FluWatch report: September 13 to September 26, 2015 (weeks 37 and 38)
Overall Summary
- Overall, there is low influenza activity in Canada; however, influenza activity and detections are increasing, especially in BC.
- In week 37, two influenza outbreaks were reported.
- In weeks 37 and 38, both paediatric and adult hospitalizations with influenza were reported.
- For more information on the flu, see our Influenza (flu) web page.
Are you a primary health care practitioner (General Practitioner, Nurse Practitioner or Registered Nurse) interested in becoming a FluWatch sentinel for the 2015-16 influenza season? Contact us at FluWatch@phac-aspc.gc.ca
On this page
- Influenza/ILI Activity (geographic spread)
- Laboratory Confirmed Influenza Detections
- Influenza-like Illness Consultation Rate
- Influenza Outbreak Surveillance
- Sentinel Pediatric Hospital Influenza Surveillance
- Provincial/Territorial Influenza Hospitalizations and Deaths
- Influenza Strain Characterizations
- Antiviral Resistance
- International Influenza Reports
- FluWatch definitions for the 2015-2016 season
Influenza/Influenza-like Illness Activity (geographic spread)
In week 38, sporadic influenza activity was reported in the Western provinces and parts of Central Canada. The majority of influenza activity was reported in the BC and ON.

Download the alternative format
(PDF format, 696 KB, 7 pages)
Related Topics
Figure 1. Map of overall influenza/ILI activity level by province and territory, Canada, Week 38
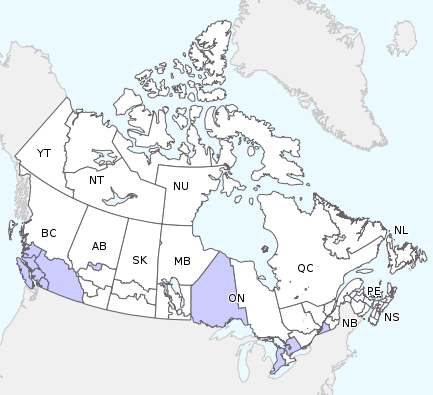

Note: Influenza/ILI activity levels, as represented on this map, are assigned and reported by Provincial and Territorial Ministries of Health, based on laboratory confirmations, sentinel ILI rates and reported outbreaks. Please refer to detailed definitions at the end of the report. Maps from previous weeks, including any retrospective updates, are available on the Flu Activity website.
Figure 1 - Text Description
In week 38, sporadic influenza activity was reported in the Western provinces and parts of Central Canada. The majority of influenza activity was reported in the BC and ON.
Laboratory Confirmed Influenza Detections
Although the number of positive influenza tests increased over the two week period, the percent positive for influenza detections remains low (1.5%) (Figure 2).
Figure 2. Number of positive influenza tests and percentage of tests positive, by type, subtype and report week, Canada, 2015-16

Figure 2 - Text Description
Although the number of positive influenza tests increased over the two week period, the percent positive for influenza detections remains low (1.5%).
Most jurisdictions have reported only sporadic numbers of influenza detections in recent weeks. The majority of detections in Canada have been reported from BC, accounting for 77% of influenza detections in Canada in week 38. To date, 94% of influenza detections have been influenza A and the majority of those subtyped have been A(H3).
Figure 3. Cumulative numbers of positive influenza specimens by type/subtype and province, Canada, 2015-16
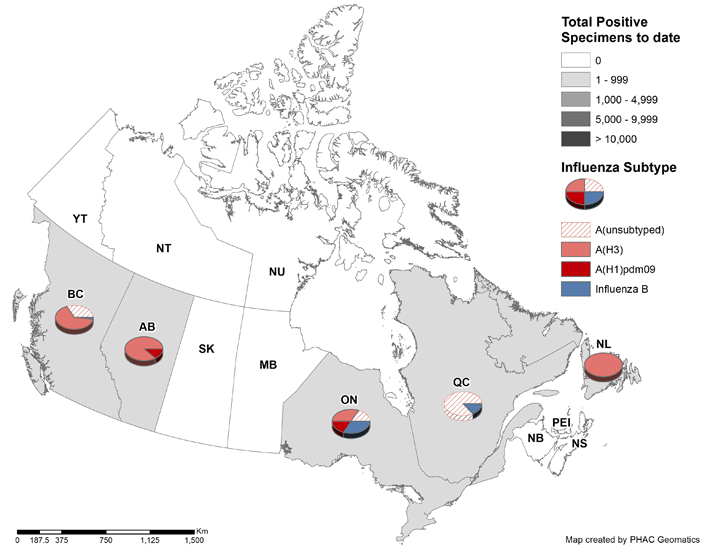
Note: Specimens from NT, YT, and NU are sent to reference laboratories in other provinces. Cumulative data includes updates to previous weeks.
Figure 3 - Text Description
| Reporting provincesTable Figure 3 - Footnote 1 | Weekly (September 13 to September 26, 2015) | Cumulative (August 30, 2015 to September 26, 2015) | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Influenza A | B | Influenza A | B | A & B Total | |||||||
| A Total | A(H1)pdm09 | A(H3) | A Table Figure 3 - Footnote UnS | B Total | A Total | A(H1)pdm09 | A(H3) | ATable Figure 3 - Footnote UnS | B Total | ||
| BC | 20 | 0 | 13 | 7 | 0 | 44 | 0 | 29 | 15 | 1 | 45 |
| AB | 2 | 0 | 2 | 0 | 0 | 8 | 1 | 7 | 0 | 0 | 8 |
| SK | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
| MB | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
| ON | 2 | 0 | 1 | 1 | 0 | 4 | 1 | 2 | 1 | 2 | 6 |
| QC | 2 | 0 | 0 | 2 | 0 | 6 | 0 | 0 | 6 | 1 | 7 |
| NB | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
| NS | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
| PE | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
| NL | 0 | 0 | 0 | 0 | 0 | 2 | 0 | 2 | 0 | 0 | 2 |
| YT | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
| NT | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
| NU | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
| Canada | 26 | 0 | 16 | 10 | 0 | 64 | 2 | 40 | 22 | 4 | 68 |
| Percentage Table Figure 3 - Footnote 2 | 100.0% | 0.0% | 61.5% | 38.5% | 0.0% | 94.1% | 3.1% | 62.5% | 34.4% | 5.9% | 100.0% |
Among cases with reported age, the largest proportion was in those ≥65 years of age (52%) (Table 1).
| Age groups (years) | Weekly (September 13 to September 26, 2015) | Cumulative (August 30, 2015 to September 26, 2015) | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Influenza A | B | Influenza A | B | Influenza A and B | ||||||||
| A Total | A(H1) pdm09 | A(H3) | A Table 1 - Footnote UnS | Total | A Total | A(H1) pdm09 | A(H3) | A Table 1 - Footnote UnS | Total | # | % | |
| <5 | 1 | 0 | 1 | 0 | 0 | 3 | 0 | 3 | 0 | 0 | 3 | 5.2% |
| 5-19 | 0 | 0 | 0 | 0 | 0 | 5 | 0 | 3 | 2 | 1 | 6 | 10.3% |
| 20-44 | 1 | 0 | 0 | 1 | 0 | 5 | 0 | 1 | 4 | 0 | 5 | 8.6% |
| 45-64 | 2 | 0 | 1 | 1 | 0 | 13 | 0 | 10 | 3 | 1 | 14 | 24.1% |
| 65+ | 9 | 0 | 4 | 5 | 0 | 29 | 0 | 20 | 9 | 1 | 30 | 51.7% |
| Unknown | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0.0% |
| Total | 13 | 0 | 6 | 7 | 0 | 55 | 0 | 37 | 18 | 3 | 58 | 100.0% |
| PercentageTable 1 - Footnote 2 | 100.0% | 0.0% | 36.2% | 53.8% | 0.0% | 94.8% | 0.0% | 67.3% | 32.7% | 5.2% | ||
For additional data on other respiratory virus detections see the Respiratory Virus Detections in Canada Report on the Public Health Agency of Canada website.
Influenza-like Illness Consultation Rate
The national influenza-like-illness (ILI) consultation rate increased from 13.2 consultations per 1,000 patient visits in week 37 to 14.8 per 1,000 visits in week 38. In week 38, the highest ILI consultation rate was found in the 5-19 age group and the lowest was found in the ≥65 age group (Figure 4).
Figure 4. Influenza-like-illness (ILI) consultation rates by age group and week, Canada, 2015-16
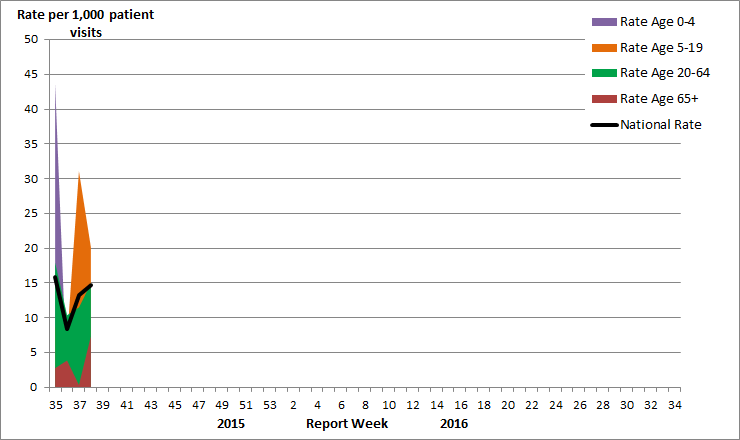
Delays in the reporting of data may cause data to change retrospectively. In BC, AB, and SK, data is compiled by a provincial sentinel surveillance program for reporting to FluWatch. Not all sentinel physicians report every week.
Figure 4 - Text Description
Influenza-like illness consultation rate by age-group in week 38 for the 2015-16 season: Age 0-4: 10.1; Age 5-19: 20.2; Age 20-64: 14.9; Age 65+: 7.4
Influenza Outbreak Surveillance
In week 37, two new outbreaks of influenza were reported. One influenza A(H3) outbreak was reported in a long-term care facility (LTCF) and the other of unknown type was reported in an institutional or community setting (Figure 5). No outbreaks were reported in week 38.
Figure 5. Overall number of new laboratory-confirmed influenza outbreaksFigure 5 - Footnote 1 by report week, Canada, 2015-2016
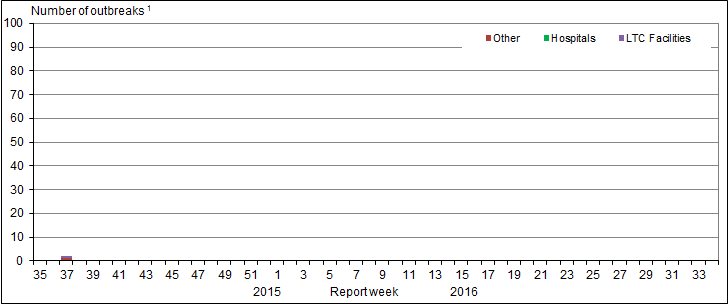
Figure 5 - Text Description
| Report week | Hospitals | Long Term Care Facilities | Other |
|---|---|---|---|
| 35 | 0 | 0 | 0 |
| 36 | 0 | 0 | 0 |
| 37 | 0 | 1 | 1 |
| 38 | 0 | 0 | 0 |
Sentinel Pediatric Hospital Influenza Surveillance
Paediatric Influenza Hospitalizations and Deaths (IMPACT)
To date, less than five laboratory-confirmed influenza-associated paediatric (≤16 years of age) hospitalizations have been reported by the Immunization Monitoring Program Active (IMPACT) network. The hospitalized cases were due to influenza A.
Figure 6. Percentage of hospitalizations, ICU admissions and deaths with influenza reported by age-group, Canada, 2015-16, Paediatric hospitalizations (≤16 years of age, IMPACT)

Figure 6 - Text Description
| Age-group (years) | Hospitalizations (n=1) | ICU Admissions (n=0) |
|---|---|---|
| 0-5m | 0.0% | 0.0% |
| 6-23m | 0.0% | 0.0% |
| 2-4y | 0.0% | 0.0% |
| 5-9y | 0.0% | 0.0% |
| 10-16y | 0.0% | 0.0% |
Figure 7. Number of cases of influenza reported by sentinel hospital networks, by week, Canada, 2015-16 Paediatric hospitalizations (≤16 years of age, IMPACT)

Note: The number of hospitalizations reported through IMPACT represents a subset of all influenza-associated paediatric hospitalizations in Canada. Delays in the reporting of data may cause data to change retrospectively.
Figure 7 - Text Description
| Report week | Influenza A | Influenza B |
|---|---|---|
| 35 | 0 | 0 |
| 36 | 0 | 0 |
| 37 | 0 | 0 |
| 38 | 0 | 0 |
Provincial/Territorial Influenza Hospitalizations and Deaths
Figure 8. Percentage of hospitalizations, ICU admissions and deaths with influenza reported by age-group, Canada 2015-16
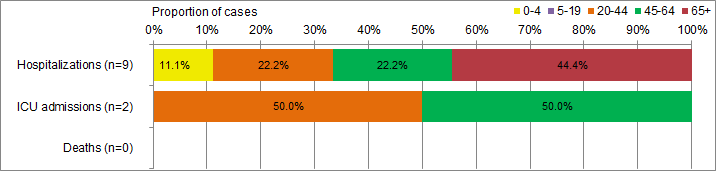
Figure 8 - Text Description
| Age-group (years) | Hospitalizations (n=9) | ICU admissions (n=2) | Deaths (n=0) |
|---|---|---|---|
| 0-4 | 11.1% | 0.0% | 0.0% |
| 5-19 | 0.0% | 0.0% | 0.0% |
| 20-44 | 22.2% | 50.0% | 0.0% |
| 45-64 | 22.2% | 50.0% | 0.0% |
| 65+ | 44.4% | 0.0% | 0.0% |
See additional data on Reported Influenza Hospitalizations and Deaths in Canada: 2011-12 to 2015-16 on the Public Health Agency of Canada website.
Influenza Strain Characterizations
The National Microbiology Laboratory (NML) has not yet reported any influenza strain characterizations for the 2015-16 season (Figure 9).
Figure 9. Influenza strain characterizations, Canada, 2015-16
The National Microbiology Laboratory (NML) has not yet conducted antigenic characterization of influenza viruses collected during the 2015-16 season.
The recommended components for the 2015-2016 northern hemisphere trivalent influenza vaccine include: an A/California/7/2009(H1N1)pdm09-like virus, an /Switzerland/9715293/2013(H3N2)-like virus, and a B/Phuket/3073/2013 -like virus (Yamagata lineage). For quadrivalent vaccines, the addition of a B/Brisbane/60/2008-like virus is recommended.
The NML receives a proportion of the number of influenza positive specimens from provincial laboratories for strain characterization and antiviral resistance testing. Characterization data reflect the results of haemagglutination inhibition (HAI) testing compared to the reference influenza strains recommended by WHO.
Antiviral Resistance
The NML has not yet reported antivirual resistance results for influenza viruses collected during the 2015-16 season (Table 2).
| Virus type and subtype | Oseltamivir | Zanamivir | Amantadine | |||
|---|---|---|---|---|---|---|
| # tested | # resistant (%) | # tested | # resistant (%) | # tested | # resistant (%) | |
| A (H3N2) | 0 | 0 | 0 | 0 | 0 | 0 |
| A (H1N1) | 0 | 0 | 0 | 0 | 0 | 0 |
| B | 0 | 0 | 0 | 0 | NA Table 2 - Footnote * | NA Table 2 - Footnote * |
| TOTAL | 0 | 0 | 0 | 0 | 0 | 0 |
International Influenza Reports
- World Health Organization influenza update
- World Health Organization FluNet
- WHO Influenza at the human-animal interface
- Centers for Disease Control and Prevention seasonal influenza report
- European Centre for Disease Prevention and Control - epidemiological data
- South Africa Influenza surveillance report
- New Zealand Public Health Surveillance
- Australia Influenza Report
- Pan-American Health Organization Influenza Situation Report
FluWatch definitions for the 2015-2016 season
Abbreviations: Newfoundland/Labrador (NL), Prince Edward Island (PE), New Brunswick (NB), Nova Scotia (NS), Quebec (QC), Ontario (ON), Manitoba (MB), Saskatchewan (SK), Alberta (AB), British Columbia (BC), Yukon (YT), Northwest Territories (NT), Nunavut (NU).
Influenza-like-illness (ILI): Acute onset of respiratory illness with fever and cough and with one or more of the following - sore throat, arthralgia, myalgia, or prostration which is likely due to influenza. In children under 5, gastrointestinal symptoms may also be present. In patients under 5 or 65 and older, fever may not be prominent.
ILI/Influenza outbreaks
- Schools:
-
Greater than 10% absenteeism (or absenteeism that is higher (e.g. >5-10%) than expected level as determined by school or public health authority) which is likely due to ILI.
Note: it is recommended that ILI school outbreaks be laboratory confirmed at the beginning of influenza season as it may be the first indication of community transmission in an area. - Hospitals and residential institutions:
- two or more cases of ILI within a seven-day period, including at least one laboratory confirmed case. Institutional outbreaks should be reported within 24 hours of identification. Residential institutions include but not limited to long-term care facilities ( LTCF) and prisons.
- Workplace:
- Greater than 10% absenteeism on any day which is most likely due to ILI.
- Other settings:
- two or more cases of ILI within a seven-day period, including at least one laboratory confirmed case; i.e. closed communities.
Note that reporting of outbreaks of influenza/ILI from different types of facilities differs between jurisdictions.
Influenza/ILI activity level
1 = No activity: no laboratory-confirmed influenza detections in the reporting week, however, sporadically occurring ILI may be reported
3 = Localized:
- evidence of increased ILIFootnote * and
- lab confirmed influenza detection(s) together with
- outbreaks in schools, hospitals, residential institutions and/or other types of facilities occurring in less than 50% of the influenza surveillance regionFootnote †
4 = Widespread:
- evidence of increased ILIFootnote * and
- lab confirmed influenza detection(s) together with
- outbreaks in schools, hospitals, residential institutions and/or other types of facilities occurring in greater than or equal to 50% of the influenza surveillance regionFootnote †
Note: ILI data may be reported through sentinel physicians, emergency room visits or health line telephone calls.