Introduction
Hypertension is a major public health concern: it is a risk factor for cardiovascular disease (CVD), kidney failure and mortality, and one of the most important in terms of disability-adjusted life years.Endnote 1, Endnote 2, Endnote 3 Kearney et al.Endnote 4 estimated the global prevalence of hypertension--generally defined as a systolic blood pressure equal to or above 140 mmHg and/or diastolic blood pressure equal to or above 90 mmHg--to be 26% in the adult population in 2000, and projected a 24% increase in developed countries and an 80% increase in developing countries by 2025. In contrast, Danaei et al.Endnote 5 found the average systolic blood pressure to be decreasing in both sexes worldwide between 1980 and 2008, with the prevalence of age-adjusted hypertension dropping from 33% to 29% for men and from 29% to 25% for women. This trend varies depending on the country and region, however. In addition, despite this downward trend, the absolute number of people with hypertension has increased as a result of the global population growth and aging. According to an Ontario study, 21% of the population aged 20 to 79 years had hypertension in 2006,Endnote 6 whereas the 2007--2009 Canadian Health Measures SurveyEndnote 7 found that 19% of Canadians aged between 20 and 79 had hypertension and 20% had a blood pressure in the prehypertension range. The prevalence of hypertension remains lower in Canada than in the United States (29%) and England (30%).Endnote 8
The Institut national de la santé publique du Québec (INSPQ)Endnote 9, Endnote 10 found that the adjusted prevalence of hypertension in Quebec rose from 15.8% in 2000 to 20.3% in 2007, with the prevalence changing faster for men than for women. At the same time, the adjusted incidence of hypertension fell for both sexes. The mortality rates for people with hypertension also decreased between 2000 and 2007 for both sexes, maybe because of better drug treatments.Endnote 9, Endnote 10 A recent studyEndnote 11 in 17 countries found the prevalence of hypertension to be nearly 40% in people between the ages of 35 and 70 years, with the definition of hypertension based on the self-reported use of an antihypertensive or on an average blood pressure of at least 140/90 mmHg (2 measurements). Less than half (46.5%) of the participants in this study were aware of their condition, and only one-third (32.5%) of those receiving treatment had controlled blood pressure.
According to the World Health Organization,Endnote 12 many factors or health determinants combine to affect the health of individuals. There are 3 types of health determinants: those that relate to people's individual characteristics (e.g. age, sex, comorbidities); those that relate to the social and physical characteristics of their areas of residence (e.g. neighbourhood socioeconomic status and rurality); and those that relate to the characteristics of the health care system and care practices.Endnote 13, Endnote 14, Endnote 15, Endnote 16 Neighbourhood characteristics can affect those behaviours, including eating habits and physical activity,Endnote 17 that affect health.Endnote 18 Other factors likely to have an impact on health are the quality and availability of affordable housing,Endnote 19 poverty,Endnote 20 safetyEndnote 21 and the sense of cohesion as a result of living in a well-organized and socially connected neighbourhood.Endnote 22
The link between neighbourhood characteristics (socioeconomic status or rurality) and the prevalence and incidence of hypertension has been previously studied. In their 2013 study, Chow et al.Endnote 11 found that study participants who lived in urban communities in low-income countries were more aware of and treated and controlled their hypertension better than did the participants in rural communities. However, the awareness, treatment and control were similar for rural and urban residents in higher-income countries. In addition, blood pressure control was more frequent in high-income countries (40.7%).Endnote 11 Lee et al.Endnote 23 found a gradient between the prevalence of hypertension and income, whereas Aubé-Maurice et al.Endnote 24 showed that the incidence of hypertension was associated with the neighbourhood material and social deprivation, although this association differed depending on the case identification algorithm.
In short, the association between deprivation-of an individual, area or country-and health indicators such as prevalence and incidence of hypertension are well documented. However, there are few studies on how neighbourhood characteristics affect mortality, morbidity, use of health services and prescription-drug treatment for a population diagnosed with hypertension in primary prevention for CVD. In addition, as a number of current studies do not have the statistical power to adequately evaluate vulnerable populations,Endnote 25 we set out to determine:
- if there is a higher risk of mortality and morbidity in this vulnerable population in deprived areas;
- who are the most frequent users of primary and secondary medical services;
- if people living in deprived areas receive treatment for their hypertension less often than those living in less deprived areas; and
- whether differences exist between urban and small town or rural areas.
Our objectives were to describe and compare the prevalence of hypertension in the primary prevention of CVD in 2006-2007 in the Quebec population, according to the level of material and social deprivation of the area of residence, as well as their mortality, morbidity, use of medical services and prescription drug treatment. Because the material and social deprivation of the area generally differs depending on the living environment (urban or rural), comparisons were made both globally and by rurality.
Methods
Data sources
We conducted a secondary analysis of medical and administrative data from the list of beneficiaries, the medical services register and the Fichier des hospitalisations Med-Écho of the Quebec health insurance board, the Régie de l'assurance maladie du Québec (RAMQ).Endnote 26 The latter lists each patient's diagnoses, hospital admission and discharge dates, and treatment details.Endnote 27 The medical services register contains the attending physician's encrypted number, the procedure(s) performed, the diagnosis and the date the service was given. The list of beneficiaries includes patient's sex, date of birth and the geographical location of the place of residence (postal code). The Institut de la statistique du Québec death file lists the date and cause of death for all deaths that occurred in Quebec. Other data were provided by the RAMQ through the health care professionals' file (physician's encrypted number and medical specialty), the public prescription drug insurance plan eligibility file (participation start and end dates) and the file on drug services billed by pharmacists to the RAMQ (which contains all the drug reimbursement claims made by people covered by the public plan, with the drug code, the claim date and the length of treatment).
RAMQ covered the costs of medications for about 41% of the Quebec population in 2006 (i.e. seniors aged 65 years or older, welfare recipients, and everyone not covered by a private prescription-drug insurance plan). Dissemination areasFootnote * (DA) were associated with each patient's area of residence based on their postal code.Endnote 28 Data on material and social deprivation indices were provided by the INSPQ.Endnote 29 DA classification as part of a urban, small town or rural area was based on Statistics Canada data.Endnote 28 Data on DA population counts by age and sex were based on the 2006 Census and were provided by Statistics Canada.Endnote 30
This project was approved by the Université de Sherbrooke ethics boards and Quebec's information access commission, the Commission d'accès à l'information.
Population
The study cohort is made up of all the residents of Quebec aged 30 years or older who, between January 2006 and December 2007, had been hospitalized with a primary or secondary diagnosis of hypertension (ICD-9 401 or ICD-10 I10) or used at least 3 medical services with a hypertension diagnosis in 365 days of the study period. Although other algorithms have been validatedEndnote 31 and have both good sensitivity and good specificity, we did not use them because they involved data from the medical records and prescription-drug files to which we did not have access for all patients. The case definition algorithm for hypertension most similar to ours was validated by Lix et al.Endnote 32 for Manitoba data (1 hospitalization or 2 services in 1 year) with a sensitivity of 51% and a specificity of 97%.
To keep only primary prevention of CVD patients in the cohort, we excluded cases with the following CVD diagnoses in the 4 years preceding the reference date (the first date with a hypertension diagnosis in the study period): ischemic heart disease (ICD-9 410-414 or ICD-10 I20-I25), heart failure (ICD-9 428 or ICD-10 I50) or a cerebrovascular disease (ICD-9 430-438 or ICD-10 I60-I69). Also excluded were all patients who had been seen by a doctor or hospitalized for pregnancy (ICD-9 630-676 and 760-779 or ICD-10 O00-O99 and Z32-Z39) in the 5 months following the reference date.Endnote 33 Finally, also excluded were patients for whom no DA could be defined or no information on the size of the population of their DA was available, as well as those in a DA for which the material and social deprivation value was unknown.
Variables
The first variable examined was the prevalence of hypertension in CVD primary prevention in relation to material and social deprivation. For each sociogeographical unit selected, the prevalence numerator is the size of the study cohort and the prevalence denominator is the population of Quebec aged 30 years or older.
We also calculated the incidence of allcause mortality and that of a given cardiovascular event-CVD mortality or hospitalization for a CVD (ICD-9: 410-414, 428 and 430-438; ICD-10: I20-I25, I50 and I60-I69)-for the entire cohort over the 2 years after the reference date. For the other dependent variables, the incidences were calculated based on number of people who survived the two-year period following the reference date. These other dependent variables are all-cause hospitalization; outpatient consultation (for any health problem) with a general practitioner, internist, cardiologist, endocrinologist or nephrologist; an emergency department visit; frequent outpatient medical consultations, regardless of specialty (42 services or more); frequent outpatient visits to a general practitioner (22 services or more); frequent outpatient visits to specialists (4 services or more) or frequent emergency department visits (4 services or more). To better take into account the Quebec context, the thresholds used to define frequent use were based on the population quartiles from a population with hypertension, diabetes or dyslipidemia diagnosed between 2006 and 2007 in Quebec. (Research information available on request.) For example, 25% (top quartile) of the patients in this population had received at least 22 services from a general practitioner. Patients who used health services above these thresholds were considered frequent users. Naessens et al.Endnote 34 chose to use a threshold of 10 consultations or more per year (with a total of 20 over 2 years) to identify frequent users of primary care. Measuring the proportion of these frequent users of health care is important because the use of care and the associated cost can be attributed to a relatively small fraction of the population. For example, in the United States, 5% of the population accounts for about 50% of all health costs.Endnote 35
Finally, for the drug-related dependent variables, we calculated the proportion of prescription-drug users among the people eligible for the provincial drug insurance plan who survived the two-year period following the reference date. These variables are use of an antihypertensive, defined globally and by antihypertensive class (angiotensin-converting enzyme inhibitor, angiotensin II receptor antagonist, diuretic, beta blocker, calcium channel blocker, other). Patients are considered to have used a drug in a specific class if they presented at least one prescription in that class at the pharmacy within 2 years following the reference date.
To determine the rurality of a neighbourhood, we used the Statistical Area Classification developed by Statistics Canada.Endnote 37 Basic Statistical Area Classification units are municipalities. Each municipality belongs to a census metropolitan area (at least 100 000 inhabitants), a census agglomeration or small town (between 10 000 and 99 999 inhabitants), or a rural area or strong-to-noinfluence metropolitan-influenced zone (if themunicipality is not classified elsewhere). On the recommendation of Statistics Canada,Endnote 37 for the purpose of this analysis we grouped the small towns and rural areas into a single category, "non-metropolitan areas."
For level of deprivation, the INSPQ has developed a deprivation index using 6 socioeconomic indicators calculated at the DA level.Endnote 38, Endnote 39, Endnote 40, Endnote 41, Endnote 42 The material component of the index takes into account the proportion of people without a high school diploma, the employment-to-population ratio and the average income, while the social component was calculated using the proportion of people living alone, the proportion of separated, divorced or widowed people, and the proportion of lone-parent families. DAs are classified by quintiles (i.e. 20% of the population), with Quintile 1 (Q1) the most advantaged and Quintile 5 (Q5) the most deprived. These categorizations were conducted separately for the material and social components, and were then combined, resulting in the 25 neighbourhood deprivation classes (Q1 x Q1 to Q5 x Q5).
Statistical analyses
The analyses were done for the entire cohort and were stratified by type of neighbourhood (metropolitan and nonmetropolitan areas). To determine whether the differences in health indicators between metropolitan and non-metropolitan areas were statistically significant, we used the chi-square test. Given the size of the study cohort (N = 276 793), minimal differences could prove statistically significant. Therefore, we also used the concept of clinical significance, where a variation of ±10% or more in the health indicators is considered clinically significant. For each dependent variable studied, the proportions were adjusted for age and sex. We measured the variability of the health indicators according to deprivation using a coefficient of variation (CV), which represents the ratio of the standard deviation to the mean. To compare the adjusted proportion of the class of interest (one of the 25 classes of neighbourhood material and social deprivation) and the proportion observed in the least materially and socially deprived class (Q1 x Q1), we calculated the relative risk (RR), which indicates the percentage increase or decrease in risk in relation to this class (Q1 x Q1) and with which we associated a confidence interval (CI).
Results
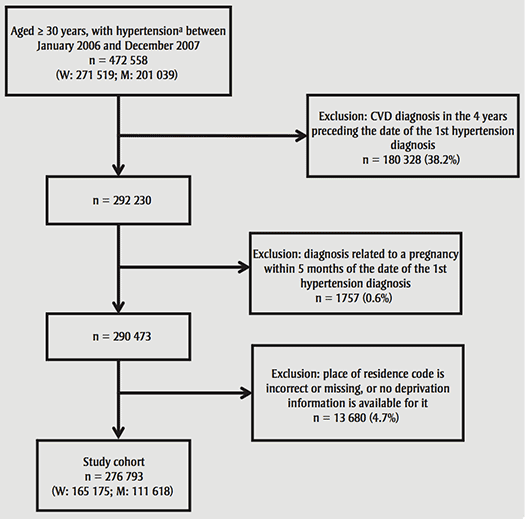
A total of 472 558 people aged 30 years or older met our inclusion criteria for the study period (1 January, 2006, to 31 December, 2007) (Figure 1). Of these, 180 328 (38.2%) had been diagnosed with CVD in the 4 years prior to the reference date or had possible pregnancy-related hypertension (n = 1757) and were excluded. Also excluded were 13 680 people for whom the place of residence was invalid or missing or who lived in DAs for which no socioeconomic information was available. The final cohort included 276 793 people.
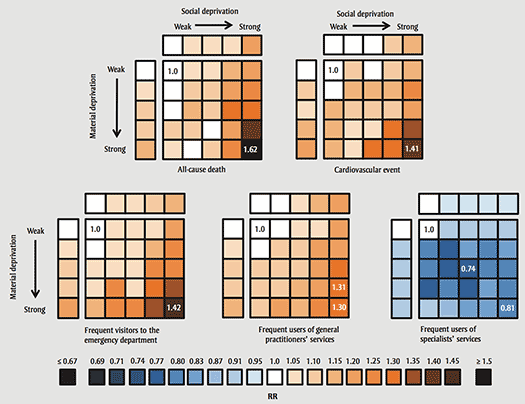
Compared with patients living in materially and socially advantaged areas (Q1 x Q1), patients living in the most materially and socially deprived areas (Q5 x Q5) were at a 58% higher risk of dying (RR = 1.58, 95% CI: 1.41-1.77), 46% higher risk of a cardiovascular event (RR = 1.46, 95% CI: 1.29-1.65), 47% more at risk of being frequent emergency department visitors (RR = 1.47, 95% CI: 1.40-1.55), and 31% more at risk of being frequent users of a general practitioner's services (RR = 1.31, 95% CI: 1.25-1.38) (Table 3). However, those patients living in the most materially and socially deprived areas had 25% less chance of being frequent users of medical specialists' services (RR = 0.75, 95% CI: 0.71-0.79).
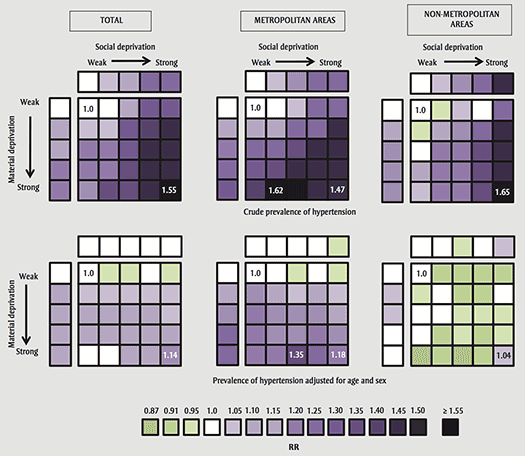
Figure 2 shows the variations observed in the prevalence of hypertension in primary prevention of CVD according to material and social deprivation. This graph helps visualize variations that relate to an area's material deprivation and those that relate to its social deprivation, notably a significant gradient in prevalences toward the most deprived areas. Once adjusted for age and sex, however, the distribution by area type is much more uniform, although the gradient persists in the metropolitan areas.
Figures 3 to 5 show the variations for a selection of health indicators with a relatively high CV (Table 2), overall (Figure 3) and by rurality (Figures 4 and 5). The indicators adjusted for age and sex that present a significant general gradient from the least deprived areas to the most deprived areas (Figure 3) are the proportion of deaths, the proportion of cardiovascular events and the proportion of frequent users of outpatient services (general practitioner, emergency). The relationship is inverse for the adjusted proportion of frequent users of medical specialists' services, as people living in the most advantaged areas use specialists' services more frequently. The 2 types of deprivation seem to play an equivalent role for some indicators (proportion of deaths, proportion of frequent users of general practitioners' services), while for other indicators (proportion of cardiovascular events, proportion of frequent emergency department visitors or frequent users of specialists' services) material deprivation predominates.
The gradients observed in the metropolitan areas (Figure 4) are similar to those seen overall (Figure 3), probably because these areas account for two-thirds of the cohort studied. The analyses stratified according to rurality reveal larger variations in the non-metropolitan areas (Figure 5) than in the metropolitan areas (Figure 4). These variations are not surprising because samples are smaller in these areas, resulting in a larger variance in the estimation of proportions. Overall, however, for most of the variables studied, the results are consistent, except perhaps for mortality and cardiovascular events, where greater instability in the estimates is observed.
Discussion
This study shows significant variations for a number of health indicators, depending on the area's material and social deprivation. Even after adjusting for age and sex, the risk of death was higher by 58%, the risk of a cardiovascular event higher by 46%, the risk of hospitalization (all causes) higher by 18% and the prevalence of hypertension higher by 14% for people living in the most materially and socially deprived areas (Q5 x Q5) than for people living in the least materially and socially deprived areas (Q1 x Q1). In addition, the adjusted proportion of frequent users of primary care services was much larger in the more deprived areas, with 47% more frequent emergency department visitors and 31% more frequent users of general practitioners' services. Previous studies have shown that people with a lower socioeconomic status make greater use of outpatient medical services, including emergency department services.Endnote 43 In our study, the patients in the most deprived areas not only visited emergency departments more frequently, confirming the results of another Canadian study,Endnote 44 but also consulted general practitioners more frequently. We also saw that the proportion of frequent users of specialty services was larger in the most advantaged areas. These variations were also present in the analyses stratified by metropolitan and non-metropolitan area. The lack of variation (or the small variation) seen in the use of antihypertensives may point to the favourable impact of the provincial policy of universal access to drugs.
In short, a large proportion of patients with hypertension who have no history of CVD and live in materially and socially deprived areas experience more serious consequences than those living in advantaged areas, even though they receive equivalent pharmacotherapy.
In our study, the prevalence of hypertension in CVD primary prevention is estimated at 5.9% over the 2 years studied (2006-2007). Our estimate is much lower than the prevalence of hypertension calculated by the INSPQEndnote10 for the same period (20.3%) or the prevalence estimated by Lix et al.Endnote 32 for 2002-2003 (10.0%). However, the populations studied differed: we included only patients with hypertension without a history of CVD, thus reducing the cohort by nearly 38% (Figure 1). In addition, we used just one diagnostic code (ICD-9: 401 and ICD- 10: I10) in our study to identify hypertension cases, as did Lix et al.,Endnote 32 while the INSPQ expanded the hypertension codes to include those related to other pathologies (heart disease, renal disease, hypertensive heart and renal disease, and secondary hypertension [ICD-9: 402-405 and ICD-10: I11-I13 and I15]). Finally, the algorithm we used to identify hypertension cases (3 diagnoses in 1 year or 1 hospitalization) was more specific than those used by the INSPQ (2 diagnoses in 2 years or 1 hospitalization) and by Lix et al.Endnote 32 (2 diagnoses in 1 year or 1 hospitalization).
We should also point out that 60% of the cohort were women. Women use health services more frequently than do menEndnote 45, Endnote 46, Endnote 47 and are therefore more likely to be diagnosed with hypertension and to be detected by our selection algorithm. In addition, we excluded all patients who had been diagnosed with CVD, which occurs in men more frequently than in women.Endnote 48, Endnote 49
The gradient in the rates of prevalence of hypertension in primary prevention of CVD according to the neighbourhood level of deprivation is evident and reflects, in good part, a real difference in the age and sex distribution in those areas (Figure 2). This is illustrated by a significant decrease in the gradient between the adjusted and unadjusted results. However, our results for prevalence differ from those published by the INSPQ, where there was a gradient in the hypertension incidence rates from the least materially deprived to the most materially deprived for women only, with an inverse gradient for social deprivation for both sexes.Endnote 50
Many studies have looked at the link between deprivation and certain health indicators. The health indicators related specifically to hypertension include incidence,Endnote 10prevalence,Endnote 51, Endnote 52, Endnote 53 treatmentsEndnote 54 and hypertension care appropriateness.Endnote 55 Hammouche et al.Endnote 55 proved that study participants with hypertension living in deprived areas in the United Kingdom received care that was at least as good, if not better, than did those living in advantaged areas. The absence of a link between deprivation and the use of antihypertensives in our study is consistent with the results of Hammouche et al.Endnote 55 but not with those of Pears et al.Endnote 54 in Scotland. This absence of a correlation between the use of certain drugs and deprivation was also observed for a cohort of patients with schizophrenia who took antipsychotic drugs,Endnote 56 and this may point to the effectiveness of the provincial policy of universal access to drugs.
Strengths and limitations
The greatest strength of our study is that we analysed the entire population of Quebec with a hypertension diagnosis but no known CVD diagnosis. In addition, we compared a large range of health indicators according to 25 area types, ranging from the most materially and socially advantaged to the most materially and socially deprived. However, this study has a number of limitations. First, as we said earlier, the algorithm used is very specific, but not very sensitive, with the result that actual prevalence is underestimated. Nevertheless, we believe that this inclusion bias makes the analyses more robust with regard to the other health indicators because our cohort has very few false positives. In addition, a large number of people with hypertension are not diagnosed Endnote 11 and are therefore not taken into account in our cohort; this is also the case for patients who saw only doctors who work on an hourly rate-for example, in a local community service centre. In 2006-2007, as many as 12% of general practitioners worked in a local community service centre.Endnote 57
Second, because the results for drugs relate to only 70% of the cohort we studied (183 156 patients out of 276 793 covered by the provincial drug insurance plan), our results should not be generalized to the overall population with hypertension (selection bias). Further, people aged under 65 years who are socioeconomically deprived are overrepresented in this subpopulation. For this age category, the RAMQ covers all social assistance recipients and all people not covered by a private drug insurance plan.
Conclusion
This study demonstrates the existence of significant variations for a number of health indicators among patients with hypertension in primary prevention of CVD according to their neighbourhood material and social deprivation. Some of the indicators, such as deaths from all causes and the incidence of cardiovascular events, can lead to a risk increase of up to 58% in the most deprived areas, compared with the least deprived, even though there is little or no variation in the use of antihypertensives and the patients in the most deprived areas seem to receive equally good primary care. In a context in which the burden of chronic disease is growing, such health inequalities have major public health implications. This study again shows the importance of taking socioeconomic status into account when planning interventions to prevent CVDs and their consequences. A better understanding of the processes underlying the social inequalities of health in relation to areas of residence is an essential area of public health research.
Acknowledgments
This project was funded by the Canadian Institutes of Health Research (CIHR). Alain Vanasse receives funding from the Department of Family Medicine and Emergency Medicine of the Université de Sherbrooke, the Centre de recherche CHUS and the Fonds de recherche du Québec-Santé (FRQS).
References