Common Definitions on Cultural Safety: Chief Public Health Officer Health Professional Forum
Download in PDF format
(748 KB, 11 pages)
Organization: Public Health Agency of Canada
Date published: 2023-06-20
On this page
- Preface
- About the CPHO Health Professional Forum and Indigenous Health Sub-Group
- Continuum of cultural safety and humility
- Definitions
- Acknowledgements
Preface
For Indigenous Peoples, racism, discrimination and stigma, which contribute to the lack of culturally safe care and support services, have created significant inequities in health in comparison to non-Indigenous Canadians. These health inequities between Indigenous Peoples and non-Indigenous Canadians have only been exacerbated by the COVID-19 pandemic. Through Canada's commitment to end racism and systemic discrimination within the health system, there has been an emergence of various terms, such as cultural safety and cultural humility. These terms describe the key elements for creating an environment where Indigenous Peoples are respected, and health services are provided in an equitable and safe manner, without discrimination.
The following Common Definitions on Cultural Safety have been developed by the Chief Public Health Officer (CPHO) Health Professional Forum's (the Forum) Indigenous Health Sub-Group. They provide clarity on the meaning of these terms, and help ensure that health professionals looking to engage meaningfully in health and healthcare improvement for Indigenous Peoples are aware of appropriate terminology.
Meaningful engagement with First Nations, Inuit, and Métis must follow a distinctions-based approach and reflect the unique interests, priorities and circumstances of each People. As such, the Forum's Indigenous Health Sub-Group has engaged, and will continue to engage with First Nations, Inuit and Métis on this resource to ensure that it reflects the perspective of Indigenous Peoples and communities in Canada.
About the CPHO Health Professional Forum and Indigenous Health Sub-Group
Formed in 2018 and comprised of 19 national health organizations, the Chief Public Health Officer (CPHO) Health Professional Forum (the Forum) brings together national health organizations to collaborate and take action on public health issues of national importance. Indigenous health, including cultural competency and safety, has been recognized by the Forum as a key priority area for collaboration. The Forum's Indigenous Health Sub-Group was formed to share and build upon the work of member organizations to advance Indigenous cultural competence, awareness, safety and humility among health professionals.
CPHO Health Professional Forum members
- Association of Medical Microbiology and Infectious Diseases Canada
- Canadian Association of Social Workers
- Canadian Dental Association
- Canadian Indigenous Nurses Association
- Canadian Medical Association
- Canadian Nurses Association
- Canadian Paediatric Society
- Canadian Pharmacists Association
- Canadian Psychological Association
- Canadian Public Health Association
- College of Family Physicians of Canada
- Community Health Nurses of Canada
- HealthCareCAN
- Indigenous Physicians Association of Canada
- Infection Prevention and Control Canada
- Public Health Agency of Canada
- Public Health Physicians of Canada
- Royal College of Physicians and Surgeons of Canada
- Society of Obstetricians and Gynecologists of Canada
Indigenous Health Sub-Group members
- Assembly of First Nations
- Association of Medical Microbiology and Infectious Diseases Canada
- Canadian Indigenous Nurses Association (co-lead)
- Canadian Paediatric Society
- Canadian Public Health Association
- College of Family Physicians of Canada
- Community Health Nurses of Canada
- Health Canada
- HealthCareCAN
- Indigenous Physicians Association of Canada
- Indigenous Services Canada
- Infection Prevention and Control Canada
- Métis National Council
- National Collaborating Centre for Indigenous Health
- Public Health Agency of Canada
- Royal College of Physicians and Surgeons of Canada (co-lead)
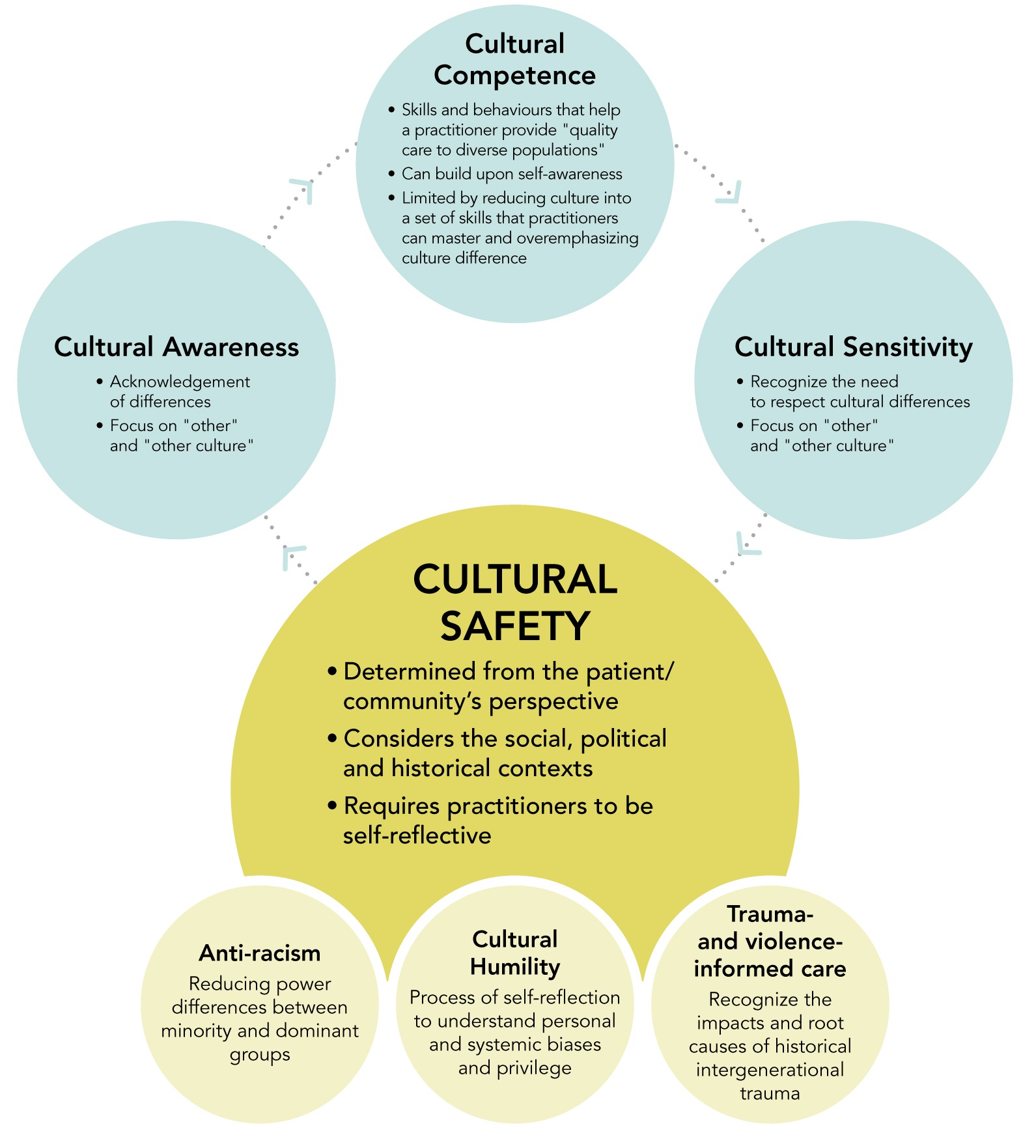
Continuum of cultural safety and humilityFootnote 1
Text description
This figure shows that cultural safety must be viewed as a continuum of knowledge, attitudes and behaviours, beginning with cultural awareness.
Cultural safety is an on-going process, one in which health professionals must continuously revisit their own knowledge, attitudes, behaviours and processes to meet the needs of Indigenous peoples.
As time progresses, this process must be continuously revisited as new understanding of what cultural safety means develops. These new developments may emerge from influences such as cultural humility, anti-racism and trauma- and violence-informed care.
All three bubbles ultimately lead to cultural safety. Cultural safety is the end-goal in this pathway, how we understand that being culturally safe is a continuous process, as new understandings of what being culturally safe means are developed. Thus, cultural safety has a different shade and larger bubble than the others do. However, it feeds back into the cycle because the learning process is ongoing.
The three bubbles of anti-racism, cultural humility and trauma- and violence-informed care are not part of the cycle. They are potential influences that change our understanding of cultural safety and hence create the cycle that is never-ending. We had them touch the bubble of cultural safety to show that they impact only this bubble.
Definitions
Cultural awareness
The acknowledgment of difference. It is the first step in understanding cultural differences and involves observing those differences. Cultural awareness focuses on the 'other' and the 'other culture.' Cultural awareness does not consider political or socio-economic influences on cultural difference, nor does it require an individual to reflect on his/her own cultural perspectives.
Source
- Canadian Indigenous Nurses Association (2013). "Cultural Safety in First Nations, Inuit and Métis Public Health"
Cultural sensitivity
Recognizing the need to respect cultural differences. Cultural sensitivity involves exhibiting "behaviours that are considered polite and respectful by the [person of the other culture]." Similar to cultural awareness, cultural sensitivity focuses on the 'other' and the 'other culture.' Cultural sensitivity also does not require an individual to reflect on his/her own culture.
Source
- Canadian Indigenous Nurses Association (2013). "Cultural Safety in First Nations, Inuit and Métis Public Health"
Cultural competency
The ability to self-reflect on one's own cultural values and how these impact the way one provides care, as well as continually learning to gain a deeper understanding of another's culture. It includes each health professional's ability to assess and respect the values, attitudes and beliefs of persons from other cultures and respond appropriately in planning, implementing, and evaluating a plan of care that incorporates health-related beliefs and cultural values, knowledge of disease incidence and prevalence, and treatment efficacy.
Source
- Canadian Nurses Association (2018). "Promoting Cultural Competence in Nursing
Cultural humility
Cultural humility is a way in which health care providers practice that enable cultural safety. It is a process of self-reflection to understand personal and systemic biases, and privilege to develop and maintain respectful processes and relationships based on mutual trust. Cultural humility involves humbly acknowledging oneself as a learner when it comes to understanding another's experience, and dismantling power imbalances.
Source
- BC First Nations Health Authority (2016). Creating a Climate for Change: Cultural Safety and Humility in Health Services for First Nations and Aboriginal Peoples in British Columbia
Cultural safety
Cultural safety is about the experience of the patient. It is an outcome based on respectful engagement that recognizes and strives to address power imbalances inherent in the healthcare system. It results in an environment free of racism and discrimination, where people feel safe when receiving health care.
Source
- BC First Nations Health Authority (2016). Creating a Climate for Change: Cultural Safety and Humility in Health Services for First Nations and Aboriginal Peoples in British Columbia
Cultural conflict
Stems from differences in beliefs and values between one culture and another. It is the result of conscious or sub-conscious imposition of one culture's beliefs and values on another culture because of an inherent belief in their superiority.
Source
- Canadian Nurses Association (2018). "Promoting Cultural Competence in Nursing
Oppression
Unearned disadvantage. Oppression is also concerned with whether a given society, economic system, or institution unjustly benefits certain groups.
Source
- Association of Medical Microbiology and Infectious Disease Canada (2019). as referenced in Peggy McIntosh (1988). "White Privilege and Male Privilege: A Personal Account of Coming to See Correspondence through Work in Women's Studies
Privilege
Unearned advantage. Privilege is concerned with whether a given society, economic system, or institution unjustly benefits certain groups.
Source
- Association of Medical Microbiology and Infectious Disease Canada (2019). as referenced in Peggy McIntosh (1988). "White Privilege and Male Privilege: A Personal Account of Coming to See Correspondence through Work in Women's Studies
Racism
Racial prejudice or discrimination. The belief that ones own race is superior to another, based specifically on ones particular racial or ethnic group.
Source
- Royal College of Physicians and Surgeons (2019). "Indigenous Health Values and Principles Statement", Second Edition.
Anti-racism
Any approach that reduces power differences by benefitting minority racial[ized] groups and/or disadvantaging dominant racial[ized] groups.
Source
- National Collaborating Centre for Indigenous Health (2013). "Understanding Racism."
Structural or systemic racism
Political, social and economic structures and institutions, where a dominant group is established and its power is reinforced through inequitable laws, policies, rules and regulations, as well as access to resources. Within these structures, stereotypes about Indigenous Peoples bring about prejudices which produces discrimination, which leads to oppression
Source
- National Collaborating Centre for Indigenous Health (2014).
- "Aboriginal Experiences with Racism and Its Impacts."
Trauma-informed care
A trauma informed care provider understands the impacts and root causes of historical intergenerational trauma (i.e. residential school experiences), recognizes the symptoms of trauma in patients and integrates this knowledge into policies, procedures, practices and settings; "trauma informed care is their commitment to provide services in a manner that is welcoming and appropriate to the special needs of those affected by trauma."
Source
- National Collaborating Centre for Indigenous Health (2017). "What's New is Really Old: Trauma Informed Health Practices Through an Understanding of Historic Trauma" & Royal College of Physicians and Surgeons "Indigenous Health Primer (2019)
Stigma
Stigma is comprised of negative, unfounded attitudes or beliefs (prejudice) towards an individual, based on their real or perceived membership of a stigmatized group. Stigma is often accompanied by negative action/behaviours (discrimination).
Source
- Government of Canada (2019).
- "Stigma: Why Words Matter" (2019)
Acknowledgements
This document was developed in collaboration with members of the CPHO Health Professional Forum:
- Association of Medical Microbiology and Infectious Diseases Canada
- Canadian Association of Social Workers
- Canadian Dental Association
- Canadian Geriatrics Society
- Canadian Indigenous Nurses Association
- Canadian Medical Association Canadian Nurses Association
- Canadian Paediatric Society
- Canadian Pharmacists Association
- Canadian Psychological Association
- Canadian Public Health Association
- College of Family Physicians of Canada
- Community Health Nurses of Canada
- HealthCareCAN
- Indigenous Physicians Association of Canada
- Infection Prevention and Control Canada
- Public Health Agency of Canada
- Public Health Physicians of Canada
- Royal College of Physicians and Surgeons of Canada
- Society of Obstetricians and Gynecologists of Canada
In addition, we gratefully acknowledge the leadership and contributions of the Indigenous Health Sub-Group of the CPHO Health Professional Forum, which, in addition to Forum members, includes the following organizations:
- Assembly of First Nations
- Indigenous Services Canada
- Métis National Council
- National Collaborating Centre for Indigenous Health
- Pauktuutit Inuit Women of Canada
Footnotes
- Footnote 1
-
This graphic has been adapted from Baba, L. (2013). Cultural safety in First Nations, Inuit and Métis public health: Environmental scan of cultural competency and safety in education, training and health services. Prince George, British Columbia, Canada: National Collaborating Centre for Indigenous Health. BC First Nations Health Authority. "Cultural Humility." 2019. Retrieved from https://www.fnha.ca/wellness/wellness-and-the-first-nations-health-authority/cultural-safety-and-humility; Brascoupé, S. and Waters, C. (2009). Cultural safety: Exploring the applicability of the concept of cultural safety to Aboriginal health and community wellness. Journal of Aboriginal Health. Retrieved from www.researchgate.net/
