ARCHIVED - Bacterial Meningitis In Canada: Hospitalizations (1994-2001)
Introduction
Bacterial meningitis remains an important public health issue, despite the availability of safe and effective vaccines against many of the common pathogens causing bacterial meningitis, including Neiserria meningitidis, Streptococcus pneumoniae,and Haemophilus influenzae type B infection (Hib). Since their introduction in the early 1990s, universal Hib vaccination programs have dramatically reduced the incidence of Hib meningitis and have caused a shift in the pathogens responsible for bacterial meningitis Footnote 1-3. In Canada, the incidence of bacterial meningitis is unknown. Although several pathogens responsible for causing bacterial meningitis are nationally notifiable, these pathogens cause other forms of invasive disease (e.g. septicemia); thus, pathogen-specific rates do not reflect meningitis rates. In addition, there are organisms that cause bacterial meningitis that are not notifiable. Because therapy for bacterial meningitis is often initiated prior to confirming an etiologic agent, knowing the relative importance of the pathogens that cause meningitis is valuable. This has implications for both public health policy and clinical management. We conducted this study to determine rates for bacterial meningitis in Canada, including pathogen- and age-specific rates.
Methods
A 7-year retrospective census of all hospitalized bacterial meningitis cases in Canada was conducted using the Canadian Institute for Health Information's (CIHI) Hospital Morbidity Database (HMDB) for the fiscal years 1 April, 1994 through 31 March, 2001. The HMDB contains standard data collected from patients' charts at discharge. All Canadian acute care hospitals were included. A case was defined as a hospital separation record with a diagnosis of bacterial meningitis (ICD9 codes 320.0 through 320.9, inclusive, 036.0, and 027.0). Hospital separations with meningitis unspecified (ICD codes 321 and 322) were excluded from this study to minimize misclassification; they may have been non-bacterial in origin.
Data elements extracted for each hospitalization included the following: principal diagnosis, associated diagnoses (up to 16 recorded), dates of admission and separation, discharge condition, length of stay, as well as age in years, sex, and province or territory of residence. Information on outpatient services in any hospital or services in psychiatric hospitals, as well as information on persons who died prior to hospitalization, are not included in the HMDB and therefore are not included in the study population.
Population estimates from Statistics Canada were used to calculate ratesFootnote 4. Data were analyzed using Epi Info version 6.04d. Differences in the average length of stay among patients according to the year of discharge, type of bacterial meningitis, and age were tested for significance using parametric or non-parametric tests (t-test, analysis of variance [ANOVA], or Kruskall-Wallis).
Results
Incidence
Over the 7-year study period, a total of 7,227 bacterial meningitis hospitalizations were identified. The number of annual hospitalizations varied from 1,072 to 940 (Table 1). Annual incidence of bacterial meningitis ranged from 3.66 to 3.37 per 100,000 population. No significant changes in overall incidence occurred over time.
| Year | |||||||
|---|---|---|---|---|---|---|---|
| 1994- 1995 |
1995- 1996 |
1996- 1997 |
1997- 1998 |
1998- 1999 |
1999- 2000 |
2000- 2001 |
|
| Number of cases | 1,063 | 1,064 | 940 | 1,072 | 1,019 | 1,030 | 1,039 |
| Incidence per 100,000 | 3.66 | 3.62 | 3.17 | 3.57 | 3.37 | 3.38 | 3.37 |
| Number of deaths | 115 | 126 | 98 | 121 | 117 | 119 | 117 |
| Case Fatality Ratio | 10.8% | 11.8% | 10.4% | 11.3% | 11.5% | 11.6% | 11.3% |
| Age (years) | |||||||
| Range | 0-95 | 0-94 | 0-90 | 0-96 | 0-92 | 0-92 | 0-97 |
| Median | 17.0 | 25.5 | 19.0 | 27.0 | 28.0 | 28.0 | 33.0 |
Unspecified bacterium accounted for the largest proportion (37%) of bacterial meningitis cases throughout the study period (Figure 1). Pneumococcal, streptococcal, and staphylococcal were the three most commonly identified etiologies, accounting for 49% of cases of bacterial meningitis and 80% of cases wherein an organism was reported.
Figure 1. Etiology of bacterial meningitis in Canada 1994-1995 through 2000-2001
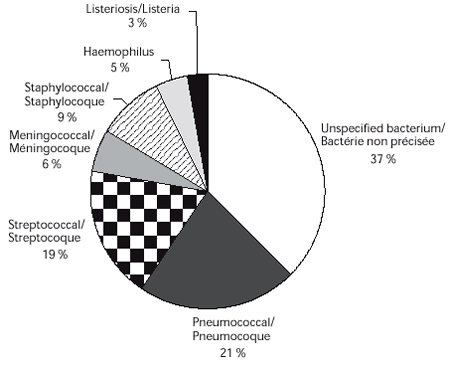
Unspecified bacterium had the highest annual rates during the study period (Table 2). Pneumococcal and streptococcal meningitis had the highest organism-specific rates. Downward trends were observed for meningococcal meningitis (p = 0.0002), whereas pneumococcal, streptococcal, Haemophilus and Listeria meningitis rates were relatively stable and demonstrated no significant trend. Only staphylococcal meningitis showed an increase in incidence throughout the study period - though not significant (p = 0.07) - having the third highest incidence by the end of the study. Data about specific strains (i.e. serotypes or serogroups) within a bacterial category were unavailable, making further sub-analyses impossible.
| Disease* | Year | |||||||
|---|---|---|---|---|---|---|---|---|
| 1994- 1995 |
1995- 1996 |
1996- 1997 |
1997- 1998 |
1998- 1999 |
1999- 2000 |
2000- 2001 |
||
| * Four cases of tuberculous meningitis were reported during the study period. | ||||||||
| Unspecified bacterium | 1.24 | 1.37 | 1.18 | 1.39 | 1.37 | 1.24 | 1.24 | |
| Pneumococcal | 0.86 | 0.88 | 0.61 | 0.68 | 0.69 | 0.77 | 0.77 | |
| Streptococcal | 0.66 | 0.57 | 0.66 | 0.71 | 0.60 | 0.60 | 0.63 | |
| Meningococcal | 0.31 | 0.30 | 0.21 | 0.16 | 0.14 | 0.12 | 0.16 | |
| Staphylococcal | 0.29 | 0.22 | 0.27 | 0.34 | 0.35 | 0.34 | 0.36 | |
| Haemophilus | 0.19 | 0.16 | 0.14 | 0.19 | 0.11 | 0.18 | 0.13 | |
| Listeriosis | 0.09 | 0.11 | 0.09 | 0.09 | 0.11 | 0.10 | 0.07 | |
Age
Persons who had bacterial meningitis ranged in age from < 1 year to 97 years; the median age was 25 years. The median age of bacterial meningitis cases varied throughout the study period, increasing from 17 years in 1994 to 33 years in 2000 (p < 0.001). As expected, the various organisms differed in age characteristics. The median age for persons with Haemophilus and streptococcal meningitis was 5 and 6 years, respectively, and below the overall median age. In contrast, Listeria and staphylococcal meningitis, although more common in children, had higher median ages of 62.0 and 43.0 years, respectively.
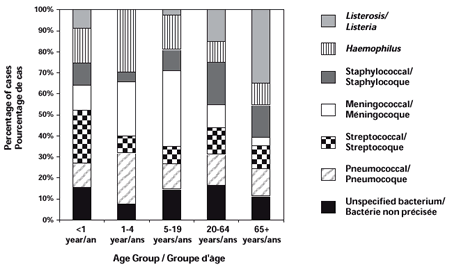
The highest incidence rates were consistently observed among infants aged < 1 year, regardless of the causative agent. Generally, the incidence varied inversely with age, until 10 years when it remained relatively stable throughout adulthood. There was a slight increased incidence in the elderly (aged ≥ 65 years). An increase in incidence was observed for persons aged 25 to 44 years with staphylococcus meningitis. The predominant pathogens associated with meningitis varied according to age (Figure 2).
Case Fatality
The overall bacterial meningitis case fatality ratio (CFR) was 11.3%, with 25% of deaths occurring within 48 hours of hospitalization. The CFR was stable throughout the study period. Regardless of the causative agent, CFR was higher in older adults, and the trend illustrated that CFR increased significantly with age (p < 0.001).
Hospital stay
The overall median length of stay (LOS) for bacterial meningitis was 11 to 12 days and remained stable over the study period. The median LOS varied by organism from 8 to 21 days. Those diagnosed with staphylococcal meningitis had the longest LOS (median of 21 days), while persons with meningococcal meningitis had the shortest at 8 days (p < 0.01).
Discussion
The overall annual rate of bacterial meningitis in Canada remained relatively stable throughout the study period, ranging from 3.17 to 3.66 per 100,000 population per year. Unfortunately, there are limited published data regarding overall bacterial meningitis rates. Published incidence rates for bacterial meningitis in the US and Europe range from 1.7 to 7.2 per 100,000 population and vary over time by country and by age, thus making comparisons difficult Footnote 5-8. In addition, some bacterial meningitis studies limit the analysis to a specified group of pathogens or present rates by organism, rather than overall, again making comparisons even more problematicFootnote 2Footnote 6Footnote 9Footnote 10.
The four most common forms of bacterial meningitis identified were as follows: pneumococcal, streptococcal, staphylococcal, and meningococcal. In several studies, the most commonly identified causes of bacterial meningitis were S. pneumoniae, N. meningitidis, Group B Streptococcus (GBS) and L. monocytogenes Footnote 2Footnote 3Footnote 6Footnote 8Footnote 10. Staphlycoccus meningitis was responsible for 14% of cases for which a bacterium was reported. One reason for this finding is that nosocomially acquired cases were included in this study; S. aureus or S. epidermidis are known to be a complication of surgical procedures Footnote 11. This has not occurred with those studies that focus on community-acquired cases, on a limited group of bacteria, or on classifying less common causative agents as "other"Footnote 6Footnote 7Footnote 8Footnote 10.
Universal Hib vaccination programs have resulted in a dramatic decrease in Hib meningitisFootnote 1. In this study, Haemophilus meningitis accounted for 5% of all bacterial meningitis cases. While Hib vaccination programs were in effect in Canada throughout the duration of the study period, pneumococcal conjugate and meningococcal C conjugate vaccines were not approved for use until 2001, and not all provinces and territories have implemented universal immunization programs with these vaccines. Consequently, the effect of meningococcal and pneumococcal immunization programs would not be evident in these data. However, because pneumococcal and meningococcal meningitis were responsible for 36% and 9% of bacterial meningitis cases with a reported organism, full implementation of these programs would likely modify the burden of illness from bacterial meningitis and cause a shift in the predominance of pathogens causing disease.
As expected, the pathogen-specific incidence and proportions varied by age. The breakdown by age is consistent with known epidemiology of specific organismsFootnote 6Footnote 12Footnote 13. GBS is the most common cause of meningitis in neonatesFootnote 6Footnote 10; in our study, the incidence of streptococcal meningitis was highest in children < 1 year of age. Unfortunately, we were unable to identify whether the cases of streptococcal meningitis were caused by GBS.
The median age of persons with bacterial meningitis has increased throughout the period under study. This shift in age distribution has also been observed in the US Footnote 10. This suggests a benefit from childhood vaccination programs. Unfortunately, vaccines are unavailable for GBS and staphylococcal meningitis, two important causes of bacterial meningitis.
This study has important limitations. Using administrative data from HMDB may allow for a relatively accurate estimate of the overall incidence of bacterial meningitis; however, the same may not be true for pathogen-specific rates. It is likely that these rates represent underestimations. Diseases caused by specific pathogens may be classified as "unspecified" disease or as unspecified bacterium. In fact, the largest proportion of cases of bacterial meningitis was "unspecified" The abundance of cases classified as "unspecified bacterium" could be a result of various issues, which include initiating treatment prior to culture, lack of culture identification, and lack of availability of laboratory results at the time of coding. Not all unspecified cases are avoidable. Negative cerebrospinal fluid cultures occur in 11% to 30% of persons with bacterial meningitis Footnote 8. Even so, this results in underestimation of pathogen-specific rates. In addition, cases with a diagnosis of unspecified meningitis (code 322.9) were not included to minimize misclassification because of the uncertainty that they were bacterial in origin. This would also result in underestimating pathogen-specific rates.
Some pathogen-specific rates could be misclassified due to coding issues. Cases of pneumococcal meningitis could have been classified as streptococcal meningitis, because the data fields are not mutually exclusive. This would result in underestimating pneumococcal meningitis rates and overestimating non-pneumococcal streptococcal rates. Relatively simple changes in coding practices, requiring the two fields to be mutually exclusive, would rectify this.
Because detail within any bacterial category is unavailable, the data disallow for further subanalysis. It is unknown what proportion of H. influenzae cases are due to Hib and are thus vaccine preventable. Similarly, the proportion of pneumococcal and meningococcal meningitis cases that are vaccine preventable cannot be ascertained; the serotypes or serogroups are unknown. A number of organisms may be included within streptococcal meningitis, including GBS and group A streptococcus, both of which have distinct epidemiology. Although it can be expected that a large proportion of streptococcal meningitis will be GBS - as it is known that GBS is the most common cause of neonatal meningitis - the data do not allow further classification Footnote 6Footnote 10.
Conclusion
Bacterial meningitis results in significant morbidity in Canada. Universal Hib immunization has changed the epidemiology of bacterial meningitis in regions of the world that have implemented programs. Fully implementing universal pneumococcal conjugate and meningococcal C conjugate vaccination programs across the country may decrease the burden of illness from bacterial meningitis.
Acknowledgements
The authors would like to thank Ora Kendall, Wai Ming Chan, Mandy Weselak, and Rob Stirling for their assistance.
Source: SL Deeks, MD, MHSc, Immunization and Respiratory Infections Division (IRID), Public Health Agency of Canada (PHAC), Toronto, Ontario; DM MacDonald, MHSc, Consultant, Georgetown, Ontario; SG Squires, BScN, MSc, IRID, PHAC, Ottawa, Ontario; A Medaglia, BA, IRID, PHAC, Ottawa, Ontario; T Tam, MD, IRID, PHAC, Ottawa, Ontario.
Page details
- Date modified: