Expert Advisory Group Report 3: Toward a world-class health data system
Download in PDF format
(2.25 MB, 35 pages)
Organization: Public Health Agency of Canada
Date published: 2022-05-03
Preface
Since December 2020, I have had the honour of leading this Expert Advisory Group to provide advice to governments on a Pan-Canadian Health Data Strategy. We have published two reports, authored editorials, and conducted many panels in the interest of advancing health data collection, access, sharing and use that improves public health event management and achieves equitable health outcomes for all people in Canada.
I am heartened that the recognition of the value of health data in Canada is growing, as demonstrated by references in the Speech from the Throne, the Annual Report from the Chief Public Health Officer and the mandate letter for the Government of Canada's Minister of Health.
In our first report, we reviewed over 60 years of reports on improving health data use, reflected on systemic barriers that prevent effective data collection, access, sharing and use, and drew attention to Canada's health data foundation. We noted that despite repeated attempts, there have been failures as a nation to deliver what Canadians deserve. We therefore suggested a bold vision to deliver a learning health system that benefits all persons in Canada guided by common principles that drive the responsible use of health data for the public good. Achieving such a vision will required sustained collective action on the part of many and will require substantial commitment on the part of leaders across the country.
Our second report advised that the health system is evolving from a focus on acute care supported by paper systems to a continuum of care supported by digital systems and that policies and governance need to catch up to this reality. Further, the report suggested that substantial coordinated investment in governance, policy, interoperability, data literacy and public trust is needed to strengthen the health data foundation.
This third and final report of the Expert Advisory Group builds on those recommendations and provides both aspirational and pragmatic advice for developing a world-class, person-centred health data system. This report highlights the excellence and success that parts of Canada have achieved with health data and the opportunities that would come from a culture of collaboration and stewardship that prioritizes scale and re-use.
On a personal level, I would like to thank members of the Expert Advisory Group for their tireless dedication and the Public Health Agency of Canada that supported the Expert Advisory Group in its deliberations.
Our hope is that this report will catalyze practical action for lasting and meaningful change. We recognize that the fundamental challenge we face is not one of technology, rather it is one of culture. We must take the disparate responsibilities for health data stewardship and orient them in a way that moves us toward a more collaborative and person-centred system. This will take time, and we must start now – to shape the future that we want rather than react to change that is brought on by others or new health threats.
Objectively, Canada has had one of the world's best responses to the pandemic. Major contributors to success have been the culture of trust and sense of community amongst Canadians alongside the heroics demonstrated by many health professionals. But we know we could have done much, much better in our response, particularly if we had more timely, comprehensive data.
Investing in a world-class health data system will make Canada better prepared for future public health events, help clinicians deliver excellent care, accelerate Canadian research, empower people to achieve their health objectives, and drive equitable outcomes for all. We have far to go. We must start the journey now. Together.
Dr. Vivek Goel, CM
Chair, Expert Advisory Group, Pan-Canadian Health Data Strategy
Table of contents
- Preface
- Executive summary: Toward a world-class health data system
- 1. Imperative for a Pan-Canadian Health Data Strategy
- 2. Approach for a Pan-Canadian Health Data Strategy
- 3. Pan-Canadian Health Data Strategy recommendations
- a. A world-class health data system guided by common principles
- b. Support for Indigenous data sovereignty
- c. Governance: Accountable governance for a learning health system
- d. Trust: Meaningful engagement and communication with the public and stakeholders
- e. Policy: Frameworks for health data stewardship and policy
- f. Interoperability: Common data standards and data architecture
- g. Literacy: Data literacy and capacity
- 4. Mobilizing change: The first year
- 5. Conclusion: The first step on a journey of a thousand miles
- Glossary
- Annex A: Summary of recommendations and immediate actions
- References
- Members of the Expert Advisory Group
- Contact
"… Lead our renewed commitment to work in partnership with and increase funding to provinces and territories to strengthen our universal public health system…advance an integrated, comprehensive and patient-centric strategy, harnessing the full potential of data and digital systems… expediting work to create a world-class health data system that is timely, usable, open-by-default, connected and comprehensive."
Excerpts from Minister of Health mandate letter, Government of Canada, December 2021
Executive summary: Toward a world-class health data system
A world-class health data system requires a strong foundation. This foundation supports the collection, access, sharing and use of health data in a timely and trusted manner for the benefit of all persons in Canada.
The last two years of the COVID-19 pandemic have demonstrated the value of a strong foundation – common standards, functions, and capabilities – to inform public health advice, deliver health services, advance research and foster virtual care. Sadly, the pandemic has also shone a light on long-standing problems that weaken the foundation: the systemic fragmentation of health data, ineffective pan-Canadian health data governance and antiquated policies that have prevented timely data sharing. Had a stronger health data foundation been in place, health inequities experienced during the pandemic would have been reduced and lives would have been saved.
Strengthening the health data foundation will require collaboration and considered effort toward a common goal. That common goal should be to establish a learning health system in Canada. In a learning health system, connected data support insights that drive evidence-informed decisions. These data and insights are embedded in health programs, services, surveillance programs and care delivery. When harnessed effectively, they can produce continual improvement and better and equitable outcomes for all.
Bringing a learning health system to life will require collaboration
Bringing a learning health system to life will require collaboration among jurisdictions (federal, provincial, and territorial governments) and stakeholders (including health authorities, providers, and researchers) to demonstrate trustworthiness, earn trust, and grow capacity and capability to use data better. Investments in a learning health system must be guided by a common set of principles that define a common approach to person-centric health data design and use. These are outlined in a Canadian Health Data Charter. When adopted, this Charter would guide partners on how to act together to optimize health data governance, policy, workflow and technology harmonization under a Pan-Canadian Health Data Strategy (the Strategy). This common approach is needed to deliver equitable, quality, integrated health programs and services, including public health surveillance, health system evaluation, human resource planning, clinical care and research.
Implementation of the Strategy by jurisdictions would be advised by a competency-based Health Information Stewardship Council (Council) and facilitated by one or more representative Learning Health System Table(s) (LHS Table(s)), accountable to the Federal/Provincial/Territorial (FPT) Conference of Deputy Ministers of Health. The Council and LHS Table(s) would support data sovereignty of First Nations, Inuit, and Métis Nation and ensure that their representative bodies and/or governments are appropriately engaged. The LHS Table(s) would work with the Council to establish integrated roadmaps to implement the learning health system and secure investment and funding for the strategy. For transparency, the Council would communicate progress on health data foundation improvements to the public.
The Council would be empowered to leverage existing expertise, convene working groups as necessary and ensure ongoing involvement of diverse perspectives. The Council would guide and advise on implementation of the Strategy, including work on:
- Creating a common policy framework for data sharing;
- Implementing interoperable data standards;
- Developing common person-centric data architecture;
- Improving health data literacy; and
- Producing sound and actionable research and analysis.
Advancing a learning health system will be bolstered by pan-Canadian efforts to improve public health surveillance and advance digital health and virtual care as critical facets of Canadian health systems. Given the common themes of interoperability and data flow across these streams of work, these must be tightly aligned to capitalize on synergies.
Irreparable fragmentation of health data will harm individuals and Canada
Failure to collaborate across Canada to build a learning health system risks continued escalation of health care costs, underperformance of health services and poor health outcomes including: avoidable illness and death, low levels of innovation, perpetuation of health inequities, and ineffective responses to future public health threats. At an extreme, there is a risk of irreparable fragmentation of health data that will harm individuals, communities, and all of Canada due to unaligned and often competing interests that may erode the common values and principles that have defined our health systems to date.
Recently, strong collaboration across jurisdictions has been demonstrated in response to the pandemic and advancement of virtual care. The journey toward a learning health system will require an unprecedented level of collaboration well beyond what has been demonstrated in the last two years. Advice in this report will help health data partners work collaboratively on strategies that can deliver a world-class health data system.
Based on past experience, we expect a great deal of wrangling and squabbling over funding and authority between jurisdictions, turf protection between organizations, and concerns from professional groups. Rather than continuing such self-defeating exercises, let us put energy into collaboration and collective action, and deliver what Canadians expect and deserve.
1. Imperative for a Pan-Canadian Health Data Strategy
There have been many attempts at advancing a health data strategy for Canada, which have had limited success and failed to realize their intended goals. These failures have led to slower public health responses and contributed to excess mortality during and between major public health events.
The COVID-19 pandemic has shone a spotlight on the real costs of these failures. The inability to integrate data in real-time across hospitals, primary care, testing, vaccination, and genomics (among others) impair insights to measure the efficacy of vaccines, track the emergence of variants of concern, and mount efforts to address health inequities. While tactical responses are in place to address some of these concerns, the root causes impeding data collection, sharing, access and use persist, and will continue to impact public health negatively, including the ability to track complications from the pandemic such as long-COVID and mental health impacts. While Canada emerges from the Omicron wave of the pandemic and public health restrictions are eased, it is understood that the COVID-19 pandemic is far from over, and the need for robust public health surveillance systems is as great as ever.
The Expert Advisory Group (EAG) was struck in December 2020 to provide advice on the development of a Pan-Canadian Health Data Strategy. While the EAG formation was catalyzed by health data issues identified during the pandemic, its review of 60 years of efforts to improve health data management showed that core barriers must finally be addressed. These persistent barriers prevent meaningful access to individuals' own data, hamper providers' ability to use comprehensive data to provide the best care, and prevent real-time analytics on collective data that could inform better evidence-informed insights and decisions.
Health care and public health information needs are strongly linked
The EAG recognized that health care and public health information needs are strongly linked. Understanding the course and impacts of the pandemic requires not only data generated by public health, but also data from across all settings of the health care sector, and beyond. Integrating these data streams is only possible through a common plan to create a robust health data foundation – one that supports a learning health system that uses real-time data to improve health outcomes while also enabling data collection and use that improve public health services and population health outcomes.
Harnessing the Potential of a Pan-Canadian Strategy
Ready access to timely and high-quality health data that are used for continuous improvement of individual, community and population health outcomes is the bedrock of a world-class health data system. Bringing Canada's health data systems into the digital age will require more than simple integration and technology improvement – it will require comprehensive change across all health data foundation pillars of governance, policy, interoperability, data literacy and public trust.
As such, a Pan-Canadian Health Data Strategy (the Strategy) would be the catalyst to mobilize:
- Investments in health information that are based on an agreed common and collective vision for health data in Canada;
- Ongoing and meaningful involvement of First Nations, Inuit, and Métis peoples to ensure that rights- and distinctions-based expectations and needs are met;
- Ongoing and meaningful public involvement to ensure data policies meet needs and expectations;
- Expert data stewardship so that data sharing is supported and advanced according to laws and ethics;
- Common public policy and data standards that promote sharing, scaling and spreading of best practices, productivity and technological innovations;
- Interoperable health data systems that are principle-based across jurisdictions and stakeholders; and
- Health data and digital health literacy among the health workforces, health sector managers, leaders, and general public to grow trustworthiness, trust, capacity and capability to deliver the vision.
The Strategy must be implemented broadly, with efforts from jurisdictions (i.e. federal, provincial and territorial governments), stakeholders (including health authorities, providers, and researchers), First Nations, Inuit, and Métis peoples, and the public. The changes brought about by implementing this Strategy would help empower all people in Canada to better achieve their individual and collective health objectives. It would also support effective and intelligent health workforce utilization while allowing continuous improvement in health care and robust, informed public health responses. Implementation would identify new opportunities for health system innovation, evaluation, planning, and research. Commitment and funding for the Strategy must be significant, sustained and strongly coordinated, through ongoing federal, provincial, and territorial investments to achieve its full potential.
Collaboration and Commitment for Equitable Health Outcomes
Health is a shared responsibility between federal, provincial and territorial (FPT) governments, and is executed in accordance with the principles of the Canada Health Act. These principles are a signature aspect of national identity for most Canadians. As people receive services within and across jurisdictional borders, there is a reasonable expectation that the fundamentals of health care are the same. While the Canada Health Act requires portability of coverage, there is also a need to ensure portability of data, to ensure continuity of evidence-informed care throughout an individuals' lifetime.
The Canada Health Act allows for variations in health and public health service delivery across Canada. Variations are a strength if they reflect local needs and are leveraged as learning opportunities by sharing data, insights, knowledge and practices. A learning health system values these variations by enabling access to comprehensive high-quality health data for continuous improvement of care and health system effectiveness. The ability to scale and spread continuous improvements relies on consistent data standards so that digital tools and analytical insights are effectively produced and can be more easily shared to drive equitable outcomes. As a result, innovation and invention thrive in a learning health system.
Cooperation between jurisdictions, stakeholders, and First Nations, Inuit, and Métis Nation representative bodies is necessary to optimize learning health systems to: (1) ensure that data and insights are available for individuals and their circle of care wherever they are and however they move within Canada; (2) minimize health inequities and achieve the best health outcomes possible; and (3) drive innovation, public health surveillance and practice, and system productivity and effectiveness through collective data analysis and use. This cooperation would also help Canada to be more effective in collaborating, contributing, and benefiting from international experiences and partnerships through common, up-to-date and agreed-upon health data standards.
2. Approach for a Pan-Canadian Health Data Strategy
There are several issues that must be addressed by implementing a Pan-Canadian Health Data Strategy with appropriate governance and accountability:
- Duplicative and competitive activities: At this point there is little formal coordination among initiatives to improve health data collection, access, sharing, and use. Some of these efforts are duplicative and may move jurisdictions in different directions that fragment data and prevent learning.
- Mis-aligned priorities and specialized agendas: Health data priorities often prioritize solutions that make sense for individual jurisdictions, but do not scale. This will lead to systemic health inequities as data capabilities advance.
- No common vision for health data across jurisdictions: Past strategies have been incoherent without a unifying goal for health data. Governance structures have been incented to deliver short-term success without priority for long-term benefits within and across jurisdictions and for all people in Canada.
- Fragmented incentives and measurements: With a common vision, incentives can be aligned and organizations held accountable for following through on the Strategy. Transparency is an essential component of ensuring success when collective action by diverse entities is required.
Focus is required to achieve an agreed common state and implement it. That focus would be bolstered with a realistic assessment of the current state to identify urgent gaps and build a comprehensive roadmap – a strategic plan that defines a desired outcome and includes the major milestones needed to reach it.
Roadmaps provide incremental benefits toward a common goal
When roadmaps are integrated, jurisdictions can work together on areas of common interest, spread innovation, increase productivity and lower cost of implementation while providing incremental benefits toward a common goal.
Collective Impact for a Health Data Strategy
The Strategy would need to span multiple electoral and capital funding cycles to achieve a world-class health data system. A robust governance ecosystem is needed to maintain momentum, address persistent barriers that have prevented progress, and solidify partnerships to leverage expert and jurisdictional-based insights.
Historical models have not worked. They have either been too centralized without buy-in from stakeholders or have been too decentralized without incentives to adopt consistent standards and practices. While governance is needed for the Strategy, there is a concern that the substantial governance in place now – with multiple uncoordinated entities – will fail to deliver the outcomes that Canadians expect.
This report recommends a Collective Impact model for implementation of this strategy. In a Collective Impact model, there is a common agenda (vision and standards); shared measurement and strong backbone (governance), and mutually reinforcing activities and continuous communication (trust, policy, interoperability, literacy).
Applying a collective impact model would bring together expertise with jurisdictional authority and funding necessary to drive a Pan-Canadian Health Data Strategy that achieves benefit for all people in Canada.
3. Pan-Canadian Health Data Strategy recommendations
This report includes ten recommendations for health data partners to implement a person-centred, digital-age, interoperable health data foundation that can meet today's needs and be nimble enough to respond to those of the future.
These recommendations are for all jurisdictions – federal, provincial, and territorial governments. Governance and implementation of the Strategy must involve First Nations, Inuit, and Métis Nation representative organizations to support Indigenous data sovereignty and implementation of Indigenous data strategies.
These recommendations include a progressive vision, principles and significant, coordinated actions on multiple fronts. It is through person-centric and community-engaged collaborations that the basic goal of health data enabling us to work smarter – rather than working harder – would benefit everyone in Canada.
Focus: Fostering a person-centric learning health system in Canada
Individual patients want the best care from health providers. With the increasing complexity of care, often associated with aging, patients have many different health care encounters over time, including with primary care providers, specialists, hospitals, pharmacists, and laboratories. Ideally, all providers for an individual would have timely access to health data organized around that individual – that is "person-centric" data.
At present, data are typically collected and held by various health care providers or custodians typically with incompatible software databases lacking standards for sharing data among members of a care team – in short, this is "provider-centric" data. Data held and arranged in this way results in numerous phone calls, faxes and re-telling of health histories – and still health providers rarely have a full understanding of their patients' histories of health care encounters and outcomes. This leads to duplicative services, missed diagnoses, frustrated patients trying to access appropriate care, and inferior overall health outcomes.
When data are organized around the individual, data follow the patient, thereby obligating participating organizations, and jurisdictions to harmonize policy, technology and workflow that has traditionally obstructed data flow. A by-product of such policy, workflow and technology harmonization will be the capacity to pool health data for the purposes of improving the management and delivery of individuals' health care, the many facets of public health and research and analysis to benefit communities, and promote innovation. A learning health system designed around person-centric data will have better safety, quality, and efficiency in addition to providing greater confidence for individuals and their health providers.
a. A world-class health data system guided by common principles
Recommendation 1: Jurisdictions endorse a vision that "by 2030, all people living in Canada will benefit from a fully integrated and continuously optimized learning health system" and that the implementation will be guided by common principles in a Canadian Health Data Charter.
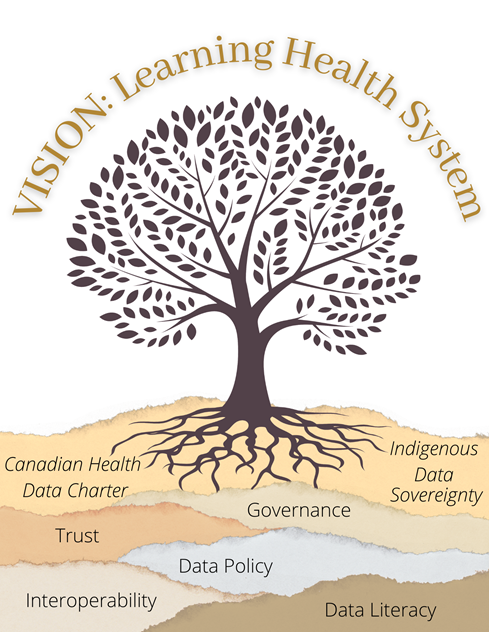
Figure 1: Text description
The image shows the roots of the tree going into the ground, the ground has different layers. Each layer represents a part of the Pan Canadian Health Data Strategy. The layers are labelled Canadian Health Data Charter; Indigenous Data Sovereignty; Trust; Governance; Data Policy; Data Literacy; Interoperability.
A common vision is essential to act as the 'north star' for navigating toward the future we want to see for health data. When agreed to by health data partners, a vision can help to align resources, prioritize budgets and focus investment. In this vision,
- All people living in Canada includes all persons in Canada with particular focus on inclusion: health equity, marginalized populations, and support for First Nations, Inuit and Métis peoples to achieve their desired health outcomes;
- Fully integrated and continuously optimized means that meaningful and comprehensive data necessary for health systems to learn and be responsive to change are fluidly available – when and where they are needed – for individual outcomes, clinical care, effective public and population health interventions, and for actionable research and analysis; and
- A learning health system drives better outcomes for individuals and populations based on insights gained from the accumulated experiences captured and analyzed via the shared and pooled use of personal health data; this system is then able to improve health care quality, planning and public health response, and health-related policies and systems are able to make evidence-informed decisions for desired outcomes.
With the tools now available, the health data in a learning health system would not be collected in a single pan-Canadian database. Rather, appropriate governance, policy, architecture, and accountability mechanisms support data held in different interoperable databases, where data are appropriately and securely accessible in real-time for approved and transparent purposes, while securely maintaining privacy and confidentiality. These data are accessed and linked through distributed networks, enabling personal and clinical use, as well as evidence-informed public health interventions, health services management, and research and innovation.
Learning health systems are best assessed against the quintuple aim
The effectiveness of learning health systems are best assessed against the "Quintuple Aim", which optimizes (1) personal health experiences, (2) population health outcomes, (3) health provider experiences, (4) systems efficiency, and (5) overall health equity as indicators for overall system performance.
Implementation of a learning health system in Canada should be guided by common health data principles that would shape a harmonized approach to health data design and use in Canada. This should be framed as a Canadian Health Data Charter (Charter) to give the principles additional weight.
Proposed Canadian Health Data Charter
Inspired by the universal human rights to health, to benefit from science, and to non-discrimination and equity, and founded on the five principles of public administration, comprehensiveness, universality, portability, and accessibility (Canada Health Act), this Canadian Health Data Charter reaffirms Canada's commitment to "improving data collection across health systems to inform future decisions …" (Speech from the Throne, November 23, 2021).
To honour the duty to put people and populations at the core of all decisions about the disclosure, access and use of health data, the Canadian Health Data Charter requires:
- Person-centric health information design to ensure that health data follow the individual across points of care to support individual, clinical, and analytical access and use.
- Common standards for terminology, health data design, stewardship, interoperability, access and portability.
- The quality, security and privacy of health data to maximize benefit and reduce harm to individuals and populations.
- Timely accessibility of meaningful and comprehensive health data to individuals, decision makers, researchers, and the health workforce to support an individual's health needs, quality health programs and services, population and public health, and research.
- The ethical use of health data for policies, programs, services, statistics and research for the public good, including the importance of open science and being open-by-design.
- Data-driven social and technological innovation through partnership, invention, discovery, value creation and international best practice.
- Literacy regarding health data and digital methods for the public, decision-makers and the health workforce.
- Harmonization of health data governance, oversight, and policy.
- Support for First Nations, Inuit and Metis Nation data sovereignty.
- Inclusion of diverse members of the public, patients, communities and other stakeholders in health information system development and oversight.
This proposed Charter provides a Canadian context for common data principles such as FAIR (Findable, Accessible, Interoperable, and Reuse) and UNDRIP (UN Declaration on the Rights of Indigenous Peoples). These principles are complementary to Canada's Digital Charter, which also prioritizes use of data for public good, interoperability, and harmonized governance.
The common set of principles in a Canadian Health Data Charter provides flexibility for implementation of a learning health system while ensuring resulting health data and information are able to be shared where needed. This Charter neither requires jurisdictions to make the same investments at the same time nor use the same technical solutions. Rather, it champions the value of Canada's federation while working toward a common goal, allowing partners to work at the pace appropriate for their context while driving collective effort.
Implementing a learning health system requires persistence and focus
Implementing a learning health system in Canada would require persistence and focus over many years and electoral cycles. Based on experiences from other countries, including Denmark, Finland, Estonia, and the United Kingdom, it is clear there are significant benefits that may take ten or more years of consistent investment and collaboration to achieve. Countries that have stayed the course on such investments have developed the foundation to generate powerful insights to improve health outcomes and were better prepared to generate their own insights for the public health response to the pandemic.
Given the challenge of balancing long-term objectives with short-term funding cycles, a novel use of such a Charter is to guide implementation of health data policy that supports foundational health data investments. Investments would be contingent on a commitment to align with the Charter and leverage health data capabilities, standards and policies. Initiatives would be expected to contribute knowledge of innovative technologies, policies and practices for others to use to increase overall productivity and effectiveness.
Immediate actions:
- 1.1 Endorse and adopt a vision for a Pan-Canadian learning health system measured by the Quintuple Aim.
- 1.2 Endorse and adopt the Canadian Health Data Charter and align principles across health data initiatives.
- 1.3 Incorporate the Canadian Health Data Charter into health investment (i.e. funding) decision-making processes to ensure future investments are aligned with a collective vision for health data in Canada.
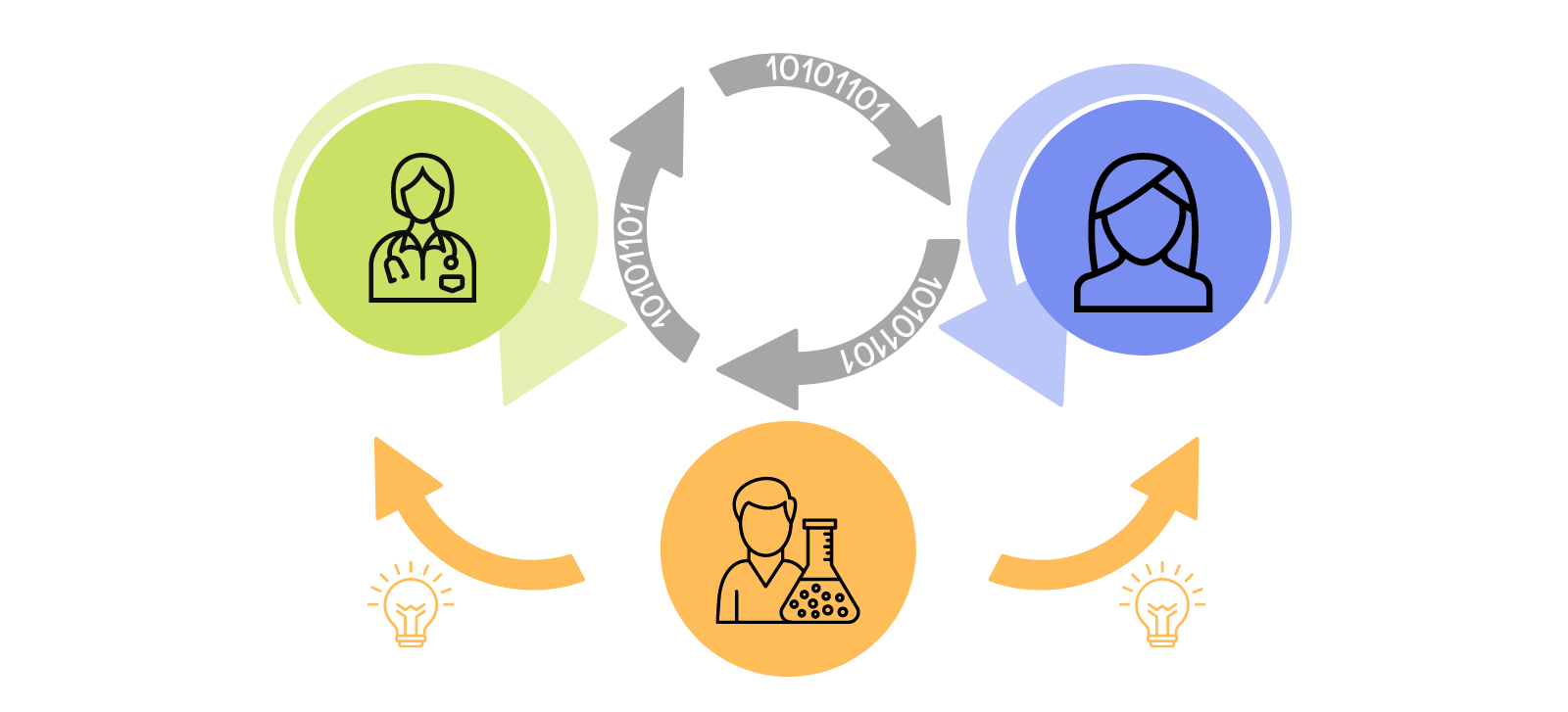
Figure 2: Text description
There are three circles. The top left circle is green and has an image of a health care provider with an arrow around it depicting that data is shared between health care providers. Beside the green is a blue circle with an image of person with an arrow around it depicting that data is shared for the use of the person whose data it is. There is an orange circle below with first two circles, with an image of a researcher. There are two arrows coming from the orange circle, one from each side pointing upwards. One towards the blue circle and one towards the green circle with an image of a lightbulb beneath each one. This indicates that new data, in the form of research findings are shared with the public and health care providers.
b. Support for Indigenous data sovereignty
Recommendation 2: Jurisdictions demonstrate support for First Nations, Inuit, and Métis Nation data sovereignty across geographies with a distinctions-based approach.
Support for First Nations, Inuit, and Métis Nation data sovereignty is included in the proposed Charter; however, that principle warrants its own recommendation, in particular to respect the United Nations Declaration of the Rights of Indigenous Peoples (UNDRIP).
In implementing a Pan-Canadian Health Data Strategy, actions must be taken to ensure respect for, and alignment with, First Nations, Inuit, and Métis Nation data principles and strategies. This includes that First Nations, Inuit, and Métis Nation populations – wherever they live across urban, rural and remote geographies – have control over data they need for their own evidence-informed approaches to health for their populations across Canada. When data about First Nations, Inuit, and Métis Nation populations are used by jurisdictions, that use is collaborative, transparent and ultimately guided by Indigenous communities.
Finally, gaps and exclusions of subpopulations of constitutionally recognized First Nations, Inuit, and Métis peoples in health information systems – based on geography of residence or Indian Act status – need to be recognized and addressed, so that no Indigenous individual or community is left behind.
For individual and clinical decision-making for Indigenous peoples, like for others in Canada, comprehensive person-centric data need to be available regardless of how and where the data were originally collected. Where mutually agreeable, tools and technologies would be shared to improve personal and clinical health data objectives.
A key step would be to ensure that First Nations, Inuit, and Métis Nation are meaningfully included in the oversight and implementation of the Strategy so they may share their own expertise and derive benefits from advances in health services and technologies.
Immediate actions:
- 2.1 Include First Nations, Inuit, and Métis perspectives and representation on senior health data committees that have decision-making power.
- 2.2 Involve distinctions-based, regional, First Nations, Inuit, and Métis health data tables in governance.
- 2.3 Ensure that First Nations living off-reserve, "non-status Indians", and First Nations, Inuit, and Métis living in urban and related homelands are recognized and their perspectives brought to all senior health data committees and decision making.
- 2.4 Support other processes that will ensure Canada is living up to health data commitments made under UNDRIP.
Focus: Support for Indigenous data strategies
In 2021, the Government of Canada allocated funding for the development of data strategies for First Nations, Inuit, and Métis, using a distinctions-based approach. As these strategies are developed, the Pan-Canadian Health Data Strategy must learn from and incorporate insights of Indigenous health data, and create mechanisms to share innovations that may help implement those strategies.
The First Nations' data governance strategy articulates practical steps toward their vision. Many actions in their strategy are similar to what is proposed in this Strategy – including an initial focus on foundations and mobilizing data stewardship, resulting in data sovereignty.
As concurrent work on the Strategy and distinctions-based Indigenous data strategies continues, there will be many mutually beneficial opportunities for collaboration and learning.
Spotlight: Addressing gaps in health information for First Nations, Inuit, and Métis living in urban and related homelands
The majority of First Nations and Métis peoples and a growing number of Inuit live in cities. However, due to jurisdictional complexities, these urban Indigenous populations are commonly overlooked in federal, provincial, and territorial policies and programming, including data strategies.
The need to address data gaps for First Nations, Inuit, and Métis peoples living in cities was highlighted during the COVID-19 pandemic, where virus transmission patterns cut across jurisdictional siloes and instead demonstrated the ongoing interconnection of First Nations, Inuit, and Métis peoples between cities and rural and remote homelands. The near absence of published COVID-19 incidence, testing, vaccine uptake, hospitalization and mortality data for First Nations, Inuit and Métis living in cities during the pandemic reinforced pre-existing unmet needs for these populations by masking inequities in outcomes.
To address this challenge, Seventh Generation Midwives Toronto worked with the Well Living House to use data from an existing representative cohort of First Nations, Inuit, and Métis living in Toronto to produce rates of COVID-19 incidence, testing, vaccination and hospitalization for the 88,000 First Nations, Inuit, and Metis people living in Toronto.
The analysis demonstrated higher rates of COVID-19 linked hospitalization for this population and significantly lower rates of vaccination uptake. Rapidly, this translated into increased Indigenous community and government investments in enhanced, tailored, and Indigenous-led testing, case management, contact tracing, health education, and vaccination programming – potentially saving many lives.
c. Governance: Accountable governance for a learning health system
Recommendation 3: Establish an independent and competency-based Health Information Stewardship Council to design and drive stewardship of the health data foundation and provide advice on health data investments to jurisdictions and First Nations, Inuit, and Métis Nation representative bodies.
Recommendation 4: Establish one or several government-led Learning Health System (LHS) Table(s), with First Nations, Inuit, and Métis Nation representative bodies, to create and drive work on an integrated learning health system roadmap, supported by substantial new funding.
At present, there is no single organization that is mandated to provide stewardship for the health data foundation. Further, there is no coherent leadership across jurisdictions toward a common objective of establishing a learning health system in Canada. Many organizations are attempting to make progress; however, no organization is accountable to ensure investments are interoperable, complementary, collaborative, and comprehensive. As a result, Canada's current health data foundation has few clear data standards and large variations in health data policies that create unnecessary friction and blockages for appropriate data sharing.
The result is duplication of effort, health data investments that do not realize their expected benefits, barriers to collaboration, and evident failures in a number of areas, such as data collection and use during the pandemic. These barriers impair the ability to demonstrate trustworthiness to the public, slow efforts to partner together, foster unconstructive competition, and can cause real harms to Canadians' health.
Competency-based Health Information Stewardship Council
To address this functional gap in Canada's data governance ecosystem, this report proposes the creation of an expert-led and competency-based Health Information Stewardship Council (Council) that would coordinate common efforts toward a world-class health data system and be accountable for stewarding the long-term process of creating and realizing the envisioned health data foundation. This recommendation:
- Reduces unnecessary duplication. The Council would be a stewardship group that advises on the "right" mix of partners work on identified issues; and that those efforts dovetail with other work; and processes / innovations are effectively shared and scaled;
- Drives scale and spread of innovation. The Council would provide strong advice to jurisdictions to allocate substantial and specific funds for health information investment that strengthens the health data foundation in a coordinated manner and supports the spread and scale of innovation;
- Prioritizes pan-Canadian data solutions. The Council would have membership based on competencies rather than representation and would ensure all activities align with a coherent long-term perspective by guiding action toward a common objective – a learning health system – based on the Charter; and
- Holds everyone to account. The Council would provide transparent public reports on performance and progress toward a learning health system to benefit all people in Canada.
Governance must be collaborative by design, harmonized by approach
The Council would be collaborative by design and harmonized by approach. Establishing the Council avoids the need to create a new organizational entity. Existing pan-Canadian organizations and experts across jurisdictions can be leveraged to deliver what is required with the Council as the keeper of the long term vision and orchestrating common efforts:
- Establishing a common model for data stewardship;
- Establishing interoperability standards and harmonized policy;
- Establishing an approach for improving health data literacy and growing capacity;
- Advising on funding required to implement the above work;
- Communicating broadly and effectively to all stakeholders;
- Promoting the change needed to achieve deliverables; and
- Measuring the performance of the health data system.
The Council would act as the overall steward of collective efforts to realize and maintain the health data foundation and uphold the Charter.
Representative Learning Health System Table(s)
Complementary to efforts to realize a stronger health data foundation through the Council, jurisdictions should create one or several Learning Health System Table(s) (LHS Table(s)) that would drive funding and action toward the common vision. Practically, there may be several LHS table(s) – some of which already exist – that collaborate toward that aim. This recommendation:
- Provides focus. The LHS Table(s) would drive priorities toward a learning health system;
- Assesses current state. The LHS Table(s) would adopt a common framework to understand the current state of the relevant portions of Canada's health data systems to identify critical areas where capacity will be needed and identify opportunities to collaborate;
- Establishes integrated roadmaps. Jurisdictions are not starting this journey from the same places with their technologies, policies, or processes. Jurisdictions would create individual roadmaps and project plans (in light of their specific policies, legislation, software systems, data standards etc.) and then prioritize various tasks and activities in a manner to move as expeditiously as possible to the overall objective of a learning health system in Canada. Roadmaps would be integrated across jurisdictions to identify opportunities to leverage existing work and collaborate; and
- Creates incremental outcomes for all people in Canada. Practically, jurisdictional roadmaps would achieve intermediate milestones, which are improvements in and of themselves, as well as moving collaboratively toward longer term success in achieving the full vision of a learning health system for all of Canada.
Collaboration between the Council and the Learning Health System Table(s)
The Council would ensure that expert groups working on health data are aligned toward the common objective of the Charter as well as the more specific objectives of the LHS Table(s).
Significant funding and human resources would be required to advance to a world-class health data system. While clear financial commitments would need to be made across all partners, it is recommended that the federal government show leadership and expect to allocate significant funds (on the order of $1B annually) for the Strategy. These funds should support jurisdictions in their implementations to meet common standards; however, accessing funds would be contingent on agreement on the overall vision, Charter and participation in the LHS Table(s).
The Council would advise on determining the amount and allocation of these funds to strengthen the health data foundation, while the LHS Table(s) align to achieve targeted priorities toward the vision of a learning health system.
Oversight and Composition of the Council and LHS Table(s)
The Council would report to the FPT Conference of Deputy Ministers of Health and coordinate with First Nations, Inuit, and Métis Nation representative bodies. The Council would provide guidance to the LHS Table(s). The Council would be expert and competency-based, drawing its members from the public, health providers, academia, research, public health, health administration, and private sector. The Council must also work to be reflective of Canada, including diverse perspectives from the public (including equity-deserving groups), First Nations, Inuit, and Métis Nation. The Council should have no more than 20 Members to ensure efficiency.
There are several viable methods for creating the Council to ensure realization of the health data foundation and appropriate stewardship of health data across Canada. It is crucial that the mechanisms for establishing the Council be transparent in order to advance its legitimacy with all critical stakeholders. The Council would be supported by a secretariat to carry out its operational and program functions. The Secretariat would have expertise in facilitation, collaboration, communication, and health data governance and would work with the secretariat(s) for the LHS Table(s) and other related secretariats.
The LHS Table(s) would report to the FPT Conference of Deputy Ministers of Health and coordinate with First Nations, Inuit, and Métis Nation representative bodies and receive advice from the Council. The LHS Table(s) would be representative across jurisdictions and incorporate First Nations, Inuit, and Métis Nation perspectives so that they would be FPT-FNIM bodies.
The Council, the LHS Table(s), and their secretariats must be established quickly to build momentum for the initial efforts of the Strategy to realize the vision of a world-class health data system.
Immediate actions:
- 3.1 Establish Terms of Reference for the Council and identify membership.
- 3.2 Identify / create expert working groups to establish frameworks for the health data foundation.
- 4.1 Establish Terms of Reference for the LHS Table(s) and membership.
- 4.2 Identify and use common capability model(s) for current state assessments.
- 4.3 Develop integrated roadmaps that quantify time and cost of achieving the vision.
- 4.4 Identify significant additional funding for initiatives that are fundamental to strengthening the health data foundation in line with the Health Data Charter and advancing a learning health system.
d. Trust: Meaningful engagement and communication with the public and stakeholders
Recommendation 5: Establish meaningful and ongoing engagement with the public and stakeholders to understand their health data needs and expectations.
Recommendation 6: Develop communications plans with the public and other stakeholders to demonstrate how their health data needs and expectations are being addressed.
A world-class health data system is person-centric
A world-class health data system is person-centric. Therefore, it is essential to engage the public and communities to inform the implementation of health data strategies. Administrators, providers and innovators need to understand the public's expectations when it comes to management of health data in particular for health data sharing and use. Better understanding would build trusted relationships to bring individual and collective benefits. Engagement and communication need to be ongoing and evolve as public expectations change in response to new societal circumstances and technological advances (e.g. the use of artificial intelligence in health care and decision-making and the use of genomics in personalized medicine).
Embedding public and stakeholder expectations in policy, processes and structures for health data sharing and use helps drive transparency, accountability and mutual respect, which are the foundations of trust. That trust supports a positive cycle that supports continuous improvement for the health systems to work better for all.
Guidance on Health Data: Giving a Voice to People
An ongoing, pan-Canadian public assembly should be established to provide insights and advice to governments on what responsible collection, access, sharing, and use of health data is in the context of Canadian values. Other public assemblies could be established at various regional or sub-regional levels to provide advice on jurisdictional implementations for health data systems.
Assemblies should be chaired by a member of the public, be designed to include diverse perspectives and experiences (including equity-deserving groups), and have fixed-term membership. The size of the assembly should reflect the nimbleness required to make progress while ensuring representative diversity. Ideally, members of public assemblies would be compensated for their contributions. Each Assembly would be presented with specific information to help inform the kind of guidance needed (e.g., on proposed investments, or newly developing technology). They would also be able to recommend deeper engagement (e.g., local focus groups or a broad survey) in cases where it is felt that a broader public conversation is needed.
Continuous Communication
To complement engagement, evergreen communication plans are needed to improve digital and health data literacy and foster trust. Clear, consistent communications would be designed to:
- Provide information on how data are collected, shared, used, and protected;
- Demonstrate the benefits of data sharing for individuals, their caregivers, and the public; and
- Provide transparency on decisions regarding health data use and other areas of general interest.
Communication plans would set core messages in plain language and should be coordinated across jurisdictions. Consistency of communication would help to amplify core messages and demonstrate trustworthiness. In turn, that would improve data sharing where deeper insights are discovered, meaningful evidence-informed action is taken, and benefits are achieved.
Creating an inventory of communication initiatives already in place, along with public opinion research on perspectives for health data sharing and use, would help target new communications appropriately.
Immediate actions:
- 5.1 Establish a Pan-Canadian public assembly for health data, building on best practices.
- 5.2 Identify and leverage stakeholder groups to gain diverse insights and viewpoints.
- 6.1 Identify and synthesize existing public opinion research, and undertake new public opinion research as appropriate.
- 6.2 Develop core messages for initial communications reflecting the common vision and unique aspects within each jurisdiction and processes for ongoing communications.
"If you don't trust me with my data, why should I trust you with mine?"
Linda Wilhelm, living with Rheumatoid Arthritis for 40 years, October 2021
e. Policy: Frameworks for health data stewardship and policy
Recommendation 7: Establish a policy framework for data stewardship that mandates appropriate data exchange, re-use and collaboration across critical health data supply chains, balanced with security, confidentiality and respect for privacy.
Recommendation 8: Establish a harmonized pan-Canadian health data policy framework that supports person-centric data, open-by-design, and the stewardship model of health data management.
Person-centric data demands rethinking rules for a data-driven world. A pan-Canadian health data policy framework (Framework) is needed to define a modern health data policy aligned with the Charter. Data stewards – as described in the EAG's second report – would drive implementation of the Framework.
Data stewards are a relatively new role for health, while it is a mature role in other industries (e.g., finance). Data stewards would be accountable to champion access to health data while ensuring it is also protected for individual, clinical, or analytical use. They also drive re-use of data, policies, and standards to simplify scale and spread of innovation, productivity and system effectiveness.
Data Stewards and Privacy Officers: Partners in Health Data Management
While there are no legislative barriers to sharing data that cannot be associated with an individual, the value of analyses on that data are limited. The most crucial analyses require detailed data to be shared, linked, and then protected to fulfil the promise of using data for the public good (e.g., health research, detection of public health threats, understanding impacts of social determinants of health on individual and population health).
Data stewards work with data custodians and privacy officers to design data sharing and use to be open-by-design and appropriately protected so these crucial analyses are timely and impactful. A framework for data stewardship would recognize different types of stewards are necessary to:
- Manage integrity, protection, appropriate access and use of data within an organization;
- Optimize timely sharing of quality data across organizations creating data supply chains; and
- Optimize across data supply chains for data, standards, and policies across a data supply network.
Jurisdictions should have a 'Chief Health Data Steward'
Given the complexity and importance of health data, jurisdictions should have a 'Chief Health Data Steward' that would optimize health data activities within their jurisdiction. Data stewards would also be identified to support organizations and data supply chains. Chief Health Data Stewards would collaborate with each other across jurisdictions, health organizations, the private sector, and with equivalent roles identified by First Nations, Inuit, and/or Métis Nation representative bodies to support Indigenous data sovereignty.
In cases where the data supply networks span jurisdictions, such as in public health surveillance, monitoring adverse drug reactions, and understanding health inequities, Chief Health Data Stewards would collaborate to eliminate friction in data access across borders for pan-Canadian intelligence. Chief Health Data Stewards would be guided by the Charter, identify priority gaps in data sharing, highlight innovations that can be scaled and spread across Canada, and incorporate international best practices, while also keeping watch to avoid blockages that impede essential and appropriate data flows.
Actions to steward the use of data for the public good would be governed by regulation and ethics, driving benefits that should be achieved for Canadians with the requirement to keep data secure and private, working in collaboration with data custodians and privacy officers.
A Common Health Data Policy Framework
A Framework should be established that describes the practical processes needed for robust data sharing that can drive better health outcomes and ensure privacy protection. Many of these processes would be supported by data stewards.
The Framework would define minimum requirements to address agreed priorities and modernize policies to minimize unnecessary friction in data access and sharing within and across jurisdictions for personal, clinical, and analytical use. In parallel, jurisdictions should clarify the intent of their existing legislation and policy (e.g., when data must be shared and with what protections) and incent appropriate action.
The Framework would be used to inform current state capability assessments and development of roadmaps which would include updates of health data policies that are harmonized with the Framework. Individual FPT legislations may differ; however, there should be a cooperative effort to align policies for mutual benefit in the interest of all people in Canada.
There are opportunities for immediate action:
- Legislation for Interoperability: The United States passed a regulatory 'interoperability rule' requiring vendors to ensure data are interoperable and sharable. This legislation explicitly directs vendors to prevent data blocking and provide solutions for data portability. Given that many vendors also operate in Canada, there is an opportunity for Canada to adopt legislation toward similar outcomes.
- Legislation for Data Management: A report by the North American Observatory demonstrates that many countries have found that legislative measures for data management are effective. Legislation should focus on the accountabilities, controls, policies, and processes that simplify data access and sharing for individual, clinical, and analytical use rather than legislating specific standards. This may include penalties for unapproved and intentional acts that impact the privacy of individuals.
- Common Data Collaboration Protocol: Create a common agreement for multi-organizational and multi-jurisdictional data collaborations (including research). This would establish expectations for data access and protection across data supply chains and networks. This has been implemented in Nova Scotia and is being implemented in the United States (Trusted Exchange Framework and Common Agreement).
- Framework for Health Technology Vendors: In advance of legislation, which will take time, a common set of requirements for vendors should be developed to clarify expectations for their data management accountabilities – adopting common standards for data portability and that data are open-by-design.
These measures would be developed and implemented collaboratively across jurisdictions. Frameworks should include strong incentives for adoption of Pan-Canadian standards, establish significant disincentives for misuse or purposeful blocking or fragmentation of data and clarify accountability to designate pan-Canadian standards.
Immediate actions:
- 7.1 Establish scope and responsibility of all data stewardship roles.
- 7.2 Appoint Chief Health Data Stewards aligned with a common policy model.
- 7.3 Prioritize data stewards to coordinate across critical health data supply chains (e.g., public health).
- 8.1 Develop a health data policy framework with jurisdictions and partners (focus on access, privacy, ethics)
- 8.2 Advance opportunities for collaborative legislation on interoperability and data management.
- 8.3 Develop a pan-Canadian data collaboration protocol to simplify data sharing agreements.
- 8.4 Develop a health technology vendors framework for common standards and requirements.
Spotlight: Nova Scotia's Data Sharing Protocol
Nova Scotia's Data Sharing Protocol has allowed them to improve timeliness in sharing data between trusted partners from months to days. Nova Scotia took the action to bring together all stakeholders – privacy officers, data professionals, policy experts, and others – and design this end-to-end process that embedded the necessary accountability and controls.
The Protocol was established at a senior management level and included a designated coordinator and decision maker role in each partner organization. The protocol has reduced paperwork, clarified accountability, accelerated data sharing and related insights and increased trust between partners.
The Nova Scotia protocol pre-dates the similar Trusted Exchange Framework and Common Agreement (TEFCA) currently being implemented in the United States. Under that agreement, rules for data access, sharing, and privacy are established in advance of data sharing, allowing individual organizations and networks to join with explicit expectations for compliance and associated penalties.
Overall these initiatives lower cost, accelerate insight, and improve outcomes. Savings gained from efficiencies associated with data sharing agreements can then be re-invested to provide more timely and meaningful insights.
f. Interoperability: Common data standards and data architecture
Recommendation 9: Establish common integrated health data standards and data architecture and drive and monitor their roll out.
The Need for Common Standards and Architecture
Common data standards and interoperability requirements, including those for data exchange and content, are essential of a world-class health data system. Commonly adopted content standards across data supply chains are necessary for moving data between systems while maintaining their meaning. For example, date of birth in one system captured as month-day-year, in the presence of common data standards, can be correctly used by another system whose date format is day-month-year. Another example where data standards help include the diagnosis of types of diabetes and classifications of reasons for visiting a primary care provider.
Integrated health data standards allow for the movement of data between systems. A health data architecture must be constructed in a way that centres on the person and requires health information technologies to use those standards in support of a pan-Canadian learning health system. With an architecture that requires use of common standards, data quality is enhanced and data are made available for personal, clinical, and analytical use. Analytical use purposes include evaluation, public health, research, administration, health human resource allocation and other essential system improvement activities. It is assumed that to support those use cases and users, multiple systems will be required. Hence there must be integrity and interoperability between and among the different systems to achieve collective impact and improved outcomes.
The pandemic has demonstrated the need for data networks to be agile
The pandemic has demonstrated the need for data networks to be agile, allowing for the expansion or modification of data standards and systems such that new data supply streams can be integrated in near real-time (e.g., vaccine availability, personal protective equipment, virus variants). Integrated data standards allow individual data collectors to use their own methods to capture data as long they are consistent with overall standards that ensure communication along data supply chains linked in a pan-Canadian data supply network.
Integrated data standards, architecture, and policies that align with the Charter would enable data portability between providers and care settings, allowing data to move as a person moves across Canada's health systems. Those standards should be open, free for use, and readily available to encourage broad adoption. Integrated data standards also enable:
- Personal and clinical benefits based on data through an individual's lifetime;
- Insights about health equity – when combined with data about individual and community characteristics;
- Robust analytics including those needed for quality, public health, population health and research; and
- Collective data analysis for purposes of creating group / population cohorts for research and evaluation.
Common identifiers (e.g., digital identities for individuals, providers, and facilities) are a critical component of advanced health data systems. Identifiers simplify linking to allow for more timely and meaningful insights.
Sample Person-centric Health Data Architecture
The goal of interoperability has been articulated through the concept of "one person-one record"; however, many of the electronic medical record (EMR) systems implemented to date were specifically chosen and tailored to meet local needs without consideration of personal or analytical uses. While calls for a single, consolidated, pan-Canadian EMR are appealing in their simplicity, the EAG does not favour this approach. Challenges in coordination across provinces and territories, the long history of major investments in existing systems with unfulfilled interoperability potential, and the higher risk of over-reliance on a single vendor are important reasons to explore other options.
The EAG has developed a conceptual model for a pan-Canadian interoperable health data architecture to help launch the Council's work in this area. This would need to be expanded to address interoperability required for a learning health system – where insights are used to continually improve health outcomes.
Data from all health encounters and sources should be linkable
In the model, data from all health encounters and sources are linkable so jurisdictions can support a comprehensive and integrated view of the patient, population, and health system. These same data are used – with appropriate controls – for analytics within the jurisdiction and across jurisdictions where appropriate. When a patient receives care out-of-province (e.g., expecting mothers from Northwest Territories have their delivery in Edmonton), data from that experience are sharable to ensure completeness of the patients' health record. This design also simplifies the ability to permanently transfer health records for Canadians who move across the country.
The health data architecture would (a) be based on common data standards, (b) enable exchange between personal, clinical, and analytical systems, (c) provide real-time access for advanced insights to be easily generated for personal, clinical, or analytical use, (d) be sufficiently flexible to allow rapid deployment for collection of newly needed data elements, as has been the case with the pandemic, and (e) ensure data are appropriately governed, secure and confidential while being open-by-design.
Each jurisdiction would evaluate its current state and then create a roadmap of changes needed to reach the collectively agreed-upon health data architecture, including integrated data standards. Implementation of the health data architecture would occur in stages, based on individual and collective priorities and readiness. For example, initial focus could be on providing comprehensive personal, clinical, and analytical access in specific data domains (e.g., pharmaceuticals, vaccinations) or to close critical health data gaps (e.g., health workforce).
Immediate actions:
- 9.1 Develop common integrated data standards that are open and facilitate person-centric intra- and inter-jurisdictional data sharing that support a pan-Canadian health data network.
- 9.2 Develop a person-centred health data architecture that integrates personal, clinical, and analytical systems, leverages integrated health data standards, and provides flexibility for its implementation while highlighting areas where immediate priority can accelerate pan-Canadian interoperability.
g. Literacy: Data literacy and capacity
Recommendation 10: Establish a common approach to digital and health data literacy that is grounded in common language and content to increase data capability among all health data users and expand professional standards for critical health data roles.
Improving Health Data Literacy as the Foundation of Building Trust
Advancing better health data collection, access, sharing and use, and helping the public benefit from it requires greater shared understanding of its benefits, risks, and the need for quality health data. Health data and digital health literacy should be grounded in standardized frameworks using a common language that improves data collaborations and optimizes the quality of health programs and services. Together, these elements of health data literacy would promote trust, collaboration and improve system design.
Improving digital and health data literacy across the span of health data users would result in benefits for health systems; however, their literacy needs are different. Literacy program topics, by stakeholder, could include:
Public: Understanding of the value of personal health data access and the complementary societal good that can come from protected health data sharing (e.g., use of personal data to determine vaccine efficacy and to detect adverse drug reactions more quickly) and controls around how others can access and use their data.
Health providers: Understanding how the data they collect can be used by them (or others in the patients' circle-of-care, care providers, or the patient) not only immediately but also more broadly to ensure continuous quality improvement in the provision of care, thereby clarifying their value-added accountabilities in data collection and sharing.
Technology providers: Understanding public expectations and their responsibilities (e.g., for interoperability, economies of scale, and transparency) so they can align with evolving health data policies, thereby enabling them to deliver value for their customers while meaningfully contributing to the health of all persons in Canada.
Government decision-makers: Understanding the broader benefits of health data sharing and data governance and their accountability to align incentives and financial resources to reduce cost and accelerate insights for decisions, even when from time-to-time the data analyses reveal problems.
Data stewards and privacy officers: Understanding current public expectations about health data to remedy the imbalance that has been seriously limiting the collection, access, sharing, and use of personal health data to inform processes, policies, legislation, and requirements for communication and transparency.
Together a common suite of literacy programs across jurisdictions would increase awareness and understanding of the investments in health data, and promote understanding of jurisdictional roadmaps to deliver a learning health system, and the policies and architecture that ensure data are as open, secure, and confidential.
Common language (lexicon and taxonomy) would be developed in phases and be continually improved. Work would be coordinated by the Council, leveraging technical expertise and participation from target audiences. Where possible, this would leverage existing literacy programs domestically or internationally.
Building Data Capacity in Canada to Deliver a Pan-Canadian Health Data Strategy
Additional capacity, in the form of trained data experts and professionals, will be necessary to bring recommendations in this report to life. While many of these recommendations would improve health system effectiveness, specialized skills and competencies related to data design, policy, management and oversight are in short supply. Investment in a digital- and data- skilled workforce would have a dramatic benefit for the productivity of a data rich health sector.
Data skills will be required in front-line care and new data functions
Data skills will be required in both front-line care and in new health data functions required to implement recommendations in this report under a Pan-Canadian Health Data Strategy. Notably all types of data stewards, data architects, data managers, and data analysts will be in demand.
Education for health providers (e.g., nurses, physicians, pharmacists) should be enhanced to include clinical health data management and data ethics. This content should be included in undergraduate training, ongoing professional development, and eventually must become a requirement in professional accreditation standards.
In addition, the formal regulation of specialized health data-focussed roles should be expanded, building on what exists for health information professionals. Health information management certification bodies should take a pan-Canadian approach to training and professionalization of health data experts. They would work to enable academia, professional health data organizations, and credentialing organizations in other industries to develop programs. In this manner, health information management should become a regulated profession in Canada, ready to fulfil an urgent need to bring greater value to and from our health systems.
Immediate actions:
- 10.1 Develop common lexicon and taxonomy for health data collection, access, sharing, use, and governance.
- 10.2 Develop common literacy objectives for the public, health workforce, and government decision-makers.
- 10.3 Measure current health data capacity and benchmark to peers to quantify data skills gap.
- 10.4 Develop approach to embed health data as a core component of undergraduate and health professional continuing education.
- 10.5 Support credentialing and program standards development to enable the creation of regulated professions in health information management.
4. Mobilizing change: The first year
Seizing the Opportunity
For 60 years, there has been recognition of the potential of data to improve health outcomes for all people in Canada. As noted in the first report of the EAG, there have been many attempts to make significant progress that have repeatedly been met with systemic barriers – largely related to policies, governance, and culture. Available technologies have not been an important barrier.
Timing and context are crucial for a strategy as complex as this to be successful. The pandemic has provided much of this timing and context:
- Public awareness of the health data challenges experienced during the pandemic that have reduced the effectiveness of interventions and slowed pandemic recovery;
- Pressures to address burnout of health workforces which are partially attributed to excessive additional burden to perform data functions without commensurate benefit, as well as insufficient understanding of workforce allocation (e.g., personal support workers in long-term care);
- Recognition of lost opportunities to foster, spread, and scale health data research and innovation;
- Desire to address systemic health inequities which need timely and meaningful data (e.g., identifying essential occupations during the pandemic and ethnicity differences in those becoming infected); and
- Demonstrated capacity in some areas, triggered by COVID-19, to rapidly scale digital tools with collaboration across jurisdictions (e.g., procurement of protective equipment, roll-out of virtual care), with serious challenges in others (e.g., timely data on excess deaths, genotyping of COVID variants).
Collectively, these recent experiences are creating an increased awareness and demand for change among the public, health providers, and government decision-makers. Many jurisdictions are starting to mobilize their own digital and health data strategies; a Pan-Canadian Health Data Strategy to link them all is essential – to coordinate these important efforts, and make the proverbial whole much greater than the sum of its parts.
Preparing to Launch
All people in Canada deserve to see progress in health data systems so they can start reaping the benefits. The following is a summary of key activities that could be undertaken in the first year, with collaboration, adequate funding, and political support:
- Jurisdictions endorse the vision and Canadian Health Data Charter.
- Jurisdictions form the Health Information Stewardship Council and Learning Health System Table(s).
- The Council, with expert groups, establish prioritized frameworks aligned to the Charter.
- Jurisdictions assess their current state of health data policy, standards, architecture, and capacity.
- The Council advises the LHS Table(s) on investments for a learning health system.
- Jurisdictions build roadmaps – with adequate funding – to achieve a learning health system.
Initial steps must focus on the highest priority areas identified during the pandemic – for example the collection of data for addressing health equity, addressing data gaps in health workforce and long-term care, and improving data for public health measures, including infectious and chronic disease surveillance, critical supply management, and vaccine efficacy.
5. Conclusion: The first step on a journey of a thousand miles
The Expert Advisory Group (EAG) has worked together for 16 months to develop this advice for advancing a Pan-Canadian Health Data Strategy. The first two reports of the EAG focussed on the negative impacts of Canada's long-standing fragmented health data foundation and exposed the risk of multi-national companies driven by profit and misaligned with Canadian values continuing to disrupt Canada's health data systems. In this third report, the EAG has laid out the framework and critical actions necessary for "expediting work to create a world-class health data system" (Ministerial mandate letter, 2021).
The EAG has learned that the problems are not technical. A review of decades of reports and studies has highlighted the fundamental importance of high-quality health data, both for excellent patient care, and for broader public good objectives – especially in areas of care quality, research, and combatting pandemics. If we are to learn anything from these decades of very limited success, it must be that the barriers to improving health data are not technical. Rather, a new approach with a common vision and stronger governance, and more collaborative culture are needed to maximize the value of health data assets for Canadians.
Strategic, incremental, and significant investment is required. A number of organizations were created and hundreds of millions of dollars have been spent to realize the potential of health data; however, few initiatives have fully achieved intended results. Technical solutions are available and have been well known for many years and continue to evolve. But implementations have tended to be provider- rather than person-centric and are not designed to scale and realize broader health benefits for all. Future investments must be guided by a common vision and principles, and leverage the value of a strong health data foundation.
The EAG believes Canada can be both aspirational and practical. This report highlights several opportunities, among many, to build on data excellence country-wide that could benefit all people in Canada. Initial steps toward a world-class health data system are to increase trust and capacity while creating common frameworks for policy and architecture, grounded in governance that has the respect and authority to drive change. When in place, a health data strategy would be implemented with collaboration, cooperation, and respect.
Other jurisdictions have succeeded, Canada can too. Based on the experience of those countries already successfully making progress, the journey toward a world-class health data system may have to take a decade. Sustained will, focus, and trust will be required, along with adequate funding and deep public and stakeholder engagement. A new and effective kind of governance and commitment to unlock health data benefits is necessary to make progress and maintain momentum through electoral cycles.
Taking the first step is necessary for success in the long-run. Initial choices should prioritize areas where there is potential for broad and significant impact that can be implemented quickly. Success must be defined as scaling fast. Data gaps highlighted during the pandemic provide many options on where to start – be it public health surveillance, genomics, health workforces, mental health and long-term care, among others.
We must overcome our own, self-imposed obstacles: The greatest risks to this Strategy are the legacy of mistrust between jurisdictions, fears of what more probing data analytics might reveal, and a culture that fails to put the individual as the focal point for benefits received through health systems investments. Recommendations in this report are written to advance a collective goal. There is no impediment to collaborate for the benefit of all persons in Canada – rather there is a moral imperative to do so.
Glossary
Anonymization: The process of removing or altering data that identifies an individual or could, foreseeably, identify an individual in the future. The degree to which data are anonymized depends upon the sensitivity of the information, what it is being used for and who has access to it (adapted from Global Alliance for Genomics and Health 2016 and Emam et al. 2021).
Data: Observations, narratives or measurements that are captured for possible use as the basis for further analysis, calculation or reasoning (adapted from Global Alliance for Genomics and Health 2016).
Data Custodian: As defined in Canadian health legislation, an individual or organization responsible for the secure collection and/or storage of health data and the curation of health data use, disclosure, retention and disposal. Primarily concerned with security and privacy of health data.
Data Steward: An entity or senior government role responsible for assuring the quality, integrity and access arrangements of data and metadata in a manner that is consistent with applicable law, institutional policy and individual permissions. Includes entities and positions that deal primarily with personal health information, and those that deal with other health information (Global Alliance for Genomics and Health 2016).
Data Supply Chain: The technological steps and human-involved processes supporting the flow of data from individuals through organizations, from its raw state, through transformation and integration, all the way through to the point of consumption or analysis (adapted from Devane 2021).
First Nations, Inuit, and Métis Nation representative bodies: Refers to governments and/or designated organizations representing constitutionally recognized First Nations or "Indian" (Status and non-Status), Inuit, and Métis peoples across all geographies.
Indigenous: In the Canadian context, "Indigenous" refers to First Nations or "Indian", Inuit, and Métis peoples. First Nations is a term used to describe Indigenous peoples of Canada who are neither Métis nor Inuit. This term came into common usage in the 1970s and '80s and generally replaced the term "Indian" (Status and non-Status), although unlike "Indian," the term "First Nations" does not have a legal definition." (From https://indigenousfoundations.arts.ubc.ca/terminology/)
Health Data: Observations, facts or measurements – captured for possible further analysis, calculation or reasoning – which relate to the physical or mental health status of individuals, health system performance and socio-economic, community and health system characteristics.
Health Information: Health data that have been analyzed or interpreted to provide insight or a narrative related to the physical or mental health status of individuals, health system performance, and socio-economic, community and health system characteristics.
Health Provider: A health care provider is defined as a health professional that a person sees or talks to when they need care or advice about their health. Health providers include many different professions including: audiologists, chiropractors, dental assistants, dental hygienists, dentists, dietitians, environmental public health professionals, genetic counsellors, health information management professionals, licensed practical nurses, medical laboratory technologists, medical physicists, medical radiation technologists, midwives, nurse practitioners, occupational therapists, opticians, optometrists, paramedics, pharmacists, pharmacy technicians, physicians, physician assistants, physiotherapists, psychologists, registered nurses, registered psychiatric nurses, respiratory therapists, social workers and speech–language pathologists (adapted from Canadian Institute for Health Information 2020; Statistics Canada 2019).
Health Sector: The general set of activities related to Individual-based health, population-based health, health research and education and health management, oversight and governance.
Health Services: Activities related to health, delivered either directly or indirectly to the public, on both an individual level (including primary, secondary and tertiary care) and a population level (disease surveillance, prevention and control; health promotion; reducing health inequity).
Health Workforces: Practitioners that deliver health services
Information: Data that have already been interpreted (i.e., they have meaning in a specific context) (Global Alliance for Genomics and Health 2016).
Interoperability: The capacity for seamless sharing of health data and information between health sector stakeholders by means of policy, governance, workflow and, especially, technical alignment including both at the level of software and standardized concepts and definitions for data elements.
Learning Health System: Drives better outcomes for individuals with their own health data and personalized insights while improving overall system quality, population health, evaluation, planning, and public health, aligned with data user needs and supporting equitable health.
Personal Health Information: Health data or information that is specific to a unique and identified individual.
Annex A: Summary of recommendations and immediate actions
| Recommendation | Immediate action |
|---|---|
| Vision and Principles | |
| Jurisdictions endorse a vision that "by 2030, all people living in Canada will benefit from a fully integrated and continuously optimized learning health system." and that the implementation will be guided by common principles in a Canadian Health Data Charter. |
|
| First Nations, Inuit, and Métis data sovereignty | |
| Jurisdictions demonstrate support for First Nations, Inuit, and Métis Nation data sovereignty across geographies with a distinctions-based approach. |
|
| Governance | |
| Establish an independent and competency-based Health Information Stewardship Council to design and drive stewardship of the health data foundation and provide advice on health data investments to jurisdictions and First Nations, Inuit and Métis Nation representative bodies |
|
| Establish one or several government-led Learning Health System (LHS) Table(s), with First Nations, Inuit, and Métis Nation representative bodies, to create and drive work on an integrated learning health system roadmap, supported by substantial new funding. |
|
| Trust | |
| Establish meaningful and ongoing engagement with the public and stakeholders to understand their health data needs and expectations. |
|
| Develop communications plans with the public and other stakeholders to demonstrate how their health data needs and expectations are being addressed. |
|
| Policy | |
| Establish a policy framework for data stewardship that mandates appropriate data exchange, re-use and collaboration across critical health data supply chains, balanced with security, confidentiality and respect for privacy |
|
| Establish a harmonized Pan-Canadian health data policy framework that supports person-centric data, open-by-design, and the stewardship model of health data management. |
|
| Interoperability | |
| Establish common integrated health data standards, drive and monitor their roll out |
|
| Literacy | |
| Establish a common approach to digital and health data literacy that is grounded in common language and content to increase data capability among all health data users and expand professional standards for critical health data roles. |
|
References
Main Text
Bernier Alexander, Liu H, McDougall R, Joly Y (2021). Law and Policy of Public Health Information Sharing in Canada. Centre of Genomics and Policy, McGill University. Available online at https://www.genomicsandpolicy.org/Ressources/LawandPolicyofPublicHealthInformationSharinginCanada-20211208.pdf.
Boyd, Mark, Milly Zimeta, Jeni Tennison, & Mahad Alassow. (2021). Secondary use of health data in Europe. Open Data Institute. Available online at https://theodi.org/wp-content/uploads/2021/09/Secondary-use-of-Health-Data-In-Europe-ODI-Roche-Report-2021-5.pdf.
Canadian College of Health Information Management. (2022). Certification. Available online at https://cchim.ca/certification/.
Canada Health Infoway. (November 11, 2020). Consulting Canadians on the Future of their Health System: A Healthy Dialogue. Available online at https://www.infoway-inforoute.ca/en/component/edocman/3850-a-healthy-dialogue-executive-summary.
Canadian Institute for Health Information. (2020). A profile of health care providers in Canada, 2020. Available online at https://www.cihi.ca/en/a-profile-of-health-care-providers-in-canada-2020.
Council of Canadian Academies (2015). Accessing Health and Health-Related Data in Canada. Ottawa (ON): The Expert Panel on Timely Access to Health and Social Data for Health Research and Health System Innovation, Council of Canadian Academies. Available online at https://cca-reports.ca/wp-content/uploads/2018/10/healthdatafullreporten.pdf.
Devane, Heather. (August 11, 2021). What Is the Data Supply Chain? Immuta. Available online at https://www.immuta.com/articles/what-is-the-data-supply-chain/.
Emam, Khaled El, Paige Moura, Vance Locton, Elizabeth Jonker, Adam Kardash, and the CANON Steering Committee. (March 2021). Practices For Generating Non-Identifiable Data: Final Report For Office Of The Privacy Commissioner Of Canada Contributions Program. Canadian Anonymization Network. Available online at https://deidentify.ca/wp-content/uploads/2021/08/CANON-OPC-Project-Final-Report-v9.pdf.
Farmer Julie, Marchildon G, Allin S. (2022). Governance of COVID-19 Vaccine Data in Federations. Toronto: North American Observatory on Health Systems and Policies. Rapid Review (No. 33). Available online at https://ihpme.utoronto.ca/wp-content/uploads/2022/03/NAO-Rapid-Review-33_EN.pdf.
General Assembly of the United Nations. (2017). United Nations Declaration on the Rights of Indigenous Peoples. Available online at https://www.un.org/development/desa/indigenouspeoples/declaration-on-the-rights-of-indigenous-peoples.html.
Global Alliance for Genomics and Health. (2016). Global Alliance for Genomics & Health Data Sharing Lexicon. Version 1.0. Available online at https://www.ga4gh.org/wp-content/uploads/GA4GH_Data_Sharing_Lexicon_Mar15.pdf.
Government of Canada. (2021). Budget 2021: A Recovery Plan for Jobs, Growth, and Resilience: Part 3: A Resilient and Inclusive Recovery. Available online at https://budget.canada.ca/2021/report-rapport/p3-en.html.
Health Innovation Network South London. (n.d.). What is person-centered care and why is it important? Available online at https://healthinnovationnetwork.com/system/ckeditor_assets/attachments/41/what_is_person-centred_care_and_why_is_it_important.pdf.
Information and Privacy Commissioner of Ontario. (2021). Use and Disclosure of Personal Health Information for Broader Public Health Purposes. Available online at https://www.ipc.on.ca/wp-content/uploads/2021/07/use_disclosure-personal-health-information-for-broader-public-health-purposes.pdf.
Innovation, Science and Economic Development Canada. (2019). Canada's Digital Charter in Action: A Plan by Canadians, for Canadians. Available online at https://www.ic.gc.ca/eic/site/062.nsf/eng/h_00109.html.
Johnston, R., Banting, K., Kymlicka, W., & Soroka, S. (2010). National Identity and Support for the Welfare State. Canadian Journal of Political Science, 43(2), 349-377. doi:10.1017/S0008423910000089.
Lee, Peter, Amy Abernethy, David Shaywitz, Adi V. Gundlapalli, Jim Weinstein, P. Murali Doraiswamy, Kevin Schulman, and Subha Madhavan. (2022). Digital Health COVID-19 Impact Assessment: Lessons Learned and Compelling Needs. NAM Perspectives. Discussion Paper, National Academy of Medicine, Washington, DC. Available online at doi:10.31478/202201c.
Nundy, Shantanu, Lisa A. Cooper, & Kedar S. Mate. (2022). The Quintuple Aim for Health Care Improvement: A New Imperative to Advance Health Equity. Journal of the American Medical Association. 327 (6): 521–522. Available online at doi:10.1001/jama.2021.25181.
Office of the Prime Minister. (December 16, 2021). Minister of Health Mandate Letter. Available online at https://pm.gc.ca/en/mandate-letters/2021/12/16/minister-health-mandate-letter.
Ontario Health. (2021). Digital Health Information Exchange Standard. Available online at https://www.ontariohealth.ca/our-work/digital-standards/digital-health-information-exchange-standard.
Statistics Canada. (2020). Primary health care providers, 2019. Health Facts Sheets. Available online at https://www150.statcan.gc.ca/n1/pub/82-625-x/2020001/article/00004-eng.htm.
The First Nations Information Governance Centre. (2020). A First Nations Data Governance Strategy: A Response to Direction Received from First Nations Leadership, Funded through Federal Budget 2018 in Support of the New Fiscal Relationship. Available online at https://fnigc.ca/wp-content/uploads/2020/09/FNIGC_FNDGS_report_EN_FINAL.pdf.
Wilkinson, M., Dumontier, M., Aalbersberg, I. et al. (2016). The FAIR Guiding Principles for scientific data management and stewardship. Scientific Data (3): 160018. Available online at doi:10.1038/sdata.2016.18.
Zhang, Pepe, and Angel Melguizo. (2022). Data 4.0 – Rethinking rules for a data-driven economy. World Economic Forum. Available online at https://www.weforum.org/agenda/2022/01/data-4-0-rethinking-rules-for-a-data-driven-economy/.
Members of the Expert Advisory Group
Chair
Dr. Vivek Goel, President and Vice-Chancellor, University of Waterloo
Members
Dr. Ewan Affleck
Dr. David Castle
Dr. Stafford Dean
Dr. Jonathan Dewar
Mr. Michael Harvey
Dr. Steven Hoffman
Prof. Bartha Maria Knoppers
Ms. Alies Maybee
Dr. Muhammad Mamdani
Dr. Kim McGrail
Mr. Jeff Nesbitt
Dr. Cory Neudorf
Ms. Glynda Rees
Dr. Janet Smylie
Dr. Gail Tomblin Murphy
Dr. Graham Tipples
Dr. Michael Wolfson
Contact
To contact the secretariat directly:
Email: PCHDS-SpCDS@phac-aspc.gc.ca
Page details
- Date modified:
