Effectiveness of Vaccine Against Medical Consultation Due to Laboratory-Confirmed Influenza: Results From a Sentinel Physician Pilot Project in British Columbia, 2004-2005
Introduction
Trivalent inactivated vaccine (TIV) is currently the only influenza vaccine marketed in Canada(1). TIV is recommended by the National Advisory Committee on Immunization (NACI) and is publicly funded in most provinces for high-risk target groups and their caregivers. TIV is only effective against influenza strains included in the vaccine and offers no protection against unrelated viruses that may cause a similar constellation of symptoms. Vaccine components must be updated to keep pace with emergence of new influenza variants. TIV contains three strains of influenza virus – two A and one B. Included vaccine components represent the three strains anticipated to dominate during the upcoming influenza season, typically spanning from November to April in the northern hemisphere. A new vaccine formulation must be considered each year. Vaccine components are selected by the World Health Organization as early as February for the mass immunization campaign to be conducted in autumn of the same year. Despite the inherent uncertainties in making predictions, vaccine composition has been matched to circulating strains over the past decade with three notable exceptions: 1997-1998 (unexpected emergence of A/H3N2/Sydney/05/97), 2003-2004 (unexpected emergence of A/H3N2/Fujian/411/2002) and 2004-2005 (unexpected emergence of A/H3N2/California/7/04)(1,2).
More TIV is distributed each year in Canada than all other vaccines combined. Despite this, no system currently exists, pre- or post-marketing, to assess efficacy or effectiveness of the new influenza formulation produced each year and administered to increasing segments of the population. For practical reasons, annual randomized placebo-controlled trials (RCTs) cannot be conducted; obstacles include the high costs of implementation, the timeliness of results and the ethical concerns associated with using placebo for a recommended product. Observational studies, such as case control or cohort designs, offer less costly alternatives to RCTs for measuring VE, but these methods may suffer from the influence of known and unknown confounding factors. When information about confounders is collected, techniques exist to adjust for these influences, in particular confounding by indication(3,4).
For the 2004-2005 season, the British Columbia Centre for Disease Control (BCCDC) piloted a novel approach for assessing influenza VE through its sentinel physician network. VE against medical consultation due to laboratory-confirmed influenza was undertaken using an observational case-control method. The purpose of the pilot study was to explore VE and to assess the feasibility of using a sentinel network for ongoing VE monitoring annually, as well as to identify key issues pertinent to that.
Methods
Sentinel surveillance system
BC has had a sentinel physician network for influenza surveillance since 1977; the system is managed by the BCCDC. Participating physicians record the number of patients presenting with influenza-like illness (ILI) every week as a proportion of the total number of patients seen. ILI is defined as a patient with acute onset of respiratory illness with fever and cough and one or more of: sore throat, arthralgia, myalgia or prostration.
For the 2004-2005 season, sentinels in BC were encouraged to increase their collection of respiratory specimens from amongst patients presenting with ILI, with additional reminders issued by phone and fax during the peak influenza period. Each sentinel was supplied with modified laboratory requisitions affixed with five questions requiring Yes/No response, including whether the patient (a) met the case definition for ILI; (b) had received influenza vaccine during the 2004-2005 season; (c) if vaccinated, whether the last age-appropriate dose was = 2 weeks prior to ILI onset; (d) if vaccinated, whether this was for a recognized high-risk condition as defined by NACI(1) and (e) whether the specimen was collected within 48 hours of ILI onset. Laboratory requisitions routinely elicit information on age and sex. Incomplete records were identified and their sentinel physicians contacted by a team of study nurses to retrieve missing information.
Study design
Case-control design was used. Participants included individuals presenting with ILI to a sentinel physician from whom a respiratory specimen was collected and tested for influenza at BCCDC during the study period. The surveillance period for 2004-2005 began 26 September, 2004. The period of study for determining vaccine effectiveness began from first detection of influenza by the sentinel system, until 31 March, 2005.
Cases were sentinel patients with ILI and laboratory-confirmed influenza identified during the study period. Controls were all other sentinel patients with ILI who tested negative for influenza during the study period. Cases and controls were compared on influenza immunization status.
The University of British Columbia clinical research ethics board approved the study.
Immunization
Immunization of patients was per routine practice. Influenza vaccine is publicly funded in BC for all NACI-recommended groups(5). For the 2004-2005 influenza season, Shire Biologics (Fluviral®) supplied TIV in BC for all age groups except infants and toddlers for whom a reduced thimerosal-containing formulation was provided from Sanofi Pasteur (Vaxigrip®). Doses were per age-specific recommendation(5). TIV formulations were standardized to contain 15 μg each of A/H1N1/New Caledonia/ 20/99, A/H3N2/Wyoming/3/2003 (antigenically equivalent to A/H3N2/Fujian/411/2002) and B/Jiangsu/10/2003 strains(5).
Laboratory identification
Respiratory specimens collected by sentinel physicians included nasal or naso-pharyngeal swabs in transport medium or nasal washings. All were forwarded to BCCDC for processing. Virus diagnosis was by real-time polymerase chain reaction (RT-PCR), isolation into R-Mix cells (Diagnostic Hybrids Inc.) and isolation in cultures of RhMK, A549, and MRC5 cells. For RT-PCR, RNA was extracted from a 250 microlitre specimen (Qiagen) and amplified on the ABI 7900 using primers and Taqman probes for influenza A and B(6,7).
Portions of the remaining specimen were inoculated into two cultures of R-Mix cells which were harvested after 24 and 48 hours, fixed and stained for immunofluorescence microscopy to be examined for the presence of influenza and other respiratory virus antigens. A final aliquot of the specimen was inoculated into cell cultures which were examined over the course of one week for the development of characteristic viral cytopathic effects.
Strain characterization of influenza virus isolates was performed at the National Microbiology Laboratory (NML). Hemagglutinationinhibition (HI) assay was carried out using post-infection fowl sera against influenza A and B, including the vaccine strains (A/H3N2/ Fujian/411/2002 and B/Shanghai/361/2002) and the antigenic variant, A/H3N2/California/7/2004, treated with receptor-destroying enzyme, four HA units of virus, and 0.7% w/v guinea pig red blood cells(8). An isolate was identified as antigenically similar to one of the prototype strains according to the reciprocal of the highest HI titres.
Data analysis
Univariate comparisons were through Chi-square test. Odds ratios (OR) for medical consultation due to laboratory-confirmed influenza in vaccinated compared to non-vaccinated individuals were computed through binomial logistic regression models, with and without adjustment for age and sex. VE was then estimated as (1-OR vaccinated/unvaccinated)(3).
Analyses of VE against influenza A and B combined (models a,c,e) and influenza A alone (models b,d,f) were performed. Models a/b are based on any immunization during the 2004-2005 season without reference to delay. In models c/d ILI onset must have been = 2 weeks after last age-appropriate immunization for patients to be considered immunized. Models e/f similarly qualified influenza immunization status and, in addition, included only individuals whose specimens were collected within 48 hours of ILI onset.
Results
Study period and patient inclusion
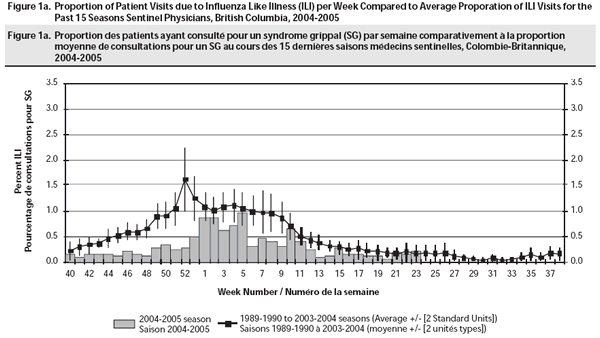
The BC surveillance system for the 2004-2005 season included 45 sentinel sites across the province, of which all but 10 contributed specimens. Patient visits to sentinel physicians for ILI as a proportion of all patient visits are shown in Figure 1a.
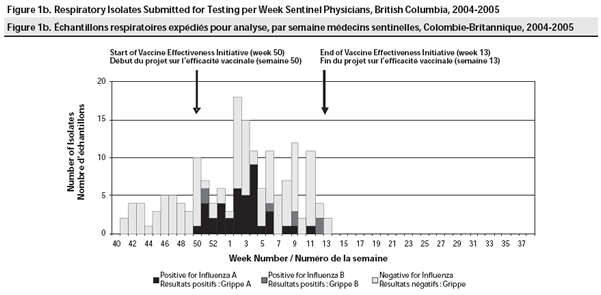
There were 219 separate submissions of respiratory specimens by a known sentinel physician during the 2004-2005 surveillance period. Of these, only 32 (15%) had all questionnaire information completed on the original laboratory requisition; 187 required follow-up interview with the submitting physician to complete missing information and 133 were completed. From the 165 patients with complete records, specimens were collected between 4 October, 2004 and 31 March, 2005 with the distribution of submissions mirroring the distribution of sentinel visits for ILI overall (Figure 1b).
First identification of influenza through the sentinel system was on 8 December, 2004. There were 134 specimen submissions accompanied by complete patient information from 8 December, 2004 until study close on 31 March, 2005. Analysis is confined to these 134 patient records.
Laboratory findings and influenza strain characterization
Of 134 participants, influenza A or B was diagnosed in the respiratory specimen of 47 (28%) of which 40/47 (85%) were identified as influenza A, and seven (15%) as influenza B. Of patients with influenza A, 7/40 (18%) were ≤ 19 years of age, 30/40 (75%) were 20 to 64 years and 3/40 (8%) were = 65 years. Corresponding age distribution of patients with influenza B was: 4/7 (57%), 3/7 (43%) and 0/7, respectively.
Of the 40 influenza A identifications, 21 were identified by viral culture – 15/21 (71%) were characterized as A/H3N2/California/ 7/2004 and six (29%) as A/H3N2/Fujian/411/2002. The first influenza A identification was from a specimen submitted 8 December, 2004 (characterized as A/H3N2/California/7/2004) with the last on 16 March, 2005; 85% of influenza A identifications were made prior to 31 January, 2005. The last influenza A/H3N2/California/7/2004 identification was submitted 27 January, 2005.
Of the seven influenza B identifications, six were identified by viral culture; half were characterized as B/Hong Kong/330/2001- like virus (similar to the vaccine component for 2003-2004) and half as B/Shanghai/361/2002-like (antigenically equivalent to the vaccine component for 2004-2005). Identification of influenza B through the sentinel network was later in the season; the first identification was on 8 December, 2004, with 5/7 (71%) identified after 10 February, 2005, and the last on 23 March, 2005.
Influenza subtype and strain characterization through the BC sentinel network for 2004-2005 was virtually identical to the profile observed nationally in Canada(1).
Patient characteristics
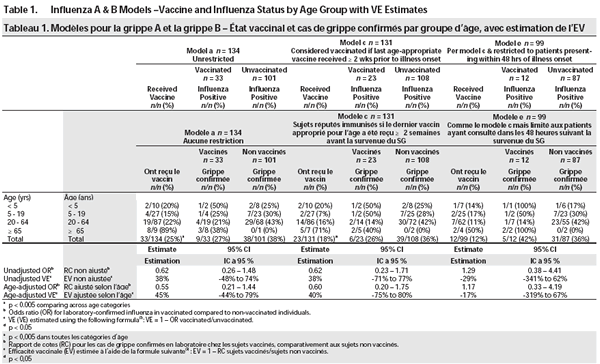
Vaccination status and laboratory findings by age group among patients included in separate analyses can be found in Tables 1 (models a/c/e) and 2 (models b/d/f).
Of 134 patients, 77/134 (58%) were female, 9/133 (7%) were 65 years of age or older, and 33/134 (25%) received influenza vaccine during the 2004-2005 season. This rate of vaccination is consistent with that found in the general population of BC (27%)(9). Persons = 65 years of age were significantly more often vaccinated (8/9 or 89%) than younger persons (25/124 or 20%) (p < 0.001). Among vaccinated persons, 6/30 (20%) were at high-risk for complications of influenza based on NACI definitions; 3/6 vaccinated high-risk persons were also elderly(1). Of vaccinated persons, 23/30 (69%) received the vaccine more than 2 weeks prior to onset of ILI.
Of 134 participants, 102 (76%) presented within 48 hours of ILI onset. Vaccinated persons (21/33 or 64%) were significantly less likely to present within 48 hours of ILI onset compared to non-vaccinated persons (81/100 or 81%) (p = 0.04). This did not vary with age/sex. Influenza A/B viruses were diagnosed among 38/102 persons (37%) presenting within 48 hours of ILI onset and 8/31 persons (26%) presenting more than 48 hours after ILI onset (p = 0.2).
Vaccine Effectiveness
Crude and age-adjusted estimates of VE against medical consultation due to laboratory-confirmed influenza are presented in Tables 1 (models a/c/e) and 2 (models b/d/f). Though sample size was small and confidence intervals are wide, point estimates show interesting trends, consistent with previous investigations of VE and with mismatch this season(10). Vaccine was more effective against influenza A alone, than against influenza A and B combined. Because of few detections (seven cases), separate analyses for influenza B are not presented. If immunization status was only considered to be positive if the last age-appropriate vaccination was = 2 weeks before ILI onset, the estimate of VE against influenza A improved. VE against influenza A also improved following adjustment for age, and, in particular, for elderly status. Statistically significant age-adjusted protection was found against influenza A in models b and d.
Age-adjusted point estimates for VE showed protection against medical consultation for influenza A/B of 40% to 45% and against influenza A of 70% to 75% with the exception of models e and f. When analysis was restricted to patients whose respiratory specimens were submitted within 48 hours of illness onset, point estimates of VE fell below zero for influenza A/B and to approximately 40% for influenza A alone.

Discussion
This pilot study was designed during the summer months and launched in September 2004. Interest in VE assessment subsequently increased when, during the 2004-2005 season, a higher than expected number of influenza outbreaks were reported in BC from long term care facilities (90); this figure is greater than the number of facility outbreaks reported previously in BC during seasons of known vaccine mismatch (60 reports in 2003-2004 and 62 in 1997-1998). This trend amongst a highly immunized, albeit elderly cohort, led to speculation of possible vaccine mismatch in 2004-2005 that was later confirmed in mid-February as related to unexpected emergence of A/H3N2/California/7/2004(1).
An observational study design was chosen as the most convenient and efficient approach to assess VE. Sentinel networks have been in place in Canada for decades. They have been used annually to provide proportionate characterization of ILI intensity. They have not previously been used for controlled epidemiologic investigation. We used the sentinel network to piggyback an evaluation of VE and to distinguish cases from controls on the basis of laboratory-confirmed outcome. All laboratory identification was performed at BCCDC, eliminating variability in detection that may exist between test sites. Both cell culture assay and RT-PCR were used to identify influenza. RT-PCR assays at BCCDC are able to reproducibly detect between 1 to 10 infectious units of virus per 200 microlitre extract (unpublished data, BCCDC).With this sensitive protocol, we found that about 25% to 30% of persons presenting to sentinels with ILI over the course of the season had laboratory-confirmed influenza. This low rate of medical consultation for ILI due to influenza highlights the importance of incorporating an element of laboratory confirmation into evaluations of VE. The case definition for ILI is known to be non-specific. Even during the peak influenza season, most cases of ILI are not due to influenza and are not preventable through immunization (10). Misclassification can result in substantial underestimation of true vaccine performance. It was this understanding that ILI is not equated with influenza that enabled us to draw controls from sentinel reports.
Our study has the advantage of assessing VE against laboratoryconfirmed influenza but is predicated on the assumption that vaccinated persons have the same likelihood of presenting to a physician as non-vaccinated persons, if either develops ILI. It is also predicated on an equal likelihood of detection of influenza, if present. Virus shedding is greatest in the early stages of influenza illness (especially the first 48 hours) and differential timing of presentation could affect virus detection and estimates of VE(11). Sensitive RT-PCR assay likely extends the period of virus detection, especially among symptomatic persons. More research into the kinetics of virus shedding and its detection through different laboratory methods in both vaccinated and nonvaccinated persons would be useful. We found that vaccinated persons were more often delayed beyond 48 hours in their presentation to a physician for ILI, possibly because of less severe illness or a belief that they were safe from complication. If vaccinated persons with influenza present later in the course of attenuated illness and virus shedding and detection are truly diminished after 48 hours, we could be over-stating VE. When analysis was restricted to persons who presented within the first 48 hours of illness onset, estimates of VE fell.
We found age-adjusted point estimates for VE against medical consultation for laboratory-confirmed influenza A during the mismatched 2004-2005 season to range as low as 40% and as high as 75%. VE varied with age, definition of immunization status and whether analysis was restricted to presentation within 48 hours of ILI onset. Overall, our estimates suggest cross-protection for the 2004-2005 season despite vaccine mismatch. Our VE estimates mostly reflect the protection conferred to young healthy adults; the sample included few elderly persons or those with underlying conditions. The higher than expected reports of facility outbreaks in 2004-2005 in BC may have reflected an even lower VE amongst the frail elderly. Because of small sample size, estimates are unstable with wide confidence intervals. The possibility of no protection cannot be ruled out.
Conclusions
The sentinel physician network is a convenient and efficient way to monitor influenza VE annually. In planning for an ongoing system using this approach, attention should be paid to the following lessons from this pilot study:
-
The pilot suffered from small sample size limiting the precision of VE estimates. Future studies should be powered to enable precise VE determination by age subgroup. Several options exist to expand sample size in subsequent years, including invitation to participate by other provinces across Canada with similar sentinel networks.
-
Sampling an equal proportion of vaccinated and nonvaccinated persons would most efficiently maximize the power of future studies.
-
Future studies should collect information on both age and high risk conditions from vaccinated and non-vaccinated persons along with information on ILI severity, delay since immunization and delay to presentation following ILI onset. These may significantly affect VE estimation. To assess the effect of repeat immunization, prior vaccine history should also be elicited(12).
-
Categorical tick box responses limit the ability to examine the effects of continuous variables such as delay between immunization and illness onset or delay to specimen collection. These values should be recorded on a continuous scale to enhance understanding of the involved kinetics and their influence on VE estimation.
-
Despite repeat reminders, few sentinels completed the questionnaire affixed to the laboratory requisition; most records required follow-up by a team of study nurses to retrieve missing information. This need for dedicated research assistance should be anticipated. Questionnaires should be kept as simple as possible to encourage completion, while enabling sufficient control for bias and confounding.
-
BCCDC is unique in Canada in that epidemiology and laboratory services are both housed within the same building. If the same approach to evaluate VE is to be expanded nationally, close collaboration and linkage between epidemiology and laboratory services will be fundamental.
-
The BC pilot project was undertaken without additional funding and all sentinels participated as volunteers. An ongoing or expanded system would require public health investment. In particular, compensation paid to sentinels per specimen collected may enhance the rate of participation and questionnaire completion.
Acknowledgements
We acknowledge the physicians across BC who voluntarily contributed to the sentinel influenza surveillance network and most notably those who participated in this pilot project.We thank also Ms. L. Hoogewerf, Family Practice Research, British Columbia for data collection and the nurses of Westcoast Clinical Research for assistance in the completion of missing information.
References
-
National Advisory Committee on Immunization. Statement on influenza vaccination for the 2005-2006 season. CCDR 2005;31(6):1-32.
-
David S, Skowronski D, Tweed S et al. Epidemiologic profile of a new H3N2 variant of influenza A mismatched to vaccine, 2003-2004 influenza season. CCDR 2005;31(2):21-31.
-
OrensteinWA, Bernier RH, Dondero TJ et al. Field evaluation of vaccine efficacy. BullWHO 1985;63:1055-68.
-
Hak E, Verheij TJ, Grobbee DE et al. Confounding by indication in non-experimental evaluation of vaccine effectiveness: The example of prevention of influenza complications. J Epidemiol Community Health 2002;56(12):951-55.
-
National Advisory Committee on Immunization. Statement on influenza vaccination for the 2004-2005 season. CCDR 2004;30(3):1-32.
-
Schweiger B, Zadow I, Heckler R et al. Application of a fluorogenic PCR assay for typing and subtyping of influenza viruses in respiratory samples. J Clin Microbiol 2000;38(4):1552-58.
-
van Elden LJ, Nijhuis M, Schipper P et al. Simultaneous detection of influenza viruses A and B using real-time quantitative PCR. J Clin Microbiol 2001;39(1):196-200.
-
Kendal AP, Pereira MS, Skethel JJ (1982). Concepts and procedures for laboratory-based influenza suveillence. U.S. Department of Health and Human Services, Public Health Service, Centers for Disease Control and Prevention, Atlanta, Georgia.
-
Johansen H, Nguyen K, Mao L et al. Influenza vaccination. Health Reports (Statistics Canada, Catalogue 82-003). 2004;15(2): 33-41.
-
Nichol KL. Efficacy/clinical effectiveness of inactivated influenza virus vaccines in adults. In: Nicholson KG, Webster RG, Hay AJ, editors. Textbook of influenza. Malden MA: Blackwell Science Ltd., 1998.
-
Nicholson KG. Human influenza. In: Nicholson KG, Webster RG, Hay AJ, editors. Textbook of influenza. MaldenMA: Blackwell Science Ltd., 1998.
-
Smith DJ, Forrest S, Ackley DH et al. Variable efficacy of repeated annual influenza vaccination. Proc Natl Acad Sci USA 1999;96(24):14001-06.
Source: DM Skowronski, MD, FRCPC Epidemiology Services, BC Centre for Disease Control; M Gilbert, MD, FRCPC, Epidemiology Services, BCCDC and Canadian Field Epidemiology Program, Public Health Agency of Canada (PHAC); SA Tweed, MSc, Epidemiology Services, BCCDC, M Petric, PhD, FCCM Laboratory Services, BCCDC, Y Li, PhD, National Microbiology Laboratory, PHAC, A Mak, BSc, RT Laboratory Services, BCCDC, G McNabb, BSc, ART, Laboratory Services, BCCDC; G De Serres, MD, PhD Quebec National Institute of Public Health.
Page details
- Date modified: