Abstract
Introduction: There are analytic challenges involved with estimating the aggregate burden of multiple risk factors (RFs) in a population. We describe a methodology to account for overlapping RFs in some sub-populations, a phenomenon that leads to ''double-counting'' the diseases and economic burden generated by those factors.
Methods: Our method uses an efficient approach to accurately analyze the aggregate economic burden of chronic disease across a multifactorial system. In addition, it involves considering the effect of body weight as a continuous or polytomous exposure that ranges from no excess weight through overweight to obesity. We then apply this method to smoking, physical inactivity and overweight/obesity in Manitoba, a province of Canada.
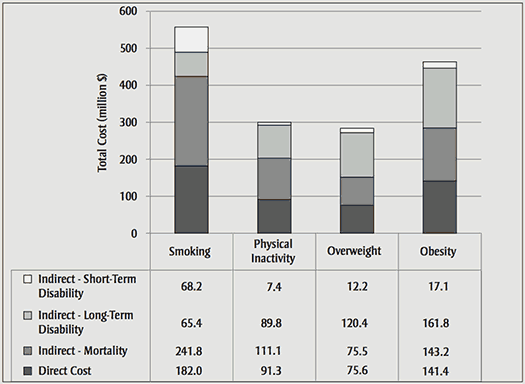
Results: The annual aggregate economic burden of the RFs in Manitoba in 2008 is about $1.6 billion ($557 million for smoking, $299 million for physical inactivity and $747 million for overweight/obesity). The total burden represents a 12.6% downward adjustment to account for the effect of multiple RFs in some individuals in the population.
Conclusion: An improved estimate of the aggregate economic burden of multiple RFs in a given population can assist in prioritizing and gaining support for primary prevention initiatives.
Keywords: population attributable fraction, risk factors, obesity, physical inactivity, tobacco smoking, chronic disease
Introduction
Health care planners have long been concerned with the ''epidemiologic transition,'' the process whereby chronic illnesses displace pandemics of infection as the primary source of morbidity and mortality in the world.Endnote 1 The latest phase of this transition is marked by increased prevalence of overweight/obesity and physical inactivity in many countries.Endnote 2 Excess body weight and/or physical inactivity have been implicated in chronic diseases such as cardiovascular disease, stroke, type 2 diabetes, chronic kidney Endnote 3, Endnote 4, Endnote 5, Endnote 6, Endnote 7, Endnote 8, Endnote 9, Endnote 10, Endnote 11, Endnote 12disease, osteoarthritis and certain cancers. Consequently, these riskEndnote 13 factors (RFs) have joined tobacco smoking as key prevention targets.
Estimations of the economic burden generated by such RFs have been undertakenEndnote 14 in many jurisdictions in the world, including Canada as a wholeEndnote 15, Endnote 16, Endnote 17, Endnote 18, Endnote 19 and a few Canadian provinces.Endnote 20, Endnote 21 In addition to understanding the costs related to a single RF such as tobacco smoking, estimating the aggregate economic burden generated by two or more RFs in a population is often of interest. This information can inform prevention strategies aimed at more than one RF, for example, public health programs that address both physical inactivity and overweight/obesity. There are, however, analytical challenges involved with the estimation of the aggregate burden of multiple RFs in a population.Endnote 22 Certain costs (such as those generated by incident disease or by death) are by definition accrued only once. Thus, it is important to account for the confounding effect of multiple RFs in the same individual, and specifically to adjust for any increase in the calculated economic burden due to double-counting cases and costs.
Population attributable fraction (PAF) offers a powerful way to interpret causation in the practical terms of prevention. In short, PAF is that proportion of disease incidence (or costs) that will be removed if exposure to the causative RF is removed. The approach, however, becomes more complicated when the aim is to assess the combined effect of multiple RFs.
A number of innovative approaches have been developed to quantify the effects of multiple RFs in specific cohorts.Endnote 23 The World Cancer Research Fund, for example, used a process that could be described as ''sequential prevention,'' explained as follows:Endnote 24p149
Because no individual case of cancer can be prevented more than once, this calculation was done in a way that avoided the possibility of ''double counting.'' The
PAF for the first exposure was subtracted from 100 per cent and the
PAF for the second exposure was applied to the remainder. This process was performed sequentially for all relevant exposures, resulting in an estimated
PAF for all exposures combined.
While it makes sense as a goal, the work of disentangling the impact of overlapping RFs is often omitted from estimations of the related economic burden. A case in point is the series of papers published from 2005 to 2009 by a British Heart Foundation group on the burden of ill health in the United Kingdom due to physical inactivity,Endnote 25 overweight/obesity,Endnote 26 tobacco smokingEndnote 27 and other RFs.Endnote 28, Endnote 29 In a summary paper, the authors acknowledge that ''the possible overlap between risk factors (such as overweight and obesity) was not addressed here but should be considered when calculating the total economic burden of these risk factors.''Endnote 30,p534
To address this challenge, we describe a methodology to account for overlapping RFs when estimating the aggregate economic burden of associated chronic illnesses. The approach involves four steps:
- consideration of the function of body weight as a continuous or ''polytomous'' exposure ranging from no excess weight through overweight to obesity;
- estimating an aggregate burden of chronic disease across a multifactorial system in a manner that adjusts for the effect of more than one RF;
- estimating the aggregate economic burden adjusted for multiple RFs occurring in some individuals; and
- disaggregating the total burden to provide an estimate of the economic cost notionally attached to each RF.
To our knowledge, this is the first published attempt to address the issue of double-counting costs due to overlapping RFs in some individuals when addressing the economic burden of multiple RFs.
As a demonstration of the utility of this approach, the economic burden of diseases attributable to tobacco smoking, physical inactivity, and overweight/obesity are estimated for the Canadian province of Manitoba. Manitoba has a population of about 1.2 million.Endnote 31 Although the province is marked by a strong agriculture and resource-based economy, some 60% of Manitobans reside in Winnipeg, the provincial capital. There is also a large First Nations presence in Manitoba (about 11% of the provincial population).Endnote 32
Methods
We used an approach based on PAF to estimate the economic burden associated with the various RFs. At its simplest, the PAF statistic refers to the proportion of disease incidence generated in a population by a particular RF.Endnote 33 The results we report in this paper required calculating a Manitoba-specific PAF for each of the diseases related to the RFs of interest and then combining that information with the estimates of Manitoba-specific costs associated with both disease treatment and the indirect impacts of mortality/morbidity.
PAF is a statistic that combines two facets of an RF and its impact on disease: relative risk (RR) of the RF in reference to a particular disease, and the prevalence of exposure to the RF in the population of interest.
Relative risk
The source for the RRs associated with physical inactivity is the meta-analyses by Katzmarzyk and Janssen.Endnote 16 The majority of the studies incorporated in the Katzmarzyk and JanssenEndnote 16 review include an index of obesity in the analysis so that the effects of physical activity on disease risk can be considered to be independent of obesity. The source for the RRs associated with overweight and obesity is the meta-analyses by Guh et al.Endnote 34 The authors did not include physical inactivity as a potentially confounding RF as ''physical inactivity is often poorly reported and requiring its inclusion would have reduced the number of included studies.''Endnote 34, p15
We consulted two sources to assemble RRs for diseases attributable to tobacco smoking. A 2008 paper by Gandini et al.Endnote 35 offers a detailed meta-analysis specific to smoking-related cancers, including RRs adjusted for known confounding factors (esophageal and upper digestive tract cancers for alcohol consumption, stomach cancer for diet, liver cancer for infection with hepatitis B or C, cervical cancer for infection with the human papillomavirus and kidney cancer for body mass index).Endnote 35 Note that tobacco smoking is no longer a significant RF for liver or cervical cancers after these adjustments. The RR of cardiovascular and respiratory diseases were taken from a publication by Thun et al.Endnote 36 Thun et al.Endnote 36 adjusted all RRs for age, race, education, marital status, employment, consumption of vegetables and fruits, aspirin use, alcohol consumption, body mass index (BMI), physical activity and consumption of fatty foods. In addition, the RR for pneumonia, influenza, bronchitis and emphysema were adjusted for occupational asbestos exposure.
Most sources, with the exception of those dealing with physical inactivity, offered RR data by sex. An additional review of research for sex variations associated with physical inactivity supported the assumption that there is no significant difference in RR between males and females for this RF.Endnote 37, Endnote 38, Endnote 39
The point estimates of the RRs are used for calculations in the base model with the upper and lower bounds of the 95% confidence intervals (CIs) assessed in a sensitivity analysis.
Risk factor exposure
The other half of a PAF calculation depends on high-quality RF prevalence data.Endnote 40 The analysis of Manitoba's population exposure to tobacco smoking, physical inactivity and overweight/obesity began with information drawn from the 2008 Canadian Community Health Survey (CCHS). Tobacco smoking included all ''current smokers'' (daily and occasional smokers); overweight and obesity included individuals with a calculated BMI of between 25 kg/m2 and 30 kg/m2 for overweight and of 30 kg/m2 and greater for obesity (based on self-reported height and weight); and physical inactivity included individuals categorized in the CCHS as ''inactive.''
We made several adjustments to the base CCHS data to address acknowledged weaknesses. First, we used data from the Manitoba Youth Health Survey (MYHS) to adjust for youth smoking and physical inactivity.Endnote 41 Data from the CCHS suggested that about 10% of Manitoba youth aged 12 to 19 years were current smokers in 2008 versus 21.2% of youth in Grades 6 to 12 in the MYHS. On the other hand, the prevalence of physically inactive youth was reduced from 32% (in CCHS) to 19.3% (in MYHS).
Second, we estimated rates of physical inactivity for children aged under 12 years based on rates in the MYHS (16.4% for males and 22.1% in females). Rates of overweight and obesity for children and youth aged under 18 years were estimated based on Manitoba-specific CCHS rates for ages 20 to 34 years (34.5%/36.6% overweight in males/females andEndnote 4215.6%/14.7% obesity in males/females). While CCHS provides an estimate of overweight and obesity combined for ages 12 to 19 years, the results have a high coefficient of variation and are to be used with caution.Endnote 42 Furthermore, obesity-related behaviours including physical (in)activity and diet tend to track from childhood into adulthood.Endnote 43
Third, the CCHS does not include individuals living on First Nation reserves, whichEndnote 44 represents about 55 000 Manitobans. We used results from the 2002/03 Manitoba First Nations Regional Health Survey to identify and then adjust for the high prevalence of smoking (62%) and overweight/obesity (75%) among adults aged 18 years and over in the on-reserve population.Endnote 45
A final adjustmentEndnote 18 was guided by the work of Anis et al., who used the prevalence of waist circumference rather than BMI for specific disease categories including ischemic heart disease, hypertension, type 2 diabetes and gallbladder disease.
Multiple exposure levels
The most basic version of a PAF calculation, derived from the prevalence of a single RF and the RR of a related disease, uses the formula (E(RR21)) / (E(RR21)+ 1), where E is the proportion of the population exposed to the factor of interest and RR is the relative risk of disease developing in the group exposed to the factor.
However, more sophisticated approaches are required to calculate PAF when a polytomous RF is involved, that is, one that is made up of many parts. This is the case for overweight and obesity. These two biological categories lie on a continuum. As such, it is not algebraically accurate to calculate basic PAFs for each of overweight and obesity, and then simply sum the two figures to derive an overall PAF for exposure to excess weight. Instead, overweight and obesity should be conceived as a trichotomous exposure to excess body weight; that is, three categories of exposure are involved:
- no excess weight,
- intermediate excess, or overweight (prevalence EOW),
- more extreme excess, or obesity (prevalence EOB).
The PAF calculation is as follows:Endnote 46
EOW(RROW–1)+EOB(RROB–1)/EOW(RROW–1)+EOB(RROB–1)+1
Multiple risk factors
When complete information is known about both the exposure to multiple RFs (i.e. smoking and overweight/obesity in the same individual) and about the RR related to each set of causes, then it is straightforward to calculate the PAF for a combined system. However, when information on the RF overlap is lacking, as is often the case, it is once again important to avoid simply adding the basic PAFs for each RF in order to obtain a combined PAF for the multifactorial system. A more accurate approximation of PAF of the system is obtained using the equationEndnote 47
1–[(1–PAF1)(1–PAF2)(1–PAF3)]
where the notation PAF1 stands for the PAF related to the first RF, and so on.
This equation is most accurate when two conditions apply:
- the RFs involved are statistically independent (i.e. experiencing one makes an individual no more or less likely to experience the other, or the clustering of RFs is limited), and
- their joint effects are multiplicative (i.e. synergistic).
These two conditions can be shown to apply very well to a system involving obesity and smoking,Endnote 48, Endnote 49 and reasonably well to obesity and physical inactivity.Endnote 50, Endnote 51 Equivalent investigations of smoking combined with inactivity are scarce.
This adjustment equation can be extended to additional RFs. It can also be applied to aspects of disease development beyond basic incidence, including rates of mortality, disability, etc. In this analysis, we used the adjustment equation to generate a more accurate PAF of the direct costs of disease.
Direct costs
We estimated the economic burden (direct and indirect costs) associated with the RFs in Manitoba using a prevalence-based cost-of-illness approachEndnote 52 and reported this in 2008 Canadian dollars.
We began calculating direct costs using the approach adopted by Anis et al.Endnote 18 In short, direct costs including hospital care, physician services, other health care professionals (but excluding dental services), drugs, health research, and ''other'' health care expenditures were extracted from the National Health Expenditure Database for Manitoba.Endnote 53 All costs, with the exception of hospital care, were allocated to each of the comorbidity categories based on weights published in the Economic Burden of Illness in Canada (EBIC) for 1998.Endnote 54 Hospital costs were allocated to each comorbidity based on the proportion of total patient bed-days (based on data from the Canadian Institute for Health Information Hospital Morbidity Database 2000/2001Endnote 55) used in treating patients in Manitoba with that comorbidity. Estimated total direct costs were distributed between males and females based on the proportion of hospital bed-days in 2000/2001 utilized by males and females for each of the comorbidities. Finally, the Manitoba sex-specific costs by comorbidity were multiplied by the calculated sex- and comorbidity-specific PAF.
Adjusting direct costs in a multifactorial system
We then applied the formula introduced earlier for calculating the combined PAF in a multifactorial system to the calculated crude direct costs attributable to each of tobacco smoking, overweight/obesity and physical inactivity. Crude direct costs for each RF were inserted into the adjustment formula (i.e. PAF1 = crude PAF of cost for tobacco smoking, etc.) in order to generate an adjusted PAF of direct costs for the multifactorial system. This approach reduced combined direct costs by 12.6% (from $560.8 to $490.3 million per year).
Having determined as accurately as possible the combined population impact of multiple RFs, it is still useful for the purposes of high-level prevention prioritization, public educational messages, etc., to have a sense of the approximate impact of a particular RF. Thus we applied a disaggregation step at the end of the direct costing process to notionally assign an economic burden to each RF. We did this by returning to the crude costs for each RF, dividing each of these figures by their sum (i.e. the crude total cost for the combined system) and thereby generating a ratio. This ratio was then applied to the adjusted total direct costs, yielding a disaggregated, adjusted economic burden by disease that is notionally attributable to each RF.
Indirect costs
We calculated indirect costs (premature mortality, short- and long-term disability) following the method used in EBIC, 1998 (a modified human-capital approach).Endnote 54
Specifically, the steps involved in estimating indirect costs were as follows:
- Six diagnostic categories within EBIC, 1998 were identified that cover the comorbidities/diseases of interest; the direct and indirect costs for these six categories were extracted.
- This information was used to determine a ratio between direct and indirect costs for each of the diagnostic categories, stratified by the specific category of indirect cost. For example, the indirect costs associated with cancer are 4.6 times (459%) higher than direct costs, largely driven by premature mortality. On the other hand, indirect costs associated with musculoskeletal diseases are 5.2 times (519%) higher than direct costs; in this instance, however, the majority of the higher costs are associated with long-term disability rather than premature death (see Table 1).
- The pertinent ratios (by diagnostic category and specific indirect cost category) were then applied to the previously identified direct costs attributable to each RF and adjusted for a multifactorial system in order to generate the equivalent indirect cost data.
Discussion
The analytic approach outlined in this document begins to address the issue of double-counting costs when estimating the aggregate economic burden of chronic illnesses associated with multiple RFs in one individual. Applied to the province of Manitoba, the approach suggests a reduction of 12.6% in the aggregate economic burden over the total that would be generated by crude summation of costs generated by each of the key RFs.
This analysis used an extension of the basic PAF formula to produce a more accurate result, including addressing both complications in assessing PAF when a polytomous RF is involved (i.e. overweight and obesity) and accounting for the possibility of multiple RFs in any given individual.
The analysis of the economic burden related to the RF system and (notionally) the individual RFs of smoking, physical inactivity and overweight/obesity is the first phase of any attempt to project the potential economic impact of applying known primary prevention initiatives.
Using the methods outlined in this paper, we estimated the total annual economic burden of the RFs in Manitoba in 2008 to be $1.6 billion ($490 million in direct costs and $1,114 million in indirect costs).
Another important result, generated by having access to sex-specific RF prevalence and RR data, was the difference between males and females in contributing to the total economic burden. The costs associated with tobacco smoking are higher in males, which is partly a reflection of the continuing higher prevalence of tobacco smoking among men. On the other hand, the economic burden associated with excess weight is higher in females, a result that appears to be anomalous since the prevalence of obesity and (especially) overweight is in fact higher in males. In addition to the burden in women that is specific to gynecological cancers, an explanation for the anomaly leans on the fact that the RR related to excess weight is higher in females for several costly conditions, including renal cancer, ischemic heart disease, hypertension and type 2 diabetes (see Table 2). The resulting overall sex-specific distribution for the burden of key modifiable RFs has important implications for prevention planning and public health messaging.
The current analysis also confirmed the emergence of overweight/obesity as a public health concern, a phenomenon that has also been noted in other jurisdictions.Endnote 56, Endnote 57 In fact, the estimated 2008 economic burden associated with excess weight in Manitoba ($747.2 million) is greater than that associated with tobacco use ($557.4 million). Even though the economic burden associated with smoking still exceeds that of obesity strictly defined, once the health effects of overweight are included, the area as a whole moves into the forefront. The United Kingdom project introduced earlier in this paper found similar results with direct costs due to overweight/obesity exceeding the total related to tobacco smoking (UK £5 billion vs. UK £3.3 billion) by a differential similar in proportion to that found in the current analysis for Manitoba.Endnote 26 However, the point at which overweight is associated with a significant increase in health effects is likely higher than a BMI of 25 kg/m2 in the North American population though it may also be lower in certain ethnic groups.Endnote 58
The quality of the results derived from a PAF analysis is inevitably limited by the quality of the inputs, specifically RR and prevalence data. The effect of any potential inaccuracies in this project was first mitigated by correcting known gaps in the RF exposure information obtained through routine Canadian population surveys. Variation in regional PAF estimates often reflects uncertainty in the degree of exposure to the RF being analyzed.Endnote 33 Thus, it is vital to refine prevalence information as much as possible.
A consistent dependence on meta-ana-lyses, which were adjusted for known confounding factors whenever possible, was used in estimating RRs. A sensitivity analysis using the 95% CI associated with each RR indicates the importance of using robust and accurate RR estimates.
Does a 12.6% adjustment (reduction) for overlapping RFs in certain individuals have face validity? Figure 2 summarizes the degree of potentially confounding RF overlaps in Canadians, based on CCHS data from 2000.Endnote 59 Summing across the pertinent sub-categories, 10.2% of the population is exposed both to smoking and overweight/obesity, 26.6% to overweight/obesity and physical inactivity and 14.0% to physical inactivity and smoking. While the overlap related to elevated BMI and physical inactivity is relatively high, the required correction (to avoid double-counting disease incidence) was, in fact, used here for RR data for physical inactivity adjusted for overweight/obesity.Endnote 16 When compared to the proportions of the population with multiple RF exposures, the 12.6% adjustment to the Manitoba economic burden appears to have face validity.