is designed to focus on quality and safety. It requires that all participating health service providers meet comprehensive IPC standards and that health systems and acute care organizations implement an antimicrobial stewardship program. These standards can be promoted to help all health services sectors achieve quality improvement in IPC and antimicrobial stewardship.
The implementation of best practice IPC policies and procedures in all healthcare settings could reduce the high costs of AMR infections and lower the risk of infections when diligently followed by all healthcare professionals. Specific examples of current IPC policies and procedures in hospitals include hand hygiene programs, routine practices and additional precautions, screening to identify infected patients, environmental hygiene and sanitation as well as the disinfection or sterilization of reusable equipment. Accreditation programs as well as audit and feedback systems help healthcare workers improve IPC practices. Public reporting of hospital-associated infection rates also increases healthcare organizations' compliance with IPC practices.
In the community, high rates of respiratory tract infections (e.g. colds, influenza, pneumonia and otitis media) cause illnesses in children and adults. These infections are more likely to spread in settings where people congregate and where good IPC is challenging, such as schools and daycares. As a result, bacteria can spread in community settings because of poor hygiene, overcrowding and inadequate environmental cleaning. Good hand and respiratory hygiene and immunization are key IPC measures that should be more widely promoted in the community.
The objective of IPC in animal agriculture and veterinary settings is to prevent and control disease in animals (e.g. companion and food animals), produce high quality and safe food for humans, protect the safety of farm workers and the public, and ensure the economic sustainability of the agriculture industry.
Canada has established pan-Canadian IPC standards for animal care in collaboration with veterinary associations and the livestock industry. These include biosecurity guidelines, on-farm management practices for varying stages of production, cleaning and disinfection procedures, on-farm food safety and certification programs, animal welfare codes of practice, and enforceable traceability systems that identity and track the movement of animals for quality assurance and effective disease control. Immunization programs are also available to prevent infectious diseases in animals.
Challenges in IPC
In spite of the many IPC measures and practices in Canada, there are challenges in implementing them within and across human and animal settings.
In healthcare settings, IPC programs are well established in Canadian acute care facilities; however they are less common in long-term care facilities and other places where healthcare service is delivered. Even in acute care facilities, IPC programs may not have the recommended personnel support, such as a practitioner trained in IPC, and a sufficient number of IPC professionals. While there are numerous IPC best practices available, healthcare facilities may sometimes experience low and inconsistent compliance due to complex, rapidly outdated guidelines. Limited resources and infrastructure, particularly in some small hospitals and rural and remote regions, may also affect their ability to participate in surveillance programs.
Community IPC interventions are further compounded by social and economic factors that impact the health and well-being of people and the risk of acquiring resistant infections, especially in low-income, rural and remote settings with a lack of sanitation, limited clean water and overcrowded housing.
Various P/T initiatives are in place to support standardized and customized approaches in IPC practices. The Alberta Veterinary Medical Association’s Biosecurity in Practice Manual and Toolkit is an example of a best practice that could be shared nationally. Public Health Ontario’s Provincial Infectious Diseases Advisory Committee has created evidence-based best practice documents providing a reference for healthcare organizations when developing their IPC policies and procedures.
In agriculture and veterinary settings, biosecurity and on-farm food safety and certification programs are variable. Some are voluntary while others are mandatory. Most of the major commodity groups have biosecurity programs that include IPC, but implementation of these programs is adapted to the realities of agricultural operations, which presents some disparities. In some cases, these programs vary at the sector level because it is left to livestock producers working with veterinarians to design their own protocols. In addition, effective vaccines are not available for all animal diseases and when accessible, the implementation of vaccines and other management practices are sometimes incomplete and may not always have an economic benefit. Improved tracking and traceability systems are also needed to address gaps related to animal movement and identification.
Disparity in governance across the country affects IPC programs in the agriculture sector. Governments and industry have different responsibilities such as enforcing safety regulations, setting policy direction and providing input to policy at the industry level. Not all jurisdictions (P/Ts and industries) have the same capacity to deliver animal health services. In addition, there is an inconsistent level of integration of IPC measures among livestock producers, companion animal owners, medical and veterinary professionals and the public.
IPC interventions must be targeted and evaluated to ensure they work as intended. Research and innovation can assist the identification of more innovative and effective approaches to gain a better understanding of sources of infection, behaviours and attitudes towards IPC. In healthcare and community settings, there is a need to identify the best interventions to facilitate good hygiene and IPC practices and to address vaccine compliance and hesitancy. In the agriculture and veterinary settings, research on management practices to avoid the preventative use of antibiotics and promote appropriate use, and on new technologies to address efficient vaccines strategies and disease surveillance should be explored.
If we are to make significant gains in preserving the effectiveness of antimicrobials, IPC must be at the forefront in preventing and controlling the spread of all infections, especially those caused by drug-resistant organisms. It is needed across all settings and governments must foster a culture in which all understand the importance of IPC and take ownership within respective roles to support effective IPC.
Case Story: Piglet skin infection resolved with IPC and management measures
An endemic problem of severe methicillin-resistant Staphylococcus hyicus bacterial skin infection (“greasy pig disease”) causing deaths in a piglet nursery, was eventually controlled by instituting a rigorous program of hygiene involving group flow control (“all-in-all-out”) and management.
Infection prevention and control opportunities for action:
- Engage all levels of government and stakeholders to take action within their realm of responsibility:
- Deliver communication, education/ training programs and tools on evidence-based IPC practices and strategies for all stakeholders and professionals in human and animal health.
- Facilitate and promote the application and oversight of IPC best practices, including immunization, through policy/guidelines development, standard-setting and knowledge translation.
- Work with communities and stakeholders to build capacity and reduce inequalities in delivering comprehensive and effective IPC programs in the human and animal health sectors.
- Invest in IPC research to expand knowledge about and improve the effectiveness and sustainability of IPC practices across human and animal health.
Component 3: Stewardship
Programs and policies that highlight education, awareness raising as well as professional and regulatory oversight will be required to reduce inappropriate prescribing, dispensing and use of antimicrobials in humans and animals and to conserve the effectiveness of new and existing antimicrobials.
Background
Widespread use of antimicrobials across human and veterinary medicine and agriculture sectors is a major factor in the emergence and spread of resistant bacteria. Appropriate AMU is recognized as a core element in managing the risks of AMR to preserve the effectiveness of antimicrobials and slow the development of drug-resistant organisms. To minimize the risk of AMR from the widespread use of antimicrobials, changes are needed in how we foster antimicrobial stewardship across human and animal health sectors.
Antimicrobial stewardship is recognized as a key component of a multidisciplinary, multipronged approach to minimize the spread and development of AMR. Antimicrobial stewardship refers to coordinated interventions designed to promote, improve, monitor and evaluate judicious AMU to preserve their future effectiveness and to promote and protect human and animal health. Successful antimicrobial stewardship should be based on this common understanding as well as on leadership, collaboration, appropriate interventions and resources that foster appropriate AMU. The four key components of promising antimicrobial stewardship programs and initiatives are governance, measurement, evidence and interventions.Footnote 14
Antimicrobial stewardship is a shared responsibility and requires an integrated perspective that coordinates and aligns actions at all levels of government as well as among livestock commodity groups, human and animal health associations and regulatory bodies, patients, health professionals, regulatory colleges, veterinarians, researchers and the public. All involved must appreciate the importance of their role in adopting practices that encourage effective antimicrobial stewardship and be supported by sufficient resources and multidisciplinary expertise.
Antimicrobial stewardship is most effective when supported by surveillance, research and evaluation, and has audit and feedback mechanisms in place. This information can be used to monitor and evaluate stewardship programs, to set performance targets and benchmarks, and to identify new tools and innovative approaches. Research into standardized indicators, alternatives to antimicrobials (e.g. vaccines, good on-farm management practices), diagnostic tools, and into the behavioural and social aspects of antibiotic prescribing practices and use in human and animal health settings should be considered.
Building knowledge about AMR and AMU among medical and veterinary health professionals, livestock producers and the public is central to effective antimicrobial stewardship. Knowledge translation and training of medical and veterinary health professionals is critically important to ensure that antimicrobials are prescribed, dispensed and administered appropriately. Medical and veterinary health professionals need ongoing training and support to effectively communicate with patients and clients about the risks and benefits of AMU. This must be complemented by increased public awareness about the appropriate use of antimicrobials for sustained antimicrobial stewardship. Collaborative awareness efforts with targeted messages across human and animal health sectors should be established and directed towards a broad audience.
In Canada, there are a myriad of hospital, community and veterinary-based antimicrobial stewardship initiatives that promote appropriate AMU among those who prescribe and dispense antimicrobials (e.g. physicians, nurses, pharmacists, dentists and veterinarians) and those who use them (e.g. patients, consumers, parents, livestock producers, farmers and pet owners). Key initiatives include hospital accreditation programs, patient and community-based educational initiatives, public awareness campaigns, best practice guidelines, regulatory mechanisms, quality assurance and on-farm food safety and certification programs. Together, these interventions are making a positive impact, but they lack the consistency and coordination to fully address the challenge of AMR.
In hospital settings, AMU may be increasing hospital-associated infections caused by resistant organisms. In 2014, AMU in hospitals represented at least 30% of all AMU in human health.Footnote 15 Insufficient resources and training for hospital health professionals about AMR as well as limited antimicrobial stewardship programs in some hospitals are also contributing to inappropriate AMU.
Do Bugs Need Drugs? is a successful education program in Alberta and British Columbia that targets AMR and AMU in the community through education on infection prevention and the promotion of responsible prescribing and use of antibiotics.
In community settings, antibiotics are often prescribed without laboratory testing and confirmation and are often used inappropriately to treat viral infections (e.g. colds, flu, acute sinusitis) for which they are ineffective and can promote the development of resistant bacteria. Many patients expect antibiotics as an immediate solution for the treatment of minor infections and some physicians prescribe antibiotics to fulfill patient expectations even if the treatment is unnecessary. In 2014, it was estimated that over 23 million antimicrobial prescriptions were written for human consumption in Canada and 93% were dispensed by community pharmacists.Footnote 8 Of these, it is estimated that 30–50% were unnecessary.Footnote 15 This highlights the need for better knowledge about the issues of AMR, improved diagnostic tools and behavioural research to better understand the drivers of prescribing and use.
Antimicrobials are critical for the management of animal health and welfare and have been used historically in the treatment, control and prevention of bacterial diseases in individual animals, herds and flocks. Some are also used to promote growth in food animals, a usage pattern that has been recognized as inappropriate for medically important antimicrobial drugs. Appropriate usage of antibiotics protects the health and welfare of animals, assures safe animal food products, maintains productivity and sustains the economic viability of the livestock industries. In 2014, approximately 82% of antimicrobials important to human medicine were distributed and/or sold for use in food-producing animals, 27% for humans, and less than 1% for companion animals and crops respectively.Footnote 13 Adjusting for underlying populations and average weights, in 2014, there was roughly 1.7 times more antimicrobials distributed for use in animals than humans.Footnote 8
Veterinarians play a key role in prescribing antibiotics for use in food animals and companion animals. They ensure the right antibiotics and correct dosage are prescribed and administered to treat disease in animals within the boundaries of a valid veterinary-client patient relationship. In Canada, veterinarians have the privilege of extra-label drug use in certain situations to accommodate the limited range of approved drug products and drug doses for treating disease in different animals. In some Canadian jurisdictions veterinarians can prescribe and dispense antibiotics simultaneously. In these instances, it is particularly important to assure that antibiotics are prescribed, dispensed and administered prudently.Footnote 15
Challenges in stewardship
There are many common gaps across human and animal health sectors that limit an integrated approach to AMU stewardship in Canada, while others are specific to each sector.
Coordinated pan-Canadian leadership on antimicrobial stewardship has been sparse and inconsistent and this creates barriers for the adoption of successful interventions beyond regional boundaries. Some jurisdictions have active stewardship programs, but there is variable collaboration. As a result, systematic approaches to foster cohesive and effective interventions and efforts to establish common definitions and benchmarks for appropriate AMU across sectors are challenging. There is varying oversight on the prescribing and dispensing of antimicrobials in jurisdictions, and this necessitates a need for consistency in the veterinary and healthcare sectors.
Insufficient investments in surveillance, behavioural research, prescription monitoring, and audit and feedback programs hamper the ability to build evidence of effective interventions that can change patterns of AMU. This makes it difficult to assess the effectiveness of stewardship programs and to identify areas for improvement, and to establish needed benchmarks to fully measure the progress of appropriate AMU in humans and animals. As such, data to fully account for medical and veterinary prescribing practices, and AMU by livestock producers are lacking.
Limited knowledge translation and exchange within and across human and animal health sectors prevent information sharing that could foster better informed stewardship and enhance understanding of AMU practices and behaviours across the continuum of human and animal medicine.
In agriculture and veterinary settings, regulatory roles and responsibilities for antimicrobial drugs are shared between F/P/T governments.
The federal role on antimicrobial stewardship is limited to the regulation of drug importation, approval and sale. P/Ts manage the actual use and control how antimicrobials are distributed and dispensed in addition to regulating the practice of medicine. While some P/Ts have long standing prescription-status regulations on access to all veterinary antimicrobials, in the majority, some of these drugs are still available for use in livestock without veterinary prescriptions. There is a need for harmonization to ensure regulatory consistency for the dispensing of all veterinary antimicrobials across jurisdictions.
The animal health sector has mobilized nationally and produced leading stewardship guidance, including the National Farmed Animal Health and Welfare Council’s Antimicrobial Stewardship in Food Animals in Canada and the Canadian Veterinary Medical Association’s Veterinary Oversight of Antimicrobial Use-A Pan-Canadian Framework for Professional Standards for Veterinarians.
To alleviate gaps in federal rules, the Government of Canada is strengthening the responsible use of antimicrobials in veterinary medicine through regulatory amendments to the Food and Drug Regulations and by putting forward complementary policy measures aimed at removing growth promotion claims and increasing veterinary oversight of the use of medically important antimicrobials in animals.Footnote 16 These efforts lay a federal foundation for further action and implementation by all sectors, including P/T authorities, food animal producers, veterinarians, industry and other animal health stakeholders. While these efforts will contribute significantly to antimicrobial stewardship, better coordination of federal and P/T efforts are needed to enhance stewardship in the veterinary medicine and agriculture sector.
Regulatory constraints and a lack of available research also limit the commercialization and use of feed additives and low-risk health management products and tools, such as vaccines, probiotics and diagnostics in Canada’s animal agriculture sector.
In healthcare settings, there are some audit and feedback programs in hospitals that encourage changes to prescribing practices, but these are not universally applied. In the community, there are no consistent or comprehensive processes for assessing the prescribing patterns of individual healthcare professionals, though some professional regulators and provinces are considering indicators for prescribing patterns.Footnote 17
Although some jurisdictions in Canada have developed guidelines for antimicrobial prescribing, the establishment of pan-Canadian guidelines could improve and harmonize antimicrobial prescribing practices across the country and among health and veterinary professionals. This could lead to greater success in altering behaviour to meaningfully reduce inappropriate AMU.Footnote 17
The magnitude of inappropriate AMU in human and animal settings is a cause for urgent action. Improved knowledge translation, awareness, communication, training and guidance about AMR and AMU by health and veterinary professionals, livestock producers and the public, in combination with better coordination of F/P/T governments efforts are needed to foster a sustained culture of antimicrobial stewardship.
Stewardship opportunities for action:
- Support the development of a pan-Canadian antimicrobial stewardship network to provide ongoing leadership and coordinated action across human and animal health sectors, while respecting the roles and responsibilities of each level of government.
- Implement a robust system for collecting AMU data to support continuous improvement of stewardship across the human and animal health sectors.
- Develop governance tools, such as regulations and organizational accreditation requirements as well as consistent standards for prescribing, dispensing and distributing of medically important antimicrobials for medical and veterinary use, while respecting the roles and responsibilities of each level of government.
- Build knowledge about antimicrobial stewardship through enhanced and coordinated educational curricula for prescribers (including continuing education opportunities), dispensers and end users of antimicrobials as well as public awareness programs and activities, which highlight the impact of AMR and AMU.
Component 4: Research and Innovation
Responses to AMR must be evidence-based and will require increased knowledge, innovative tools and collaborative approaches to better understand resistance and the development of new treatments and strategies.
Background
Research and innovation are key factors in a multi-faceted approach to overcome the challenges of AMR. They offer tremendous possibilities to improve our understanding of the development and spread of AMR to foster appropriate AMU to preserve antimicrobial effectiveness, to stimulate the development of new antimicrobials, and to find better diagnostic tools. As mentioned in previous sections, research and innovation are also important to support the strengthening of surveillance systems, antimicrobial stewardship and IPC programs.
The effectiveness of antimicrobial medicines is declining while the number of resistant organisms is increasing. There is an urgent need to develop new antimicrobials, alternative therapies and tools to meet current and future medical requirements. Pharmaceutical companies have slowed investments in their research and development in this area because antibiotics are costly, take many years to develop and yield low profit returns due to their short duration of use and low price. Antimicrobials have high failure rates in the development process and the current regulatory processes could be amended to facilitate a speedier introduction to market.
The Joint Programming Initiative on Antimicrobial Resistance is an international collaboration of 26 countries, including Canada, aimed at coordinating research and actions of the diverse countries to achieve long-term reductions in resistance levels and better health outcomes. Current areas of focus include AMR transmission and developing or repurposing antibiotics.
All around the world, countries are grappling with the lack of new medicines to treat AMR infections. The global community (e.g. G7 and G20) has made commitments to research and innovation and is seeking effective solutions such as antibiotic development, alternative medicines, vaccines, diagnostics, economic incentives for research and development, and collaboration across countries and sectors. Substantial investments are being made to forge collaborative partnerships to maximize existing and future AMR efforts and to pool financial resources. Canada and other countries must consider new approaches to treat resistant infections and examine ways to encourage large drug companies to re-enter the AMR research and development field.
Canada has a strong and collaborative research and innovation culture with expertise in (but not limited to) drug discovery, microbiology, alternatives and adjuvants to antimicrobials, livestock management/housing and vaccine research. Academic institutions, government, non-governmental organizations and industry researchers are making important contributions to protect the health of humans and animals against AMR.
In academia, the research and innovation landscape is robust and internationally competitive. University-based researchers are working at large teaching hospitals and veterinary schools. Innovation hubs have been established that focus on human health as well as animal and agriculture research and many have strong collaborations with industry. These hubs are applying basic research to advance the development and commercialization of AMR-related products. Canadian researchers are also enlisting commercial livestock producers to develop regionally-appropriate solutions that are acceptable to industry. Complementary research work is being carried out by federal and provincial government researchers to inform AMR research and innovation.
Most university-based research funding is provided through federal granting councils and complemented by funding from provincial research-funders and non-governmental organizations. Funding to support AMR and AMU discovery efforts is provided at the federal level by the Canadian Institutes of Health Research (CIHR), the Natural Sciences and Engineering Research Council, the Industrial Research Assistance Program of the National Research Council (NRC) and Agriculture and Agri-Food Canada. CIHR is the primary federal human health research funder. Between 2011-12 and 2015-16 it invested more than $96 million in AMR-related research, including $20 million in 2015-16. At the provincial level, funding has been provided by the Saskatchewan Agriculture Development Fund, the Alberta Livestock and Meat Agency and the Ontario Ministry of Agriculture, Food and Rural Affairs, among others.
Major industry not-for-profit funding agencies such as Swine Innovation Porc, the Beef Cattle Research Councils, Canadian Poultry Research Council and their provincial counterparts also directly fund AMR research.
Challenges in research and innovation
Notwithstanding Canada’s considerable research efforts, we continue to lack new antimicrobials, diagnostic tools and alternative treatments to antimicrobials (e.g. vaccines, antibodies, probiotics, phage and lysin therapies). Canadian firms involved in AMR-related research and development have a very small competitive niche and account for less than 1% of Canada’s life sciences sector. Only a few of these companies have a specific focus on AMR. Large pharmaceutical companies do not view the Canadian market as financially lucrative because of the relatively smaller size of the market and the lack of regulatory incentives or policies specifically aimed at addressing AMR. Policy initiatives to support companies to develop and bring new drugs, alternative therapies and technologies to market should be explored. This could ensure that Canadians have access to new and effective antimicrobial medicines, alternatives and tools.
Research and innovation centres across Canada are involved in leading edge vaccine development including the production of conjugate Neisseria vaccine (NRC Ottawa), several cattle and chicken vaccines [Vaccine and Infectious Disease Organization (VIDO), Saskatoon and Guelph] and building capability for genomics-based vaccine development [VIDO and the University of British Columbia (UBC)]. Microbiome and probiotics research (BioK Inc. Quebec; Microbiome Insights BC, and UBC) and a therapeutic monoclonal antibody pipeline with the potential to be used for infections (Centre for Drug Research and Development) are also under development.
More discovery research is needed into tools and therapeutics for human and veterinary medicine, particularly on-farm to test the many diseases in animals for which there are no effective vaccines. New diagnostic tools for human medicine and food animals must consider costs and economic impacts for medical practice and food animal production. There is an urgent need for diagnostic technologies to rapidly identify resistant bacteria and viral infections in both human and veterinary medicine to facilitate more appropriate and immediate treatment.
If any of these new interventions and technologies are developed, understanding the implications for livestock production and the health care system will be critical. This could increase costs to the human and animal sectors given that there is little knowledge about the economic impacts of policy changes in this regard. Research into the economic costs of AMR and the development of evidence-based policy should be considered.
Research that increases knowledge about AMR transmission and risks to human and animal health and the environment will facilitate the development of tools and medicines, and enhance the evaluation of stewardship and IPC interventions. There is insufficient understanding of AMR in the environment and about the social factors that contribute to its development. This includes the degree to which AMU in the environment influences the development of resistance in humans and animals as well as a better understanding of the relationship between AMU in agriculture and its effects on human and animal health. Likewise, more evidence is needed to understand medical and veterinary prescribing practices, the public and livestock producers’ behaviours towards antimicrobials, and to identify innovative approaches to improve livestock management practices in agricultural settings, and IPC practices in healthcare and community settings.
While Canadian researchers have a strong history of collaboration, the human and animal research sectors often work in siloes and there are varied research approaches across the country. In addition, Canada is experiencing a shortage of researchers working on innovative solutions to AMR. This is due to a lack of strategic investments in AMR research and innovation which puts Canada at risk of losing our best innovators to other countries. Those presently active are generally established researchers and support is needed to attract the next generation.
Public funding for AMR is directed primarily towards basic discovery research, which can weaken our capacity to translate research findings into concrete products. Public investment is not always readily accessible due to limited funding timeframes and inflexibility in the use, transfer and access to funds.
In spite of these limitations, Canada has fostered significant expertise in AMR that will enable us to identify niche areas for targeted investment resources in research and innovation that will strengthen domestic capacity and contribute to global AMR research and innovation initiatives.
Case Story: Dog fight with an untreatable infection
A Jack Russell Terrier was infected by two types of multidrug-resistant bacteria (Staphylococcus pseudintermedius and Enterococcus faecium) after being attacked by another dog. The combined infection was resistant to methicillin and all other antibiotics. The dog died three days after the fight.
Research and innovation opportunities for action:
- Support a cross-sectoral, multidisciplinary research network to facilitate antimicrobial discovery, best practices, behavioural research and economic and production impacts across sectors and jurisdictions.
- Explore mechanisms to develop the capacity and appropriate infrastructure required to further support the development of human and veterinary medicines and alternative tools.
- Establish a fast-tracked cost-effective process for licensing antimicrobial drugs, alternatives to antimicrobials and new diagnostic tools in Canada to incentivize pharmaceutical investment without compromising safety, efficacy and quality.
4. Implementation
The Pan-Canadian AMR Framework is the first phase in Canada’s response to AMR and provides a foundation to identify and develop steps to address AMR and AMU challenges. The second phase will focus on the development of a corresponding pan-Canadian action plan. This action plan will further define roles and responsibilities of F/P/T governments, lay out the details of concrete deliverables, timelines, measurable outcomes, priorities and allow for the tracking of progress against actions. Its development and implementation will bring together F/P/T governments in collaboration with human and animal health stakeholders to identify concrete actions within their spheres of responsibility to support coordination and leveraging within and across sectors.
5. Conclusion
Canada is currently taking significant steps to address AMR and AMU domestically and internationally. Tackling Antimicrobial Resistance and Antimicrobial Use: A Pan-Canadian Framework for Action affirms the commitment of F/P/T governments to take coordinated and comprehensive action to mitigate the risk of AMR and to protect the health of Canadians.
Annex I. Roles and responsibilities in Canada relating to Antimicrobial Resistance
In Canada, responsibility for healthcare and agriculture is shared between F/P/T governments. Although F/P/T governments’ roles and responsibilities are distinct in these areas, they complement each other.
The federal role in AMR includes promoting animal health; surveillance of infectious diseases; liaising with international organizations; health promotion and delivering health care services to federal populations (e.g. on-reserve First Nations communities); supporting AMR awareness and education of federally employed healthcare providers; facilitating research and innovation to understand AMR and find new treatment options and tools; regulating the safety and effectiveness of antimicrobial products through the approval of antimicrobial drugs and other health products and tools; establishing pan-Canadian policies and standards on animal health; and ensuring the safety of the Canadian food supply through inspection and biosecurity standards setting.
Provinces and territories are responsible for healthcare settings and the delivery of healthcare services; establishing policies and standards for healthcare settings; promoting human and animal health; education and awareness raising of the appropriate use of antimicrobials; immunization programs; supporting research and academic initiatives; managing surveillance systems for monitoring the prevention and control of diseases in order to gather information on AMR and AMU; approving antimicrobials for medical formularies; establishing and implementing regulations for the distribution, dispensing and use of antimicrobials in agriculture and veterinary medicine; establishing on-farm food-safety and certification programs, inspection programs; biosecurity standards for the agriculture sector, setting IPC measures and undertaking surveillance in healthcare settings.
External stakeholders have a range of roles and responsibilities related to AMR:
Professional associations and licensing bodies (e.g. medical and veterinary medicine associations and regulatory colleges) establish standards and certification for their professions and prescribing guidelines in addition to playing roles of awareness and training, etc.
Health professionals conduct accurate diagnosing of infections, proper prescribing and dispensing of medications, contribute to surveillance, educate patients and owners of animals and establish infection prevention and control programs including biosecurity.
Individual healthcare settings (e.g. hospitals, community practice, and long-term care facilities) implement IPC measures and perform surveillance.
Non-governmental organizations take action within the human, animal and agriculture sector to advance AMR issues (e.g. collect information on AMR and AMU, deliver education and awareness programs, address sector specific issues [e.g. livestock, microbiology]).
The academic sector undertakes research to better understand AMR and discover solutions to counteract and treat resistance.
Life science firms support AMR-related technology development, or partner with academia to facilitate the commercialization of research innovations.
The agriculture industry advances especially the appropriate use of antimicrobials and establishes some control programs in farmed animal productions to protect the health of animals and to preserve the quality of the food supply.
The public protect themselves and others from infections and have a responsibility to use antibiotics properly.
Annex II. Glossary
- Adjuvant
- A substance added to a vaccine or antimicrobial to enhance its effectiveness.
- Antibiotics
- Are either produced by microorganisms or are synthetic substances derived from microorganisms. They are used to treat infections caused by bacteria.
- Antimicrobials
- Are natural or synthetic substances that can kill or block the growth of microorganisms.
- Antimicrobial resistance (AMR)
- Ability of microorganisms to evolve to survive and develop ways to evade antimicrobial agents (e.g., antibiotics, antivirals).
- Antimicrobial use
- How antimicrobials are used including treatment goal, duration of use, route of administration, and species (e.g. human, animal or plant).
- Broad spectrum antibiotics
- Antibiotics that work against a wide range of bacteria.
- Community-acquired infection
- Infections acquired outside of a hospital setting.
- Enterobacteriaceae
- Family of Gram-negative bacteria including Escherichia coli (E. coli) and Klebsiella. Some (E. coli) are part of a normal gut flora while others can cause infection.
- Extra label drug use
- Use or intended use of a drug approved by Health Canada in an animal in a manner not in accordance with the label or package insert.
- Food-producing animals
- Animals raised for the production of meat or other food products.
- Growth promotion
- The use of antimicrobials to increase rate of weight gain and/or efficiency of feed in animals.
- Healthcare-associated infection
- Infection that a patient contracts (or acquires) in a setting where healthcare is delivered (e.g. a hospital, long-term care facility).
- Hospital-associated infection
- Infections acquired in a hospital setting.
- One Health
- Coordinated, collaborative, multi-disciplinary approach to address health risks that originate at the animal-human-ecosystems interface.
- Medically important antimicrobial
- Antimicrobials essential for the treatment of serious bacterial infections with limited or no availability of alternative antimicrobials for effective treatment in case of emergence of resistance to these agents.
- Methicillin-resistant Staphylococcus aureus (MRSA)
- Healthcare associated infection resistant to the methicillin, one of the first-line antibiotics used to treat Staphylococcus aureus infections.
- Multidrug-resistant
- Microorganisms that have acquired resistance to one or more classes of antimicrobial agents.
- Preventative use
- Administration of an antimicrobial to provide protection in advance of disease development.
- Salmonella
- A bacterium that attacks the digestive system. It is one of the most common causes of food-borne infection.
- Vancomycin-resistant Enterococci (VRE)
- Bacteria that cause a range of infections in the urinary tract, bloodstream and surgical wounds of hospital patients and are resistant to the antibiotic vancomycin.
- Veterinary-client-patient relationship (VCPR)
- Pre-requisite to establish medical need and consequently to prescribe or dispense antimicrobials, a VCPR is an on-going working relationship between the veterinarian, client and specific animal patient(s) established on trust.
References
Note: The AMR Framework was informed by the reports on the components of the Framework developed by the four Task Groups.
- Surveillance Federal, Provincial and Territorial AMR Task Group. Surveillance Report; 2016
- Infection Prevention and Control Federal, Provincial and Territorial AMR Task Group. Infection Prevention and Control Report; 2016
- Stewardship Federal, Provincial and Territorial AMR Task Group. Stewardship Report; 2016
- Research and Innovation Federal, Provincial and Territorial AMR Task Group. Research and Innovation Report; 2016