Update on the use of 13-valent pneumococcal conjugate vaccine (PNEU-C-13) in addition to 23-valent pneumococcal polysaccharide vaccine (PNEU-P-23) in immunocompetent adults 65 years of age and older – Interim Recommendation
An Advisory Committee Statement (ACS) National Advisory Committee on Immunization (NACI)
Preamble
The National Advisory Committee on Immunization (NACI) provides the Public Health Agency of Canada (hereafter referred to as the Agency) with ongoing and timely medical, scientific, and public health advice relating to immunization. The Agency acknowledges that the advice and recommendations set out in this statement are based upon the best current available scientific knowledge and is disseminating this document for information purposes. People administering the vaccine should also be aware of the contents of the relevant product monograph(s). Recommendations for use and other information set out herein may differ from that set out in the product monograph(s) of the Canadian manufacturer(s) of the vaccine(s). Manufacturer(s) have sought approval of the vaccine(s) and provided evidence as to its safety and efficacy only when it is used in accordance with the product monographs. NACI members and liaison members conduct themselves within the context of the Agency’s Policy on Conflict of Interest, including yearly declaration of potential conflict of interest.
Table of Contents
Summary of information contained in this NACI Statement
The following table highlights key information for immunization providers. Please refer to the remainder of the Statement for details.

Download the alternative format
(PDF format, 1022 KB, 28 pages)
Organization: Public Health Agency of Canada
Date published: October 2016
Cat.: HP40-160/2016E-PDF
ISBN: 978-0-660-05838-2
Pub.: 160085
1. What
Streptococcus pneumoniae is a bacterium that causes invasive pneumococcal disease (IPD) – such as bloodstream infection and meningitis, and community-acquired pneumonia (CAP). Symptoms are dependent on the site of infection. More information is available online.
PNEU-C-13 is a conjugate vaccine containing 13 pneumococcal serotypes (conjugated to diphtheria CRM197 protein).
PNEU-P-23 is a polysaccharide vaccine containing 23 pneumococcal serotypes.
2. Who
Immunocompetent adults, 65 years and older, who may opt for additional protection against the 13 pneumococcal serotypes afforded by PNEU-C-13, in addition to that provided by the routinely recommended PNEU-P-23.
3. How
Dose and Schedule
For PNEU-C-13 vaccine, the dose is 0.5mL, administered IM.
Precautions and Contraindications: PNEU-C-13 is contraindicated in any individual with a history of anaphylaxis to any component of the vaccine, including diphtheria toxoid.
Co-administration: PNEU-C-13 can be co-administered (using a different site) with other vaccines, but not with PNEU-P-23.
4. Why
This interim recommendation for use of PNEU-C-13 vaccine in immunocompetent adults over 65 years of age is provided to allow evidence-informed decision-making when the vaccine is considered for use on an individual basis.
Following the completion of this statement, in addition to epidemiological, efficacy, safety and immunogenicity data, NACI will be developing a recommendation that considers the impact of the PNEU-C-13 childhood vaccination program on adult disease and strain replacement.
I. Introduction
The objective of this Statement Update is to provide evidence and interim recommendations for the use of PNEU-C-13 in immunocompetent adults over 65 years of age and to allow informed decision making in cases when PNEU-C-13 is being considered on an individual basis for use in this age group.
This statement:
- Updates the epidemiology of pneumococcal disease in Canada for strains prevented by PNEU-C-13 to the year of the most recently available data (2013);
- Provides an update to the review of the literature on the use of PNEU-C-13 in immunocompetent adults, which includes the recently published CAPiTA trial, as well as randomised controlled trials (RCTs) that investigate safety and immunogenicity;
- Provides updated, interim, recommendations for the use of PNEU-C-13 in immunocompetent individuals who are 65 years of age and over.
Since January 2012, PNEU-C-13 vaccine has been authorized for use in adults 50 years of age and older for the prevention of invasive pneumococcal disease (IPD) caused by Streptococcus pneumoniae serotypes included in the vaccine. In July 2015, PNEU-C-13 vaccine received an expanded adult indication for the prevention of community-acquired pneumonia (CAP) caused by the serotypes included in the vaccine. Previously published NACI Statements are available online. A summary of current NACI recommendations is provided in the Pneumococcal Vaccine chapter of the Canadian Immunization Guide.
II. Methods
NACI reviewed the key questions for the literature review as proposed by the NACI Pneumococcal Working Group (PWG), including such considerations as the burden of illness of disease to be prevented, the target population(s), safety, immunogenicity, efficacy and effectiveness of the vaccine(s), vaccine schedules, and other aspects of the overall immunization strategy. The knowledge synthesis was performed by a research co-ordinator and supervised by the Chair of NACI’s PWG. Following critical appraisal of individual studies, summary tables with ratings of the quality of the evidence using NACI's methodological hierarchy (Tables 5, 6 and 7) were prepared, and proposed recommendations for vaccine use developed. The Chair of NACI’s PWG presented the evidence and proposed recommendations to NACI on October 6, 2015. Following a thorough review of the evidence and consultations, on October 6, 2015 and November 2, 2015, NACI voted on specific recommendations. The description of relevant considerations, rationale for specific decisions, and knowledge gaps are described in the text.
III. Epidemiology
III.1 Disease description
The bacterium Streptococcus pneumoniae is the cause of IPD and a common cause of CAP. There are currently over 90 serotypes recognized worldwide, 15 of which cause the majority of disease. S. pneumoniae can spread from person to person by droplets from the nose or mouth, by sneezing or coughing.
Although asymptomatic upper respiratory tract colonization is common, infection with S. pneumoniae may result in severe disease. IPD is a severe form of infection that occurs when the bacterium invades normally sterile sites, such as the bloodstream or central nervous system, leading to bacteremia and meningitis. Certain conditions predispose to IPD and complicated CAP, including sickle-cell disease, other hemoglobinopathies, chronic renal failure, chronic liver disease, immunosuppression, anatomic or functional asplenia, cerebrospinal fluid leaks, diabetes mellitus and HIV infection.
III.2 Disease distribution
Infections caused by S. pneumoniae are a major cause of morbidity and mortality worldwide. In developed countries, the burden of disease is highest in young children and older adults. Data on IPD disease distribution in Canada prior to 2012 are available in previous statements by NACI on pneumococcal vaccines.
National surveillance data for IPD are available through a number of sources, including the Canadian Notifiable Disease Surveillance System (CNDSS) and the National Microbiology Laboratory (NML)’s National Laboratory Surveillance of Invasive Streptococcal Disease in Canada. In 2013, the incidence rate of IPD in Canada was 9.0 cases per 100,000 populationFootnote 1.
In Canada, sentinel surveillance of hospitalized community acquired pneumonia (including IPD and non-bacteremic pneumococcal pneumonia) is conducted through the Serious Outcome Surveillance (SOS) network with its 15 participating hospitals in 5 provinces. Between January 2010 and December 2014, the SOS network enrolled over 12 500 cases of CAP, among which S. pneumoniae was confirmed as the etiologic agent in 805 cases (7.5%). On average, 40% of patients were tested using the serotype-specific urinary antigen detection that can discriminate amongst the 13 serotypes included in PNEU-C-13. Of those, 11% tested positive (personal communication, S. McNeil).
To understand better the importance of S. pneumoniae in the overall burden of CAP, all-cause CAP that occurred between 2010 and 2012 were studied in the United States of America (USA). The estimated annual incidence rate of CAP in adults was 248 cases per 100,000 population, of which only 5% were caused by S. pneumoniae – most were diagnosed by urinary antigen detection (67%) – for an overall incidence rate of 12 per 100 000 adult population (95%CI: 10-14). The incidence rate of CAP caused by S. pneumoniae was five times higher in adults 65 years of age and older compared to younger age groupsFootnote 2.
III.3 Age Distribution
The crude incidence rate of IPD in Canada declined significantly (p<0.05), from 9.8 cases per 100,000 in 2009, to 9.0 cases per 100,000 in 2013 (Figure 1).
Figure 1. Crude incidence rate of invasive pneumococcal disease (per 100,000 population) in Canada, by age group and year, 2009-2013.

Figure 1 - Text Description
The image consists of a clustered bar graph. It depicts the crude incidence rate of invasive pneumococcal disease (per 100,000 population) in Canada, by age group and year for the period 2009 to 2013.
The y-axis represents the number of reported cases per 100,000 population, with a minimum of 0 and a maximum of 30. The x-axis represents age groups: less than 1 year; 1 to 4 years; 5 to 9 years; 10 to 14 years; 15 to 19 years; 20 to 24 years; 25 to 29 years; 30 to 39 years; 40 to 59 years; 60 years and older; and all ages. For each age group, there are 5 bars, representing the number of reported cases per 100,000 population for the years 2009 to 2013.
Across the five years, the number of reported cases is highest in the less than one age group, followed by the 60 years and older age group. The graph depicts a decline in reported incidence among those less than one year, and those aged 1 to 4 years from 2009 to 2013. The reported incidence rate in all other age groups remains relatively consistent across the period depicted in the image.
The crude incidence rate per 100,000 population for less than one year olds was 27.79 in 2009, 25.14 in 2010, 20.73 in 2011, 18.32 in 2012, and 18.60 in 2013. The crude incidence rate per 100,000 population for one to four year olds was 18.68 in 2009, 16.44 in 2010, 15.43 in 2011, 13.61 in 2012, and 11.25 in 2013. The crude incidence rate per 100,000 population for five to nine year olds was 5.75 in 2009, 4.75 in 2010, 5.25 in 2011, 4.34 in 2012, and 3.77 in 2013. The crude incidence rate per 100,000 population for ten to 14 year olds was 1.60 in 2009, 1.84 in 2010, 2.40 in 2011, 2.49 in 2012, and 1.50 in 2013. The crude incidence rate per 100,000 population for 15 to 19 year olds was 1.77 in 2009, 1.24 in 2010, 1.61 in 2011, 1.58 in 2012, and 1.24 in 2013. The crude incidence rate per 100,000 population for 20 to 24 year olds was 2.36 in 2009, 1.85 in 2010, 1.40 in 2011, 2.50 in 2012, and 1.47 in 2013. The crude incidence rate per 100,000 population for 25 to 29 year olds was 3.44 in 2009, 3.14 in 2010, 3.04 in 2011, 3.97 in 2012, and 2.78 in 2013. The crude incidence rate per 100,000 population for 30 to 39 year olds was 5.47 in 2009, 5.17 in 2010, 5.32 in 2011, 5.07 in 2012, and 4.54 in 2013. The crude incidence rate per 100,000 population for 40 to 59 year olds was 8.87 in 2009, 9.02 in 2010, 9.10 in 2011, 9.13 in 2012, and 8.39 in 2013. The crude incidence rate per 100,000 population for those 60 years of age and older was 22.35 in 2009, 23.44 in 2010, 21.64 in 2011, 22.72 in 2012, and 21.73 in 2013. The crude incidence rate per 100,000 population for Canada overall was 9.79 in 2009, 9.83 in 2010, 9.55 in 2011, 9.80 in 2012, and 9.02 in 2013.
Since the introduction of PNEU-C-13 to the routine childhood immunization schedule (by January 2011 in most jurisdictions), significant declines in incidence (p<0.05) were observed among infants aged < 1 year (27.6 to 17.9 cases per 100,000 population), and children aged 1 to 4 years (18.7 to 11.2 cases per 100,000 population) (Figure 1).
III.4 Serotype distribution of IPD by age groups
From 2010 to 2013, between 2577 and 2717 isolates of S. pneumoniae causing invasive disease were characterized each year. Among these isolates, between 34.1% (2011) and 40.6% (2013) of the total occurred in persons aged 65 years and older.
During this time, the proportion of isolates identified as PNEU-C-13 serotypes that are not included in PNEU-C-7 (i.e. 1, 3, 5, 6A, 7F and 19A) in Canada decreased significantly (p<0.05) from 45.6% to 30.5% (n=1235 and 784) in all combined age groups (Figure 2), and from 40.6% to 28.4% (n=393 and 296) among those aged 65 years and older (Figure 3).
Figure 2. Proportion of isolates of invasive S. pneumoniae for all ages in Canada, by serotype and year, 2010 to 2013.
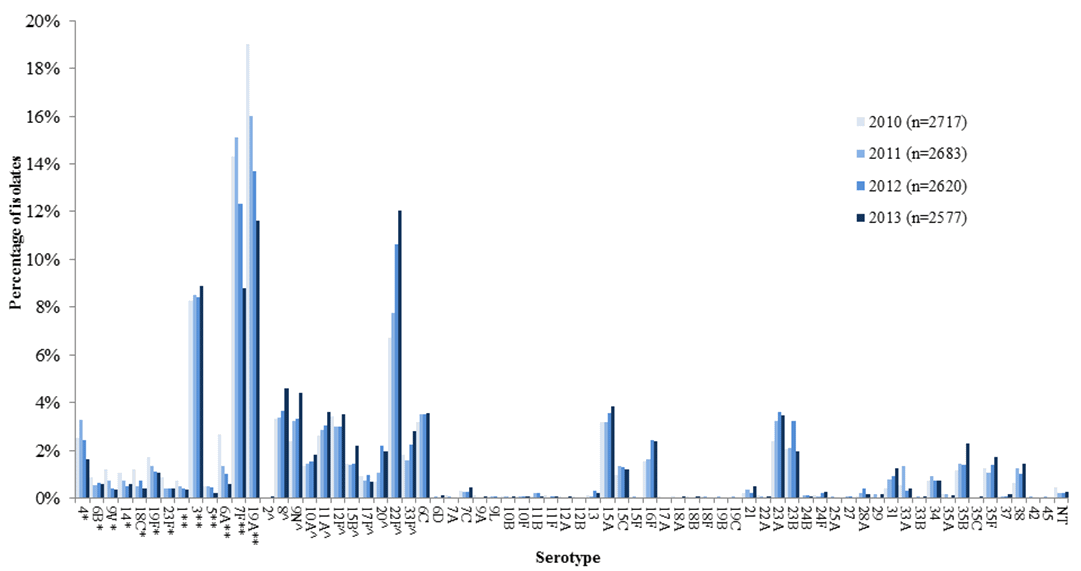
Figure 2 - Text Description
The image consists of a clustered bar graph. It represents the number of isolates of each serotype from all isolates collected between 2010-2013.
| Serotype | 2010 (n=2717) | 2011 (n=2683) | 2012 (n=2620) | 2013 (n=2577) |
| 4* (69,88,63,42) ‡ | 2.54% | 3.28% | 2.40% | 1.63% |
| 6B* (23,14,16,15) | 0.85% | 0.52% | 0.61% | 0.58% |
| 9V* (32,19,11,9) | 1.18% | 0.71% | 0.42% | 0.35% |
| 14* (29,19,13,15) | 1.07% | 0.71% | 0.50% | 0.58% |
| 18C* (33,13,19,10) | 1.21% | 0.48% | 0.73% | 0.39% |
| 19F* (47,36,29,27) | 1.73% | 1.34% | 1.11% | 1.05% |
| 23F* (24,11,11,10) | 0.88% | 0.41% | 0.42% | 0.39% |
| 1** (20,13,10,9) | 0.74% | 0.48% | 0.38% | 0.35% |
| 3** (225,228,221,229) | 8.28% | 8.50% | 8.44% | 8.89% |
| 5** (13,13,12,5) | 0.48% | 0.48% | 0.46% | 0.19% |
| 6A** (72,36,27,15) | 2.65% | 1.34% | 1.03% | 0.58% |
| 7F** (389,406,323,226) | 14.32% | 15.13% | 12.33% | 8.77% |
| 19A**(517,430,359,299) | 19.03% | 16.03% | 13.70% | 11.60% |
| 2^ (0,0,0,1) | 0.00% | 0.00% | 0.00% | 0.04% |
| 8^ (90,90,96,119) | 3.31% | 3.35% | 3.66% | 4.62% |
| 9N^ (65,87,87,113) | 2.39% | 3.24% | 3.32% | 4.38% |
| 10A^ (37,39,40,47) | 1.36% | 1.45% | 1.53% | 1.82% |
| 11A^ (71,76,80,93) | 2.61% | 2.83% | 3.05% | 3.61% |
| 12F^ (93,80,78,90) | 3.42% | 2.98% | 2.98% | 3.49% |
| 15B^ (39,37,38,56) | 1.44% | 1.38% | 1.45% | 2.17% |
| 17F^ (25,20,25,18) | 0.92% | 0.75% | 0.95% | 0.70% |
| 20^ (18,28,57,50) | 0.66% | 1.04% | 2.18% | 1.94% |
| 22F^ (183,208,278,311) | 6.74% | 7.75% | 10.61% | 12.07% |
| 33F^ (49,42,58,72) | 1.80% | 1.57% | 2.21% | 2.79% |
| 6C (86,94,92,92) | 3.17% | 3.50% | 3.51% | 3.57% |
| 6D (0,1,0,3) | 0.00% | 0.04% | 0.00% | 0.12% |
| 7A (3,1,0,0) | 0.11% | 0.04% | 0.00% | 0.00% |
| 7C (8,7,7,12) | 0.29% | 0.26% | 0.27% | 0.47% |
| 9A (3,0,0,1) | 0.11% | 0.00% | 0.00% | 0.04% |
| 9L (1,2,2,0) | 0.04% | 0.07% | 0.08% | 0.00% |
| 10B (1,1,0,1) | 0.04% | 0.04% | 0.00% | 0.04% |
| 10F (1,1,1,1) | 0.04% | 0.04% | 0.04% | 0.04% |
| 11B (2,6,6,1) | 0.07% | 0.22% | 0.23% | 0.04% |
| 11F (3,0,1,1) | 0.11% | 0.00% | 0.04% | 0.04% |
| 12A (1,0,0,1) | 0.04% | 0.00% | 0.00% | 0.04% |
| 12B (1,0,0,0) | 0.04% | 0.00% | 0.00% | 0.00% |
| 13 (3,2,8,5) | 0.11% | 0.07% | 0.31% | 0.19% |
| 15A (87,85,93,99) | 3.20% | 3.17% | 3.55% | 3.84% |
| 15C (26,36,34,31) | 0.96% | 1.34% | 1.30% | 1.20% |
| 15F (0,1,0,0) | 0.00% | 0.04% | 0.00% | 0.00% |
| 16F (42,44,63,61) | 1.55% | 1.64% | 2.40% | 2.37% |
| 17A (1,0,0,0) | 0.04% | 0.00% | 0.00% | 0.00% |
| 18A (1,0,0,2) | 0.04% | 0.00% | 0.00% | 0.08% |
| 18B (1,0,0,1) | 0.04% | 0.00% | 0.00% | 0.04% |
| 18F (1,2,0,0) | 0.04% | 0.07% | 0.00% | 0.00% |
| 19B (0,1,0,0) | 0.00% | 0.04% | 0.00% | 0.00% |
| 19C (0,2,0,0) | 0.00% | 0.07% | 0.00% | 0.00% |
| 21 (6,9,6,13) | 0.22% | 0.34% | 0.23% | 0.50% |
| 22A (3,1,0,1) | 0.11% | 0.04% | 0.00% | 0.04% |
| 23A (65,86,94,89) | 2.39% | 3.21% | 3.59% | 3.45% |
| 23B (55,56,84,50) | 2.02% | 2.09% | 3.21% | 1.94% |
| 24B (0,3,3,1) | 0.00% | 0.11% | 0.11% | 0.04% |
| 24F (3,2,6,6) | 0.11% | 0.07% | 0.23% | 0.23% |
| 25A (0,2,0,0) | 0.00% | 0.07% | 0.00% | 0.00% |
| 27 (0,1,1,0) | 0.00% | 0.04% | 0.04% | 0.00% |
| 28A (1,6,10,4) | 0.04% | 0.22% | 0.38% | 0.16% |
| 29 (2,4,0,4) | 0.07% | 0.15% | 0.00% | 0.16% |
| 31 (11,21,24,32) | 0.40% | 0.78% | 0.92% | 1.24% |
| 33A (15,36,8,10) | 0.55% | 1.34% | 0.31% | 0.39% |
| 33B (0,1,0,1) | 0.00% | 0.04% | 0.00% | 0.04% |
| 34 (20,24,19,19) | 0.74% | 0.89% | 0.73% | 0.74% |
| 35A (5,4,0,3) | 0.18% | 0.15% | 0.00% | 0.12% |
| 35B (31,39,36,59) | 1.14% | 1.45% | 1.37% | 2.29% |
| 35C (0,0,0,1) | 0.00% | 0.00% | 0.00% | 0.04% |
| 35F (34,28,36,44) | 1.25% | 1.04% | 1.37% | 1.71% |
| 37 (2,1,2,4) | 0.07% | 0.04% | 0.08% | 0.16% |
| 38 (17,33,27,37) | 0.63% | 1.23% | 1.03% | 1.44% |
| 42 (0,1,0,0) | 0.00% | 0.04% | 0.00% | 0.00% |
| 45 (0,1,0,0) | 0.00% | 0.04% | 0.00% | 0.00% |
| NT (12,5,6,6) | 0.44% | 0.19% | 0.23% | 0.23% |
|
||||
Figure 3. Proportion of isolates of invasive S. pneumoniae among those aged 65 years and older in Canada, by serotype and year, 2010 to 2013.
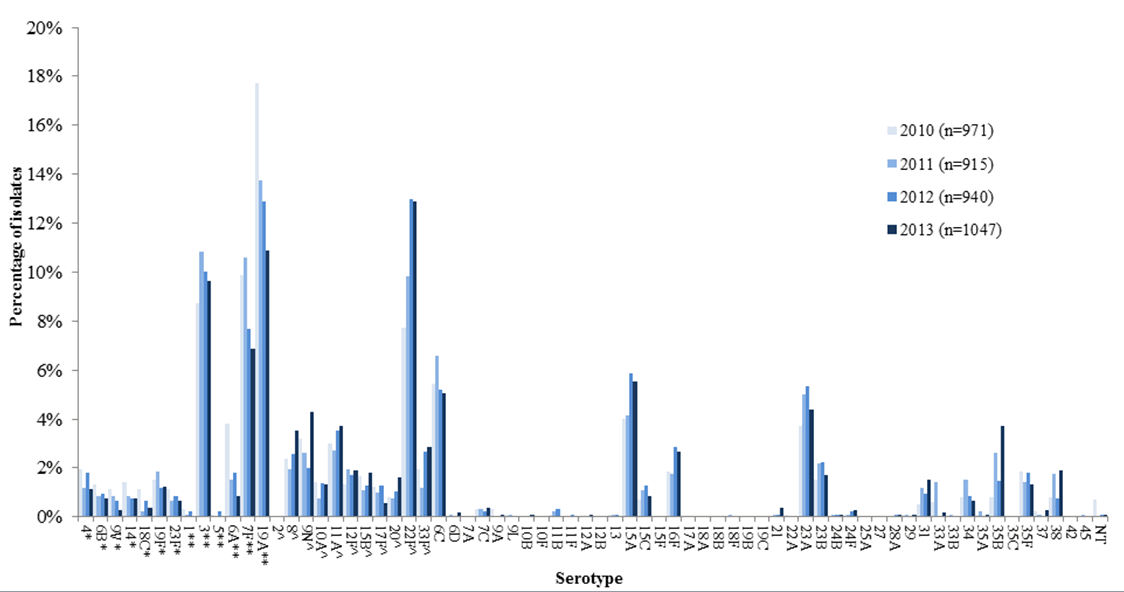
Figure 3 - Text Description
The image consists of a clustered bar graph. It represents the number of isolates of each serotype from adults 65 years and older collected between 2010-2013.
| Serotype | 2010 (n=971) | 2011 (n=915) | 2012 (n=940) | 2013 (n=1047) |
| 4* (19,11,17,12) | 1.96% | 1.20% | 1.81% | 1.15% |
| 6B* (13,8,9,8) | 1.34% | 0.87% | 0.96% | 0.76% |
| 9V* (11,8,6,3) | 1.13% | 0.87% | 0.64% | 0.29% |
| 14* (14,8,7,8) | 1.44% | 0.87% | 0.74% | 0.76% |
| 18C* (11,2,6,4) | 1.13% | 0.22% | 0.64% | 0.38% |
| 19F* (15,17,11,13) | 1.54% | 1.86% | 1.17% | 1.24% |
| 23F* (11,6,8,7) | 1.13% | 0.66% | 0.85% | 0.67% |
| 1** (3,1,2,0) | 0.31% | 0.11% | 0.21% | 0.00% |
| 3** (85,99,94,101) | 8.75% | 10.82% | 10.00% | 9.65% |
| 5** (1,0,2,0) | 0.10% | 0.00% | 0.21% | 0.00% |
| 6A** (37,14,17,9) | 3.81% | 1.53% | 1.81% | 0.86% |
| 7F** (96,97,72,72) | 9.89% | 10.60% | 7.66% | 6.88% |
| 19A**(172,126,121,114) | 17.71% | 13.77% | 12.87% | 10.89% |
| 2^ (0,0,0,0) | 0.00% | 0.00% | 0.00% | 0.00% |
| 8^ (23,18,24,37) | 2.37% | 1.97% | 2.55% | 3.53% |
| 9N^ (31,24,19,45) | 3.19% | 2.62% | 2.02% | 4.30% |
| 10A^ (14,7,13,14) | 1.44% | 0.77% | 1.38% | 1.34% |
| 11A^ (29,25,33,39) | 2.99% | 2.73% | 3.51% | 3.72% |
| 12F^ (13,18,16,20) | 1.34% | 1.97% | 1.70% | 1.91% |
| 15B^ (16,10,12,19) | 1.65% | 1.09% | 1.28% | 1.81% |
| 17F^ (12,9,12,6) | 1.24% | 0.98% | 1.28% | 0.57% |
| 20^ (8,7,10,17) | 0.82% | 0.77% | 1.06% | 1.62% |
| 22F^ (75,90,122,135) | 7.72% | 9.84% | 12.98% | 12.89% |
| 33F^ (19,11,25,30) | 1.96% | 1.20% | 2.66% | 2.87% |
| 6C (53,60,49,53) | 5.46% | 6.56% | 5.21% | 5.06% |
| 6D (0,1,0,2) | 0.00% | 0.11% | 0.00% | 0.19% |
| 7A (0,0,0,0) | 0.00% | 0.00% | 0.00% | 0.00% |
| 7C (3,3,2,4) | 0.31% | 0.33% | 0.21% | 0.38% |
| 9A (3,0,0,1) | 0.31% | 0.00% | 0.00% | 0.10% |
| 9L (1,1,0,0) | 0.10% | 0.11% | 0.00% | 0.00% |
| 10B (0,0,0,1) | 0.00% | 0.00% | 0.00% | 0.10% |
| 10F (0,0,0,0) | 0.00% | 0.00% | 0.00% | 0.00% |
| 11B (1,2,3,0) | 0.10% | 0.22% | 0.32% | 0.00% |
| 11F (0,0,1,0) | 0.00% | 0.00% | 0.11% | 0.00% |
| 12A (0,0,0,1) | 0.00% | 0.00% | 0.00% | 0.10% |
| 12B (0,0,0,0) | 0.00% | 0.00% | 0.00% | 0.00% |
| 13 (1,1,1,0) | 0.10% | 0.11% | 0.11% | 0.00% |
| 15A (39,38,55,58) | 4.02% | 4.15% | 5.85% | 5.54% |
| 15C (7,10,12,9) | 0.72% | 1.09% | 1.28% | 0.86% |
| 15F (0,0,0,0) | 0.00% | 0.00% | 0.00% | 0.00% |
| 16F (18,16,27,28) | 1.85% | 1.75% | 2.87% | 2.67% |
| 17A (0,0,0,0) | 0.00% | 0.00% | 0.00% | 0.00% |
| 18A (0,0,0,0) | 0.00% | 0.00% | 0.00% | 0.00% |
| 18B (0,0,0,0) | 0.00% | 0.00% | 0.00% | 0.00% |
| 18F (0,1,0,0) | 0.00% | 0.11% | 0.00% | 0.00% |
| 19B (0,0,0,0) | 0.00% | 0.00% | 0.00% | 0.00% |
| 19C (0,0,0,0) | 0.00% | 0.00% | 0.00% | 0.00% |
| 21 (0,1,1,4) | 0.00% | 0.11% | 0.11% | 0.38% |
| 22A (1,0,0,0) | 0.10% | 0.00% | 0.00% | 0.00% |
| 23A (36,46,50,46) | 3.71% | 5.03% | 5.32% | 4.39% |
| 23B (15,20,21,18) | 1.54% | 2.19% | 2.23% | 1.72% |
| 24B (0,1,1,1) | 0.00% | 0.11% | 0.11% | 0.10% |
| 24F (1,1,2,3) | 0.10% | 0.11% | 0.21% | 0.29% |
| 25A (0,0,0,0) | 0.00% | 0.00% | 0.00% | 0.00% |
| 27 (0,0,0,0) | 0.00% | 0.00% | 0.00% | 0.00% |
| 28A (0,0,1,1) | 0.00% | 0.00% | 0.11% | 0.10% |
| 29 (1,1,0,1) | 0.10% | 0.11% | 0.00% | 0.10% |
| 31 (5,11,9,16) | 0.51% | 1.20% | 0.96% | 1.53% |
| 33A (6,13,0,2) | 0.62% | 1.42% | 0.00% | 0.19% |
| 33B (0,1,0,0) | 0.00% | 0.11% | 0.00% | 0.00% |
| 34 (8,14,8,7) | 0.82% | 1.53% | 0.85% | 0.67% |
| 35A (1,2,0,1) | 0.10% | 0.22% | 0.00% | 0.10% |
| 35B (8,24,14,39) | 0.82% | 2.62% | 1.49% | 3.72% |
| 35C (0,0,0,0) | 0.00% | 0.00% | 0.00% | 0.00% |
| 35F (18,13,17,14) | 1.85% | 1.42% | 1.81% | 1.34% |
| 37 (2,1,0,3) | 0.21% | 0.11% | 0.00% | 0.29% |
| 38 (8,16,7,20) | 0.82% | 1.75% | 0.74% | 1.91% |
| 42 (0,0,0,0) | 0.00% | 0.00% | 0.00% | 0.00% |
| 45 (0,1,0,0) | 0.00% | 0.11% | 0.00% | 0.00% |
| NT (7,0,1,1) | 0.72% | 0.00% | 0.11% | 0.10% |
|
||||
In contrast, between 2010 and 2013, the proportion of isolates identified as serotypes unique to PNEU-P-23, and thus not included in PNEU-C-13 (i.e. 2, 8, 9N, 10A, 11A, 12F, 15B, 17F, 20, 22F, 33F), increased significantly (p<0.05) from 24.7% to 37.7% (n=670 and 969) in all combined age groups (Figure 2), and from 24.8% to 34.6% (n= 240 and 361) among those aged 65 years and older (Figure 3).
Among the 2577 IPD isolates serotyped in 2013, the most predominant serotypes were: 22F (12.1%), 19A (11.6%), 3 (8.9%), and 7F (8.8%) – 19A, 3 and 7F are part of PNEU-C-13 and PNEU-P-23, while 22F is only included in PNEU-P-23 – together representing 41.3% (n=1065) of the total (Figure 2). Similarly, for those aged 65 years and older, predominating serotypes were: 22F (12.9%), 19A (10.9%), 3 (9.7%), and 7F (6.9%), representing 40.3% (n=422) of the total.
Additional information on serotype distribution of IPD prior to 2013 is available from the NML’s National Laboratory Surveillance of Invasive Streptococcal Disease in Canada – Annual Summary 2013, and in previous NACI pneumococcal vaccine statements.
IV. Vaccines
IV.1 Preparations authorized for use in Canada
Two preparations of pneumococcal vaccine are available in Canada. PNEU-C-13 (Prevnar13®) is a sterile solution of polysaccharide capsular antigen of 13 serotypes of S. pneumoniae (1, 3, 4, 5, 6A, 6B, 7F, 9V, 14, 18C, 19A, 19F and 23F). The antigens are individually conjugated to a diphtheria CRM197 protein carrier. The CRM197 protein carrier is adsorbed on aluminum phosphate as an adjuvant. Each dose of vaccine contains 4.4 µg of the 6B polysaccharide, and 2.2 µg each of the remaining polysaccharides. PNEU-C-13 is marketed in a single dose, prefilled 1.5ml syringe containing 0.5mL of vaccine.
PNEU-P-23 (Pneumovax® 23) is a sterile solution of 23 highly purified capsular polysaccharides (1, 2, 3, 4, 5, 6B, 7F, 8, 9N, 9V, 10A, 11A, 12F, 14, 15B, 17F, 18C, 19A, 19F, 20, 22F, 23F, 33F). PNEU-P-23 is available as a 3 ml single-dose vial containing 0.5 ml dose of liquid vaccine and a 1.5 ml prefilled syringe containing 0.5 ml dose of liquid vaccine. A comprehensive list of contents of PNEU-C-13 and PNEU-P-23 is available in the Canadian Immunization Guide.
IV.2 Efficacy
Data from a RCT investigating the efficacy of PNEU-C-13 to prevent IPD and CAP in adults who were immunocompetent at enrolment were published in March 2015 (CAPiTA study). This study is the first to present data on the efficacy of PNEU-C-13 in this populationFootnote 3.
Bonten et al.Footnote 3 conducted a randomized, double-blind, placebo-controlled trial involving 84,496 adults, 65 years of age or older, who were immunocompetent at enrolment, in which they investigated the efficacy and safety of PNEU-C-13 in preventing first episodes of CAP caused by pneumococcal serotypes included in the vaccine, both bacteremic and non-bacteremic. In this study, subjects were recruited from September 15, 2008 to January 30, 2010 and followed until August 28, 2013. Overall, 42,237 subjects received the PNEU-C-13 vaccine, 42,255 subjects received placebo, and all were followed-up for an average of 3.97 years.
The study population consisted of individuals who were 65 years of age or older, with no previous pneumococcal vaccination and an absence of immunocompromising conditions at enrolment. The exclusion criteria were residency in a nursing home, long-term care facility or other institution, or a requirement for nursing care. The following immune deficiencies were listed also as exclusion criteria: HIV, leukemia, lymphoma, Hodgkin’s disease, multiple myeloma, generalized malignancy currently present or within the last 5 years, chronic renal failure or nephrotic syndrome, receipt of immunosuppressive therapy--including steroids within 3 months of the study vaccine--and receipt of a solid organ or bone marrow transplant. A diagnostic routine standard of practice was used for all individuals presenting with symptoms of lower respiratory tract infection. The presence of S. pneumoniae was detected by culture, a commercially available urinary antigen assay and a serotype-specific urinary antigen detection (UAD) assay developed by the vaccine manufacturer.
Immunocompetent Population
In the CAPiTA study, Bonten et al.Footnote 3 reported vaccine efficacy (VE) and its 95% confidence intervals (CI) for patients 65 years of age or older. For overall CAP, 49 cases caused by vaccine-type serotypes were identified in the PNEU-C-13 arm and 90 cases in the placebo arm, for a VE of 45.6% (95% CI: 21.8, 62.5). For non-bacteremic CAP, 33 cases caused by vaccine-type serotypes were identified in the PNEU-C-13 arm and 60 cases in the placebo arm, for a VE of 45.0% (95% CI: 14.2, 65.3). For IPD, 7 cases caused by vaccine-type serotypes were identified in the PNEU-C-13 arm and 28 cases in the placebo arm, for a VE of 75.0% (95% CI: 41.4, 90.8). The efficacy was reported to persist throughout the mean follow-up time of 3.97 years.
A modified intention-to-treat analysis of all-cause CAP (including non-vaccine-type serotypes and all other etiologies) reported a much lower VE: 747 cases of all-cause CAP were identified in the PNEU-C-13 arm and 787 cases in the placebo arm, giving an overall VE of 5.1% (95% CI: -5.1, 14.2), which is very similar to VE estimates from the 23-valent polysaccharide pneumococcal vaccine derived from a meta-analysis that included studies in which participants were similar to those in the CAPiTA studyFootnote 4. Table 1 below summarizes the VEs for the different study endpoints. The overall VE to prevent death from confirmed vaccine-type pneumococcal CAP or IPD was 0, whereas it was 14.3 (95%CI: -197.9, 76.2) for the prevention of confirmed pneumococcal CAP or IPD (all pneumococcal strains). These VE estimates, in an immunocompetent elderly population, were measured in a population in which the 7-valent pneumococcal conjugate vaccine (PNEU-C-7) was the vaccine in use for infant vaccination schedule (3+1 schedule) from 2006 to 2011, at which point PNEU-C-7 was replaced by PNEU-C-10. The declining incidence of IPD caused by serotypes contained in PNEU-C-7 and -13 vaccines was reported by study authors: in 2008, a total of 68.4% of the episodes of IPD among patients 65 years of age or older were caused by PNEU-C-13 serotypes (49.7% by PNEU-C-7 serotypes and 5.3% by serotype 19A); in 2013, this percentage decreased to 42.3% caused by PNEU-C-13 serotypes (6% by PNEU-C-7 serotypes and 11.4% by serotype 19A).
| Study end points | Percent vaccine efficacy (95%CI) | |
|---|---|---|
| Per protocol analysisFootnote * | Modified intention-to-treatFootnote ** | |
| First episode | ||
| CAP – VT | 45.6 (21.8 – 62.5) | 37.7 (14.3 – 55.1) |
| CAP – VT non-bacteremic | 45.0 (14.2 – 65.3) | 41.1 (12.7 – 60.7) |
| IPD – VT | 75.0 (41.4 – 90.8) | 75.8 (46.5 – 90.3) |
| CAP – all pneumococcal strain | 30.6 (9.8 – 46.7) | 22.4 (2.3 – 38.5) |
| CAP – non-bacteremic (all pneumococcal strains) | 24.1 (-5.7 – 45.8) | 17.4 (-10.2 – 38.2) |
| IPD – all pneumococcal strains | 51.8 (22.4 – 70.7) | 48.5 (20.9 – 67.0) |
| CAP – all etiologies | 5.1 (-5.1 – 14.2) | |
| All episodes | ||
| CAP – VT | 42.4 (18.4 – 59.7) | 37.5 (15.0 – 54.3) |
Abbreviations: CAP: community-acquired pneumonia; VT: vaccine-type; IPD: invasive pneumococcal disease
|
||
Immunocompromised population
Study participants who became immunocompromised during the course of the study were kept in the study and analyzed as a sub-population. Table 2 summarizes the VE for this population.
Of note is that the reported VE in immunocompromised populations, when compared to the immunocompetent population, was always lower and not statistically significant, likely due to the small sample size. There was no sub-analysis provided for patients with chronic obstructive pulmonary disease, another population at high risk for pneumococcal CAP and in whom the PNEU-P-23 vaccine is considered less efficacious.
| Study end points | Percent vaccine efficacy (95%CI) - MITT | |
|---|---|---|
| Immunocompetent | Immunocompromised | |
| First episode | ||
| CAP – VT | 45.2 (21.8 – 61.9) | -27.3 (-212.1 – 46.7) |
| CAP – VT non-bacteremic | 44.4 (14.1 – 64.5) | 30 (-105.5 – 77.6) |
| IPD - VT | 75.0 (41.4 – 90.8) | 66.7 (-315.1 – 99.4) |
| CAP – all pneumococcal strain | 30.6 (9.8 – 46.7) | 22.4 (2.3 – 38.5) |
Abbreviations: MITT: modified intention-to-treat; CAP: community-acquired pneumonia; VT: vaccine-type; IPD: invasive pneumococcal disease |
||
IV.3 Effectiveness
There is currently no available study on the effectiveness of PNEU-C-13 in elderly patients. With the ACIP’s recommendation to use PNEU-C-13 in all adults aged 65 years and older, vaccine effectiveness data should become available in the future as the effect of vaccine in that population is analysed.
IV.4 Immunogenicity
Immunocompetent Population
Detailed information regarding the immunogenicity of PNEU-C-7 and PNEU-P-23 vaccines is available in previously published NACI Statements. Limited data exist on the immunogenicity of PNEU-C-13 in both younger and elderly adults. Information from available studies in elderly populations is summarized below.
In an open-labeled multicenter clinical trial conducted in Mexico, between July 29, 2011 and December 5, 2011, Tinoco et al.Footnote 5 compared otherwise healthy adult subjects who had never received a pneumococcal vaccine by age groups: those 50 to 64 years of age and those ≥65 years of age. All participants received one dose of PNEU-C-13. For all vaccine serotypes in both age groups, the opsonophagocytic activity (OPA) geometric mean titres (GMT) increased significantly from immediately before to 1 month after vaccination, as indicated by geometric mean fold rises (GMFRs). The OPA GMFRs were higher in the younger age group (GMFR range 5.3 to 63.6) compared to the older age group (GMFR range: 3.4 to 35.8). The pre-vaccination OPA GMTs were statistically significantly lower in the younger age group for 8 of the 13 serotypes and similar to the older age group for serotypes 1, 4, 6B, 9V, and 14. Post-vaccination OPA GMTs were similar between age groups for 10 of the 13 serotypes, but higher for serotypes 4, 7F, and 9V in the younger age group.
Jackson et al.Footnote 6 randomized 831 pneumococcal vaccine naïve adults aged 60 to 64 years of age to receive either PNEU-C-13 or PNEU-P-23 in a modified, double blind, comparative trial to assess the immunogenicity and safety of PNEU-C-13. The authors also evaluated immunogenicity of PNEU-C-13 in 403 patients aged 50-59 years old. For the older patient group, 411 received PNEU-C-13 and 407 received PNEU-P-23. At baseline, OPA GMTs were similar between the two groups and at 1 month after vaccination, OPA GMTs were non-inferior for the 12 common serotypes and statistically significantly greater in the PNEU-C-13 group for 8 out of 12 common serotypes (1, 4, 6B, 7F, 9V, 18C, 19A, and 23F) with the highest ratio (comparing PNEU-C-13 to PNEU-P-23) occurring for the 23F serotype at 5.2 (95% CI: 3.67, 7.33), while 6A (contained only in the 13-valent vaccine) had a ratio of 12.1 (95% CI: 8.63, 17.08). Comparing OPA GMTs 1 month after vaccination between the older age group to the younger age group indicated that in the younger age group, 9 out of 13 serotypes were statistically significantly higher. OPA titres declined between 1 month and 1 year after vaccination, but remained above pre-vaccination baseline levels. Except for serotypes 6B and 23F, there was no clear superior immunogenicity of PNEU-C-13 compared to PNEU-P-23 at 1 year after vaccination. The immune responses in the younger age group remained consistently higher than in the older age group.
Immunocompromised Population
Detailed information regarding the immunogenicity of PNEU-C-7 and PNEU-P-23 vaccines is available in previously published NACI Statements. The literature search identified only one immunogenicity study of PNEU-C-13 in HIV seropositive adults.
In a phase 3, open-label, single-arm trial, Glesby et al.Footnote 7 investigated the immunogenicity of PNEU-C-13 in HIV infected adults (CD4 cell counts > 200 cells/mm3 and a viral load < 50 000 copies/ml) > 18 years of age (mean age 47.3 years) with a documented history of PNEU-P-23 vaccination. The study was conducted in the USA between November 2009 and May 2012 and a total of 329 subjects received > 1 dose of the vaccine, with an intended schedule of 3 doses of PNEU-C-13 administered 6 months apart. The mean interval from the most recent PNEU-P-23 dose was 3.7 years. Of the 169 participants who had previously received more than one dose of PNEU-P-23, 26 had received three or more. The IgG and OPA geometric mean fold rises (GMFR) were greatest after dose 1. Differences between IgG GMFR before and after doses 2 and 3 were small and not significant. The IgG levels before and 1 month after vaccination were similar between subjects who had received one previous versus at least 2 previous doses of PNEU-P-23.
IV.5 Vaccine Administration and Schedule
Please refer to the Canadian Immunization Guide for information regarding the administration and vaccine schedules for PNEU-C-13 and PNEU-P-23 vaccine, including minimum intervals between PNEU-C-13 and PNEU-P-23 vaccine.
IV.6 Serological Testing
Pre- or post-immunization serology for pneumococcal vaccines need not be undertaken.
IV.7 Storage Requirements
Please refer to the Canadian Immunization Guide for information regarding storage of pneumococcal vaccines.
IV.8 Simultaneous Administration with Other Vaccines
Please refer to the Canadian Immunization Guide for information regarding simultaneous administration of pneumococcal vaccines with other vaccines.
IV.9 Adverse Events
Please refer to the previous PNEU-C-13 Statements and the Canadian Immunization Guide for adverse events reported in studies published prior to 2013. The following section serves as an update that includes studies published since the previous statement.
Four clinical trials have been published, in addition to the six trials reported in the previous statement, in which the authors assessed the safety of PNEU-C-13. The results of which are summarized below.
Local reactions
In the study by Glesby et al.Footnote 7, subjects (mean age 47.3 years old) received one to three doses of PNEU-C-13. The most common adverse event occurring through 14 days after vaccination was injection site pain, which occurred in 78.8% of participants receiving one dose, 81.4% of participants receiving two doses, and 81.9% of participants receiving three doses. Moderate injection site pain was more common in those who received ≥2 doses of PNEU-C-13 (33.3% in those receiving two, and 30.2% in those receiving three). Swelling occurred in 6.8%, 12.7%, and 11.2% after one dose, two doses, and three doses respectively, while redness occurred in 5.6%, 8.2%, and 9.5% after one dose, two doses, and three doses respectively. After the 3rd dose of PNEU-C-13, the percentage of participants with any redness or swelling was slightly higher in those who had received 2 doses or more of PNEU-P-23 (12.3% and 13.6%, respectively) compared to those who had received one previous dose of PNEU-P-23 (6.3% and 8.3%, respectively).
In the study by Tinoco et al.Footnote 6 for subjects 50-64 years of age, injection site pain was the most commonly reported adverse event and occurred in 75.5% of subjects (moderate pain was reported in only 21.5% of subjects). For subjects ≥65 years of age, injection site pain was reported in 60.6% of subjects, with moderate pain reported in only 8.5% of subjects. Swelling and redness were recorded in up to 21.5% of study participants.
In the study by Jackson et al.Footnote 6 comparing the safety of PNEU-C-13 to PNEU-P-23 vaccine in subjects 60 to 64 years of age, pain was most commonly reported adverse event (80.1% and 73.4% in the 13-valent and 23-valent groups respectively). Pain was moderate in 23.3% vaccinated with the PNEU-C-13 and 30.0% in those receiving PNEU-P-23. Swelling occurred in 19.3% and 13.1%, while redness occurred in 20.2% and 14.2% of those receiving PNEU-C-13 and PNEU-P-23, respectively.
In the trial by Bonten et al.Footnote 3, for subjects 65 years of age and older, pain was more common in the PNEU-C-13 group (36.1%) than in the placebo group (6.1%). Similarly, swelling occurred more frequently in the PNEU-C-13 group (6.8%) than in the placebo group (1.2%), while redness occurred in 4.9% receiving PNEU-C-13 and 1.2% receiving placebo. All other local events were mostly mild.
Systemic events
In the study by Glesby et al.Footnote 7) (HIV seropositive individuals, mean age 47.3 years), 88.4%, 85.6%, and 83.3% receiving 1 dose, 2 doses, and 3 doses reported a systemic event of any kind. The most common events were fatigue (occurring in 60.0%, 63.3%, and 56.3% for 1 dose, 2 doses, and 3 doses respectively), and headache (occurring in 61.6%, 56.1%, and 46.7% for those receiving 1 dose, 2 doses, and 3 doses respectively). Newly occurring generalized muscle pain occurred in 65%, 71.9%, and 65.9% of those receiving 1 dose, 2 doses, and 3 doses respectively. After dose 3, fatigue, headache and vomiting rates tended to be slightly higher in subjects who had previously received at least 2 doses of PNEU-P-23 (62%, 51.9% and 14.8%) compared to those who had previously received one dose of PNEU-P-23 (48.5%, 40% and 6.3%, respectively). The recommendations in this Statement, however, are directed at use of this vaccine in a different population, namely healthy adults 65 years of age and older.
In the Tinoco study, 76.8% of subjects 50-64 years of age and 60.7% of subjects 65 years and older reported a systemic adverse event, with muscle pain as the most common (60.5% in the younger age group and 43.9% in the older age group), followed by fatigue (47.2% and 38.6% for the younger and older age group, respectively), headache (44.3% and 32.6% for the younger and older age group, respectively), and diarrhea (26.1% and 15% for the younger and older age group, respectively)Footnote 5.
The Jackson study reported that for subjects 60 to 64 years of age, fatigue was the most common (63.2% in PNEU-C-13 group and 61.5% in the PNEU-P-23 group), followed by newly occurring generalized muscle pain (56.2% in PNEU-C-13 group and 57.8% in the PNEU-P-23 group), and headache (54.0% in PNEU-C-13 and 54.4% in the PNEU-P-23)Footnote 6.
IV.10 Contraindications and Precautions
Please refer to the previous statement and the Canadian Immunization Guide for more information. PNEU-C-13 is contraindicated in any individual with a history of anaphylaxis to any component of the vaccine, including diphtheria toxoid.
V. Recommendations
Although the burden of CAP is significant, S. pneumoniae only represents between 5% and 8% of identified etiological agents. Moreover, the publicly funded PNEU-C-13 childhood vaccination program implemented in most jurisdictions as of January 2011 is likely to reduce the circulation of pneumococcal vaccine serotypes in adults at the population level, including those 65 years of age and older. With the introduction of PNEU-C-7 immunization programs in children, vaccine strains have almost disappeared in the elderly population. Among adults 65 years of age and older, CAP and IPD caused by serotypes not contained in the currently available vaccines, but also by PNEU-P-23 serotypes that are not included in PNEU-C-13, continue to be the most important contributors to the pneumococcal disease burden of illness.
Recommendations for immunocompetent individuals provided below have been developed to guide protection at the individual level. In developing these recommendations, NACI has not considered other public health aspects of immunization, which will be addressed in a forthcoming statement. For optimal protection of immunocompromised individuals, NACI continues to recommend immunization with PNEU-C-13 vaccine followed by PNEU-P-23 vaccine. Detailed information is available in the NACI Statement on the Use of Conjugate Pneumococcal Vaccine – 13 Valent in Adults (Pneu-C-13).
Recommendation 1: NACI concludes that there is good evidence, on an individual basis, to recommend in immunocompetent adults aged 65 years and older not previously immunized against pneumococcal disease, the use of PNEU-C-13 vaccine followed by PNEU-P-23, for the prevention of CAP and IPD caused by the 13 pneumococcal serotypes included in the conjugate vaccine. (NACI recommendation grade A).
In immunocompetent adults aged 65 years and older, PNEU-C-13 vaccine has been shown to be safe and moderately efficacious against CAP and IPD caused by the 13 serotypes included in the vaccine. There are no effectiveness studies on PNEU-C-13 in adult populations. In clinical trials, local adverse events such as injection site pain and systemic adverse events such as fatigue and newly occurring generalized pain were common but overall mild.
If immunization with PNEU-C-13 vaccine is being considered, pneumococcal vaccine-naïve individuals should first receive PNEU-C-13 vaccine, followed by PNEU-P-23 vaccine at least 8 weeks later (Figure 4). The purpose of administering PNEU-P-23 to an individual who has already received PNEU-C-13 is to expand the breadth of serotypes against which an individual is protected. For immunization of individuals who have previously received PNEU-P-23 vaccine, NACI recommends administration of PNEU-C-13 at least one year after any previous dose of PNEU-P-23 vaccine, due to the theoretical potential for decrease in antibody titers following immunization with PNEU-P-23 vaccine.
There is no evidence on the safety and immunogenicity of concomitant administration of PNEU-C-13 with PNEU-P-23 vaccine and, as a precaution, co-administration of these two vaccines should be avoided until this information becomes available. There are no data on the additional benefit of booster immunization in immunocompetent individuals 65 years or older following the receipt of PNEU-C-13 or PNEU-P-23 vaccine, and therefore there is no recommendation at this time for additional vaccine doses.
Please refer to previous NACI Statements for additional background information about recommended booster doses and intervals for PNEU-P-23 vaccine.
Recommendation 2: NACI concludes that, based on circulating serotypes, there is fair evidence to recommend the use of PNEU-P-23 vaccine in routine immunization programs for adults aged 65 years and older. (NACI recommendation Grade B)
Because the burden of pneumococcal disease caused by serotypes included in the PNEU-P-23 vaccine, but not contained in the PNEU-C-13 vaccine remains significant, NACI continues to recommend the administration of PNEU-P-23 for all adults 65 years of age and older who have not received either vaccine previously. PNEU-C-13 vaccine effectiveness is dependent on the circulation of vaccine specific serotypes. Comparative immunogenicity studies between PNEU-C-13 and PNEU-P-23 indicate that GMTs are higher in elderly subjects vaccinated with PNEU-C-13 for 8 serotypes that are common to both vaccines, but the clinical and population-level implications associated with this improved immunogenicity remains unclear. No additional booster dose of PNEU-P-23 vaccine is currently recommended for those over the age of 65 years who do not have other underlying medical conditions that would put them at higher risk for IPD or severe CAP.
A statement from the population level perspective, taking into account the impact of PNEU-C-13 childhood vaccination programs and serotype circulation will be available in the future.
Figure 4. Summary of recommendations for individuals who wish to protect themselves against the 13 serotypes included in PNEU-C-13
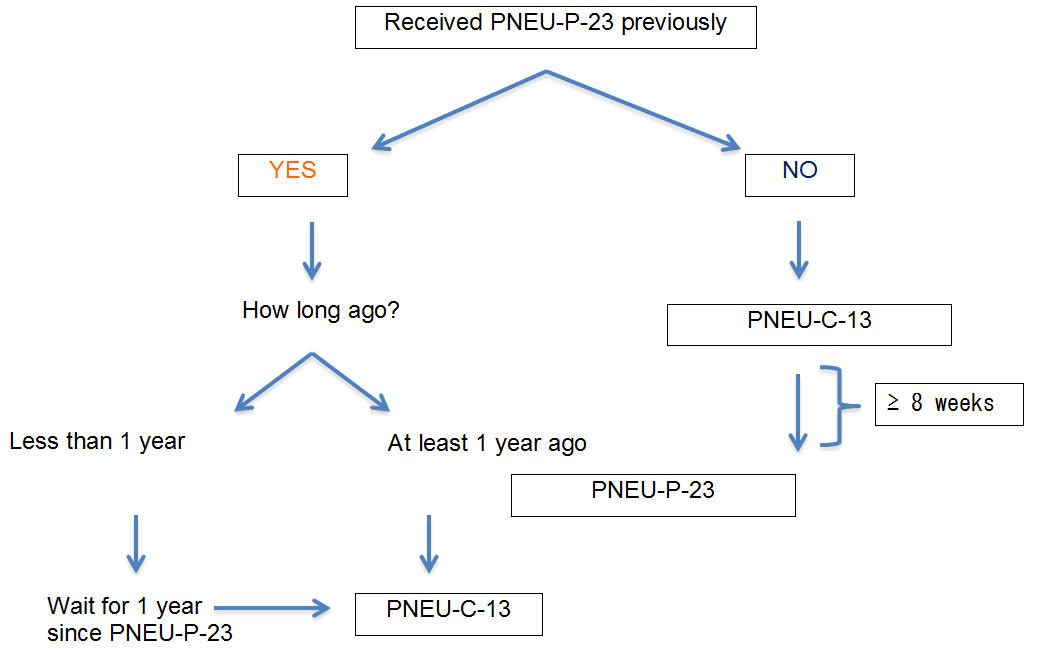
Figure 4 - Text Description
The figure is a flowchart depicting the summary of recommendations for individuals who wish to protect themselves against the 13 serotypes included in PNEU-C-13.
Has the individual received PNEU-P-23 vaccine previously?
- If yes, how long ago?
- If it was less than one year ago, wait for one year since receipt of PNEU-P-23 vaccine before administering PNEU-C-13 vaccine.
- If it was at least one year ago, administer PNEU-C-13.
- If no, administer PNEU-C-13 and then wait at least 8 weeks before administration of the PNEU-P-23 vaccine.
VI. Surveillance and Research Priorities
- Determine whether the concomitant administration of PNEU-C-13 and PNEU-P-23 increases the risk of immune interference or the risk of adverse events.
- Conduct research on the efficacy and effectiveness of PNEU-C-13 boosters in immunocompetent adults over 65 years of age.
- Collect and analyze national serotype-specific and age-specific data for IPD and CAP
Tables
| Evidence of Efficacy | ||||||
|---|---|---|---|---|---|---|
| Study details | Summary | |||||
| Study | Vaccine | Study Design | Participants | Summary of Key Findings Using Text or Data [VE (95% CI)] |
Level of Evidence | Quality |
| Bonten, 2015Footnote 3 | PNEU-C-13 vs. placebo Route: IM Schedule: 0 weeks Dose: 0.5 ml single dose |
Randomized, double-blind, placebo controlled trial Length of follow-up: mean time 3.97 years Power: 90% |
84,496 total PNEU-C-13: 42,240 Placebo: 42,256 Patients were immunocompetent adults ≥65 years of age who were previously unvaccinated with any pneumococcal vaccine |
New episode of vaccine type CAP (VT-CAP), nonbacteremic and noninvasive (nonbac/inv-CAP), new episode of all cause CAP (AC-CAP), and vaccine type IPD (VT-IPD) Per-protocol: VT-CAP: VE 45.6% (21.8, 62.5) Nonbac/inv-CAP: VE 45.0% (14.2, 65.3) VT-IPD: VE 75.0% (41.4, 90.8) Intention to treat: VT-CAP: VE 37% AC-CAP: VE 5.1% Nonbac/inv-CAP: VE 41.1% VT-IPD: VE 75.8% |
Level I | Good |
| Evidence of immunogenicity | ||||||
|---|---|---|---|---|---|---|
| Study details | Summary | |||||
| Study | Vaccine | Study Design | Participants | Summary of Key Findings Using Text or Data [Ratio (95% CI)] |
Level of Evidence | Quality |
| Glesby, 2015Footnote 7 | PNEU-C-13 Schedule: 1 dose at enrollment, 6 months, and 12 months. Route: IM?? Dose = 0.5ml |
Phase III, open-label, single-arm study Study period Nov 2009 to may 2012 HIV seropositive patients CD4 cell counts ≥ 200 cells/mm3 and viral loads <50,000 copies/mL |
329 subjects received ≥1 dose of PNEU-C-13 (mean age: 47.3 years) 300 subjects received dose 2 279 received dose 3 Response: 2 fold rise Patients were followed-up after 1 month for each dose, and 6 months after the 3rd dose. Response: fold rise in GMFRs and GMTs |
IgG GMFRs (after dose 1 vs. before dose 1; after dose 2 vs. after dose 1; after dose 3 vs. after dose 2): S1: 3.93 (3.33–4.63); 1.10 (1.00–1.20); 0.94 (.88–1.01) S3: 2.44 (2.18–2.74); 1.18 (1.08–1.28); 1.01 (.95–1.08) S4: 5.40 (4.67–6.24); 1.20 (1.09–1.32); 1.01 (.94–1.08) S5: 1.65 (1.51–1.80); 1.13 (1.05–1.22); 0.99 (.94–1.05) S6A: 3.11 (2.70–3.58); 1.38 (1.25–1.52); 1.19 (1.11–1.27) S6B: 2.76 (2.45–3.12); 1.54 (1.40–1.70); 1.21 (1.13–1.31) S7F: 3.85 (3.29–4.50); 0.99 (.90–1.08); 1.07 (1.00–1.14) S9V: 2.83 (2.53–3.16); 1.14 (1.05–1.24); 1.08 (1.02–1.15) S14: 2.64 (2.28–3.05); 1.23 (1.10–1.37); 1.08 (0.99–1.17) S18C: 4.26 (3.64–5.00); 0.93 (.86–1.01); 1.09 (1.02–1.16) S19A: 2.45 (2.17–2.76); 1.17 (1.06–1.28); 1.03 (.98–1.09) S19F: 3.81 (3.27–4.45); 2.07 (1.78–2.41); 1.17 (1.08–1.27) S23F: 3.36 (2.95–3.83); 1.46 (1.32–1.62); 1.25 (1.15–1.37) OPA GMFRs (after dose 1 vs. before dose 1; after dose 2 vs. after dose 1; after dose 3 vs. after dose 2): S1: 5.9 (4.74–7.31); 1.0 (.84–1.20); 1.2 (1.06–1.39) S3: 4.7 (3.90–5.55); 1.5 (1.29–1.73); 1.3 (1.13–1.44) S4: 22.7 (16.40–31.55); 1.1 (.92–1.36); 1.0 (.90–1.18) S5: 8.4 (6.55–10.80); 1.0 (.79–1.20); 1.1 (.95–1.28) S6A: 55.6 (39.25–78.64); 1.7 (1.39–2.15); 1.2 (1.04–1.39) S6B: 12.5 (9.11–17.17); 1.6 (1.34–2.02); 1.3 (1.16–1.50) S7F: 17.7 (12.53–25.08); 1.2 (.96–1.45); 1.1 (.95–1.28) S9V: 12.7 (8.81–18.25); 1.6 (1.26–2.14); 1.4 (1.09–1.81) S14: 3.2 (2.49–4.11); 1.1 (.98–1.30); 1.1 (.97–1.24) S18C: 13.2 (9.42–18.60); 1.2 (.95–1.47); 1.3 (1.10–1.60) S19A: 8.4 (6.69–10.56); 1.3 (1.15–1.50); 1.0 (.95–1.15) S19F: 9.6 (7.00–13.16); 1.9 (1.48–2.39); 0.9 (.76–1.09) S23F: 12.3 (9.06–16.66); 2.9 (2.29–3.77); 1.3 (1.16–1.56) |
Level II | Good |
| Jackson 2013Footnote 6 | PNEU-C-13 compared to PNEU-P-23 Schedule: 1 dose at enrolment Route: IM Dose: 0.5mL |
Randomized, modified double-blind trial. Vaccine naïve adults Response: 2 fold increase in GMR |
417 subjects received PNEU-C-13 (mean age 61.8 years) 414 subjects received PNEU-P-23 (mean age 61.7 years) Followed for up to 1 year Safety followed for 6 months Adults 60-64 years of age |
Comparison of OPA GMTs 1 month after PNEU-C-13 vs. PNEU-P-23 [ratio (95% CI)] age group: 60-64 years: 1: 1.4 (1.10, 1.78) 3: 1.1 (0.90, 1.32) 4: 1.6 (1.19, 2.13) 5: 1.2 (0.93, 1.62) 6B: 2.5 (1.82, 3.48) 7F: 2.8 (1.98, 3.87) 9V: 2.9 (2.00, 4.08) 14: 0.9 (0.64, 1.21) 18C: 1.9 (1.39, 2.51) 19A: 1.9 (1.56, 2.41) 19F: 1.0 (0.72, 1.28) 23F: 5.2 (3.67, 7.33) 6A: 12.1 (8.63, 17.08) |
Level I | Good |
| Tinoco 2015Footnote 5 | PNEU-C-13 in adults who have not received PNEU-P-23 Schedule: 1 dose at enrolment Route: IM Dose: 0.5mL |
Open label, multicenter clinical trial Response: OPA GMT GMFR |
Two age groups: 50-64: 161 subjects ≥ 65: 161 subjects Subjects ≥50 years of age, including those with underlying diseases (but stable ≥6 months with no required change in therapy), no previous vaccination or infection with S. pneumoniae for past 5 years, and no immunodeficiency of any kind. |
Comparison between age groups on OPA GMT in younger vs. older populations [ratio (95% CI)] 1: 1.4 (0.96, 2.10) 3: 1.0 (0.74, 1.33) 4: 1.4 (1.05, 1.95) 5: 1.0 (0.65, 1.58) 6A: 1.0 (0.73, 1.39) 6B: 1.2 (0.88, 1.58) 7F: 1.6 (1.25, 2.11) 9V: 1.7 (1.17, 2.54) 14: 1.2 (0.89, 1.60) 18C: 1.4 (0.99, 1.96) 19A: 1.3 (0.98, 1.70) 19F: 0.9 (0.63, 1.38) 23F: 0.9 (0.60, 1.48) |
Level II | Good |
| Level | Description |
|---|---|
| I | Evidence from randomized controlled trial(s). |
| II-1 | Evidence from controlled trial(s) without randomization. |
| II-2 | Evidence from cohort or case-control analytic studies, preferably from more than one centre or research group using clinical outcome measures of vaccine efficacy. |
| II-3 | Evidence obtained from multiple time series with or without the intervention. Dramatic results in uncontrolled experiments (such as the results of the introduction of penicillin treatment in the 1940s) could also be regarded as this type of evidence. |
| III | Opinions of respected authorities, based on clinical experience, descriptive studies and case reports, or reports of expert committees. |
| Quality of Rating | Description |
|---|---|
| Good | A study (including meta-analyses or systematic reviews) that meets all design- specific criteriaFootnote * well. |
| Fair | A study (including meta-analyses or systematic reviews) that does not meet (or it is not clear that it meets) at least one design-specific criterionFootnote * but has no known "fatal flaw". |
| Poor | A study (including meta-analyses or systematic reviews) that has at least one design-specificFootnote * "fatal flaw", or an accumulation of lesser flaws to the extent that the results of the study are not deemed able to inform recommendations. |
|
|
| Grade | Description |
|---|---|
| A | NACI concludes that there is good evidence to recommend immunization. |
| B | NACI concludes that there is fair evidence to recommend immunization. |
| C | NACI concludes that the existing evidence is conflicting and does not allow making a recommendation for or against immunization; however other factors may influence decision-making. |
| D | NACI concludes that there is fair evidence to recommend against immunization. |
| E | NACI concludes that there is good evidence to recommend against immunization. |
| I | NACI concludes that there is insufficient evidence (in either quantity and/or quality) to make a recommendation, however other factors may influence decision-making. |
List of Abbreviations
- Abbreviation
- Term
- CAP
- Community-acquired pneumonia
- CAPiTA
- Community-Acquired Pneumonia Immunization Trial in Adults
- CNDSS
- Canadian Notifiable Disease Surveillance System
- GMFR
- Geometric mean fold rises
- GMT
- Geometric mean titres
- IPD
- Invasive pneumococcal disease
- NACI
- National Advisory Committee on Immunization
- NML
- National Microbiology Laboratory
- OPA
- Opsonophagocytic activity
- PNEU-C-7
- 7-valent pneumococcal conjugate vaccine
- PNEU-C-13
- 13-valent pneumococcal conjugate vaccine
- PNEU-P-23
- 23-valent pneumococcal polysaccharide vaccine
- PWG
- Pneumococcal Working Group
- SOS
- Serious Outcome Surveillance
- UAD
- Urinary antigen detection
- VE
- Vaccine efficacy
- VT
- Vaccine-type
Acknowledgments
NACI Members: Dr. I. Gemmill (Chair), Dr. C. Quach (Vice-Chair), Dr. N. Dayneka,
Dr. S. Deeks, Dr. B. Henry, Ms. S. Marchant-Short, Dr. M. Salvadori, Dr. N. Sicard,
Dr. W. Vaudry, Dr. D. Vinh, Dr. R. Warrington.
Liaison Representatives: Dr. J. Blake (Society of Obstetricians and Gynaecologists of Canada), Dr. J. Brophy (Canadian Association for Immunization Research and Evaluation),
Dr. A. Cohn (Centers for Disease Control and Prevention, United States), Dr. J. Emili (College of Family Physicians of Canada), Dr. M. Lavoie (Council of Chief Medical Officers of Health),
Dr. C. Mah (Canadian Public Health Association), Dr. D. Moore (Canadian Paediatric Society),
Dr. A. Pham-Huy (Association of Medical Microbiology and Infectious Disease Canada),
Ms. E. Sartison (Canadian Immunization Committee).
Ex-Officio Representatives: Dr. (LCdr) K. Barnes (National Defence and the Canadian Armed Forces), Ms. G. Charos (Centre for Immunization and Respiratory Infectious Diseases [CIRID], Public Health Agency of Canada [PHAC]), Dr. G. Coleman (Biologics and Genetic Therapies Directorate, Health Canada [HC]), Dr. J. Gallivan (Marketed Health Products Directorate [MHPD], HC), Ms. J. Pennock (CIRID, PHAC), Dr. T. Wong (First Nations and Inuit Health Branch [FNIHB], HC).
This statement was prepared by Dr. O. Baclic (CIRID, PHAC), Dr. C. Quach (McGill University) and Dr. N. Winters (McGill University), and approved by NACI.
NACI gratefully acknowledges the contribution of Dr. P. DeWals (Pneumococcal Working Group (PWG)), Dr. D. Fisman (PWG), Ms. C. Jensen (CIRID, PHAC), Dr. J. Johnstone (PWG),
Dr. J. Kellner (PWG), Dr. S. McNeil (PWG), Dr. S. Rechner (PWG), Ms. L. Sherrard (CIRID, PHAC) and Dr. G. Tyrrell (PWG).