Summary of Assessment of Public Health Risk to Canada Associated with Middle East Respiratory Syndrome Coronavirus (MERS-CoV)
The risk assessment is reviewed on a regular basis and updated as required.
Updated: 22 November 2018
What's New?
- The event summary, epidemiologic curve and spatial distribution map have been updated to reflect cases reported since the last update (July 13, 2017): 227 new cases have been reported, with 137 cases between January 1 and October 30, 2018
- The Summary of Literature has been revised to include newly published literature on the detection of MERS-CoV in alpacas, variation in epidemiologic profiles between outbreak and non-outbreak MERS cases and new evidence for the effectiveness of infection, prevention and control (IPC) measures
- Additional information on sources of both zoonotic and secondary transmission has been provided
Summary
- The public health risk posed by MERS-CoV to Canada remains low
- To date, no human cases of MERS have been reported in Canada
- As of October 30, 2018, 2266 cases including 804 deaths (case fatality rate [CFR]~35%) have been reported from 27 countries since emergence in 2012, with approximately 80% of cases being reported by the Kingdom of Saudi Arabia
- Infection is associated with exposure to infected dromedary camels and contact with infected individuals, most often in healthcare settings
- The most likely threat to Canadians remains a risk of importation to Canada from travelers infected while in the Middle East.
Risk Assessment
The public health risk posed by MERS-CoV to Canada is considered low based on available information at this time. The risk may change as new information arises.
MERS-CoV is considered a zoonotic virus since transmission of MERS-CoV to humans is thought to be associated with direct or indirect contact with infected dromedary camels or camel-related products. Current evidence suggests that camels are the reservoir host for MERS-CoV and are the animal source of MERS-CoV infection in humans; however, there is also evidence of human-to-human transmission as clusters of MERS have been reported among close contacts and in health care settings. Although no community-wide transmission has been observed, human-to-human transmission has been observed in households in affected countries. Most human cases of MERS-CoV reported to date have resulted from human-to-human transmission in health care settings.
MERS-CoV infections largely exist in the Arabian Peninsula. The most likely threat to Canadians remains a risk of importation to Canada from travelers infected while in the Middle East. No cases of MERS have been reported in Canada.
Event Summary
Since January 2018, the incidence of MERS cases has remained relatively stable with 20 cases or less reported each month. Between January 1 and October 30, 2018, 137 cases of MERS, including 42 deaths (CFR=31%), have been reported (World Health Organization [WHO] Regional Office for the Eastern Mediterranean, 2018a).
The age and sex distribution of cases reported between January 1 and October 30, 2018 has remained relatively consistent compared to previous years: 82% male and median age of 57 years (range 62% to 82% male and 47 to 55 years between 2013 and 2017) (World Health Organization [WHO] Regional Office for the Eastern Mediterranean, 2018a). At the last update, the proportion of cases reporting exposure to a MERS case was 59%, attributable to the nosocomial outbreaks reported in June 2017. Since then, out of cases with reported dromedary exposure history (n=122), the proportion of cases reporting exposure to a dromedary before symptom onset has been 64%.
Geographically, cases of MERS are less dispersed than previous years with only six countries (Saudi Arabia, Malaysia, Oman, United Arab Emirates, United Kingdom of Great Britain and Northern Ireland, and the Republic of Korea) having reported cases to date in 2018 (range 5 to 14 countries between 2013 and 2017).
Globally, since April 2012, 2266 cases of MERS including at least 804 deaths (CFR ~35%) have been reported (Figure 1) (World Health Organization [WHO], 2018b). The highest annual number of cases occurred in 2014 (n=758 cases) (World Health Organization [WHO] Regional Office for the Eastern Mediterranean, 2018b). Since 2014, the number of cases reported annually has declined: from 672 cases reported in 2015 to 250 cases reported in 2017 (World Health Organization [WHO] Regional Office for the Eastern Mediterranean, 2018b). The global case count of MERS is likely to underestimate the true burden of illness as surveillance systems are often unable to capture mild and asymptomatic cases. For the latest updates on cases and deaths please visit the WHO's MERS-CoV website.
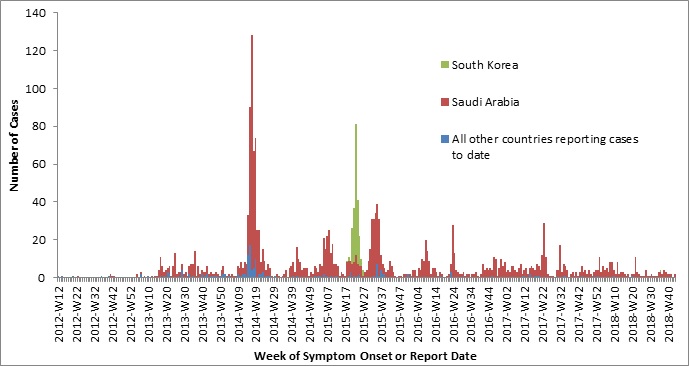
Figure 1 - Text Description
Globally, since April 2012, 2266 cases of MERS including at least 804 deaths (CFR ~35%) have been reported. The highest annual number of cases occurred in 2014 (n=758 cases). Since 2014, the number of cases reported annually has declined: from 672 cases reported in 2015 to 250 cases reported in 2017.
Note: Epidemiological curve was prepared using information compiled by the Public Health Agency of Canada’s Global Public Health Intelligence Network (GPHIN) and the World Health Organization’s Disease Outbreak News (n=2125). This figure excludes 132 cases that were reported by the WHO between 2012-2017 and cases whose week of symptom onset or report date is unreported or under investigation.
Geographically, 27 countries located in North America, Europe, the Middle East, Northern Africa and Asia have reported imported and locally-acquired cases of MERS with the majority, approximately 83%, reported from Saudi Arabia (Figure 2) (World Health Organization [WHO], 2017a). To date, the largest number of cases to be reported outside the Middle East occurred in South Korea in 2015: the majority of the 186 reported cases were associated with a large multi-hospital outbreak (Normile, 2015).
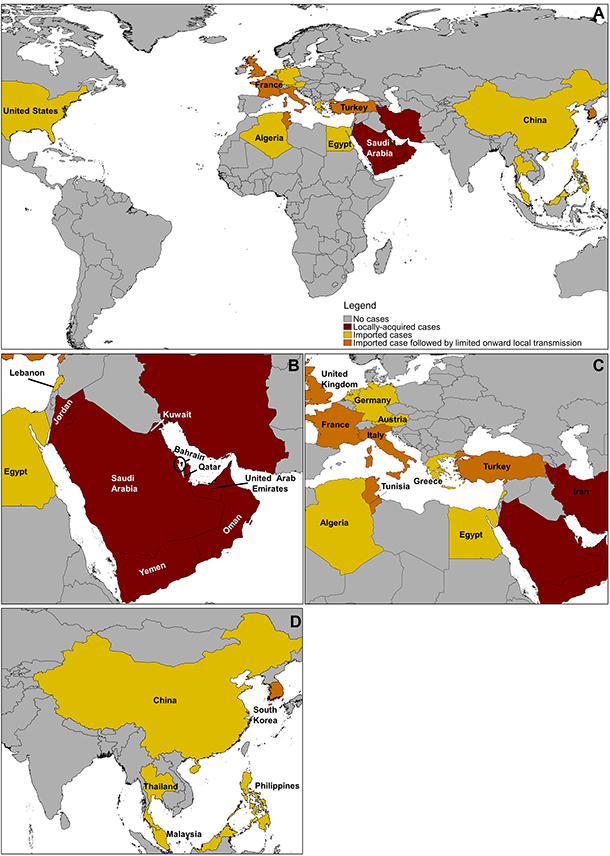
Figure 2 - Text Description
Geographically, 27 countries located in North America, Europe, the Middle East, and Asia have reported imported and locally-acquired cases of MERS with the majority, approximately 80%, reported from Saudi Arabia.
Note: Map was prepared using information compiled by the World Health Organization.
Summary of literature
Middle East Respiratory Syndrome (MERS) is a viral respiratory disease caused by a lineage C Betacoronavirus that emerged in the human population in 2012. Since 2012, the World Health Organization (WHO) has reported 2266 confirmed human cases, including 804 deaths. Epidemiologic patterns of MERS reflect sporadic zoonotic infections with amplified human to human transmission in health care settings. Large outbreaks of MERS have mainly resulted from nosocomial transmission in healthcare facilities due to lapses in infection prevention and control measures. Some of these large outbreaks have led to limited community transmission within households; however, sustained human to human transmission has not been observed.
Human infection with MERS-CoV results in a wide range of clinical presentations from asymptomatic infection to severe acute clinical disease (Fehr, Channappanavar, & Perlman, 2017). Common clinical symptoms include fever, cough and shortness of breath that can progress to severe acute pneumonia, acute respiratory distress syndrome, multi-organ failure and death; however asymptomatic and mild symptomatic cases have also been reported (Arabi Y.M. et al., 2017; Fehr et al., 2017). Severe illness is often seen in elderly patients or individuals with comorbid conditions (Alhamlan et al., 2017).
The temporal distribution of cases is characterized by introductions of primary zoonotic cases followed by increases in secondary cases due to nosocomial outbreaks and lapses in Infection Prevention and Control (IPC). Early analysis of the temporal distribution of MERS cases between 2012 and 2014 suggested a seasonal pattern with cases increasing from March to April each year. At the time, this seasonal pattern had been linked to the calving and weaning patterns of camels; however, this pattern hasn't been consistently observed each year since 2014 (Hemida et al., 2017).
Different age and sex patterns are observed amongst primary and secondary cases. Primary cases (cases with no history of contact with a MERS case) are predominantly seen in older males: the 50 to 59 year age group is at the highest risk for acquiring infection (Gossner et al., 2016; World Health Organization [WHO] Regional Office for the Eastern Mediterranean, 2017b). This observed pattern has been associated with camel rearing being an activity popular among middle-aged and retired men (Gossner et al., 2016). Secondary cases (cases with history of contact with MERS case) are predominantly seen in the younger age group with an equal gender distribution; the 30 to 39 year age group is the most at risk for acquiring infection (Gossner et al., 2016; World Health Organization [WHO] Regional Office for the Eastern Mediterranean, 2017b).
More than 80% of the MERS cases have been reported from the Arabian Peninsula. This geographic distribution has been associated with the high camel density in this area (Gossner et al., 2016; Hemida et al., 2017). Further information on the geographical distribution of MERS-CoV in camels can be found on the FAO website.
Source of Zoonotic Transmission
Research to date suggests that MERS-CoV emerged from bats (Sharif-Yakan & Kanj, 2014). Genomic sequencing and phylogenic analysis from bats in Saudi Arabia and Africa support this theory, with similarities identified between bat coronavirus sequences and MERS-CoV (Ithete et al., 2013; Memish et al., 2013; Wang et al., 2014). Multiple studies on the emergence and transmission of MERS-CoV point to the role of dromedary camels as a reservoir and primary source of zoonotic infection due to (1) the high prevalence of MERS-CoV antibodies in camels across the Arabian Peninsula, North and Eastern Africa, (2) the detection of MERS-CoV by RT-PCR in respiratory secretions, feces, and milk of dromedary camels and (3) similarities in the genomic sequence of viruses isolated from infected individuals and camels (Omrani, Al-Tawfiq, & Memish, 2015). There is evidence to suggest that MERS-CoV has been circulating in camels for more than 20 years (since at least 1992) (Alagaili et al., 2014; Corman et al., 2014). Challenge studies conducted in camels suggest that MERS is a mild respiratory infection resulting in little to no signs of illness in camels (Adney et al., 2014). Based on seroepidemiological studies carried out in other livestock, alpacas are the only other livestock in which MERS-CoV specific antibodies have been identified; however, no human cases with exposure to alpacas have been reported to date (Reusken et al., 2016).
Although the route of camel to human transmission is not fully understood, zoonotic infections of MERS-CoV likely occur through direct or indirect contact with infected camels or camel-related products (e.g. raw milk) (Gossner et al., 2016). The detection of MERS-CoV RNA in camel milk suggests a potential food-borne transmission of the virus by consuming raw milk (Reusken et al., 2014). Epidemiological studies have demonstrated a greater risk of MERS-CoV infection among individuals exposed to camels when compared to the general population (Muller M.A. et al., 2015; World Health Organization [WHO], 2015b). To date, zoonotic transmission has only been reported from countries in the Arabian Peninsula where the virus is highly prevalent and widespread within the camel population. Further studies need to be conducted in order to fully understand the role human-animal interaction play in the transmission of this disease.
Source of Secondary Transmission
Secondary transmission of MERS-CoV has largely been associated with nosocomial outbreaks; however, family clusters have also been reported (Abroug et al., 2014; Memish, Zumla, Al-Hakeem, Al-Rabeeah, & Stephens, 2013). Nosocomial outbreaks of MERS have played a significant role in increasing the magnitude of reported cases. To date, large scale hospital outbreaks have been reported in Saudi Arabia and South Korea. Lack of IPC (e.g., overcrowding, delay in isolation of cases, lack of knowledge of MERS case definitions amongst healthcare workers) along with intra- and inter-hospital transmission, super spreaders, and asymptomatic cases are a few of the factors that have contributed to these hospital outbreaks (Al-Tawfiq & Perl, 2015). Strict adherence to IPC has been shown to result in the rapid identification of cases and a significant reduction in the number of secondary cases in nosocomial outbreaks, and allows for early identification of new cases (El Bushra et al., 2017).
An outbreak in South Korea, which began in May 2015, was the largest nosocomial outbreak of MERS outside the Middle East. This outbreak started from a super spreader who travelled to four countries in the Middle East and who appeared to have transmitted infection to close relatives, patients sharing the same room and health care workers providing care upon return to South Korea (Kim et al., 2017). These exposures happened before MERS-CoV was suspected or diagnosed. The outbreak in the Republic of Korea was declared over on December 23, 2015 (Normile, 2015). The current evidence from contact tracing studies suggests that transmission did not extend beyond close contacts into the community (Memish, Zumla, & Assiri, 2013)
Vaccines against MERS-CoV
No vaccine or effective antiviral treatment is currently available for MERS-CoV. However, research is underway and many candidate vaccines targeted for humans are in development. These candidates use a wide range of platforms including whole virus vaccine (live attenuated and inactivated), vectored-virus vaccines, DNA vaccine, and protein-based vaccines (Okba, Raj, & Haagmans, 2017). Thus far, only one candidate vaccine has advanced to clinical development: a DNA-only vaccine that has been shown to generate protective MERS-CoV antibodies in mice, camels and monkeys advanced to Phase 1 human clinical trials in February 2016 (Modjarrad, 2016).This candidate vaccine has also been tested in dromedary camels. Additionally, a modified vaccinia Ankara based vaccine that reduced virus shedding and generated protective antibodies and mucosal immunity is currently scheduled for a Phase 1 safety trial (Alharbi, 2017).
Virus Characteristics
MERS-CoV is an enveloped and single stranded RNA virus belonging to the Coronaviridae family (Fehr et al., 2017). Though caused by the same genera of coronavirus as severe acute respiratory syndrome (SARS) (Betacoronavirus genera), MERS-CoV belongs to lineage C whereas SARS belongs to lineage B (Arabi Y.M. et al., 2017). Entry of MERS-CoV into host cells is mediated by its spike (S) protein binding to the host cell receptor, dipeptidyl peptidase 4 (DPP4) (Fehr et al., 2017). In the case of SARS, extensive mutations in the virus resulted in its ability to adapt to the human cell receptor angiotensin-converting enzyme 2 [ACE2] which allowed for increased human-to-human transmission (Chinese SARS Molecular Epidemiology Consortium, 2004). Though sequenced viral isolates from camels and humans indicate that MERS-CoV has undergone recombination and genetic changes since its introduction to humans in 2012 (Sabir et al., 2016), none of these changes have resulted in virus mutation allowing for more efficient adaptation to human cell receptor, DPP4. In fact, analysis of viral isolates from the South Korea outbreak with a mutation in the receptor binding domain showed reduced affinity to human DPP4 (Kim et al., 2016). These findings further convolute the role of the S protein and DPP4 in the human adaptation of this virus given the magnitude of the South Korea outbreak.
Recommendations for Canada
Surveillance
Health care professionals are encouraged to maintain vigilance for cases of MERS-CoV infection, and notify the appropriate Public Health Departments of any persons under investigation. The national case definition for MERS-CoV is to be used for the surveillance of MERS-CoV. For guidance on surveillance objectives and activities, please refer to the national surveillance guidelines for MERS-CoV.
Provinces and Territories are asked to report confirmed cases of MERS-CoV infection to the Public Health Agency of Canada using the Emerging Respiratory Pathogens and Severe Acute Respiratory Infection (SARI) Case Report Form.
Laboratory
Laboratory testing should be conducted in accordance with the Canadian Public Health Laboratory Network's Protocol for Microbiological Investigations of Severe Acute Respiratory Infections (SARI). Follow infection prevention and control guidelines when collecting respiratory specimens. Be aware of approaches in your jurisdiction.
Laboratory confirmation is obtained by detection of the virus using (a) MERS-CoV specific nucleic acid amplification test (NAAT) with up to two separate targets and/or sequencing; or (b) virus isolation in tissue cultureFootnote 1; or (c) serology on serum tested in a WHO collaborating center with established testing methods. Initial screening tests specific for MERS-CoV can be performed in select laboratories (i.e. primarily provincial public health laboratories); however, such cases are considered probable pending NML confirmation. Laboratories with specimens that screened positive for MERS-CoV should forward these to their local public health laboratory (PHL) that can facilitate confirmatory testing at the NML.
For more detailed information, refer to the National Surveillance Guidelines for Human Infection with Middle East Respiratory Syndrome Coronavirus (MERS-CoV).
The WHO published interim recommendations for laboratory testing for MERS-CoV. (September 2014).
Travel Health Notice
The Agency releases Travel Health Notices outlining potential risks to Canadian travellers and to the Canadian public, and recommends measures that can be taken to help reduce these risks. Any travel health notices for MERS-CoV are posted on the Government of Canada's website: travel.gc.ca.
Infection Prevention and Control (IPC)
No vaccine or prophylactic therapy is available to prevent MERS-CoV infection. Health care organizations are reminded of the importance of systematic implementation of infection prevention and control (IPC) measures to minimize the risk of exposure to and transmission of microorganisms within health care settings. Health care facilities that may receive patients suspected or confirmed with MERS-CoV infection should take appropriate measures to decrease the risk of transmission of the virus to other patients, health care workers and visitors. Recommendations for IPC measures for patients presenting with suspected or confirmed infection with MERS-CoV in acute care settings are posted on the Agency's website. This guidance is updated as new information becomes available.
As presently there is no vaccine available to prevent MERS-CoV infection, it is recommended that Canadians protect themselves from respiratory illnesses while travelling to the Middle East and South East Asia by washing their hands frequently, avoiding contact with people at risk and touching their eyes and nose with unwashed hands, and disinfecting frequently touched surfaces.
Biosafety
MERS-CoV is classified as a Risk Group 3 human pathogen given that this virus can cause serious illness in humans. The public health risk is low since the risk of spread of the virus in the community appears to be low. Containment Level 3 is required for all proliferative work (in vitro in vivo), and non-propagative diagnostic activities can be conducted at Containment Level 2 with the use of additional operational practices as outlined in Biosafety Advisory: Middle East Respiratory Syndrome Coronavirus (MERS-CoV).
References
- Abroug, F., Slim, A., Ouanes-Besbes, L., Hadj Kacem, M. A., Dachraoui, F., Ouanes, I., et al. (2014). Family cluster of Middle East Respiratory Syndrome coronavirus infections, Tunisia, 2013. Emerging Infectious Diseases, 20(9), 1527-1530. doi:10.3201/eid2009.140378 [doi]
- Adney, D. R., van Doremalen, N., Brown, V. R., Bushmaker, T., Scott, D., de Wit, E., et al. (2014). Replication and shedding of MERS-CoV in upper respiratory tract of inoculated dromedary camels. Emerging Infectious Diseases, 20(12), 1999-2005. doi:10.3201/eid2012.141280 [doi]
- Alagaili, A. N., Briese, T., Mishra, N., Kapoor, V., Sameroff, S. C., Burbelo, P. D., et al. (2014). Middle East Respiratory Syndrome coronavirus infection in dromedary camels in Saudi Arabia. MBio, 5(2), e00884-14. doi:10.1128/mBio.00884-14 [doi]
- Alhamlan, F. S., Majumder, M. S., Brownstein, J. S., Hawkins, J., Al-Abdely, H. M., Alzahrani, A., et al. (2017). Case characteristics among Middle East Respiratory Syndrome coronavirus outbreak and non-outbreak cases in Saudi Arabia from 2012 to 2015. BMJ Open, 7(1), e011865-2016-011865. doi:10.1136/bmjopen-2016-011865 [doi]
- Alharbi, N. K. (2017). Vaccines against Middle East Respiratory Syndrome coronavirus for humans and camels. Reviews in Medical Virology, 27(2), 10.1002/rmv.1917. Epub 2016 Oct 27. doi:10.1002/rmv.1917 [doi]
- Al-Tawfiq, J. A., & Perl, T. M. (2015). Middle East Respiratory Syndrome coronavirus in healthcare settings. Current Opinion in Infectious Diseases, 28(4), 392-396. doi:10.1097/QCO.0000000000000178 [doi]
- Arabi Y.M., Balkhy H.H., Hayden F.G., Bouchama A., Luke T., Baillie J.K., et al. (2017). Middle East Respiratory Syndrome. New England Journal of Medicine, 376(6), 584-594.
- Chinese SARS Molecular Epidemiology Consortium. (2004). Molecular evolution of the SARS coronavirus during the course of the SARS epidemic in China. Science (New York, N.Y.), 303(5664), 1666-1669. doi:10.1126/science.1092002 [doi]
- Corman, V. M., Jores, J., Meyer, B., Younan, M., Liljander, A., Said, M. Y., et al. (2014). Antibodies against MERS coronavirus in dromedary camels, Kenya, 1992-2013. Emerging Infectious Diseases, 20(8), 1319-1322.
- El Bushra, H. E., Al Arbash, H. A., Mohammed, M., Abdalla, O., Abdallah, M. N., Al-Mayahi, Z. K., et al. (2017). Outcome of strict implementation of infection prevention control measures during an outbreak of Middle East Respiratory Syndrome. American Journal of Infection Control, 45(5), 502-507. doi:S0196-6553(17)30003-2 [pii] Fehr, A. R., Channappanavar, R., & Perlman, S. (2017). Middle East Respiratory Syndrome: Emergence of a pathogenic human coronavirus. Annual Review of Medicine, 68, 387-399. doi:10.1146/annurev-med-051215-031152 [doi]
- Gossner, C., Danielson, N., Gervelmeyer, A., Berthe, F., Faye, B., Kaasik Aaslav, K., et al. (2016). Human-dromedary camel interactions and the risk of acquiring zoonotic Middle East Respiratory Syndrome coronavirus infection. Zoonoses and Public Health, 63(1), 1-9. doi:10.1111/zph.12171 [doi]
- Hemida, M. G., Elmoslemany, A., Al-Hizab, F., Alnaeem, A., Almathen, F., Faye, B., et al. (2017). Dromedary camels and the transmission of Middle East Respiratory Syndrome coronavirus (MERS-CoV). Transboundary and Emerging Diseases, 64(2), 344-353. doi:10.1111/tbed.12401 [doi]
- Ithete, N. L., Stoffberg, S., Corman, V. M., Cottontail, V. M., Richards, L. R., Schoeman, M. C., et al. (2013). Close relative of human Middle East Respiratory Syndrome coronavirus in bat, South Africa. Emerging Infectious Diseases, 19(10), 1697-1699. doi:10.3201/eid1910.130946 [doi]
- Kim,K.H., Tandi, T.E., Choi, J.W., Moon, J.M., & M.S. Kim (2017). Middle East respiratory syndrome coronavirus (MERS-CoV) outbreak in South Korea, 2015: epidemiology, characteristics and public health implications. Journal of Hospital Infection, 95:207-213. doi:10.1016/j.jhin.2016.10.008 [doi]
- Kim, Y., Cheon, S., Min, C. K., Sohn, K. M., Kang, Y. J., Cha, Y. J., et al. (2016). Spread of mutant Middle East Respiratory Syndrome coronavirus with reduced affinity to human CD26 during the South Korean outbreak. MBio, 7(2), e00019-16. doi:10.1128/mBio.00019-16 [doi]
- Memish, Z. A., Mishra, N., Olival, K. J., Fagbo, S. F., Kapoor, V., Epstein, J. H., et al. (2013). Middle East Respiratory Syndrome coronavirus in bats, Saudi Arabia. Emerging Infectious Diseases, 19(11), 1819-1823. doi:10.3201/eid1911.131172 [doi]
- Memish, Z. A., Zumla, A. I., Al-Hakeem, R. F., Al-Rabeeah, A. A., & Stephens, G. M. (2013). Family cluster of Middle East Respiratory Syndrome coronavirus infections. The New England Journal of Medicine, 368(26), 2487-2494. doi:10.1056/NEJMoa1303729 [doi]
- Memish, Z.A., Zumla, Al., Assiri, A. (2013). Middle East respiratory syndrome coronavirus infections in health care workers. The New England Journal of Medicine, 369(9): 884-886. doi: 10.1056/NEJMc1308698
- Modjarrad, K. (2016). MERS-CoV vaccine candidates in development: The current landscape. Vaccine, 34(26), 2982-2987. doi:10.1016/j.vaccine.2016.03.104 [doi]
- Muller M.A., Meyer B., Corman V.M., AlMasri M., Turkestani A., Ritz D., et al. (2015). Presence of Middle East Respiratory Syndrome coronavirus antibodies in saudi arabia: A nationwide, cross-sectional, serological study. The Lancet Infectious Diseases, 15(5), 559-564.
- Normile, D. (2015, December 23 2015). South Korea finally MERS-free.Science Magazine,
- Okba, N. M., Raj, V. S., & Haagmans, B. L. (2017). Middle East Respiratory Syndrome coronavirus vaccines: Current status and novel approaches. Current Opinion in Virology, 23, 49-58. doi:S1879-6257(16)30148-1 [pii]
- Omrani, A. S., Al-Tawfiq, J. A., & Memish, Z. A. (2015). Middle East Respiratory Syndrome coronavirus (MERS-CoV): Animal to human interaction. Pathogens and Global Health, 109(8), 354-362. doi:10.1080/20477724.2015.1122852 [doi]
- Reusken, C.B., Farag, E.A., Jonges, M., Godeke, G.J., El-Sayed, A.M., Pas, S.D., et al. (2014). Middle East respiratory syndrome coronavirus (MERS-CoV) RNA and neutralising antibodies in milk collected according to local customs from dromedary camels, Qatar, April 2014. Eurosurveillance, 19(23)
- Reusken, C. B., Schilp, C., Raj, V. S., De Bruin, E., Kohl, R. H., Farag, E. A., et al. (2016). MERS-CoV infection of alpaca in a region where MERS-CoV is endemic. Emerging Infectious Diseases, 22(6), 1129-1131. doi:10.3201/eid2206.152113 [doi]
- Sabir, J. S., Lam, T. T., Ahmed, M. M., Li, L., Shen, Y., Abo-Aba, S. E., et al. (2016). Co-circulation of three camel coronavirus species and recombination of MERS-CoVs in saudi arabia. Science (New York, N.Y.), 351(6268), 81-84. doi:10.1126/science.aac8608 [doi]
- Sharif-Yakan, A., & Kanj, S. S. (2014). Emergence of MERS-CoV in the Middle East: Origins, transmission, treatment, and perspectives. PLoS pathogens, PLoS, 10(12)
- Wang, Q., Qi, J., Yuan, Y., Xuan, Y., Han, P., Wan, Y., et al. (2014). Bat origins of MERS-CoV supported by bat coronavirus HKU4 usage of human receptor CD26. Cell Host & Microbe, 16(3), 328-337. doi:10.1016/j.chom.2014.08.009 [doi]
- World Health Organization [WHO]. (2015a). Media centre: WHO statement on the tenth meeting of the IHR emergency committee regarding MERS. Retrieved April 1, 2017, from http://www.who.int/mediacentre/news/statements/2015/ihr-emergency-committee-mers/en/
- World Health Organization [WHO]. (2015b). Summary of current situation, literature update and risk assessment: July 7, 2015. Retrieved April 25, 2017, from http://apps.who.int/iris/bitstream/10665/179184/2/WHO_MERS_RA_15.1_eng.pdf?ua=1
- World Health Organization [WHO]. (2018a). Coronavirus infections: Disease outbreak news. Retrieved November 22, 2018, from http://www.who.int/csr/don/archive/disease/coronavirus_infections/en/
- World Health Organization [WHO]. (2018b). Middle East Respiratory Syndrome coronavirus (MERS-CoV). Retrieved November 15, 2018, from http://www.who.int/emergencies/mers-cov/en/
- World Health Organization [WHO] Regional Office for the Eastern Mediterranean. (2018a). MERS situation update, October 2018. Retrieved November 15, 2018, from http://www.emro.who.int/health-topics/mers-cov/news.html
- World Health Organization [WHO] Regional Office for the Eastern Mediterranean. (2017b). MERS situation update, january-february 2017. Retrieved May 15, 2017, from http://www.emro.who.int/health-topics/mers-cov/news.html