Chapter 3: The Chief Public Health Officer's Report on The State of Public Health in Canada 2010 – The health and well-being of Canadian seniors
Chapter 3: The Health and Well-being of Canadian Seniors
This chapter provides an overview of the current health and well-being of the Canadian population aged 65 years and older, including patterns of ill health and disability within this age group. It focuses on their physical and mental health as well as economic and social well–being.
The health status of individuals between 65 and 79 years is often different than that of those aged 80 years and older. Similarly, the health status of senior men often differs from that of senior women. For this reason, when appropriate and available, data in this report will be presented accordingly.
Demographics of the senior population
According to the 2006 Census, of the 31.6 million people who live in Canada, 4.3 million (14%) are 65 years and older (see Table 3.1).Footnote 84 Within Canada's senior population, 73% are between the ages of 65 and 79 years and more than one-quarter (27%) are 80 years and older.Footnote 84 Immigrants account for approximately 28% of the senior Canadian population, while Aboriginal peoples account for 1%.Footnote 84-Footnote 86
| Year | ||
|---|---|---|
| Population (thousand people aged 65+ years) | ||
| Population | 4,335.3 | 2006 |
| Aboriginal | 56.5 | 2006 |
| First Nations | 32.0 | 2006 |
| Métis | 20.0 | 2006 |
| Inuit | 1.8 | 2006 |
| Immigrant | 1,215.3 | 2006 |
| Recent (<= 10 years) | 78.3 | 2006 |
| Long-term (>10 years) | 1,137.0 | 2006 |
| Living in private households | 4,011.9 | 2006 |
| Living in health care and related facilities | 301.3 | 2006 |
| Urban population | 3,208.6 | 2006 |
Note: More detailed information can be found in Appendix C: Definitions and Data Sources for Indicators. |
||
Over the past 30 years, the proportion of the population made up of those aged 65 years and older has increased from 9% to 14%.Footnote 42 This trend is also evident in other developed countries (see Figure 3.1).Footnote 87-Footnote 89 For example, between 1960 and 2007, the population of seniors in Japan more than tripled, from 6% to 22%.Footnote 87 In Sweden, it increased from 12% to 17% and in the United States it rose from 9% to 13%.Footnote 87 Given continuing increases in life expectancy and remaining years of expected life at age 65, seniors will become an even larger proportion of the population over the next 40 years.Footnote 43 For example, while today's seniors represent 14% of the total population, it is estimated they will make up more than one-quarter (27%) of the population by the year 2050.Footnote 42 Footnote 43 Footnote 88 Footnote 89
Figure 3.1 Proportion of population, aged 65 years and older, select countries, 1960 to 2007, projected 2010 to 2050Footnote 87-Footnote 89
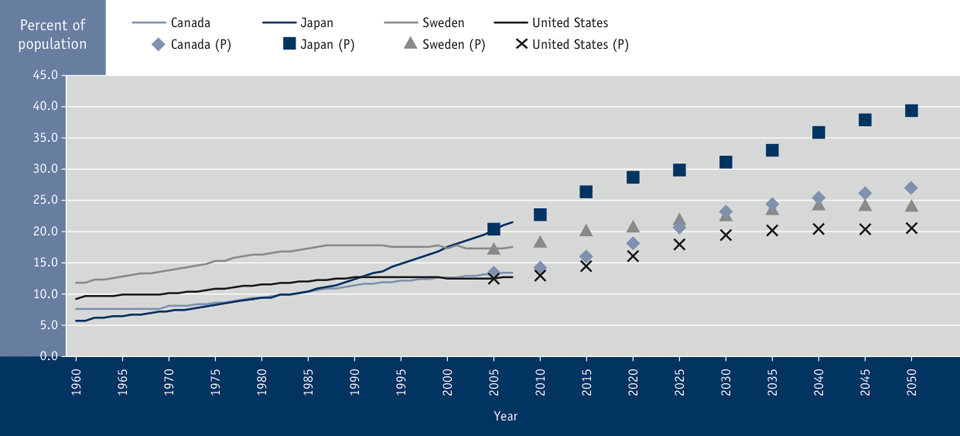
(P) Future population projections.
Sources: Organisation for Economic Co-operation and Development (OECD) Health Data 2009 and United Nations.
[Figure 3.1, Text equivalent]
Summary: The senior population has increased between 1960 and 2007 from 7.6 to 13.4 percent in Canada; from 5.7 to 21.5 percent in Japan; from 11.8 to 17.4 percent in Sweden and from 9.2 to 12.6 percent in the United States. This increase is projected to continue through to 2050 with the seniors population estimate to be 26.9 percent in Canada; 39.3 percent in Japan; 24.0 percent in Sweden; and 20.5 percent in the United States.
| Country | Percent of population 1960 | Percent of population 2007 | Percent of population 2050Footnote 1acsup> |
|---|---|---|---|
| Canada | 7.6 | 13.4 | 26.9 |
| Japan | 5.7 | 21.5 | 39.3 |
| Sweden | 11.8 | 17.4 | 24.0 |
| United States | 9.2 | 12.6 | 20.5 |
| Footnote 1 Future population projections. | |||
Sources: Organisation for Economic Co–Operation and Development (OECD) Health Data 2009 and United Nations.
In 2006, seniors accounted for 5% of the overall Aboriginal population and this number is projected to grow to nearly 7% by 2017.Footnote 73 Footnote 86 During the same period, the senior Métis population is expected to see the most growth, increasing from 5% to 8%, First Nations seniors are expected to increase from 5% to 6% and the senior Inuit population is expected to remain constant around 4%.Footnote 73 Footnote 86 Between 1996 and 2006, the immigrant seniors population increased from 18% to 19% of the total immigrant population.Footnote 90-Footnote 93 The proportion of first- and second-generation senior immigrants within the immigrant population is expected to decrease from 51% in 2006 to 41% in 2031.Footnote 94
The majority of seniors (80%) live in private households in urban settings across Canada, which is similar to the rest of the Canadian population (82%).Footnote 91 Footnote 95 Although more seniors are living in urban areas versus rural areas, they represent a larger proportion of the Canadian rural population than in the past.Footnote 90 Footnote 91 Footnote 96 This is due to the fact that an increasing number of younger rural residents have moved to urban areas, leaving senior residents to make up more of the overall rural population.Footnote 97 Most seniors (92%) also live in private homes.Footnote 84 Footnote 95 The remaining 8% reside elsewhere, including long-term care facilities, assisted living facilities and retirement residences.Footnote 84 Footnote 91 Footnote 95 Footnote 98 Footnote 99
| Year | ||
|---|---|---|
| Physical health | ||
| Life expectancy (remaining years of expected life at age 65)¹ | 19.8 | 2005-2007 |
| Male | 18.1 | 2005-2007 |
| Female | 21.3 | 2005-2007 |
| Health-adjusted life expectancy (remaining years of expected healthy life at age 65)¹ | 13.6 | 2001 |
| Male | 12.7 | 2001 |
| Female | 14.4 | 2001 |
| Mortality² (deaths per 100,000 population aged 65+ years per year) | ||
| Circulatory diseases | 1,381.2 | 2006 |
| Cancers | 1,126.9 | 2006 |
| Respiratory diseases | 397.9 | 2006 |
| Ill health and disease (percent of population age 65+ years) | ||
| Excellent or very good self-rated health*¹ | 43.6 | 2009 |
| Excellent or very good functional health*¹ | 62.0 | 2005 |
| High blood pressure*¹ | 56.1 | 2009 |
| Heart disease*¹ | 22.6 | 2009 |
| Arthritis*¹ | 43.7 | 2009 |
| Diabetes² | 21.3 | 2006-2007 |
| Often has difficulties with activities*¹ | 25.3 | 2008 |
| Cancer incidence (new cases per year per 100,000 population aged 65+ years)¹ | 2,044.2 | 2006 |
| Mental health | ||
| Satisfied or very satisfied with life*¹ | 96.5 | 2009 |
| Excellent or very good self-rated mental health*¹ | 70.4 | 2009 |
| Alzheimer's disease and other dementias (estimated)³ | 8.9 | 2008 |
| Economic well-being¹ (percent of population aged 65+ years) | ||
| Persons living in low-income (after-tax) | 5.8 | 2008 |
| Social well-being¹ (percent of the population aged 65+ years) | ||
| Very or somewhat strong sense of community belonging* | 70.2 | 2009 |
| Living alone | 28.1 | 2006 |
| Volunteering* | 35.7 | 2007 |
| Provider of unpaid care* | 24.4 | 2007 |
| Paid employment rate | 10.1 | 2009 |
| Regular family physician* | 95.7 | 2009 |
| Contact with dental professional in the past 12 months* | 55.9 | 2009 |
* Denotes self-reported data |
||
Physical health
Data presented throughout this chapter often comes from health survey data. Despite the inherent limitations of this type of data, such as the subjectivity of individual responses and the exclusion of those living in institutions and on reserves, self-reported data can provide useful information otherwise not available. Unless otherwise stated, data presented from these sources reflect only those seniors who live in the community.
Although seniors are often impacted by multiple physical health issues, such as chronic conditions and reduced mobility and functioning, many feel healthy and are willing to take action to improve their health. According to the 2009 Canadian Community Health Survey (CCHS) – Healthy Aging, 44% of seniors perceived their health to be excellent or very good.Footnote 100 In the same year, 37% of seniors reported they had taken some action to improve their health, such as increasing their level of physical activity (71%), losing weight (21%) or changing their eating habits (13%).Footnote 100
Life expectancy
The life expectancy of Canada's seniors has been steadily increasing over time (see Figure 3.2).Footnote 101 Footnote 102 In 2006, seniors who turned 65 could expect to live nearly 20 additional years (18 years for men and 21 years for women).Footnote 101 Footnote 102 Canadian women have historically experienced greater longevity, but the gap between men and women has been closing.Footnote 101-Footnote 103 Between 1980 and 2006, the gap in remaining life expectancy at age 65 between Canadian men and women decreased from five years to three years.Footnote 101 Footnote 102
However, not all population groups in Canada have a similar life expectancy. Despite a growth in the number of senior Aboriginal persons, life expectancy at birth for this group was 71 years for men and 77 years for women in 2001, which lags behind the Canadian average of 77 years for men and 82 years for women during the same period.Footnote 104 Footnote 105
Internationally, other developed countries are also experiencing increases in remaining life expectancy at the age of 65. Some of these countries, such as Sweden and the United States, have also seen the gap in remaining life expectancy at the age of 65 decrease between men and women, while Japan has seen the gap increase.Footnote 101 Footnote 102
Figure 3.2 Remaining life expectancy at age 65 by sex, select OECD countries, 1980 to 2008Footnote 101 Footnote 102
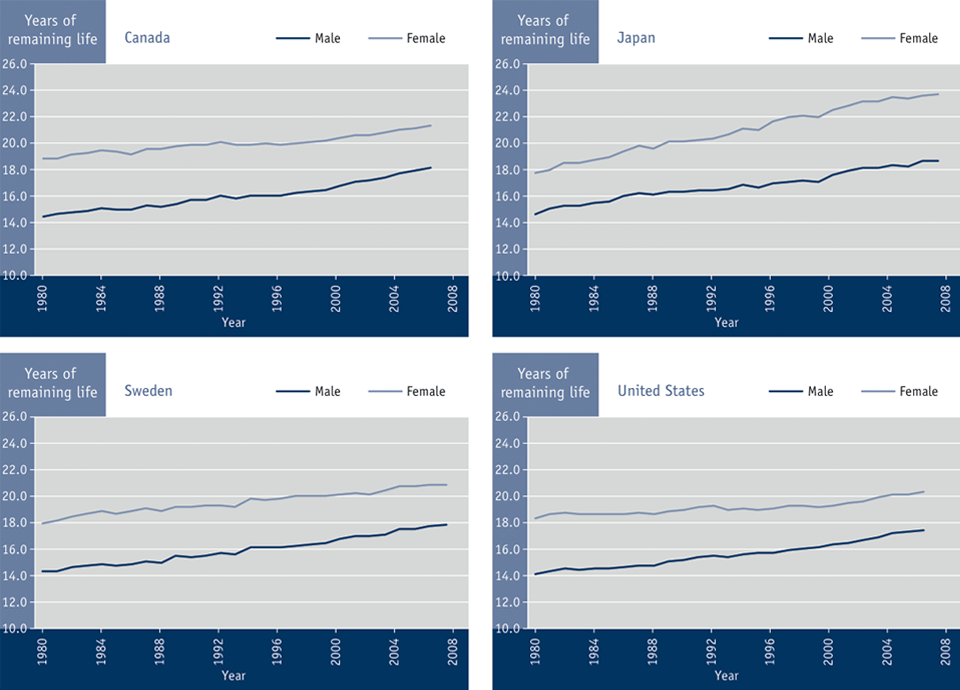
Sources: OECD Health Data 2009.
[Figure 3.2, Text equivalent]
Summary: Between 1980 and 2008 the life expectancy has increased from 14.5 to 18.2 for men and 18.9 to 21.4 for senior women in Canada; from 14.6 to to 18.6 for senior men and 17.7 to 23.6 for senior women in Japan; from 14.3 to 17.8 for senior men and 17.9 and 20.0 for senior women in Sweden; and from 14.1 and 17.4 for senior men and 18.3 and 20.3 for senior women I the United States.
Source: OECD Health Data 2009.
Mortality
The main causes of death among Canadians who die before age 45 tend to be quite different than those for seniors, with a large proportion of all deaths for this younger age group being due to injuries and poisonings. However, the main causes of death for seniors aged 65 years and older do not differ greatly from those for persons aged 45 to 64 years, although the proportion of all deaths within each age group attributable to those causes varies (see Figure 3.3). In 2006, the three main causes of death for all seniors were circulatory diseases (including cerebrovascular and ischemic heart disease), cancers (including cancers of the lung, colon, breast and prostate) and respiratory diseases (chronic obstructive pulmonary disease, influenza and pneumonia).Footnote 106-Footnote 125
The most common causes of death due to circulatory diseases in 2006 were ischemic heart disease (IHD) and cerebrovascular disease.Footnote 114 Deaths during that year from cerebrovascular disease were more common among women (309 deaths per 100,000 women compared to 266 deaths per 100,000 men), while deaths related to IHD were more common in men (836 deaths per 100,000 men compared to 635 deaths per 100,000 women).Footnote 42 Footnote 114
Figure 3.3 Mortality by major causes and age groups, Canada, 2006Footnote 106-Footnote 125
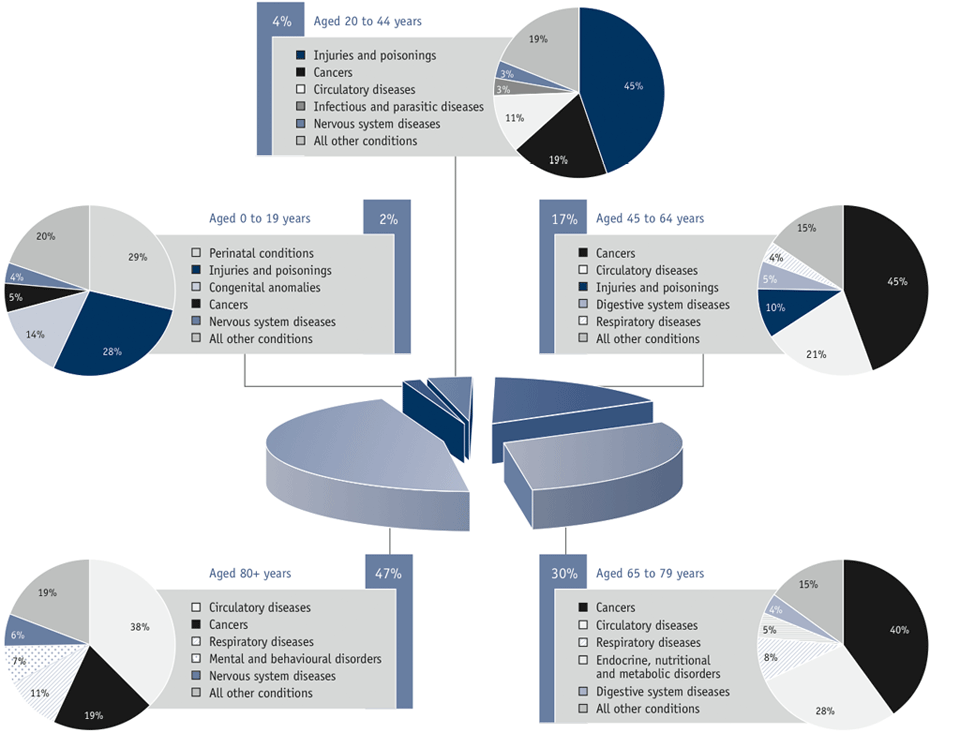
Sources: Statistics Canada
[Figure 3.3, Text equivalent]
Summary: The major causes of mortality for those aged 0 to 19 years included perinatal conditions (29%), injuries and poisonings (28%) and congenital anomalies (28%); aged 20 to 44 years included injuries and poisonings (45%), cancers (19%) and circulatory diseases (11%); aged 45 to 64 years included cancers (45%), circulatory diseases (21%) and injuries and poisonings (10%); aged 65 to 79 years included cancers (40%), circulatory diseases (28%) and respiratory diseases (8%); and aged 80 years and older included circulatory diseases (38%), cancers (19%) and respiratory diseases (11%).
Source: Statistics Canada.
Cancer of the bronchus and lung, as well as of the colon, were the most common causes of death due to cancers among seniors in Canada in 2006.Footnote 107 Deaths during that year related to each of these diseases were more common in men than in women (bronchus and lung cancer: 393 deaths per 100,000 men compared to 229 deaths per 100,000 women; colon cancer: 113 deaths per 100,000 men compared to 86 deaths per 100,000 women).Footnote 42 Footnote 107
Chronic obstructive pulmonary disease, along with influenza and pneumonia, were the most common causes of death due to respiratory diseases among Canadian seniors in 2006.Footnote 115 Deaths during that year related to influenza and pneumonia were equally common among both senior men and women (107 deaths per 100,000 men compared to 108 deaths per 100,000 women), while deaths related to chronic obstructive pulmonary disease were more common in men (225 deaths per 100,000 men compared to 156 deaths per 100,000 women).Footnote 42 Footnote 115
While the three major causes of death are the same for seniors aged 65 to 79 years and those 80 years and older, the less frequent causes of death vary more widely between these age groups. After deaths from circulatory diseases, cancers and respiratory diseases, those aged 65 to 79 die most often due to endocrine, nutritional and metabolic disorders (including diabetes and thyroid disorders), and digestive diseases (including cirrhosis of the liver and hernias). Seniors aged 80 years and older die due to mental and behavioural disorders (including dementia and schizophrenia) and nervous system diseases (including Alzheimer's disease and Parkinson's disease).Footnote 106-Footnote 125
Deaths due to injuries, both intentional and unintentional, were ranked eighth in overall causes of death for seniors in 2006.Footnote 106-Footnote 125 Half of all deaths among seniors from injuries were caused by falls (41%) or motor vehicle crashes (10%), including those where a senior was a driver, passenger or pedestrian.Footnote 42 Footnote 124
Chronic conditions and infectious disease
In 2009, 89% of Canadian seniors had at least one chronic condition. Arthritis and rheumatism was identified as one of the more common chronic conditions, affecting 44% of seniors in 2009.Footnote 100 Similarly, 53% of Aboriginal seniors not living on a reserve in 2001 and 46% of First Nations seniors aged 60 years and over living on reserve in 2002/03 reported these conditions.Footnote 73 Footnote 74 Osteoarthritis is the most common type of arthritis seen in seniors aged 75 years and older, affecting an estimated 85% of that population.Footnote 126
Osteoporosis, characterized by low bone mass and thinned and weakened bones over time, was estimated to have affected 29% of women and 6% of men age 65 and older in 2009.Footnote 100 The most common injuries associated with osteoporosis are fractures of the wrist, spine and hip.Footnote 127 Footnote 128 It is estimated that osteoporosis is responsible for approximately 70% of hip fractures in those 45 years and older.Footnote 129
Many seniors live with one or more cardiovascular diseases. In 2009, nearly one-quarter (23%) of seniors indicated they had some form of heart disease and just over 4% stated they suffered from the effects of stroke.Footnote 100 High blood pressure, a key risk factor for cardiovascular diseases, was reported by 56% of senior Canadians.Footnote 100 Among on-reserve First Nations populations, 20% of adults aged 60 years and older reported living with some type of heart disease in 2002/03.Footnote 74
In 2006, approximately 39% of all new cases (61,000) of cancer occurred in Canadians 65 to 79 years and approximately 17% of all new cases (27,000) occurred in Canadians 80 years and older.Footnote 130 Among new cases, the most common for senior men are prostate (28%), lung (17%) and colon cancer (14%); for senior women they breast (21%), lung (16%) and colon cancer (16%) (see Figure 3.4).Footnote 130
Figure 3.4 Incidence and death rate by selected cancers and sex, Canadian population aged 65 years and older, 2006Footnote 42 Footnote 107 Footnote 130
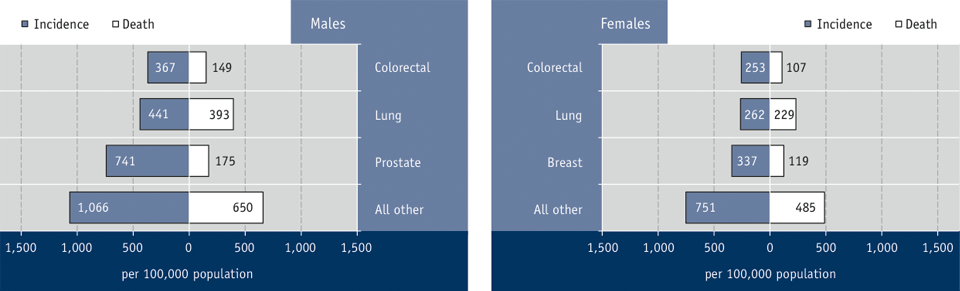
Sources: Statistics Canada
[Figure 3.4, Text equivalent]
Summary: In 2006 the most common new cases of cancer for senior men and women were not the same as the most common causes of death due to cancer for the same population.
| Type of Cancer | Incidence per 100,000 population | Death per 100,000 population |
|---|---|---|
| Male - Colorectal | 367 | 149 |
| Male - Lung | 441 | 393 |
| Male - Prostate | 741 | 175 |
| Male - All other | 1,066 | 650 |
| Female - Colorectal | 253 | 107 |
| Female - Lung | 262 | 229 |
| Female - Breast | 337 | 119 |
| Female - All other | 751 | 485 |
Source: Statistics Canada.
In 2006/07, 21% of the senior Canadian population had diabetes.Footnote 131 Some studies have suggested that as many as one-third of seniors with diabetes have not been diagnosed.Footnote 132 Footnote 133 In 2002/03, the First Nations Regional Longitudinal Health Survey estimated that 35% of First Nations seniors living on a reserve had diabetes.Footnote 74 Type 2 diabetes can result in blindness, lower limb amputation, heart disease, stroke and kidney failure.Footnote 134
Chronic conditions affecting vision and hearing are also common among seniors. In 2009, one-fifth (21%) of Canadians 65 to 79 years and nearly one-third (32%) of Canadians 80 years and older reported having been diagnosed with cataracts at some point, although most are able to undergo simple corrective surgery.Footnote 100 Glaucoma is not as prevalent, but it affects 6% of seniors aged 65 to 79 years and 13% of those aged 80 years and older.Footnote 100 Age-related macular degeneration (AMD), a degenerative disease leading to blindness, is estimated to affect 19% of Canadian seniors aged 65 to 74 years and 37% of Canadian seniors aged 75 years and older.Footnote 135 Hearing limitations, including being deaf, hard of hearing or having some hearing loss, are more common among seniors compared to younger Canadians.Footnote 136 According to the 2006 Participation and Activity Limitation Survey, 12% of seniors aged 65 to 74 years and 26% of those aged 75 years and older indicated having some form of hearing limitation.Footnote 136
Figure 3.5 Proportion of population with one or more chronic diseases*, by selected age groups, Canada, 2009Footnote 100
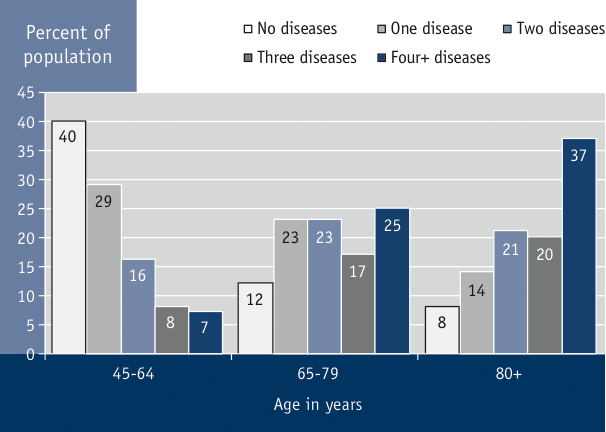
* Diseases include angina, asthma, arthritis or rheumatism, osteoporosis, high blood pressure, bronchitis, emphysema, chronic obstructive pulmonary disease, diabetes, heart disease, cancer, effects of a stroke, Crohn's disease, colitis, Alzheimer's disease, Parkinson's disease, cataracts, glaucoma, thyroid condition, mood disorder and anxiety disorder.
Source: Statistics Canada.
[Figure 3.5, Text equivalent]
Summary: Many seniors are affected by a combination of chronic conditions. Of those aged 45 to 64 years 40 percent reported having no chronic diseases compared to 7 percent with four or more; of those aged 65 to 79 years 12 percent reported having no chronic diseases compared to 25 percent with four or more; and of those aged 80 years and older 8 percent reporting having no chronic diseases compared to 37 percent with four or more.
| Number of chronic diseases | Ages 45 to 64 years | Ages 65 to 79 years | Ages 80 years and older |
|---|---|---|---|
| No diseases | 40 | 12 | 8 |
| One disease | 29 | 23 | 14 |
| Two diseases | 16 | 23 | 21 |
| Three diseases | 8 | 17 | 20 |
| Four diseases | 7 | 25 | 37 |
|
|||
Source: Statistics Canada.
While the chronic conditions mentioned here are some of the more prevalent illnesses experienced by seniors, it is important to note that many seniors are affected by a combination of chronic conditions. In 2009, 25% of Canadian seniors aged 65 to 79 years and 37% of those aged 80 years and older reported having four or more of a wide-ranging list of chronic conditions (see Figure 3.5).Footnote 100
Chronic conditions, as well as vulnerabilities of the immune system and some medications, can make seniors more susceptible to infectious diseases such as seasonal influenza, West Nile virus and health care-associated infections (HAI).Footnote 137-Footnote 139 In 2008, 1,373 health care- associated methicillin-resistant Staphylococcus aureus (MRSA) infections were reported, nearly half (42%) of which were in patients aged 65 years and over.Footnote 140 During the same period, cases of vancomycin-resistant enterococcus (VRE) HAI and Clostridium difficile infection (CDI or C. difficile) were also more common in patients 65 years of age and over (50% and 65% respectively).Footnote 140 Based on hospitalized data from 2008/2009, seniors were also disproportionately affected by influenza infections (36%).Footnote 140 In February 2009, a point prevalence survey conducted in 49 hospitals across Canada demonstrated that 13% of hospitalized patients 65 years of age and older had one or more HAI, including either urinary tract infection (6%), pneumonia (3%), surgical site infection (2%), CDI (2%), blood stream infection (1%) or viral respiratory infection (1%).Footnote 140
Mobility and functional health
Generally, Canadian seniors report themselves to be in good functional health (based on levels of vision, hearing, speech, mobility, dexterity, feelings, cognition and pain).Footnote 141 In 2005, 62% of seniors (65% of men and 59% of women) were considered to have at least very good functional health.Footnote 141 Canadians aged 65 to 74 years were more likely to have levels of very good or perfect functional health (71%) than those aged 75 years and older (50%).Footnote 141
Despite these positive self-reports, some seniors do experience limitations as a result of long-term physical conditions caused by injury, disease and aging. One- quarter of Canadian seniors and 70% of Aboriginal seniors not living on a reserve reported they often have difficulty with one or more activities including hearing, seeing, communicating, walking, climbing stairs, bending, learning or other similar activities.Footnote 73 Footnote 142 Furthermore, activities of daily living (ADL) can be impaired. In all age groups, women were more likely than men to report requiring assistance with ADL such as meal preparation, housework, heavy household chores and personal care.Footnote 143
It is important to note that many issues of functional health that are common among seniors, such as age-related changes in vision, reaction time, power, coordination and the speed of cognitive processing, can have an effect on driving ability. Seniors who experience such limitations may be at an increased risk of motor vehicle collisions, depending on the extent of the decrease in function.Footnote 144 Footnote 145
Falls and related injuries
The most common cause of injuries among seniors in Canada is falls. It is estimated that one in three seniors is likely to fall at least once each year.Footnote 146 Footnote 147 In 2006, this translated into approximately 1.4 million Canadian seniors.Footnote 84 Footnote 146 Footnote 147
Various biological, medical, behavioural, environmental and socio-economic risk factors can contribute, either on their own or in complex interactions, to falls by seniors.Footnote 148 Aspects of physical health, such as chronic and acute illnesses, represent one such risk factor.Footnote 148 This may include visual or hearing impairment, lung disease, cardiovascular disease, arthritis, Parkinson's disease, stroke and disorders of blood pressure.Footnote 148-Footnote 150 Physical limitations – such as a physical disability, muscle weakness, reduced physical fitness (particularly in the lower body), difficulty with gait and balance, and disorders affecting the legs and feet – can also increase the risk of falling.Footnote 148-Footnote 151
As people age, certain situations or behaviours can increase the likelihood of falling due to mobility or balance issues. These can include climbing a ladder, wearing loose-fitting clothing or shoes, or carrying heavy or awkward objects.Footnote 149-Footnote 151 Additionally, many illnesses and conditions are treated with medications that can result in adverse reactions, either on their own or in combination with other medications, that can also increase the risk of falls.Footnote 148-Footnote 151
Seniors suffering from cognitive impairment due to depression, anxiety or dementia may also be at an increased risk of falling.Footnote 148 Footnote 149 Alcohol consumption, regardless of quantity and particularly in connection with other medical conditions, may also contribute to falls.Footnote 149
Seniors who are housebound or living alone are at greater risk for falls.Footnote 150 Footnote 151 As well, those who lack social networks may be more likely to undertake higher-risk activities that can increase their risk of falls.Footnote 150 Footnote 152
It is estimated that more than 180,000 Canadians 65 years and older suffered a fall in 2002/03 that caused injury.Footnote 148 More than two-thirds (68%) of those who fell and sustained injury were women.Footnote 148 Most of the injuries (37%) sustained from falls were to the hip, thigh, knee, lower leg, ankle or foot.Footnote 148 In fact, 95% of all hip fractures in this age group were the result of a fall.Footnote 153 Footnote 154 The most common cause of injurious falls was slipping, tripping or stumbling on a surface (44%), followed by falling on stairs (26%), and stumbling on ice or snow (20%).Footnote 148
In 2008/09, more than 50,000 Canadian seniors were hospitalized due to a fall.Footnote 153 The most common injuries due to falls were hip (38%) and other fractures (39%).Footnote 153 These injuries resulted in an average length of stay in the hospital of 15 days – a period 70% longer than the length of stay for any other cause of hospitalization for seniors.Footnote 153
Also during 2008/09, more than half (51%) of falls among seniors resulting in hospitalization occurred at home and approximately 18% occurred in residential institutions.Footnote 153 It is likely that seniors living in long-term care facilities, because of their frailty and disabilities, are more prone to falls and to suffer an injury due to the fall than those living in the community. Approximately half of long-term care facility residents fall each year, with one in ten falls resulting in a serious injury.Footnote 148
Most seniors who suffer falls eventually heal from their injuries but many never fully recover.Footnote 155-Footnote 158 For all falls among seniors, half result in minor injuries while an estimated 5% to 25% result in serious injuries including traumatic brain injuries and bone fractures.Footnote 148 Footnote 159 Footnote 160 Up to 40% of all fall-related hospitalizations among seniors involve hip fractures, which can have very serious consequences including a decline in overall quality of life, institutionalization and a decrease in life expectancy.Footnote 148 Footnote 151 Footnote 161 Among seniors who sustain a broken hip resulting from a fall, 20% die within a year of their fracture due to post-operative complications and/or pre-existing conditions such as cardiovascular or neurological diseases.Footnote 148 Footnote 162 Footnote 163 Other seniors recovering from hip fracture may develop post-fall syndrome, which includes dependence on others for daily activities, as well as a loss of autonomy, confusion, immobilization, fear of falling and depression.Footnote 146
Residual effects of injuries sustained by seniors can leave them with chronic pain, reduced functional abilities and curtailment of activities.Footnote 155-Footnote 158 Even if no injury occurs, the psychological impacts of falling can result in a loss of confidence and restriction of activities.Footnote 148 Footnote 164 Withdrawal from social activities can lead to isolation, making seniors vulnerable to loneliness and depression.Footnote 148 Further, fear of falling often results in dependence and reduced mobility, both of which can increase the risk of future falls.Footnote 148 Footnote 149 Footnote 151
Underweight and obesity
The body mass index (BMI) is a ratio of weight-to- height calculated as BMI = weight (kg)/height (m2).Footnote 165 There are six categories of BMI ranges in the weight classification system, each of which has a predetermined level of associated health risk:Footnote 165
| Classification | BMI Category (kg/m²) |
Level of Health Risk |
|---|---|---|
| Underweight | < 18.5 | Increased risk |
| Normal weight | 18.5-24.9 | Least risk |
| Overweight | 25.0-29.9 | Increased risk |
| Obese | ≥ 30.0 | |
| Obese Class I | 30.0-34.9 | High risk |
| Obese Class II | 35.0-39.9 | Very high risk |
| Obese Class III | ≥ 40.0 | Extremely high risk |
As in other age groups, being obese contributes to increased risk of poor health outcomes in seniors, including type 2 diabetes, hypertension and heart disease.Footnote 166-Footnote 168
Body mass index (BMI) is a common measure used to determine healthy and unhealthy weights. While BMI has been seen as an adequate measure for a portion of the population, standard BMI categories may not accurately reflect the state of overweight and obesity in seniors due to changing body composition.Footnote 6 Footnote 166 However, BMI is still the most commonly used measure for seniors given that there is no agreement on a better alternative.Footnote 6 Footnote 166
Using the standard classifications and BMI calculated from respondents' measured heights and weights, the percentage of seniors considered to be obese has increased from 22% in 1978/79 to 29% in 2008.Footnote 169 Footnote 170 In total, 28% of senior men and 31% of senior women were obese, which is greater than the proportions for all Canadians aged 18 years and older who were considered to be obese (26% of men and 24% of women).Footnote 170
Although the risks associated with being overweight are known for those under the age of 65, it is thought that there may be a protective effect associated with being slightly overweight for seniors. For example, overweight seniors may be more likely to survive acute illnesses, handle stress better and recover more quickly from traumas as a result of excess nutritional reserves.Footnote 171 In fact, being underweight may be a more important predictor of poor health than being overweight for those aged 65 years and older.Footnote 165 Footnote 172 Footnote 173 However, in determining weight classification research suggests the standard BMI underweight cut-off of less than 18.Footnote 5 may be inappropriate for seniors. This is because they may experience the increased health risks associated with being underweight, such as malnutrition, osteoporosis and mortality, at a higher BMI within the lower end of the standard "normal" BMI range.Footnote 165 Footnote 171-Footnote 173 Using an adjusted, higher, underweight BMI cut-off in the low 20s – a point thought to be more appropriate for this age group – 17% of seniors are estimated to be underweight.Footnote 165 Footnote 172-Footnote 174
Healthy behaviours
Many aspects of seniors' daily living are important factors in maintaining and improving their health. In particular, certain individual behaviours can significantly influence health and well-being for older Canadians such as physical activity, healthy eating and nutrition, smoking, alcohol and other substance use, and use of medications.
Physical activity
Physical activity plays an important role in preventing illness and dependence and enhancing mental health. However, as seen among many other age groups in Canada, most seniors are physically inactive, with activity levels tending to decrease with age.Footnote 7 In 2008, based on self-reported frequency, duration and intensity of participation in leisure-time physical activity, the majority of Canadian seniors (57%) were considered to be physically inactive.Footnote 175 Overall, 50% of senior men and 64% of senior women were inactive.Footnote 175 Seniors who have low-income or education levels, disabilities, chronic conditions, pain, lack of energy or motivation, or who have a fear of injury are less likely to be physically active.Footnote 7 Footnote 176 Seniors living in institutions, those who are isolated and those who have caregiving responsibilities may also be less physically active. Among the external barriers seniors face that can prevent or limit physical activity are cost, lack of transportation, adverse weather, and a lack of safe, accessible and affordable outdoor and indoor community space and recreational activities.Footnote 176 Footnote 177
The benefits of physical activity on the health and well- being of seniors, including a reduced risk of premature death, are well documented.Footnote 176 Footnote 178 Even physical activity that is not initiated until later in life, if it is maintained, still results in significant health benefits.Footnote 176 Regular physical activity is known to have a positive influence on functional capacity, mental health, fitness and overall well-being.Footnote 176 Footnote 179 Physical activity can also aid in the prevention or management of chronic conditions such as heart disease, high blood pressure, osteoporosis, stroke, obesity, and colon and breast cancers, and can aid in protection against anxiety and depression.Footnote 176 Footnote 179 Regular physical activity also helps maintain muscle and bone strength, coordination, joint function and flexibility, and supports independence by facilitating ADL.Footnote 176 As an added benefit, seniors can maintain social connectedness by participating in physical activities with others.Footnote 178
Healthy eating and nutrition
Healthy eating habits and nutrition can help to prevent illness and may reduce the necessity for medications and health care services over time.Footnote 180 When seniors eat a healthy diet, they benefit from increased mental acuity, improved resistance to illness and disease, faster recovery from illness and injury, a more robust immune system, higher energy levels and improved management of chronic health issues.Footnote 181 Yet reported food consumption of seniors shows that, like younger Canadians, many do not eat a balanced diet. For example, in 2004, 52% of men and 60% of women aged 71 and older reported that they did not consume the recommended daily minimum of five servings of fruits and vegetables.Footnote 182
As seniors age, a decrease in lean body mass means they require fewer calories, and therefore must consume foods with a higher concentration of nutrients to maintain the required intake of vitamins and minerals while decreasing calories.Footnote 180 Footnote 183 Food insecurity exists when someone does not have physical and economic access to sufficient, safe and nutritious foods to meet the needs of a healthy and active life.Footnote 184 While the majority of seniors are thought to be food secure, Aboriginal peoples and those living in rural or remote communities are more likely to face increased barriers to accessing nutritious foods through issues such as cost and availability.Footnote 185 Footnote 186 Poor nutrition or malnutrition, meaning a decrease in nutrient reserves, can result from "an insufficient or poorly balanced diet or faulty digestion or utilization of foods."Footnote 180 Footnote 187 Poor appetite, poor choice of foods or poor absorption of certain nutrients can all lead to malnutrition. These factors can be influenced by dietary restrictions, medications, physical or psychological diseases such as hypertension and depression, a change in the ability to taste or smell, difficulty chewing or swallowing, and alcoholism.Footnote 180 Footnote 181 Footnote 188 Footnote 189
Malnutrition is more prevalent (as much as 60%) among seniors in nursing homes or hospital environments where the health and functional capacities of residents are more likely to have deteriorated, than among seniors living in the community.Footnote 180 Seniors living alone or with health problems are also more prone to malnutrition as they may not enjoy eating meals alone, may make poor food choices, may not feel like cooking or may not know how to cook.Footnote 181 Footnote 188
Malnutrition among seniors can exacerbate the decline of immune and sensory functions and aggravate symptoms of chronic diseases such as cancer, cardiovascular disease, diabetes and osteoporosis.Footnote 7 Footnote 190 Unhealthy eating can also result in fatigue, problems with the heart, lungs and digestive system, low red blood cell count (anaemia), poor skin integrity and depression.Footnote 188 Additionally, malnourished seniors are at risk of reduced independence, early institutionalization and mortality.Footnote 180 Seniors who do not eat enough can experience dizziness and weakness, which increases the risk of falls. An inadequate intake of B vitamins can lead to reduced cognitive functions and an increased risk of dementia.Footnote 7 Footnote 191 Unintentional weight loss can lead to muscle and bone loss, which negatively impacts strength, balance and endurance, increasing the possibility of injuries.Footnote 7 Footnote 12
Smoking
Smoking is less prevalent among seniors than among the younger population, with 9% of Canadians aged 65 years and older being current smokers (either daily or occasional) and 47% being former smokers.Footnote 192 However, smoking is much more common among Aboriginal seniors, with 24% of those age 65 years and older not living on a reserve being daily smokers.Footnote 73 More specifically, 22% of First Nations seniors, 24% of Métis seniors and 36% of Inuit seniors are smokers and 39% of First Nations seniors, 43% of Métis seniors and 38% of Inuit seniors were smokers at one time but have since quit.Footnote 73
The effects of smoking on health and well-being are well documented.Footnote 7 Footnote 193 Footnote 194 Aside from its well-known association with lung cancer, heart disease and stroke, cigarette smoking is also related to an increased risk of hip fractures, cataracts, chronic obstructive pulmonary disease, kidney and pancreatic cancers, and periodontitis.Footnote 193-Footnote 195 Smoking can also interfere with various drug therapies, including anti-depressants, causing medications to be less effective.Footnote 194 Among seniors, the mortality rate of current smokers is double that of those who have never smoked.Footnote 194 Eight of the top fourteen causes of death among seniors have been linked to smoking and half of all long-term smokers die of tobacco-related illness.Footnote 193 Footnote 194
The majority of seniors who currently smoke have been smokers for most of their lives. Almost half (49%) of all seniors who have ever smoked (now or in the past) had their first cigarette by the age of 16 and 83% had done so by the age of 20.Footnote 192 Seniors who smoke tend to be less accepting of any health risks associated with smoking and, along with some of the general smoking population, may actually see smoking as a positive coping mechanism and use it to deal with emotional or stressful situations or to alleviate psychiatric symptoms.Footnote 7 Footnote 194
Contrary to the idea that seniors are too old to benefit from quitting smoking, overall health risks and risk of death from smoking-related illnesses decrease after seniors quit, while their quality of life improves within the first two years.Footnote 7 Footnote 196 Even someone who does not quit smoking until age 60 can expect to increase their life expectancy, on average, by three years compared to those who continue to smoke.Footnote 7 Footnote 196 Footnote 197 Seniors that do quit smoking tend to do so because of advice from a physician, self-motivation or as a consequence of being diagnosed with a serious health problem.Footnote 7 Footnote 194
Alcohol and other substance use
As with smoking, the rate of alcohol use among seniors is lower than that of younger age groups. However, the proportion of seniors with alcohol problems (6% to 10%) is the same as is found in other adult groups.Footnote 198 Footnote 199 Seniors, like younger Canadians, may use alcohol to cope with problems related to their life situation including stress, poverty, and lack of proper nutrition or housing.Footnote 199 Similarly, emotional problems arising from negative situations such as abuse, grief, loneliness or depression can also lead to alcohol use.Footnote 199 Footnote 200 Those faced with large amounts of free time after retirement may also turn to alcohol to help pass the time.Footnote 200
Seniors are more vulnerable to the effects of alcohol than are younger adults, as seniors' bodies process it more slowly.Footnote 199 Alcohol reduces muscle control, which increases the risk of falling for seniors and can also exacerbate certain health issues, including confusion and memory loss, liver damage, diabetes, heart or blood pressure problems, and stomach problems.Footnote 199 As well, more than 150 medications commonly prescribed to seniors can result in problems if consumed with alcohol; some may not work as they are meant to, while others may have an increased or dangerous effect.Footnote 199 This is a concern given that high rates of depression and suicide are associated with substance use issues among seniors.Footnote 198 Footnote 201
Among all age groups, health care professionals may have the most difficulty identifying seniors experiencing substance use/abuse issues given that indicators such as memory problems, confusion, lack of self-care, depression, sleep problems and falls may be incorrectly attributed to the effects of aging.Footnote 198
Medication use
When surveyed, 76% of Canadian seniors in private households reported using at least one medication (prescription and/or over-the-counter) in the past two days and 13% had used five or more different medications.Footnote 202 The proportions are even higher among seniors living in institutions, where 97% used one medication and 53% used five or more.Footnote 202
Properly prescribed and supervised pharmaceutical therapy can prolong life, reduce suffering and increase quality of life for seniors. Unfortunately, about 50% of prescriptions are not taken properly by seniors, which may reduce the medication's effectiveness or be potentially dangerous.Footnote 199 There is also a concern that some medications, such as those for anxiety, insomnia and inflammation, are over-prescribed for seniors.Footnote 203 This may be due to a communication gap between seniors and physicians, inaccessibility of alternate therapies, or the use of multiple physicians and pharmacies.Footnote 203
On their own, medications can cause adverse side- effects such as unsteadiness and confusion, delirium and increased levels of depression.Footnote 199 Up to 20% of hospitalizations of people over the age of 50 are the result of problems with medications.Footnote 199 Further, taking multiple medications can lead to unwanted drug interactions in which medications may not work as well or can cause dangerous reactions.Footnote 199 When used over a long period of time, certain medications can lead to dependence.Footnote 199
Mental health
Mental health is the capacity of each of us to feel, think and act in ways that enhance our ability to enjoy life and deal with the challenges we face. It is a positive sense of emotional and spiritual well-being that respects the importance of culture, equity, social justice, interconnections and personal dignity.Footnote 204
Mental illnesses are characterized by alteration in thinking, mood or behaviour – or any combinations thereof – associated with some significant distress and impaired functioning. Mental illnesses take many forms, including mood disorders, schizophrenia, anxiety disorders, personality disorders, eating disorders and addictions such as substance dependence and gambling.Footnote 204
Positive mental health can help seniors cope with many difficult issues and life events, such as chronic illness or the loss of partners and friends.Footnote 205 For seniors suffering from poor mental health or mental illness, the negative impacts are far-reaching. Mental health issues can affect physical health, emotional and social well-being, and quality of life.Footnote 205
In 2009, the majority of seniors reported they were, in general, satisfied with life (97%) and that they had very good or excellent mental health (70%).Footnote 100 Among those living in the community, an estimated 20% have some form of mental health issue versus 80% to 90% of those living in an institution.Footnote 206 Footnote 207 It is important to recognize however, that neither poor mental health nor mental illness can de dismissed as part of the normal aging process.Footnote 208 If left unmanaged, they can have a significant impact on the overall health and well-being of seniors.Footnote 208
Early life experiences and circumstances contribute to mental health over the lifecourse. Suffering abuse or living in a low-income household, for example, can negatively impact mental health.Footnote 205 Aboriginal seniors aged 55 and older who attended residential schools have reported experiencing higher rates of depression than those who did not attend residential schools.Footnote 73 Footnote 74 Footnote 209-Footnote 211 Conversely, learning positive coping skills early in life may contribute to positive mental health during childhood and into adulthood.Footnote 205 Most mental illnesses are known to manifest themselves in the early years and persist throughout the lifecourse, impacting overall health, happiness and productivity.Footnote 212 Footnote 213
Factors that can detract from mental health in the senior years and are more prevalent during this part of the lifecourse include stress related to a deterioration of physical health, isolation and loneliness, physical inactivity and chronic physical conditions.Footnote 205 Additionally, seniors caring for seniors are more likely to report psychological than physical health consequences.Footnote 214 Senior women, in particular, are more likely than senior men to report that they sometimes or nearly always feel stressed between helping others, trying to meet other responsibilities and finding time for themselves (31% of women compared to 19% of men).Footnote 214
Suicide is often associated with younger people, but men over the age of 85 have – on average – higher suicide rates (29 per 100,000) than all other age groups.Footnote 42 Footnote 124 Footnote 205 Although the rate of suicide deaths are lower among senior women, they have an overall higher rate of attempted suicide compared to senior men.Footnote 205
Common mental illnesses affecting the health of seniors include Alzheimer's disease and other dementias, depression and delirium.Footnote 205
Alzheimer's disease and other dementias
Although many people use the terms dementia and Alzheimer's interchangeably, dementia is actually the medical term used to describe a number of conditions characterized by the gradual loss of intellectual functions. Alzheimer's disease is one of those conditions and is the most common.Footnote 215
In 2008, an estimated 400,000 senior Canadians were living with dementia and it is estimated that this number will more than double within 30 years (see Figure 3.6).Footnote 215 Footnote 216 The estimated prevalence of dementia is higher among those aged 80 years and older, with a rate of 212 per 1,000 (55% of all Canadians with dementia), while seniors aged 65 to 79 years have a rate of 43 per 1,000.Footnote 42 Footnote 216 Senior women are more likely than senior men to be affected by dementia (103 per 1,000 versus 72 per 1,000 respectively).Footnote 42 Footnote 216
Figure 3.6 Projected prevalence of dementia in senior Canadians* by sex, Canada, 2008 to 2038Footnote 216
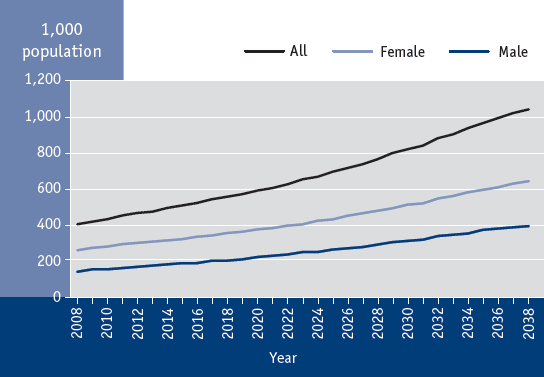
* The population over the age of 65 was simulated within the current model using data obtained from the Canadian Study of Health and Aging.
Sources: Smetanin, P. et al. Rising Tide: The Impact of Dementia in Canada 2008 to 2038.
[Figure 3.6, Text equivalent]
Summary: Between 2008 and 2038, prevalence of dementia among senior Canadians is projected to increase from 407,531 to 1,042,301 cases; from 144,372 to 396,944 among male seniors; and from 263,159 to 645,357 among female seniors. The population over the age of 65 was simulated within the current model using data obtained from the Canadian Study of Health and Aging.
| Year | All seniors | Male seniors | Female seniors |
|---|---|---|---|
| 2008 | 407,531 | 144,372 | 263,159 |
| 2013 | 473,872 | 172,459 | 301,414 |
| 2018 | 550,912 | 203,035 | 347,877 |
| 2023 | 648,016 | 245,212 | 402,804 |
| 2028 | 761,526 | 287,879 | 473,647 |
| 2033 | 902,024 | 344,334 | 557,691 |
| 2038 | 1,042,301 | 396,944 | 645,357 |
|
|||
Source: Smetanin, P. et al. Rising Tide: The Impact of Dementia in Canada 2008 to 2038
The cause of Alzheimer's disease is unknown though research suggests that it results from a combination of risk factors.Footnote 217 One risk factor is age itself given that, as a person ages, the brain's ability to repair itself decreases. Canadian seniors are also at greater risk of other factors associated with Alzheimer's disease such as high blood pressure, elevated cholesterol and being overweight.Footnote 215 Footnote 217 Type 2 diabetes, stroke and chronic inflammatory conditions such as some forms of arthritis are also known to be risk factors for Alzheimer's disease and associated dementias.Footnote 215 Footnote 217
Genetics can also contribute to the risk of developing both inherited Familial Alzheimer's disease and the more common sporadic forms of the disease. Those with an immediate family member with the disease are two to three times more likely to develop it themselves than those who do not have a direct relative with the disease.Footnote 215 Footnote 217 Women are at greater risk for Alzheimer's disease and associated dementias than men, in part due to the fact that they generally live longer. Hormonal changes at menopause are also thought to contribute to women's increased risk.Footnote 217 Other identified risk factors are a history of prior head injury, Down syndrome, a history of episodes of clinical depression, chronic stress, lack of physical exercise, inadequate intellectual stimulation, unhealthy eating habits, low levels of formal education and low socio-economic status.Footnote 215 Footnote 217
Memory problems are one of the earliest symptoms of Alzheimer's disease.Footnote 218 The disease is progressive and, depending on the stage, can range in severity from mild to severe.Footnote 218 Mild forms can cause problems such as getting lost, difficulty handling money or paying bills, taking longer to complete routine tasks, repeating of sentences, poor judgement and small changes in mood or personality.Footnote 218 Moderate Alzheimer's disease causes damage to parts of the brain controlling language, reasoning, sensory perception and conscious thought resulting in increased memory loss and confusion. Persons with moderate Alzheimer's disease also experience difficulty recognizing friends and family, difficulty or an inability to learn new things, difficulty performing tasks with multiple steps, difficulty coping with new situations, hallucinations, delusions, paranoia and impulsive behaviour.Footnote 218 In those diagnosed with severe Alzheimer's disease, significant shrinkage of the brain tissue results in an inability to communicate, as well as complete dependence on others for care.Footnote 218
Depression
Depression, being a mood disorder, can prevent seniors from fully enjoying life and affect many aspects of their health.Footnote 205 Footnote 219 Emotional and psychological manifestations of depression include sadness, feelings of worthlessness or guilt, fixation on death with thoughts of and/or attempts at suicide, trouble concentrating, loss of interest in hobbies or other enjoyable activities, and social withdrawal and isolation.Footnote 208 Footnote 219 Seniors living with depression can suffer from fatigue, changes in weight and appetite, sleep disturbances, and physical aches and pains.Footnote 208 Footnote 219 If left untreated, depression may also result in alcohol and prescription drug abuse.Footnote 208 Footnote 219
There are several factors that can cause or increase the risk of depression in seniors and many are the result of life changes that occur with aging. Physical influences include chronic illness, disability, chronic pain, cognitive decline and certain medications.Footnote 219 Footnote 220 Emotional events such as the loss of a spouse, friend or family member can contribute to depression in seniors, as can the reduced sense of purpose which may come with retirement or physical limits on activities.Footnote 219 Footnote 220 Loneliness and isolation – which may result from living alone, a reduced social circle or decreased mobility – are also potential risk factors for depression, as are common fears among seniors such as challenges with health issues or a fear of falling.Footnote 219 Footnote 220
The prevalence of depression is higher among women than men, although the reasons why are not entirely understood. For both sexes, those who have been depressed in the past or who have a biological relative with depression are at greater risk of depression.Footnote 220 Levels of diagnosed depression also vary by location of residence. Seniors who continue to live within the community tend to have lower rates of diagnosed depression (1% to 5%) compared to seniors living in long-term care facilities (14% to 42%).Footnote 221-Footnote 225 A recent study of Canadian seniors living in residential care found that 44% had either been diagnosed with depression or showed symptoms of depression without diagnosis.Footnote 221
Although it is not clear why, depression can also lead to higher mortality rates, even when other risk factors are taken into account.Footnote 219 Footnote 226 Footnote 227 In studies, seniors with depression were one and a half to two times more likely to die than those without depression.Footnote 221 Footnote 222 Footnote 225 Footnote 227-Footnote 230
Delirium
Delirium (also known as acute confusion) is another mental health condition found most commonly among seniors. It is characterized by impairment in the ability to think clearly, to pay attention or to remember a few days or hours ago. Onset is fairly rapid over a short period of time – from several hours to days – and is usually temporary, lasting for a few hours up to several weeks.Footnote 231 Footnote 232 Delirium often occurs in hospitalized seniors. It is estimated that 10% to 15% of hospitalized seniors have the condition at the time of admittance while 15% to 25% develop it during their stay.Footnote 233 Delirium can also increase the risk of falling and the length of hospitalization.Footnote 234 While the number of seniors in the community who experience episodes of delirium are unknown, it is thought that 32% to 67% of seniors with delirium go undiagnosed.Footnote 233 Footnote 235 Footnote 236
Causes for delirium can include severe infections, high fever, lack of fluids, diseases of the kidney or liver, lack of certain vitamins, seizures, lack of oxygen, head injury, reaction to certain medications or alcohol, or as the result of surgery or a fall.Footnote 231 Footnote 232 In many cases, delirium is not recognized or is misdiagnosed as another condition such as dementia or depression.Footnote 232 Footnote 237
Economic well-being
Income is known to be an important determinant of health, with those living in low-income – including seniors – at greater risk of poor health.Footnote 174 Seniors living in low-income may be unable to access nutritious foods, have difficulties paying their mortgage, rent or utilities, be unable to complete necessary repairs on their homes, and experience limitations in terms of access to and affordability of transportation and non-insured health services, all of which can impact negatively on health.Footnote 238
In 2008, 6% of Canadian seniors were living in low-income. As illustrated by Figure 3.7, this number represents a large decrease from 29% in 1978. Rates have dropped over this time period following the earlier introduction of retirement and financial income supplement programs in Canada.Footnote 239
Figure 3.7 Persons with incomes below the after-tax* low-income cut-offs, by selected age groups, Canada, 1978 to 2008Footnote 239

* These income limits were selected on the basis that families with incomes below these limits usually spent 63.6% or more of their income on food, shelter and clothing. Low-income cut-offs were differentiated by community size of residence and family size.
Source: Statistics Canada.
[Figure 3.7, Text equivalent]
Summary: Between 1978 and 2008, the percentage of the population with incomes below the after-tax low-income cut-offs changed from 12.5 to 9.1 among persons under 18 years; from 9.6 to 10.2 among persons 18 to 64 years; and from 29.4 to 5.8 among persons 65 years and over.
| Year | Percentage of population for Persons under 18 years | Percentage of population for Persons 18 to 64 years | Percentage of population for Persons 65 years and over |
|---|---|---|---|
| 1978 | 12.5 | 9.6 | 29.4 |
| 1983 | 15.8 | 12.5 | 19.4 |
| 1988 | 12.2 | 10 | 13 |
| 1993 | 17 | 13.6 | 10.7 |
| 1998 | 15.7 | 13.9 | 8.6 |
| 2003 | 12.7 | 12.2 | 6.8 |
| 2008 | 9.1 | 10.2 | 5.8 |
|
|||
Source: Statistics Canada
The decrease in the proportion of seniors living in low-income has been similar for men and women when measured using both before- and after-tax income (see Figure 3.8).Footnote 239 However, the decrease for women has been slightly greater, contributing to the narrowing gap between the percentage of men and women living in low-income.Footnote 73 Between 1978 and 2008 the gap in after-tax income between senior men and women decreased from 10% to 4%.Footnote 239
However, not all subpopulations of seniors are experiencing such low proportions of those living in low-income. In 2001, 13% of Aboriginal seniors were living in low-income households compared to 7% of non-Aboriginal seniors. Similarly, 50% of unattached Aboriginal seniors (those not living with family) were living in low-income compared to 40% of unattached non-Aboriginal seniors.Footnote 73 In the same year, 17% of immigrant seniors living in Canada for less than 20 years and 8% of those living here 20 years or more lived in low-income households compared to 5% of Canadian-born seniors. For unattached immigrant seniors, 67% of those living in Canada less than 20 years and 43% of those living in Canada 20 years or more were living in low-income compared to 39% of unattached Canadian-born seniors. Also in 2001, 19% of all unattached senior Canadian women were living in low-income.Footnote 239
Figure 3.8 Canadian seniors living in low-income before-tax† and after-tax* by sex, Canada, 1978 to 2008Footnote 239
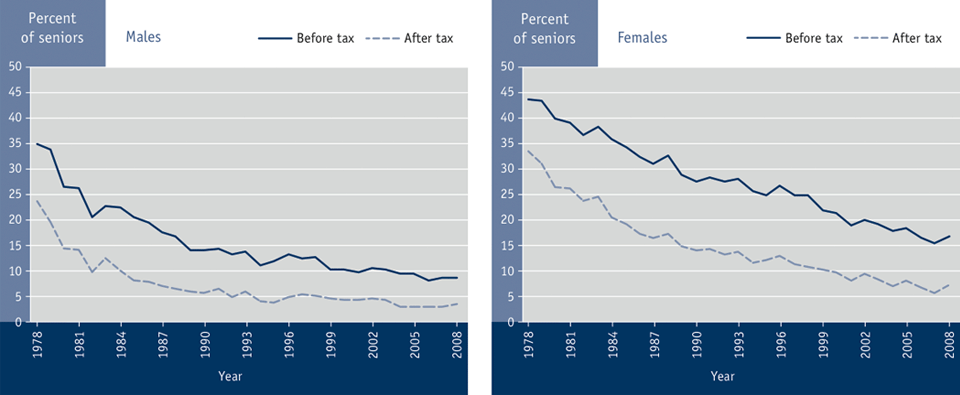
† These income limits were selected on the basis that families with incomes below these limits usually spent 54.7% or more of their income on food, shelter and clothing. Low-income cut-offs were differentiated by community size of residence and family size.
* These income limits were selected on the basis that families with incomes below these limits usually spent 63.6% or more of their income on food, shelter and clothing. Low-income cut-offs were differentiated by community size of residence and family size.
Source: Statistics Canada.
[Figure 3.8, Text equivalent]
Summary: Between 1978 and 2008, the percent of Canadian seniors living in low-income before-tax decreased from 23.8 to 3.6 for males and from 33.7 to 7.6 for females; the percent of Canadian seniors living in low-income after-tax decreased from 34.9 to 8.7 for males and from 43.8 to 16.8 in females.
| Year | Percent of Males living in low-income, after tax |
Percent of Females living in low-income, after tax |
Percent of Males living in low-income, before tax |
Percent of Females living in low-income, before tax |
|---|---|---|---|---|
| 1978 | 23.8 | 33.7 | 34.9 | 43.8 |
| 1983 | 12.6 | 24.6 | 22.7 | 38.2 |
| 1988 | 6.8 | 17.5 | 16.6 | 32.6 |
| 1993 | 6.2 | 14.1 | 13.8 | 28.1 |
| 1998 | 5.4 | 11.1 | 12.6 | 24.8 |
| 2003 | 4.4 | 8.7 | 10.2 | 19.2 |
| 2008 | 3.6 | 7.6 | 8.7 | 16.8 |
|
||||
Source: Statistics Canada
The additional benefits available to Canadians since the inception of Canada's public pension system have helped to increase the average after-tax income for senior couples by 18% between 1980 and 2003.Footnote 73 The Luxembourg Income Study has credited Canada's pension system as being a major factor in the shift from ranking Canada as a nation with one of the highest occurrences of low-income seniors in the late 1980s to one of the lowest in the mid-2000s (see Figure 3.9).Footnote 73 Footnote 240
In 2006, over 95% of seniors received some of their income from OAS, the GIS or the Spouse's Allowance (SPA).Footnote 241 In addition, 96% of older men and 84% of older women received CPP/ QPP benefits.Footnote 241 Those who did not receive these benefits were either ineligible or did not apply to receive them.Footnote 242 For example, in 2006 more than 150,000 seniors who were eligible to receive the GIS did not.Footnote 243 Combined, these federal supplements accounted for 43% of the total income of all Canadian seniors.Footnote 241 In 2000, 73% of Aboriginal seniors' income came from OAS, CPP, GIS and Employment Insurance (EI), compared to 48% for non-Aboriginal seniors.Footnote 73 More than half of seniors (62%) receive some sort of retirement income from private sources, such as workplace pension plans and Registered Retirement Savings Plans (RRSPs), representing 34% of the total annual income for all Canadian seniors.Footnote 241
Figure 3.9 Relative low-income* rates among older persons, select countriesFootnote 240

* A relative measure based on low-income cut-off defined as one-half of the median family income after-tax in each country.
Source: Luxembourg Income Study.
[Figure 3.9, Text equivalent]
Summary: The relative low-incomes rate has changed in Poland from 17.0 in 1986 to 3.5 in 2004; in Canada from 10.8 in 1987 to 6.3 in 2004; in Sweden from 7.2 in 1987 to 6.6 in 2005; in Norway from 21.7 in 1986 to 8.5 in 2004; in the United Kingdom from 7.0 in 1986 to 16.3 in 2004; in Australia from 24.3 in 1985 to 22.3 in 2003; and in the United States from 23.5 in 1986 to 24.6 in 2004.
| Country | Percent of Population | Year (Mid-1980s) | Percent of Population | Year (Mid-2000s) |
|---|---|---|---|---|
| Poland | 17.0 | 1986 | 3.4 | 2004 |
| Canada | 10.8 | 1987 | 6.3 | 2004 |
| Sweden | 7.2 | 1987 | 6.6 | 2005 |
| Norway | 21.7 | 1986 | 8.5 | 2004 |
| United Kingdom | 7.0 | 1986 | 16.3 | 2004 |
| Australia | 24.3 | 1985 | 22.3 | 2003 |
| United States | 23.5 | 1986 | 24.6 | 2004 |
|
||||
Source: Luxembourg Income Study
The level of educational attainment of seniors during their formal schooling years is reflected in their income levels throughout life (see Figure 3.10).Footnote 244 Between 2002 and 2007, Canadians aged 65 and older whose highest level of education was a high school diploma or less were more than twice as likely as those with a university degree (13% vs. 5%) to have lived in a low-income household at some point during that five-year period.Footnote 245
Figure 3.10 Median after-tax income for seniors by sex and highest education level attained, Canada, 2006Footnote 244
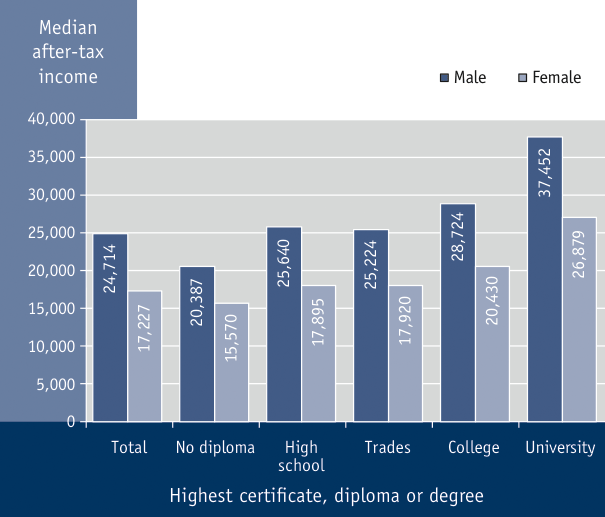
Source: Statistics Canada.
[Figure 3.10, Text equivalent]
Summary: In 2006, the median after-tax income for Canadian seniors was $24,714 for males and $17,227 for females; for those with no diploma, $20,387 for males, $15,570 for females; for those with high school diplomas, $25,640 for males, $17,895 for females; for those with trades degrees, $25,224 for males, $17,920 for females; for those with college degrees, $28,724 for males, $20,430 for females; and for those with university degrees, $37,452 for males, $26,879 for females.
| Highest certificate, diploma or degree | Males | Females |
|---|---|---|
| Total | 24,714 | 17,227 |
| No diploma | 20,387 | 15,570 |
| High school | 25,640 | 17,895 |
| Trades | 25,224 | 17,920 |
| College | 28,724 | 20,430 |
| University | 37,452 | 26,879 |
Source: Statistics Canada
Social well-being
The social well-being of seniors is influenced by a number of factors, including satisfaction with life, social connectedness with others, and whether or not they are productive and active in the community. Poor levels of social well-being can negatively impact health and quality of life.
Social connectedness and isolation
Canadians who are not able to access, or do not participate in, social support networks may lack social connectedness, become isolated or lonely, or lack a sense of belonging.Footnote 205 Footnote 246 In 2009, approximately 70% of seniors reported feeling a somewhat or very strong sense of belonging to their community.Footnote 175 In fact, more seniors reported feeling a strong sense of community belonging than any other age group except youth (aged 12 to 19 years).Footnote 175
Although it is unclear whether it is good health that follows from or leads to social connectedness, the two are interrelated. In the 2003 CCHS, 62% of seniors who reported a strong sense of community belonging also reported good health, compared to only 49% of those who felt less connected.Footnote 179 A study of older U.S. adults (aged 50 years and older) found that higher levels of social integration based on marital status, volunteer activity, and frequency of contact with children, parents and neighbours, was associated with delayed memory loss as they aged.Footnote 247
The process of aging reduces social networks, as seniors tend to focus their networks around those with whom they have an emotional closeness, whereas younger adults tend to have broader social circles.Footnote 248 Additionally, as people age, they are faced with illness, disability and the increasing loss of friends and family members, which further limits their opportunity for social networking.Footnote 7 Footnote 249 Footnote 250
Life circumstances such as living arrangements, retirement and geographic proximity to family can also factor into the level of social connectedness experienced by seniors.Footnote 7 Footnote 249 Footnote 250 The majority of seniors (93%) live in private households; nearly two-thirds (65%) live with a spouse; and more than one-quarter (28%) live alone.Footnote 73 Footnote 95 A larger proportion of men live with a spouse than women (79% compared to 54% respectively) and of those aged 75 to 84 years, women (43%) are more likely to live alone than men (18%).Footnote 95 Immigrant seniors, particularly those who are recent immigrants, are less likely to live alone compared to Canadian-born seniors.Footnote 73
Having at least one close friend can be an important factor in reducing a sense of isolation. In 2003, 88% of those aged 65 to 74 years and 82% aged 75 years and older reported they had at least one close friend.Footnote 73 Footnote 251 In 2001, the majority of Aboriginal seniors not living on a reserve (70%) reported that they had someone to listen when they needed to talk, all or most of the time.Footnote 73 Canadian seniors who belong to an organization (e.g. community group, political party, religious organization) are less likely to report a sense of social isolation and are more likely to report having six or more friends.Footnote 73
Transportation or economic barriers can sometimes limit or prevent social opportunities.Footnote 7 Footnote 249 Footnote 250 Issues of physical mobility and lack of access to safe and affordable public spaces are also barriers to social connectedness.Footnote 7 Footnote 82 Additionally, some individuals may not call on others for the support they need because they feel they are supposed to be, or should appear to be, independent.Footnote 252
Remaining connected through various activities, including organizational involvement or volunteering, gives seniors a sense of purpose and belonging to something bigger than themselves.Footnote 253 In 2007, 36% of seniors aged 65 and older volunteered in some capacity and, on average, contributed more hours annually than any other age group.Footnote 254 More than half (54%) of the seniors surveyed indicated a health problem or being physically unable, as a reason for not volunteering or not volunteering more.Footnote 254 Research on the effect of volunteering on well-being showed that those aged 60 years and older who volunteered reported higher levels of well-being, regardless of the number of organizations for which they volunteered, the type of organization or the perceived benefit of the work to others.Footnote 255
Ongoing involvement in volunteer activities has been shown to moderate the negative psychological impacts associated with developing functional limitations.Footnote 256 In addition to improved mental health, seniors who volunteer may reduce their chances of developing heart disease, diabetes and cardiovascular disease.Footnote 7 Research has shown that seniors who participated in social activities had significantly lower mortality rates than those who did not.Footnote 257
Labour and retirement
Whether due to a return to work after retirement or simply delaying retirement past the age of 65, participation in the paid labour force among senior Canadians has been increasing (see Figure 3.11).Footnote 73 Footnote 258 In 2009, more than 400,000 seniors (11%) were active in the paid workforce (15% of senior men and 7% of senior women).Footnote 258 This was up from nearly 200,000 (7%) in 1990.Footnote 258
Figure 3.11 Paid employment rate of seniors by sex, Canada, 1990 to 2009Footnote 258
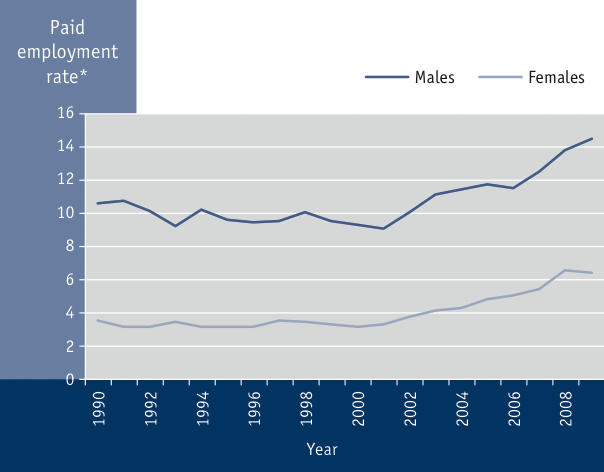
* The number of persons employed expressed as a percentage of the population 65 years of age and over.
Source: Statistics Canada.
[Figure 3.11, Text equivalent]
Summary: From 1990 to 2009, the paid employment rate (the number of persons employed is expressed as a percentage of the population 65 years of age and over) among Canadian seniors has increased from 10.6% to 14.5% for males and from 3.5% to 6.4% for females.
Source: Statistics Canada
Retirement from the labour force can be a significant change for many individuals and can influence their standard of living, daily activities and social networks. Recent changes to labour laws and retirement policies have affected the age at which Canadians retire in some provinces.Footnote 47 Mandatory retirement policies were the reason why one in five retirees reported that they left the labour force at the age of 65 years in 2002.Footnote 73 Health problems were also cited as a reason for retirement (24% of retirees).Footnote 73 Of all retirees aged 50 years and older, 26% reported they would have continued to work if ill health had not been an impediment.Footnote 73
Almost half of recent retirees (47%) reported that they enjoyed their retired life more than their pre-retirement life.Footnote 73 Those who reported good to excellent health entering retirement also indicated an increase in life satisfaction post-retirement.Footnote 73 After retirement, some individuals choose to return to the labour force for various reasons including unhappiness with retirement, missing employment, looking for an opportunity to do more satisfying work or because of financial need.Footnote 73 In general, men are more likely than women to return to the labour force (25% compared to 18%).Footnote 73
Giving and receiving care
Canadians, regardless of age, occasionally depend on social networks of family, friends and neighbours to help with errands and daily tasks. In 2003, 29% of seniors aged 75 and older reported receiving help from someone outside their home for transportation or running errands.Footnote 73 The majority of seniors aged 65 to 75 years old (84%) did not receive transportation help, partly because they had access to a vehicle (89%) and possessed a valid driver's license (85%).Footnote 73 Overall, seniors living alone were more likely to receive help with domestic work, home maintenance, outdoor work and emotional support.Footnote 73
In 2002, approximately 25% of seniors living in private homes reported that they received help or care due to a long-term health problem.Footnote 73 Another 2% reported they needed care but did not receive it.Footnote 73 Almost three-quarters (72%) of seniors receiving care got some or all of their help from informal sources, such as family and friends.Footnote 73 Seniors living alone were more likely (64%) to receive help from formal sources such as government and non- government organizations.Footnote 73
Seniors are not only care recipients; many are also caregivers to others, including other seniors. While many seniors (47%) care for immediate family, they also take care of friends and neighbours (38%) and other relatives (13%).Footnote 259 In 2007, of caregivers aged 45 and over who provided some form of unpaid/informal care to a senior with a long-term health condition or physical limitation, 16% were seniors aged 65 to 74 years and 8% of were seniors aged 75 years and older.Footnote 259 Footnote 260 Among seniors caring for other seniors, most (63%) were caring for two or more people.Footnote 259 A quarter (25%) of seniors caring for other seniors spent 10 or more hours per week and 15% spent 20 or more hours per week engaged in unpaid care of another senior.Footnote 261 Two-thirds of seniors caring for seniors are younger than age 75 and more than half (57%) are women, although the gender gap is narrowing as more men become involved in caring for older family members and friends.Footnote 262
About one in five seniors caring for other seniors reported that their social activities changed as a result of their caring roles (23% of women; 21% of men).Footnote 214 The social isolation and lack of "downtime" that may result from caregiving responsibilities have the potential to manifest as poorer physical and emotional health for caregivers.Footnote 214 While the ability of seniors caring for seniors to partake in social activities can be limited, 70% of senior women caregivers and 66% of senior men caregivers reported the benefit of a strengthened relationship between themselves and their care recipient.Footnote 214
Access to care and services
Canadian seniors must be able to access appropriate care and services in order to maintain or improve their health and well-being. This can include a wide range of resources and support such as physician services, in-home care and social support. In 2009, most seniors (96%) reported having a regular family physician.Footnote 100
Seniors who receive care and support do so through formal home care services (government-subsidized, private agency or volunteer) and informal support (provided by friends, family or neighbours).Footnote 263 In 2003, 15% of senior households reported receiving either formal or informal care.Footnote 263 And more senior women than senior men indicated they received formal (10% compared to 7%) and informal (5% compared to 3%) care services.Footnote 263 Not surprisingly, as seniors age the demand for both formal and informal home care services increases (see Figure 3.12).Footnote 263
Figure 3.12 Percentage of seniors who received home care in the past year, Canada, 2003Footnote 263
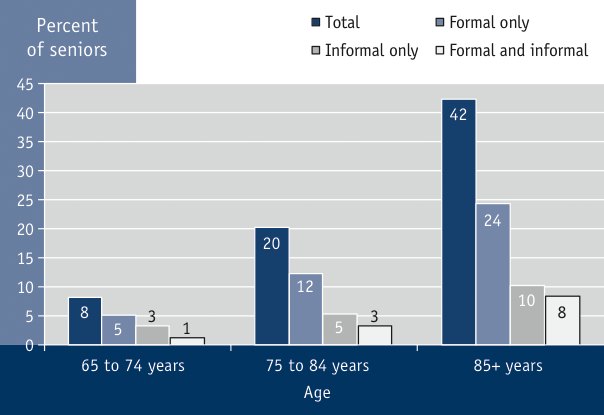
Source: Statistics Canada.
[Figure 3.12, Text equivalent]
Summary: In 2003, 8% of Canadian seniors age 65 to 74 had received home care in the past year, with 5% receiving only formal care, 3% receiving only informal care, and 1% receiving both formal and informal care; 20% of Canadian seniors age 75 to 84 had received home care in the past year, with 12% receiving only formal care, 5% receiving only informal care, and 3% receiving both formal and informal care; 42% of Canadian seniors age 85 or older had received home care in the past year, with 24% receiving only formal care, 10% receiving only informal care, and 8% receiving both formal and informal care.
| Age | Total | Formal care only | Informal care only | Formal and informal care |
|---|---|---|---|---|
| 65 to 74 years | 8 | 5 | 3 | 1 |
| 75 to 84 years | 20 | 12 | 5 | 3 |
| 85+ years | 42 | 24 | 10 | 8 |
Source: Statistics Canada
Seniors requiring intense, ongoing care that cannot be provided at home are more likely to reside in long-term care facilities. Over the last two decades the proportion of seniors living in these facilities has remained fairly constant at about 7%, although the degree of unmet need for, and within, such facilities is not known.Footnote 264 The number of facilities where support is provided has also remained fairly stable over the same period, ranging from approximately 2,000 operating facilities across Canada with 160,000 beds in 1986 to 2,100 operating facilities with 207,000 beds in 2006.Footnote 265 Of the total operating facilities in existence in 2006, 54% were run by private organizations or corporations, 26% were run by religious and other non-profit organizations, and 20% were run by municipal, provincial, territorial or federal governments.Footnote 266
In 2009, 56% of Canadian seniors had visited a dental professional in the past 12 months, while 20% had not visited one in five or more years.Footnote 100 Good oral health is important to the overall health and well-being of seniors. Poor oral health can result in a range of negative health outcomes including gum disease, lung infections and respiratory disease.Footnote 267 Additionally, tooth loss or pain from such things as gum disease, tooth decay or ill-fitting dentures can lead to difficulty chewing and subsequent poor nutrition or malnutrition.Footnote 268 According to the results from the oral health component of the Canadian Health Measures Survey (CHMS) (2007-2009), 13% of adults aged 60 to 79 avoided eating certain foods because of problems with their mouth.Footnote 269 Limited ability to endure a procedure, anxiety or fear of procedures, and reduced desire to access dental services as a result of medications or a decline in cognitive ability can all present barriers to appropriate dental care for seniors.Footnote 270 Further, some seniors mistakenly feel that they have no need for such care.Footnote 270 Footnote 271
Results from the CHMS (2007-2009) indicated that costs associated with dental care was a contributing factor for 13% of adults aged 60 to 79 years avoiding seeing a dental professional, while a further 16% declined care due to cost.Footnote 269 These percentages increase for persons aged 60 to 79 years who are living in low-income with 24% avoiding visits and 22% declining all recommended care due to costs.Footnote 269 As well, a dentist may be reluctant to treat elderly patients due to the fact that treatment may take longer and be more difficult, or based on the misconception that seniors have insufficient patience, endurance or finances to undergo treatment.Footnote 270 For the many seniors who do not have dental insurance, financial considerations may be the greatest barrier.Footnote 272
Seniors' access to care and services can be affected by a number of factors such as availability of resources and health information, awareness regarding community health services or inclination to inquire about them.Footnote 272
Moreover, physicians may mistakenly attribute a senior's health concerns to the natural aging process, which can lead to inadequate assessment and follow-up.Footnote 272 Seniors who are deaf or hard of hearing can experience communication barriers, and for seniors with mobility issues or disabilities, physical access to a building can be an obstacle to services.Footnote 272 Seniors may also face attitudinal barriers that can prevent them from obtaining appropriate care and information. For example, being considered a "hard-to-serve" client or being treated as incapable of making their own decisions, may result in service providers consulting with family members about important decisions instead of with the seniors themselves.Footnote 272
Seniors may also need to travel great distances to reach a doctor, hospital, or specialized health or diagnostic testing service not available in their local community.Footnote 273 Therefore, transportation issues (including costs associated with travel), physical mobility issues or reliance on outside help for transportation can limit seniors' access to these services.Footnote 272 Many of these factors can be further compounded by weather conditions that can make travel difficult.Footnote 273 In northern, rural and remote areas, seniors often have to manage with limited services since health care facilities are fewer and more dispersed compared to urban regions.Footnote 273 There is also a limited number of health care providers (e.g. physicians, nurses, dentists) to offer health care services in northern, rural and remote areas.Footnote 273 As a result, families may end up caring for seniors without adequate support. In the event families are not able to provide this care, seniors may have to be relocated to institutions in larger communities, potentially isolating them from family, friends and their home communities.Footnote 273
For some seniors, financial concerns can create additional barriers to care and services. The high cost of prescription medication and assistive devices (such as mobility aids or information technologies) may make these items prohibitive to seniors who require them.Footnote 272 Even those seniors with private health benefits or who are eligible for a provincial health or drug plan may not be covered for some of the costs associated with these drugs and devices.Footnote 272 Footnote 274
Health Literacy is "the ability to access, understand, evaluate and communicate information as a way to promote, maintain and improve health in a variety of settings across the life-course."Footnote 275
Another factor influencing seniors' health and well-being is the level of health literacy among this population. In order to manage chronic conditions or other health problems and to make healthy lifestyle choices, seniors need to be able to read and interpret nutrition labels, follow dosage directions for medications and understand health information and instructions.Footnote 276 Only one in eight adults (12%) over age 65 has adequate health literacy skills for many basic health-related decisions.Footnote 276-Footnote 278 Age is associated with lower health literacy of seniors due to several factors, including less opportunity for higher education earlier in life, slower processing of new information, higher incidence of mild cognitive impairment and dementia, and increased vision and hearing impairment.Footnote 73 Footnote 277 Footnote 279 Seniors with lower health literacy scores are more likely to report poorer health, including an increase in the prevalence of diabetes, as health literacy decreases.Footnote 280
Seniors who are Aboriginal, part of an ethnic minority group or who are new to Canada may face several additional barriers to accessing proper health care, such as conflicting cultural values or language barriers.Footnote 281 They may also avoid residential care unless they can retain their culture by speaking their language, eating their own food and properly observing their religion.Footnote 281 For immigrants, a lack of understanding of the roles of the health authority and service providers, and unfamiliarity with the various types of community services may present further impediments.Footnote 281 They may also be ineligible for full access to health care services or financial assistance depending on their immigration status.Footnote 281
Abuse and neglect of seniors
The term abuse as it relates to seniors, has been defined by the World Health Organization as "a single, or repeated act, or lack of appropriate action, occurring within any relationship where there is an expectation of trust which causes harm or distress to an older person."Footnote 282
One particularly concerning issue for the well-being of seniors is the potential for physical, psychological and financial abuse or neglect. It is difficult to know the extent of this problem in Canada since the data are extremely limited, outdated and, due to the nature of the issue, most likely under-reported. Research estimates, however, that between 4% and 10% of Canadian seniors experience some form of abuse or neglect from someone they trust or rely on.Footnote 283-Footnote 285 Further, there is a lack of data on abuse and neglect of older adults in institutional settings although light has been shed on this problem through anecdotal reports and localized studies.Footnote 286 Just as the abuse and neglect of seniors can take many forms, the resulting effects of the abuse can have an impact on many aspects of their health and well-being.Footnote 287 Footnote 288
In 2007, 48 out of every 100,000 seniors in Canada were the victims of a police-reported crime at the hands of a relative.Footnote 289 The most frequently reported form of violent crime committed by relatives towards seniors was common assault (52%), which includes actions associated with physical abuse such as pushing, punching, slapping and threatening to apply force.Footnote 289 Another 19% of violent crimes were threats and 16% were major assaults in which a weapon was used or which caused bodily harm.Footnote 289 Adult children and spouses (both current and former) were the most common perpetrators of violent crimes against senior victims.Footnote 289 Senior women were victimized by a spouse or ex-spouse at almost twice the rate of senior men (17 per 100,000 compared to 9 per 100,000 respectively). Senior male victims of family violence were more likely to be victimized by their adult children (15 per 100,000) than by any other relative.Footnote 289 The extent of unreported cases of physical abuse against seniors in Canada is unknown.Footnote 284 Footnote 285
Abuse can result in direct physical outcomes such as injuries. In 40% of the police-reported cases of physical abuse involving seniors in 2007, the victim sustained some form of injury, usually due to physical force.Footnote 289 Canadian seniors may be more frail than younger adults and, as a result, their bones may break more easily and take longer to heal.Footnote 288 Additionally, abuse can cause other less obvious negative physical health outcomes such as gastrointestinal problems and headaches, and may aggravate other pre-existing health problems.Footnote 288 Footnote 290 Research has also shown that seniors who are victims of abuse have higher mortality rates than non-abused seniors.Footnote 288 Footnote 291 Footnote 292
The health of seniors can also be impacted by psychological and/or emotional abuse. This type of abuse can include any action, verbal or non-verbal, which lessens a person's sense of identity, dignity or self-worth.Footnote 293 Available data from 1999 shows that approximately 7% of Canadians aged 65 years and older surveyed by Statistics Canada reported that they experienced some form of emotional abuse.Footnote 294 Seniors who reported emotional abuse reported that they were abused by a partner or ex-partner (78%), their children (26%) or a caregiver (2%).Footnote 295
Financial abuse is broadly defined as the manipulation or exploitation of someone else's money.Footnote 296 According to the 1999 General Social Survey, 1% of seniors reported some sort of financial abuse by a partner, ex-partner, child or caregiver.Footnote 295 Partners and ex-partners were most often responsible for the abuse (61%), followed by children (36%) and caregivers (6%).Footnote 295
Beyond physical impacts, abuse and neglect of seniors can have significant impacts on emotional and social well-being.Footnote 287 Footnote 288 Research shows that both older men and women who are abused have higher rates of depression and anxiety than those who do not experience abuse.Footnote 287 Footnote 288 Resulting depression can, in turn, increase seniors' isolation.Footnote 297 Footnote 298 Abuse and neglect perpetrated by family members or others close to the victim can cause shame, guilt or embarrassment.Footnote 288 Financial abuse of seniors can impact their health and well-being by reducing the resources necessary to maintain good health such as proper nutrition, physical activity, medications and care.Footnote 288 For some seniors who are victims of abuse and neglect, coping with the effects may lead to problems with alcohol or substance abuse.Footnote 288
Some seniors, including women, the frail, and those who have a cognitive impairment or physical disability, are more likely to experience abuse or neglect. Chronic and physical illnesses and disability coupled with dependency and the need for greater care, place seniors at higher risk of abuse and neglect.Footnote 299 Other well-substantiated factors that increase the risk of abuse for older adults include living in a shared residence, social isolation and dementia. Risk factors associated with the abusive person include mental illness, hostility, alcohol misuse and dependency on the older adult. Within Aboriginal communities, shared living arrangements, poverty, low education and unemployment are identified as risk factors for abuse and neglect of seniors.Footnote 300 Footnote 301
Summary
Seniors are living longer lives and most are experiencing good overall health. As life expectancy continues to increase, so too will issues related to physical and mental health and economic and social well-being of Canada's seniors. Although most seniors experience the conditions necessary for healthy outcomes, such as adequate income and strong connections to family and community, the lack or decreased availability of these conditions can lead to poor health and diminished well-being. This chapter has shown that in addition to the positive health experienced by most Canadian seniors, there are many negative influences and outcomes on seniors' health that need to be prevented, addressed, mitigated and/or improved. In some cases it is later-life transitions and challenges that pose a risk, while in other cases multiple influences along the lifecourse have compounded to create current health outcomes and serve as precursors to future health and well-being. Although in many instances prevention can be initiated much earlier in the lifecourse, action taken later in life can also be preventative, serve to delay the onset of some conditions or lessen the severity of existing health concerns. A discussion of approaches and interventions to address some of the key challenges facing the health of seniors and to provide the conditions necessary for healthy aging will be presented in the following chapter.
Page details
- Date modified: