Adverse Events Following Immunization (AEFI) Quarter 3 Report for 2016 (July 1 – September 30)
Safety Assessment Summary for Quarter 3:
- No vaccine safety signals were identified in Quarter 3 of 2016.
- This report presents 532 AEFI reports routinely received from federal, provincial and territorial health jurisdictions during Q3.
Background
Vaccines are closely monitored in Canada at all phases of the vaccine product ‘life cycle’ from discovery through market authorization (pre-market) and beyond, as people begin using them (post-market). Many stakeholders are involved in vaccine safety surveillance including the federal government, provincial, territorial and local public health authorities, health care providers, vaccine industry and the public. Provincial and territorial vaccination programs monitor AEFIs and report them to the Public Health Agency of Canada (the Agency). The Agency conducts post-market safety surveillance through the Canadian Adverse Events Following Immunization Surveillance System (CAEFISS). Vaccine safety concerns are monitored and addressed through the Vaccine Vigilance Working Group (VVWG).
An Adverse Event Following Immunization (AEFI) is defined as any untoward medical occurrence which follows immunization and which does not necessarily have a causal relationship with the usage of the vaccine. The adverse event may be any unfavourable or unintended sign, abnormal laboratory finding, symptom or disease. Serious AEFIs are those which are life-threatening, result in hospitalization or a prolongation of hospitalization, result in persistent or significant disability, or where the outcome is a birth defect or death, as defined by the World Health Organization (WHO). AEFIs not meeting the definition of a serious event are classified as non-serious.
WHO defines a vaccine safety signal as information (from one or multiple sources) that indicates a new and potentially causal association, or a new aspect of a known association, between a vaccine and an event previously unknown or incompletely documented that could affect health. Epidemiological studies are usually needed to assess the causal relationship between the vaccine and the signal. The primary purpose of vaccine post market surveillance is to detect safety concerns. These concerns include a possible increase in the severity or frequency of expected AEFIs, or occurrence of one or more unexpected events (i.e., an event that is not consistent with Canadian product information or labeling). This allows vaccination providers and public health vaccination program providers to take public health action at the level of the:
- individual (such as further investigations to confirm a diagnosis and determine possible causes, consultation to rule out allergy to one or more vaccine components, or evaluate whether or not to give subsequent doses of a vaccine), and/or
- vaccination program (such as investigation of a cluster of adverse events, review of procedures to ensure that vaccine storage requirements have been strictly followed, or consideration of a change in policy to adopt a less reactogenic vaccine).
The Agency also shares AEFI data with Health Canada’s Health Products and Foods Branch, the national regulatory authority for vaccines in Canada. This enables formal action related to vaccines marketed in Canada to take place if needed. These actions may include issuing communications to vaccination providers or the public regarding the safety concern or requiring additional information or investigation by the vaccine distributor, or changes to the product labeling.
Vaccine safety surveillance reports summarizing CAEFISS data are released by the Agency on a routine basis. The Quarterly Reports summarize all AEFI reports received by the Agency from January to March (Quarter 1), April to June (Quarter 2), July to September (Quarter 3) and October to December (Quarter 4), regardless of the date the vaccine was given.
In order to reflect variability in the AEFIs reported from year to year, each quarter’s data are shown along with an average of the preceding four years’ quarterly data; in other words, the data in this quarter, Quarter 3, are shown along with the average Quarter 3 data from the previous four years. However, because these data reflect reports received in the particular quarter, and not necessarily when the vaccine was given, they can be subject to variation depending on both when and how reports are received, processed and forwarded by provincial/territorial public health authorities as well as on the type of vaccine products used, distributed, and how many and which populations received them in a given quarter. Therefore, the ability to compare and interpret patterns in these data is limited. The report does provide a data snapshot that highlights serious and non-serious AEFI reports received for descriptive purposes.
Notes on interpretation: AEFI reports submitted to the Public Health Agency of Canada represent a suspicion, opinion, or observation by the reporter as opposed to an assertion or proof that the vaccine may have caused the event. Additional limitations to AEFI report data include potential underreporting, lack of certainty regarding the diagnostic validity of a reported event, missing information regarding other potential causes and other reporting biases. These biases are mitigated by the Agency through use of a reporting form for AEFI with a guide to its use, standardized medical coding using the Medical Dictionary for Regulatory Activities (MedDRA), follow-up with the jurisdictions for completeness of information, high reporting rates and inclusion of an active pediatric surveillance component in CAEFISS.
Results Highlighted for Quarter 3 of 2016
Data presented in this Quarterly Report (Q3) include AEFI case reports routinely received from July 1, 2016 to September 30, 2016 and comparisons are made to the average number of reports received in the same quarter over the previous four calendar years (2012-2015). The data analysed were extracted from the CAEFISS database on March 20, 2017 by the Agency. Due to technical issues in data submission in one jurisdiction since mid-2013, there has been a substantial decrease in the total number of AEFI reports.
All reports are processed and coded using MedDRA, a standardized medical terminology that supports data entry, retrieval, evaluation and presentation of clinical information and further coded with a main reason for reporting through a detailed review of individual case safety reports. Therefore, if more than one event is described, the one that is determined to have led to reporting is coded as the primary AEFI. In addition, all reports describing a serious event were reviewed and unless highlighted in this report, found either to be expected (based on known vaccine-related adverse reactions), to have alternate explanations not related to vaccination, or are currently being monitored or investigated further.
Number of AEFI and Serious AEFI Reports
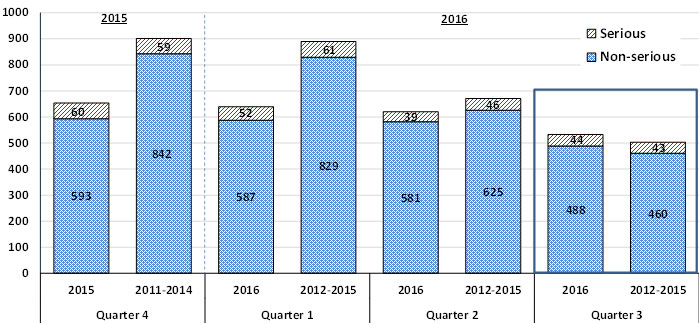
A total of 532 AEFI reports were submitted to the Agency in the third quarter of 2016; during Q3 of 2012, 2013, 2014 and 2015, the Agency received an average of 503 (range: 400-668) [Figure 1].
A total of 44 AEFI reports received by the Agency in Q3 of 2016 were classified as serious (8% of all AEFI reports). During Q3 of 2012, 2013, 2014 and 2015, the Agency received an average of 43 (range: 34-50) serious AEFI reports (7% to 10% of all AEFI reports).
Text Equivilant
This is a stacked columns bar graph. The bars show the total number of AEFI reports received each calendar quarter (Q) with Q1 encompassing January, February and March, Q2 April, May and June, Q3 July, August and September and Q4 October, November and December. The y-axis shows the total count for each quarter, ranging from 0-1000. The x-axis shows the quarter and ranges from Q1 to Q4. Two time periods are depicted on the graph. The first bars shows the total number of reports received in 2015 for Q4 and 2016 for Q1, Q2, and Q3, for non-serious cases in blue and serious cases in red: non-serious: 593 in Q4, 587 in Q1, 581 in Q2, and 488 in Q3; serious: 60 in Q4, 52 in Q1, 39 in Q2, and 44 in Q3. A second set of bars shows the average number of reports of each quarter from 2011 to 2014 for Q4 and 2012 to 2015 for Q1, Q2, and Q3, for non-serious cases in blue and serious cases in red: non-serious: 842 in Q4, 829 in Q1, 625 in Q2, and 460 in Q3; serious: 59 in Q4, 61 in Q1, 46 in Q2, and 43 in Q3.
Frequency of Serious and Non-serious AEFI Reports by Age Group
Table 1 shows the number of serious and non-serious AEFI reports by age group in Q3 of 2016, with no significant change when compared to the 2012-2015 Q3 average.
| Age Group | Serious AEFI reports | Non-serious AEFI reports | ||
|---|---|---|---|---|
| 2016 | Average 2012-2015 | 2016 | Average 2012-2015 | |
| 0 to <1 year | 20 | 16 | 100 | 83 |
| 1 to <2 years | 12 | 16 | 92 | 77 |
| 2 to <7 years | 5 | 3 | 33 | 58 |
| 7 to <18 years | 4 | 5 | 70 | 71 |
| 18 to <65 years | 3 | 3 | 136 | 132 |
| 65+ years | 0 | 1 | 54 | 32 |
| Unknown | 0 | 0 | 3 | 9 |
| Total | 44 | 43 | 488 | 460 |
AEFIs by Major Classification
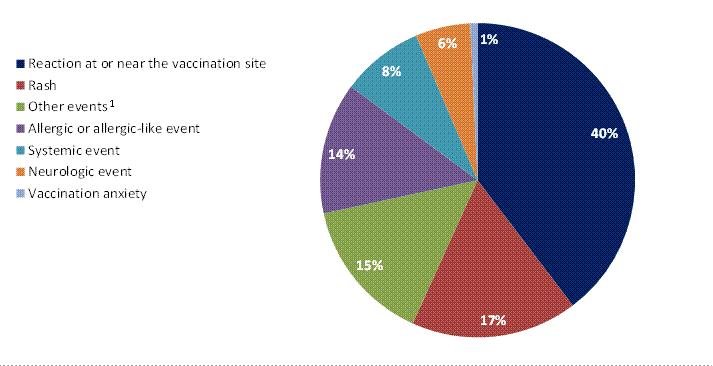
Figure 2 presents the main types of AEFIs (both serious and non-serious) reported during Q3 of 2016. Most of the AEFIs reported are vaccination site reactions.
Text Equivilant
This is a pie chart presenting the main reasons for reporting an adverse event following immunization during Q3 of 2016. In order of decreasing frequency, main reasons for reporting are: reaction at or near the vaccination site (40%), rash (17%), other events (15%), allergic or allergic-like event (14%), systemic event (8%), neurologic event (6%), para/anaesthesia, intussusception, arthritis, hypotonic-hyporesponsive episode, thrombocytopenia, persistent crying, or parotidis (---%), and vaccination anxiety (1%).
The main types of AEFI reported by level of seriousness for Q3 of 2016 compared to the 2012-2015 Q3 average are shown in Table 2. In Q3 of 2016 as well as in the past four years, reactions at or near the vaccination site, rash and allergic or allergic-like events were the main AEFIs reported for non-serious cases; neurologic events (which are most often seizures triggered by fever) and systemic events (i.e., events involving many body systems often accompanied by fever) were the most frequent AEFIs reported for the serious cases. The number of allergic or allergic-like reactions increased in 2016 due to a change in the classification of serious cases in mid-2015, as now all anaphylaxis cases are coded as life-threatening and therefore classified as serious, even if they did not result in hospitalization, prolongation of hospitalization, or death.
| Primary AEFI reported | Serious AEFI reports | Non-serious AEFI reports | ||
|---|---|---|---|---|
| 2016 | Average 2012-15 | 2016 | Average 2012-15 | |
| Reaction at or near the vaccination site | 2 | 3 | 209 | 174 |
| Rash | 1 | 0 | 90 | 99 |
| Allergic or allergic-like event | 8 | 1 | 64 | 44 |
| Systemic event | 10 | 11 | 35 | 59 |
| Neurologic event | 13 | 18 | 17 | 14 |
| Vaccination anxiety | 0 | 0 | 4 | 4 |
| Vaccination error | 0 | 0 | 0 | 5 |
| Other eventsTable Note 1 | 10 | 10 | 69 | 62 |
| Total | 44 | 43 | 488 | 460 |
|
||||
Vaccines Administered in AEFI Reports
Table 3 lists the most commonly administered vaccines among AEFI reports received for Quarter 3 of 2016. The majority of AEFIs (serious and non-serious) were reported following the administration of pneumococcal, DTaP infant series, measles, mumps, rubella, varicella (MMRV and MMR + V) and meningococcal vaccines, which is consistent with the high number of vaccinations scheduled in children and often given in conjunction with each other. Other than DTaP infant series which had 2 more serious cases, fewer serious reports were received for these vaccines in 2016 compared to the 2012-2015 average.
| Vaccines administered | Serious AEFI reports | Non-serious AEFI reports | ||
|---|---|---|---|---|
| 2016 | Average 2012-2015 | 2016 | Average 2012-2015 | |
| 1. DTaP booster | 1 | 1 | 5 | 22 |
| 2. DTaP infant series | 19 | 17 | 138 | 101 |
| 3. Hepatitis B | 3 | 2 | 37 | 34 |
| 4. Human papillomavirus (HPV) | 3 | 1 | 31 | 25 |
| 5. Influenza | 5 | 3 | 20 | 31 |
| 6. Measles, mumps, rubella, varicella (MMRV and MMR + V) | 16 | 21 | 133 | 129 |
| 7. Meningococcal | 11 | 18 | 97 | 88 |
| 8. Other vaccines | 0 | 1 | 30 | 23 |
| 9. Pneumococcal | 23 | 25 | 176 | 126 |
| 10. Rotavirus | 12 | 8 | 52 | 33 |
| 11. Tdap booster | 4 | 1 | 86 | 73 |
| 12. Travel vaccines | 0 | 2 | 35 | 54 |
| 13. Zoster virus | 0 | 1 | 27 | 25 |
|
||||
Summary
This Quarter 3 report for 2016 is based on reports of adverse events received at the Agency from federal/provincial/territorial public health authorities and active, pediatric hospital based surveillance. Detailed evaluation of the reports and reporting patterns in collaboration with provincial/territorial vaccine safety focal points of the VVWG and Health Canada have not identified any vaccine safety signals of concern. The tables and figures in this report provide a snapshot of the data provided to, and reviewed by, the PHAC.