Metabolic syndrome and chronic disease - CDIC: Vol 34, No 1, February 2014
Volume 34 · Number 1 · February 2014
Chronic Diseases and Injuries in Canada
Metabolic syndrome and chronic disease
D. P. Rao, MSc (1, 2); S. Dai, MD (2); C. Lagacé, MSc (2); D. Krewski, PhD (1, 3)
https://doi.org/10.24095/hpcdp.34.1.06
This article has been peer reviewed.
Author references:
- Institute of Population Health, University of Ottawa, Ontario, Canada
- Public Health Agency of Canada, Ottawa, Ontario, Canada
- Risk Sciences International, Ottawa, Ontario, Canada
Correspondence: Deepa Rao, Institute of Population Health, University of Ottawa, 1 Stewart Street, Room 300, Ottawa, ON K1N 6N5; Tel.: 613-897-8111; Fax: 613-562-5380; Email: Deepa.Rao@uottawa.ca
Abstract
Introduction: Metabolic syndrome (MetS) is a combination of risk markers that appear to promote the development of chronic disease. We examined the burden of MetS in Canada through its current and projected association with chronic disease.
Methods: We used measures from the Canadian Health Measures Survey 2007–2009 to identify the prevalence of MetS in Canadian adults and examine associations between sociodemographic factors and major chronic diseases. We estimated the projected cumulative incidence of diabetes and percent risk of a fatal cardiovascular event using the Diabetes Population Risk Tool (DPoRT) and Framingham algorithms.
Results: After adjusting for age, we found that 14.9% of Canadian adults had MetS. Rates were similar in both sexes, but higher in those who are non-Caucasian or overweight or obese (p < .001 for all three). The importance of MetS for public health was demonstrated by its significant association with chronic disease relative to the general population, particularly for diagnosed (11.2% vs. 3.4%) and undiagnosed (6.0% vs. 1.1%) type 2 diabetes. The ten-year incidence estimate for diabetes and mean percent risk of a fatal cardiovascular disease (CVD) event were higher in those with MetS compared to those without (18.0% vs. 7.1% for diabetes, and 4.1% vs. 0.8% for CVD).
Conclusion: MetS is prevalent in Canadian adults and a high proportion of individuals with MetS have diagnosed or undiagnosed chronic conditions. Projection estimates for the incidence of chronic disease associated with MetS demonstrate higher rates in individuals with this condition. Thus, MetS may be a relevant risk factor in the development of chronic disease.
Introduction
The vast majority of patients in the Canadian healthcare system are living with one or more chronic diseases.Endnote 1 Cardiovascular disease, chronic obstructive pulmonary disease, cancer and diabetes are the most common causes of hospitalization and premature death in Canada, accounting for almost three-quarters of all deaths.Endnote 2 Together, these chronic diseases account for 80% of primary care visits and more than two-thirds of medical costs.Endnote 1,Endnote 3 Knowing more about the risk factors and indicators for chronic disease may, therefore, help public health efforts aimed at addressing this growing concern.
Metabolic syndrome (MetS) is a condition that describes the clustering of risk markers that increase an individual's likelihood of developing chronic disease.Endnote 4 A number of leading chronic conditions have been shown to be associated with MetS. These include cardiovascular disease (CVD)Endnote 5, type 2 diabetes,Endnote 6 cancers,Endnote 7 and chronic kidney disease (CKD)Endnote 8.
The growing prevalence of obesity and sedentary lifestyles contributes to the prevalence of MetS.Endnote 9,Endnote 10,Endnote 11 While the pathogenesis of MetS may be attributed to obesity and metabolic susceptibility,Endnote 12 a variety of socioeconomic factors have also been shown to influence the prevalence of MetS. For example, Canadian adults with a postgraduate degree had half the odds of acquiring MetS compared with those who have completed high school (odds ratio [OR] = 0.45, 95% confidence interval [CI]: 0.25–0.81).Endnote 13 Ethnicity also affects observed prevalence rates (OR = 0.54, 95% CI: 0.4–0.73 in non-Hispanic Blacks relative to non-Hispanic Whites).Endnote 14 Considering differences based on ethnicity has resulted in a variety of official MetS definitions being sanctioned by international health authorities.Endnote 4,Endnote 15,Endnote 16 MetS has also been described as a progressive disorder; the several components of MetS tend to worsen over time and collectively contribute to an increased risk for chronic disease.Endnote 17
Hivert et al.Endnote 18 demonstrated the utility of MetS as a relevant public health tool. Using electronic health records to identify and track patients with MetS for future development of CVD and diabetes, they showed that patients with MetS had a higher incidence of these chronic conditions and incurred higher healthcare costs than did those patients without MetS.Endnote 18 This signifies an important role for MetS as a chronic disease indicator that could benefit individual health as well as healthcare costs and resources.Endnote 18 The limited availability of prevalence estimates derived from Canadian data to date has meant that international estimates are often used instead. It is therefore important to develop Canadian findings on MetS and its association with chronic conditions.
In this study, our aim was to
- estimate the prevalence of MetS in the Canadian adult population;
- examine the relationship between MetS, risk factors and chronic disease;
- and characterize the future risk of chronic diseases associated with MetS through measures of undiagnosed disease, as well as through 10-year projections for diabetes and CVD, using established prediction tools.
Methods
Data source
We used data from the 2007–2009 Canadian Health Measures Survey (CHMS).Endnote 19 This cross-sectional survey, conducted by Statistics Canada, recruited a representative sample of 5600 Canadians aged 6 to 79 years, which covers about 96.3% of the Canadian population. The survey used a mobile examination clinic to measure, for example, participants' blood pressure (BP) and serum factors. Information about current health status, socioeconomic variables, etc., was gathered through a general household interview.Endnote 19 Statistics Canada provides weights for each participant that capture the number of people represented by that participant in the population and account for non-response and the demographic distribution of the population. Additional information on sampling and estimations is described elsewhere.Endnote 20,Endnote 21
Study population
Some of the CHMS study participants (n = 2634) were asked to fast before the tests at the mobile examination clinic; we used data from this subsample in this study. The response rate for this subsample was 85.2%, which when combined with the overall response rate for the CHMS, makes the overall fasting subsample response rate 46.3%.Endnote 19,Endnote 20,Endnote 22 Pregnant women (n = 8) and individuals aged under 20 years (n = 933) were excluded from the analysis, leaving a study population of 1693 participants. For analyses using this subsample, Statistics Canada provided separate weights, based on the 2006 Census, for fasting participants, to ensure that analyses in this restricted subpopulation would remain representative of the entire Canadian population. These weighting factors account for nonresponse and for the demographic distribution of the country. Missing values were removed prior to analyses.
To test for potential selection bias as a result of various exclusion criteria, we performed a sensitivity analysis to compare the baseline demographic status of our study population with national-level estimates. Comparing our study population with recent Canadian estimates, we found that our study population (Table 1) showed similar estimates for age,Endnote 23 education,Endnote 24 gender,Endnote 25 ethnicityEndnote 26 and income,Endnote 27 indicating that it is representative of the general Canadian population.
TABLE 1
Characteristics of the study population (N = 1693)
| Characteristics |
N |
% |
95% CI |
|
|
| Sex |
| Women |
886 |
50.4 |
49.8–50.9 |
| Men |
807 |
49.6 |
49.1–50.2 |
| Age, years |
| 20–39 |
536 |
37.8 |
37.1–38.4 |
| 40–59 |
603 |
41.3 |
40.8–41.8 |
| 60–80 |
554 |
20.9 |
20.6–21.2 |
| Mean age (SE), years |
45.3 (0.2) |
|
|
| Cultural / ethnic background |
| Caucasian |
1441 |
84.3 |
74.2–94.4 |
| Non-Caucasian |
205 |
15.7Table 1 - Footnote E |
5.6–25.8 |
| Total household income, $ |
| ≤ 29 999 |
290 |
14.6 |
11.6–17.7 |
| 30 000–49 999 |
324 |
18.4 |
16.3–20.5 |
| 50 000–79 999 |
400 |
26.4 |
22.5–30.3 |
| ≥ 80 000 |
583 |
40.6 |
33.6–42.9 |
| Highest level of education |
| Less than secondary |
206 |
11.4 |
7.6–15.2 |
| Secondary graduate |
289 |
18.8 |
13.1–24.5 |
| Some post-secondary / post-secondary graduate |
1178 |
69.8 |
61.5–78.2 |
| Smoking status |
| Never smoked |
810 |
45.7 |
41.8–49.5 |
| Former smoker |
553 |
31.2 |
27.9–34.5 |
| Current smoker – daily or occasional |
325 |
23.1 |
20.6–25.6 |
| Leisure time physical activity |
| Active / moderately active |
800 |
44.3 |
37.2–51.5 |
| Inactive |
893 |
55.7 |
48.5–62.8 |
| BMI, kg/m2 |
| < 25 |
676 |
43.5 |
37.8–49.2 |
| 25–29 |
638 |
37.8 |
33.8–41.8 |
| ≥ 30 |
351 |
18.7 |
15.6–21.2 |
Key definitions
Metabolic syndrome
We used the revised National Cholesterol Education Program (rNCEP) Adult Treatment Panel III definition for MetS, which uses revised waist circumference criteria.Endnote 4 We also examined prevalence rates of MetS using the International Diabetes Federation (IDF) and Harmonized definitions.Endnote 15,Endnote 16
Undiagnosed and diagnosed chronic conditions
In the absence of any longitudinal data to determine whether individuals with MetS may develop chronic diseases with time, we determined whether participants may have had an undiagnosed condition. This is treated as a proxy measure for future chronic disease risk. Participants were deemed to have a particular condition undiagnosed if they said that they did not have the condition but had measurable physical attributes of the condition.
Diagnosed hypertension was based on a positive response to the question ''Do you have high blood pressure?'' or from self-reported use of specific medications (list available from the authors on request). Average systolic BP and diastolic BP were derived from an average of six blood pressure measurements.Endnote 22,Endnote 28,Endnote 29 We determined that individuals had undiagnosed hypertension if they reported no diagnosed hypertension but had BP readings above 140/90 mmHg (for either reading).
Diagnosed diabetes (type 2) was based on positive responses to the questions, ''Do you have diabetes?'' and ''Were you diagnosed with non-insulin dependent diabetes (type 2)?'' or from self-reported use of specific medications (list available from the authors on request).Endnote 22 As with BP, we determined that individuals had undiagnosed diabetes if they gave a negative response to questions about having physician-diagnosed diabetes but their fasting plasma glucose levels measured at 7.0 mmol/L or more. Individuals with type 1 diabetes were not included in the analysis.
Diagnosed CKD was based on a positive response to the question ''Do you suffer from kidney dysfunction or disease?''Endnote 22 Undiagnosed CKD was based on a negative response to this question plus either a low measured glomerular filtration rate (≤ 60 mL/min using the Modification of Diet and Renal Disease Study equationEndnote 30) or a high measured microalbumin to creatinine ratio (> 2.65 mg/mmol).
Diagnosed dyslipidemia was based on a positive response to the question ''Have you ever been told by a health professional that your blood cholesterol was high?''Endnote 22 Undiagnosed dyslipidemia was based on a negative response to this question plus the participant either meeting both the total cholesterol to high density lipoprotein (HDL) ratio (≥ 5.5 in men, ≥ 4.5 in women) and low density lipoprotein (LDL) criteria (≥ 3.5 mmol/L) or using appropriate medications (list available from the authors on request).
Descriptive variables
Analyses are described by sex, age (at clinic visit), education, ethnicity (self-reported cultural or racial group, not including Aboriginal populations) and total household income. Lifestyle factors include measured body mass index (BMI) and self-reported leisure time physical activity and smoking status.Endnote 19
Analysis
We undertook multivariate analyses using statistical software SAS Enterprise Guide 4.1 (Cary, NC, US).Endnote 31 National estimates were calculated with the CHMS weights for the subsample of the population who had fasted and were age-adjusted using Canadian Census data. We calculated variance estimates using Statistics Canada Bootvar software (Statistics Canada, Ottawa, ON) and followed their reporting guidelines. Horvitz-Thompson estimation was used to analyze statistical significance following a t distribution with 11 degrees of freedom.
We examined prevalence estimates using the frequency procedure on SAS Enterprise Guide 4.1, and adjusted for these as described for individual reported estimates in the Results section. OR estimates were calculated from logistic regression models and adjusted for age and sex, where mentioned. Ten-year cumulative incidence projections for type 2 diabetes were estimated using the Diabetes Population Risk Tool (DPoRT).Endnote 32
Originally developed using the National Population Health Survey, this prediction tool uses commonly collected survey data, such as self-reported estimates for health behaviours and sociodemographic factors, to predict the risk of developing incident physician-diagnosed diabetes. Sex-specific Weibull survival models were used to create DPoRT for individuals without diabetes mellitus, who are not pregnant and who are aged over 20 years. Predictive variables used in the model include age, sex, self-reported ethnicity, self-reported BMI, immigrant status (for women), education, smoking status and history of hypertension and heart disease, all of which were available for our analysis.Endnote 32
We used the lipid-based Framingham 10-year risk calculator to estimate the risk of a fatal general CVD event, defined as either coronary death, myocardial infarction, coronary insufficiency, angina, ischemic stroke, hemorrhagic stroke, transient ischemic attack, peripheral artery disease or heart failure. This risk prediction tool was originally created using data from the Framingham Heart Study and Framingham Offspring Study. Sex-specific Cox proportional hazards regressions were used to relate various risk factors to the incidence of fatal general CVD events. Mathematical CVD risk functions derived from this were then used in the development of the Framingham Risk Tool. Results are presented as high risk (≥ 20%) or intermediate and high risk (≥ 10%). The population subset for CVD projections was restricted to individuals aged 30 to 74 years who had no previous history of a CVD event.Endnote 33
Ethics approval
Approval to conduct our study was obtained from the Ottawa Hospital Research Ethics Board (Protocol # 20120767-01H) prior to commencement.
Results
The majority of the survey participants were Caucasian, physically inactive and former or current smokers. Most had at least some post-secondary education and an annual household income of more than $50 000. The mean age of the study population was 45 years, and the population was equally represented by each sex (Table 1).
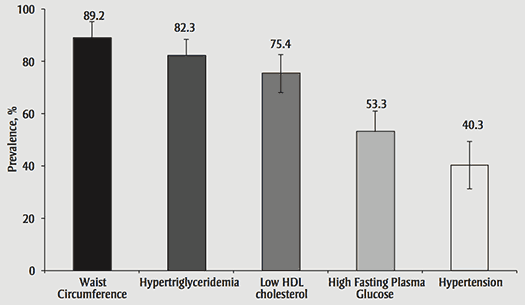
Participants were deemed to have MetS when they met three or more rNCEP MetS criteria, resulting in a crude prevalence of 15.5% and an age-adjusted prevalence of 14.9%. In the overall population, 34.9% had no MetS risk markers, whereas 29.5% had one and 20.2% had two. The most prevalent MetS risk markers among those identified as having MetS were waist circumference (89.2%), hypertriglyceridemia (82.3%), low HDL cholesterol (75.4%), high fasting plasma glucose (53.3%) and high systolic or diastolic BP (40.3%) (Figure 1).
FIGURE 1
Prevalence of different metabolic syndrome risk markers in individuals with metbolic syndrome, CHMS 2007–2009
[Click to enlarge]
[FIGURE 1, Text Equivalent]
Chronic Diseases and Injuries in Canada - Volume 34, no. 1, December 2013
FIGURE 1
Prevalence of different metabolic syndrome risk markers in individuals with metbolic syndrome, CHMS 2007–2009
The most prevalent MetS risk markers among those identified as having MetS were waist circumference (89.2%), hypertriglyceridemia (82.3%), low HDL cholesterol (75.4%), high fasting plasma glucose (53.3%) and high systolic or diastolic BP (40.3%).
Abbreviation: HDL, high density lipoprotein.
The rNCEP estimates were compared to prevalence estimates based on the IDF and Harmonized definitions, both of which resulted in significantly larger prevalence estimates (crude prevalence: IDF = 23.1%, Harmonized = 19.6%; age-adjusted prevalence estimates: IDF = 22.3%, Harmonized = 19.1%) (Table 2).
TABLE 2
Metabolic syndrome prevalence and odds ratios according to population characteristics, CHMS 2007–2009
| Definitions |
Prevalence |
Odds Ratios |
| % |
95% CI |
p value |
OR |
95% CI |
|
|
| rNCEP ATP III |
| Crude |
15.5 |
12.0–19.0 |
— |
|
|
| Adjusted |
14.9 |
13.3–16.6 |
|
|
|
| IDF |
| Crude |
23.1 |
20.4–25.8 |
< .001 |
|
|
| Adjusted |
22.3 |
20.4–24.3 |
|
|
|
| Harmonized |
| Crude |
19.6 |
15.9–23.2 |
< .001 |
|
|
| Adjusted |
19.1 |
17.3–20.9 |
|
|
|
| Characteristics |
| Overall population |
| SexTable 2 - Footnote a,Table 2 - Footnote b |
| Men (ref) |
14.5 |
10.4–18.6 |
— |
1 |
— |
| Women |
16.5 |
12.6–20.3 |
.25 |
1.12 |
0.87–1.42 |
| EthnicityTable 2 - Footnote a,Table 2 - Footnote b,Table 2 - Footnote c |
| Caucasian (ref) |
15.5 |
12.1–18.8 |
— |
1 |
— |
| Non-Caucasian |
16.6Table 2 - Footnote E |
5.4–27.7 |
< .001 |
2.66 |
1.29–5.45 |
| Men |
| AgeTable 2 - Footnote b |
| 20–39 (ref) |
8.0Table 2 - Footnote E |
4.4–11.5 |
— |
1 |
— |
| 40–59 |
14.5Table 2 - Footnote E |
6.7–22.4 |
.05 |
1.48 |
0.67–3.26 |
| 60–80 |
26.9 |
21.3–32.5 |
.012 |
3.33 |
2.07–5.34 |
| Smoking statusTable 2 - Footnote a,Table 2 - Footnote b |
| Current |
6.6Table 2 - Footnote E |
2.0–11.1 |
.01 |
0.65 |
0.23–1.86 |
| Former |
24.1 |
15.5–32.7 |
.12 |
1.54 |
0.66–3.61 |
| Never (ref) |
11.4Table 2 - Footnote E |
5.6–17.3 |
— |
1 |
— |
| LTPATable 2 - Footnote a,Table 2 - Footnote b |
| Active (ref) |
12.0 |
8.5–15.6 |
— |
1 |
— |
| Inactive |
16.9Table 2 - Footnote E |
10.0–23.9 |
.001 |
1.39 |
0.69–2.78 |
| BMI, kg/m2 Table 2 - Footnote a |
| < 25 (ref) |
—Table 2 - Footnote F |
— |
— |
1 |
— |
| 25–29 |
15.8 |
10.4–21.2 |
< .001 |
—Table 2 - Footnote F |
— |
| ≥ 30 |
38.6 |
25.5–51.8 |
< .001 |
—Table 2 - Footnote F |
— |
| Women |
| AgeTable 2 - Footnote b |
| 20–39 (ref) |
—Table 2 - Footnote F |
— |
— |
1 |
— |
| 40–59 |
18.7Table 2 - Footnote E |
11.7–25.7 |
.003 |
3.67 |
1.20–11.17 |
| 60–80 |
31.5 |
24.3–38.6 |
< .001 |
7.43 |
2.62–21.05 |
| Smoking statusTable 2 - Footnote a,Table 2 - Footnote b |
| Current |
21.1 |
13.6–28.5 |
.71 |
3.15 |
1.63–6.07 |
| Former |
21.3Table 2 - Footnote E |
10.8–31.8 |
.38 |
2.06 |
0.93–4.59 |
| Never (ref) |
11.0 |
8.7–13.3 |
— |
1 |
— |
| LTPATable 2 - Footnote a,Table 2 - Footnote b |
| Active (ref) |
10.5Table 2 - Footnote E |
6.6–14.5 |
— |
1 |
— |
| Inactive |
20.2 |
15.4–25.0 |
< .001 |
1.76 |
1.13–2.73 |
| BMI, kg/m2 Table 2 - Footnote a |
| < 25 (ref) |
—Table 2 - Footnote F |
— |
— |
1 |
— |
| 25–29 |
22.9 |
16.1–30.0 |
< .001 |
—Table 2 - Footnote F |
— |
| ≥ 30 |
43.2 |
34.2–52.2 |
< .001 |
—Table 2 - Footnote F |
— |
The prevalence of MetS varied by age group, but the difference by sex for each age group was not statistically significant (Figure 2). Variation occurred according to smoking status as well, although these patterns varied by sex (Table 2). On the other hand, ethnic background significantly influenced prevalence rates, with people of non-Caucasian origin having a higher prevalence than those of Caucasian origin. For both sexes, a high BMI and being physically inactive were significantly associated with a higher prevalence of MetS.
FIGURE 2
Prevalence of metabolic syndrome by gender and by age group, CHMS 2007–2009
[Click to enlarge]
[FIGURE 2, Text Equivalent]
Chronic Diseases and Injuries in Canada - Volume 34, no. 1, December 2013
FIGURE 2
Prevalence of metabolic syndrome by gender and by age group, CHMS 2007–2009
The prevalence of MetS varied by age group, but the difference by sex for each age group was not statistically significant.
Source:Canadian Health Measures Survey, 2007–2009, clinic dataset.
Abbreviation:CHMS, Canadian Health Measures Survey.
Note:For all reported age groups, except for ages 60–74 years, estimates should be interpreted with caution (coefficient of variation: 16.6%–33.3%). Estimates that could not be reported (coefficient of variation: > 33.3%) were not included in the figure.
The odds of MetS varied according to participant characteristics, and was significantly associated with being non-Caucasian and older (Table 2). Other characteristics were also significant, although this varied based on sex. For example, the odds of MetS was significantly associated with being a current smoker in women but not in men.
We examined the prevalence of chronic conditions across three population groups: the overall population, individuals with obesity (BMI ≥30 kg/m2) and individuals with MetS. Undiagnosed disease was more prevalent in those with MetS compared with those with obesity or the overall study population for all conditions examined, and was most prominent for dyslipidemia (28.3% vs. 18.5% and 10.0%, respectively) (Table 3). Note that the rate of undiagnosed diabetes was more than five times higher in those with MetS than in the overall population (6.0% vs. 1.1%, p = .009; interpret with caution).
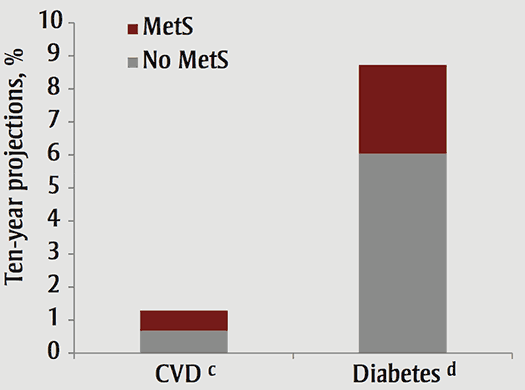
We estimated the future burden of type 2 diabetes and CVD that can be attributed to MetS using existing algorithms. The mean 10-year predicted risk of diabetes in individuals with MetS, as opposed to those without, is 18.0% (95% CI: 15.3–20.7) versus 7.1% (95% CI: 6.2–8.1). The proportion of Canadian adults anticipated to develop diabetes between 2007 and 2017 is thus 8.7% (95% CI: 7.5–9.9) (Figure 3). Similarly, the mean predicted risks for fatal CVD are 4.1% (95% CI: 2.3–6.0; interpret with caution) vs. 0.8% (95% CI: 0.6–1.0). The risk of CVD can be further analyzed as being high, that is, a 20% or higher risk of a CVD event in 10 years, or as intermediate to high, a 10% to 20% CVD risk in 10 years. The proportion of Canadian adults with MetS with a high risk of a CVD event is 6.81% (95% CI: 3.2–10.4, p = .004 relative to those without MetS; interpret with caution). Furthermore, the proportion of Canadian adults at intermediate to high risk of a CVD event is 8.9% (95% CI: 4.3–13.6; interpret with caution) in those with MetS, compared with 2.0% (95% CI: 1.3–2.7, p = .008) in those without MetS.
FIGURE 3
Ten-year projections for the cumulative incidence of diabetesa and mean percent risk of a fatal CVDb event in individuals with or without MetS,c CHMS 2007–2009
[Click to enlarge]
[FIGURE 3, Text Equivalent]
Chronic Diseases and Injuries in Canada - Volume 34, no. 1, December 2013
FIGURE 3
Ten-year projections for the cumulative incidence of diabetesa and mean percent risk of a fatal CVDb event in individuals with or without MetS,c CHMS 2007–2009
We estimated the future burden of type 2 diabetes and CVD that can be attributed to MetS using existing algorithms. The mean 10-year predicted risk of diabetes in individuals with MetS, as opposed to those without, is 18.0% (95% CI: 15.3–20.7) versus 7.1% (95% CI: 6.2–8.1). The proportion of Canadian adults anticipated to develop diabetes between 2007 and 2017 is thus 8.7% (95% CI: 7.5–9.9). Similarly, the mean predicted risks for fatal CVD are 4.1% (95% CI: 2.3–6.0; interpret with caution) vs. 0.8% (95% CI: 0.6–1.0). The risk of CVD can be further analyzed as being high, that is, a 20% or higher risk of a CVD event in 10 years, or as intermediate to high, a 10% to 20% CVD risk in 10 years. The proportion of Canadian adults with MetS with a high risk of a CVD event is 6.81% (95% CI: 3.2–10.4, p = .004 relative to those without MetS; interpret with caution). Furthermore, the proportion of Canadian adults at intermediate to high risk of a CVD event is 8.9% (95% CI: 4.3–13.6; interpret with caution) in those with MetS, compared with 2.0% (95% CI: 1.3–2.7, p = .008) in those without MetS.
Source:Canadian Health Measures Survey, 2007–2009, clinic dataset.
Abbreviations:CVD, cardiovascular disease; CHMS, Canadian Health Measures Survey; CI, confidence interval; MetS, metabolic syndrome.
Note:Given the identified population prevalence of MetS among Canadian adults (85.1% without MetS, 14.9% with MetS), this suggests a projected 10-year risk of a fatal CVD event as 1.29%, and a projected 10-year cumulative incidence of diabetes as 8.7% (95% CI: 7.5–9.9).
a Estimated using the Diabetes Population Risk Tool (DPoRT).Endnote 32
b Calculated using the lipid-based Framingham 10-year risk calculator.Endnote 33 The population subset for CVD projections was restricted to adults aged 30–74 years who have no previous history of a CVD event.
c Projections: With MetS = 4.1% (95% CI: 2.3–6.0), p < .01; without MetS = 0.8% (95% CI: 0.6–1.0), p < .01.
d Projections: With MetS = 18.0% (95% CI: 15.3–20.7), p < .01; without MetS = 7.1% (95% CI: 6.2–8.1), p < .01.
Discussion
Prevalence of metabolic syndrome
Comparing prevalence for MetS using the same rNCEP definition, the age-adjusted rate in Canada is less than half that reported in the United States (14.9% vs. 34.4%),Endnote 14 but similar to previously published findings for the Canadian population.Endnote 34 Using newly suggested IDF definitions, which take into account variations in waist circumference for different ethnic groups, or the Harmonized definition, the age-adjusted prevalence of MetS in Canada is higher than with the rNCEP (22.3% and 19.1%, respectively), showing that the choice of definition for MetS does appear to matter.
We chose to use the rNCEP definition for MetS in our study to facilitate comparisons with previously published epidemiological data.Endnote 14 The rNCEP definition was reasonably accurate in representing the ethnic composition of our study population (84% Caucasian; Table 1). While sample size limitations did not allow us to explore variations in MetS prevalence based on self-reported ethnic origin, when this information was used to apply the IDF definition of MetS, it appears as though more people are being included as having MetS.Endnote 15
Risk factors and metabolic syndrome
Our findings indicate that the prevalence of MetS in Canada is associated with age, ethnicity, BMI and leisure time physical activity. Older age was significantly associated with MetS, but the patterns of prevalence varied by age and sex. Prevalence was higher in men than in women in the 30- to 39-year age group. Thereafter, the prevalence of MetS increases steadily in women, exceeding the prevalence of MetS in men, from age 40 through 60 to 74 years, after which time it levels off. In men, the steady increase in prevalence seems to occur after the age of 40. TjepkemaEndnote 35 suggested that this transition reflects the marked increase in rates of obesity in men after age 45 years. In the same study, TjepkemaEndnote 35 also showed that obesity rates increase steadily in women until age 65 years. The changes in prevalence that we observed align with reported increased rates of MetS in peri- and post-menopausal women.Endnote 36
The odds of MetS were significantly higher in non-Caucasian individuals, and we found greater risk of MetS in non-Caucasian Canadians than was found in Mexican American and non-Hispanic white individuals in the United States.Endnote 14 In addition to Hispanic and African Canadians, we included Filipino, Chinese, South Asian, Arab and other populations in our study. It is possible that the inclusion of these additional groups may account for the difference in the odds of MetS by ethnicity between the two studies. Previous findings using the rNCEP definition also showed higher prevalence rates in some of the ethnic groups included in our study relative to our overall population.Endnote 37,Endnote 38
Our results indicate that being physically active lowers the odds of MetS compared with being inactive, although this lower risk is only statistically significant in women. Our analysis clearly shows that rates of overweight and obesity are high in adults, with a prevalence of almost 57%. This is of concern given the close association of obesity with MetS, as well as with pre-diabetes.Endnote 39
MetS is commonly associated with pre-diabetes, wherein individuals have elevated plasma glucose levels as well as systemic inflammation. It is also associated with characteristics such as pro-thrombotic state and dyslipidemia, which may account for its link to cardiovascular risk.Endnote 40 The increased risk of type 2 diabetes and of a fatal CVD event in individuals with MetS is thus not surprising, given the research demonstrating these associations.Endnote 5,Endnote 41 The proportion of individuals identified as being at risk of developing diabetes in the next 10 years, relative to those without MetS, indicates the role of MetS as a potential chronic disease indicator. These findings are corroborated by a 2010 study that estimated risk of diabetes for Canadians at 8.9%.Endnote 42 When considering the projections for CVD, which estimate the risk of a fatal event, the concern is clear.
We need to be aware of a possible overlap in definitions for chronic disease risk factors and for MetS. In the case of dyslipidemia, this overlap may contribute to the high rates of abnormal lipid levels in those with MetS. The risk marker of low HDL cholesterol was prevalent in 75% of the population with MetS, but it is worth noting that the definition of dyslipidemia was based on a high total cholesterol to HDL cholesterol ratio combined with elevated LDL levels. Similarly, MetS is defined based on waist circumference, not BMI, which makes both populations distinct but potentially related.
Public health impact of metabolic syndrome
Independent of race/ethnicity, age, sex and health status, evidence shows an increased risk of developing certain chronic diseases with each additional MetS risk marker.Endnote 41 ReavenEndnote 43 suggests that even though an individual may not meet the number of risk markers (3 or more) necessary to be diagnosed with MetS, they may still be at risk of future disease and should therefore not be overlooked. We found that 50% the study population had one or two MetS risk markers, by no means a small proportion.
We compared MetS with a well-studied chronic disease risk factor, obesity. Our findings demonstrated a higher prevalence of chronic disease in individuals with MetS compared with those with obesity (shown in Table 3), although the differences were not statistically significant. A previous study has described MetS as more predictive of future disease than obesity alone.Endnote 44 The greater association between chronic disease and MetS in our study may, therefore, further signify a public health utility for MetS as a key indicator of disease risk.
Limitations
Working with the CHMS data, sample size proved to be a limiting factor in providing reportable estimates for key covariates, such as for sociodemographic characteristics, and limited the scope of the study to a national viewpoint, since it is not built to produce regional estimates. Further, the use of self-reported information for activities such as smoking or leisure time physical activity may have proven to be a limitation. Due to the lack of pertinent variables to measure undiagnosed diabetes, our definition is limited in scope and interpretations should be made with caution. To limit the effects of confounders, BMI, age and sex were all controlled for in multivariate analyses. The removal of missing values may have contributed to a downward bias in our diabetes risk projections since the proportion of missing values for BMI tends to be higher among females. However, since missing values for women only represent a small proportion of all responses for BMI among females, their removal should not skew our results.
Conclusion
MetS represents a condition that is strongly associated with factors such as obesity, ethnicity and leisure time physical activity. Our study demonstrates the differential pattern by which MetS affects specific subpopulations and indicates an association between MetS and major chronic conditions.Endnote 45 Since Canadians with MetS have significantly higher rates of undiagnosed chronic diseases than the overall population and higher predicted rates of future chronic disease, it may be of value for clinicians to include MetS, in addition to obesity, as an indicator for chronic disease and useful for public health policy-makers to consider MetS when directing preventive population health efforts.
Acknowledgements
Deepa P. Rao is supported by a Frederick Banting and Charles Best Doctoral Research Award from the Evidence-Informed Healthcare Renewal Initiative of the Canadian Institutes of Health Research (CIHR) Knowledge Translation Branch. Dr. D. Krewski holds a Natural Sciences and Engineering Research Council of Canada (NSERC) Industrial Research Chair in Risk Science.
The Canadian Health Measures Survey was conducted by Statistics Canada in partnership with Health Canada and the Public Health Agency of Canada with funding from the Canadian Federal Government.
We thank Dr. Michael J. Pencina, of Boston University, for providing us with the SAS-based macro to calculate the CVD risk projections and Dr. Laura Rosella and Mr. Michael Lebenbaum, of Public Health Ontario, for helping us use the DPoRT algorithm for diabetes risk projections.
References