Surveillance for Methicillin-Resistant Staphylococcus aureus in Canadian Hospitals - A Report Update from the Canadian Nosocomial Infection Surveillance Program
 1 February 2005
1 February 2005
Methicillin-resistant Staphylococcus aureus (MRSA) remains an important nosocomial pathogen, although the organism has increasingly been recognized as a significant cause of community-acquired infection around the world. Surveillance for MRSA in sentinel Canadian hospitals participating in the Canadian Nosocomial Infection Surveillance Program (CNISP) has been ongoing since its inception in January 1995. Initial results have previously been published(1-3). This report, which covers the years 1995 to 2003, provides an update of the program results.
Methods
The CNISP is a collaborative effort involving hospitals across the country participating as members of the Canadian Hospital Epidemiology Committee (a sub-committee of the Association of Medical Microbiology and Infectious Diseases Canada), and the Nosocomial and Occupational Infections Section, Public Health Agency of Canada. From 1995 to 2003, the number of participating hospital sites increased from 22 to 38, with representation from nine Canadian provinces.
Surveillance methods have previously been described(3). The surveillance was laboratory-based. When a new case of MRSA from an inpatient was identified, the patient's medical records were reviewed for clinical and epidemiologic data. The presence of infection caused by MRSA was determined according to standard definitions(4). MRSA colonization was defined as the presence of MRSA without any clinical signs or symptoms of infection. MRSA was thought to have been hospital-acquired if, in the judgment of the infection control professional, there was no evidence that the organism was present at the time of admission to hospital, or if there was evidence that it was likely to have been acquired during a previous hospital admission. Cases were classified as having been acquired in the community if there was no evidence of hospital or nursing home acquisition.
All isolates were confirmed to be MRSA by detection of the mecA gene by polymerase chain reaction (PCR) assay(5). Antimicrobial susceptibility was tested by microbroth dilution methods in accordance with the guidelines of the National Committee for Clinical Laboratory Standards(6). Isolates were further characterized by pulsed-field gel electrophoresis (PFGE) after extraction of DNA and digestion of the extract with Smal(7). Electrophoretically generated DNA profiles were digitized and analyzed using Gel Compar software, and isolates with specific DNA profiles were grouped into one of the previously described, or newly identified Canadian epidemic clones(2,8).
Results
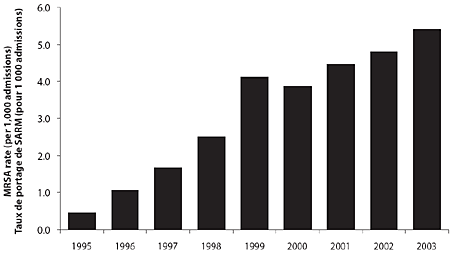
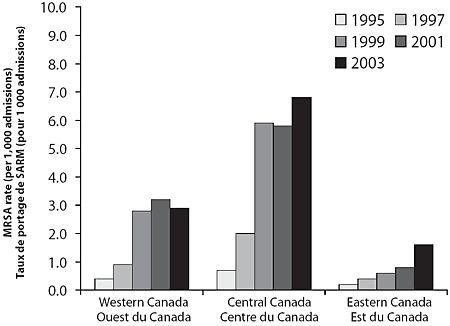
Between 1995 and 2003, MRSA rates increased in CNISP hospitals from 0.46 cases per 1,000 admissions to 5.10 per 1,000 admissions (p = 0.002) (Table 1 and Figure 1). Most of the increase in MRSA cases occurred in central Canada (Ontario and Quebec), although there were also increases elsewhere in the country (Figure 2).
Year |
Rate per 100 |
Rate per 1,000 |
| ALL MRSA* | ||
| 1995 | 0.95 | 0.46 |
| 1996 | 1.97 | 1.07 |
| 1997 | 3.07 | 1.67 |
| 1998 | 3.90 | 2.50 |
| 1999 | 5.97 | 4.12 |
| 2000 | 6.96 | 3.87 |
| 2001 | 8.73 | 4.46 |
| 2002 | 8.62 | 4.81 |
| 2003 | 10.39 | 5.10 |
| MRSA infections | ||
| 1995 | 0.51 | 0.25 |
| 1996 | 0.85 |
0.46 |
| 1997 | 1.33 | 0.72 |
| 1998 | 1.52 |
0.98 |
| 1999 | 1.62 | 1.11 |
| 2000 | 1.70 |
1.09 |
| 2001 | 1.41 |
1.14 |
| 2002 | 1.71 |
1.38 |
| 2003 | 2.00 |
1.61 |
| * infections and colonizations | ||
Overall, 57% of the patients with MRSA were male. The median age was 73 years, and 63% were > 65 years of age. The indications for obtaining a culture that eventually yielded MRSA are shown in Table 2. Between 1995 and 2003, the proportion of cases identified by a culture of a specimen obtained for a clinical indication (infection suspected) decreased from 71% to 39%, and the proportion obtained from a screening specimen increased from 20% to 47% (p < 0.001). A total of 6,435 (38%) patients were thought to have had an MRSA infection. The most common sites of infection were skin and soft tissue in 24%, respiratory tract (23%), and at a surgical site (21%). Infection was associated with bacteremia in 13% of the patients. MRSA infection rates increased from 0.25 per 1,000 admissions in 1995 to 1.61 per 1,000 admissions in 2003 (p < 0.001).
Table 2. Indications for MRSA cultures in Canadian hospitals, 1995-2003
Reason culture was done |
Year | ||
1995 |
1999 |
2003 |
|
Clinical indication (infection was suspected) |
71% |
52% |
39% |
Outbreak investigation |
9% |
15% |
14% |
Admission screening |
0 |
19% |
31% |
Other screening |
20% |
14% |
16% |
MRSA was thought to have been acquired in a hospital in the majority of cases (72%), in a long-term care facility (7%), and 8% were thought to have been community-acquired; in 13% of cases the source of MRSA acquisition could not be determined. Rates of nosocomial acquisition of MRSA increased, from 0.91 cases per 1,000 admissions in 1997 to 3.66 per 1,000 admissions in 2001, and 3.83 per 1,000 admissions in 2003 (p < 0.001). An epidemiologic link between the index case and another patient in the hospital with MRSA was identified for slightly more than half of the cases (52%). An epidemiologic link was more likely to have been identified in 2003 (51%) than in 1995 (41%) (p < 0.001).
Antimicrobial susceptibility testing of 4,033 randomly selected isolates from 1995 and 2002 revealed uniform resistance to the ß-lactam antibiotics. Resistance rates to other antimicrobial agents were as follows: erythromycin (94% of isolates), clindamycin (85%), ciprofloxacin (90%), trimethoprim-sulfamethoxazole (46%), tetracycline (28%), fusidic acid (6%), mupirocin (4%), and rifampin (2%). None of the isolates were found to have reduced susceptibility to vancomycin, but five strains resistant to linezolid (MIC = 8 µg/ml) have been identified. Isolates recovered from hospitals in provinces west of Ontario were more likely to be resistant to tetracycline (63% vs. 8%; p < 0.001) and to trimethoprim-sulfamethoxazole (61% vs. 38%; p < 0.001) than were those recovered from Ontario, Quebec, or the Atlantic provinces. Mupirocin resistance (MIC > 128 µg/ml) rates increased from 2% before 1998 to 6% in 2002 (p < 0.001).
A total of 4,033 isolates were also characterized by PFGE. Of these, 91% could be grouped into one of six Canadian "epidemic" clones (CMRSA-1, CMRSA-2, etc) (Figure 3). The most commonly identified clones of MRSA were found in most regions of the country and have been designated CMRSA-1 (43% of isolates) and CMRSA-2 (16% of isolates).

Discussion
Surveillance for MRSA in CNISP hospitals has shown that MRSA rates continue to climb in Canadian hospitals. Rates of MRSA are now 10 times higher than they were when surveillance started in 1995. Increases have occurred across the country, although the highest rates are seen in hospitals in Quebec and Ontario. Rates in the Atlantic Provinces remain low, but appear to have increased significantly in the past year. Although much of the observed increase in MRSA detection may be attributed to screening programs in hospitals, there has also been a five-fold increase in MRSA infection rates. MRSA infections are associated with increased morbidity and mortality, prolonged hospitalization, and increased costs(9,10).
In the past few years, community-acquired MRSA has emerged as a major problem in many parts of the United States, associated with the transmission of a strain of the organism possessing a specific staphylococcal chromosomal cassette (SCCmec type IV), and the Panton-Valentine leukocidin (PVL) genetic determinant(11). In Canada, most (approximately 85%) MRSA remains hospital-acquired, but these community-acquired strains have occasionally been seen in CNISP hospitals, particularly in aboriginals residing in western provinces (data not shown). In these patients, MRSA was associated with the development of skin and soft tissue infections.
MRSA is typically resistant to multiple classes of antibiotics. Therefore treatment options for the management of serious MRSA infections are limited. Vancomycin is generally regarded to be the treatment of choice(12). Currently, < 3% of S. aureus infections in Canadian hospitals are due to MRSA, so vancomycin should not be used routinely for the management of staphylococcal infections unless risk factors for MRSA (e.g., prior colonization or known exposure) are present. This recommendation would have to be reassessed if MRSA infection rates continue to rise. It is noteworthy that the number of reported bacteremias due to MRSA has increased in Ontario, such that in 2003, 11% of S. aureus isolates from blood cultures in the province were MRSA(13).
MRSA strains with reduced susceptibility to glycopeptides have been reported from the United States and other countries, but have not yet been identified in Canada. However, there has been an increase in high-level resistance to mupirocin (6% in 2002), an agent that is potentially useful for decolonization of MRSA carriers. These results suggest that mupirocin should be used selectively (in those most likely to benefit) in order to prevent further increases in mupirocin resistance rates.
Although MRSA demonstrate considerable genetic diversity, molecular characterization by PFGE indicates that there are a relatively small number of epidemic clones circulating in Canadian hospitals. Many of these clones have also been described globally(14) (Table 3). The virulence factors associated with greater ease of transmission of epidemic strains of MRSA have not yet been identified.
Canadian MRSA epidemic clones |
MRSA epidemic clones in the United States* |
Pandemic clones, nomenclature |
MLST type† |
CMRSA-1 |
USA500 |
Iberian, Archaic |
247 |
CMRSA-2 |
USA100 |
NY, Japan |
5 |
CMRSA-3 |
not named |
Brazilian, Hungarian |
239 |
CMRSA-4 |
USA200 |
EMRSA-16 |
36 |
* McDougal et al., 200314 |
|||
The results of this surveillance program suggest that in the past decade Canadian hospitals have been only partially successful in limiting the transmission of MRSA. The continued spread of MRSA poses a significant risk to patients and contributes to a substantial financial burden on healthcare resources. Many studies have now confirmed the cost-effectiveness of control programs that include screening and implementation of contact barrier precautions(15,16). Hospitals should make prevention of the emergence and transmission of antibiotic-resistant organisms and other hospital-acquired infections a patient safety priority, and should commit adequate resources to screening and implementation of other preventative measures. Ongoing surveillance is also essential in order to monitor the constantly evolving epidemiology of antibiotic-resistant organisms such as MRSA.
References
-
Simor A, Ofner-Agostini M, Patin S et al. The Canadian Nosocomial Infection Surveillance Program: Results of the first 18 months of surveillance for methicillin-resistant Staphylococcus aureus in Canadian hospitals. CCDR 1997;23:41-5.
-
Simor AE, Boyd D, Louie L et al. Characterization and proposed nomenclature of epidemic strains of MRSA in Canada. Can J Infect Dis 1999;10:333-6.
-
Simor AE, Ofner-Agostini M, Bryce E et al. The evolution of methicillin-resistant Staphylococcus aureus in Canadian hospitals: 5 years of national surveillance. CMAJ 2001;165:21-6.
-
Garner JS, Jarvis WR, Emori TG et al. CDC definitions for nosocomial infections, 1988. Am J Infect Control 1988;16:128-40.
-
Louie L, Matsumura SO, Choi E et al. Evaluation of three rapid methods for detection of methicillin resistance in Staphylococcus aureus. J Clin Microbiol 2000;38:2170-3.
-
National Committee for Clinical Laboratory Standards. Methods for dilution antimicrobial susceptibility tests for bacteria that grow aerobically [approved standard M7-A6]. Sixth ed. Wayne, Pa., 2003.
-
Mulvey MR, Chui L, Ismail J et al. Development of a Canadian standardized protocol for subtyping methicillin-resistant Staphylococcus aureus using pulsed-field gel electrophoresis. J Clin Microbiol 2001;39:3481-5.
-
Simor AE, Ofner-Agostini M, Bryce E et al. Laboratory characterization of methicillin-resistant Staphylococcus aureus in Canadian hospitals: Results of 5 years of national surveillance, 1995-1999. J Infect Dis 2002;186:652-60.
-
Cosgrove SE, Sakoulas EN, Schwaber MJ et al. Comparison of mortality associated with methicillin-resistant and methicillin-susceptible Staphylococcus aureus bacteremia: A meta-analysis. Clin Infect Dis 2003;36:53-9.
-
Kim T, Oh PI, Simor AE. The economic impact of methicillin-resistant Staphylococcus aureus in Canadian hospitals. Infect Control Hosp Epidemiol 2001;22:99-104.
-
Vandenesch F, Naimi T, Enright MC et al. Community-acquired methicillin-resistant Staphylococcus aureus carrying Panton-Valentine leukocidin genes: Worldwide emergence. Emerg Infect Dis 2003;9:978-84.
-
Simor AE, Loeb M. The management of infection and colonization due to methicillin-resistant Staphylococcus aureus: A CIDS/CAMM position paper. Can J Infect Dis 2004;15:39-48.
-
McGeer A, Fleming CA, Green KA et al. Antimicrobial resistance in Ontario - are we facing defeat? QMPLS News October 2004;83:1-10.
-
McDougal LK, Steward CD, Killgore GE et al. Pulsed-field gel electrophoresis typing of oxacillin-resistant Staphylococcus aureus isolates from the United States: Establishing a national database. J Clin Microbiol 2003;41:5113-20.
-
Muto CA, Jernigan JA, Ostrowsky BE et al. SHEA guideline for preventing nosocomial transmission of multidrug-resistant Staphylococcus aureus and Enterococcus. Infect Control Hosp Epidemiol 2003;24:362-86.
-
Boyce JM, Havill NL, Kohan C et al. Do infection control measures work for methicillin-resistant Staphylococcus aureus? Infect Control Hosp Epidemiol 2004;25:395-401.
Source: AE Simor, MD, Sunnybrook & Women's College Health Sciences Centre, Toronto, Ont.; M Ofner-Agostini, BScN, MHSc, D Gravel, BScN, MSc, CIC, M Varia, BSc, MHSc, S Paton, MN, RN, Centre for Infectious Disease Prevention and Control, Public Health Agency of Canada, Ottawa; A McGeer, MD, Mount Sinai Hospital, Toronto, Ont.; E Bryce, MD, Vancouver General Hospital, Vancouver, BC; M Loeb, MD, McMaster University, Hamilton, Ont.; M Mulvey, PhD, National Microbiology Laboratory, Public Health Agency of Canada, Winnipeg, Man., for CNISP.
Members of the Canadian Nosocomial Infection Surveillance Program (CNISP): Dr. Elizabeth Bryce, Vancouver General Hospital, Vancouver, BC; Dr. John Conly, Foothills Medical Centre, Calgary, Alta.; Dr. Gordon Dow, The Moncton Hospital, Moncton, NB; Dr. John Embil, Health Sciences Centre, Winnipeg, Man.; Dr. Joanne Embree, Health Sciences Centre, Winnipeg, Man.; Dr. Michael Gardam, University Health Network, Toronto, Ont.; Ms. Denise Gravel, Centre for Infectious Disease Prevention and Control, Public Health Agency of Canada; Dr. Elizabeth Henderson, Peter Lougheed Centre, Calgary, Alta.; Dr. James Hutchinson, Health Sciences Centre, St. John's, Nfld.; Dr. Michael John, London Health Sciences Centre, London, Ont.; Dr. Lynn Johnston, Queen Elizabeth II Health Sciences Centre, Halifax, NS; Dr. Pamela Kibsey, Victoria General Hospital, Victoria, BC; Dr. Joanne Langley, I.W.K. Grace Health Science Centre, Halifax, NS; Dr. Mark Loeb, Hamilton Health Sciences Corporation, Hamilton, Ont.; Dr. Anne Matlow, Hospital for Sick Children, Toronto, Ont.; Dr. Allison McGeer, Mount Sinai Hospital, Toronto, Ont.; Dr. Sophie Michaud, CHUS-Hôpital Fleurimont, Sherbrooke, Que.; Dr. Mark Miller, SMBD-Jewish General Hospital, Montreal, Que.; Dr. Dorothy Moore, Montreal Children's Hospital, Montreal, Que.; Dr. Michael Mulvey, National Microbiology Laboratory, Public Health Agency of Canada; Ms. Marianna Ofner-Agostini, Centre for Infectious Disease Prevention and Control, Public Health Agency of Canada; Ms. Shirley Paton, Centre for Infectious Disease Prevention and Control, Public Health Agency of Canada; Dr. Virginia Roth, The Ottawa Hospital, Ottawa, Ont.; Dr. Andrew Simor, Sunnybrook and Women's College Health Sciences Centre, Toronto, Ont.; Dr. Geoffrey Taylor, University of Alberta Hospital, Edmonton, Alta.; Ms. Monali Varia, Centre for Infectious Disease Prevention and Control, Public Health Agency of Canada; Dr. Mary Vearncombe, Sunnybrook and Women's College Health Sciences Centre, Toronto, Ont.; Dr. Alice Wong, Royal University Hospital, Saskatoon, Sask.; Dr. Dick Zoutman, Kingston General Hospital, Kingston, Ont.
Page details
- Date modified: