Canadian Pain Task Force Report: March 2021
(PDF Version, 572 KB, 23 pages)
An action plan for pain in Canada
Table of contents
- Opening remarks
- Background and context
- Pain in Canada: A Public Health emergency in need of action
- The action plan for pain
- Goal #1 - Pain is recognized as a public health priority and coordination of action across jurisdictions spurs collaboration, leadership, and support to ensure a consistent approach to pain throughout Canada
- Goal #2 - People have equitable and consistent access to a continuum of timely, evidence-informed, and person-centred pain care and supports across jurisdictions
- Goal #3 - People living with pain and health professionals have the knowledge, skills, and educational supports to appropriately assess and manage pain based on population needs. The broader community understands pain as a legitimate, biopsychosocial condition and stigma is reduced
- Goal #4 - Pain research and related infrastructure enables discovery, catalyzes innovation, and results in the translation of knowledge into real world impact
- Goal #5 - Data enables effective monitoring of pain and facilitates improvement of health system quality
- Goal #6 - There is improved and equitable access to services for populations disproportionately impacted by pain
- Conclusion and next steps
Opening remarks
The Canadian Pain Task Force (CPTF) was established in 2019 to provide advice to guide the federal government toward an improved approach for the prevention and management of chronic pain, a diagnosis affecting nearly 8 million people living in Canada. The Task Force was asked to assess the current state of pain, resulting in our first report, and to identify best practices and an improved approach to care, education and awareness, research and related infrastructure, and health system monitoring, resulting in our second report. In December 2020, the Task Force mandate was strengthened and accelerated to provide recommendations on priority actions. These actions are meant to ensure that people with pain are recognized and supported and that pain is understood, prevented, and effectively treated across Canada.
The strengthening of the Task Force mandate reflects the urgency to take action on pain. The turbulent events over 2020 have laid bare the significant impacts of systemic inequity on the health of people in Canada. The COVID-19 pandemic, racial injustice, growing income inequity, and the opioid overdose crisis have exposed many shortcomings in our society and in the health system. They have also created an unprecedented opportunity for broad system reform.
The recommendations presented in this Action Plan build on system improvement efforts underway in federal, provincial, territorial, and regional jurisdictions. The Plan lays out specific and targeted actions necessary to improve outcomes for people living with chronic pain and to reduce its impact on families, communities, and society. Recommendations are clustered around six primary goals:
- Enable coordination, collaboration, and leadership across Canada
- Improve access to timely, equitable, and patient-centred pain care
- Increase awareness, education, and specialized training in pain
- Support pain research and strengthen related infrastructure
- Monitor population health and health system quality
- Ensure equitable approaches for populations disproportionately impacted by pain
Addressing chronic pain requires multiple and diverse approaches to change, from policy and regulation to changes in programs, practices, and attitudes. It will require broad engagement and depend on perseverance, collaboration, commitment, leadership, and resources. While presenting this action plan is a critical milestone, we recognize it is but one step in a longer journey. We have a lot to build on: advocacy and peer support, established and emerging networks, clinical experts, world-renowned researchers, and growing awareness among the public and policy makers. Together, we will work to create a better future for all people living with and impacted by pain.
With sincere gratitude,
The Canadian Pain Task Force
Fiona Campbell, Co-Chair
Maria Hudspith, Co-Chair
Manon Choinière
Hani El-Gabalawy
Jacques Laliberté
Michael Sangster
Jaris Swidrovich
Linda Wilhelm
Background and context
The Canadian Pain Task Force
The Canadian Pain Task Force (CPTF) was established to provide advice and information to guide Health Canada toward an improved approach to the prevention and management of chronic pain in Canada. It is comprised of people personally impacted by chronic pain, Indigenous Peoples, researchers, educators, and health professionals with expertise across many disciplines in the field of pain. An External Advisory Panel provides additional subject-matter guidance and further broadens this expertise.
Phase I Report
In June 2019, the Task Force submitted its first report to Health Canada – Chronic Pain in Canada: Laying a Foundation for Action. The report highlighted significant gaps in access to timely and appropriate pain care; education, training, and awareness for patients, the public, and health care professionals; research and related infrastructure; and chronic pain surveillance and health system quality monitoring.
Phase II Report
Between July 2019 and August 2020, the Task Force conducted national consultations with over 2000 stakeholders (representing a sampling of the wide spectrum of opinions regarding chronic pain) and reviewed evidence to identify best and leading practices, areas for action, and elements of an improved approach to better understand, prevent, and manage chronic pain in Canada. The results of this engagement and evidence synthesis, including the voices of people living with pain, were summarized in Working Together to Better Understand, Prevent and Manage Chronic Pain: What We Heard.
Phase III Goals
In January 2021, the mandate of the CPTF was strengthened and accelerated to provide recommendations on priority actions with a focus on ensuring people with pain are recognized and supported and that pain is understood, prevented, and effectively treated across Canada. This final CPTF report provides an Action Plan consisting of recommendations across six goals:
- Enable coordination, collaboration, and leadership across Canada
- Improve access to timely, equitable, and person-centred pain care
- Increase awareness, education, and specialized training for pain
- Support pain research and strength related infrastructure
- Monitor population health and health system quality
- Ensure equitable approaches for populations disproportionately impacted by pain
These six goals represent a national consensus, echoing international agreement, on the key areas for action that will transform how pain is understood and treated. An overview of the evidence underpinning these goals can be found in the CPTF’s first two reports.
Pain in Canada: A Public Health emergency in need of action
Chronic pain is a disease in its own right
The International Association for the Study of Pain defines pain as “an unpleasant sensory and emotional experience associated with, or resembling that associated with, actual or potential tissue damage”. For most people, pain is temporary and serves as a warning that something is wrong, that something has caused or may cause damage to some part of our body. This is acute pain, which usually resolves as we heal.
When pain persists for longer than 3 months, it is defined as chronic. The World Health Organization (WHO) in its 11th revision of the International Classification of Diseases (ICD-11) includes chronic pain as a diagnosis in its own right, further categorizing chronic primary pain and chronic secondary pain. Chronic primary pain refers to pain that exists despite complete tissue healing, or pain that has no identifiable cause. Chronic secondary pain occurs in association with underlying diseases (e.g., rheumatoid arthritis).
Biological, psychological, spiritual, environmental, and social factors influence our experience of pain. Chronic pain, like other chronic diseases, is best understood within a biopsychosocial framework, and its treatment should integrate pharmacological, physical, psychological, spiritual, self-management, and other approaches, as appropriate.
Nearly 8 million people in Canada live with chronic pain
It is a critical time for action on pain in Canada. An estimated 7.6 million, or one in five people (across the lifespan), live with chronic painFootnote 1, many of whom report it adversely affecting some or most daily activities. Pain impacts all demographics in Canada, although not equally. One in five children and youth experience ongoing pain, which can have affects across the life course. It is even more common as we age, with approximately one in three people over 65 experiencing chronic pain. As Canada’s population ages, the prevalence of chronic pain and its impacts are expected to grow.
Like many other chronic conditions, chronic pain disproportionately affects seniors, people living in poverty, people living with mental health and substance use disorders, people working in the trades and transportation industry, Veterans, Indigenous Peoples, certain ethnic and racialized communities, sexually and gender diverse persons, those who have experienced past trauma or violence, persons with disabilities, and women. Such disparities demonstrate the importance of addressing equity as a cornerstone of Canada’s response to chronic pain.
Untreated pain results in poor outcomes for individuals, families, and communities
Pain impacts people’s ability to work, attend school, and participate in family and community life. Chronic pain often accompanies other physical and mental health conditions, from sickle cell disease, arthritis and diabetes to post-traumatic stress disorder, depression, and anxiety. Chronic pain is largely invisible, and those affected often feel disbelieved and stigmatized. Living with chronic pain can take a tremendous toll on sleep, physical functioning, mental health, and social relationships. Children with pain have unique needs and when their pain goes unmanaged, it is associated with poor academic, social, and developmental outcomes, including higher rates of chronic pain, substance use, and mental health issues in adulthood. The lack of specialized pain services, the lack of effective treatment for some chronically painful conditions, long wait times, barriers to access for care, and the scarcity of health professionals trained in pain management exacerbate hopelessness for people who live with pain.
“My pain has had a significant impact on my life. It impacts my ability to get out of bed, get ready, go to school, go to work, exercise, and spend time with my friends and loved ones. Pain causes me to compromise on every aspect of my life.”
Person living with pain
Chronic pain is taking a massive economic toll
Chronic pain also has a tremendous impact on the economy. According to Health Canada’s analyses, the total direct (health care) and indirect (lost productionFootnote 2) cost of chronic pain in 2019 was $38.2 - $40.3 billion. Direct costs (expenditures for physician’s services, prescription drugs, and hospital inpatient and outpatient care) were between $15.1 and $17.2 billion, representing over 10% of total combined health expenditures for these costs.
Preliminary analysis by Health CanadaFootnote 3 estimates the total number of individuals living with chronic pain will increase by 17.5% from 2019 to 2030 due to population growth and agingFootnote 4. Preliminary projections indicate as many as 8.3 million Canadians may live with chronic pain by 2025 and as many as 9.0 million by 2030. By 2030, the estimated direct costs will rise to $20.5 - $23.4 billion and indirect costs to $31.5 billion. This results in a total cost increase of 36.2% during this period ($52 - $55 billion).
Despite the substantial cost, people living with pain in Canada continue to face tremendous barriers to care, employment supports, and other services.
Chronic pain and its impacts can be reduced
A substantial proportion of people develop chronic pain following injury (e.g., at work or home, through sports or motor vehicle accidents) or surgery. Various risk factors contribute to the development of chronic pain, providing a substantial opportunity to intervene early, to prevent pain from becoming intractable, and to mitigate its many impacts.
Preliminary analysis by Health Canada estimates a 1% annual reduction in the number of Canadians living with chronic pain could yield an average annual saving of $165.2 - $188.5 million (2020 CAD) in direct costs, and an average annual saving of $232.6 million (2020 CAD) in indirect costs between 2020 to 2030. The estimated present value of cumulative savings in direct and indirect cost is $3.5 - $3.7 billion (2020 CAD) over the 10-year periodFootnote 5.
Various strategies can reduce the likelihood that pain will persist over time: improving surgical techniques, preventing and managing injury and trauma, optimizing pain management in the peri-operative period, and intervening early with multi-modal, biopsychosocial approaches to address risks for chronicity and comorbidities. Many existing strategies, including those focused on primary prevention of chronic disease through improved nutrition, healthier built environments, improved sleep, increased physical activity, and supports for mental health and resiliency could also potentially reduce the occurrence and severity of chronic pain and improve function.
Preliminary analysis by Health Canada estimates that a 3% to 5% annual improvement in functionalityFootnote 6 and related improvements in production (i.e., unemployment and absenteeism), among individuals living with activity-limiting chronic pain could result in an average annual saving of $132.4 million to $217.4 million (2020 CAD) in indirect costs between 2020 and 2030. The estimated present value of cumulative savings in indirect costs is in the range of $1.2 to $1.9 billion (2020 CAD)Footnote 7 over the 10-year period.
Investment in pain prevention and management has the potential to not only improve outcomes for Canadians but also deliver sizable savings
"It may surprise people to learn that pain itself is not the biggest factor affecting my life but the by-product of the pain – financial insecurity. Most significant was having to leave the workforce long before retirement age. At the time of my highest earning potential, I was forced to stop working because of unremitting chronic pain."
Person living with pain
Untreated chronic pain is connected to the opioid overdose crisis
A large proportion of people who use substances also live with untreated chronic pain. People who use substances and their families often point to the lack of appropriate pain care as a contributor to their substance use and an impediment to successful treatment and recovery. The substance use system is also poorly connected to other systems (e.g., primary care, tertiary multidisciplinary pain treatment clinics); this lack of coordination can further complicate access to care and exacerbate substance use-related harms. Numerous factors have contributed to a significant increase in opioid-related harms and deaths over the last two decades; increase in opioid prescribing, particularly for people at risk of substance use disorder, lack of access to non-opioid options to treat pain, widespread market availability of opioids, the introduction of potent illicit synthetic opioids (e.g., fentanyl), and association between high doses and risk of death as well as broader socio-economic drivers of substance use (e.g., racial injustice, poverty, trauma).
Efforts to address opioid-related harms have led to serious and unintended consequences for some people living with chronic pain, including unmanaged pain, increased stigma, reduced access to care for people who use opioids for pain relief, and preventable deaths. This has led some people to obtain illicit drugs to self-medicate, putting them at serious risk of overdose. Despite widespread decreased opioid prescribing, and investments in a continuum of harm reduction, treatment, and prevention initiatives, there are record high numbers of overdose deaths in Canada. We must urgently address untreated pain as a driver of this crisis.
Pain and its impacts are exacerbated by the COVID-19 pandemic
For many people with pre-existing chronic pain, the COVID-19 pandemic has led to stress, social isolation, exacerbation of concurrent mental health conditions, reduced opportunities to maintain physical functioning, and increased pain and disability. The pandemic-related disruptions in health care and services have reduced access to supports and therapies that people living with pain rely on to maintain quality of life. Elective surgeries and procedures to alleviate pain have been postponed, resulting in prolonged pain and reduced ability to function. Such challenges have contributed to increased reliance on prescription medications, including opioids, and increased use of other substances.
As the COVID-19 pandemic continues, and the effects of public health measures are felt over the longer term, people who live with pain are increasingly vulnerable to harm. People who live with chronic conditions – many of which are associated with chronic pain – have been shown to experience worse outcomes from COVID-19 infection. There is also the potential for the pandemic to result in large numbers of new cases of complex chronic pain over time due to not only these noted challenges but also post-viral complications among those who were infected.
There is an emerging consensus about what works and what is needed for meaningful change
Many people living with pain, health care professionals, researchers, policy makers, and non-governmental organizations have been contributing to a movement for action on pain in Canada. Innovative treatments and clinical models, proven educational approaches, novel support programs, and world-renowned research ready for real-world implementation already exist across the country. Through the CPTF’s assessment and consultation phases, it is clear that there is consensus on both the gaps and the remedies. What is needed now is national policy, coordination, and resources to amplify, build, and accelerate this work, and to address current gaps and inequities.
The opportunity for integrating pain into system reform and health in all policies
Large-scale and complex societal problems such as the COVID-19 pandemic, racial injustice, poverty, and the overdose crisis have exposed many shortcomings in the health system. They have also resulted in fast-tracking of meaningful solutions and created an unprecedented opportunity for broad system reform. People in Canada have witnessed accelerated changes in health care that have improved access, safety, and efficiency for some services. Rapid mobilization of virtual care, access to expanded income supports, improved access to prescription medications and pharmaceutical alternatives to toxic drugs, expanded access to mental health services, and enhanced self-management tools and resources are a few of the many changes that will contribute to improved health. Such change will also have secondary benefits, improving assessment, prevention, and management of chronic pain for millions of Canadians.
The Action Plan and recommendations presented in this report leverage such health system expansion and improvement activities underway in federal, provincial, territorial, and regional jurisdictions. This Plan lays out specific and targeted actions necessary to improve outcomes for people living with chronic pain in Canada and to reduce its impact on families, communities, and society. It provides an ideal opportunity for federal, provincial, territorial, Indigenous, and other leaders to champion and dedicate resources to take action on chronic pain.
The action plan for pain
Addressing chronic pain requires multiple and diverse approaches to change. National strategies conventionally articulate top-down approaches through policy and regulation. Although these levers are tremendously powerful, policy change – on its own – will not realize the overarching outcome of the Action Plan: improved prevention and quality of life for people living with pain and fewer impacts on individuals, families, community, and society. Shifting outcomes also requires culture change – changing peoples’ attitudes, judgements, and ways of being.
Building from the extensive evidence reviews and consultations informing the work of the CPTF reports to date, this Plan recommends a wide range of actions to ensure people with pain in Canada are recognized and supported and that pain is understood, prevented, and effectively treated. The roles and influence of many actors are noted; governments, provincial and regional health authorities, educational institutions, non-profit organizations, and other stakeholder groups will need to consider how best to make strategic and targeted choices on specific activities, mindful of their respective mandates and levers for action.
Equity lens
Overlapping biological, psychological, social, environmental, cultural, historical, and other factors not only influence how pain is experienced, but also impact who develops chronic pain in the first place and how it is treated. Addressing systemic inequities must be a central, integrated pillar of Canada’s efforts to understand, prevent, and treat pain; the Task Force has applied this lens to the following recommendations.
Figure 1: An Action Plan for Pain in Canada
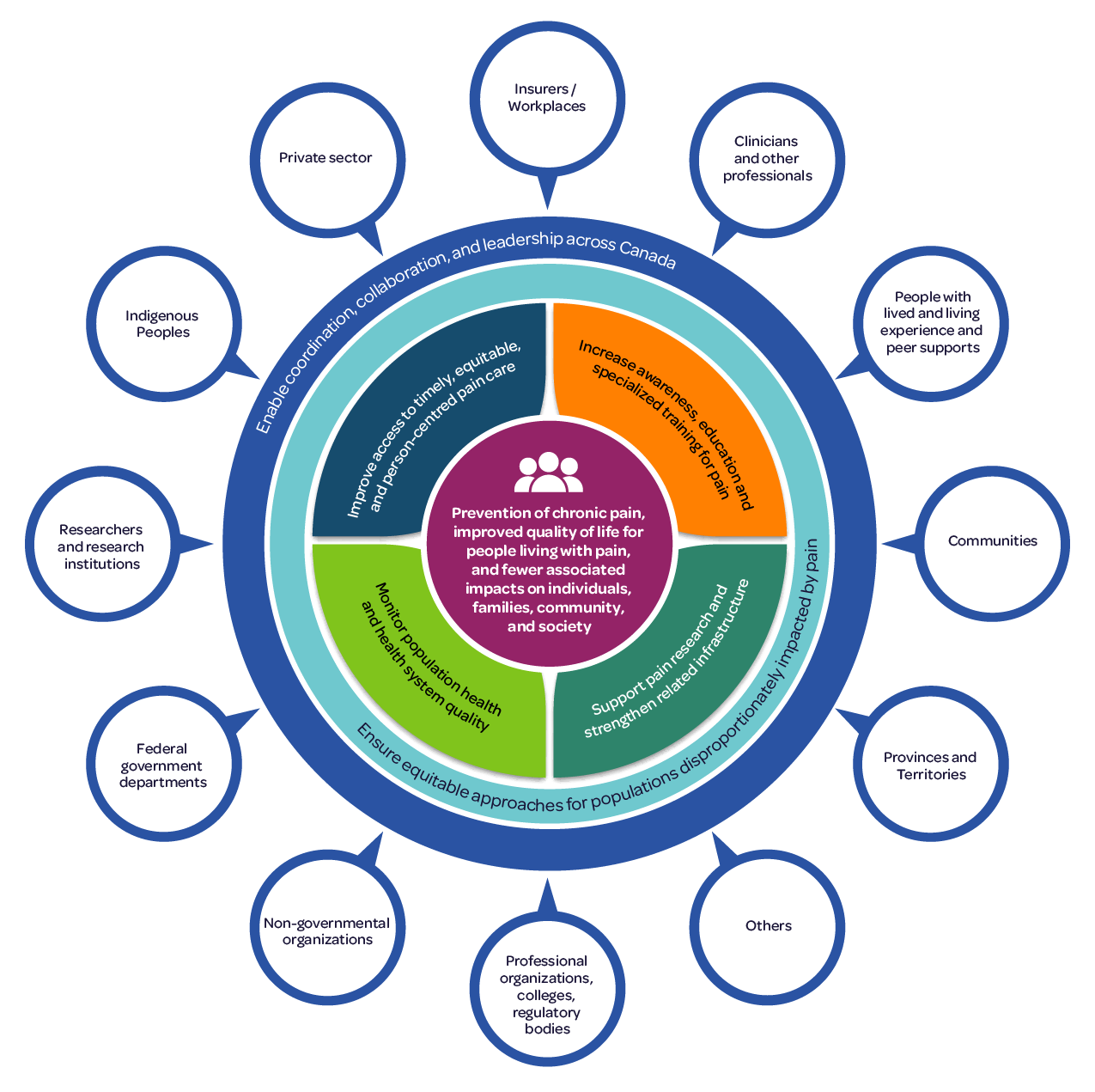
Figure 1 - Text Description
Concentric circles showing the interplay between the action plan goals and the outcome. The centre circle is the outcome:
- Prevention of chronic pain, improved quality of life for people living with pain, and fewer associated impacts on individuals, families, community, and society.
Moving outwards, the next concentric circle is divided into four quadrants:
- Improve access to timely, equitable, and person-centred pain care
- Increase awareness, education, and specialized training for pain
- Support pain research and strength related infrastructure
- Monitor population health and health system quality
The four quadrants are surrounded by two more concentric circles, the goals of:
- Ensure equitable approaches for populations disproportionately impacted by pain
- Enable coordination, collaboration, and leadership across Canada
The types of stakeholders and partners make up the outer layer.
Concentric circles showing the action plan outcome supported by four central goals, with overarching goals of equity, coordination, and stakeholder involvement.
This figure depicts the Canadian Pain Task Force Action Plan for pain in Canada. At its centre is the overall outcome the action plan hopes to achieve. This outcome will be enabled with a focus on four main goals related to improving access, education, research, and surveillance as well as foundational goals underpinning all recommendations that include attention to equity for different populations and coordination, collaboration, and leadership across Canada.
Outcome: Prevention of chronic pain, improved quality of life for people living with pain, and fewer associated impacts on individuals, families, community, and society.
Goal #1 - Pain is recognized as a public health priority and coordination of action across jurisdictions spurs collaboration, leadership, and support to ensure a consistent approach to pain throughout Canada
Chronic pain is a complex problem that currently exists everywhere and yet belongs nowhere. It is highly prevalent, drives utilization across virtually every domain of health care, and has significant impacts in many other systems. Despite this, chronic pain remains an issue without an institutional home or a champion accountable to drive improvement.
“We urgently need an [action plan] embraced by policymakers, health professionals, and patients to provide effective pain management services for all Canadians who need them.”
Person living with pain
This Action Plan outlines specific policy and program recommendations for federal, provincial, and territorial governments and calls others – from federal agencies to Pan-Canadian Health Organizations – to act within their jurisdictions and spheres of influence. Engaging a diverse network, with a range of skills, perspectives, resources, and tools, is necessary when tackling large-scale and societal problems. Many organizations and stakeholders have a role to play but coordination is required to foster collaboration, reduce duplication of effort, and ensure results are achieved over time.
Over the last decade, people living with chronic pain have begun to mobilize in communities (both geographic and online) across Canada and internationally, non-profit organizations have been formed, networks of pain researchers have been created, and clinicians and educators have come together to change practice. This momentum represents a tremendous opportunity; harnessing the power of this movement will be key to success and is necessary for achieving each of the ensuing goals.
Recommended actions:
- Support the development of a national mechanism that enables collaboration and brings together federal, provincial and territorial governments, regulators and health professional organizations, people with lived experience, Pan-Canadian Health Organizations, non-governmental organizations, researchers, employers, and other stakeholders with a role to play in the Action Plan’s implementation for regular knowledge sharing and planning around future actions.
- Integrate chronic pain as a condition eligible for funding under relevant federal, provincial, and territorial funding programs (e.g., the Integrated Strategy for Healthy Living and Chronic Disease, Health Care Policy Contribution Program, Substance Use and Addictions Program, Supporting Pathways to Care funding program).
- Convene recipients of past funding with a focus on pain management to discuss lessons learned and identify future opportunities and needs.
- Establish a funding mechanism to enable the development and coordination of national, provincial, territorial, and relevant community-based pain initiatives, with a particular emphasis on supporting patient and peer-led organizations.
- Collaborate with Pan-Canadian Health Organizations, such as Healthcare Excellence Canada to accelerate the identification, spread, and scale of pain-related health care innovations.
- Empower each Province and Territory to develop a provincial pain strategy and/or coordinated action plan to enable future activities and system improvements. Such work should have a mechanism for sharing approaches and lessons learned.
- Increasing federal, provincial, and territorial health funding to improve access to evidence-informed pain prevention and treatment services.
- Create a mechanism to oversee and coordinate the implementation of the Action Plan, connect governments and stakeholders, monitor progress, and report back to stakeholders through a formal evaluation after 3-5 years to identify gaps, further areas of opportunity, and additional overarching goals.
- Create a series of working groups involving various federal, provincial, and territorial government departments with an interest in pain with dedicated mandates and terms of reference.
Goal #2 - People have equitable and consistent access to a continuum of timely, evidence-informed, and person-centred pain care and supports across jurisdictions
Pain – whether acute or chronic – must be appropriately treated and/or managed. Knowledge of risk factors that drive acute pain to become chronic are emerging, presenting an opportunity to both mitigate risk and enhance protective factors. Timely access to evidenced-informed strategies to prevent the transition from acute to chronic pain will help substantially reduce prevalence of chronic pain in Canada.
People in Canada currently have inconsistent and insufficient access to pain services in primary care, and wait too long for speciality services. Evidence points to the need for access to a broad spectrum of options matched to the unique needs of each individual, including self-management, primary care, wellness-oriented programming, community-based care, specialized services, and interprofessional care.
Recommended actions:
System reform and innovative person-centred pathways and models of care
- Leverage federal, provincial, and territorial governments and existing government committees on health workforce development to discuss the support of alternative clinician reimbursement models that reflect the complex needs of people living with pain and improve remuneration and incentives for team-based care and biopsychosocial approaches, particularly at the primary care level and in the delivery of virtual care.
- Convene federal, provincial, and territorial governance bodies to develop a health human resource strategy designed to build pain specialist capacity and ensure adequate succession planning across the multiple health professions involved in pain care.
- Assemble federal, provincial, and territorial governments to discuss how best to develop and implement innovative person-centred care pathways (such as stepped care, hub and spoke models, or transitional pain services) to improve early access to pain assessment, treatment, and management.
- Enable models that cross provincial boundaries to support seamless care and consistent access to specialty hubs.
- Ensure adequate connection of rural, remote, and Indigenous communities to specialty networks, hubs, and services.
- Integrate pain management into broad system initiatives devoted to building capacity for virtual care. Harness technology to scale a virtual continuum of pain care that includes online self-management programs, peer and lay-enabled programs, clinician-supported self-management, and person-centred primary, secondary, and tertiary care.
- Establish mechanisms in all jurisdictions to provide support, coordination of care, and assistance to people living with pain as they navigate the health system and the resources available to manage pain and other co-morbidities.
Regulatory measures and reforms
- Build capacity among health professionals and community-based organizations to support people living with intractable pain who are considering medical assistance in dying, ensuring people are directed to appropriate care and treatment options and have adequate psychosocial supports.
- Permanently implement regulatory changes to the Controlled Drugs and Substances Act enacted during the COVID-19 pandemic to extend pharmacist authority with the aim of ensuring access to opioid medications for all populations that need them.
Tax and fiscal measures
- Expand access to evidence-informed self-management, pharmacological, physical, psychological, and spiritual and traditional Indigenous medicine and practice approaches to peoples who receive direct federal health care coverage (Veterans, Indigenous Peoples, active Military Personnel, and people who are incarcerated). Consider how best to provide assistance in the navigation of the health system, treatment options, and potential transitions in care.
- Expand access to a broader spectrum of evidence-informed pain treatments under provincial health care coverage, including working with private insurers to incentivize expanded coverage of self-management, pharmacological, physical, psychological, and spiritual and traditional Indigenous medicine and practice approaches into insurance plans.
- Consider how to improve federal and provincial tax credits for eligible medical and paramedical expenses to reduce the financial burden on people living with pain who must pay out-of-pocket for pain management services. Consider alternative tax measures or direct payment options specific to individuals and households with low-income.
- Undertake a feasibility study to explore fiscal measures (e.g., employer subsidies, enhanced health benefits) that would address untreated pain in the workplace, including impacts on employees, caregivers, and families.
- Convene stakeholders to explore options and innovative approaches for reimbursement of services currently not covered in public systems.
National standards and guidance
- Assemble federal, provincial, and territorial governments to work together with all medical regulatory authorities to issue a statement and other guidance regarding the risks associated with rapid opioid discontinuation and tapering, and the dangers of opioid deprescribing in the absence of shared decision-making with patients. Such guidance must also emphasize the need to end discrimination against people living with pain and denial of care based on a history or current use of opioids.
- Create a national mechanism to develop and disseminate pain-related guidance and best practices in the organization and provision of care. The mechanism must also include dedicated activities that support knowledge translation and mobilization as well as ongoing review and evaluation of guidelines over pre-determined intervals (e.g., every 3 to 5 years).
- Create a Canadian interprofessional clinical guideline to facilitate evidence-informed, trauma-informed, equity-oriented, and biopsychosocial management of chronic pain across health care settings.
- Update the Canadian Guideline for the Use of Opioids for Chronic Non-Cancer Pain to better balance the risks of opioids with the risks of opioid discontinuation, including adding guidance on how to interpret dose limits, evidence-informed alternatives to opioids, best practices in deprescribing with biopsychosocial supports when needed, and specific populations including children and youth. Evaluate the guideline for additional updates and changes and invest in appropriate knowledge translation for both health professionals and people living with pain.
- Develop a guideline to prevent transition from acute to chronic pain in children and adults undergoing surgery.
- Develop a guideline to improve recovery after injury and early recognition of, and support for, people at risk of chronic pain.
- Support the development, dissemination, and evaluation of evidence-informed clinical guidance for health care professionals who authorize access to cannabis for medical purposes to treat and manage chronic pain while actively working to support more research into potential applications.
- Standardize, disseminate, and implement evidence-informed guidelines for interventional pain procedures (e.g., nerve blocks) to ensure common approaches across jurisdictions and care settings.
- Develop specific clinical guidelines and quality standards for children and youth, adults and seniors, those living in long-term care settings, and other key populations.
- Standardize, disseminate, and implement guidelines for the delivery of virtual, in-person, and hybrid models of pain care to ensure common approaches across jurisdictions and care settings.
- Review the current state of condition-specific clinical guidelines and invest in updating and filling gaps for chronic pain conditions that require specific approaches.
- Create a Pan-Canadian, standardized suite of pain indicators, assessment tools, and accreditation standards for use along the continuum of institutional care, including acute care and long-term care settings, in partnership with Accreditation Canada and the Health Standards Organization (building on work already underway for pediatric populations).
Virtual treatment, self-management, and peer supports
- Create a national pain specific online portal for people to access an interactive repository of services, information, and resources, with appropriate psychosocial supports for navigation of resources as needed.
- Connect this portal and integrate pain-related content with other online resources (e.g., federally funded platforms like Wellness Together Canada and the Knowledge Development and Exchange youth mental health HUB).
- Ensure these online platforms have telephone options and alternative means of access for those without adequate internet service.
- Enable data collection related to access to services, pain management, and treatment outcomes within the platform to enable health system monitoring and improvement.
- Ensure self-management resources are provided at no cost and are available in multiple languages.
- Support the coordination and spread of evidence-informed pain prevention and self-management support programs – virtual and in-person – to ensure they are widely accessible regardless of geography; this includes the development of culturally safe and relevant pain self-management support programs in multiple languages through collaboration with Indigenous communities and various ethno-cultural groups.
- Provide resources to further develop and scale peer support initiatives across all jurisdictions in Canada to reduce isolation and enable re-engagement with activities. Establish a mechanism for connecting these initiatives at a national level for knowledge sharing and coordination.
Goal #3 - People living with pain and health professionals have the knowledge, skills, and educational supports to appropriately assess and manage pain based on population needs. The broader community understands pain as a legitimate, biopsychosocial condition and stigma is reduced
Despite a wealth of knowledge on different aspects of chronic pain, it is still not well understood by many and remains stigmatized and invalidated, contributing to poor outcomes for people who live with pain. Legitimizing pain – in the health care system, in workplaces and schools, and in society more broadly – is essential to combating stigma and improving quality of life for Canadians with chronic pain.
“My personal vision is that the awareness about chronic pain takes on the same level of awareness that conditions such as mental health and breast cancer have received.”
Person living with pain
People living with pain need knowledge of pain science and evidence-informed treatments and supports to enable them to improve their quality of life. Innovative self-management programs exist but they require support to scale and to be tailored for diverse populations and contexts.
Pain education for health professionals is inadequate, with significant knowledge gaps in both pre- and post-licensure contexts. There are pockets of excellence across the country in health professional education and training, although there is work to be done to scale these and to integrate trauma and violence-informed approaches and cultural relevance and safety.
Recommended actions:
Public education and awareness
- Ensure the federal health portfolio aligns with the WHO to recognize chronic pain as a distinct chronic disease and communicate this across federal government Departments.
- Develop and implement a Pan-Canadian public awareness campaign about chronic pain that engages provinces, territories, and community organizations to improve understanding of pain and related risk and protective factors, address misconceptions, reduce stigma, and connect people to resources and supports.
- Create targeted materials to increase understanding of evidence-informed, biopsychosocial approaches to pain assessment and management for health professionals and people living with pain.
- Ensure public education and awareness is culturally safe, trauma and violence-informed, translated into multiple languages, and complies with accessibility standards (e.g., expanded beyond written form to include videos, infographics, and other media).
- Leverage existing federal, provincial, territorial, and organizational relationships to create and integrate pain prevention and awareness into existing health education curricula at the primary and secondary school levels and develop educational pain resources for children, families, mentors (e.g., coaches), sporting associations, and others involved in child and youth development.
- Amend Senate order to align the current National Pain Awareness Week in November with International Pain Awareness Month in September to leverage the resources, tools, and activities created by the international community, extend reach, and build awareness.
Health system organization and delivery of care
- Assemble health regulators and professional associations in each jurisdiction to address stigma and discrimination directed toward people living with pain by health professionals and ensure that clinicians understand their obligations to treat or redirect patients regardless of pain condition, complexity of symptoms, and/or history or current use of opioids.
- Create capacity to spread existing and develop new best practice education/training programs and initiatives across Canada at the community, regional, provincial, and national levels.
- Enable staff in telehealth and general referral systems to link people to necessary chronic pain resources and supports.
- Educate clinicians on chronic pain specific diagnostic coding and measurement resources.
- Encourage health professionals working with Indigenous Peoples to understand Indigenous specific definitions of pain and hurt, how it is expressed, preferences for treatment and management, and concepts of Two-Eyed Seeing.
Pre-licensure education and training
- Convene health professional associations and regulatory bodies to build on the work underway to create standardized pain related curricula and competencies for regulated health professional programs involved in the management of pain.
- Align with international best practices by building specific competency frameworks for Canada that adapt those created by the International Association for the Study of Pain.
- Focus on not only profession-specific but also interprofessional competencies that recognize the full range of professions relevant to pain.
- Ensure adequate competencies for both specialist and generalist practitioners.
- Integrate individuals with lived and living experience into training, education, and curricula development.
- Include pain competencies into health care practitioner licensure exams.
- Empower leadership from University and College programs to create sub-specializations in pain management across all relevant health care professions.
- Create guidelines and policies for equity-oriented and trauma and violence-informed pain care that recognize the differences in pain experience and expression across populations. Integrate such approaches into pre-licensure for health professionals.
Post-licensure education and continuing professional development
- Assemble relevant organizations and academic institutions to determine how best to disseminate and create discipline-specific and interprofessional continuing education programs to improve knowledge and skills in pain assessment, management, and referral among health professionals.
- Leverage Pan-Canadian Health Organizations and federal, provincial, and territorial funding programs to promote development, uptake, and sharing of interprofessional mentorship programs on pain management to build knowledge, skills, and interprofessional support among health care professionals.
- Enable the integration of equity-oriented and trauma and violence informed care into post-licensure educational programs.
- Expand post-graduate positions (e.g., residencies, post-doctoral fellowships) to train health professionals as pain specialists.
- Build on existing initiatives to develop evidence-informed clinical guidelines on chronic pain by establishing credentialing programs to ensure health professionals have appropriate training for interventional pain procedures.
Goal #4 - Pain research and related infrastructure enables discovery, catalyzes innovation, and results in the translation of knowledge into real world impact
There have been recent significant investments in pain research and knowledge mobilization in Canada. Our country is home to many internationally renowned pain researchers and boasts a strong pain research community. However, many knowledge gaps persist and strategies to spark discovery and foster innovation are needed.
Research and advocacy-based funders, organizations, and networks, some collaborating with people living with chronic pain, have worked to define directions for a national research agenda. Further investment is required to support and accelerate basic science, clinical trials, research in social determinants, and evaluation of health services in the area of pain, and to ensure knowledge is mobilized to change practice and policy.
Recommended actions:
Engagement of people living with pain
- Encourage the engagement of people with lived experience to co-design pain research across the entire research process, including strategic planning for funding bodies, study design, recruitment, analysis, knowledge mobilization, publication, and advocacy.
- Enable Indigenous Peoples to lead, develop, and own pain research that is specific to various community needs as per Tri-Council Policy Statement: Ethical Conduct for Research Involving Humans – TCPS 2 (2018), Chapter 9 and the National Inuit Strategy on Research.
Coordinated and collaborative opportunities specific to pain research
- Establish pain as a cross-cutting priority at Canada’s research funding agencies (Canadian Institutes of Health Research [CIHR], Canada Foundation for Innovation [CFI], Social Sciences and Humanities Research Council [SSHRC] and Natural Sciences and Engineering Research Council [NSERC]) to drive innovation, discovery, and knowledge creation and mobilization.
- Facilitate international collaborations with established pain-related funding initiatives, such as the National Institutes of Health Helping to End Addiction Long-term (HEAL) Initiative, the Analgesic, Anesthetic, and Addiction Clinical Trials Translations, Innovations, Opportunities, and Networks (ACTTION) Initiative, and European Pain Research initiatives, to bring Canadian discovery, knowledge, and innovation to the world, and aid in the translation of these discoveries to new pain treatments.
- Collaborate with the private sector, including the pharmaceutical industry, health care professional associations, and private insurers to support improved surveillance and research into the effectiveness of interventions (e.g., enhancing existing reporting systems on adverse drug reactions with additional information).
- Convene provincial and federal health charities and non-government organizations to discuss the importance of pain research and to enable collaborations and supports across community-based funding bodies.
- Evaluate federally and provincially funded research networks to better understand gaps and successes as well as potential areas for consolidation, collaboration, coordination, or expansion.
- Link researchers, health care professionals, policy makers, people with lived experience of chronic pain, and existing pain networks and hubs of expertise, by creating a larger “network of networks” across pain research priorities similar to the infrastructure created for the Canadian Research Initiative in Substance Misuse (CRISM).
- Establish central coordination, collaboration, and administrative supports.
- Build a transparent, inclusive, multi-jurisdictional recruitment and membership process.
- Create resource and data sharing policies and agreements, and focus on increasing efficiencies and reducing duplication.
Invest in research infrastructure to enable precision and personalized care
- Apply evidence and bridge the gap between science and practice by investing in knowledge mobilization and pain professionals trained in knowledge translation. In parallel, expand and link existing specialized knowledge mobilization networks that focus on specific pain conditions and populations (e.g., Solutions for Kids in Pain).
- Sustain early successes built by the CIHR Chronic Pain Network, while exploring how best to link different data collected by the network and expand it to be more inclusive of a range of researchers from across Canada.
- Strengthen existing national patient registries for adults and children living with pain to establish a multidimensional, uniform minimal dataset and standard set of data collection questions for both adult and pediatric populations in Canada.
- Expand networks devoted to clinical research to increase the number of sites and capacity for multi-site projects focused on clinical research and real world studies.
- Create national infrastructure to systematically collect biomarkers (e.g., imaging, blood samples, and genetic data) for chronic pain through clinical trials and observational studies to enable open science and discovery outside of competitive funding schemes.
- Establish guidance to ensure research into innovative technologies, methodologies, and care solutions considers the barriers experienced by different segments of the population, ethical concerns, and the need to reduce stigma and legitimize people’s pain.
- Connect and foster collaborations between national and provincial pain research networks and leadership and organizations representing Indigenous Peoples to encourage Indigenous-led research and research participation within Indigenous communities.
Invest in strategic research priorities
- Stimulate research into the basic science of pain to support the development of novel health products, individualized and targeted approaches to pain, and innovative clinical practices. Ensure that the translation of findings is supported from the laboratory to care settings.
- Focus strategic research investments to explore the effectiveness of models of pain care (e.g., care pathways, multidisciplinary and interprofessional approaches, complementary and integrative therapies) to reduce fragmentation of care and improve understanding of what types of clinical care models work best for whom, when, and under what circumstances.
- Promote and expand research in populations that are disproportionally affected by pain to improve understanding of risk and protective factors (e.g., genetic, sex, gender, biomarkers, environmental, historical, and experiential) and to better predict the trajectories and care needs for those at-risk for developing chronic pain.
- Support research efforts to improve processes, technology, and interventions in the area of digital technologies for health including e-health and virtual care.
Build future research capacity
- Scan current funding mechanisms available for pain research and map pain research in Canada to better assess the state and capacity-building needs for future research.
- Enable Canadian researchers to conduct clinical trials on cannabis products for medical purposes by establishing exemptions and alternatives to requirements related to preclinical data and product manufacturing while maintaining appropriate safety and quality standards.
- Incentivize researchers to work on pain related challenges. Build on initiatives to institutionalize sex, gender, population, and equity-based analyses by encouraging researchers to integrate pain related considerations and measures in all areas of health research, including federally and provincially supported cohort studies (e.g., Canadian Longitudinal Study on Aging).
- Launch supports (e.g., fellowship grants, mentorship programs, training and career support awards) dedicated to building capacity for trainees and early career investigators across pain disciplines and research pillars.
- Invest in fellowships and/or national applied research chair programs supporting clinician-scientists working in the field of pain.
- Create supports and fund research on promising complementary and integrative therapies for pain to provide researchers the opportunity to explore their mechanisms, usefulness, and safety.
Goal #5 - Data enables effective monitoring of pain and facilitates improvement of health system quality
Due to the lack of surveillance infrastructure, governments, researchers, and health care professionals do not have enough information about chronic pain (e.g., mechanisms, manifestations, management), the unique challenges and needs of people living with pain, and the capacity of respective health care systems to respond to these needs. Taking action on pain must be enabled by improved, consistent, and sustained national data collection on the prevalence, course, and impact of chronic pain in Canada. There is also a need to monitor the impact of interventions intended to improve health outcomes for people living with pain and health system performance.
Canada’s public health surveillance system offers turn-key opportunities to integrate questions on pain into existing surveys as well as building new tools to enhance our understanding. These data will help to create health profiles at federal, provincial, territorial, and regional levels, identify populations at-risk, monitor changes over time, and enable big data approaches and evidence-informed policy, programming, and investments to ensure all Canadians living with or at-risk of chronic pain achieve the best outcomes possible.
Recommended actions:
National indicators and reporting
- Conduct a national and international environmental scan of pain surveillance and monitoring initiatives, including the types of measures currently used to assess pain. Compare findings to the consensus-driven core minimum data-set established through national pain registries.
- Improve the ongoing, systematic collection, analysis, and reporting of health data to monitor pain incidence, prevalence, impact, and health outcomes over time (e.g., including the Health Utilities Index Pain Questions in the Canadian Community Health Survey (CCHS) annually).
- Expand the scope of pain surveys to capture more comprehensive information on chronic pain, the longitudinal impact of chronic pain, and the effectiveness of interventions for different types of pain and populations. For example, adding more pain-related questions to existing surveys (e.g., CCHS, Canadian Health Measures Survey, Canadian Survey on Disability), implementing nationally representative surveys, and integrating pain questions into rapid surveys conducted by Statistics Canada (e.g., Labour Force Web Panel).
- Enable collaboration between federal, provincial, territorial, and local governments, clinicians, and people living with pain to standardize national pain indicators and surveillance initiatives across jurisdictions (e.g., common chronic pain definition, minimum dataset, standardized data collection and reporting methods).
- Integrate pain indicators and measures into other government strategies, policies, and plans, including those for chronic diseases, mental health, and substance use disorders (e.g., Canadian Strategy for Disability and Work, Canadian Task Force on Preventive Health) and for priority populations (e.g., seniors and long-term care settings, Veterans, people who are incarcerated).
- Implement a national surveillance report card to evaluate the progress of pain surveillance initiatives across all provincial and territorial governments.
- Further analyze the direct and indirect costs of chronic pain in the most affected groups of the population, including the cost-effectiveness of interventions provided in publicly funded primary care, those not covered by provincial and territorial health insurance plans, and services provided by multi-disciplinary health professionals.
Novel approaches to monitoring pain
- Collaborate with institutions such as the Canadian Institute for Health Information to leverage existing surveillance systems, databases, and algorithms to develop standardized case definitions of chronic pain, validating them against known cases of chronic pain.
- Explore ways of monitoring and reporting that respect and integrate different social and cultural approaches to defining and measuring pain (e.g., Indigenous Peoples ways of knowing).
- Conduct a feasibility study for the development of a provincial pain surveillance system, including assessing the potential use of the ICD-10 algorithm currently being trialled by researchers in some provinces. Recommend potential options for integrating pain information into national chronic disease reporting (e.g., the Canadian Chronic Disease Surveillance System overseen by the Public Health Agency of Canada).
- Enable a more unified long-term administrative classification of chronic pain by adopting the WHO’s ICD-11, which recognizes chronic primary pain and chronic secondary pain as distinct diagnostic disease entities in their own right.
- Monitor off-label medication use in the treatment of pain and integrate evidence and surveillance data in a manner that rapidly updates product monographs and clinical guidance based on real-world use and experience.
Novel collaborations and data sources
- Explore the potential of big data approaches that incorporate different data types from novel sources such as wearable technologies and sensors and how they could be used to improve surveillance and research activities.
- Leverage prescription monitoring programs for better data and information on the effectiveness of pharmacotherapy (e.g., opioid and non-opioid prescribing practices) for pain in specific populations and how they may have shifted longitudinally due to COVID or with changing guidelines.
- Partner with the private sector to explore how to harness innovative data and care platforms being developed through programs like Canada’s Digital Technology Supercluster supported by Innovation, Science, and Economic Development Canada.
- Collaborate with the Association of Worker Compensation Boards of Canada to collect and report on pain and pain-related disability resulting from workplace injuries.
- Develop and scale existing chronic pain registries and collaborate with clinics offering care in the private sector to regularly gather information and monitor how patients are accessing services, the impact of interventions, and other relevant outcomes.
Populations disproportionately impacted by chronic pain
- Ensure the scope of surveys administered include populations who are particularly underserved (e.g., children, on-reserve Indigenous populations, people living in long-term care facilities) and those that are disproportionally affected by pain by capturing relevant demographic information, socioeconomic and structural determinants of health, other known risk factors, and conditions that co-occur with pain (e.g., mental illness, substance use disorder).
- Closely monitor the long-term health impacts of individuals infected by COVID-19 and other viral infections with the potential to cause chronic pain and assess the impact of delayed elective surgeries and procedures on health outcomes, medication use, and health care utilization.
- Expand surveillance of opioid-related drug overdose deaths to monitor the impacts of changes to opioid prescribing practices and to better distinguish contributions of different types of opioids (e.g., prescribed opioids, illicit opioids).
Goal #6 - There is improved and equitable access to services for populations disproportionately impacted by pain
The prevalence of chronic pain in Canada is not equitably distributed. Occurrence of disease, severity of illness, and barriers to care are higher in populations affected by social inequities, racism, poverty, violence, trauma, and other experiences of marginalization. Various intersecting forms of discrimination may also lead to compounded challenges in receiving care and outcomes. An equity-oriented and trauma and violence-informed approach will be essential to understand, prevent, and treat pain.
"Many marginalized groups, in particular people of colour, Indigenous people and women, have their pain outright dismissed by the public and medical professionals. People of colour and Indigenous people are often regarded as 'drug seekers' and women are regarded as being 'dramatic'. These barriers not only prevent people from getting proper care but also prevent them from seeking help in the first place, due to negative experiences and shame."
Person living with pain
First Nations, Inuit, Métis Peoples
- Commit to joint action on addressing the harmful intersection between stigma related to substance use, chronic pain, and Indigenous-specific racism.
- Amplify Indigenous-led change in health systems and link unique community needs and strengths with solutions identified by community members, recognizing the interplay between different dimensions of Indigenous wellness and pain (e.g., emotional, spiritual, physical, mental).
- Engage First Nations, Inuit, and Métis Peoples, clinicians, Elders, youth, and Knowledge Keepers to identify priorities for improving pain management in communities and for Indigenous Peoples living with pain in urban, rural, and remote community settings, including the best ways to reach these communities.
- Expand access to traditional Indigenous medicine and practices for pain or pain care approaches that align with Indigenous ways of knowing across all insurers including the Non-Insured Health Benefits (NIHB) Plan. Harmonize funding for comprehensive medication reviews for First Nations and Inuit covered by NIHB.
- Support Indigenous-led community-based initiatives and systems that take a distinction-based approach and recognize the differences between and within First Nations, Inuit, and Métis Peoples. Blend traditional Indigenous medicine and practices with conventional medicine to function in an inclusive way and increase their use in clinical practice and in all health systems.
- Enable accessible Indigenous-led pain care, supports, and resources within communities, where families and community members can play a greater role in providing care and support.
- Consider how best to provide assistance in the navigation of NIHB and the health system, treatment options, potential transitions in care, and receiving services across systems of care.
- Collaborate with the National Consortium on Indigenous Medical Education and other organizations to support the creation and delivery of cultural safety, anti-racism, and unconscious bias training to change attitudes, behaviours, practices, and policies across the pain care system and address systemic inequities for First Nations, Inuit, and Métis Peoples.
Racialized Peoples
- Support the creation and delivery of anti-racism and unconscious bias training and establish policies and accountability mechanisms to change attitudes, behaviours, and practices across the health care system and to address systemic inequities for racialized peoples.
- Examine culturally-specific beliefs and understanding about pain and values, preferences, and approaches to pain management for major cultural groups in Canada and explore opportunities to integrate this knowledge with evidence-informed approaches to pain care.
People who use substances
- Develop pre- and post-licensure chronic pain competencies and education programming for health care professionals involved in the treatment of substance use disorders and those working in multidisciplinary pain treatment clinics to make them aware of the prevalence, impacts, and under-treatment of chronic pain among people who use substances.
- Integrate pain assessment and management into harm reduction services and the treatment of substance use disorders across all care settings, including expanding access to multidisciplinary pain management services for people who use substances.
- Integrate assessment and management of substance use disorder and harm reduction principles into specialty pain programs and all other pain-related care settings.
- Integrate opioid use disorder services and pain services as part of primary care.
- Educate all pharmacists, particularly those working in rural and remote areas, to understand the significant need and critical importance for the provision of opioid agonist therapy services (including methadone and buprenorphine / naloxone).
- Facilitate equitable access to harm reduction services (e.g., needle and syringe programs, naloxone kit distribution) in community settings across Canada, including pharmacies and primary care clinics.
People with mental illness
- Develop pre- and post-licensure chronic pain competencies and education programming for health care professionals involved in the treatment of mental health disorders and those working in multidisciplinary pain clinics to ensure people living with mental illness have access to equitable pain care.
- Develop quality standards for the treatment of chronic pain in mental health services and integrate pain assessment and management into the treatment of mental health disorders across all care settings.
- Build capacity and provide intensive day and/or inpatient treatment programs for people with severe concurrent pain and mental health related disability.
Workers
- Recognize the intermittent nature of pain and incentivize employers and unions to provide flexible work options to enable people with pain to remain in the workforce.
- Update employment standards to require fully paid sick leave for all workers regardless of workplace size, type of work, or immigration status, to enable those with pain to remain in the workforce, and to prevent individuals with acute pain from experiencing further injury and chronic pain.
- Partner with employers and unions to develop and implement pain educational tools in the workplace that support prevention, assessment, treatment, and management – similar to those for mental health and other chronic conditions.
- Integrate a greater range of evidence-informed pain management approaches into employee benefits plans and employee assistance programs.
- Integrate more comprehensive, biopsychosocial pain assessment and management into return to work assessment and planning and remove policies that incentivize return to work over employee well-being.
- Partner with the Association of Workers Compensation Boards of Canada, the Canadian Injured Workers’ Alliance, and the Canadian Labour Congress subcommittees on disability and injury, to collect and publish data on chronic pain and workplace injury as well as the intersect of these conditions with mental health and substance use.
Persons with disabilities
- Update terminology and definitions used for eligibility for chronic pain disability benefits to ensure alignment with current evidence on pain.
- Enable the range of practitioners involved in the management of pain to assess and diagnose related disability as part of benefit programs.
- Recognize that persons with disabilities are disproportionately impacted by pain, and that pain may itself be a disability, and take into account the unique barriers for these different groups.
- Recognize the intermittent nature of pain and related disability, and incentivize employers to provide flexible work options to enable people with disabilities to remain in the workforce when able.
Children and youth
- Support the creation of pediatric transitional pain services and chronic pain services to support those at highest risk of chronic pain.
- Invest in specialist pediatric chronic pain services in each Province and Territory through the creation of dedicated facilities or interprovincial agreements.
- Invest in intensive day and/or inpatient treatment pain management programs, for children and youth with severe pain related disability.
Seniors
- Ensure national standards for long-term care and home care include pain assessment and management as critical considerations in all aspects of care.
- Educate health professionals and caregivers on the unique pain-related needs of people living with physical, cognitive, or developmental conditions or disabilities, who may not be able to fully communicate their pain (e.g., people living with dementia).
- Encourage development of pain-specific competencies in health professionals involved in geriatric specialities and care.
Women
- Integrate a sex and gender lens into pain education and awareness efforts to address the additional barriers of gendered invalidation that women living with pain experience and how these may be further compounded for racialized peoples. Recognize that women are also disproportionately impacted by intimate partner and gender-based violence, which can cause and/or exacerbate pain.
- Support the expansion of specialized services for painful conditions experienced predominantly by women (e.g., pelvic pain, fibromyalgia, myalgic encephalomyelitis/chronic fatigue syndrome).
People who are sexually and gender diverse
- Implement pre- and post-licensure training for health professionals regarding sexual and gender diversity and pain specific considerations.
- Encourage and normalize the use of gender inclusive pronouns in all teaching, research, and service delivery related to pain.
- Use gender and sexual identity affirming language in all communication to/with people living with pain and families (e.g., patient intake forms, research surveys), and health professionals.
People who are incarcerated
- Review available pain care options – self-management, pharmacological, physical, spiritual, psychological – offered in federal institutions to identify regional patterns of care and work to address care gaps and geographic disparities.
- Fully implement the Guidance for Chronic Non-Cancer Pain Management established by Correctional Service Canada across federal institutions and help to inform approaches to pain care in provincial and territorial institutions.
- Consider how best to provide assistance in the navigation of health and social services systems, and pain treatment options when transitioning from federal institutions back into the community.
Veterans
- Examine current policies, procedures, and criteria used to determine eligibility for accessing care with the goal of accelerating a pain diagnosis, removing barriers and unnecessary wait times, and improving access to interdisciplinary care for all Veterans including evidence-informed self-management, pharmacological, physical, psychological, and spiritual and traditional Indigenous medicine and practice approaches.
- Consider how best to provide assistance in the navigation of the health system, treatment options, and potential transitions in care, including leaving the service for both Veteran’s and their families. Evaluate the current number of case managers and resources available for navigation to determine and address gaps as well as promote and empower self-management.
- Support training for primary care practitioners and others involved in pain management on the unique needs of Veterans.
- Enable additional research that explores the unique context, chronic pain conditions, and risk and protective factors specific to Veterans, including a detailed examination of gender and sex differences. Improve coordination and partnership between the Department of National Defence and Veteran Affairs Canada, in both research and programming to create adequate longitudinal evidence and seamless supports that span service and transitions to civilian life.
- Leverage the research and learning from the Chronic Pain Centre of Excellence for Canadian Veterans to support scale of innovative approaches for pain care more generally.
Conclusion and next steps
Chronic pain is ubiquitous. It is a serious public health emergency impacting people across Canada, their families, the health system, and society. There is an urgent need to address pain in Canada. The Action Plan for Pain in Canada is a critical step towards laying a strong foundation for change, and provides a blueprint to advance an improved approach to the prevention and management of chronic pain.
National leadership, supported by resources, is needed now to put these recommendations into action. Health Canada and the Government of Canada must lead the way, in partnership with Provinces and Territories and with all levels of government. It does not stop there. A range of other actors working inside and outside of the health system, from peer advocates, non-governmental organizations, academic institutions, insurers, and others, must step forward in order to enable positive and lasting change.
Together, we must act to build, amplify and accelerate activities, coordinate responses, and address gaps and inequities. Investing in these priority actions will ensure people with pain are recognized and supported, and that pain is understood, prevented, and effectively treated across Canada.
Page details
- Date modified: