Report summary: A Vision to Transform Canada's Public Health System
Chief Public Health Officer's Report on the State of Public Health in Canada 2021
Download in PDF format
(984 kb, 12 pages)
Organization: Public Health Agency of Canada
Date published: 2022-04-01
On this page
Executive summary
The COVID-19 pandemic has shown us that an effective health system does more than treat illnesses with medicines and procedures. It works to prevent these illnesses from happening in the first place and protects us from health threats, whenever possible. It also promotes healthy environments and public policies that create the conditions to support and enable health. These are the roles of public health.
As the first line of defense against health emergencies, COVID-19 pushed our public health system into overdrive. Canada, like the rest of the world, was not prepared to face a health emergency of this size and scope.
While the pandemic has highlighted the strengths of Canada's public health system, it also exposed age-old challenges. Public health lacks the necessary data, resources, and tools to carry out its critical work. In her 2021 annual report, the Chief Public Health Officer of Canada (CPHO), Dr. Theresa Tam, reflects on Canada's experience with COVID-19 and offers a blueprint for a stronger and more prepared public health system.
Moving forward, our public health system must be better equipped to deal with new and ongoing challenges to our collective health. We are already dealing with the effects of climate change, through extreme weather events, air pollution, and emerging infectious diseases. At the same time, other pressing public health issues are worsening, like the opioid overdose crisis, declining mental health, and growing bacterial resistance to antibiotics.
A strengthened public health system must also work with other sectors to address the broader social, economic, and ecological circumstances that influence whether people can reach their full health potential. As we are seeing with COVID-19, communities that experience unfair disadvantages in relation to housing, education, income, employment, food security, and other daily living conditions, also experience worse health outcomes.
In her report, the CPHO presents 4 priority action areas for public health transformation, to help ensure we are better equipped to meet present and future health challenges:
Support and reinvigorate the public health workforce
We must work to recruit and retain the next generation of public health professionals and continue to build a workforce that is highly skilled, inclusive, and reflective of the communities it serves. We also need to increase the capacity of the public health workforce, so it can quickly expand in times of emergency.
Upgrade the public health toolbox
Public health professionals need to have the right information and tools to do their work in a timely way. To get there, we have to address long-standing gaps in data and surveillance systems. We must also prioritize First Nations, Inuit, and Métis ownership of data and ensure greater transparency in our data systems.
Modernize how we collaborate and govern public health
We cannot continue to treat the health sector in isolation from the other sectors, like education, housing, business, and the environmental sector, that have an impact on our health. This requires us to take a "whole of society" approach and consistently work together across sectors, jurisdictions, industries, communities, and borders. We also need clear ways of knowing whether we are achieving better health for populations. We must explore new ways to empower and engage communities in public health decision-making, including supporting First Nations, Inuit, and Métis communities in developing and leading their own public health priorities, plans, and solutions.
Step up investments in public health
Public health resources are often scaled back after health emergencies. This puts public health systems at a disadvantage in the face of future, as well as ongoing, health challenges. Appropriate and stable financing is critical for allowing public health systems across Canada to carry out their everyday work while also making much-needed upgrades to their workforces, tools, and capabilities. Federal funding can help realize common priorities across all jurisdictions.
COVID-19 has served as a wake-up call. We know that the best defense against the next emergency includes a strong public health system and a healthy population. To get there, we need to value public health as much as we do health care. This means a societal shift in how we view our health system, from primarily treating illnesses towards preventing disease and promoting health for all.
Report overview
Building on the 2020 Chief Public Health Officer of Canada (CPHO) report, From Risk to Resilience: An Equity Approach to COVID-19, the 2021 CPHO annual report begins with an overview of the health impacts of COVID-19 on people living in Canada, setting the stage for why now is the time to strengthen the public health system in Canada.
The report is organized into 4 sections. Section 1 reviews the key COVID-19 events that took place between August 2020 and August 2021. Section 2 describes public health and its unique role and impact on the health of people in Canada. It sets out the building blocks of a public health system as a frame to consider opportunities for system-wide improvements. Section 3 builds on these opportunities and outlines aspirational elements for our public health system. The final section proposes some immediate steps by priority area for achieving a more resilient public health system.
The report draws from a range of evidence sources, including the valuable input of public health leaders, researchers, community experts, intersectoral collaborators, and First Nations, Inuit, and Métis leaders.
Section 1. COVID-19 in Canada and the world
The COVID-19 pandemic remains one of the most significant public health crises in recent memory. As of August 31, 2021, there were about 1,500,000 reported COVID-19 cases and close to 27,000 COVID-19-related deaths in Canada. Different "waves" have characterized the ebbs and flows of the pandemic since the beginning.
Key characteristics of each wave of the pandemic
- 1st wave (January 2020 to August 2020): Long-term care homes were the hardest hit. By the summer of 2020, stringent public health measures brought disease activity to low levels.
- 2nd wave (August 2020 to February 2021): There were increases in community spread, impacting areas and populations less significantly affected in the first wave (e.g., the Territories, the Prairie provinces, some Indigenous communities).
- 3rd wave (February 2021 to August 2021): A rise of highly transmissible variants of concern, combined with easing of public health measures, fueled a large wave. Overall mortality rates decreased with higher vaccination coverage among older Canadians. There was higher transmission among younger age groups.
- 4th wave (began August 2021): The 4th wave was driven by the highly transmissible Delta variant and incomplete vaccine coverage, coinciding with many regions entering their final phases of reopening.
COVID-19 inequities
We know that the burden of COVID-19 affected some communities more than others. For example, some racialized populations, Indigenous Peoples, and lower-income groups were more likely to be exposed to the virus due to the circumstances of their lives, such as crowded housing or an inability to work from home. Individuals in these groups were also more likely to be hospitalized or die if they tested positive for the virus. This relates to social and economic inequities that predated the pandemic, including barriers to accessing health care and a higher likelihood of having chronic conditions.
Broader health and social consequences of the COVID-19 pandemic
The COVID-19 pandemic has affected, and continues to affect, many aspects of health in Canada. This includes estimates of life expectancy, which will likely decline because of COVID-19 deaths. It also includes worsening mental health and a growing opioid overdose crisis. Health resources diverted away from other priorities to address the pandemic, for example, resulted in surgery and diagnostic procedure backlogs. The pandemic also affected the broader circumstances that influence people's health, such as employment conditions, financial stability, food insecurity, social connection, and government policies.
Future public health emergencies require a stronger public health system
This pandemic has brought extraordinary challenges to Canada's public health system. These have included delays or gaps in data and other necessary information, mis- and disinformation, rapidly evolving evidence, increased demands for personal protective equipment, and public health workforce burnout. We found short-term solutions for many of these challenges. It is clear, however, that we need lasting solutions so public health systems can continue to tackle the COVID-19 pandemic, address other pressing public health priorities, and prepare for future health emergencies.
The next section lays the groundwork for opportunities to strengthen the broader public health system in Canada by first outlining how this system works and how it touches people's lives every day.
Section 2. Public health in Canada: opportunities for transformation
The COVID-19 pandemic has brought the world's attention to public health, revealing its essential, but often invisible, role in a nation's well-being. Emergency preparedness and response is one of the essential functions of public health; however, this is only one of the ways public health promotes and protects the health of populations.
What is public health
Public health is the part of the health system that focuses on promoting health and preventing disease, illness, and injury. It can protect healthcare systems by reducing the need for medical treatments, and helping people to stay healthy and well. The results of public health efforts can be seen in outbreaks that did not happen, traumatic injuries that did not occur, and drug overdoses that were avoided.
While the healthcare system treats individual patients, public health's patient is the population. In this way, the patient can be a community of people that share an identity, neighbourhood, region, or, as was clear with COVID-19, a country or the collective global community.
In taking a "big picture" approach to health, public health focuses on persistent challenges faced by many people. This includes the broader circumstances of people's lives, such as shelter, income, food, and the ecosystem, that impact how healthy they can be and possibly lead to unfair differences among groups. Immediate pressing challenges for public health continue to be the COVID-19 pandemic, the opioid overdose crisis, declining mental health, the health impacts of climate change, and antimicrobial resistance.
The contributions of public health are vast, including vaccines, safe living and working conditions, health promotion, and infectious disease control. In the 20th century alone, scientists estimated that advances in public health increased the average life expectancy at birth in Canada by 25 years (see text box: Contributions of Public Health).
Contributions of public health
- Advancements in maternal and infant health
- Improvements to water safety and sanitation
- Fluoridation of drinking water for oral health
- Tobacco control
- Occupational safety
- Motor vehicle safety
- Declines in deaths from cardiovascular disease and strokes
- Infectious disease control and prevention
- Safer and healthier foods
However, despite these successes, it is important to acknowledge that current public health systems in Canada are rooted in colonial policies and practices that profoundly affect the health and well-being of many, including First Nations, Inuit, and Métis Peoples. To address these longstanding issues, public health systems across Canada are working to acknowledge and understand this history, and commit to truth, justice, and reconciliation. This involves working with Indigenous leaders and communities towards self-determination.
Public health systems in Canada
Although public health has become more visible during the COVID-19 pandemic, much of the work is behind the scenes, done by many organizations, groups, communities, and sectors (Figure 1). To serve everyone in Canada, public health mandates span federal, provincial, territorial, local, and Indigenous systems. These make up Canada's "public health system of systems", which itself is part of the country's larger federated health system.
Government ministries, public health agencies, and public health departments form the hub of public health systems, fulfilling important leadership and coordination roles. They also motivate and support other sectors outside of health to consider and act on issues that are important to the health and well-being of populations.
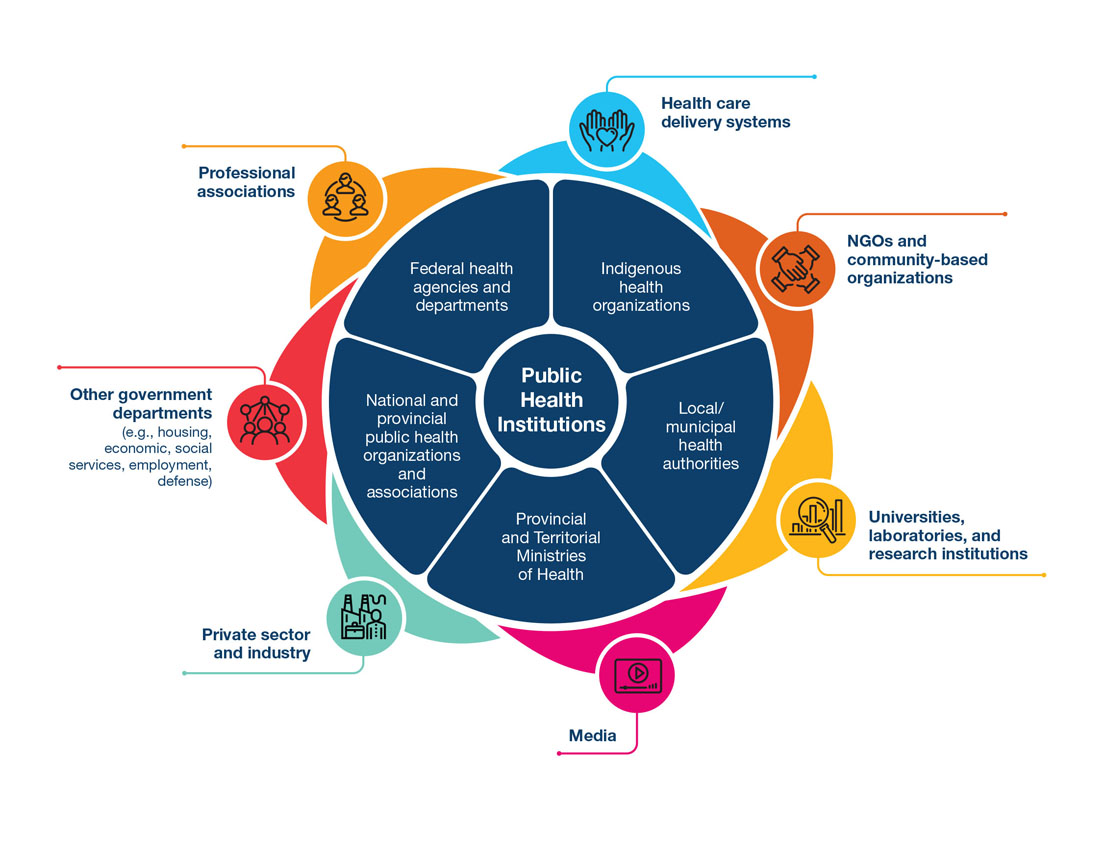
Figure 1: Text equivalent
The figure describes organizations in the public health system.
A circle in the centre of the image describes public health institutions, which have roles and responsibilities for public health and are able to legislate public health policies. These organizations are:
- Indigenous health organizations,
- Local/municipal health authorities,
- Provincial and Territorial Ministries of Health,
- National and provincial public health organizations and institutions; and,
- Federal agencies and departments.
Surrounding this circle are institutions and organizations that do not have a public health mandate, but work closely with the public health system. These organizations are:
- Professional associations,
- Healthcare delivery systems,
- NGOs and community-based organizations,
- Universities, laboratories, and research institutions,
- Media,
- Private sector and industry; and,
- Other government departments (e.g., housing, economic, social services, employment, defense).
The overarching purpose of the public health system is to work toward optimal health and well-being for all people in Canada (Figure 2). The public health system aims to protect and enhance the health of populations while achieving equitable health outcomes.
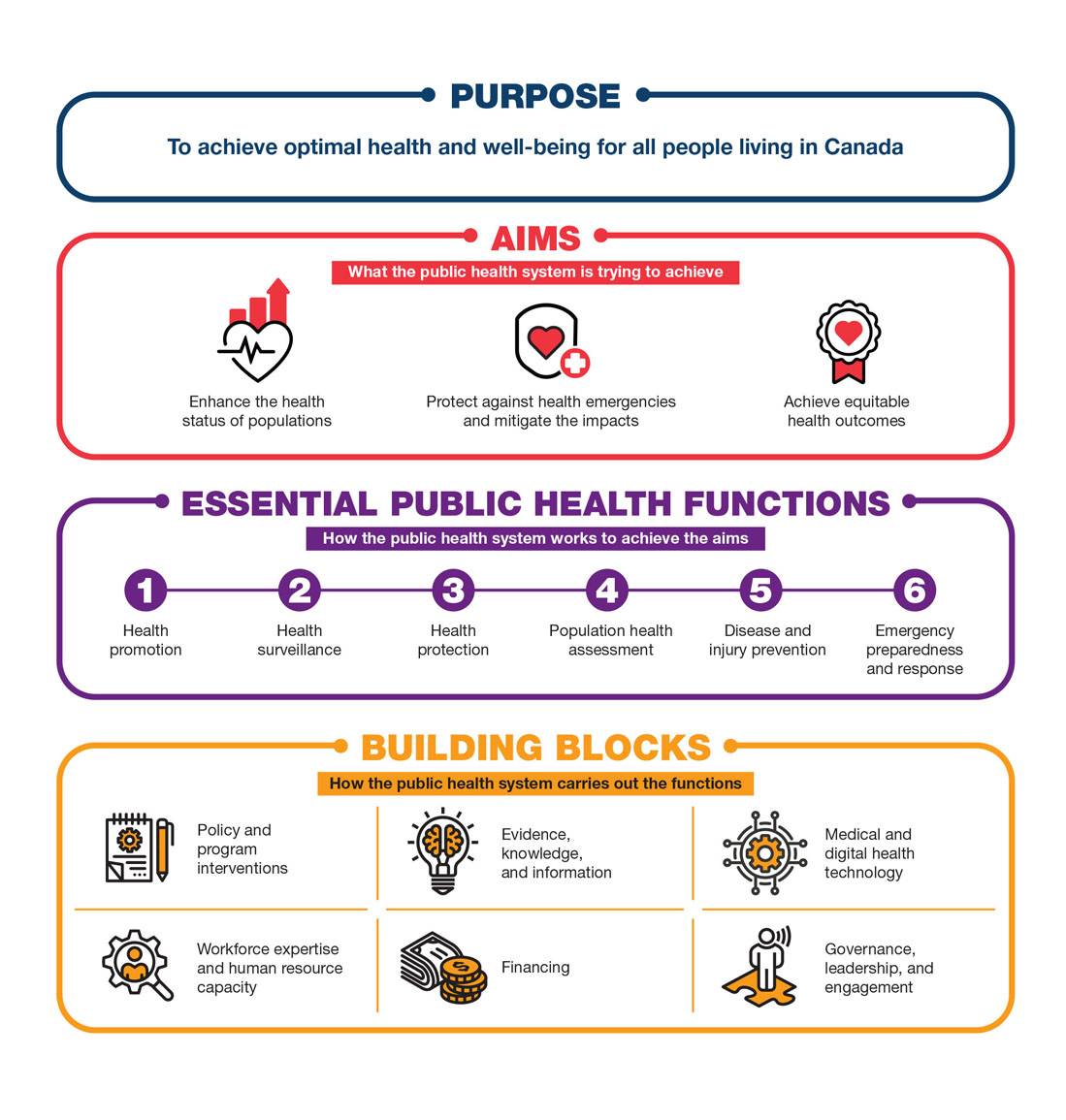
Figure 2: Text equivalent
This figure describes the purpose, aims, functions, and building blocks of public health systems in Canada. The figure works from top to bottom and describes the following components:
Purpose: to achieve optimal health and well-being for all people living in Canada.
Aims (what the public health system is trying to achieve): (1) enhance the health status of populations; (2) protect against health emergencies and mitigate the impacts; and (3) achieve equitable outcomes.
Essential public health functions (how the public health system works to achieve the aims): (1) health promotion; (2) health surveillance; (3) health protection; (4) population health assessment; (5) disease and injury prevention; and, (6) emergency preparedness and response.
Building blocks (how the public health system carries out the functions): (1) policy and program interventions; (2) evidence, knowledge, and information; (3) medical and digital health technology; (4) workforce expertise and human resource capacity; (5) financing; and (6) governance, leadership, and engagement.
Six essential functions drive action in public health (Table 1). During the COVID-19 pandemic, public health systems activated these functions simultaneously.
| Function | Description | Example from the COVID-19 pandemic |
|---|---|---|
| Health promotion | Working collaboratively with communities and other sectors to understand and improve health; this is done through healthy public policies, community-based interventions, public participation, and advocacy or action on the underlying circumstances that shape health (e.g., determinants of health such as housing, income, systemic racism) | Health promotion efforts informed and developed policies, programs, and interventions that worked across sectors to promote mental health, food security, and economic stability |
| Health surveillance | Collecting health data to track diseases, the health status of populations, the determinants of health, and differences among populations | Health surveillance efforts first detected the disease and led to technologies to identify SARS-CoV-2, and data systems to track the spread of the virus |
| Health protection | Protecting populations from infectious disease, environmental threats, and unsafe water, air, and food | Health protection functions focused on implementing public health measures to slow the spread of the virus |
| Population health assessment | Assessing the changing strengths, vulnerabilities, and needs of communities | Population health assessment supported the quick mobilization of research on ways to prevent infection and reduce the spread of the SARS CoV-2 virus |
| Disease prevention | Supporting safe and healthy lifestyles to prevent illness and injury, and reducing risk of infectious disease outbreaks through investigation and preventive measures | Disease prevention efforts included vaccination campaigns alongside interventions to reduce the immediate impact of other health concerns made worse by COVID-19, such as substance use harms |
| Emergency preparedness and response | Planning for, and taking action on, natural or human-made disasters to minimize serious illness, injury, or death | Emergency preparedness and response included coordinating activities across the country, securing vaccine supplies, and creating public health guidance and communication tools |
Moving to the interrelated building blocks of public health systems in Figure 2, these help us understand how public health systems are organized, enabling public health professionals to carry out these functions.
The first 3 blocks (i.e., Policy and program interventions, Evidence knowledge and information, and Medical and digital health technology) are the tools that public health professionals use to understand and tackle population health issues.
The final 3 building blocks (i.e., Workforce expertise and human resource capacity, Financing, and Governance, leadership and engagement) form the foundation, shaping the ability of public health to meet its mandate.
Section 3. A vision to transform public health in Canada
A world-class health system is one that is equipped and supported to achieve its purpose of working toward optimal health and well-being for everyone. Figure 3 illustrates the elements needed for such a system.
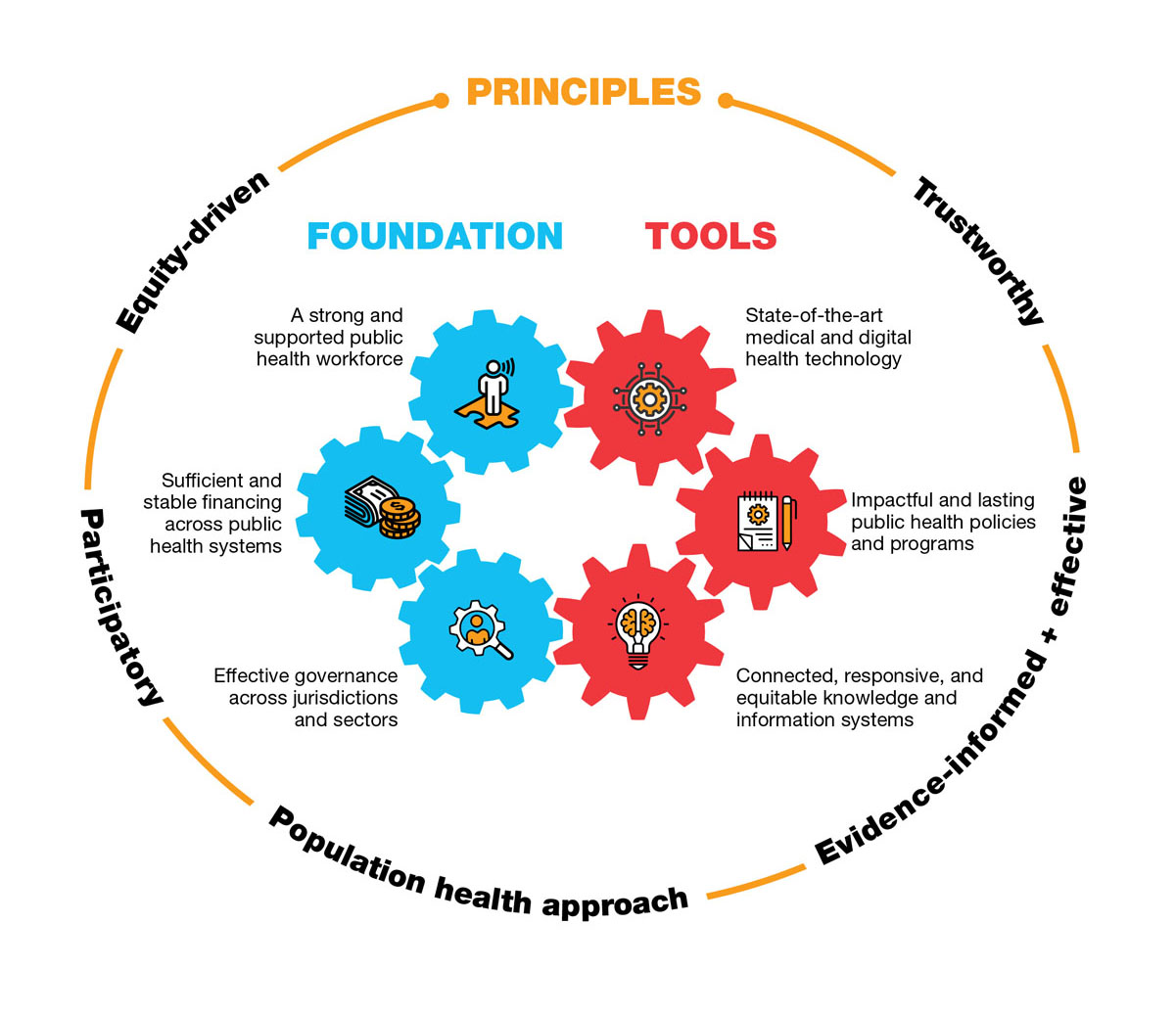
Figure 3: Text equivalent
The figure describes the elements needed for a world-class public health system to achieve optimal health and well-being for all people living in Canada.
The elements of a world-class public health system are displayed in 3 categories.
- Foundation of the public health system, displayed as interconnected gears:
- A strong a supported public health workforce;
- Sufficient and stable financing across public health systems; and,
- Effective governance across jurisdictions and sectors.
- Tools of the public health system, displayed as interconnected gears:
- State of the art medical and digital health technology;
- Impactful lasting public health policies and programs; and,
- Connected, responsive, and equitable knowledge and information systems.
- Principles:
- Surrounding the foundation and tools in a circle are principles of the public health system: trustworthy, evidence informed and effective, population health approach, participatory, and equity driven.
The principles show the overarching values that drive the work of public health systems. They can help steer the collective efforts of people, organizations, and institutions as they move through and achieve transformation. The cogs represent the building blocks, which are now outcome-oriented and form the basis of a strong and well-equipped public health system. Like the inner cogs in a machine, they need to work together for full impact.
Although not exhaustive, these elements represent important entry points for system-wide conversations about public health transformation in Canada. Many of these ideas are not new, and have been called for at different points in our history. However, using these as a guide for the kind of public health system we want now can lead to a true culture shift, one that brings public health into focus and elevates health and well-being to a fundamental priority for people living in Canada.
The way forward
Transformation will take sustained commitment and investment. It will also require public health to embrace a culture of continuous learning, be on the cutting-edge of innovation, and build strong bridges between communities, governments and other partners, and across all public health systems in the country.
Below is a summary of shorter-term actions to spark and encourage bigger and on-going discussions across Canada about a stronger, more resilient public health system (see the report for the full list of actions). These actions are aimed at enhancing excellence in the public health workforce, improving and sharpening the tools at public health's disposal, modernizing public health governance and collaboration structures, and ensuring stable and consistent funding.
Foster excellence in the public health workforce
The pandemic had a tremendous impact on the public health workforce across Canada, taking a toll on those who have been working day and night for nearly 2 years, with frequent reports of burnout. At the same time, it has also sparked increased interest in the field of public health. It is urgent that we build capacity and invest in the current and future public health workforce so it can meet unforeseen needs in times of emergency. We must work to recruit, retain, and build a highly skilled, diverse, and inclusive workforce that best reflects the communities it serves.
Improve public health tools
There are gaps in public health surveillance and data systems, including a lack of data on race and ethnicity, a lack of comparable data between provinces and territories, and information gaps at the local level. These gaps hindered, in part, the response to COVID-19. Our public health system and workforce need the right tools, at the right time, for effective decision-making - including better data, evidence, and insights.
Working across federal, provincial, and territorial governments, we must fast track the ongoing Pan-Canadian Health Data Strategy to address these gaps in a secure and ethical manner, including honouring principles of data governance for First Nations, Inuit, and Métis Peoples. We must also develop stronger research partnerships that can get evidence into public health practice quicker. New research and knowledge should focus on identifying the interventions and models that are most effective for improving the health of populations and reducing health inequities between populations.
Modernize public health governance and collaboration structures
Complex public health challenges require a "whole-of-society" approach. The pandemic has confirmed that we cannot work in siloes; rather, we must work together across jurisdictions, sectors, communities, and borders to address public health crises and the circumstances that shape health. This means making space for, and actively supporting, self-determination in public health for First Nations, Inuit, and Métis Peoples, and empowering communities to shape public health priorities and co-design solutions.
We must support these efforts by finding new ways to collaborate and having clear and transparent ways to measure whether we are meeting our goals.
Ensure stable and consistent funding
Public health faces "boom and bust" funding cycles that leave us ill prepared for new emergencies. As we have seen in the past, public health resources are often scaled back after health emergencies as governments move to address other priorities. This places public health systems at a disadvantage at the onset of each crisis since the capacity and networks required for a rapid response are not there. We need to invest in public health up front and consistently. This investment will be cost saving and provide many long-term social and economic benefits. Federal funding could support common public health priorities across systems along with a "public health report card" to show the impact of these investments.
We have seen during the pandemic that when we work together we can achieve what just a few years ago may have seemed impossible. We all deserve to have good health, and improving our collective health and well-being is everyone's responsibility. Transforming our public health system requires that we all work together and learn from one another across communities, governments, sectors, and internationally. Indeed, the most important lesson from the COVID-19 pandemic is that we can rise to the challenge. Lasting solutions are possible and within our reach.
