Section 3: Evaluation of food-borne enteric illness prevention, detection and response activities at the Public Health Agency – Findings
3. Findings
This section provides a summary of the findings organized under two broad headings:
- Relevance: the need, federal public health role and priority in preventing, detecting and responding to food-borne enteric illness.
- Performance: the effectiveness, efficiency and economy of the Public Health Agency’s activities in this area.
This summary is based on an analysis of the descriptive information found in available documents and on the themes that emerged from interviews with key informants.
3.1 Relevance: the need, federal public health role and priority in preventing, detecting and responding to food-borne enteric illness
3.1.1 Many Canadians experience food-borne enteric illness each year
Estimating the true number of illnesses caused by a specific food-borne pathogen each year is a challenge. Data on the burden of illness are difficult to obtain because acute enteric food-borne illnesses are under-diagnosed and under-reported, including enteric illnesses due to foreign travel. An unknown proportion of ill people do not consult a doctor and many doctors never detect the causative agent because a stool sample was not collected or the laboratory testing was unable to identify the pathogen. Moreover, not all laboratory isolates are routinely forwarded to laboratories.Footnote 16 A study estimating the rate of under-reporting for infectious gastrointestinal illness in Ontario found that for each reported case of enteric illness, an estimated 313 cases of illness occurred in the community.Footnote 17
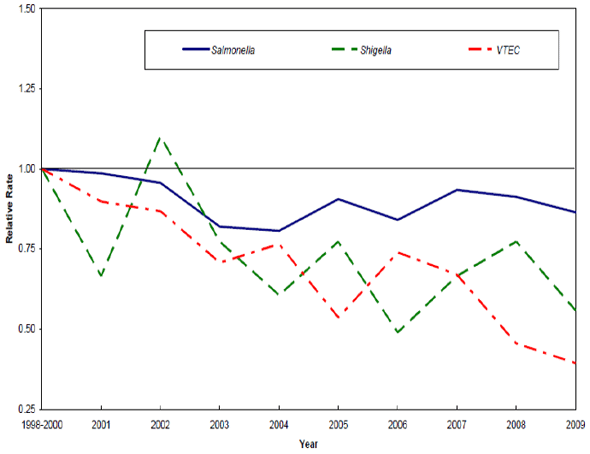
Despite this limitation, Canadian surveys of self-reported acute gastrointestinal illnesses estimate that there are about 11 million cases of food-borne illnesses every year.Footnote 18 For the last 10 years, the relative incidence of laboratory confirmed cases of Salmonella, Shigella and Verotoxigenic E. coli (VTEC)compared to the baseline years 1998-2000 have shown a decreasing trend (figure from the National Enteric Surveillance Program 2009 Annual Report).Footnote 19
Few countries routinely collect reliable epidemiological data on food-borne enteric illnesses. Even fewer have consistent and comparative data going back 20 years or so with which to identify trends.Footnote 20 The Public Health Agency collects data on food-borne illnesses submitted from all provinces and territories. In Canada, the National Enteric Surveillance Program has collected data and reported on the national incidence of food-borne pathogens since April 1997. In 2009, the National Enteric Surveillance Program recorded a total of 14,262 cases of enteric-associated infections. The most commonly reported organisms were Salmonella (43 per cent), enteric viruses (22 per cent), Campylobacter (12 per cent), parasites (11 per cent), Shigella (4 per cent) and E. coli (4 per cent).Footnote 21
Figure 3: Trends of Laboratory-Confirmed Bacteria
Text Equivalent - Figure 3
Figure 3 illustrates trends in laboratory-confirmed cases of Salmonella, Shigella and Verotoxigenic E. coli (VTEC) in Canada from the baseline years of 1998-2000 through to 2009. Specifically, relative incidence rates for Salmonella, E. coli and Shigella since 2001 are compared to the baseline years 1998-2000. According to data collected by the National Enteric Surveillance Program (NESP) through laboratory confirmed cases, there is a decreasing trend of bacteria-related cases. In 2009, the number of Salmonella Enteridis infections was lower than in 2008 but still remains at an elevated level. Some serotypes, such as Salmonella Enteridis have increased due to the adaptation process of the pathogen and changing environmental factors. Reported cases of E. coli infection dropped in 2009 and Shigella infections overall decreased in 2009, while Shigella flexneri identifications increased and outnumbered Shigella sonnei infections for the first time since NESP was established.
Source: National Enteric Surveillance Program, Annual Summary 2009
Although the overall number of laboratory confirmed bacteria-related cases is decreasing, some serotypes (such as Salmonella Enteridis) and enteric viruses have increased. This is a result of an evolution and adaptation process to ever changing environmental factors.Footnote 22
Campylobacter is the most commonly reported enteric organism in Canada. However, isolates are not routinely forwarded to provincial and federal laboratories for further typing. For that reason, it is significantly under-represented in the National Enteric Surveillance Program.Footnote 23 Data from the National Notifiable Disease Surveillance System is more reflective of this pathogen in Canada. Enteric illnesses caused by toxin-producing bacteria are also underestimated due to a lack of diagnostic tools.Footnote 24
In addition to the yearly trend, most cases of food-borne enteric illness show a distinct seasonal pattern, related to certain human behavioural patterns, such as barbecuing in the summer. Food-borne enteric illnesses tend to increase during the summer, as well as in December.Footnote 25
Although most food-borne enteric illnesses are sporadic, not outbreak-related and not reported, they continue to be a threat to the health of Canadians. Most food-borne illnesses are the result of improper food handling and preparation by consumers.Footnote 26 They occur locally and are under municipal and provincial/territorial jurisdiction. However, a significant number of cases occur in clusters and outbreaks. The National Enteric Surveillance Program plays a role in detecting food-borne illness outbreaks with a provincial/territorial or multi-jurisdictional (more than one province or territory) distribution. In 2009, there were 344 outbreaks and case clusters reported to the National Enteric Surveillance Program, involving 847 ill persons. The most common organisms related to these outbreaks were Norovirus (90 per cent), followed by Salmonella (5.5 per cent) and E. coli (1.4 per cent).Footnote 27
In 2009, the Public Health Agency was involved in 50 multi-jurisdictional investigations, involving multiple provinces or territories and other countries. In 2010, the most reported organisms associated with 41 outbreak issues were Salmonella (49 per cent), E. coli (17 per cent), Listeria (17 per cent) and Clostridium botulinum (5 per cent).Footnote 28
Food-borne illnesses are frequent causes of morbidity and mortality worldwide. They are expected to continue to pose challenges to public health in the 21st century. Food-borne illness outbreaks seem to be on the rise in industrialized countries.
The global burden of food-borne illnesses is currently unknown in both industrialized and developing countries. They generate a considerable financial cost but the extent of this cost is largely unknown. Studies conducted in the United States estimate the yearly cost for Salmonella food-borne infections alone is $365 million in direct medical expenditures.Footnote 29 The annual per capita cost of acute gastrointestinal illnesses in Canada is estimated at $115. When applied to the entire Canadian population, this amounts to approximately $3.7 billion annually in healthcare and societal costs.Footnote 30
Although most people infected with enteric pathogens get well, a few may develop chronic health problems. It is estimated that two to three per cent of food-borne illness cases can develop long-term secondary complications, such as chronic arthritis and in some cases kidney damage that result in higher medical costs to society.Footnote 31
The evolution of food-borne illness
External drivers play a role in increasing the number and complexity of food-borne pathogens. Key external drivers include the following.
- Antimicrobial Resistance: Resistance to antibiotics is a significant issue for bacterial pathogens in the food chain. Antimicrobial agents used in humans, animals or plants help select and promote the dissemination of bacteria with resistance genes that can provide a direct risk of infection following ingestion or food handling.Footnote 32
- Nature of Pathogens: Well recognized food-borne pathogens such as Salmonella seem able to evolve and respond to environmental challenges. A troubling feature of E. coli is its ability to evolve types that have never previously been reported or characterized. Food-borne enteric illness outbreaks in industrialized countries have shifted from the usual problems with foods of animal origin to fresh foods such as produce and shellfish, and dry foods and ingredients such as peanuts. As a result of this adaptation process, all the improvements in production, processing and monitoring along the food-chain are not able to successfully contain the food-borne pathogens.Footnote 33
- Climate Change: Changes in the climate affect how pathogens are able to influence the safety of food.Footnote 34 For example, environmental changes likely increase pathogen levels in water, which then affects food.Footnote 35
- Consumer Demands: Since 1998, fresh leafy produce that is ready-to-eat has been responsible for multiple outbreaks of E. coli O157:H7 or Salmonella infections.Footnote 36 Microwavable food products such as pot pies, chicken nuggets and ready-to-cook pizzas have all been associated with food-borne enteric illness outbreaks. Consumers are relying more on convenience when it comes to food. Processed foods, although an easy selection, involve multiple stages of handling compared to foods that are not processed. This increases the chance of the product being contaminated.Footnote 37
- Globalization: Global food supply chains, new food technologies and cost pressures have resulted in worldwide sourcing of food products and ingredients. However, many countries are poorly equipped to respond to existing and emerging food safety problems. Not all food trading countries have strong regulatory systems.Footnote 38
- Food Industrialization: As food production has become more industrialized, “a single food processing establishment distributing its products to millions of consumers can now result in food-borne illness that is international in scope”.Footnote 39 Changes in livestock farming and industrialization of the slaughtering of animals play a critical role in the transfer of pathogens. As well, changes in food technology such as the use of vacuum packaging, which allows food to be kept longer at refrigeration temperatures, has increased the growth of bacteria.Footnote 40
- Vulnerable Populations: Segments of the population such as young children, seniors, pregnant women and anyone with a weakened immune system are more at risk once they have become sick with a food-borne enteric illness. An emerging issue is the growing population who have reduced immunity to counteract food-borne illnesses. Trends suggest that people with compromised immune systems will be a larger segment of the future population.Footnote 41
In summary, many Canadians experience food-borne enteric illness each year. Although cases are under-reported and under-diagnosed, estimates show the magnitude of this problem. The number and complexity of food-borne pathogens are further exacerbated by external drivers, such as antimicrobial resistance and food industrialization.
3.1.2 There is a federal public health role in the prevention, detection and response to food-borne enteric illness outbreaks
The Department of Health Act and the Public Health Agency of Canada Act guide the Public Health Agency’s roles and responsibilities for the prevention and response to infectious disease outbreaks. Under the Department of Health Act, the Minister of Health has a broad mandate to protect Canadians against health risks and the spread of disease. The Minister's duties, functions and powers include the investigation and research into public health, including the surveillance of diseases. Both Health Canada and the Public Health Agency can exercise various duties, functions and powers, on behalf of the Minister.Footnote 42 Under the leadership of the Chief Public Health Officer, and in collaboration with its partners, the Public Health Agency is mandated to lead federal efforts and to mobilize pan-Canadian action in preventing disease and injury. It is also mandated to promote and protect national public health.Footnote 43
Although the Public Health Agency has a mandate to lead action in preventing illness, its role in preventing food-borne illness is limited. Other government departments, namely Health Canada and the Canadian Food Inspection Agency, have specific mandates in the area of food safety. This situation will be further explained below.
3.1.2.1 The Public Health Agency’s role is clear in the detection of, and response to, food-borne enteric illness outbreaks
Role in detecting and responding
There is a federal public health role in detecting and responding to food-borne enteric illness. The federal public health role in a multi-jurisdictional context, which includes conducting national surveillance of illnesses, coordinating national laboratory and epidemiological investigations, leading communications to the public, and coordinating outbreak response, is confirmed by the FIORP and understood by food safety partners. The FIORP sets out the key guiding principles and operating procedures, including roles and responsibilities during the investigation of, and response to, multi-jurisdictional food-borne enteric illness outbreaks in Canada.Footnote 44 It was collectively developed by the Public Health Agency, Health Canada and the Canadian Food Inspection Agency, in consultation with the provinces and territories.
For this evaluation, all key informants interviewed agreed that the Public Health Agency’s role in detecting and responding to food-borne outbreaks is clear and understood. The FIORP exercises were mentioned as key activities that helped all partners to clarify roles, understand the context under which partners operate and build strong relationships. This is further substantiated by a 2011 evaluation report from the Canadian Food Inspection Agency on interdepartmental interfaces.Footnote 45
The Public Health Agency’s role in detecting and responding to food-borne enteric illness outbreaks is reiterated through other key documents, such as Memoranda of Understanding and program authorities. Through the funding of activities, the Public Health Agency was given the authority to conduct surveillance, develop laboratory technology, lead protocol and emergency plan development and conduct epidemiological investigations, which confirm that these are recognized federal public health roles.
Role in communicating to the public
The FIORP and the federal Food Safety Communications Protocol define and further clarify the Public Health Agency’s leadership role in communicating to the public during a multi-jurisdictional outbreak. According to key informants, the communications roles and responsibilities of federal food safety partners are much clearer now than they were prior to the 2008 Listeriosis outbreak. However, there are instances where communication roles will need to be defined as the situation unfolds.
According to these protocols, the Public Health Agency takes the lead in communicating to the public when there are multi-jurisdictional outbreaks (i.e. outbreaks in more than one province and/or territory). To communicate prevention messages when there are no identified outbreaks, the Public Health Agency provides expertise, if needed, to support Health Canada and the Canadian Food Inspection Agency’s communication activities.
Although roles and responsibilities in communicating to the public have been clarified, communications to the public under unusual circumstances, especially when there are outbreaks in other countries but no human illnesses in Canada, remain a gray area. Key informants felt it was not clear what role the Public Health Agency should play in communicating to the public in such a case. Some felt that the Public Health Agency should lead in communicating prevention messages to the public. According to the risk management scenarios developed for the Food Safety Communications Protocol, Health Canada is the federal government communications lead to respond to international situations relating to significant food-borne contamination issues. Once an illness has been identified in Canada, however, the Public Health Agency is the federal government lead in communicating to the public.
Role in capacity building
There is also an ongoing need for a federal public health role to assist in building capacity in the provinces and territories. The Public Health Agency of Canada Act and the Department of Health Act both refer to a federal public health role in cooperating with provincial and territorial governments. Some of the key roles of the Public Health Agency, according to the Public Health Agency of Canada Act, are to foster collaboration and coordination in the field of public health and to promote cooperation and consultation with the provinces and territories.
The specific roles for capacity building are outlined in the funding authorities for Listeriosis and the Food and Consumer Safety Action Plan, which confirm the Public Health Agency’s role in some capacity building activities — FIORP exercises, the PulseNet Canada training program and outbreak response tools. These activities have all been undertaken to assist provinces and territories in improving their outbreak response capacity. While some may be based on time-limited funds, it provides context for the Agency’s role in capacity building.
As presented above, there is a federal public health role in detecting and responding to food-borne enteric illness. The Public Health Agency’s role in this area is clear and well understood.
3.1.2.2 The Public Health Agency’s role is clear in upstream prevention surveillance activities
The Public Health Agency’s role is clear in active surveillance for antimicrobial resistance (CIPARS) and source attribution (C-EnterNet). The Food and Consumer Safety Action Plan funding gave the Public Health Agency the authority to lead the CIPARS and C-EnterNet programs. Through the key informant interviews, federal partners confirmed the importance of the Public Health Agency’s role in leading these surveillance activities. The Action Plan confirms that food safety is a shared responsibility between industry, consumers and government. The funding received is intended to allow a more proactive and integrated approach to identify and address risks in the food supply.
There are Memoranda of Understanding guiding the work of both surveillance programs. These documents describe the Public Health Agency’s role in these surveillance activities.
The Centers for Disease Control and Prevention undertakes similar activities in the United States through FoodNet (the equivalent to C-EnterNet) and the National Antimicrobial Resistance Monitoring System (the equivalent to CIPARS). The source attribution function under the FoodNet program, however, covers a wider proportion of the population and is narrower in focus (human health surveillance versus the Public Health Agency’s human health/animal/food/environmental surveillance).
3.1.2.3 The Public Health Agency’s role is less clear for other upstream prevention activities
The other upstream prevention activities the Public Health Agency carries out are conducted by the Laboratory for Food-borne Zoonoses. This laboratory focuses its work on food hazards, which entails the analysis of animals, food products and water samples. The Laboratory for Food-borne Zoonoses therefore does not look at human clinical samples, which are analyzed by the National Microbiology Laboratory at the request of partners and used to inform the outbreak detection and response activities of the Centre for Food-borne Environmental and Zoonotics Infectious Diseases.
The work conducted by the Laboratory for Food-borne Zoonoses, in conjunction with other Public Health Agency partners, is strictly focused on upstream prevention and is also referred to as veterinary public health or the interaction of human, environment and animal health. This is in line with the One Health concept. (See following text box for further information)
The Laboratory for Food-borne Zoonoses conducts risk modelling for the food safety system. These activities predict the points in the food safety system — whether at the farm, processing or retail-level — where interventions would reduce human health risks to public health. It includes the development of quantitative risk assessments and models. Risk assessments identify specific food hazards such as location (e.g. on the farm), exposure route and any potential human exposure to food-borne pathogens while risk models look at multiple interventions (e.g. at food processing plants) and estimate which intervention would provide the optimal solution for reducing human illnesses and saving costs.
- building robust and well-governed public and animal health systems
- preventing regional and international crises by controlling disease outbreaks through national and international emergency capabilities
- promoting collaboration across sectors and disciplines
- targeting disease control programs through strategic research.
The Memorandum of Understanding between Health Canada, the Public Health Agency and the Canadian Food Inspection Agency mentions the risk assessment activities conducted by the Public Health Agency. The Food and Consumer Safety Action Plan funding also gave the Public Health Agency the authority to conduct risk modelling activities.
The Laboratory for Food-borne Zoonoses also conducts research synthesis, which analyzes the scientific literature on food safety risks, including animal health risks and risks associated with the consumption of food products, to determine the best scientific evidence. This work is usually undertaken to inform the work of other activities, especially health risk modelling activities. These activities can then rely on sound literature to undertake further research and make decisions.
In addition, the Laboratory for Food-borne Zoonoses develops laboratory tools and methods to improve identification of pathogens. This includes reference services to provide information about food-borne pathogens in non-human samples (animal and food products) to support surveillance programs and source attribution.
However, federal partners and some internal key informants expressed confusion over the activities conducted by the Laboratory for Food-borne Zoonoses. Overall, internal and external key informants felt that the Public Health Agency’s role in some of the upstream prevention activities carried out by the Laboratory for Food-borne Zoonoses was not clear. Some internal informants did not understand why the Public Health Agency was undertaking research focused on food products and animals, while some internal and external informants questioned whether certain activities such as laboratory testing and risk modelling of animal and food products should be carried out by Health Canada or the Canadian Food Inspection Agency given their respective mandates.
Some key informants noted that these activities may respond to gaps not filled by others. They may also be conducted by the Laboratory for Food-borne Zoonoses as a result of its history in the federal government. It was a part of Agriculture and Agri-Food Canada until 1996 when it was transferred to Health Canada during the creation of the Canadian Food Inspection Agency, then subsequently transferred to the Public Health Agency when it was created in 2004.Footnote 46 These changes are reported to have been made to allow for a more adequate fit within the federal government to address the One Health concept, which is essentially a public health initiative. There is limited information available on the implementation of the One Health concept at the Public Health Agency. However, the Infectious Disease Prevention and Control Branch is considering the implementation of this approach to guide the Branch’s food-borne, zoonotic, environment, early diagnostic and collaboration activities. This is outlined in their 2011-2016 Strategic Plan.
Ultimately, Health Canada is responsible for establishing the policies, regulations and laws that govern food safety in Canada.Footnote 47 The Canadian Food Inspection Agency is responsible for enforcing those regulations through ongoing monitoring of products, food safety investigations and enforcement (i.e. product recalls).Footnote 48 Agriculture and Agri-Food Canada assists food producers in the area of product development and marketing, in addition to providing assistance in developing and maintaining safe food practices.Footnote 49 Given these roles, there appears to be duplication in these areas.
- The Canadian Food Inspection Agency and Health Canada, for their own monitoring activities, collect food and animal product samples. The Public Health Agency also collects samples for the purpose of its active surveillance systems (CIPARS and C-EnterNet). As recommended in the C-EnterNet Evaluation,Footnote 50 activities may be better integrated to avoid duplication of data collection. The Public Health Agency has looked into integration of CIPARS and C-EnterNet sampling and, where feasible, samples are collected to address the sampling needs of both surveillance systems. However, there does not appear to be much progress in integrating other government departments’ sampling activities.
- Risk modelling activities look at the areas in the food continuum where health risks are greater. In addition to the Public Health Agency, Health Canada, Agriculture and Agri-Food Canada and the Canadian Food Inspection Agency conduct activities in this area. Some examples are listed below.
- Health Canada conducts health risk assessments as part of its mandate to determine the risks associated with product consumption.
- Agriculture and Agri-Food Canada conducts food research on risks to determine routes of product contamination.
- The Canadian Food Inspection Agency conducts risk profiling and prioritization activities to determine food hazards along the food continuum and to prioritize food safety risks.
Although there have been annual meetings organized to discuss risk assessment activities and priorities in response to the funding received through the Food and Consumer Safety Action Plan, federal food safety partners expressed concern over potential duplication of activities.
The upstream prevention activities conducted by the Laboratory for Food-borne Zoonoses in the area of risk modelling, research synthesis and laboratory testing, do not clearly align with a typical public health role. In addition, there appears to be a risk for duplication of activities and/or a misalignment of mandates especially in the area of risk modelling.
3.1.3 Food safety is a priority for the Government of Canada, as well as for the Public Health Agency
The 2010 Speech from the Throne emphasized the Government of Canada’s commitment to strengthening Canada's food safety system. The Listeriosis outbreak was an important catalyst for improving Canada’s food safety capacity. Food safety and Listeriosis were specifically mentioned in the 2011 Budget, which described food safety as fundamental to the health and daily life of Canadian families. Budget 2011 also noted the magnitude of the Government of Canada’s investments in food safety since the Listeriosis outbreak, totaling $175 million as of that time.
However, among federal food safety partners, the Canadian Food Inspection Agency has received the majority of this funding to hire additional inspectors. The Public Health Agency’s food safety funding is significantly lower than the Canadian Food Inspection Agency’s and is split between ongoing (Food and Consumer Safety Action Plan) and time-limited (Listeriosis) funds.
Food-borne illness was identified as one of the top ten risks that the Public Health Agency faces in its 2011 Corporate Risk Profile. The Corporate Risk Profile saw as probable the likelihood that food-borne illness could impact all Canadians, with the potential for considerable health, social and economic consequences.
The Public Health Agency’s corporate documents have continually highlighted its efforts to respond to food-borne illness. The 2010-11 Report on Plans and Priorities emphasized collaboration with the Public Health Agency’s food safety partners. There is recognition that effective prevention, detection and response to food-borne illness requires the collective efforts of numerous partners within the Public Health Agency as well as other federal departments and provincial and territorial governments. The Public Health Agency’s 2010-11 Departmental Performance Report states “[our] accomplishments speak to the PHAC’s leadership in working with provinces, territories, public health practitioners and international public health agencies. These partnerships drive real progress in public health”.Footnote 51
Public Health Agency internal documents, including the Infectious Disease Prevention and Control Branch's Strategic Plan, identify food safety as a priority and significant public health issue of concern to all Canadians. The strategic plan details how in upcoming years, the Branch will develop targeted prevention and control initiatives, strengthen the national public health system and build capacity, and enhance national surveillance of infectious diseases. Achievement of these goals will be supported by specific food safety activities that capitalize on strategic partnerships, apply a One Health focus to the Infectious Disease Prevention and Control Branch's activities, and advance surveillance and science and research efforts that address food-borne illness.
Food-borne enteric illness activities of the Public Health Agency are part of Canada’s food safety system. Since the 2008 Listeriosis outbreak, food safety has continued to be a priority for the Government of Canada as well as the Public Health Agency.
3.2 Performance
Key outputs and outcomes were identified by the evaluation team in collaboration with the program area. Key outcomes include: increased coordination and integration of activities; increased generation and use of evidence; and increased knowledge and awareness of food-borne enteric illnesses. The following section explores the achievement of outcomes. It is followed by an analysis of the key challenges faced by the Public Health Agency’s activities in preventing, detecting and responding to food-borne enteric illness.
3.2.1 Detection and response activities, as well as some upstream prevention activities, are well coordinated
The detection of, and response to, food-borne enteric illness requires coordination with many partners to monitor clusters of outbreaks early, and ensure an efficient response.
Coordination of activities between epidemiological and laboratory monitoring and investigations
Epidemiological and laboratory monitoring and investigation activities are well coordinated. The activities of the National Microbiology Laboratory through PulseNet Canada are closely coordinated with the Outbreak Management Division within the Centre for Food-borne, Environmental and Zoonotic Infectious Diseases. Due to the nature of real-time surveillance, both groups communicate daily. Both groups manage the National Enteric Surveillance Program, a laboratory surveillance system for outbreak detection that is coordinated through the Canadian Public Health Laboratory Network. The National Enteric Surveillance Program’s weekly report is also a joint collaborative effort.
Formal coordination activities include weekly meetings between PulseNet Canada and the Outbreak Management Division of the Centre for Food-borne, Environmental and Zoonotic Infectious Diseases. PulseNet Canada provides detailed updates on any clusters detected, reported infections caused by similar strains and other laboratory issues. Issues are identified for follow-up and action.
These two complementary laboratory systems lead to information sharing and a coordinated assessment of the laboratory evidence during multi-jurisdictional epidemiologic investigations. Other formal collaborations are the weekly National Food Safety calls that include all federal laboratories and departments with a food safety mandate.
Coordination of outbreak management activities
The Centre for Food-borne, Environmental and Zoonotic Infectious Diseases’ Outbreak Management Division plays a strong coordination role in detecting and responding to food-borne enteric illness outbreaks affecting more than one province, territory or country. To conduct its work, the Division works closely with many partners within and outside of the Public Health Agency, including the Canadian Food Inspection Agency, Health Canada, provinces/territories and international partners. The Division’s involvement in outbreak issues ranges from active monitoring to coordination of information, providing content expertise, and managing an outbreak response. The Outbreak Management Division also works with provinces and territories to expand their use of the web-based Outbreak Summaries Reporting System, which can be accessed by public health professionals through the Canadian Network for Public Health Intelligence application.
In 2010, the Outbreak Management Division was notified of more than 200 food-borne illness issues and followed up with actions for 41 of them. Of the 41 issues, 36 were human illness investigations (e.g. human illness first identified) while five were food safety issues (e.g. contaminated food first identified). The most common way that the Outbreak Management Division was informed of outbreak issues was through a direct communication from a province or territory (46 per cent of cases). The remaining case notifications came from Public Health Alerts and through the National Enteric Surveillance Program, as well as federal and international partners.
In the 2010-11 fiscal year, the Outbreak Management Division led four Outbreak Investigation Coordinating Committees under the revised FIORP. Internal and external key informants involved in these committees have all noted their appreciation of the work conducted by the Outbreak Management Division in terms of ongoing and timely communications and the quality of the services provided. The Outbreak Management Division’s strong leadership was also noted.
Coordination of laboratory detection and response activities
There is a strong coordination of laboratory detection and response activities through the certification of member laboratories and the identification of clusters of outbreaks. This work is conducted by the National Microbiology Laboratory through PulseNet Canada, a virtual electronic network which ties provincial public health laboratories and some federal laboratories together by linking their computers and databases. This national network is dedicated to tracking the DNA fingerprints of human food-borne pathogens.
Through the National Microbiology Laboratory’s work in PulseNet Canada certification, the number of personnel certified to perform laboratory tests and analysis of results across the country has increased. Testing and analysis of samples has also increased (see figure below for the percentage of cases that were analyzed by PulseNet member laboratories and shared with PulseNet Canada). In 2010, 100 per cent of Listeria cases were tested; 88 per cent of E. coli O157:H7; and 48 per cent of Salmonella cases. All provinces with the exception of Alberta and Ontario perform DNA fingerprinting on almost all cases of Salmonella (Ontario and Alberta do not have the resources to perform DNA fingerprinting on every case).
| 2006 | 2007 | 2008 | 2009 | 2010 | |
|---|---|---|---|---|---|
| E. coli | 74% | 95% | 86% | 91% | 88% |
| Salmonella | 20% | 35% | 34% | 36% | 48% |
| Shigella | 3% | 30% | 34% | 20% | 35% |
| Listeria | 5% | 31% | 44% | 74% | 100% |
| Source: PulseNet Canada document titled Proportion of Cases Captured by PulseNet | |||||
Through PulseNet Canada, the National Microbiology Laboratory coordinates the identification of clusters of outbreaks by analyzing the pulsed-field gel electrophoresis (PFGE) patterns posted in the system. Once these PFGE patterns are generated, they are entered into an electronic database of DNA fingerprints at the National Microbiology Laboratory, which are available on the system. At any given time there are approximately 70 to 100 active clusters identified in the PulseNet Canada discussion board. According to key informant interviews, all member laboratories routinely verify their data to confirm whether or not there are matches in their provinces.
Once clusters are confirmed as food-borne outbreaks requiring an Outbreak Investigation Coordinating Committee, the National Microbiology Laboratory leads laboratory investigations by coordinating activities with provincial member laboratories. This work includes submission of requests to provincial member laboratories for DNA fingerprinting on specific organisms.
Coordination of laboratories through the Network of Networks Initiative
Another activity demonstrating the Public Health Agency’s coordination role is its participation on the Canadian Food Inspection Agency’s integrated national network, referred to as the Network of Networks Initiative. The goal of the initiative is to integrate all federal and provincial laboratories on the human, animal and food side. This initiative was established following recommendations from the Weatherill Report.
The Public Health Agency and the Canadian Food Inspection Agency hosted a national Network of Networks workshop in 2011 with 60 representatives from Canada's federal, provincial, private and university laboratories. Some of the topics discussed included considerations for the formation of an integrated network and strategies to move forward. By June 2012, a business case for the creation of an integrated laboratory and response network is expected to be completed.
According to key informants, the initiative will be built upon the existing principles and relationships already encompassed by PulseNet Canada as a model of good integration of federal, provincial and territorial partners that share both public health and food data for the purposes of coordinated response activities.
Coordination of communication activities
Federal food safety communications are well coordinated. The Canadian Food Inspection Agency, Health Canada and the Public Health Agency collaborate to ensure that the three departments/agencies have consistent messages on food safety. Through the revised Foodborne Illness Outbreak Response Plan, guidance on communicating during an outbreak was developed to share with all communication partners.
The federal Food Safety Communications Protocol has been tested twice: once in November 2010, and again in February 2011; these tests were interdepartmental training exercises. Both internal and external key informants have pointed to the frequent communications as helping collaboration among partners. Strong partnerships have developed both at the working level and the senior management level through the Federal Food Safety Communications working group.
The provinces and territories sit on the Public Health Network Communications Working Group, at the Director General level and the working level, helping to ensure collaboration.
Finally, the Public Health Agency’s Communications Directorate is part of the Global Health Security Initiative Communication Group. They maintain senior level communication contact with the United States (the Centers for Disease Control and Prevention and the Food and Drug Administration) to allow for information sharing on food-borne illness issues and coordinate communications at the international level.
Coordination of detection and response activities with international partners
There are both formal and informal coordination mechanisms at the international level with the United States Centers for Disease Control and Prevention. PulseNet Canada has a formal link including a Memorandum of Understanding with the United States and their PulseNet database. This allows for read-only access to each other’s database and access to PulseNet International Network to monitor laboratory surveillance for emerging bacterial pathogens. According to key informants, the Outbreak Management Division has established an informal agreement with the United States Centers for Disease Control and Prevention for the exchange of non-identifying information on confirmed cases of food-borne human enteric illnesses to manage outbreaks.
In addition to collaboration through PulseNet, the Outbreak Management Division collaborates directly with the United States on epidemiological investigations, usually involving coordination of information for investigations with a few Canadian cases.
The Outbreak Management Division also coordinates activities with international partners on travel issue investigations, where Canadians travelling abroad become ill. This collaboration is often in the form of information sharing; including the sending and receiving of International Health Regulations notifications. In 2010, Canada sent notifications regarding travel issues to Cuba, Mexico and the Dominican Republic. In 2011, during the German E. coli outbreak, the International Health Regulations National Focal Point Office and the Outbreak Management Division communicated daily to provide the World Health Organization with updated information on the cases potentially linked to the outbreak.
Coordination of source attribution surveillance
C-EnterNet activities are well coordinated within and outside of the Public Health Agency. The C-EnterNet program is jointly managed by the Centre for Food-borne, Environmental and Zoonotic Infectious Diseases and the Laboratory for Food-borne Zoonoses. The Centre is leading the human health side while the Laboratory for Food-borne Zoonoses is leading the food and animal side. According to interviewees there is clarity about the respective roles more broadly.
Each sentinel site has a Steering Committee for information sharing and validation. Sentinel sites have built strong partnerships with the local public health unit, private laboratories, water and agri-food sectors, as well as the provincial and federal institutions responsible for public health, food and water safety. In addition, an advisory committee composed of governmental and non-governmental stakeholders provides advice and guidance to the program through quarterly planning meetings.Footnote 52
The C-EnterNet evaluation found that there may be potential for better collaboration between C-EnterNet and CIPARS, especially in terms of data collection. To address this challenge, C-EnterNet and CIPARS have compared activities as well as results and identified, where feasible, potential areas to streamline common data collection requirements.
Coordination of antimicrobial resistance surveillance related to food-borne enteric illness
The Public Health Agency has successfully maintained effective coordination and communications with partners in the surveillance of antimicrobial resistance related to food-borne enteric illness. In partnership with numerous private and public sector groups, CIPARS coordinates the national surveillance of antimicrobial resistance in bacteria from humans, animals and food. The Public Health Agency’s activities are well recognized, and appreciated, at the national and international level.
- The CIPARS surveillance system was developed and implemented in partnership with numerous private and public sector groups, with support and coordination from the Public Health Agency, through the National Steering Committee on Antimicrobial Resistance in Enterics.
- CIPARS worked in partnership with Health Canada and the Canadian Food Inspection Agency on international projects, such as the Health Products and Food Branch Codex Task Force on Antimicrobial Resistance Team. The Codex Alimentarius (latin for 'food code') was originally set up in the 1960s by the Food and Agriculture Organisation (FAO) and the World Health Organisation (WHO) to guide and promote the elaboration and establishment of definitions and requirements for foods, to assist in their harmonization and, in doing so, to facilitate international trade.Footnote 53 The Laboratory for Food-borne Zoonoses group was awarded the Health Canada Assistant Deputy Minister Award for Collaborative Leadership for its work.
- CIPARS data are available to all partners through customized reports. In addition, all partners are invited to participate in analysis meetings where trends are discussed.
- All external key informants said they appreciate that the Public Health Agency takes into consideration their priorities. All key external informants noted the quality and timeliness of data as well as the regular communications that the Public Health Agency undertakes to keep partners informed of activities and findings.
In summary, one of the Public Health Agency’s key roles in detecting and responding to food-borne enteric illness is to coordinate activities. The evaluation found that the Public Health Agency plays a strong coordination role in monitoring potential food-borne enteric illness outbreaks through ongoing formal and informal communications among federal departments and provincial laboratories. The Public Health Agency also plays a role in international coordination by collaborating with the United States Centers for Disease Control and Prevention, and other government departments through upstream prevention surveillance activities.
3.2.2 Some food-borne enteric illness activities are well integrated across the Public Health Agency
Some of the detection and response activities are well integrated within the Public Health Agency. The Centre for Food-borne, Environmental and Zoonotic Infectious Diseases, the National Microbiology Laboratory and Communications Directorate have integrated activities, especially in detecting and responding to food-borne enteric illness outbreaks.
All groups communicate on a regular basis to prepare for potential multi-jurisdictional outbreaks. As reported in previous sections, there are weekly meetings between National Microbiology Laboratory’s PulseNet Canada and the Outbreak Management Division of the Centre for Food-borne, Environmental and Zoonotic Infectious Diseases. Key informants were satisfied with the current level of collaboration.
The Outbreak Management Division and the International Health Regulations National Focal Point Office have integrated their activities. The Public Health Agency is the "national focal point" for Canada's communications with the World Health Organization in the event of a potential public health emergency of international concern. During the German E. coli Outbreak in the summer of 2011, the International Health Regulations Coordination Unit and the Outbreak Management Division communicated daily on the status of the Canadian case involved in the outbreak. The World Health Organization communicated its satisfaction with the prompt and thorough Canadian response.
3.2.3 Other food-borne enteric illness activities are not well integrated across the Public Health Agency
Surge capacity and surveillance platform activities do not appear to be strongly coordinated. According to key informants, there does not appear to be strong integration between the Centre for Food-borne, Environmental and Zoootic Infectious Diseases and the Office of Public Health Practice in the areas of the Public Health Reserve pilot project and the outbreak management module of Panorama, a pan-Canadian health surveillance program. Although there is collaboration through meetings and demonstrations, program staff are not consistently aware of the overall status, progress and next steps for these two projects.
There is limited evidence of the integration of the Laboratory for Food-borne Zoonoses activities with the Centre for Food-borne, Environmental and Zoonotic Infectious Diseases and the National Microbiology Laboratory. According to key informants, there is good collaboration and integration of activities with C-EnterNet, CIPARS and the development of some laboratory methodologies. However, other activities conducted by the Laboratory for Food-borne Zoonoses do not appear to be linked to detection and response activities. For instance, there is limited evidence that shows that risk modelling and research synthesis activities contribute to the Public Health Agency’s detection and response activities. Through the Food and Consumer Safety Action Plan funding, however, a systems modelling program is expected to assist the Public Health Agency in assessing health risks associated with consumption of products. This project is scheduled to be completed by the end of March 2012.
Although the Infectious Disease Prevention and Control Branch has developed a Branch-specific strategic plan and is finalizing its implementation, overall, there is no evidence of a food-specific Public Health Agency-wide strategic plan, nor a priority-setting mechanism for food-borne illness activities. The absence of an overall Agency-wide plan may inhibit the integration of activities across all Public Health Agency program areas involved in food-borne illness.
Although most of the Public Health Agency’s food-borne enteric activities are well integrated, there are areas for improvement with surge capacity and surveillance platforms activities.
3.2.4 Evidence on public health food safety risks is generated and used in surveillance and laboratory activities
Figure 5: Science to Public Health Action

Text Equivalent - Figure 5
Figure 5 illustrates the process from producing scientific evidence to influencing policy and/or public health action. In order to use evidence to make improvements, scientific evidence should be translated and assessed by policy and program areas in order to enable change and make improvements to public health.
Source: Adapted from - Canadian Centre for Management Development. (2002). Creating common purpose: The integration of science and policy in Canada's Public Service.
One of the key outputs of the Public Health Agency’s food-borne enteric illness activities is evidence. Scientific evidence should be translated by policy and program areas to enable change and improvements to food safety. In the final or ideal form, there should be changes in guidelines, legislation, or policy, especially in the upstream prevention activity area (see Appendix G for a summary of the use of evidence at the Agency). However, as key informants noted, one must recognize that science is fast but changes in legislation can be much slower.
Evidence is generated through a number of different detection and response activities such as national enteric surveillance and laboratory detection technologies, and through upstream prevention activities, including antimicrobial resistance and source attribution surveillance. Key informants were able to provide a description of how evidence was used and supplemented this description with key documents substantiating the use of evidence at the Public Health Agency.
Evidence used from enteric surveillance activities
In response to evidence generated by the Public Health Agency, improvements have been made in the detection and response of food-borne illness. Weekly National Enteric Surveillance Program reports produced jointly by the National Microbiology Laboratory and the Centre for Food-borne, Environmental Zoonotic Infectious Diseases provide the Public Health Agency and the National Enteric Surveillance Program’s provincial and territorial partners with the identification of clusters of outbreaks emerging in Canada, and therefore allow for a more timely response.Footnote 54 In addition to weekly reports, the National Enteric Surveillance Program produced four annual reports from 2006 to 2009 that provide a summary of outbreaks and case clusters reported to the program.
In addition to the National Enteric Surveillance Program, PulseNet Canada data also assists the Public Health Agency in identifying clusters of outbreaks. Overall, the percentage of cases analyzed and shared by provinces with PulseNet Canada has increased from under 5,000 cases in 2006-07 to more than 6,000 in 2010. During this time there also has been an increase in the identification of clusters. This evidence has led to a more efficient response to food-borne outbreaks.
Evidence used from laboratory activities
Current research to better understand new pathogens and new detection technology has progressed. The work of the National Microbiology Laboratory and the Laboratory for Food-borne Zoonoses in genomics provides greater knowledge about organisms. Genome sequencing is an emerging laboratory tool used to study outbreak-associated pathogens. It is a platform capable of providing the entire genetic blueprint of a pathogen and has the capacity to distinguish strains to a precise level. The National Microbiology Laboratory applied genome sequencing in response to the 2008 Listeriosis outbreak. Using the genome data and analysis that was developed during the original Listeria project, the National Microbiology Laboratory has now sequenced 29 additional Listeria genomes, in collaboration with the Canadian Public Health Laboratory Network, Health Canada and the Canadian Food Inspection Agency.
In October 2010, a large cholera outbreak began in Haiti resulting in more than 325,000 cases and more than 5,400 deaths. Upon the release of three Haiti cholera genomes in the early weeks of the outbreak, staff at the National Microbiology Laboratory applied genomic sequencing and analyses and provided a preliminary outbreak analysis to the United States Centers for Disease Control and Prevention. As a result of this work, the National Microbiology Laboratory was invited to participate in a Haiti cholera genomics working group made up of global partners. The collaboration resulted in a larger comparative study led by the National Microbiology Laboratory. Research scientists at the Centers for Disease Control and Prevention approached the National Microbiology Laboratory for guidance and training on genome sequencing in the event of a public health crisis caused by a bacterial pathogen.
The Laboratory for Food-borne Zoonoses has used whole genome sequencing on Salmonella to enhance accuracy and speed in identifying bacteria. Scientists have sequenced 24 Salmonella genomes and are currently sequencing an additional 39 Salmonella strains.
The work in genomics has led to collaboration between staff at the National Microbiology Laboratory and the United States Centers for Disease Control and Prevention on the cholera outbreak in Haiti.
The National Microbiology Laboratory leads a range of research activities intended to better understand pathogens involved in food-borne illness and to support early detection efforts. According to annual reports, for the period of 2006-10, the National Microbiology Laboratory Enteric Program was involved in 34 research projects, submitted 55 abstracts for presentation at conferences and had 90 peer review publications.
Evidence used from antimicrobial resistance surveillance activities related to food-borne enteric illness
Surveillance data produced by CIPARS related to antimicrobial resistance in food-borne enteric illness is being used at both the national and international level. Since 2006, the program has produced three annual reports as well as an annual preliminary report which is posted on the Public Health Agency website. The preliminary report contains antimicrobial results available at the time of analysis. CIPARS has been involved in 21 collaborative research studies on antimicrobial resistance and susceptibility in food sources, companion animals in the home environment and farm animals. Several studies have been published in scientific journals or have been accepted for publication.Footnote 55
Evidence from CIPARS has led to at least one key change to food safety. The Public Health Agency tracked the emergence of a specific antimicrobial resistance in chicken meat and in human cases of Salmonella Heidelberg. The antimicrobial, ceftiofur, is considered to be of very critical importance in human medicine as it is used in the treatment of serious bacterial infections. Through presentations and publications, this finding facilitated the voluntary ban of extra-label use of cetifofur in Quebec hatcheries. While the action was temporary, it resulted in the reduction of ceftiofur resistant Salmonella in both chicken meat and in humans. The findings were also used by the Veterinary Drugs Directorate at Health Canada to modify veterinary drug labels. As well, the United States Food and Drug Administration imposed a new rule banning extra-label use of ceftiofur in United States hatcheries. Internationally, the Advisory Group on Integrated Surveillance of Antimicrobial Resistance uses the experience of CIPARS to promote the adoption of a similar model by member countries.
Evidence used from source attribution surveillance activities
Data from sentinel site surveillance through the C-EnterNet program are intended to reduce the burden of enteric disease.Footnote 56 The C-EnterNet program has produced a series of information products since 2006-07 including three complete and two short annual reports, two accomplishment reports on C-EnterNet results and seven newsletters.Footnote 57 There have been over 100 presentations between 2006-07 to 2010-11 on the C-EnterNet program and results have been presented to local, provincial and international audiences. The 2010 C-EnterNet evaluation report, based on one site in the Region of Waterloo which was operational at that time, noted that the program staff authored or co-authored several peer review articles on source attribution.
Source attribution data are key because they analyze each of the many combinations of factors that can cause illness and also determine whether changes in the food safety system are effectively decreasing the prevalence of illnesses.Footnote 58 While preliminary source attribution estimates have been developed by C-EnterNet, progress is limited because there are, at this time, only two sites. This impacts the representativeness of the information produced.
Although not fully representative, C-EnterNet data provide a current assessment of trends in disease and exposures in the Canadian context enabling, in some cases, the Public Health Agency to determine the proportion of human illness that stems from various sources (e.g. undercooked chicken or raw milk). For example, the information generated at one of the sentinel sites was used at the local level to develop a raw milk information sheet that addressed the risk identified through enhanced surveillance. According to the 2010 C-EnterNet evaluation report, the information produced by the C-EnterNet program is well received by those who receive C-EnterNet documents or outputs, including annual reports and newsletters, and appears to be used by researchers and by those in service and program delivery. External key informants for this evaluation noted the value of the concept of C-EnterNet; however, none of the interviewees had used information produced by C-EnterNet to date.
Additionally, C-EnterNet data have been accessed on multiple occasions to look for potential sources in provincial/territorial and national outbreaks. For example, epidemiologists working on a recent Salmonella investigation in one province accessed C-EnterNet data on food consumption as part of their investigation.
3.2.5 There is limited evidence on the use of some upstream prevention activities
Outside of the CIPARS and C-EnterNet surveillance programs, other Laboratory for Food-borne Zoonoses upstream prevention activities, such as risk modelling, resulted in the publication of 76 research articles in peer reviewed journals in 2010-11 on topics of food-borne pathogens and public health (some were jointly conducted with Health Canada). The articles included sources of food-borne outbreaks, the burden of gastrointestinal illness and pathogens in animals and farm samples. The other Laboratory for Food-borne Zoonoses upstream activities resulted in the presentation of research results at numerous international conferences and reports that will be published in an upcoming book. Various risk models and decision analysis tools have been developed and used by international partners. In addition to all of this work, the Laboratory for Food-borne Zoonoses has participated on numerous committees, whether at the international level (e.g. Codex committees), or with federal, provincial and territorial partners.
There is therefore a considerable amount of information produced in the area of risk modelling and research synthesis, but there is limited evidence of how this work is being used by federal partners to inform further research, program and/or policy decision making.
As discussed in section 3.1.2.3, in addition to conducting work that may be duplicative of the work conducted by federal food safety partners, the role of the Public Health Agency in upstream prevention activities is not clear. Key informants noted that the risk modelling and research synthesis activities conducted by the Laboratory for Food-borne Zoonoses are not well known to the majority of food safety partners. Improved knowledge translation has been suggested so that information can be tailored to the appropriate level and needs of particular target audiences to increase the use of evidence to inform public policy.
The Science to Policy Division from the Laboratory for Food-borne Zoonoses has the analytical capability to assess and interpret information on risk factors, interventions and other interacting factors. For example, a risk model for E. coli O157:H7 in ground beef was developed to measure the effectiveness of various interventions from on-farm to processing practices, and the impact these have on the number of illnesses. While some of this work has been acknowledged internationally, there is limited demonstration of use by federal partners. The only confirmed use of evidence by a federal food safety partner has been for the multi-criteria decision analysis (MCDA) tool for pathogen prioritization. This tool has assisted the Canadian Food Inspection Agency in prioritizing its food inspection activities.
Systematic reviews of food safety research are undertaken to inform the policy decision-making process. According to a key informant, research synthesis in food safety began at the Public Health Agency to strengthen the risk modelling work. As a result, it remained a component of risk modeling and was not entrenched in an overall food safety policy decision-making process. This may help explain why there is limited evidence of how research synthesis has been used by federal partners to improve food safety.
Although a lot of information is produced from upstream prevention activities, there is limited evidence that shows the information has been used to improve the Canadian food safety system.
3.2.6 The Public Health Agency is now better prepared than before the 2008 Listeriosis outbreak to communicate to the public
Communicating during a food-borne enteric illness outbreak
Communicating public health risks is an ongoing challenge. As outlined in the Lessons Learned Review: Public Health Agency of Canada and Health Canada Response to the 2009 H1N1 Pandemic: “As a science-based organization, there are a number of times when communication will have to focus on not knowing the response but at the same time instilling confidence in the general population that the government is capable of responding”.Footnote 59 Uncertainty is linked to the basic scientific process although this may not be an easy message to communicate to the general public.
During a food-borne enteric illness outbreak, it is not unusual to have certain sources suspected at first, only to be ruled out later. In 2008, there was a Salmonella outbreak in the United States where tomatoes were suspected as the source; consumers stopped buying them, thereby costing the industry millions. It was later discovered that it was jalapeno peppers that were contaminated.Footnote 60
From May to July 2011 Germany experienced a severe outbreak of E. coli O104:H4, with symptoms including bloody diarrhoea and haemolytic uremic syndrome. The outbreak resulted in over 4,000 cases of related illness and over 50 deaths. On May 26, 2011, a public advisory was issued warning against the consumption of cucumbers, lettuce and tomatoes. At the same time, Spanish cucumbers were implicated as a likely source of the E. coli Outbreak. By June 7th, sprouts were added to the advisory list, but it was later confirmed that none of the above were responsible. Sprouts grown from Fenugreek seeds were then confirmed as the source of the outbreak.
The Public Health Agency’s Strategic Risk Communications Framework was requested by Germany after the outbreak to assist in improving their communications strategies.
Risk communications
As demonstrated by the German example (see box above), food safety communications are complex because messages often include a degree of uncertainty. As a result they can raise concern among the public. In fact, a key informant identified the proper communication of this uncertainty as the central challenge of food safety communications. Accordingly, the World Health Organization has urged countries to integrate risk communications into their response planning for public health crises, stating that “appropriate risk communications procedure fosters public trust and confidence, both of which are vital in a crisis situation”.Footnote 61
From a Canadian perspective, another dimension of this complexity is the number of players involved. In the independent review of the 2008 Listeriosis outbreak, investigator Sheila Weatherill stated that:
“From everything we heard, if there is a single issue that garnered near unanimous agreement, it is that the public was confused and did not understand what they should be doing following news of the food recalls. This is not surprising, considering the complexity of the issues involved in the outbreak and the many organizations providing varying levels of information at different points in the event”.Footnote 62
There were many different players delivering information to the public, including industry, the federal government as well as provincial and territorial governments. The key messages did not meet the public’s needs because the focus of the messages was on food safety and not public health. Furthermore, the roles and responsibilities of the federal departments involved in the Listeriosis outbreak were not well understood by the public.Footnote 63
As a result, recommendations were made in the Weatherill Report and the Public Health Agency’s Listeriosis Lessons Learned Review to address these challenges, including revision and testing of the FIORP. This revision of the FIORP, endorsed in 2010, includes an annex (Annex 11) outlining communication responsibilities to the public and those at greater risk. The review also recommended that principles of risk communications drive the federal communications strategy.
Subsequently, having recognized the need to establish guidelines to improve communications, the Public Health Agency, the Canadian Food Inspection Agency and Health Canada collaborated to develop the federal Food Safety Communications Protocol. The annex to the federal Food Safety Communications Protocol, Food-borne Incident Federal Risk Management Scenarios, outlines seven scenarios representing a sample of situations related to potential food-borne illness, with the communications actions being based on the FIORP.
In line with the recommendations made in the Weatherill Report, progress has been made in preparing communications during a food-borne enteric illness outbreak. Key tools, such as public notice templates, online content and key messages for spokespeople, have been developed. This falls in line with the needs of Canadians. In 2010, Canadians were asked to indicate their main source of information during a food-borne enteric illness outbreak. Nearly three-quarters of Canadians (74 per cent) cited traditional media (newspapers, radio and television) as their primary source of information. In contrast, only about one in six Canadians (16 per cent) listed information from websites as their main source of information.Footnote 64
In addition to messaging for the general public, fact sheets also have been adapted to ensure that messaging is appropriate for at-risk groups. A distribution list has been created for stakeholders to ensure there are additional avenues for informing those who may be at-risk during a food-borne enteric illness outbreak.
Web analytics
Without many large, multi-jurisdictional outbreaks, it is difficult to assess how well communications to the Canadian public have performed since the Listeriosis outbreak in 2008. However, there are other indirect indicators of these types of activities. The Public Health Agency’s website provides food-borne enteric illness information to the public. Measuring from December 1, 2010 to December 1, 2011, Canadians appear to be using the website as a source of information on food-borne enteric illness.
- Out of more than 31,000 Public Health Agency web pages, the Food Safety homepage ranks high in popularity (#64 in English and #179 in French).
- The level of visitor engagement with the Food Safety section overall was high because visitors spent an average of five minutes and 29 seconds on the website compared to the site average of two minutes, 16 seconds.
- Visitors to the Food Safety section viewed an average of one and a half pages per visit, and this is likely due to the fact that there are many external links within the section which drive visitors off the site.
- However, equally important, visitors to the Food Safety homepage seemed engaged, with nearly half (47 per cent) going on to a second Public Health Agency page.
- In total, there were 63,049 visits to the Food Safety section, with 95,999 page views (the number of page views refers to each time a web page was accessed).
- While the Food Safety homepage is popular and visitors to the site appear to be engaged, search engine optimization of the site could increase the amount of traffic arriving from Google (currently at 39 per cent), to bring it closer to the Public Health Agency site average of 57 per cent.
| Rank | Page Title | Page views |
Avg. Time on Page |
|---|---|---|---|
| 1 | Food Safety homepage | 35,552 | 0:01:20 |
| 2 | Food Safety homepage (French) | 12,277 | 0:01:03 |
| 3 | Listeriosis (Listeria) Outbreak Homepage | 6,204 | 0:01:24 |
| 4 | Public Advisory: E. coli outbreak - April 4, 2011 | 5,303 | 0:02:51 |
| 5 | Listeria – Protecting Your Pregnancy (French) | 4,167 | 0:03:04 |
| Source: Public Health Agency of Canada | |||
The Public Health Agency also responds to ad hoc requests for information. Between January and October 2011, there were a total of 20 requests from the media. Those requests can generally be divided into two categories: requests generated by news of an outbreak, and requests generated by a person’s research on a topic.
The Public Health Agency is in a much better position to communicate to the public than it was during the 2008 Listeriosis outbreak. In terms of communication material available to the public, it appears that Canadians are using the Public Health Agency’s website as a source of information on food-borne enteric illness.
3.2.7 There appears to be a gap in sharing standardized tools and techniques
As reported in the Canadian Food Inspection Agency’s Evaluation of Changes to Inter-Departmental Interfaces and by key informants for this evaluation, the provinces and territories look to the federal government to provide them with resources and tools to facilitate an outbreak response.
Capacity building for outbreak management guidance and tools
Federal, provincial and territorial stakeholders have invested time and attention to better manage and respond to food-borne enteric illness outbreaks. They have enhanced documentation, clarified roles and responsibilities and updated governance structures.Footnote 65 According to key informants, the FIORP has provided clarity on roles and responsibilities and has assisted provinces and territories in understanding multi-jurisdictional outbreak response. Training exercises for the FIORP have helped to build relationships. To best meet the training needs of each province and territory, working groups were established to facilitate collaboration and to identify specific training objectives. Various scenarios were developed and tested according to the needs of the provinces and territories.
With funding from the Food and Consumer Safety Action Plan, the Public Health Agency has expanded the capacity of the web-based Outbreak Summaries Reporting System, which was developed with extensive provincial and territorial input. The System allows standardized dissemination of the results of disease outbreak investigations. It provides an opportunity for provinces and territories to share best practices. An enteric module of the application has been launched in the Atlantic provinces and British Columbia, and discussions are underway to extend the application to other jurisdictions in 2011-12.
Capacity building for epidemiological investigations
While progress has been made, the provinces and territories require additional guidance so that managing and responding to multi-jurisdictional food-borne enteric illness outbreaks is consistent.Footnote 66 Also, there appears to be a gap in providing the provinces and territories with standardized tools and techniques to conduct epidemiological investigations.
The capacity-building activities conducted by the Outbreak Management Division are mostly training on outbreak investigations. Some of the training offered in 2010-11 included, but is not limited to:
- training sessions offered at the PulseNet Canada Meeting 2010 and the Field Services Training Institute
- a three-week course titled Epidemiology in Action offered primarily to Field Epidemiologists and Public Health Officers
- speaking engagements with students and guest lectures at various universities
- six-day training sessions in Kenya offered to 40 participants from 10 African countries, to enhance collaboration with and between countries (training coordinated by the Global Food Network and offered in partnership with the Surveillance Division of the Centre for Food-borne, Environmental and Zoonotic Infectious Diseases).
In addition to the Outbreak Management Division, the Office of Public Health Practice also offers training for epidemiologists. In 2010-11, the training offered included but is not limited to:
- Field Services Training Institute
- Epidemiology in Action
- Skills Online (Basic Epidemiological Concepts, Epidemiological Methods, Outbreak Investigation and Management, Introduction to Surveillance, Communicating Data Effectively, Introduction to Biostatistics, Introduction to Public Health in Canada).
Capacity building for public health laboratories
With the development of new technologies to help improve the detection of food-borne enteric illness, additional laboratory capacity building (i.e. people, equipment and training) will be required on an ongoing basis. Time-limited funding received to address the 2008 Listeriosis outbreak helped develop public health genomics expertise and the PulseNet Canada training program. However, these are not permanent resources.
PulseNet Canada has built and connected a decentralized network of laboratories across Canada, including training to the provincial public health microbiology laboratories, as well as equipment (for pathogen fingerprinting), PulseNet software (to complete the initial steps of fingerprint analysis), and standardized methods and quality assurance programs (to ensure data accuracy, comparability and interoperability across the network). PulseNet member certification and method standardization is an ongoing activity. As noted above, PulseNet has been providing tools and support to provinces so that they can do the testing and analysis themselves. As a result, there has been an increase in the number of laboratories and personnel certified to conduct testing and analysis of E. coli O157, Salmonella, Shigella and Listeria across the country.
According to the Canadian Food Inspection Agency’s Interdepartmental Interfaces Evaluation, additional improvements are required to improve the capacity of provincial laboratories. While data are now shared more easily during food-borne illness occurrences, not all provincial laboratories have the capacity to implement the new testing methods developed by the National Microbiology Laboratory. Some provinces continue to send samples to the National Microbiology Laboratory for testing. According to key informants, the provinces that are not adopting new testing methods do not have the internal capacity. For these provinces, the National Microbiology Laboratory continues to test on their behalf, as part of its national role. In addition, the federal laboratory has been working closely with three provinces to increase capacity. For example, a Public Health Agency laboratory liaison technical officer trained in DNA fingerprinting has been deployed to a provincial laboratory that needs capacity. As well, the National Microbiology Laboratory has hosted staff from provincial laboratories in an effort to build capacity. Plans are underway for these provinces to begin their own testing.
The model for PulseNet Canada is to ensure a standardized method of DNA fingerprinting, a standardized analysis platform and operating procedures to build the capacity of provincial laboratories across Canada to conduct their own testing locally. The goal is to transfer method development, evaluation and technology back to the provinces. The continuing work is to maintain testing proficiency to ensure an appropriate level of quality control, as well as to continue to build capacity in new methodology. For example, PulseNet Canada is working to increase the capacity of members to perform DNA fingerprinting on non-O157 E. coli. The new methodology for these organisms is built into PulseNet Canada and it provides instruction and technical guidance to member laboratories on use of the new method. Increased capacity for testing and analysis in non-O157 E. coli will improve efficiency and overall capacity for PulseNet Canada to detect outbreaks of this emerging bacterium.
The National Microbiology Laboratory provides provincial laboratories with a menu of recommended tests specific to each pathogen. According to key informants, the role of the federal laboratory is to carry out applied research that can help to develop new testing methods, as well as to collaborate with the provinces to identify the gaps and methods that can be developed. The federal laboratory role is to provide the most advanced testing on organisms to identify the specific serotype. Funding from the Food and Consumer Safety Action Plan helped the National Microbiology Laboratory to develop the ability to perform the latest generation fingerprinting method (Multiple Loci VNTR Analysis or MLVA). This method was certified for PulseNet Canada by the United States Centers for Disease Control and Prevention. PulseNet Canada now offers E. coli MLVA laboratory service to all PulseNet Canada members.
The need for regular training on the DNA fingerprinting technique and on the interpretation of results will be addressed in part by a web-based training program being developed by PulseNet Canada. This training will enable more personnel in the laboratories to become certified. A comprehensive and fully interactive online training program is expected to be launched by March 31, 2012. It is intended to reduce the need for on-site training and to ensure that training needs are met in the most efficient manner.
In summary, the provinces and territories look to the federal government to provide them with tools to facilitate an outbreak response. Capacity building activities for public health laboratories have resulted in new innovative tools as well as training opportunities. Capacity building activities for epidemiologists, on the other hand, could be enhanced.
3.2.8 Epidemiological outbreak capacity to respond to food-borne enteric illness outbreaks could be improved
Once an outbreak has been identified and a diagnosis has been confirmed, the food-borne illness detective (or epidemiologist) collects information from patients about possible risk factors, such as what they ate, where they went, how many animals and sick people they had contact with, etc. If most patients consumed a particular product or attended a similar function, a hypothesis is generated and investigated further through case control studies (i.e. comparing the dietary intake of ill individuals to individuals who have similar experiences and characteristics but are not ill) among other methods. This can be very difficult since most people do not remember what they ate the day before and most cases of food-borne enteric illness are caused by food eaten several days, or potentially weeks, before any signs of the illness. For instance, E. coli takes three to ten days for symptoms to appear while it takes up to 60 days for Listeria.
Once all information has been collected, results are examined in conjunction with laboratory results of human and/or food samples (when available). The hypothesis is then confirmed or rejected. If rejected, a second hypothesis is developed along with additional gathering of information.
Once a source has been identified, public health action such as a recall can occur and the results of the epidemiological investigation can be summarized.
Epidemiological capacity is the foundation for a public health organization’s ability to respond to and investigate outbreaks. Epidemiologists are public health professionals with training, expertise and experience in studying the occurrence, distribution and determinants of diseases in a defined population, such as one affected by food-borne illness.
The Public Health Agency has several initiatives that identify and provide additional epidemiological capacity in the event of significant multi-jurisdictional outbreaks, as listed below.
- The Public Health Agency has conducted a Human Resources Skills Survey which assessed the number of potentially available epidemiologists at the Public Health Agency. This roster has been used on a variety of occasions, including during the H1N1 response in 2009, as it identifies individuals who have self-reported epidemiologic skills and knowledge. As of October 2011, there were approximately 100 people on the list.
- The Canadian Field Epidemiology Program and the Canadian Public Health Service are other options that can be used by the provinces or territories in an outbreak. The programs provide training in epidemiological investigations.
- Through time-limited Listeriosis funding, the feasibility of a public health reserve of provincial or territorial epidemiologists is currently being examined as another option that provinces and territories could use in the event of a food-borne outbreak. In addition, this pilot project is expected to provide a framework for integrated surge capacity for the Public Health Agency.
The coordination of all of these resources, however, is not evident. In the event of a large multi-jurisdictional outbreak, the Public Health Agency does not appear to have an overarching surge capacity plan to assist the Outbreak Management Division in (a) coordinating epidemiological investigations, (b) leading the Outbreak Investigation Coordinating Committee which coordinates all aspects of the investigation (laboratory, epidemiological and food safety investigations), or (c) providing additional provincial and territorial epidemiological capacity during a significant outbreak.
As food-borne outbreak epidemiology employs specific tools and methods, trained resources need to be continually available to provide necessary surge capacity. Some key informants mentioned that the number of epidemiologists may not be an issue within the Public Health Agency, although what may be lacking is a single window or coordination unit that supports the identification and mobilization of resources. However, other key informants mentioned that investigating food-borne enteric illness outbreaks requires specific skills and knowledge that need to be developed prior to any outbreak to ensure a timely and efficient response. According to these key informants, in addition to the Outbreak Management Division relying on time-limited resources allocated through the Listeriosis funding, there does not appear to be Public Health Agency epidemiologists trained in investigating food-borne enteric illnesses to meet possibly emerging demand, external to the Outbreak Management Division.
Although the Public Health Agency can rely on the Food-borne Illness Emergency Response Plan to managean outbreak with its federal food safety partners, there do not appear to be one overarching surge capacity plan that identifies and coordinates epidemiological capacity within the Public Health Agency and within provinces and territories. As seen in the Germany E. coli outbreak (see Appendix B), Germany’s federal public health organization had to rapidly deploy 100 epidemiologists for outbreak response and related support. The Public Health Agency lacks a specific epidemiological surge capacity plan to manage a similar large food-borne outbreak.
3.2.9 Exercising of the Foodborne Illness Outbreak Response Protocol resulted in a better understanding of roles and processes during a multi-jurisdictional outbreak
The Weatherill Report on the 2008 Listeriosis outbreak identified gaps in the Canadian food safety system and made 57 recommendations for improvement. The Public Health Agency was assigned the lead for a number of the recommendations, in particular recommendation number 24, which pertains to revisions and training exercises on the FIORP. Specifically, this recommendation states that federal, provincial and territorial governments should:
- complete the revision of the FIORP currently underway at the earliest opportunity
- include in the FIORP periodic mock exercises to validate that the Protocol is fully understood by federal, provincial, territorial and local governments.
Following the 2010 revisions to the FIORP, the Public Health Agency’s Outbreak Management Division made a plan to validate the Protocol in each of the 13 provinces and territories through a series of bilateral training exercises. Between January 17, 2011 and April 6, 2011, 13 bilateral training exercises were held across Canada and were attended by over 640 participants, including Medical Officers of Health, program managers and directors, public health inspectors/environmental health officers, veterinarians, food safety specialists, epidemiologists, public health nurses, communications staff, microbiologists and laboratory technologists. In addition, federal representatives from the Public Health Agency, the Canadian Food Inspection Agency, and Health Canada, were present at the training exercises as participants and observers.
The training exercises included a mock outbreak scenario to help participants practice all the components of the Foodborne Illness Outbreak Response Protocol in a multi-jurisdictional outbreak situation. To measure the knowledge participants gained through the exercises, a pre- and post-exercise evaluation form was given to them. The figure below shows the marked increase in self-reported knowledge following the training exercises.
| Pre-test | Post-test | |
|---|---|---|
| I am confident that I know... | Somewhat Agree or Strongly Agree | Somewhat Agree or Strongly Agree |
| When the Outbreak Investigation Coordination Committee (OICC) is established in relation to the evolution of a food-borne illness outbreak. | 43% | 96% |
| How the OICC is established in relation to the evolution of a food-borne illness outbreak. | 36% | 93% |
| How the OICC lead is determined. | 33% | 91% |
| The roles and responsibilities of the OICC lead. | 36% | 93% |
| How the FIORP Duty Officers are determined. | 26% | 79% |
| The roles and responsibilities of the FIORP Duty Officers. | 28% | 84% |
| Number of tests completed | 478 | 408 |
| Source: Public Health Agency of Canada | ||
In addition, the Canadian Food Inspection Agency’s Evaluation of Changes to Inter-Departmental Interfaces found that the training exercises were “highly beneficial to raising awareness about the FIORP, and individual and collective partner roles and responsibilities”.Footnote 67 This was reinforced by external and internal key informants for this evaluation who found the exercises very useful.
The FIORP guides multi-jurisdictional action during food-borne enteric illness outbreaks. But in some rare instances, a food-borne enteric illness outbreak requires a response beyond the scope of the FIORP. This is why the Weatherill Report also recommended that a Food-borne Illness Emergency Response Plan be developed and exercised. In June 2011, the Health Portfolio’s Food-borne Illness Emergency Response Plan was endorsed by the Health Portfolio Joint Emergency Preparedness Committee.Footnote 68 During the North Atlantic Treaty Organization Crisis Management Exercise 11 that took place in October 2011, the Public Health Agency and Health Canada exercised a small portion of the Food-borne Illness Emergency Response Plan with a simulated food-borne enteric illness outbreak. A full scale, nationally distributed food safety exercise that will test the entire Plan is tentatively scheduled for 2012-13.
3.2.10 There are no data sharing agreements between provinces, territories and the Public Health Agency
The Public Health Agency currently relies on program specific protocols and Memoranda of Understanding with provinces and territories to ensure effective flow of information.
Sharing information between the Public Health Agency and provinces and territories is essential for the system to be responsive. The detection of food-borne enteric illness depends on receiving accurate and timely data to ensure proper response. Currently, there are no data sharing agreements between provinces, territories and the Public Health Agency. The lack of data sharing agreements has been raised previously by the Public Health Agency’s Lessons Learned Review on the 2008 Listeriosis outbreak and the Auditor General’s Report on Surveillance of Infectious Disease.Footnote 69 Footnote 70
To address these recommendations, the Public Health Agency is leading a Multilateral Information Sharing Agreement initiative through a federal, provincial and territorial task group under the Public Health Network. The Public Health Network Council approved the initiative’s approach and governance. As a federal, provincial and territorial initiative, the Public Health Agency and Health Canada recently agreed that the Multilateral Information Sharing Agreement initiative will be a joint initiative presenting a common approach to addressing shared public health responsibilities.Footnote 71
While the work on the Multilateral Information Sharing Agreement initiative is progressing, it is experiencing a few challenges. A few interviewees noted that limited resources, unclear data requirements in the Public Health Agency, as well as unclear roles and responsibilities are obstacles to developing data-sharing agreements. However, key informants noted that food-borne illness program areas established clear criteria about the type and use of information they are collecting from their provincial and territorial partners which contribute to the effective flow of data. In the absence of data-sharing agreements, multiple protocols and Memoranda of Understanding have been signed. These various accords were described by some interviewees as a successful alternative, as they generally guide collaboration of partners in the detection and response to food-borne enteric illness outbreaks. However, it was noted that they do not establish an obligation to share information.
A few key Memoranda of Understanding guide the Public Health Agency’s activities in detecting and responding to food-borne enteric illness outbreaks:
- Memorandum of Understanding between Health Canada, and the Public Health Agency and the Canadian Food Inspection Agency — through this memorandum, federal partners’ key roles and areas of collaboration are highlighted.
- Federal/Provincial/Territorial Memorandum of Understanding on the Sharing of Information during a Public Health Emergency — this memorandum provides a framework for the sharing of information between the parties during a public health emergency in accordance with agreed-upon principles.
- PulseNet Canada Memorandum of Understanding between the Public Health Agency of Canada and member laboratories — the National Microbiology Laboratory signed memoranda with all ten provinces related to the data-sharing and operational details related to PulseNet Canada. It represents an active concurrence of all provincial laboratories regarding information exchange and the real-time discussion and analysis of laboratory and epidemiological data.
- PulseNet Canada Memorandum of Understanding between the Public Health Agency of Canada and the Centres for Disease Control and Prevention in the United States — this memorandum confirms that both countries will collaborate in responding to outbreaks through PulseNet.
In addition to those Memoranda of Understanding, the Foodborne Illness Outbreak Response Protocol does include a section on the sharing and centralization of information during an outbreak.
Although there is some progress in developing a Multilateral Information Sharing Agreement initiative, data-sharing agreements remain a gap. To fill this gap, many Memoranda of Understanding guide the work of the Public Health Agency and its federal and provincial/territorial partners in preventing, detecting and responding to food-borne illnesses.
3.2.11 Although some performance data are collected, there is no overarching performance measurement strategy for food-borne enteric illness activities
The Public Health Agency does not have one overarching performance measurement strategy to monitor the performance of its food-borne enteric illness activities. There are, however, a few separate mechanisms through which food-borne activities are monitored, at an initiative level and at a program level.
Initiative-level performance measurement activities
Through the funding received under the Food and Consumer Safety Action Plan, the Public Health Agency identified performance indicators in the action plan’s interdepartmental Results-based Management and Accountability Framework. The activities undertaken by each of the funded government departments are contained in internal annual reports detailing their progress.
An interdepartmental performance measurement framework was developed for the Government Response and Action Plan to the 2008 Listeriosis outbreak. Through the Federal Food Safety Progress Reports, the Public Health Agency has provided data detailing progress of the funded activities.
In addition to the interdepartmental reports, the Public Health Agency has created internal ‘performance stories’ reports to inform management of the key achievements of the Listeriosis-funded activities. Individual ‘performance stories’ have been produced for the majority of the funded activities.
Program area-level performance measurement activities
There is a good amount of performance data collected and reported on in some program areas. Although the data are not part of a performance measurement strategy and no targets have been established, data are collected on an ongoing basis for some food-borne illness activities.
- National Microbiology Laboratory Enterics Program: Through the Canadian Public Health Laboratory Network, the Enterics Program produces annual reports on the performance of its activities. The reports are peer reviewed and include a vast amount of data.
- Centre for Food-borne, Environmental and Zoonotics Infectious Disease: The Centre produced an annual report outlining activities and outputs. In addition, the Outbreak Management Division within the Centre also produced an annual report, detailing some of their specific key achievements.
Given the visibility of large outbreaks such as the 2008 Listeriosis outbreak, there may be merit in developing an Agency-wide performance measurement strategy for its food-borne enteric illness activities.
3.2.12 Although recent time-limited food safety funding is systematically tracked, there is no mechanism to track ongoing expenditures
As outlined in section 2.4, the Public Health Agency receives both ongoing and time-limited funding for its food-borne enteric illness activities. Financial information is tracked for all recent program authorities in this area. However, a lack of tracked financial information for ongoing expenditures makes it difficult to completely assess the efficient use of overall funding for food-borne enteric illness activities.
Recent food safety funding
The Food and Consumer Safety Action Plan and the funding received to address the 2008 Listeriosis outbreak were tracked at the activity level. The figure below provides an overview of funding allocated and expended. Generally, the Public Health Agency did not fully spend allocated funding.
| Food and Consumer Safety Action Plan (A-base) | Funding Allocation | Expenditures | Variance Allocation to Expenditures (Lapsed funds) | |
|---|---|---|---|---|
| Salary | O&M | |||
| 2008-09 | $2,100,000 | $133,033 | $939,209 | $1,027,758 |
| 2009-10 | $4,000,000 | $764,883 | $2,206,911 | $1,028,206 |
| 2010-11 | $4,100,000 | $905,783 | $2,610,428 | $583,790 |
| Listeriosis (time-limited) | ||||
| 2009-10 | $2,800,000 | $255,285 | $1,191,301 | $1,354,414 |
| 2010-11 | $6,900,000 | $1,837,898 | $3,756,418 | $1,305,684 |
| Source: Public Health Agency of Canada | ||||
The Food and Consumer Safety Action Plan’s deviation from planned versus actual spending is attributed to challenges in finding skilled staff to conduct the work associated with funded activities. As mentioned in section 3.2.11, there is continuous tracking of activities through annual reports.
In 2009-10, most of the lapsed Listeriosis funds were due to the Office of Public Health Practice experiencing delays with the development and implementation of Panorama which is a federal/provincial/territorial initiative. It was anticipated early in the 2010-11 fiscal year that Panorama would lapse funds. Therefore, on the recommendation of the Listeria Directors Group, it was agreed to move some of the Listeriosis funding dollars for this particular activity to other activities that also address food-borne enteric illness gaps. Among the criteria established to secure funding for lapsed dollars, program areas had to demonstrate that their proposed projects advanced a key deliverable in response to the Weatherill recommendations or that they addressed a gap identified in the Weatherill Report.
Overall funding efficiencies
As discussed in section 2.4, the Infectious Disease Prevention and Control Branch conducted an exercise to estimate the financial resources it dedicates to preventing, detecting and responding to food-borne illness. It was estimated that the Branch was allocated approximately $17.2 million on food-borne enteric illness-related activities in 2010-11. The Laboratory for Food-borne Zoonoses was allocated almost half of that amount (54 per cent), with the Centre for Food-borne, Environmental and Zoonotic Infectious Diseases and the National Microbiology Laboratory accounting for almost a quarter each (24 and 23 per cent respectively).
Key informants note that antimicrobial resistance and source attribution surveillance account for a large proportion of the Laboratory for Food-borne Zoonoses’ overall spending (over 50 per cent). These activities have a clearer role with evidence used, at least with antimicrobial resistance surveillance, by our federal food safety partners. This evaluation highlights that, while receiving half of the Public Health Agency’s budgetary allocation for food-borne enteric illness activities, the Laboratory for Food-borne Zoonoses’ role is unclear in some areas and some of the evidence it generates does not appear to be used by food safety partners. Key informants also specified that some of the funding accounted for by the Laboratory for Food-borne Zoonoses included funding secured externally. However, given that the financial data is not systematically tracked, it is difficult to confirm this explanation.
Page details
- Date modified: