What we heard: Indigenous Peoples and COVID-19: Public Health Agency of Canada’s companion report
Download in PDF format
(2.49 MB, 32 pages)
Organization: Public Health Agency of Canada
Published: 2021-03-03
February 2021
This report was led by the Waakebiness-Bryce Institute for Indigenous Health (WBIIH) at the Dalla Lana School of Public Health, University of Toronto and submitted to the Public Health Agency of Canada.
Table of contents
Acknowledgements
We want to acknowledge and thank Elder Claudette Commanda, Elder Julie Ivalu, and Knowledge Keeper Clayton Shirt for providing traditional openings, closings, and reflections during the August 10th and September 2nd, 2020 community engagement sessions to ensure that our conversations and work was grounded and done in a good way. Elder Claudette, Elder Julie, and Knowledge Keeper Clayton brought knowledge and spirit to this important work.
We also want to acknowledge the helpers: Adriana Gonzalez, Devon Bowyer, Lauren Yates, and Lisa Howard of the 2019-2021 MPH-Indigenous Health program at the Dalla Lana School of Public Health as well as Andrea Bowra, Denise Webb, Claire Hiscock, Harrison Mair, Sharon Tan, and Victoria Pringle from the Waakebiness-Bryce Institute for Indigenous Health for note taking and facilitating the community engagement sessions on September 2nd, 2020. We want to extend a further acknowledgement to Andrea Bowra and Sharon Tan for their copy-editing assistance for this report.
We wanted to thank the Office of the Chief Public Health Officer of Canada (CPHO) for inviting us to be a part of this important project.
Lastly, we would like to extend our gratitude to the First Nations, Inuit, and Métis community members who shared their knowledge and experiences with us, and those who have taken time to correspond and submit documentation at the consultations in August and September, and throughout the Fall and Winter 2020/2021 as the report was being finalized.
We hope that this report is an accurate reflection of what Indigenous community members provided. Out of respect for privacy, this report does not identify individual speakers. It is our hope that the voices and experiences of all First Nations, Inuit and Métis individuals who participated in the community engagement process are heard and reflected in this report. We also hope this report can support the Chief Public Health Officer of Canada, Dr. Teresa Tam, her team at the Public Health Agency of Canada, and Indigenous community members in the work that is to come.
Introduction/Preface
This report is to complement the CPHO’s Annual Report on the State of Public Health in Canada 2020, “From Risk to Resilience: An equity approach to COVID-19”. During late February 2020, COVID-19 became a growing concern in Canada with reported cases in multiple regions. COVID-19 has changed the way we live, work, and socialize. Dr. Mashford-Pringle and the research team were asked to author a companion report as a reflection of what was heard during the August and September engagement sessions.
Situating ourselves
This report is a summary of what we heard from Indigenous community members. The authors of this report worked to summarize and contextualize the information we were provided. The authors are:
- Angela Mashford-Pringle: I am from Timiskaming First Nation (Bear Clan), but I was born and raised in Toronto. I come to this work as an Anishinawbe scholar.
- Christine Skura: I am Métis. I was born and raised in the Greater Toronto Area. I am a registered nurse, and currently taking my Master of Public Health in Indigenous Health at the University of Toronto.
- Sterling Stutz: I am a settler with Ashkenazi Jewish and Irish/English ancestry living in Toronto and am completing my Master of Public Health in Indigenous Health at the Dalla Lana School of Public Health at the University of Toronto.
- Thilaxcy Yohathasan: I am a Tamil settler, but I was born and raised in the Greater Toronto Area. I am currently working towards my Master of Public Health in Indigenous Health at the Dalla Lana School of Public Health at the University of Toronto.
Background
The rapid spread of the SARS-CoV-2 globally and in Canada has shown a glimpse of its potential to leave an extraordinary shock on our systems and those most vulnerable. Without the prioritization of equitable access to basic needs and resources to communities at risk, the fast spread of the virus will make it difficult for many to promptly and properly respond to their needs. For many years, Indigenous communities have experienced social and economic inequalities due to colonialism and face health inequities such as a high burden of cardiovascular disease, food insecurity, lack of clean water, etc. These circumstances leave many communities disproportionately unprepared for the COVID-19 pandemic.
Maunula (2013) argued First Nations communities cannot fully implement public health behaviours like frequent hand washing due to concerns about the availability of clean water, nor can they physically distance or self-isolate as houses are overcrowded and there are insufficient community buildings to house those who are infected (like a makeshift hospital). Further, Maunula argued that the inequalities that First Nations people face every day are amplified in emergency, which could lead to a higher risk of the number of cases and deaths due to the pandemic.
Charania (2011) studied three James Bay communities (Fort Albany, Attawapiskat, Kashechewan) for their Master’s thesis. Charania highlighted that during interviews with community members and band leadership, they stated social factors like overcrowding, inability to isolate, inability to follow public health messaging like frequent handwashing were extremely difficult to do as resources were unavailable. This is echoed throughout the literature (Boggild et al., 2011; Charania and Tsuji, 2011; O'Sullivan and Bourgoin, 2010; White, Murphy, and Spence, 2012); clean and usable water, adequate housing without mold or overcrowding, and health human resources sufficient for the community size as well as access to specialists and specialized equipment are necessary for daily living, but extremely important when in a pandemic situation.
The need to increase preparedness within Indigenous communities has been recognized with recommendations provided in plans such as the Canadian Pandemic Influenza Plan for the Health Sector (CPIPHS) and First Nations and Inuit Health Branch - Ontario Region Pandemic Influenza Plan (FNIHB-ORPIP). The recommendations included additional supplies and services in times without crises/infectious diseases outbreaks, in order to be prepared during an emergency. An emergency fund should be established federally, and possibly through regional and provincial/territorial health authorities or at the local First Nation level. Indigenous communities require additional healthcare workforce, with the means to hire and train Indigenous healthcare providers who are supported to remain in their communities and are recognized for their expertise and professional skills. Furthermore, an interdisciplinary team of allied healthcare professionals (specialized physicians, additional nurses, preventative health, public health, and others) should be deployed to communities who request these services in an emergency to support through the provision of immediate physical health care as well as prevention and mental/emotional well-being. There should be alternate care sites established or easily erected/commandeered with federal funds to support conversion or upgrades necessary for the care and treatment of Indigenous Peoples. In order to address longstanding concerns regarding food insecurity, a food supply plan should be developed and upgraded frequently; and, working with government bureaucrats, housing improvements and expansions as needed in each First Nation should be a priority to reduce homelessness and overcrowding as one of the mitigating factors of disease transmission.
Some of the key barriers or challenges that were consistently addressed in the literature were focused and clear communications to ensure that messaging is not contradicting governmental guidelines or is provided from many sources as well as having the interdisciplinary team of front-line responders (doctors, nurses, police, leadership, etc.) work together to limit community spread of fear, rumours and misinformation (Charania, 2011; Maunula, 2013; Public Health Agency of Canada, 2006a, 2006b; Sistovaris et al., 2020). It is a part of communications, however the importance of who, how and where messaging is provided helps to diminish misleading or incorrect information quickly.
Due to historical and ongoing inaction on the part of government officials and the ongoing impacts of colonization, there are Indigenous communities (First Nations, Inuit, or Métis) concerned the government will not hear or address the strengths and challenges they are facing in this ever-shifting pandemic (Malloy, 2001; Royal Commission on Aboriginal Peoples, 1996; Truth and Reconciliation Commission of Canada, 2015). True Indigenous relationship building is required. A relationship must be reciprocal and exists beyond “another consultation or engagement” which is limited by time and government priorities.
Terminology
The terminology associated with Indigenous Peoples has changed several times over the past 150 years. Table 1 explains the terminology used within this report.
Terminology used in this report
- Indigenous Peoples
- The term ‘Indigenous Peoples’ refers to the original people of any land around the world. Within the context of this report, the term ‘Indigenous Peoples’ refers to individuals who are First Nations, Inuit and Métis.
- First Nation(s)
- Legally defined under the Indian Act (1876) to describe the First Peoples in North America who are living in what is now known as Canada.
- Inuit
- Circumpolar Indigenous peoples who have a distinct language, culture and traditions. Canadian Inuit live primarily in Inuit Nunangat, which is made up of four regions: Inuvialuit in the Northwest Territories, Nunavut, Nunavik in Northern Quebec, and Nunatsiavut in Northern Labrador.
- Métis
- “Métis means a person who self-identifies as Métis, is distinct from other Aboriginal peoples, is of historic Métis Nation Ancestry and who is accepted by the Métis Nation” (Metis Nation of Canada, 2017).
- Community(s)
- Lands held for First Nations and Inuit to use and benefit from according to the Indian Act (2019).
- Rural
- Communities that are those with a population of less than 30,000 and are more than 30 minutes away in travel time from a community with a population of more than 30,000 (Ontario Ministry of Health and Long-Term Care, 2011).
- Isolated
- Geographic area with scheduled flights and telephone services but does not have year-round road access (Public Health Agency of Canada, 2009).
- Remote
- Communities located over 350 km from the nearest service centre and may or may not have year-round road access or which rely on third parties for transportation to large centres (Public Health Agency of Canada, 2009).
- Urban Indigenous Peoples
- Refers to First Nations, Inuit, and Métis peoples who reside in cities, towns and rural areas and recognizes diversity between and within Indigenous communities (Ontario Ministry of Indigenous Affairs, 2019).
As authors of this report, we recognize that language is fluid and can change over time. We also acknowledge that many Indigenous Peoples self-identify and may not use language or definitions identified above.
Methodology
As a result of the COVID-19 pandemic, the method for producing this report and holding community engagements was adapted to consist of entirely remote/virtual communication. The adaptation resulted in virtual recruitment of Indigenous community members and virtual talking circles which was specifically used for the second discussion. The community voices reflected are those who voluntarily responded to the request for participants and contributed to either one of the online discussions or electronically submitted information. Participants from Indigenous organizations and communities were asked to submit any information (e.g., flyers, social media, documents, etc.) through email to the Office of the CPHO and/or Dr. Mashford-Pringle.
The August 10th, 2020 virtual discussion was opened by First Nations Elder Claudette Commanda and consisted of two presentations (See Appendix C):
- Dr. Theresa Tam presented on the current state of COVID-19 in Canada
- Dr. Margo Greenwood presented on strengthening structural inequities after COVID-19
The remainder of the time (approximately one hour) was allocated for participants to speak about their community and/or organization responses to COVID-19. Participants from First Nations, Inuit, and Métis communities were present for these discussions.
The September 2nd virtual discussion utilized a modified virtual talking circle to gather data and answer three pertinent questions after traditional openings by Inuit Elder Julie Ivalu and First Nations Knowledge Keeper Clayton Shirt:
- What makes you proud about your community’s response to the COVID-19 pandemic?
- What has helped keep your community strong when responding to COVID-19?
- What changes have you made that could be taken up by other Indigenous communities?
During the approximately three hour Zoom call, participants moved into six virtual talking circles and consisted of 4 to 8 participants each. The Research Team Facilitator asked each question and allowed all participants to speak and provide at least two rounds of answers before moving on to the next question. The virtual talking circle concluded with a traditional closing. Participants were reminded to email the Research Team with any additional materials that they wished to be included in the report. Detailed notes were taken by the Research Team during the virtual talking circles. To honour Indigenous epistemologies and methodologies, we offered tobacco and invited two Elders and a Knowledge Keeper to provide opening and closing prayers at the discussions to ensure we started and ended in a good way.
After the discussions and submissions were sent, the Research Team coded the notes and analysed the themes that emerged. The thematic analysis was sent to all the participants on both calls for their feedback about the themes. After receiving participants’ feedback on the thematic analysis, the Research Team wrote the Companion Report to reflect on the stories and themes. Participants were provided the full Companion Report for further feedback before the report was submitted to the Public Health Agency of Canada.
Key themes
The following sections are the key themes and input that was provided by the participants of both online discussions as well as the submissions sent to the Research Team.
Sovereignty
Sovereignty is the inherent rights and freedoms assigned to Indigenous Peoples, which include self-determination (the right, power, and authority) to continue to live by Indigenous ways of being and knowing.
Community-led shutdowns
Some communities were concerned with decisions made by external governments (e.g., federal, provincial/territorial and/or municipal) as they impact the health and well-being of Indigenous people. However, by-laws or other policy documents were already in place or revised at the First Nations level to assist with emergency preparedness. Thus, many Indigenous communities had locked down their borders as sovereign authorities, in some cases ahead of regional, provincial or territorial orders. Some communities felt they could take control and keep outside peoples from entering their communities to protect their residents from COVID-19. An Inuk participant spoke to the quick community response to shut down which was a point of pride to that participant. As such, some participants noted that this autonomy and sovereignty needs to continue after the pandemic in more substantial ways.
Some rural First Nations communities, acting as sovereign authorities, had their own local police services to prevent people from entering the community if they were not members. Other communities partnered with their local hospitals, police stations, and community organizations to lock down the community. Some communities were also able to hire a public health contact tracer to monitor those who travelled into the community as well as implementing a mandatory 14-day quarantine policy for visitors.
In some regions in Canada, Indigenous communities denied non-residents entry into their communities by using physical barricades to control road access. Some First Nations participants expressed that the federal and/or provincial/territorial governments did not adequately support or respect their community-specific barriers. Conversely, some provincial governments stated that First Nations communities could still be in lockdown and that non-residents would be denied entry. However, in these situations, provincial governments did not assist in enforcing barricades or non-entry orders. This resulted in instances where non-Indigenous people attempted to force their way into First Nations communities, like in the case of the Beausoliel First Nation. One participant said, “Proud to say, that we kept people outside of the community outside the FN. Included a checkpoint to manage people entering the community. Happy to do it to help the community. Saying no to people in Toronto who take advantage of the shorelines was very important.”
Some First Nations communities are located close to the border to the United States. This was brought forward by participants in British Columbia and Ontario. Other Indigenous Peoples live in cities near border crossings that have trucks and essential travelers from areas with high COVID-19 rates being allowed to enter Canada. Some Indigenous communities are at risk of multiple entries by non-community members which increases the risk of COVID-19 transmission and outbreaks. Strong community leadership about inherent rights of Indigenous communities in protecting their lands was key to reducing or eliminating non-community members and preventing the transmission of COVID-19. However, some participants stated the federal government should be discussing border openings with all communities near these border crossings before reopening as this could put lives at risk from entering or trespassing.
Need for Indigenous Engagement in Decision-making
Some First Nations communities were concerned with the lack of consultation about the potential re-opening of the international borders (e.g., United States/Canada or airports) as it is a matter beyond their jurisdiction, yet Indigenous Peoples and communities will be affected by Canadian policy regarding border re-opening.
Community members shared that sovereignty is applied when they have the capacity to govern the public health of members within their communities and have decision-making ability to develop their own plans and protocols. Support can come from provincial and territorial governments if it is requested by the community. In the current context of COVID-19, provincial and territorial governments should be working collaboratively with communities to partner on plans for re-opening of borders, schools, and businesses.
However, some participants felt they should not be expected to follow provincial guidelines (e.g., provincial timelines on phased re-opening). Instead, communities should have the self-determination to decide when and how their schools would re-open, and how to have social or physical distanced visits and ceremonies. As indicated in discussions and submissions, Indigenous communities developed, revised, implemented, and enforced pandemic plans which incorporated current messaging from the Public Health Agency of Canada at the federal level, as well as provincial and territorial messaging.
Kinship
The Indigenous ancestors “saw a kinship between plants, insects, birds, animals, fish and human beings” (Johnston, 2003, p. vii) or all things in the universe as “All My Relations” or “All in Creation” (Mohawk, 2008). “This was a relationship model, a kincentric model, one in which we are all equal, but we have different jobs to do here on earth” (Martinez, Salmón, and Nelson, 2008, p. 90).
From a strengths-based approach, Indigenous community members and organizations relayed how they delivered foods, medicines and supplies to Elders and community members (rural, remote, and urban). There was discussion about youth resiliency and how they were engaged in activities during the first wave (February 2020 to September 2020) of the COVID-19 pandemic.
Supporting seniors and Elders
Elders are respected leaders in the community and support the transmission of tradition, culture, language, and knowledge. Not all Indigenous senior community members are Elders. Elders share ancestral knowledge and provide guidance on personal and community issues. In many cases, Elders are the holders of knowledge that needs to be passed along to future generations. Traditional Knowledge Keepers are leaders who possess talents or knowledge that they pass onto future generations. Children and youth identify Elders and Knowledge Keepers as significant figures in helping them understand their culture and the loss of an Elder or Knowledge Keeper symbolizes a loss in language, wisdom, and knowledge.
In urban, rural and remote areas, most communities worked collaboratively to ensure that Elders were given meals and protected or isolated from individuals who may have been in close contact with someone who has COVID-19. Elders comprise a small proportion of Indigenous populations and were heavily protected during isolation stages of COVID-19. In many First Nations communities, Elders living in congregate settings were not allowed to be visited due to their increased risk of severe health complications from COVID-19. In many cases, virtual and remote visits were used to compensate for this. Groceries and meals were also delivered daily.
Like the protection of Elders, Knowledge Keepers were also protected to ensure cultural continuity and protection. Some First Nations participants also indicated that Clan Mothers and/or Grandmothers had the ability to help communities to stay focused. They are also important as they are the culture keepers of traditional foods, medicines and ways of being. As such, some participants stated that some Indigenous communities worked with Elders, Knowledge Keepers and other culture practitioners to plant and harvest medicines and foods for traditional healing and medicines.
In some cases, community members expressed that Elders were fearful that they may be removed from the community to enter a hospital or that one would never be able to come home. Due to this, some Elders feared speaking about their health as they did not want to be relocated. Furthermore, a tension was identified by community members between the need to protect Elders from risk of COVID-19 transmission and the need to continue to visit and protect the mental, emotional, and spiritual health and well-being of Elders. One participant shared that, “Elders were sequestered, dampening their spirits...people were saying that’s not our way, we don’t do that to our Elders”. This highlights the important tension of how to respect the free will of Elders while also working alongside them and their caregivers to ensure a safe environment during the pandemic. Yet, many Elders experienced increased social isolation as communities worked to protect them from virus transmission, but it is not yet clear about the impacts of socially isolating Elders, but multiple participants expressed concern. Despite challenges, community members expressed pride in their innovative solutions to maintain social connections with Elders by using technology, such as electronic tablets and Zoom calls.
Youth
Youth are important part of Indigenous communities and represent the future. Indigenous youth have and continue to demonstrate a strong sense of leadership, creativity, and resilience in response to the COVID-19 pandemic. In some communities, youth have led engagement activities to support other children and youth while maintaining physical distancing protocols. Some participants explained that youth used social media platforms such as Facebook to attend to the social health of family and community members. In some instances, youth facilitated education and discussion with social media posts. These initiatives were connected back to Indigenous ways of knowing such as through human, animal, and land characters and illustrations according to a few participants. COVID-19 has also led to a lack of employment opportunities for high school and university students according to a few participants. For example, employment opportunities or school curriculums and teachings expect students to work from home. However, there are barriers associated with accessing these opportunities such individuals being unable to access devices, social media, or the Internet.
Food security
Discussions and submissions showed how Indigenous Peoples bonded together and found ways to support each other through the hardships of the first wave of the COVID-19 pandemic. Some examples include sharing supplies or food (traditional and market-based). Inuit participants expressed that communities worked together to ensure that no one was going hungry and that Elders, families, and single parents were given enough food and supplies. There were some Inuit and First Nations communities that assisted community members to return to the land to avoid being in close spaces with each other. In the Northwest Territories, there was assistance given to Indigenous Peoples to be on the land during the first wave; some participants stated that being on the land assisted with physical distancing as well as being able to harvest traditional foods. Some remote First Nations communities created food delivery services to alleviate the realities of food insecurity during COVID-19 with some communities delivering health supplies such as masks and hand sanitizer. Meals contained fruits and vegetables that were delivered in large quantities to families. In some cases, communities grew their own produce and ensured there was a supply of wild rice and traditional meat/country food, as people grew to be less reliant on outside sources.
Community members emphasized the importance of local access to nutritional food and raised concerns about the increased costs of accessing food. These rising prices are because of economic impacts of the pandemic such as increased transportation limitations because of lockdowns. One participant remarked, “administratively, we totally had to re-engineer how we did things. We had to be less reliant on outside sources. We need to make sure we have a supply of wild rice and meat. We need to grow our own produce and have our own food markets. However, sharing traditional food is difficult to do while acting in accordance with physical distancing measures. Also looking at how we manage our human capital - we expect people to come to work if they’re not feeling well and we need to examine different ways to work.”
Tradition
Some First Nations participants reported using strengths-based approaches to the pandemic such as by including humour, fun, and games. For example, one community opened their school grounds and sectioned off areas so people could take turns using the land to gather in small groups to de-stress. It is important to highlight that the communities organized and implemented these opportunities to have fun and be creative; for Indigenous Peoples by Indigenous Peoples. Some First Nation communities implemented physically distanced activities like bingo and dance challenges. In some communities, they created collaborative social media projects such as the ‘Pass the brush challenge’ featuring community members in regalia. Virtual Pow Wows were held online, giving individuals the chance to connect virtually despite the physical distancing requirements.
Indigenous participants spoke about the gift of time to spend with their families. Prior to COVID-19, “families spent as little as 3 to 4 hours a day together with many competing priorities” according to one participant. With the lockdown and subsequent changes in society, families have been able to spend much more time together. Some Indigenous communities helped people to (re)connect with the land in old and new ways like gardens, ceremonies, and traditional teachings. One participant said, “we went back to the language, and started to communicate with the community and had ceremony. We went back to our traditional teachings, despite the struggles and addictions.”
Physical distancing
Indigenous communities and nations are kinship-oriented which presents difficulties for following the public health guidelines of physical distancing and limiting close contact to one’s household and/or immediate family. Many participants spoke to how physical distancing within households would “be extremely difficult or… impossible.” For some Indigenous Peoples, they lacked the space needed to physical distance or isolate within their homes or in their community (e.g., urban areas, overcrowded homes). Physical distancing impacted First Nations, Inuit and Métis as they could not gather or hold ceremonies as they had prior to COVID-19. This meant that they could not participate in activities with physical distancing and may have needed to choose between adhering to public health guidelines and spending time with their extended family and cultural practices. These conditions are harmful as well for Indigenous Peoples in urban spaces who experience high rates of homelessness. In some First Nations and Inuit homes, overcrowding leads to shift sleeping or inaccessibility of bathroom facilities that increase one’s risk of COVID-19. Participants expressed concerns that if a member of the household did contract COVID-19, there would not be enough space or resources to isolate them from the rest of the household.
Mental health
Connecting with community
Some participants shared that connecting with others helped staff, adults, youth, and children build a connectedness that included physical, cultural or spiritual connections. By finding this common ground, communities, whether virtual or in close proximity, were able to support each other in many different ways; this included sharing food/stories and online/physically distanced organized activities. In addition, when First Nations, Inuit and Métis youth can connect with land, language, family and cultural ways of being, it has had positive impacts on Indigenous youth now, and likely in the future as well. A participant on the September 2nd call shared, “When you love and care for one another, great things can happen. People should be putting money to food and mental health services. I hope the government continues to put money into these services even after COVID”.
Implications
Participants expressed concern for the mental and emotional well-being of community members. Many participants stated that Indigenous Peoples may be experiencing increased challenges in accessing cultural practices due to public health protocols, lack of ability to travel to communities due to lockdown measures, increased fear/concern surrounding contracting the virus and the shutdown of recreational activities such as sports, entertainment, cultural gatherings, and family vacations. Close living quarters also impacted mental health, especially in cases of unhealthy emotional and physical situations for women, children, and LGBTQ2S+ peoples as a non-exhaustive list. Indigenous Peoples experiencing mental health distress are at increased risk of experiencing incarceration or suicide.
While many Indigenous communities and organizations have tried to reduce the isolation and loneliness that individuals may feel, some Indigenous communities have experienced a marked increase in both suicide deaths and attempts since the beginning of the COVID-19 pandemic. “People are being cut off from their cultural practices and, if you lived off reserve in the first few months, you couldn’t go back, so there were people floating without their support systems”, as noted by a participant on September 2nd call. Some Métis and First Nations participants created new support networks with people online or in close proximity to them if they were in the city. This helped to improve people’s outlook on COVID-19 and helped those struggling. Yet, participants expressed concern about the potential consequences of the lack of employment opportunities and increased isolation on youth including increased fear, depression, and considerations of suicide.
Community support and funding
Participants shared that they did not see adequate mental health related considerations in the federal and/or provincial/territorial COVID-19 planning in addition to previous planning that existed ahead of the pandemic. While some participants noted increasing availability and funding of community support services as a crucial step and it is acutely important in the context of COVID-19 where the pandemic is taxing existing resources and services beyond reasonable limits. Some participants expressed difficulty in accessing needed support due to lengthy waitlist soft services which may also affect rural, remote, and isolated communities over the long-term.
Historical trauma
Indigenous Peoples have and continue to experience inter- and intra-generational traumas, which are re-lived/experienced by Indigenous Peoples across Canada because of government policies and practices rooted in colonization. For example, some First Nations participants expressed that the lockdown was similar to the pass system that was in place for decades in Canada. Lockdown did not allow Indigenous People to move about or see people, which is reminiscent of how First Nations peoples needed permission from the Indian Agent to leave the reserve. Some public health messaging also urged individuals to stop taking part in ceremonies because of uncertainty of how COVID-19 was transmitted culminating in a consequence whereby the government is dictating to Indigenous Peoples when they can access ceremony.
Substance use
The Canada Emergency Response Benefit (CERB) distributed by the federal government aimed to help individuals manage financial consequences of the lockdown. It has been extremely necessary and beneficial for many people. Multiple participants brought forward concerns around some individuals experiencing addiction who used the CERB to purchase substances (e.g., drugs and/or alcohol). Both participants and the research team believe this merits being investigated further to mitigate increased stigmatization of substance use and income supports. Resoundingly, participants spoke to the positive benefits of the CERB which provided needed income support to families; many participants stated that CERB allowed them to feed themselves and their families. Some participants explained that their communities are experiencing a doubling of opioid-related and fentanyl-related overdoses. Some participants spoke to the damaging impacts of substance use and mental health concerns on cultural traditions and kinship. One participant stated, “BC is suffering from COVID and opioid crisis, over 170 deaths a month since the opioid crisis, this was a crisis before COVID.” Another participant said “And yes, we had our problems, we became aware of who was selling drugs, addiction to drugs, gambling. We were able to take a step back to see the real challenges of our community. We had to be a lifeline to those who were having challenges in the community. When you love and care for one another, great things can happen.”
Some participants shared that as Indigenous communities entered lockdown, some residents within their communities experienced withdrawal from opioids or other drugs/alcohol as travel to/from remote communities became more difficult, which impacted the drug supply making it to community. Some Indigenous communities were able to increase the availability of drug/alcohol treatment programs and services including naloxone kits. Some participants relayed that increased funding for mental health and addictions is necessary especially during COVID-19.
Community leadership and preparedness
Resiliency
Indigenous communities swiftly took control and worked collaboratively, as is traditionally done in times of crisis. Communities and community leaders were resourceful in finding innovative ways to utilize the on-hand resources to keep community members safe, calm, and protected from COVID-19 and its subsequent impacts on food insecurity, isolation, and depression. One participant said, “The Inuit community really tried to make sure the community was not hungry. The community tried to inform themselves of what is happening about the pandemic. Very proud of how the community is taking care of Elder, families, and single parents.” Another participant explained that they provided personal protective equipment (PPE) and nutritional hampers to community, giving access to more food so community members didn’t have leave their home, and “tried to improve programming to keep families busy and safe, able to provide COVID-19 testing for anyone that lives in the territory. Community has come together; people are stepping up doing anything that they can.”
Pandemic preparedness was diverse across communities. Many participants identified that experiences with past pandemics have been a source of resiliency in their communities. There were lessons learned from the past pandemics which Indigenous communities have been subject to (e.g., H1N1, Smallpox, SARS-1, Spanish Flu). The resiliency of Indigenous Peoples is a source of pride and was honoured by many participants. The power of resiliency has led to successful leadership in Indigenous communities and organizations. Leadership was fundamental for delegating funding and services to First Nations, Inuit, and Métis communities. Some organizations and communities were able to adapt pre-existing emergency plans in order to respond to the COVID-19 pandemic.
Participants expressed that some communities have needed to manage without supports such as: stable sourcing for PPE , emergency management training, or fully developed pandemic preparedness plans. Despite the release of funding to support communities in response to COVID-19, many needed to persevere with limited support from federal, provincial/territorial, or municipal governments.
A greater investment and dedication to community-specific pandemic and emergency preparedness training and planning is needed, especially for remote and rural Indigenous communities. Some participants spoke of the decrease in funding over the years that Indigenous communities rely upon for public health planning, despite the need to increase funding to address this gap, which would include pandemic planning and emergency preparedness.
Knowledge exchange
Some participants noted that COVID-19 brought about “new and wonderful collaborative working relationships” with different sectors who may not have worked as closely before. This includes collaborations between sectors such as health social services, and housing. Some participants noted that cross-community collaborations improved emergency response plans by helping overworked and understaffed communities. For some First Nations communities, working collaboratively and effectively with other Indigenous groups or organizations helped to foster long-term relationships, which will likely continue after COVID-19.
A First Nations participant noted that Hereditary Chiefs and traditional governance structures are available for support and consultation in many communities but are not, from their perspective, included in partnerships and communication with government as most government processes involve collaboration with elected band councils and national organizations. Participants expressed that engaging all community members and levels of governance is necessary to create and implement effective emergency response plans.
Community members of a northern First Nation community expressed that their community was able to effectively collaborate with relevant government bodies. This included the co-development of a COVID-19 action plan to manage outbreaks and the sourcing of necessary resources for the community. One First Nation community created a new project manager position responsible for outreach to other communities in order to gain a sense of best practices for developing their emergency response plan. It is important to highlight that not all communities have the resources and capacity to support a paid position such as this, which some participants highlighted. One participant stated that any community requiring resources to support similar activities should be supported to achieve the effective development and implementation of emergency response plans.
Communications
Many participants expressed their pride for their communities’ and leaders' swift transition from in-person to online platforms in order to maintain consistent health communications. Booklets, flyers, videos, and other content was created by community members to disseminate the most up-to-date public health messaging. Communication outputs include books titled, “Skoden COVID” and “Surviving and Thriving”. These messages were translated into Indigenous languages, which addresses language barriers and increases accessibility to public health education for individuals who are not fluent in English. These culturally appropriate communication products are needed for all community members to fully understand public health messages on COVID-19, which has the potential to ultimately reduce COVID-19 infection rates according to some participants.
Innovation and program delivery
COVID-19 has demonstrated the need to redesign programs to ensure sustainability amidst crises including sudden outbreaks of infectious diseases and changes in environmental conditions. Communities found that lockdown measures brought new challenges such as increased responsibilities to provide services to community members with health conditions and challenges regarding the arrival and distribution of PPE, food, and other supplies. Participants expressed that many of their communities worked diligently to ensure clients experienced little to no interruption in accessing health programs and services. Communities rapidly implemented changes in programming such as transitioning programs/services to online or telephone platforms. For example, while under lockdown measures, some communities established a flag system that households could use to indicate their needs by raising a flag outside an individual’s home. Under the program, if a household displayed a blue flag, it communicated that they were experiencing a water shortage. Some communities instituted local patrols who travelled throughout the community to distribute goods and services to those who required them. In some communities, this program has continued after lockdown measures have been lifted due to its success.
Childcare, childhood development, and education are areas that some communities are examining to ensure that sustainable changes are implemented. First Nations and Métis participants expressed concern regarding the cost of childcare and care for children with specialized/individualized needs. Participants shared that, in many cases, community members used funds from their own pockets to financially support and deliver childcare and special needs services during the COVID-19 pandemic, as these services were not covered in COVID-19 related government funding. The additional cost for communities to finance these services may impact their ability to provide affordable services to community members as the communities move their budgets around.
Some participants addressed the need to create programming that is sustainable beyond COVID-19 as community members will continue to be impacted by long-term health implications. In particular, programs and services will need to remain responsive and adaptive to changing circumstances. Participants stated that although communities were generally able to adapt to the immediate consequences, long-term implementation strategies have not been discussed or are in preliminary stages.
Public health infrastructure
Some First Nations participants stated that public health staff were moved and/or redeployed to other regions based on the instructions received from federal and provincial/territorial governments. This reduced the capacity for community leaders to effectively develop pandemic response plans during the course of the first wave of the pandemic. One participant from a remote First Nations community highlighted that there is no current public health structure to support an emergency response to the pandemic in their community. Many participants from different communities expressed that the chronic lack of financial investment in Indigenous communities has restricted the potential of an effective community-led public health structure and response to the pandemic. Many communities and organizations are “overworked and under-resourced”, impacting their ability to respond adequately to the effects of COVID-19. It is critical for government bodies to invest in pandemic planning for Indigenous communities that incorporates a culturally safe definition of health by focusing on the physical, mental, spiritual, and emotional aspects of community members.
Personal protective equipment was identified as essential by public health authorities for reducing the risk and spread of COVID-19. Getting PPE from the public health authority was difficult for some communities due to confusion around how to correctly use the PPE, locating the personnel responsible for PPE distribution, and the transfer of responsibility to some provincial governments. Some participants said they had difficulty determining who to contact or where to look for PPE during the first wave. In urban settings, it was difficult for some Indigenous organizations to access PPE as governments did not prioritize distributing to these organizations and regions. Some First Nations communities resorted to sourcing PPE from the United States and some Métis communities expressed difficulty in accessing PPE which resulted in the community needing to source PPE privately to ensure access for their community members. Access to COVID-19 testing kits was also difficult for some communities though some communities were successful in organizing local in-home testing once testing kits were received.
Mistrust
Most participants stated that governments at all levels have broken promises and dismissed the rights and freedoms of Indigenous Peoples across Canada. This has resulted in a relationship of deep mistrust felt by many Indigenous Peoples towards governments, political leaders, and key policy actors responsible for institutional structures including but not limited to health, education, justice, and politics. Many participants stated that government bodies need to engage in true relationship building with various levels instead of connecting with only high-level organizations (e.g., Assembly of First Nations, and Inuit Tapiriit Kanatami Métis National Council). Collaboration must also include local and regional Indigenous communities and occur over time to build meaningful relationships that span across present and future generations.
Participants stated that they were concerned with who will have access to the content from the calls. They also inquired if and how sharing their experiences and perspectives will truly change the fractured relationship many have with various levels of government as well as with everyday Canadians. Some Indigenous organizations and communities shared that they feel that all levels of government must build reciprocal relationships with Indigenous Peoples, communities, organizations, and nations, which has not been adequately done in the past. However, some participants noted that there are some relationships, existing in their infancy, that are taking on the spirit of reciprocity.
Additionally, some participants stated that there is mistrust at the community-level for government representatives and authorities to enforce laws or public health orders. Participants noted that systemic racism has also made Indigenous people wary of accessing health care or interacting with police as these entities are often governed by non-Indigenous people and have previously and continue to mistreat and traumatize Indigenous people before and during COVID-19. Participants highlighted during the first wave of the COVID-19 pandemic, there have been more than four Indigenous people killed when police have been involved (e.g., wellness checks, routine traffic stops, etc.). Many participants stated that COVID-19 has spotlighted instances of systemic racism across Canada, demonstrating the reluctance for Indigenous Peoples to engage with non-Indigenous authorities.
Structural inequalities
Resoundingly, participants on both calls spoke to the many structural inequalities that have and continue to hinder the well-being of Indigenous communities, regardless of their location or identity. Employment levels dropped across Indigenous communities because of COVID-19. Participants identified that the impacts of the COVID-19 pandemic and rates of infection are expected to remain ongoing issues for many remote and isolated Indigenous communities, even when the pandemic is considered over for many urban and southern regions in Canada. Participants noted many structural issues, defined as the institutions (e.g., health, education, justice, policing/corrections, finances, politics, media, social services) and rights (e.g., Charter of Rights and Freedoms, Royal Proclamation of 1763, United Nations Declaration for the Rights of Indigenous Peoples, and international rights), that are part of Canadian and global societies, but simultaneously impact Indigenous Peoples, families, communities, nations and organizations in different ways and at different intensities. A few participants spoke about Indigenous Peoples in Canada being considered a minority population and often do not receive the same opportunities for input, collaboration, or opportunities to assist in implementing governmental changes that will reduce and/or eliminate the discrimination, racism, or inequities existing within our society.
Issues brought forward by participants and identified within supplemental submissions (see Appendix A) are quite varied and have been discussed throughout this report. A list of issues specifically brought forward has been provided. In order to avoid duplicating discussions, some of the issues are discussed in separate sections of the report and are only briefly discussed in this section. Other issues are discussed in this section in great detail as they are not discussed in other sections.
Structural inequalities brought forward by participants
- broadband internet access and infrastructure
- affordable and safe homes
- access and available clean usable water
- food security and sovereignty
- land and environmental stewardship
- employment, labour and workforce participation
- health and healthcare and mental health services
- materials, supplies, and other needs
- transportation
- funding and finances
- stereotypes, discrimination, myths, and racism
- relationships (or lack thereof) with different governments
- policy discounts and discredits Indigenous Worldviews: values, beliefs, ceremonies, knowledges, and kinships
Internet
As most participants noted, the majority of their programs, services, and communications as well as employment, education and health care services have moved to online or virtual platforms as a result of the COVID-19 pandemic.
Many remote and isolateds First Nations and Inuit communities may face barriers accessing video calls (e.g., Zoom, MS Teams, etc.) as the bandwidth is inadequate for the heavy demands of video and audio especially when multiple users rely upon the same network according to some participants. Children and youth cannot attend virtual classes when the resources are made inaccessible through language (e.g., not in an Indigenous language where in-person classes can be taught in Indigenous languages), and because the internet infrastructure is not stable enough to have “so much draw on just one internet for the community”.
Some participants spoke about community members who do not have cell phones or internet-ready devices. This presents a challenge to accessing external resources, educational, employment and health services. A few participants spoke about there being no changes made to internet access while COVID-19 has exposed the dire need to update broadband internet technology for First Nations and Inuit communities who are heavily relying on it. It is extremely important to ensure that all areas of Canada have reliable access to high speed broadband internet. Therefore, there is a need for increased investment to improve internet infrastructure to ensure high speed broadband internet access.
Housing
Many participants shared that COVID-19 has exacerbated inadequate housing, homelessness and access to water. Some participants discussed issues of overcrowding, shift sleeping, and lack of available housing. Some unhoused individuals may have been able to couch-surf before COVID-19 but, for many, that possibility diminished as a result of the virus. The COVID-19 pandemic has led to increased homelessness and the inability to self-isolate depending on where community members live. Those who couch-surfed before COVID-19 are now reliant on shelters in urban areas, while some Indigenous individuals are choosing to stay in tent-cities instead of shelters due to fear of contracting COVID-19 in the facility. Additionally, individuals forced to leave northern/remote communities for medical purposes (e.g., hospital stays, birthing, etc.) are required to stay at a quarantine hotel without any family or friends. At times, the food delivered while in isolation is not food they would eat normally nor is it necessarily provided at the times when the person would ordinarily eat.
There has been an increase in the use of homeless shelters in some Inuit and remote communities as well. Some rural Métis communities set up isolation centres to respond to the overcrowding shelters. However, some spaces in the North lack adequate space for isolation requiring existing spaces, such as schools, to be used. As the school year begins, these spaces are no longer available, and this problem will be exacerbated in the colder months. Other communities and homes have closed their doors due to fear of COVID-19 and this has impacted the options available for individuals to couch-surf or find meals according to some urban participants. Economic measures have led to an increase in prices for renovation, maintenance and building costs, increasing the likelihood that homes remain unsafe due to deterioration and mitigation costs. For those who do not work from home and/or who live in an overcrowded household, adhering to physical distancing protocols may be difficult as was noted by a few participants. A few participants discussed overcrowded and inadequate housing availability can also increase COVID-19 risk for a community if a neighbouring community is experiencing an outbreak as multiple household members who are unable to maintain physical distance from each other, if needed, will increase COVID-19 risk and exposure.
Lack of relationships
A number of participants spoke about the relationship (or lack of one) with federal and/or provincial/territorial governments and the means by which Indigenous Peoples continue to be ignored or treated as just one minority in Canadian society instead of honouring treaties and agreements established hundreds of years ago and remain lasting. COVID-19 continues to illustrate that governments at all levels must build relationships and maintain those relationships to address the longstanding issues and realities of Indigenous Peoples, families and communities. For decades, reports given to the federal government have illustrated the need for the government to develop and maintain relationships with Indigenous groups and Indigenous organizations to rectify the issues brought forward in this section. Some of the participants pointed to the Truth and Reconciliation Commission and other reports that have discussed many of the issues that are still affecting Indigenous Peoples. Past reports have illustrated the government-Indigenous relationships need to be renewed, reciprocal, and improved in order to address structural inequalities.
These include:
- The Story of a National Crime - Bryce (1922)
- The Report of the Mackenzie Valley Pipeline Inquiry - Justice Berger (1980)
- Study of Health Services for Canadian Indians - Booz, Allen and Hamilton Canada (1969)
- Report of the Royal Commission on Aboriginal Peoples (1996)
- Building on values: the future of health care in Canada - Romanow (2002)
- Truth and Reconciliation Commission Final Report (2015)
Water
FNIGC released “RHS Statistics for Shaping a Response to COVID-19 in First Nations Communities” (2020) that noted 27.5% of First Nations adults reported that their main source of water is not suitable for drinking year-round and that proper hygiene and sanitation has become even more critical now that COVID-19 requires a high frequency of hand-washing, laundering clothes, and eliminating wastes. Participants expressed concern with the availability of clean water especially in light of COVID-19 and that there are many communities who remain under ‘boil water’ and ‘do-not-consume’ advisories or warnings with little guidance from the federal government around when this will be addressed.
Healthcare access
Testing
Access to health care is a foundational piece for maintaining and achieving good health during COVID-19. Some communities worked in partnership with their local public health units to access testing kits. Development of a community-led approach to COVID-19 testing with sites located in the community or near Elder’s residences was a key issue among participants. Some communities completed door-to-door testing in order to reduce barriers related to fear of leaving the house or infecting others. Some participants from urban centres spoke to instances where non-Indigenous people accessed testing at Indigenous organizations which increased the backlog of test results while reducing the number of Indigenous Peoples able to access testing. Some Métis did not have access to testing altogether. Communities also spoke about a need for a dedicated public health workforce rather than placing that burden on healthcare workers already focused on acute care.
Physician and nursing availability
At the height of the pandemic, nursing stations and physician availability were greatly reduced. For example, a nurse fly-in program for remote communities was stopped during COVID-19 and replaced with personal support workers and virtual care delivered by nurses according to many participants from remote or isolated communities. There was a rapid transition to virtual care, instead of in-person health service delivery to limit the possible spread of COVID-19 in all communities. In some capacities this may have allowed for more flexibility in physician and nursing availability but also raised other issues such as access to stable broadband internet service and virtual devices according to many remote and isolated participants (see Section 4.7.1). Some participants and communities reflected that the key to their management of COVID-19 was a community health team who were able to incorporate cultural and traditional knowledge with biomedical approaches. One First Nation has advocated for the building of a hospital in one of the larger communities, which is especially important in the backdrop of a second wave of COVID-19. This nation has also reported a drop in funding to check health equipment such as blood pressure machines.
Accessibility
Prior to the COVID-19 pandemic, many Indigenous Peoples have experienced racism and a lack of culturally safe health care which was expressed by participants and members of the research team. This has led community members (whether in urban, rural, remote, or isolated communities) to be skeptical of using telemedicine as this could lead to further stereotypes or be misconstrued if the health care practitioners were not culturally safe. Additionally, some individuals may not have a private space to make a telemedicine phone call where they reside, so it may not feel safe to disclose certain information or access healthcare in this way. Many health care workers have transitioned to virtual care in order to ensure the safety of themselves and their clients; however, this has raised concerns about increased internet costs and individuals’ inability to pay increased fees. For Indigenous Peoples with no access to phone or internet, health care workers must either visit them at home or send taxis, in order to ensure that access to health care is guaranteed according to some participants.
Racism
Indigenous Peoples continue to face racial stereotyping, discrimination, and violence when accessing health services. Participants expressed that as a result of past experiences of systemic racism in healthcare, some First Nations, Inuit and Métis felt uncomfortable accessing testing or healthcare services even more so during the pandemic. Some urban Indigenous organizations utilized mobile testing units which helped mitigate this barrier as administering the test was in a culturally safe manner. Institution and systemic racism in healthcare and allied health professions continues to be one of the biggest issues for many First Nations, Inuit and Métis.
Refer to:
- BC health workers (2020)
- Systemic racism in health system - Joyce Echaquan (2020)
- Structures of Indifference - Brian Sinclair (2018)
- Jordan's Principle - Jordan River Anderson (2014)
Some of the participants spoke about the racism in their provincial health care system and their reluctance to interact with health care professionals.
Cultural safety
Many participants spoke about health care and interactions with health professionals. Some First Nations participants spoke about being allowed to conduct traditional practices, such as smudging and pipe ceremonies. Community members spoke of being stopped from engaging in traditional funeral practices in hospitals which impacted families’ and communities’ abilities to move forward in their grieving process. This, combined with the knowledge that Indigenous Peoples frequently experience racism in accessing health care, can have strong and lasting impacts on how individuals, families, and communities access health care and consider/interact with health care institutions.
Funding
Funding considerations
Multiple participants discussed how funding is structured to be provided to the majority (mainstream society), with Indigenous Peoples receiving the minority of programs, services, and funding as they are deemed to be a minority population. Indigenous communities and organizations have long been underfunded. During the first wave of the COVID-19 pandemic, the underfunding became much more pronounced according to participants. Some northern communities expressed that they received resources in Spring 2020 but that funding availability since June has been less pronounced leading to a disruption in services provided by northern communities due to this lack of funding. Participants stated that First Nations identified that there remains a lack of funding for services to support individual mental health, trauma, and healthy coping mechanisms.
In response to gaps in available funding, many Indigenous organizations and communities have attempted to meet the need by using their own sources of revenue. Some participants said that a long-term consequence of this may be an impact on their regular service delivery and, ultimately, communities and organizations should not need to go to such lengths to address these funding gaps.
Participants spoke about how funding was designated to services provided on-reserve despite the majority of Indigenous Peoples (specifically Métis and First Nations peoples) living off-reserve and/or within or nearby urban areas. Concern was raised by participants regarding the restricted funding that disallowed on-reserve communities from providing their services to those who live off the reserve. One participant shared that in their urban area, between 85% to 95% of the local Indigenous population lives off-reserve and because of the imposed funding restrictions, the on-reserve community organizations were unable to provide the needed services to their family members and kin if they did not reside on the reserve.
Relationship with governments
Effective collaboration
Many community members expressed that their experience navigating COVID-19 thus far has allowed them to develop stronger relationships between government agencies amidst the landscape of often overlapping federal, provincial/territorial, regional, and local jurisdictions. In the past, many public health approaches have been top-down and only allowed communities to respond in a reactive manner. Now, some communities have identified that their local public health units and governmental structures have opted to work in collaboration with Indigenous community members.
Ensuring that communication channels remain open between government structures and Indigenous communities has created more effective and sustainable pandemic plans which demonstrates the importance of collaboration, relationship building, and reciprocity. The need for clear communication between government authority and communities was echoed by participants regarding rural Inuit communities as well. Some rural First Nations communities were able to meet weekly with the local mayor and other leaders. In northern First Nation communities, the COVID-19 Regional Response Team has ensured that communities have the educational material required to make safe and informed choices during the pandemic. One First Nation has identified that a significant success for them has been the transfer of responsibility for contact tracing to Sioux Lookout First Nations Health Authority. First Nation Inuit Health Branch (FNIHB) of Indigenous Services Canada began providing weekly reports on breakdown of PPE supplies allocated and distributed to each community.
Gaps in collaboration
Community members expressed concerns that, despite engagement on many topics, there are still gaps where Indigenous communities are not represented during key discussions and decision-making moments, one example shared by a participant during the August 10th discussion was regarding meetings pertaining to the COVID-19 vaccine testing. It is imperative that Indigenous representatives are included in all levels of decision making to ensure that Indigenous Peoples’ needs are met. One participant spoke to an existing gap within emergency measures as the governing agreements created by the Government of Yukon had been developed prior to agreements between communities and the territorial government. Issues that affect Indigenous Peoples such as barriers to technology, food insecurity, and inadequate infrastructure may not be understood or considered by decision makers. Participants in one breakout room felt that it is unethical for decisions to be made on behalf of Indigenous communities without appropriate Indigenous representation and inclusion.
Land
Connection to the land is central to many Indigenous individuals and communities. As previously mentioned, some Indigenous communities and territorial governments supported community members in spending extended time on the land at the beginning of COVID-19. Being on the land allowed Indigenous Peoples to (re)connect with traditions and ways of knowing that may have been shuffled aside in busier times as many were not working or working reduced hours because of the pandemic. Activities on the land include hunting and working on the land as well as finding food and sharing it with community members. Being with and on the land was spoken about as a positive experience in COVID-19; “We had to be less reliant on outside sources. We need to make sure we have a supply of wild rice and meat. We need to grow our own produce and have our own food markets.”
Some participants spoke of how mining and extraction companies used COVID-19 as a ‘free pass’ to move ahead with projects that Indigenous Peoples and communities had been protesting (e.g. Coastal Gas Pipeline spill on Wet’suwet’en Territory and the proposed housing development on Six Nations of the Grand River Territory). The federal government announced significant changes to environmental obligations during COVID-19, which has led to mining, fracking and deforestation projects moving forward with much less stringent environmental obligations. The relaxing of the Environmental Protection Act to allow mining, fracking and deforestation projects has significant impacts on First Nations, Inuit and Métis, families and communities as this work is often on or near Indigenous communities as was discussed by some participants.
Ceremony
A strength of Indigenous Peoples and communities has always been in Indigenous ways of knowing and being with the land, this continued in amended ways during the COVID-19 pandemic. One participant from a remote First Nations community shared that, at the height of COVID-19, their community lit a sacred fire from April to June in order to provide spiritual strength to the community. Communities have also seen an uptake in cultural programming enrollments which are largely delivered online. Cultural centres in some communities were able to deliver medicines and continued operations by inviting Elders to hold sunrise ceremonies, morning prayers, lighting sacred fires, using traditional medicines and lifting pipes. These spiritual practices were accessible online through livestream and video-calling platforms such as Facebook. Participants spoke to the means by which Elders, community leaders and community members made decisions about how to safely hold ceremonies. Ultimately, strength through prayer allowed community members to feel united.
A couple of participants spoke about how some communities were impacted by provincial fire bans, which relates to the need to respect Indigenous sovereignty and is a violation of Indigenous rights and freedoms guaranteed under the Charter as limiting personal fires can, in response, be seen as limiting Indigenous Peoples’ ability to practice ceremony. In some cases, public health messaging also urged individuals to stop taking part in ceremonies, such as sweat lodge, because of uncertainty of how COVID-19 was transmitted. Indigenous Services Minister Marc Miller expressed that Canada will not prohibit Indigenous Peoples from accessing and participating in ceremony. However, some communities experience police intervention when holding ceremonies (Shield, 2020) on reserve despite having permission from local Indigenous leadership and following community-approved public health protocols. Participants on both the August 10th and September 2nd calls spoke to praying in their own manner and that ability to connect with land and ceremony was heavily restricted and difficult during the first wave of the pandemic.
Domestic violence
Some participants spoke about how physical distancing and stay-at-home orders were created to reduce the spread of COVID-19 but may place some individuals at increased risk for experiencing violence. Closing schools, social programs, and the inability of individuals to leave their house have resulted in children, adults, and Elders living in close living quarters. Some participants explained that this further exacerbates negative impacts on mental health and can cause unhealthy emotional and physical situations. In fact, household overcrowding is among the risk factors linked to domestic violence (Moffitt, 2013) and child sexual abuse (O Afifi, 2015).To mitigate the negative effects of lockdown and self-isolation on domestic violence, one participant said that some communities have opened shelters for women and children during COVID-19 to ensure their safety. This approach also extends to the larger community in which a safety plan has been reviewed so that individuals are understanding of the circumstances regarding those involved in domestic violence situations. However, some places have inadequate numbers of safe shelters, crisis centres, and safe homes. For example, in Inuit Nunangat there are only 15 such facilities in place to serve 51 Inuit communities.
Communication
Connecting virtually
Lockdown situations have led to communities using creative outlets to engage community members such as a First Nations community who designated a pickup truck to move across the community and play music to encourage dancing and exercise. Others used social media to convey safety messages such as “keep a moose length apart!” Many Indigenous Peoples, communities, Elders, and organizations have used social media or virtual platforms (e.g. Zoom, YouTube, TikTok, Instagram, Facebook) to transmit cultural knowledge or spread the word/issue quickly and efficiently.
Community Elders and Knowledge Keepers joined the virtual and online communities to ensure that ways of knowing and being were transmitted during the pandemic. For example, community members connected spiritually by watching morning prayers or drum calls virtually to keep morale up. Group programming shared cultural knowledge by asking community members to share their own story or by opening discussion posts to discuss how to protect Elders and children. Virtual kitchens were an activity in communities to promote family bonding and healthy eating.
Public health messaging
According to a few participants and through submissions, It is also important that public health messaging is taken by the community to be further distributed to community members. This builds trust between people and government authorities. This is in the form of regular updates from administration and social media.
Though public health messaging needs to be tailored to communities’ specific contexts and geographies, it also must be consistent in terms of health information and directions given to the public to avoid misinformation and confusion which was discussed in one breakout room. There was discussion about the different levels of public health messaging and how there seemed to be a lack of consistency from federal to provincial/territorial to regional/municipal and how that information was then transmitted to Indigenous Peoples. Participants understood that the information was changing but felt there needed to be more cooperation between the different public health professionals to ensure that the messaging was congruent across levels. Some northern First Nations communities were able to succeed by emphasizing their relationships with other communities that they serve with the weekly touch base. Some participants spoke about how messaging changed in a few hours, making it difficult to communicate a clear message and adapt programming to support current public health measures. In addition, datasets from the governments contained language and information that took up a large sum of resources to interpret. It may be helpful to include information in simple English that would allow a larger population to understand the science and precautionary information requested by a couple of participants and in a few of the submissions.
Data
The collection of race-based data is beginning in many jurisdictions in Canada, while some jurisdictions continue to not collect this information. Any data collected, including for the purposes of responding to the COVID-19 pandemic, would need to abide by the OCAP (Ownership, Control, Access and Possession) Principles developed with First Nations Information Governance Centre (regarding First Nations peoples) and the Inuit Tapiriit Kanatami (ITK) research principles regarding Inuit research practices. Participants stated that for small communities, confidentiality issues may occur. ITK’s President Obed has met with Dr. Tam and provided Inuit priorities and concerns about the collection of Inuit-specific public health data in Canada (D. Van Dyk, personal communication 10/19/20). Contact tracing and testing would also provide data, but this has been different by community or region. For example, community members spoke to the lack of consistent data collection by public health. In addition, Indigenous leadership were not provided access to data on cases disaggregated by community/First Nation according to some submissions and participants. This impacted the ability of communities and organizations to adequately prepare against the spread of COVID-19 in their communities as well as difficulties in designating PPE numbers.
The way forward
Participants provided some directions and challenges they have faced during COVID-19. This section is based on participants discussions and analysis of all the materials provided (discussions and submissions) by the research team
- The federal government must commit to authentic community engagement of Indigenous Peoples, communities and organizations in urban, rural, remote and isolated regions of Canada. Through the discussions and strategy of Indigenous engagement for this report, it is clear that the federal government should develop reciprocal and long-standing relationships for community engagement. Participants noted that First Nations, Inuit, and Métis communities and organizations may have existing relationships with different federal departments or agencies, and that building on those relationships in an authentic and reciprocal manner would be advantageous.
- Through the coordinating and engaging of First Nations, Inuit and Métis, communities and organizations for this report, it was clear that Indigenous Peoples are often perceived and engaged as a homogeneous group of peoples when in fact there are many different cultures, languages, values and beliefs among the groups. Future engagement and relationship building should be distinctions-based through engaging and consulting with multiple First Nations, Inuit and Métis communities and organizations to truly reflect the voices of the communities.
- The definitions of rural, remote, isolated and urban communities are not available from any one federal government department or agency. These definitions may differ from available provincial and territorial definitions. To ensure that all involved are working from the same definitions, it is important to have clear and transparent definitions of rural, remote, isolated and urban Indigenous communities. It is recommended that the federal government work in collaboration with Indigenous Peoples, communities and organizations to develop definitions for future work like pandemic planning, funding, and resource development.
- As has been recommended by the Royal Commission on Aboriginal People (RCAP) (1996) report, and in other reports commissioned or provided to the federal government that funding, resources and programming needs must be holistic and be a continuum of care approach that supports Indigenous ways of being and knowing. Funding, resources and programming must support the needs of the physical, mental, spiritual, and emotional aspects of individuals, families and communities (see Volume 3, Chapter 3 of the RCAP [1996] report with numerous recommendations).
- Public health communications and messaging have changed as COVID-19 evolves. Participants found the changes in the messaging are slow to reach all of the Indigenous communities and to take into consideration cultural, linguistic, and social implications. It is recommended that the Public Health Agency of Canada keeps the communication channels open and ensure that First Nations, Inuit and Métis voices and knowledge of issues happening in the communities and organizations be taken into consideration and help to inform government responses and communications.
- Participants addressed the need to have reliable, timely and evidence-based strategies for COVID-19 testing especially in remote and isolated communities. The testing must reflect the realities of First Nations, Inuit, and Métis communities and organizations as there are significant differences in how testing can be accessed at this point.
- There is a need to have Indigenous-specific statistics that are owned and controlled by Indigenous communities and/or organizations. In collaboration and through authentic relationships, it is important that the federal government engages and discusses methods that are congruent with Indigenous ownership and control of information and statistics. Data collected by Indigenous identity, gender, and disabilities in order to improve evidence-based knowledge that impacts funding, resources, policies and needs, must reflect the Indigenous groups, communities and organizations that it is intended to assist. This can only occur if discussions include First Nations, Inuit and Métis voices.
- Participants were frustrated with the lack of First Nations, Inuit and Métis representation in public health decision-making spaces. Moving forward, the Public Health Agency of Canada should make time and space for genuine engagement of Indigenous representation in their decision-making spaces and tables.
- For many remote and isolated First Nations and Inuit communities, people who require diagnostics or specialized health care services are required to leave the community and be taken to services in southern parts of Canada. As was recommended in the RCAP (1996) and Romanow Report (2002), it is necessary to develop health human resources and virtual care as a requirement of health services, especially during a pandemic when people are flown out of their community to access services and put at risk of contracting COVID-19. Participants recommended that hospitals and/or health clinics with many specialized services be built in the North to further improve access and provide Indigenous control in health care.
- Many participants noted that Indigenous public health programming is underfunded. During COVID-19, many participants noted that their communities or organizations had to pivot and make quick decisions leading to changes in services. Moving forward, funding for Indigenous public health needs to be increased.
- The pandemic plans for First Nations and Inuit communities highlighted the need to have pre-existing issues in domestic violence, housing, water, and child welfare considered and included in future plans. Updated pandemic plans must also take into consideration Indigenous community lockdowns and restrictions, which were not necessarily built in to previous pandemic plans. Additionally, as public health messaging recommends frequent hand-washing, isolating in the home and having enough food and supplies in the home for lockdowns, participants noted that this was not possible for many of their communities or peoples. Moving forward, the federal government must re-examine the timelines for improving water access, improving and increasing adequate housing, and funding for Indigenous child welfare.
- First Nations, Inuit and Métis communities and organizations have a continuum of capacity to apply for and run programs and services. Due to COVID-19, many Indigenous communities had to re-deploy staff into programs and services that were essential to the community(s) staying safe. COVID-19 funding for First Nations and Inuit communities was announced on April 9, 2020 (Easter long weekend) with a proposal due date of April 13, 2020. A proposal-based model in tight timelines creates a competitive environment to access funding and rewards those who have more capacity to manage and address such requests quickly. Participants recommended that emergency or pandemic funding needs to be needs-based similar to other subsidy programs provided to non-Indigenous cities and businesses.
- Governments must apply an intersectional Gender-Based Analysis Plus (GBA+) lens to pandemic planning and emergency situations. It is also necessary to understand how systemic racism continues to affect Indigenous Peoples. During COVID-19 lockdowns, participants noted that a gender lens would greatly help to protect Indigenous women who may be facing domestic violence.
- Funding has been provided to employers and businesses to assist them with economic recovery across Canada. First Nations, Inuit and Métis will need a long-term plan to deal with the economic fallout of lockdowns, closures, and business changes. Participants recommended that funding be established to assist Indigenous communities, organizations and businesses throughout COVID-19 and after its recovery.
- COVID-19 has fully exposed the structural inequalities experienced by Indigenous Peoples when they interact with institutions and organizations like healthcare. There have been highly publicized incidents of racism against Indigenous Peoples when they are interacting with healthcare. In order to truly change structural inequities, it is necessary for all public servants in the federal, provincial, territorial and municipal governments to take mandatory cultural safety training with performance evaluation built into the annual employee performance review. By reviewing how people are integrating cultural safety into their everyday work, it will help with authentic relationship building, self-awareness of power, privilege and positionality, and will be seen as an action toward truth and reconciliation.
Cultural safety
The Way Forward section, specifically bullet # 15, provides a brief overview of the cultural safety continuum and the significance of having self-awareness of a person’s power, privilege and positionality in all aspects of their lives. Many governmental agencies and organizations are looking to develop meaningful relationships with Indigenous communities, and this cannot be done without considering and implementing learnings from the cultural safety continuum.
Baba (2013) conducted an environmental scan of cultural safety that illustrated the continuum upon which people move from cultural awareness, to cultural sensitivity, to cultural competence, and finally to cultural safety. Cultural awareness is being aware that there are differences between cultural groups (Baba, 2013). Cultural sensitivity is understanding and respecting cultural differences (Baba, 2013). Cultural competence moves beyond understanding and respecting difference to acknowledging one’s own culture by acquiring “skills and behaviours that help” with working in a cross-cultural manner (Baba, 2013; p. 7). Cultural safety has had many definitions, but requires that an individual examine their power, privilege, and positionality while “considering ‘the social, political, and historical contexts’” of “racism, discrimination, and prejudice” (Baba, 2013; p. 7). A key aspect of cultural safety is the self-determination of cultural safety by the care receivers. Although attaining cultural safety can be uncomfortable, it is necessary to have everyone move into this area of culturally safe actions in order to reduce physical, emotional, spiritual, mental, social, political, and financial inequalities.
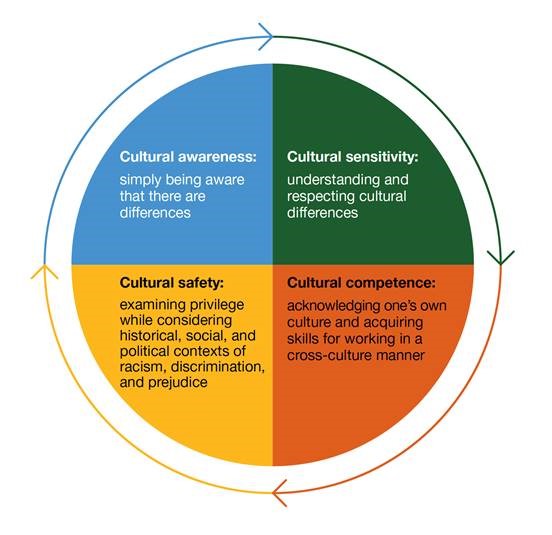
Figure 1 - Text description
Figure 1 illustrates how an individual can move from cultural awareness to cultural sensitivity to cultural competency and finally into cultural safety. Cultural awareness is simply being aware that there are differences; cultural sensitivity is understanding and respecting cultural differences; cultural competence is acknowledging one's own culture and acquiring skills for working in a cross-cultural manner; and cultural safety is examining privilege while considering historical, social, and political contexts of racism, discrimination and prejudice. There are online and in-person options for cultural safety training that non-Indigenous people and organizations can take as per the Truth and Reconciliation Commission's Calls to Action (2015). To engage and build relationships with Indigenous Peoples, organizations, communities and leadership, it is recommended that all public servants in the federal, provincial, territorial and municipal governments take cultural safety training to become self-aware and better able to work in collaboration with Indigenous Peoples.
References
Baba, L. (2013). Cultural Safety in First Nations Inuit and Métis Public Health: Environmental Scan of Cultural Competency and Safety in Education, Training and Health Services. National Collaborating Centre for Aboriginal Health.
Berger, J. T. R. (1980). Report of Advisory Commission on Indian and Inuit Health Consultation. Ottawa, Ontario: Minister of Public Works
Boggild, A., Yuan, L., Low, D., & McGeer, A. (2011). The impact of Influenza on the Canadian First Nations. Canadian Journal of Public Health, 102(5), 345-348. doi: https://pubmed.ncbi.nlm.nih.gov/22032099/
Booz-Allen & Hamilton Canada Ltd. (1969). Study of Health Services for Canadian Indians. Ottawa, Ontario: National Health and Welfare Canada
Bryce, P. H. (1922). The Story of A National Crime: An Appeal for Justice to the Indians of Canada. Retrieved from Ottawa, Ontario
Charania, N. (2011). The 2009 H1N1 Health Sector Pandemic Response in Remoteand Isolated First Nation Communities of Sub-Arctic Ontario, Canada.(Master of Environmental Studies). University of Waterloo, Waterloo, Ontario.
Charania, N., & Tsuji, L. (2011). The 2009 H1N1 pandemic response in remote First Nation communities of Subarctic Ontario: barriers and improvements from a health care services perspective. International Journal of Circumpolar Health, 70(5), 564-575. doi:10.3402/ijch.v70i5.17849
First Nations Child and Family Caring Society of Canada. (2014). Jordan's Principle: A brief history. Retrieved from http://www.fncaringsociety.com/sites/default/files/Jordan%27s%20Principle%20Information%20Sheet.pdf
First Nations Information Governance Centre. (2020). RHS Statistics for Shaping a Response to COVID-19 in First Nations Communities. Retrieved from Ottawa, Ontario: https://fnigc.ca/wpcontent/uploads/2020/09/0ab2092ec4f6262599ed396de5db3cf0_FNIGC-RHS-Covid-19-Report1.pdf
Follett Hosgood, A. (2020). RCMP, Pipeline Firm Spill Fuel on Wet'suwet'en Territory. TheTyee.ca. Retrieved from https://thetyee.ca/News/2020/06/04/Pipeline-Spill-Wetsuweten-Territory/
Government of Canada. (2020). Announcements related to the COVID-19 pandemic. Retrieved from /content/canadasite/en/environment-climate-change/services/canadian-environmental-protection-act-registry/methane-regulations-covid19-announcements.html
Government of Ontario. (2018). Urban Indigenous Action Plan. Toronto, ON: https://www.ontario.ca/page/urban-indigenous-action-plan
Johnston, B. (2003). Honour Earth Mother = Mino-audjaudauh Mizzu-Kummik-Quae (1st ed.). Wiarton, Ont.: Kegedonce Press.
Kirby, M., & Keon, W. J. (2004). Mental Health, Mental Illness and Addiction: Overview of Policies and Programs in Canada. Interim Report of the Standing Senate Committee on Social Affairs, Science and Technology. Ottawa, Ontario
Malloy, J. (2001). Double Identities: Aboriginal Policy Agencies in Ontario and British Columbia. Canadian Journal of Political Science, 36(1), 131-155.
Martinez, D., Salmón, E., & Nelson, M. K. (2008). Restoring Indigenous History and Culture to Nature. In M. K. Nelson (Ed.), Original Instructions: Indigenous Teachings for a Sustainable Future. Rochester, VT: Bear and Company.
Maunula, L. (2013). The Pandemic Subject: Canadian Pandemic Plans and Communicating with the Public about an Influenza Pandemic. Healthcare Policy, 9 (Special Issue).
McCallum, M. J., & Perry, A. (2018). Structures of Indifference: An Indigenous Life and Death in a Canadian City. Winnipeg, MB: University of Manitoba Press.
Metis Nation of Canada. (2017). Métis Nation Citizenship. Retrieved from http://www.metisnation.ca/index.php/who-are-the-metis/citizenship
Mohawk, J. (2008). Clear Thinking: A Positive Solitary View of Nature. In M. K. Nelson (Ed.), Original Instructions: Indigenous Teachings for a Sustainable Future. Rochester, VT: Bear & Company.
Moffitt, P., Fikowski, H., Mauricio, M., and Mackenzie, A. (2013). Intimate partner violence in the Canadian territorial north: perspectives from a literature review and media watch. International Journal of Circumpolar Health.
O Afifi, T., Taillieu, T., Cheung, K., Katz, L., Tonmyr., L., and Sareen, J. (2015). Substantiated reports of child maltreatment from the Canadian incidence study of reported child abuse and neglect 2008: examining child and household characteristics and child functional impairment. Canadian Journal of Psychiatry.
Ontario Ministry of Health and Long-Term Care. (2011). Rural and Northern Health Care Framework/Plan: Stage 1 Report. Retrieved from Toronto, Ontario: http://www.health.gov.on.ca/en/public/programs/ruralnorthern/docs/report_rural_northern_EN.pdf
Ontario Ministry of Indigenous Affairs. (2019). The Urban Indigenous Action Plan. Retrieved from https://www.ontario.ca/page/urban-indigenous-action-plan#:~:text=Urban%20Indigenous%3A%20For%20the%20Urban,between%20and%20within%20Indigenous%20communities
Ontario Ministry of Indigenous Affairs. (2019). The Urban Indigenous Action Plan. Retrieved from. https://www.ontario.ca/page/urban-indigenous-action-plan
O'Sullivan, T., & Bourgoin, M. (2010). Vulnerability in an Influenza Pandemic: Looking Beyond Medical Risk. Retrieved from Ottawa, Ontario: https://www.semanticscholar.org/paper/Vulnerability-in-an-Influenza-Pandemic- %3A-Looking-%2C-O%E2%80%99Sullivan-Bourgoin/48b390413d140b148a598a81dc4ec4515f1d458e
Paradkar, S. (2020). Arrests at Six Nations' Land Back Lane protests against a Caledonia housing development show the ugly face of colonial violence. The Star. Retrieved from https://www.thestar.com/opinion/star-columnists/2020/09/11/arrests-at-six-nations-land-back-lane-protests-against-a-caledonia-housing-development-show-the-ugly-face-of-colonial-violence.html
Public Health Agency of Canada. (2006a). Canadian Pandemic Influenza Preparedness: Planning Guidance for the Health Sector. Ottawa, ON: Government of Canada Retrieved from /content/canadasite/en/public- health/services/flu-influenza/canadian-pandemic-influenza-preparedness- planning-guidance-health-sector.html
Public Health Agency of Canada. (2006b). On-Reserve First Nations communities: Canadian Pandemic Influenza Preparedness: Planning Guidance for the Health Sector. Ottawa, ON: Government of Canada Retrieved from /content/canadasite/en/public-health/services/flu-influenza/canadian-pandemic-influenza-preparedness-planning-guidance-health-sector/influenza-pandemic-planning-considerations-in-on-reserve-first-nations-communities.html
Public Health Agency of Canada. (2009). Considerations for Definitions of "Remote" and "Isolated" in the Context of Pandemic (H1N1) 2009. Ottawa, Ontario Retrieved from http://web.archive.org/web/20091118023500/http://www.phac-aspc.gc.ca/alert-alerte/h1n1/guidance_lignesdirectrices/cdricp-cdeicp-eng.php
Romanow, R. (2002). [Building on Values: The Future of Health Care in Canada, Chapter 10: A New Approach to Aboriginal Health]. Web Page.
Royal Commission on Aboriginal Peoples. (1996). Report of the Royal Commission on Aboriginal Peoples. Ottawa: The Commission.
Shield, D., & Martell, C. (2020). RCMP 'had no understanding' of sun dance ceremony that was interrupted, dancer says. CBC News. Retrieved from https://www.cbc.ca/news/canada/saskatoon/beardys-okemasis-sun-dance-1.5566551
Sistovaris, M., Fallon, B., Miller, S., Birken, C., Denburg, A., Jenkins, J., Stewart, S. (2020). Child Welfare and Pandemics. Retrieved from Toronto, ON:
Truth and Reconciliation Commission of Canada. (2015). Truth and Reconciliation Commission of Canada: Calls to Action. http://trc.ca/assets/pdf/Calls_to_Action_English2.pdf
White, J., Murphy, L., & Spence, N. (2012). Water and Indigenous Peoples: Canada's Paradox. International Indigenous Policy Journal, 3(3).
Zimonjic, P., & Stefanovich, O. (2020). Federal ministers, Indigenous leaders plan to discuss systemic racism in health system. CBC News. Retrieved from https://www.cbc.ca/news/politics/marc-miller-joyce-echaquan-1.5755912
Zussman, R. (2020). B.C. health workers allegedly bet on Indigenous patients' blood alcohol levels. Global News. Retrieved from https://globalnews.ca/news/7085230/bc-health-care-racist-allegations/#:~:text=B.C.%20health%20workers%20allegedly%20bet%20on%20Indigenous%20patients'%20blood%20alcohol%20levels,-By%20Richard%20Zussman&text=The%20province%20is%20investigating%20reports,to%20Health%20Minister%20Adrian%20Dix
Appendices
Appendix A: Community submissions
- Arctic Indigenous Wellness Foundation
- The union of B.C. Indian Chiefs impacts of COVID-19 on Indigenous Peoples
- Nishnawbe Aski Nation briefing note
- Arctic Council
- Cowichan Tribes impacts of COVID-19: input into the Chief Public Health Officer’s
- North American Observatory preliminary draft North American COVID-19 policy response monitor: Indigenous communities across Northern Canada
- FNIGC RHS statistics for shaping a response to COVID-19 in First Nations communities
- Inuit Tapiriit Kanatami the potential impacts of COVID-19 on Inuit Nunangat
- International Centre for Indigenous Education and Wellness: National Elders of Turtle Lodge make statement about ceremony
- Yellowhead Institute (Gina Starblanket and Dallas Hunt): COVID-19, the numbered treaties and the politics of life
- Sioux Lookout First Nations Health Authority – numerous attachments
Appendix B: Community websites
- Cree Board of Health and Social Services of James Bay. (n.d.). COVID-19 (Coronavirus). Retrieved from: https://eeyouistcheecovid19.org/
- Nishnawbe Aski Nation. (n.d.). Updates: COVID-19. Retrieved from: http://www.nan.on.ca/covid19
- Six Nations of the Grand River. (n.d.). COVID-19 Information Centre. Retrieved from: https://www.sixnationscovid19.ca/
- Morning Star Lodge. (n.d.) Blog. http://www.indigenoushealthlab.com/blog
Appendix C: Communication for community engagement sessions
Annotated agenda
Impacts of COVID-19: Input into the Chief Public Health Officer’s Annual Report
Monday, August 10, 2020 / 1:30pm – 4:00pm (EDT)
Schedule
- Welcome and Housekeeping (1:30 – 1:35)
Speaker: Christine Maika - Opening prayer and cultural teaching (1:35 – 1:45)
Speaker: Elder Claudette Commanda - Introduction of CPHO (1:45 – 1:50)
Speaker: Dr. Carrie Bourassa - Setting the Scene: The 2020 CPHO Report (1:50 – 2:15)
Dr. Tam to orient participants to the nature of the annual report and the objectives of today’s meeting and provide an overview of the 2020 Annual Report - Break (2:15 – 2:20)
Please leave your Zoom meeting on - Strengthening Structural Determinants of Health Post-COVID-19 (2:20 – 2:50)
Dr. Greenwood will discuss the impacts of COVID-19 on Indigenous Peoples
Speaker: Dr. Margo Greenwood - Discussion (2:50 – 3:45)
Dr. Bourassa will facilitate a conversation with participants to share Indigenous experiences and points-of-view on the impact of COVID-19 on Indigenous communities
Speakers: All, Facilitated by Dr. Carrie BourassaDiscussion Questions
- What makes you proud when you think about your community’s (or the community you serve’s) response to the COVID -19 pandemic?
- What has helped keep you and your community (or the community you serve) strong when responding to the COVID-19 pandemic?
- What changes (big or small) made in response to COVID-19 could or should be taken up by other communities?
- Reflections and Closing (2:20 – 2:50)
Speakers: Dr. Theresa Tam/Christine Maika, Elder Claudette Commanda
