Archived Measles surveillance in Canada: 2016

Download the alternative format
(PDF format, 2 MB, 17 pages)
Organization: Public Health Agency of Canada
Date published: September 2017
Table of Contents
- Acronyms and abbreviations
- Introduction
- Methods
- Results
- Discussion
- Limitations
- Conclusion
- Acknowledgements
- Appendix: Summary of measles events in Canada, ordered by earliest date of rash onset, 2016
- References
List of figures
- Figure 1: Number of reported measles cases, by epidemiological week of rash onset and reporting province or territory, Canada, 2016
- Figure 2: Distribution of measles genotypes detected in 2016 (n=10) by week of rash onset
List of tables
- Table 1: Confirmed measles cases and incidence rates by age group, gender, and reporting province or territory, Canada, 2016
- Table 2: Vaccination status of confirmed measles cases reported in Canada in 2016 by age group
- Table 3: Hospitalization status of confirmed measles cases by age group, Canada, 2016
- Table 4: Pan American Health Organization essential criteria for the verification of measles elimination
Acronyms and abbreviations
- CMRSS
- Canadian Measles and Rubella Surveillance System
- MeaNS
- Measles Nucleotide Surveillance database
- NML
- National Microbiology Laboratory
- PAHO
- Pan American Health Organization
- PHAC
- Public Health Agency of Canada
- RT-PCR
- Reverse transcription-polymerase chain reaction
- WHO
- World Health Organization
Introduction
Measles is one of the most highly contagious respiratory infectious diseases. Before vaccination became available, measles was responsible for millions of deaths in the world. No animal reservoir maintains measles virus transmission and no latent or persistent measles virus infections result in prolonged contagiousness, making elimination possibleReference 1. Measles elimination is defined as the absence of endemic measles transmission in a defined geographic area for 12 months or more, in the presence of a well-performing surveillance systemReference 2. Enhanced surveillance of measles provides evidence for measles elimination. In Canada, measles has been a nationally notifiable disease between 1924 and 1959, and since 1968. Enhanced, case-based surveillance of measles is coordinated by the Public Health Agency of Canada (PHAC), through the Canadian Measles and Rubella Surveillance System (CMRSS). Measles elimination in Canada has been described as an important and attainable public health objective since 1980Reference 3. Moreover, Canada set the goal of achieving measles elimination by 2005 during the 1992 Consensus Conference on MeaslesReference 4. This was revised at the 1994 XXIV Pan American Sanitary Conference, where Canada and other member states agreed to eliminate measles in the Americas by 2000Reference 5. A two-dose routine vaccination program against measles and rubella was implemented in all provinces and territories in 1996-1997. As the last endemic case of measles was reported in 1997, measles elimination status in Canada was achieved in 1998 and reconfirmed in 2016 (Reference 6, Reference 7, Reference 8, Reference 9). However, Canada's elimination status remains a challenge due to importations of measles from other countries, where the disease is still endemic. In order to verify measles elimination status on an ongoing basis, Canada submits surveillance data to the Pan American Health Organization (PAHO). The objective of this report is to provide an epidemiologic summary of measles activity reported in Canada for the 2016 epidemiologic year.
Methods
Surveillance data
Measles cases meeting the national case definitionReference 7 were reported weekly to PHAC by provinces and territories through CMRSS, including zero-reporting. Surveillance data were extracted and non-identifying case data were submitted to PAHO. Confirmed measles cases included in this report had rash onset during the 2016 epidemiologic year (January 3rd, 2016 to December 31st, 2016).
Genotyping
All measles virus genotyping was performed at the PHAC's National Microbiology Laboratory. World Health Organization (WHO) standardized genotyping: sequencing of 450 nucleotides of the nucleoprotein (N) gene (the N-450), with the addition of the full length haemagglutinin (H) geneReference 10 was attempted on all reverse transcription-polymerase chain reaction (RT-PCR) confirmed measles cases. The clinical specimens (respiratory and/or urine) were referred to the NML by provincial laboratories and were RT-PCR-confirmed in the provincial laboratories or at the NML. Genotypes were assigned by maximum homology of the N-450 sequences to the WHO genotype reference sequences (Reference 11, Reference 12). Sequences were also deposited in the WHO Measles Nucleotide Surveillance database (MeaNS) and compared to so called "named strains" as well as sequences deposited by other members of the global measles laboratory network (Reference 11, Reference 13).
Data management and validation
Measles surveillance data were managed using Microsoft Access 2010. A data validation process was conducted in March 2017, with all provinces/territories. This included querying for blank fields, identifying illogical field entries and confirming values with reporting jurisdictions.
Analysis
Microsoft Excel 2010 and SAS Enterprise Guide v.5.1 were used to perform descriptive epidemiologic analyses, for categorical variables (counts, proportions) and continuous values (medians, ranges). Incidence rates were calculated using Statistics Canada July 1, 2016 population estimates by provinces and territories. Measles cases were assessed by demographics (e.g., age, sex, and location), risk characteristics (e.g., vaccination status, hospitalization, and source of exposure) and genotype. Event characteristics were summarized and surveillance data were evaluated against the essential criteria for the maintenance of measles elimination status, as described by PAHOReference 14. This routine public health surveillance activity was exempt from research ethics board approval.
Results
In 2016, the incidence of measles in Canada was 0.3 cases per 1,000,000 population, with a total of 11 reported cases. All cases were laboratory-confirmed. The majority of cases were reported in March (epidemiologic weeks 9-11, n=4, 36%) and August-September (weeks 34-37, n=3, 27%). A maximum of two cases (18%) were reported during a single week (weeks 9, 11, and 34) (Figure 1).
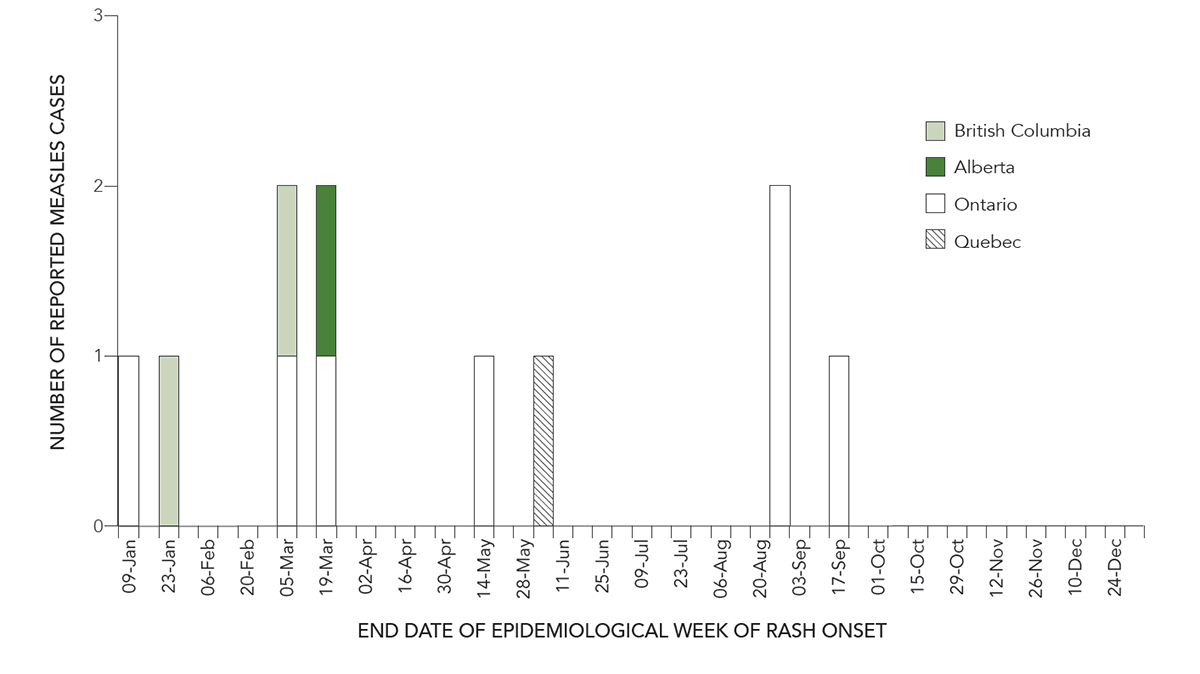
Figure 1 - Text version
| Epidemiologic Week Ending | Reporting province or territory | TOTAL | |||
|---|---|---|---|---|---|
| British Columbia | Alberta | Ontario | Quebec | ||
| 09-Jan-2016 | 0 | 0 | 1 | 0 | 1 |
| 16-Jan-2016 | 0 | 0 | 0 | 0 | 0 |
| 23-Jan-2016 | 1 | 0 | 0 | 0 | 1 |
| 30-Jan-2016 | 0 | 0 | 0 | 0 | 0 |
| 06-Feb-2016 | 0 | 0 | 0 | 0 | 0 |
| 13-Feb-2016 | 0 | 0 | 0 | 0 | 0 |
| 20-Feb-2016 | 0 | 0 | 0 | 0 | 0 |
| 27-Feb-2016 | 0 | 0 | 0 | 0 | 0 |
| 05-Mar-2016 | 1 | 0 | 1 | 0 | 2 |
| 12-Mar-2016 | 0 | 0 | 0 | 0 | 0 |
| 19-Mar-2016 | 0 | 1 | 1 | 0 | 2 |
| 26-Mar-2016 | 0 | 0 | 0 | 0 | 0 |
| 02-Apr-2016 | 0 | 0 | 0 | 0 | 0 |
| 09-Apr-2016 | 0 | 0 | 0 | 0 | 0 |
| 16-Apr-2016 | 0 | 0 | 0 | 0 | 0 |
| 23-Apr-2016 | 0 | 0 | 0 | 0 | 0 |
| 30-Apr-2016 | 0 | 0 | 0 | 0 | 0 |
| 07-May-2016 | 0 | 0 | 0 | 0 | 0 |
| 14-May-2016 | 0 | 0 | 1 | 0 | 1 |
| 21-May-2016 | 0 | 0 | 0 | 0 | 0 |
| 28-May-2016 | 0 | 0 | 0 | 0 | 0 |
| 04-Jun-2016 | 0 | 0 | 0 | 1 | 1 |
| 11-Jun-2016 | 0 | 0 | 0 | 0 | 0 |
| 18-Jun-2016 | 0 | 0 | 0 | 0 | 0 |
| 25-Jun-2016 | 0 | 0 | 0 | 0 | 0 |
| 02-Jul-2016 | 0 | 0 | 0 | 0 | 0 |
| 09-Jul-2016 | 0 | 0 | 0 | 0 | 0 |
| 16-Jul-2016 | 0 | 0 | 0 | 0 | 0 |
| 23-Jul-2016 | 0 | 0 | 0 | 0 | 0 |
| 30-Jul-2016 | 0 | 0 | 0 | 0 | 0 |
| 06-Aug-2016 | 0 | 0 | 0 | 0 | 0 |
| 13-Aug-2016 | 0 | 0 | 0 | 0 | 0 |
| 20-Aug-2016 | 0 | 0 | 0 | 0 | 0 |
| 27-Aug-2016 | 0 | 0 | 2 | 0 | 2 |
| 03-Sep-2016 | 0 | 0 | 0 | 0 | 0 |
| 10-Sep-2016 | 0 | 0 | 0 | 0 | 0 |
| 17-Sep-2016 | 0 | 0 | 1 | 0 | 1 |
| 24-Sep-2016 | 0 | 0 | 0 | 0 | 0 |
| 01-Oct-2016 | 0 | 0 | 0 | 0 | 0 |
| 08-Oct-2016 | 0 | 0 | 0 | 0 | 0 |
| 15-Oct-2016 | 0 | 0 | 0 | 0 | 0 |
| 22-Oct-2016 | 0 | 0 | 0 | 1 | 1 |
| 29-Oct-2016 | 0 | 0 | 0 | 0 | 0 |
| 05-Nov-2016 | 0 | 0 | 0 | 0 | 0 |
| 12-Nov-2016 | 0 | 0 | 0 | 0 | 0 |
| 19-Nov-2016 | 0 | 0 | 0 | 0 | 0 |
| 26-Nov-2016 | 0 | 0 | 0 | 0 | 0 |
| 03-Dec-2016 | 0 | 0 | 0 | 0 | 0 |
| 10-Dec-2016 | 0 | 0 | 0 | 0 | 0 |
| 17-Dec-2016 | 0 | 0 | 0 | 0 | 0 |
| 24-Dec-2016 | 0 | 0 | 0 | 0 | 0 |
| 31-Dec-2016 | 0 | 0 | 0 | 0 | 0 |
| TOTAL | 2 | 1 | 7 | 1 | 11 |
Age, sex and location
Information on age, sex and reporting province or territory was available for every case reported in 2016. Cases ranged from four months to 40 years, with a median age of 10 months. The most frequently reported age group was less than one year (64%, n=7), followed by those aged one to four years (18%, n= 2). Incidence rates were also highest for these groups, at 17.9 and 1.3 cases per 1,000,000 population respectively (Table 1). There were no cases reported among those aged five to 19 years, 25 to 39 years, and 60 years and older. Approximately half of the reported cases (54%, n=6) were male. Four Canadian provinces reported measles cases in 2016: British Columbia, Alberta, Ontario and Quebec. Incidence was highest in Ontario, followed by British Columbia, Alberta and Quebec (0.5, 0.4, 0.2 and 0.1 cases per 1,000,000 population respectively).
| Age group | Sex | Provinces | CA | Overall incidence rate | ||||
|---|---|---|---|---|---|---|---|---|
| M | F | BC | AB | ON | QC | |||
| <1 year | 4 | 3 | 1 | 1 | 4 | 1 | 7 | 17.9 |
| 1 to 4 years | 1 | 1 | 0 | 0 | 2 | 0 | 2 | 1.3 |
| 5 to 9 years | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0.0 |
| 10 to 14 years | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0.0 |
| 15 to 19 years | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0.0 |
| 20 to 24 years | 0 | 1 | 0 | 0 | 1 | 0 | 1 | 0.4 |
| 25 to 29 years | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0.0 |
| 30 to 39 years | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0.0 |
| 40 to 59 years | 1 | 0 | 1 | 0 | 0 | 0 | 1 | 0.1 |
| 60 years or more | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0.0 |
| Total | 6 | 5 | 2 | 1 | 7 | 1 | 11 | - |
| Incidence rate: | 0.3 | 0.3 | 0.4 | 0.2 | 0.5 | 0.1 | 0.3 | 0.3 |
Table 1 - Abbreviations
|
||||||||
Vaccination
In 2016, nine of 11 cases were not vaccinated, and two had unknown vaccination status (Table 2). Of the nine unvaccinated cases, seven were age ineligible according to the routine immunization schedule. Two cases were adults with unknown vaccination history. None of the reported cases were born before 1970, the cut off used for presumed natural immunity to measles in CanadaReference 15.
| Age group | Unvaccinated | Vaccinated | Unknown | Total |
|---|---|---|---|---|
| <1 year | 7 | 0 | 0 | 7 |
| 1 to 4 years | 2 | 0 | 0 | 2 |
| 5 to 9 years | 0 | 0 | 0 | 0 |
| 10 to 14 years | 0 | 0 | 0 | 0 |
| 15 to 19 years | 0 | 0 | 0 | 0 |
| 20 to 24 years | 0 | 0 | 1 | 1 |
| 25 to 29 years | 0 | 0 | 0 | 0 |
| 30 to 39 years | 0 | 0 | 0 | 0 |
| 40 to 59 years | 0 | 0 | 1 | 1 |
| 60 years or more | 0 | 0 | 0 | 0 |
| TOTAL | 9 | 0 | 2 | 11 |
Hospitalization
In 2016, five cases were hospitalized (45%) (Table 3). All hospitalizations occurred among children zero to four years of age.
| Age group | Total | Not hospitalized N |
Hospitalized N |
|---|---|---|---|
| <1 year | 7 | 4 | 3 |
| 1 to 4 years | 2 | 0 | 2 |
| 5 to 9 years | 0 | 0 | 0 |
| 10 to 14 years | 0 | 0 | 0 |
| 15 to 19 years | 0 | 0 | 0 |
| 20 to 24 years | 1 | 1 | 0 |
| 25 to 29 years | 0 | 0 | 0 |
| 30 to 39 years | 0 | 0 | 0 |
| 40 to 59 years | 1 | 1 | 0 |
| 60 years or more | 0 | 0 | 0 |
| Total | 11 | 6 | 5 |
Table 2 - Abbreviation
|
|||
Canadian measles in the global context
Importations accounted for 91% (n=10) of cases in 2016; only one case had an unknown source of exposure. Seven cases were infants under one year old, which is too young to be immunized according to the routine schedule. However, measles, mumps and rubella (MMR) vaccine may be given as early as six months of age to children travelling to countries outside of North America, thus six cases were eligible for vaccine as per the previously stated travel recommendationsReference 16. These children also represent missed opportunities for vaccination. One case was under six months of age, which is too young to be vaccinated even in a travel context. Imported cases were exposed to measles during travel within four of the six WHO regions: Eastern Mediterranean (n=6; Pakistan and Afghanistan), South-East Asian (n=2; China and/or Malaysia, India), African (n=1, Gabon) and European (n=1, Italy and/or Montenegro) regions. There was one event with two co-index cases where the source of exposure was Afghanistan (Appendix).
Molecular epidemiology
Of the 11 measles cases in 2016, 10 had specimens available for genotyping (91%). Two of the 11 cases were epidemiologically linked while remaining nine were individual cases with no secondary spread. Of the measles events 91% were genotyped. The genotypes detected were B3 (n=7) and D8 (n=3) (Figure 2). Globally, these were two of the most frequently detected genotypes, outside of China, based on submissions to the MeaNS.
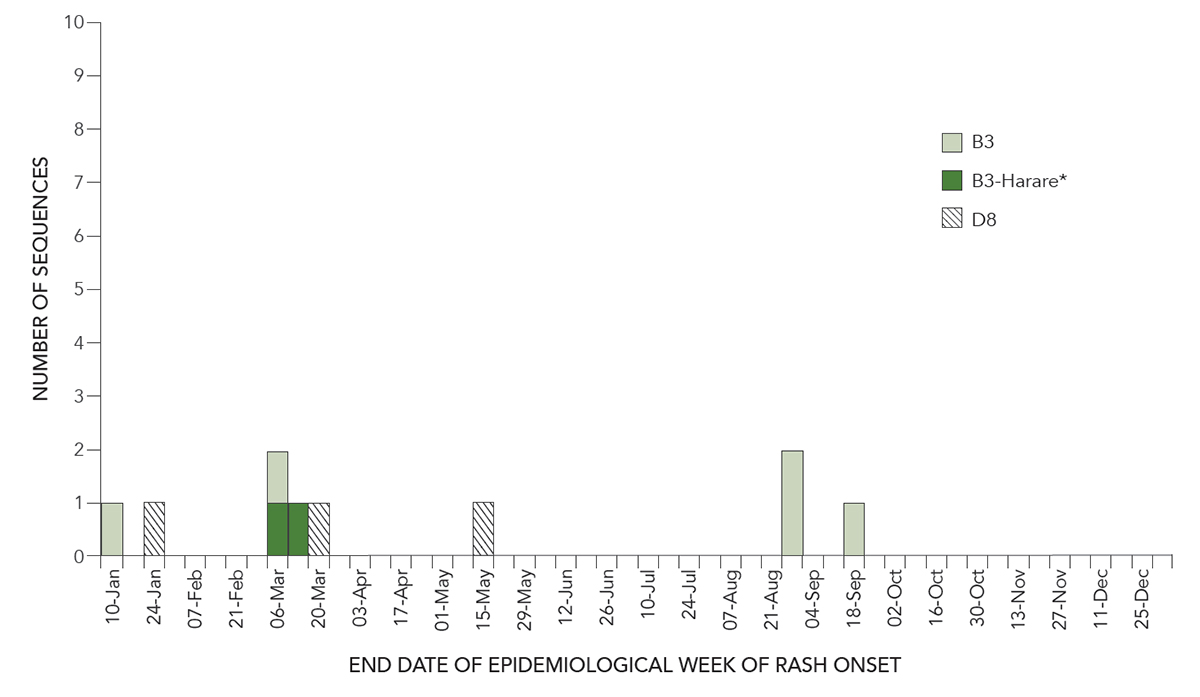
Figure 2 notes
- Figure 2 note †
-
Epidemiological weeks are assigned in accordance with the CDC guidelinesReference 10 with week 1 beginning on the first Sunday of the year.
- Figure 2 note *
-
Genotype B3 sequences identical to sequence variant MVi/Harare.ZWE/38.09 (GenBank accession number JF973033).
Figure 2 note * referrer
Figure 2 - Text version
| Epidemiologic Week Ending | B3 | B3 - HarareFugure 2 table note * | D8 | Total |
|---|---|---|---|---|
| 09-Jan-2016 | 1 | 0 | 0 | 1 |
| 16-Jan-2016 | 0 | 0 | 0 | 0 |
| 23-Jan-2016 | 0 | 0 | 1 | 1 |
| 30-Jan-2016 | 0 | 0 | 0 | 0 |
| 06-Feb-2016 | 0 | 0 | 0 | 0 |
| 13-Feb-2016 | 0 | 0 | 0 | 0 |
| 20-Feb-2016 | 0 | 0 | 0 | 0 |
| 27-Feb-2016 | 0 | 0 | 0 | 0 |
| 05-Mar-2016 | 1 | 1 | 0 | 2 |
| 12-Mar-2016 | 0 | 1 | 0 | 1 |
| 19-Mar-2016 | 0 | 0 | 1 | 1 |
| 26-Mar-2016 | 0 | 0 | 0 | 0 |
| 02-Apr-2016 | 0 | 0 | 0 | 0 |
| 09-Apr-2016 | 0 | 0 | 0 | 0 |
| 16-Apr-2016 | 0 | 0 | 0 | 0 |
| 23-Apr-2016 | 0 | 0 | 0 | 0 |
| 30-Apr-2016 | 0 | 0 | 0 | 0 |
| 07-May-2016 | 0 | 0 | 0 | 0 |
| 14-May-2016 | 0 | 0 | 1 | 1 |
| 21-May-2016 | 0 | 0 | 0 | 0 |
| 28-May-2016 | 0 | 0 | 0 | 0 |
| 04-Jun-2016 | 0 | 0 | 0 | 0 |
| 11-Jun-2016 | 0 | 0 | 0 | 0 |
| 18-Jun-2016 | 0 | 0 | 0 | 0 |
| 25-Jun-2016 | 0 | 0 | 0 | 0 |
| 02-Jul-2016 | 0 | 0 | 0 | 0 |
| 09-Jul-2016 | 0 | 0 | 0 | 0 |
| 16-Jul-2016 | 0 | 0 | 0 | 0 |
| 23-Jul-2016 | 0 | 0 | 0 | 0 |
| 30-Jul-2016 | 0 | 0 | 0 | 0 |
| 06-Aug-2016 | 0 | 0 | 0 | 0 |
| 13-Aug-2016 | 0 | 0 | 0 | 0 |
| 20-Aug-2016 | 0 | 0 | 0 | 0 |
| 27-Aug-2016 | 2 | 0 | 0 | 2 |
| 03-Sep-2016 | 0 | 0 | 0 | 0 |
| 10-Sep-2016 | 0 | 0 | 0 | 0 |
| 17-Sep-2016 | 1 | 0 | 0 | 1 |
| 24-Sep-2016 | 0 | 0 | 0 | 0 |
| 01-Oct-2016 | 0 | 0 | 0 | 0 |
| 08-Oct-2016 | 0 | 0 | 0 | 0 |
| 15-Oct-2016 | 0 | 0 | 0 | 0 |
| 22-Oct-2016 | 0 | 0 | 0 | 0 |
| 29-Oct-2016 | 0 | 0 | 0 | 0 |
| 05-Nov-2016 | 0 | 0 | 0 | 0 |
| 12-Nov-2016 | 0 | 0 | 0 | 0 |
| 19-Nov-2016 | 0 | 0 | 0 | 0 |
| 26-Nov-2016 | 0 | 0 | 0 | 0 |
| 03-Dec-2016 | 0 | 0 | 0 | 0 |
| 10-Dec-2016 | 0 | 0 | 0 | 0 |
| 17-Dec-2016 | 0 | 0 | 0 | 0 |
| 24-Dec-2016 | 0 | 0 | 0 | 0 |
| 31-Dec-2016 | 0 | 0 | 0 | 0 |
| Total | 5 | 2 | 3 | 10 |
Figure 2 Table Notes
|
||||
Six of the seven cases with genotype B3 detected were imported from the Eastern Mediterranean Region (4 from Pakistan and 2 from Afghanistan), where genotype B3 is endemicReference 17. Two of these were identical to the MVi/Harare.ZWE/38.09 named strain (GenBank accession number JF973033.1) while a third was identical to the MVs/Dublin.IRL/8.16 named strain (GenBank accession number KY013331.1). The seventh genotype B3 case was associated with travel in the European region and was identical to the MVs/Iasi.ROU/19.15 named strain (GenBank accession number KX372739.1).
Genotype D8 was detected in three cases and each case had a distinct viral sequence. One case, associated with travel to the Western Pacific Region, had a viral sequence identical to the MVi/Hulu Langat.MYS/26.11 named strain (GenBank accession number JX486001.1) while the remaining two viruses weren't identical to any named strains. One genotype D8 case was imported from India where this genotype is endemicReference 17.
Maintenance of measles elimination
There are four criteria set out by PAHO, for the ongoing verification of measles elimination (Table 4). As per the detail described earlier, Canada met or partially met three indicators.
| Criterion | Indicator | Description |
|---|---|---|
Verify the interruption of endemic measles cases for a period of at least three years from the last known endemic case, in the presence of high-quality surveillance. |
Zero cases of endemic transmission. |
Criterion met. Canada achieved measles elimination status in 1998 and this was recertified in 2016. Molecular and epidemiological data continue to demonstrate that no viral strain has circulated for a period of one year or more in Canada (Reference 6, Reference 9, Reference 18, Reference 19). |
Maintain high-quality surveillance sensitive enough to detect imported and import-related cases. |
>2 suspect cases per 100,000 population adequately investigated. |
Criterion partially met. CMRSS allows identifying imported and import-related cases, but suspected cases are not nationally notifiable. |
Verify the absence of endemic measles virus strains through viral surveillance. |
Measles genotype assessed in 80% of outbreaks. |
Criterion met. No outbreak occurred in Canada in 2016. However, there was one event with co-index cases exposed outside of Canada. Genotype was assessed in 9/10 events (90%). |
Verify adequate immunization in the population |
95% of population cohorts aged 1 to 40 years have received a measles-containing vaccine |
Criterion not met. Canada currently measures (biannually) measles vaccination coverage rates at 2 and 7 years of age, and therefore is unable to assess measles vaccination coverage for all ages 1 through 40 years. The 2013 estimates for measles-containing vaccine age 2 and 7 years are 89.6% and 85.5% respectively, below the indicator of 95% (Reference 20, Reference 21). |
Discussion
Eleven confirmed cases of measles, in 10 unique events, were reported in Canada in 2016. Almost all cases were imported (91%); one had an unknown source of exposure. This is the lowest number of cases reported annually since 2012 (n=9)Reference 8. No cases had a documented history of vaccination, nine were unvaccinated and two had an unknown vaccination history. The burden was highest among children, especially those aged less than one year. All hospitalized cases were in children less than five years of age. Ten cases had genotype information available: seven were B3, and three were D8 genotype, which reflected the genotypes circulating globally. Two cases had the same source of exposure outside of Canada but no outbreaks occurred in Canada in 2016.
Canada meets or partially meets three of the four PAHO essential indicators for maintenance of measles elimination. Canada has a high performing surveillance system for measles, which is able to detect imported and import-related cases as well as the infrequent cases with unknown source of exposure. Molecular epidemiologic laboratory data confirms the absence of a circulating endemic measles virus genotype in Canada.
Canada falls short of the criterion regarding measles containing vaccination coverage. Canada currently measures (biannually) measles vaccination coverage rates at 2 and 7 years of age, and therefore is unable to assess measles vaccination coverage for all ages 1 through 40 years as is set out in the PAHO elimination criterion indicator. The 2013 estimates for measles-containing vaccine age 2 and 7 years are 89.6% and 85.5% respectively, below the PAHO indicator of 95%Reference 20. Despite this, endemic transmission of the measles virus has not been re-established. Therefore, based on a combination of the epidemiologic, laboratory and vaccination coverage data, Canada's National Certification Committee recertified Canada's measles elimination status in 2016Reference 9.
The Global Vaccine Action Plan adopted by the World Health Assembly in 2012 set a goal of eliminating measles in four regions by 2015. Failure to close vaccination coverage gaps has resulted in a failure to meet the goalReference 22. Globally, measles elimination continues to be a public health priority, with all six WHO regions now aiming to achieve measles elimination by 2020Reference 23.
Measles continues to be an important public health issue globally. Although only 92 cases of measles were reported in the Region of the Americas in 2016, worldwide over 174,000 cases of measles were reported to the WHOReference 24.
Limitations
These data have limitations that merit consideration. The indicators of a well-performing surveillance system established by PAHO are based on investigation of measles-like illness (i.e., suspected cases), whereas only confirmed cases are nationally notifiable in Canada. As such, these data can only indirectly address the PAHO criteria. Moreover, information on mortality and detailed information on morbidity (e.g., length of hospitalization, sequelae) are not currently captured by CMRSS, limiting the ability to completely describe the burden of illness due to measles in Canada.
Conclusion
Both in Canada and abroad, maintaining high vaccination coverage with measles-containing vaccine remains a significant public health effort, as well as an essential component of a strategy for achieving and maintaining measles elimination. Although importations and suboptimal vaccination coverage continue to challenge Canada's elimination status, surveillance data provided strong evidence that measles elimination has been maintained.
Acknowledgements
PHAC gratefully acknowledge the continued cooperation and efforts of provincial and territorial surveillance and laboratory partners for providing and validating data captured by CMRSS, for referring specimens for molecular surveillance (genotyping) and for their review of the report content. PHAC wants to acknowledge the contribution of the National certifying committee in support of Canada continuous elimination status.
Appendix: Summary of measles events in Canada, ordered by earliest date of rash onset, 2016
| Event | Province | Number of cases | Genotype | Index case |
|---|---|---|---|---|
| 1 | ON | 1 | B3 (Not identical to named strain) |
|
| 2 | BC | 1 | D8 (Mvi/Hulu Langat.MYS/26.11) |
|
| 3 | BC | 1 | B3 (Not identical to named strain) |
|
| 4 | ON | 1 | B3 (Mvi/Harare.ZWE/38.09) |
|
| 5 | AB | 1 | B3 (Mvi/Harare.ZWE/38.09) |
|
| 6 | ON | 1 | D8 (Not identical to named strain) |
|
| 7 | ON | 1 | D8 (Not identical to named strain) |
|
| 8 | QC | 1 | N/A |
|
| 9 | ON | 2 | B3 (Not identical to named strain) |
|
| 10 | ON | 1 | B3 (Not identical to named strain) |
|
References
- Reference 1
-
Moss JW, Griffin E D, Measles, Seminar, The Lancet, 379; 9811 (2012) 153-164.
- Reference 2
-
World Health Organization (WHO). Monitoring progress towards measles elimination. Wkly Epidemiol Rec 2010;85(49):490-494.
- Reference 3
-
National Advisory Committee on Immunization (NACI). Statement on elimination of indigenous measles in Canada. Can Dis Wkly Rep 1980;6:33-4.
- Reference 4
-
Laboratory Centers for Disease Control (LCDC). Consensus Conference on Measles. Can Comm Dis Rep 1995;19(10).
- Reference 5
-
Pan American Health Organization (PAHO). The XXIV Pan American Sanitary Conference. Expanded program on immunization - Resolution CSP24.R16. (1994).
- Reference 6
-
King A, Varughese P, De Serres G, Tipples GA, Waters J, Working Group on Measles Elimination. Measles elimination in Canada. J Infect Dis 2004 May;189-Suppl 1:S236-42.
- Reference 7
-
Public Health Agency of Canada. Case definitions for diseases under national surveillance. Can Comm Dis Rep 2009;35-Suppl 2:71-72.
- Reference 8
-
Public Health Agency of Canada. Elimination of Measles Rubella and Congenital Rubella Syndrome in Canada, Documentation and Verification Report, submitted to PAHO December 2011.
- Reference 9
-
Public Health Agency of Canada, Sustainability of Measles, Rubella and Congenital Rubella Syndrome (CRS) Elimination, Country template for the update of country reports (PAHO/WHO), April 2016
- Reference 10
-
Centers for Disease Control and Prevention. MMWR Weeks fact sheet. Retrieved on August 2, 2017 from www.cdc.gov/nndss/document/MMWR_week_overview.pdf
- Reference 11
-
Mulders M, Rota P, Brown K, Goodson J. Genetic diversity of wild-type measles viruses and the global measles nucleotide surveillance database (MeaNS). Wkly Epidemiol Rec 2015;90(30):373.
- Reference 12
-
Tamura K, Peterson D, Peterson N, Stecher G, Nei M, Kumar S. Molecular evolutionary genetics analysis using maximum likelihood, evolutionary distance, and maximum parsimony methods. Mol Biol Evol 2011;28:2731.
- Reference 13
-
World Health Organization (WHO). Laboratory Network, Immunization, Vaccines and Biologics. [Updated March 10th 2016; Accessed April 4th 2017]
- Reference 14
-
Pan-American Health Organization (PAHO). Plan of action. Documentation and verification of measles, rubella and congenital rubella syndrome elimination in the region of the Americas. Technical Document. 2010.
- Reference 15
-
McLean HQ, Fiebelkorn AP, Temte JL, Wallace GS. Prevention of measles, rubella, congenital rubella syndrome, and mumps, 2013: Summary recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR 2013;62(RR04):1-34.
- Reference 16
-
National Advisory Committee on Immunization (NACI). Canadian immunization guide. Part 3: Vaccination of Specific Populations. Ottawa: PHAC; 2017. [Updated March 2017; Accessed April 2017]. www.canada.ca/en/public-health/services/publications/healthy-living/canadian-immunizationguide- part-3-vaccination-specific-populations/page-9-immunization-travellers.html
- Reference 17
-
Rota PA, Brown K, Mankertz A, et al. Global distribution of measles genotypes and measles molecular epidemiology. J Infect Dis 2011;204-Suppl 1:8514.
- Reference 18
-
Sherrard L, Hiebert J, Cunliffe J, Mendoza L, Cutler J. Measles surveillance in Canada: 2015. Can Comm Dis Rep 2016;42:139-45.
- Reference 19
-
Sherrard L, Hiebert J, Squires S. Measles surveillance in Canada: Trends for 2014. Can Comm Dis Rep 2015;41(7):157.
- Reference 20
-
Public Health Agency of Canada. Vaccine coverage in Canadian children: Highlights from the 2013 childhood National Immunization Coverage Survey (cNICS). [Updated October 2016; Accessed April 2017]. Ottawa: PHAC; 2015. http://healthycanadians.gc.ca/publications/healthy-living-vie-saine/immunization-coverage-children-2013-couverture-vaccinale-enfants/index-eng.php
- Reference 21
-
Public Health Agency of Canada. Vaccine coverage in Canadian children: Results from the 2011 Childhood National Immunization Coverage Survey. Ottawa: PHAC; 2015
- Reference 22
-
Strategic Advisory Group of Experts on Immunization, 2016 Midterm review of the Global Vaccine Action Plan, www.who.int/immunization/global_vaccine_action_plan/en
- Reference 23
-
World Health Organization (WHO). Measles and Rubella Global Strategic Plan 2012-2020 Midterm Review, Overarching conclusions, p.12
- Reference 24
-
World Health Organization (WHO). Immunization, Vaccines and Biologics, Measles Surveillance Data, Regional summary of reported measles cases [Updated March 2017, Accessed April 2017] www.who.int/immunization/monitoring_surveillance/burden/vpd/surveillance_type/active/big_ measlesregionalsummary.jpg?ua=1