Chronic bronchitis in Aboriginal people—prevalence and associated factors
S. Konrad, MSc (1); A. Hossain, MSc (1); A. Senthilselvan, PhD (2); J. A. Dosman, MD (3); P. Pahwa, PhD (1, 3)
https://doi.org/10.24095/hpcdp.33.4.03
This article has been peer reviewed.
Author references:
- Department of Community Health and Epidemiology, University of Saskatchewan, Saskatoon, Saskatchewan, Canada
- Department of Public Health Sciences, School of Public Health, University of Alberta, Edmonton, Alberta, Canada
- Canadian Centre for Health and Safety in Agriculture, University of Saskatchewan, Saskatoon, Saskatchewan, Canada
Correspondence: Punam Pahwa, Canadian Centre for Health and Safety in Agriculture, University of Saskatchewan, 103 Hospital Drive, Saskatoon, SK S7N 0W8; Tel.: 306-966-7944; Fax: 306-966-7920; Email: pup165@mail.usask.ca
Abstract
Introduction: Knowledge about chronic bronchitis (CB) among Aboriginal people in Canada is limited. The aim of this study was to determine the prevalence of CB and its associated factors among Aboriginal people aged 15 years plus.
Methods: Logistic regression analysis was used on data from the cross-sectional 2006 Aboriginal Peoples Survey to determine risk factors associated with CB.
Results: CB prevalence was 6.6% among First Nations, 6.2% among Métis and 2.4% among Inuit. Prevalence was higher among females than males (7.2% versus 5.0%). Individuals with CB were more likely to be older, living at a lower income, with a lower educational attainment and residing in rural areas. Smoking status and body mass index were also significantly associated with CB, but their effect differed by sex. Obesity was particularly significantly associated with CB among females compared with males, and current smoking and non-smoking status was significantly associated with CB among females but not males.
Conclusion: These findings identify factors associated with CB among Aboriginal people. As such, they may represent potentially preventable risk factors that can inform health promotion and disease prevention practices.
Keywords: chronic bronchitis, Aboriginal people, Aboriginal Peoples Survey
Introduction
The health of Aboriginal people—First Nations, Metis and Inuit—is notably poorer than that of the general Canadian population,Endnote 1 a trend also observed in their respiratory health.Endnote 2 Approximately 15% of Aboriginal people have been diagnosed with at least one of four respiratory diseases (asthma, chronic bronchitis [CB], emphysema and chronic obstructive pulmonary disorder [COPD]) compared to 10% for non-Aboriginal people in Canada, according to the 2005 Canadian Community Health Survey (CCHS).Endnote 3 Age-standardized hospital separation rates in western Canada for Aboriginal people for all respiratory diseases in 2000 were 3040 per 100 000 population compared with 920 per 100 000 population in their non-Aboriginal counterparts.Endnote 4
CB is one such respiratory disease defined as ''cough productive of sputum for at least three months of the year for at least two years.''Endnote 5 CB is a significant cause of morbidity and an underlying condition for the development of COPD.Endnote 6
Our knowledge of CB and its associated factors in Canadian Aboriginal people is limited. The 2002/03 First Nations Regional Longitudinal Health Survey found age-standardized prevalence of self-reported physician-diagnosed CB to be 3.7% in First Nations living on-reserve;Endnote 7 the prevalence in Aboriginal people living off-reserve is 4.9%, according to the 2005 CCHS.Endnote 3 Both of these rates are higher than the prevalence of 2.4% found in the non-Aboriginal Canadian population, according to the 2005 CCHS.Endnote 3
The prevalence of CB in Aboriginal people may be high due to the high prevalence of various risk factors. Smoking, low family income, poor schooling and inadequate housing, which have been significantly associated with the prevalence and incidence of CB,Endnote 8, Endnote 9, Endnote 10 are more prevalent among Aboriginal people. According to the 2002/03 First Nations Regional Longitudinal Health Survey, roughly 59% of First Nations self-reported currently smoking, with smoking rates for on-reserve First Nations slightly higher than for those living off-reserve.Endnote 7 Smoking rates among Inuit have been reported to be as high as 70%.Endnote 11
In 2005, Aboriginal people aged 25 to 54 years had a much lower median total individual income ($22 000) compared with their non-Aboriginal counterparts ($33 000).Endnote 12 Of those aged 25 to 64 years, 44% of Aboriginal people compared with 60% of the general population had completed some post-secondary schooling.Endnote 13 Lower education is often associated with lower socio-economic status, which may correlate with lower income and worse housing conditions. In 2006, Aboriginal people were almost four times as likely to live in crowded homes, and three times as likely to live in a dwelling in need of major repairs than non-Aboriginal people.Endnote 14 Poor housing conditions are often associated with damp and mould, which may lead to adverse respiratory outcomes.Endnote 2
We carried out a descriptive study to assess the relationship between demographic, environmental and population characteristics and CB. To date, the determinants of CB among Aboriginal people in Canada have not been well established. Thus, the objective of this study was to confirm the prevalence (crude and adjusted) of CB and determine its associated factors in off-reserve Canadian Aboriginal people aged 15 years and older.
Methods
Study population and data source
The Aboriginal Peoples Survey (APS) 2006 is a national cross-sectional survey conducted from October 2006 through March 2007 by Statistics Canada in partnership with Aboriginal organizations.Endnote 15 This is the third time that Statistics Canada has administered the APS, the first being in 1991 and the second in 2001. The target population of this survey was off-reserve First Nations, Métis and Inuit people living in urban, rural and northern locations throughout Canada. A multi-stage sampling design was used to select and collect data from all the provinces. Details of this sampling design can be found elsewhere.Endnote 15 Briefly, a target sample was created based on responses to four screening questions in the 2006 Census long form that indicated that the respondents had Aboriginal ancestors and/or identified as North American Indian and/or Métis and/or Inuit and/or had treaty or registered Indian status and/or had Indian Band membership. The sample was then divided according to domains of estimation, based on Aboriginal identity, age groups and geographical regions. A random sample was then selected within each domain of estimation. The APS included information on Aboriginal identity and ancestry, education, language, labour activity, income, health, communication technology, mobility, housing and family background. There were a total of 48 921 participants, with a response rate of 80.1%. Data were collected via self-administered questionnaires or personal interviews over the phone or in person.
The target populations of this survey were Aboriginal children and youth (6–14 years) and Aboriginal adults (≥ 15 years). Since our study focused on the adult population, we excluded APS participants aged less than 15 years.
The University of Saskatchewan Research Ethics Board approved this research. We obtained permission to access the data from Statistics Canada and conducted all analyses within the Statistics Canada Research Data Centre at the University of Saskatchewan.
Measures
The APS included a set of questions designed to investigate survey participants' chronic conditions. The variables used for the analysis are defined below.
Outcome
In this report, the outcome variable of interest for adults was based on the following question: ''Have you been told by a doctor, nurse or other health professional that you have: chronic bronchitis?''Endnote 15
Factors
Of interest were demographic, environmental, and health and lifestyle variables (see Table 1). Demographic variables consisted of age, sex, ethnicity and marital status; environmental variables consisted of location of residence, number of persons per household and geographical area. Location of residence, rural or urban, was based on Statistics Canada determinations (minimum population concentrations and population density per square kilometer). Geographical areas were broken down into Territories (Yukon, Northwest Territories, Nunavut), British Columbia, Prairies (Alberta, Saskatchewan, Manitoba), Ontario, Quebec, and Atlantic (New Brunswick, Prince Edward Island, Nova Scotia, Newfoundland and Labrador). Health-related variables consisted of self-perceived general health status, smoking status and body mass index (BMI). BMI was introduced as a continuous variable in the multivariate model, and was afterwards categorized for a schematic depiction (Figure 2). Socio-economic status variables consisted of education and income.
Statistical analysis
We calculated the percentage of participants reporting CB and associated factors. Weight variables computed by Statistics Canada methodologists used in all analyses ensured that the final estimates were representative of the surveyed population. We used weighted multiple logistic regression modelling based on a maximum likelihood to test the association of CB risk factors. Balanced repeated replication resampling technique was used to estimate the standard errors of regression coefficients in order to account for clustering inherited in the study design of the cross-sectional complex survey. Statistically significant two-way interactions were examined. The results of the models are presented as odds ratios (OR) along with the 95% confidence intervals (CIs). Statistical packages SAS version 9.2 (SAS Institute Inc., Cary, NC, US) and STATA version 11.0 were used to conduct all analyses.
Results
Of the adult APS respondents, 50.0% were First Nations, 45.2% were Metis and the remaining 4.8% were Inuit. Due to the small number of Inuit in the dataset, they were excluded from all multivariate analyses.
Crude prevalence of chronic bronchitis
Table 1 summarizes both the prevalence and odds ratio for CB. The crude prevalence of CB was 6.6%, 6.2% and 2.4% among First Nations, Metis and Inuit, respectively (Table 1). Overall prevalence was 6.0% for off-reserve Aboriginal people. Prevalence was 8.3% among smokers and 3.3% among non-smokers. CB was more prevalent among females than males (5.0% vs. 7.2%) and increased with age, from 2.7% for those aged 15 to 19 years to 10.1% for those aged 55 years and older. The prevalence was highest in Ontario, at 9.1%, and the Atlantic region, at 7.4%. Prevalence was also higher in those living at a lower income and with a lower educational attainment.
Those with diabetes had a prevalence of 13.2%, while those without had a prevalence of 8.1%.
Adjusted prevalence of chronic bronchitis
Table 2 summarizes all the variables that were found to be significant predictors of CB in the multivariate model.
In the multivariate model, the prevalence of CB among Métis did not significantly differ from that among First Nations (OR = 1.05; 95% CI = 1.00–1.10). As expected, older respondents were more likely to report CB compared to those in the youngest age group (≥ 55 years: OR = 3.06; 95% CI = 2.73–3.43). Those who had never married or else were divorced or widowed were less likely to report CB (never married: OR = 0.72; 95% CI = 0.68–0.78; divorced/widowed: OR = 0.90; 95% CI = 0.84–0.96). Income and educational attainment were inversely associated with CB; participants who had not completed high school had 1.4 (95% CI = 1.30–1.57) times greater odds of having CB than those with a university degree, and those with an income of less $20 000 had 3.4 (95% CI = 3.1–3.6) times greater odds of having CB than those with an income of $80 000 or more. Urban residence was also positively associated with CB (OR = 1.31; 95% CI = 1.25–1.38). BMI was found to be a significant predictor as a quadratic term, representing a U-shaped relationship (BMI = 25.0–29.9 kg/m2: OR = 0.91, CI = 0.73–1.13; BMI > 29.9 kg/m2: OR = 1.26, CI = 1.02–1.55).
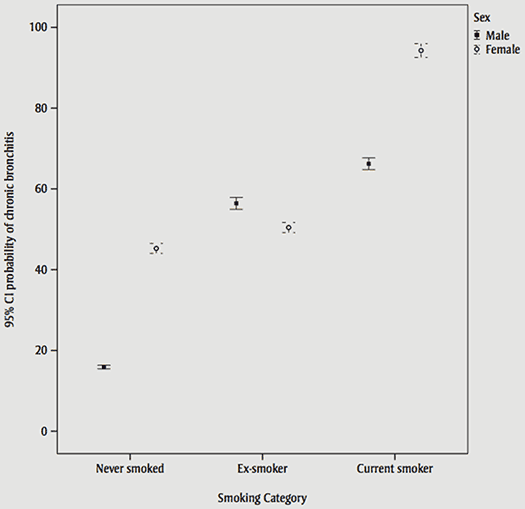
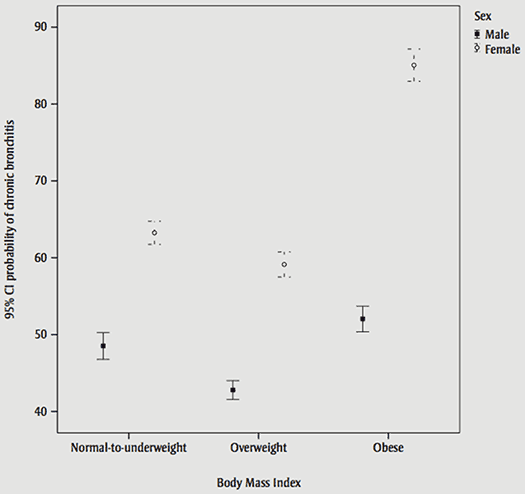
There were also two significant interactions between sex and smoking status and sex and BMI. Among non-smokers and current smokers, females have a higher probability of CB than do men, whereas among ex-smokers, the probability of CB was slightly lower for females than males (Figure 1). In all the three categories of BMI (healthy and underweight, overweight, and obese), the probability of CB was significantly higher in females than males. However, this difference was notably greater in obese people.
Discussion
By using a cross-sectional cohort, this study determined the prevalence of CB and examined the associated factors in Aboriginal adults. We found the prevalence of CB to be 6.0% overall, 6.6% for First Nations, 6.2% for Metis, and 2.4% for Inuit. The multivariate analysis showed older age, smoking, obesity, lower educational attainment, lower income, and urban residence to be significantly associated with self-reported physician-diagnosed CB. Two-way interactions between sex and smoking and between sex and BMI were also observed.
Our analysis found the prevalence of CB to be slightly higher than the 4.9% found by the 2005 CCHS among off-reserve Aboriginal people and the 2.4% found among non-Aboriginal people. The CCHS measures self-reported health-provider-diagnosed CB in a way similar to the APS.
The prevalence of CB was particularly low among Inuit compared with First Nations and Métis. Since the rates of smoking were highest in this group,Endnote 16 the low prevalence of CB may be attributed to geographical barriers in access to care and thus decreased opportunities for a diagnosis. This rationale could also be used to at least partly explain the difference observed between locations of residence, in which urban residents were more likely to self-report physician-diagnosed CB compared with rural residents.
Supporting our findings of differences by sex in the prevalence of CB, a study from a small Saskatchewan town that focused on a grain-farming population found the prevalence of CB to be 9.6% among women and 4.2% among men.Endnote 17
Numerous other studies also found smoking, income and poor schooling to be independently associated with CB.Endnote 5, Endnote 18, Endnote 19 Smoking is an established and major risk factor for CB.Endnote 19 Income and education, indicators of socio-economic status, suggest that other variables may be mediating this association.Endnote 18 Low income, for example, limits individual options in healthy living environments and foods, which may, in turn, contribute to obesity.Endnote 20
The link between obesity and chronic respiratory diseases has also become increasingly recognized. In a longitudinal cohort, Guerra et al.Endnote 21 found that patients with CB were more likely to be obese. In our study, we observed a possible U-shaped risk trend (shown in Figure 1), meaning that both low and high BMI correlated with the disease. Guerra et al.Endnote 21 also observed a similar, albeit non-significant, trend. In addition, they observed a temporal relationship; a BMI of 28 kg/m2 or more increased the risk of receiving a physician-confirmed diagnosis of CB (OR = 1.80; 95% CI = 1.32–2.46) two years later.Endnote 21 While their study suggests a causal relationship, more research is needed to elucidate this relationship. Nevertheless, obesity increases the risk of respiratory dysfunction, as indicated by a review of obesity.Endnote 22
Limitations
There were several limitations to our study. In surveys such as the APS, the measurement of CB lacks clinical accuracy, which could introduce misclassification.Endnote 23 The APS asks a single question about CB, whether respondents have been told by a health care professional that they have CB. Diagnosis of chronic diseases may also be influenced by availability and use of health care services, possibly causing systemic bias. In addition, all answers in this survey are self-reported: self-reporting may underestimate the prevalence of some risk factors, such as weight, smoking status and income. Finally, this survey only collected data on off-reserve First Nations. Based on the 2006 Census, about 40% of First Nations people live on reserve.Endnote 14 Various statistics do show significant differences between on-reserve and off-reserve First Nations, and thus these results may not necessarily be generalizable to all First Nations. In addition, Inuit were removed from the multivariate analysis, further limiting the generalizability of these findings to this population.
Conclusion
To our knowledge this is the first report that has specifically examined factors associated with CB among the Aboriginal population. Our research provides a snapshot of CB and its determinants; nevertheless, further analyses are needed to explore these associations, particularly how low socio-economic status and obesity may be affecting CB. Our study highlights the importance of smoking cessation and reduction in BMI in this population, particularly among females.
In conclusion, this study showed that potentially preventable risk factors (low socio-economic status, obesity and smoking) were significantly associated with CB after adjusting for possible confounders. Such information may be useful for designing and promoting preventive campaigns specifically for the Aboriginal population.
Acknowledgements
This study was supported by the Canadian Institute for Health Research pilot project program and the Canadian Centre for Health and Safety in Agriculture.
Conflict of interest: none.
References