Original quantitative research – Determining the accuracy of the Canadian Hospitals Injury Reporting and Prevention Program for the representation of the rates of mild traumatic brain injuries in Quebec
Health Promotion and Chronic Disease Prevention in Canada
Glenn Keays, MPHAuthor reference 1Author reference 2; Debbie Friedman, BSc Pht, MMgmtAuthor reference 1Author reference 2Author reference 3; Isabelle Gagnon, PT, PhDAuthor reference 3Author reference 4; Marianne Beaudin, MD, MSc, MPH, FRCSCAuthor reference 5
https://doi.org/10.24095/hpcdp.39.11.01
This article has been peer reviewed.
Author references:
- Author reference 1
-
Canadian Hospitals Injury Reporting and Prevention Program (CHIRPP), The Montreal Children's Hospital, McGill University Health Centre, Montréal, Quebec, Canada
- Author reference 2
-
Montreal Children's Hospital Trauma Centre, McGill University Health Centre, Montréal, Quebec, Canada
- Author reference 3
-
Department of Pediatrics & Pediatric Surgery, Faculty of Medicine, McGill University, Montréal, Quebec, Canada
- Author reference 4
-
School of Physical and Occupational Therapy, Faculty of Medicine, McGill University, Montréal, Quebec, Canada
- Author reference 5
-
Centre hospitalier universitaire mère-enfant Sainte-Justine, Montréal, Quebec, Canada
Correspondence: Glenn Keays, Trauma Department, The Montreal Children's Hospital, McGill Health Centre, 1001 Boulevard Décarie, Room B.S1.2766.2, Montréal, QC H4A 3J1; Tel: 514-412-4400 ext. 23167; Email: Glenn.Keays@muhc.mcgill.ca
Abstract
Introduction: The recent rise in mild traumatic brain injuries (mTBI) in the pediatric population has been documented by many studies in Canada and the United States. The objective of our study was to compare mTBI rates from the Canadian Hospital Injury Reporting and Prevention Program (CHIRPP) in Montréal with population-based rates (Quebec mTBI rates).
Methods: We calculated CHIRPP's mTBI rates via two methods: (1) using all CHIRPP injuries as the denominator; and (2) using the number of children aged 0 to 17 years living within 5 km of either of two CHIRPP centres in Montréal as the denominator. We plotted CHIRPP's mTBI rates against the provincial rates and compared them according to sex and age.
Results: Whether using all CHIRPP injuries or the number of children aged 0 to 17 years living within 5 km of either CHIRPP centre in Montreal as the denominator, CHIRPP paralleled the fluctuations seen in Quebec's rates between 2003 and 2016. When stratifying by sex and age, CHIRPP was better at estimating the population-based rates for the youngest (0 to 4 years) and the oldest (13 to 17 years) age groups.
Conclusion: CHIRPP in Montréal proved a valid tool for estimating the variations in rates of mTBI in the population. This suggests that CHIRPP could also be used to estimate population-based rates of other types of injuries.
Keywords: mild traumatic brain injury, epidemiology, children, adolescents, emergency primary care, surveillance, evaluation, Quebec
Highlights
- The four distinct fluctuations in Quebec's mTBI rates (i.e. a sudden increase in 2009, then a drop, followed by a steady increase between 2010 and 2014 and another drop in 2015) were captured by CHIRPP Montréal.
- When compared with other studies of mTBI rates, CHIRPP Montréal reported similar results according to the years and age groups these studies used.
- CHIRPP proved to be particularly accurate in estimating the fluctuations in Quebec's mTBI rates in males aged 0 to 4 years.
- The average rates of mTBI between CHIRPP and Quebec were quite similar: 106.3 per 10 000 in CHIRPP and 98.2 per 10 000 for Quebec, when adjusting the provincial rates to compensate for repeat visits for the same mTBI.
Introduction
The collection of information on traumatic injuries for the purpose of creating a computerized database dates back to 1969, at the Cook County Hospital in Chicago, Illinois.Footnote 1 In Canada, before the 1990s, trauma databases only included the most severe injuries—those that caused mortality or required hospitalization. The Canadian Hospitals Injury Reporting and Prevention Program (CHIRPP) was created in August 1990 to provide a broader understanding of injuries, especially those occurring in the child population (under age 18 years), by gathering data about emergency room visits from 10 pediatric hospitals. As of 2018, CHIRPP has collected data from over 3.5 million injuries. It has been expanded to gather data from 19 hospitals: 11 pediatric and 8 general.Footnote 2
One of CHIRPP's limitations is that it is not population-based, and only represents a sample of the injuries in Canada.Footnote 3Footnote 4Footnote 5Footnote 6 Yet, some have argued that CHIRPP data can be a useful tool in describing the injuries of the population. Kang et al.Footnote 7 and Pickett et al.Footnote 3 have hinted at the representativeness of CHIRPP for specific injuries, such as those related to sports and recreational activities. Macpherson et al.,Footnote 8 who compared the injuries captured by a CHIRPP centre in Ottawa with those seen in four other emergency departments in Ottawa, found that CHIRPP was better at capturing the injuries of younger children (< age 15 years) and those whose injuries required hospitalization. Keays et al.Footnote 9 found that the Canadian rates of injuries in youth football, calculated using CHIRPP data, mirrored those reported in the United States over a period of 20 years using data from the National Electronic Injury Surveillance System (NEISS).
The representativeness of CHIRPP regarding mild traumatic brain injuries (mTBI) has never been studied; we wanted to see if CHIRPP captured the increase of mTBI in recent years that has been reported by several studies. Footnote 10Footnote 11Footnote 12Footnote 13Footnote 14Footnote 15 We also wanted to take advantage of a recently published articleFootnote 16 that estimated population-based mTBI rates in Quebec's children and see if variations in rates of mTBI in CHIRPP would mirror those of the population.
The specific goal of the present paper was to assess the representativeness of mTBI-related CHIRPP data from two provincially designated pediatric trauma centres in Montréal (The Montréal Children's Hospital at McGill University Health Centre, and Centre hospitalier universitaire mère-enfant Sainte-Justine [CHU Sainte-Justine]) by comparing it to population-based mTBI rates. Our hypothesis was that the fluctuations in yearly provincial mTBI rates in the child population demonstrated by Keays et al.Footnote 16 would also be captured by CHIRPP.
Methods
This study compared retrospective cohort data (CHIRPP) with population-based data from the Régie de l'assurance maladie du Québec (RAMQ).Footnote 16 As per CHIRPP protocol, patients or parents of patients who presented to the emergency department (ED) of either of the CHIRPP centres in Montréal for an injury were asked to fill out a one-page questionnaire and provide detailed information about the injury. In addition, clinical data such as nature of the injury, body part and type of treatment were extracted from the ED record by CHIRPP coordinators at each site. For cases for which there was no CHIRPP form filled out, information was extracted from the patients' medical records by the coordinator. In order to ensure full confidentiality, the patients' hospital medical record numbers were scrambled, and the day in their date of birth was rounded to 15 or 31 (depending on the day of the month of the actual birthday) prior to submission to the central CHIRPP data centre. In Montréal, both CHIRPP pediatric trauma centres capture over 97% of all ED injury-related visits at their site.
Because CHIRPP data are ED-based, we do not know with certainty how to determine the exact denominator for the population that presents to each site, as children with an mTBI can consult several other hospitals, not to mention private clinics, and thus not be recorded in CHIRPP. We thus opted to estimate the denominator for CHIRPP using two different methods. First, we chose the total number of CHIRPP-reported injuries in both hospitals, as this was thought to be the simplest method, considering that CHIRPP data are current and easy to access. Our second estimate was constructed using the total population of children under 18 years of age living within a 5 km radius of either hospital. The justification for this radius was that, since Montréal is an island, going further than 5 km north or south would have captured patients that have to cross a bridge to get to either hospital and patients from the South Shore and North Shore (suburbs located off of the island) are much more likely to consult the closest hospital. While there is no perfect way to estimate the best distance to use, one that would guarantee that all children living within this radius would visit one of the hospitals when injured, we are confident that a 5 km radius captured those most likely to come.
We structured the current study according to the same age groups and time period reported for the population-based mTBI rates in the province of Quebec,Footnote 16 where total numbers of medical services (billing information) for "concussion" (ICD-9 code 850.00) and "intracranial injury of other and unspecified nature without mention of open intracranial wound, unspecified state of consciousness" (ICD-9 code 854.00) were reported by year (2003–2016), and further broken down by age groups (0–4 years, 5–8 years, 9–12 years and 13–17 years) and sex. In CHIRPP, two codes are used for mTBI: 41, corresponding to ICD-9 code 854.00, and 42, corresponding to ICD-9 code 850.00.
For the first estimated denominator (all CHIRPP injuries), we calculated mTBI rates according to the sex and age of the patient. As an example, the rates of mTBI in females aged 13 to 17 years in 2003 were calculated using the number of mTBI for that year divided by the total number of injuries in females aged 13 to 17 years in CHIRPP in 2003.
For our second denominator, we set out to determine the population (by sex and age) of children living within 5 km of either hospital. We used Google Maps to determine the postal codes (the first three digits only) within a 5 km radius of either of the CHIRPP centres. Once we determined which postal codes to use, we obtained the population living in the area using data from Statistics Canada censusesFootnote 17 from 2001, 2006, 2011 and 2016, which break down the population by age and sex for each postal code (first three digits). For years for which there were no data, the average increase, or decrease, was evenly distributed between census years. We calculated the mTBI rates for each year as follows: number of mTBI cases in CHIRPP in patients living within 5 km of either hospital divided by the population living within 5 km of either hospital. As an example, the rates of mTBI in females aged 13 to 17 years in 2003 were calculated using the total number of mTBI in CHIRPP in 2003 for females aged 13 to 17 years who lived within 5 km, divided by the number of females aged 13 to 17 years who lived within 5 km of either hospital in 2003.
All results are presented as graphs in which CHIRPP mTBI rates are compared to the provincial population-based rates.Footnote 16 Since the provincial rates are nonlinear, we did not calculate regressions but rather looked at how CHIRPP mTBI rates paralleled the population-based rate, such as by comparing slopes (with confidence intervals) where increases and decreases occurred.
The Research Ethics Boards of the McGill University Health Centre and CHU Sainte-Justine approved this research.
Results
Between 2003 and 2016, a total of 340 241 injuries in children less than 18 years of age were recorded in the CHIRPP databases of the two child trauma centres in Montréal, averaging 24 300 injuries per year. Of these 340 241 cases, 60 635 were mTBI.
When we used all injuries as a denominator for CHIRPP rates, fluctuations in CHIRPP mTBI rates were similar to those of the provincial rates: a sudden increase in 2009, then a drop, followed by a steady increase between 2010 and 2014, and another drop in 2015 and 2016. For both CHIRPP and provincial rates, the lowest point was in 2008 and the highest point was in 2014. When we used the population of children living within 5 km of either hospital between 2007 and 2016 as the denominator, CHIRPP's rates again paralleled the provincial rates, and there were no statistically significant differences between the rate of increase (i.e. slopes 2007–2016) for CHIRPP (3.55; 95% CI: 1.27–5.83) and for the province (4.60; 95% CI: 2.56–6.64) (Figure 1).
Figure 1. Quebec provincial mTBI rates versus CHIRPP rates at two Montréal hospitals, in children aged 0 to 17 years, 2003–2016
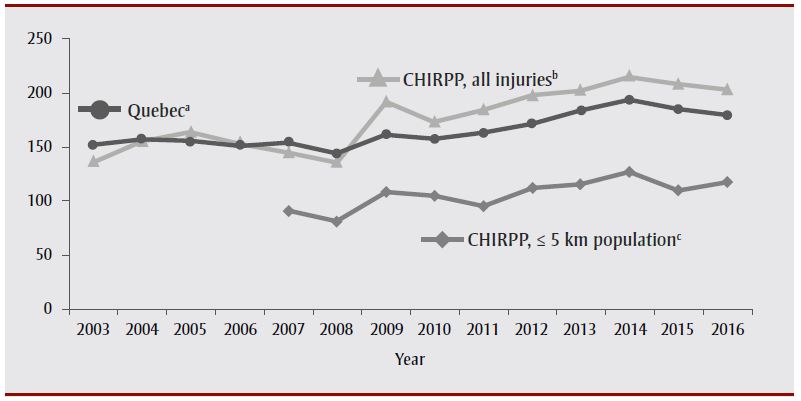
Abbreviations: CHIRPP, Canadian Hospitals Injury Reporting and Prevention Program; mTBI, mild traumatic brain injury.
a Quebec provincial mTBI rates per 10 000 children aged 0 to 17 years.
b Number of mTBI per 1000 CHIRPP injuries in children aged 0 to 17 years at The Montreal Children's Hospital and Centre hospitalier universitaire mère-enfant Sainte-Justine.
c Number of mTBI in children aged 0 to 17 years living within 5 km of either hospital per 10 000 children aged 0 to 17 years living within 5 km of either hospital.
Text description
| Year | QuebecFigure 1 Footnote a | CHIRPP, all injuriesFigure 1 Footnote b | CHIRPP, ≤ 5 km populationFigure 1 Footnote c |
|---|---|---|---|
| 2003 | 152 | 137 | N/A |
| 2004 | 157 | 156 | N/A |
| 2005 | 155 | 164 | N/A |
| 2006 | 152 | 154 | N/A |
| 2007 | 154 | 145 | 90.96 |
| 2008 | 144 | 136 | 81.12 |
| 2009 | 162 | 192 | 108.34 |
| 2010 | 157 | 173 | 104.96 |
| 2011 | 163 | 184 | 95.21 |
| 2012 | 172 | 197 | 112.12 |
| 2013 | 184 | 202 | 115.83 |
| 2014 | 194 | 216 | 126.72 |
| 2015 | 185 | 208 | 110.14 |
| 2016 | 179 | 203 | 117.73 |
|
|||
Sex played an important role in the CHIRPP rates, as it did in the provincial rates. Rates in males were always higher than those in females (an average of 1.5 times more). For males, when using all CHIRPP injuries as a denominator, the rates of mTBI were similar to the published provincial rates over four distinct periods: a decrease from 2006 to 2008, a sudden increase in 2009, followed by a drop, then an increase from 2010 to 2014 followed by a decrease from 2015 to 2016. Interestingly, for males, the rates were the same as the provincial rates in 2009 and 2014. For our second denominator, the number of males aged 0 to 17 years living within 5 km of either hospital, there were no statistically significant differences between the rate of increase (i.e. slopes: 2007–2016) between CHIRPP (3.87; 95% CI: 1.58–6.16) and the provincial rates (3.80; 95% CI: 1.21–6.39) (Figure 2).
Figure 2. Quebec provincial mTBI rates versus CHIRPP rates at two Montréal hospitals, in males aged 0 to 17 years, 2003–2016
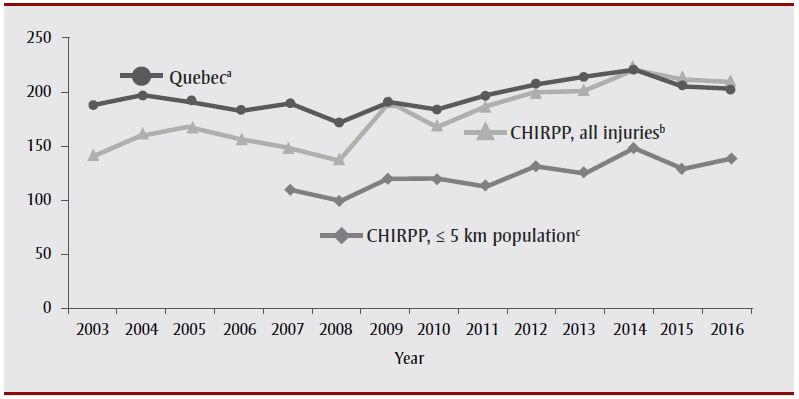
Abbreviations: CHIRPP, Canadian Hospitals Injury Reporting and Prevention Program; mTBI, mild traumatic brain injury.
a Quebec provincial mTBI rates per 10 000 males aged 0 to 17 years.
b Number of mTBI per 1000 CHIRPP injuries in males aged 0 to 17 years at The Montreal Children's Hospital and Centre hospitalier universitaire mère-enfant Sainte-Justine.
c Number of mTBI in males aged 0 to 17 years living within 5 km of either hospital per 10 000 males aged 0 to 17 years living within 5 km of either hospital.
Text description
| Year | QuebecFigure 2 Footnote a | CHIRPP, all injuriesFigure 2 Footnote b | CHIRPP, ≤ 5 km populationFigure 2 Footnote c |
|---|---|---|---|
| 2003 | 188 | 141 | N/A |
| 2004 | 197 | 161 | N/A |
| 2005 | 191 | 167 | N/A |
| 2006 | 183 | 155 | N/A |
| 2007 | 190 | 148 | 110.54 |
| 2008 | 172 | 137 | 97.50 |
| 2009 | 191 | 191 | 118.23 |
| 2010 | 184 | 169 | 119.43 |
| 2011 | 197 | 186 | 111.68 |
| 2012 | 206 | 201 | 130.97 |
| 2013 | 215 | 202 | 124.58 |
| 2014 | 222 | 224 | 147.82 |
| 2015 | 207 | 213 | 127.77 |
| 2016 | 204 | 210 | 137.59 |
|
|||
The same cannot be said for females. CHIRPP's rates (using all CHIRPP injuries as the denominator) did not parallel the published provincial rates between 2003 and 2008 but, similar to males, from 2008 onward, the rates paralleled one another. When using the number of females living within 5 km of either hospital as denominator for CHIRPP, the rate of increase (2007–2016) was smaller in CHIRPP (3.19; 95% CI: 0.42–5.96) than the published provincial rate (5.43; 95% CI: 3.51–7.35) (Figure 3).
Figure 3. Quebec provincial mTBI rates versus CHIRPP rates in two Montréal hospitals, in females aged 0 to 17 years, 2003–2016
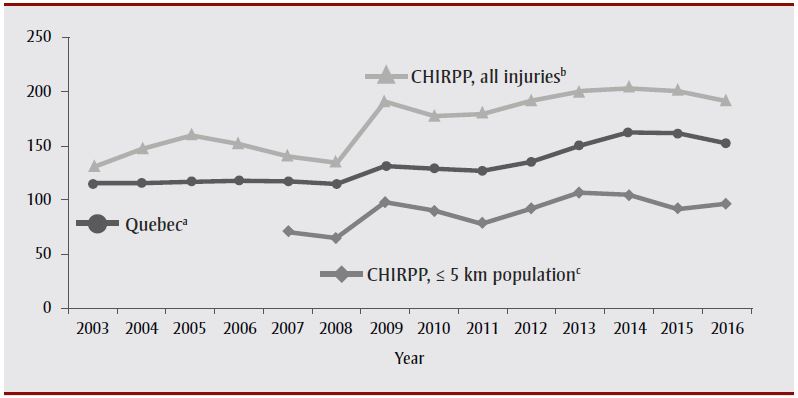
Abbreviations: CHIRPP, Canadian Hospitals Injury Reporting and Prevention Program; mTBI, mild traumatic brain injury.
a Quebec provincial mTBI rates per 10 000 females aged 0 to 17 years.
b Number of mTBI per 1000 CHIRPP injuries in females aged 0 to 17 years at The Montreal Children's Hospital and Centre hospitalier universitaire mère-enfant Sainte-Justine.
c Number of mTBI in females aged 0 to 17 years living within 5 km of either hospital per 10 000 females aged 0 to 17 years living within 5 km of either hospital.
Text description
| Year | QuebecFigure 3 Footnote a | CHIRPP, all injuriesFigure 3 Footnote b | CHIRPP, ≤ 5 km populationFigure 3 Footnote c |
|---|---|---|---|
| 2003 | 115 | 131 | N/A |
| 2004 | 116 | 148 | N/A |
| 2005 | 117 | 161 | N/A |
| 2006 | 119 | 152 | N/A |
| 2007 | 117 | 141 | 70.72 |
| 2008 | 114 | 135 | 64.22 |
| 2009 | 132 | 193 | 98.13 |
| 2010 | 129 | 179 | 90.04 |
| 2011 | 128 | 181 | 78.23 |
| 2012 | 135 | 193 | 92.62 |
| 2013 | 151 | 202 | 106.75 |
| 2014 | 164 | 205 | 104.75 |
| 2015 | 163 | 202 | 91.77 |
| 2016 | 153 | 193 | 96.99 |
|
|||
When looking at all combinations of age and sex, the best fit between CHIRPP and the provincial rates was found in males aged 0 to 4 years using all CHIRPP injuries as denominator (Figure 4), where the rates paralleled one another from 2003 to 2016. Inversely, the greatest variations between CHIRPP and the provincial rates were found in the older groups, using the number of children aged 13 to 17 years living within 5 km of either hospital as denominator for CHIRPP (Figure 5).
Figure 4. Quebec provincial mTBI rates versus CHIRPP rates in two Montréal hospitals, in males aged 0 to 4 years, 2003–2016
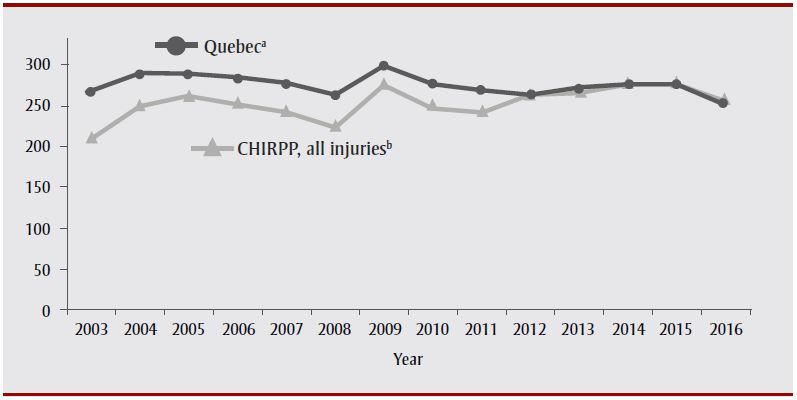
Abbreviations: CHIRPP, Canadian Hospitals Injury Reporting and Prevention Program; mTBI, mild traumatic brain injury.
a Quebec provincial mTBI rates per 10 000 males aged 0 to 4 years.
b Number of mTBI per 1000 CHIRPP injuries in males aged 0 to 4 years at The Montreal Children's Hospital and Centre hospitalier universitaire mère-enfant Sainte-Justine.
Text description
| Year | QuebecFigure 4 Footnote a | CHIRPP, all injuriesFigure 4 Footnote b |
|---|---|---|
| 2003 | 268 | 207 |
| 2004 | 289 | 248 |
| 2005 | 289 | 260 |
| 2006 | 284 | 250 |
| 2007 | 276 | 241 |
| 2008 | 263 | 221 |
| 2009 | 299 | 274 |
| 2010 | 276 | 246 |
| 2011 | 268 | 241 |
| 2012 | 261 | 265 |
| 2013 | 272 | 264 |
| 2014 | 277 | 279 |
| 2015 | 275 | 273 |
| 2016 | 251 | 255 |
|
||
Figure 5. Quebec provincial mTBI rates versus CHIRPP rates in two Montréal hospitals, in children aged 13 to 17 years, 2007–2016
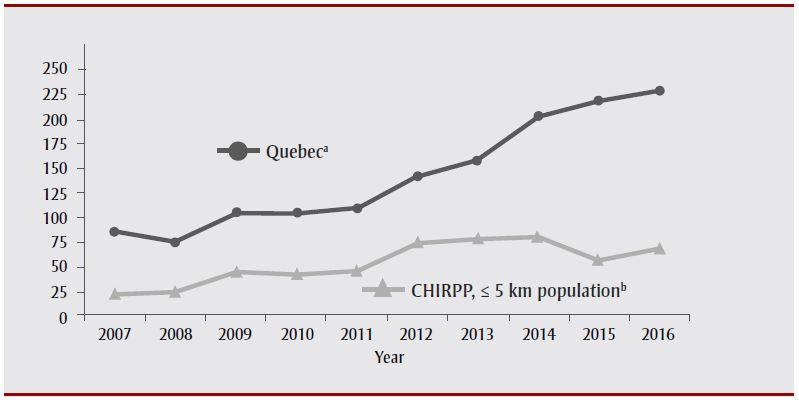
Abbreviations: CHIRPP, Canadian Hospitals Injury Reporting and Prevention Program; mTBI, mild traumatic brain injury.
a Quebec provincial mTBI rates per 10 000 children aged 0 to 4 years.
b Number of mTBI in children aged 13 to 17 living within 5 km of either The Montreal Children's Hospital or Centre hospitalier universitaire mère-enfant Sainte-Justine per 10 000 children aged 13 to 17 years living within 5 km of either hospital.
Text description
| Year | QuebecFigure 5 Footnote a | CHIRPP, ≤ 5 km populationFigure 5 Footnote b |
|---|---|---|
| 2007 | 86.7 | 22.2 |
| 2008 | 75.4 | 24.1 |
| 2009 | 104.5 | 45.2 |
| 2010 | 105.3 | 41.2 |
| 2011 | 110.7 | 45.1 |
| 2012 | 141.2 | 74.4 |
| 2013 | 159.2 | 78.1 |
| 2014 | 203.7 | 80.1 |
| 2015 | 217.8 | 57.6 |
| 2016 | 230.4 | 68.7 |
|
||
Discussion
The population-based pediatric mTBI rates in QuebecFootnote 16 and CHIRPP Montréal's mTBI rates were similar in many regards. Whether using all CHIRPP injuries or the population of children living within 5 km of either child trauma centre in Montréal as the denominator in our calculations, CHIRPP Montréal's mTBI rates mirrored four distinct fluctuations of the population-based rates: a sudden peak in 2009, then a sudden drop in 2010, followed by an increase until 2014, then another drop in 2015.
Several studies outside of Quebec have reported increases in mTBI rates in recent years, varying according to age and sex.Footnote 10Footnote 11Footnote 12Footnote 13Footnote 14Footnote 15Footnote 18 Within Quebec, mTBI rates increased 1.35-fold between 2008 (lowest rate) and 2014 (highest rate). Similarly, 2008 and 2014 were also the years of the lowest and highest CHIRPP rates, representing a 1.59-fold increase when using all CHIRPP injuries or a 1.56-fold increase when using the population living within 5 km. The drop in mTBI rates in Quebec from 2014 to 2016, a 1.08-fold decrease, was also observed in CHIRPP, with a 1.08-fold decrease using all CHIRPP injuries and a 1.06-fold decrease using population within 5 km.
Several studies have reported that the increases in rates of mTBI were more important in females than in males,Footnote 14Footnote 19Footnote 20Footnote 21Footnote 22Footnote 23 and that females had significantly higher odds of reporting concussions than males.Footnote 24 This phenomenon was also captured by our CHIRPP data. In the province of Quebec, the fold increase for females between 2008 and 2014 was 1.43, while in CHIRPP it was 1.52 (all CHIRPP injuries) and 1.63 (population within 5 km). In males, the fold increase was less than in females: 1.29 for the province of Quebec, 1.33 using all CHIRPP injuries, and 1.52 using population within 5 km. As to the decrease in mTBI rates between 2014 and 2016, the fold decrease was the same for males and females, for the province as well as for CHIRPP.
Rates by age group and sex showed large variations between CHIRPP and the provincial rates. When using all CHIRPP data as denominator, the best fit was found in males aged 0 to 4 years, while the worst fit was in females aged 5 to 8 years. As to the population within 5 km, the best fit between CHIRPP and the provincial rates was found in males aged 5 to 8 years, and the worst in children (males and females) aged 13 to 17 years.
Because the recent increase in mTBI rates has been reported in other studies, we compared CHIRPP mTBI rates with findings from these other studies (Table 1). As with each of the other studies, CHIRPP reported positive increases for the different periods, but also concurred with these studies on how the increases varied with age. The two studies with similar designs to ours produced strikingly similar results. Chen et al.,Footnote 25 who only considered ED visits in the United States, observed that between 2006 and 2013, for the ages 0 to 17 years, the fold increase in mTBI rates was 1.3; in CHIRPP it was 1.3 (when using all injuries as the denominator). Fridman et al.,Footnote 13 who only considered the index concussion (as CHIRPP does—only the first visit for an injury is tabulated) reported that in the age group 5 to 18 years, there was a 3.7-fold increase for concussions between 2004 and 2013. For CHIRPP, when only considering concussions, the fold increase was also 3.7 (using all CHIRPP injuries as the denominator).
| Location | Age | Period | Fold increase | CHIRPP rates in the same time period | |
|---|---|---|---|---|---|
| CHIRPP allTable 1 Footnote a | CHIRPP ≤ 5kmTable 1 Footnote b | ||||
| Fold increase | Fold increase | ||||
| Ambulatory visits, United StatesFootnote 23 | 6–21 | 2007–13 | 4.0 | 1.7 | 1.3 |
| Private insurer, United StatesFootnote 15 | 0–17 | 2004–13 | 1.7 | 1.4 | — |
| ED visits, United StatesFootnote 25 | 0–17 | 2006–13 | 1.3 | 1.3 | — |
| ED visits, United StatesFootnote 12 | 12–18 | 2005–15 | 1.4 | 2.0 | — |
| NEISSFootnote 20 | 0–10 | 2007–11 | 1.6 | 1.2 | 1.1 |
| Private insurer, United StatesFootnote 18 | 0–4 | 2007–14 | no variation | no variation | no variation |
| 5–9 | 2.3 | 1.5 | 1.5 | ||
| 10–14 | 2.9 | 2.1 | 2.2 | ||
| 15–19 | 2.2 | 2.4 | 3.0 | ||
| ED visits, United-StatesFootnote 11 | 0–4 | 2006–12 | 1.2 | no variation | — |
| 5–9 | 1.4 | 1.1 | — | ||
| 10–14 | 1.7 | 2.1 | — | ||
| 15–19 | 2.0 | 2.4 | — | ||
| Private insurer, United StatesFootnote 26 | 0–9 | 2010–15 | 1.2 | 1.1 | 1.0 |
| 10–19 | 1.7 | 1.6 | 1.4 | ||
| All visits, OntarioFootnote 14 | 5–18 | 2003–13 | 1.8 | 1.5 | — |
| Ontario, only index concussions (all visits)Footnote 13 | 5–18 | 2004–13 | 3.7 | 3.7 | — |
| 5–18 | 2007–13 | 3.7 | 3.5 | 5.6 | |
Abbreviations: CHIRPP, Canadian Hospitals Injury Reporting and Prevention Program; ED, emergency department; NEISS, National Electronic Injury Surveillance System. Note: — Unavailable for the given period.
|
|||||
One advantage of CHIRPP is that it only considers the first visit for an injury and discards any follow-up consultations, thus providing true rates of injuries, rather than reporting on utilization of medical services. Conclusions drawn from administrative data that include all visits by the same patient for the same injury, introduce a significant bias for anyone wanting to comment on the increased rates of mTBI. While data from the Quebec studyFootnote 16 confirmed that the number of visits per patient for mTBI remained the same between 2003 and 2016, another from OntarioFootnote 13 concluded that follow-up visits, within three months of the first visit for a concussion, tripled between 2003 and 2013 in patients aged 5 to 18 years. Interestingly, if we adjust the rates of the Quebec studyFootnote 16 down 1.75, the average number of mTBI visits per patient per year (to represent the number of mTBI rather than the number of consultations for an mTBI, as patients consult more than once for the same mTBI) and compare them to CHIRPP's mTBI rates for children living within 5 km of either of the two trauma hospitals, we find that the average rates of mTBI between 2007 and 2016 were quite similar: 106.3 per 10 000 (95% CI: 96.5–116.1) in CHIRPP and 98.2 per 10 000 (95% CI: 91.5–104.8) for Quebec.
As for CHIRPP data, the main limitation when using it as a tool to study yearly fluctuations pertains to patients who consult the ED and leave without being seen (LWBS). The proportions of LWBS vary from one year to the next, from 4.5% to 9.4%, which means that some years, more patients are not recorded in CHIRPP. This, we believe, only impacts the mTBI CHIRPP rates when using the population living within 5 km of either hospital as the denominator; rates calculated using CHIRPP's total injuries would not be affected, we believe, since the proportion of mTBI in those who LWBS remains the same from one year to the next.
Conclusion
Our study suggests that CHIRPP's representativeness of a population may be greater than suggested in earlier studies,Footnote 3Footnote 4Footnote 5Footnote 6Footnote 7Footnote 8Footnote 9 and our results support the usefulness of CHIRPP as a surveillance tool and its capacity to identify fluctuations in injuries within the population.
The data were limited to the two CHIRPP centres in Montréal, and we cannot say if other CHIRPP centres in Canada would produce similar results. Further research could answer these questions more definitively, but so far, there is encouraging evidence that CHIRPP rates are representative of the population.
Acknowledgements
This research was made possible by a grant from the Public Health Agency of Canada. The authors would like to thank the Canadian Hospital Injury Reporting and Prevention Program for their support.
Conflicts of interest
The authors declare they have no conflicts of interest.
Authors' contributions and statement
Four authors contributed to this manuscript: Glenn Keays, Debbie Friedman, Isabelle Gagnon and Marianne Beaudin. GK drafted the manuscript, and all authors contributed to its revision. GK analyzed the data and DF, IG and MB contributed to the development and revisions. GK takes responsibility for the paper as a whole.
The content and views expressed in this article are those of the authors and do not necessarily reflect those of the Government of Canada.
References
- Footnote 1
-
Nwomeh BC, Lowell W, Kable R, Haley K, Ameh EA. History and development of trauma registry: lessons from developed to developing countries. World J Emerg Surg [Internet]. 2006 [cited 2019 Feb 10];1:32. doi: 10.1186/1749-7922-1-32.
- Footnote 2
-
Health Canada. Canadian Hospitals Injury Reporting and Prevention Program Ottawa [Internet]. Ottawa (ON): Government of Canada; [modified 2018 Nov 15; cited 2018 Jun]. Available from: https://www.canada.ca/en/public-health/services/injury-prevention/canadian-hospitals-injury-reporting-prevention-program.html
- Footnote 3
-
Pickett W, Brison RJ, Mackenzie SG, et al. Youth injury data in the Canadian Hospitals Injury Reporting and Prevention Program: do they represent the Canadian experience? Inj Prev. 2000;6(1):9-15. doi: 10.1136/ip.6.1.9.
- Footnote 4
-
Lindsay H, Brussoni M. Injuries and helmet use related to non-motorized wheeled activities among pediatric patients. Chronic Dis Inj Can. 2014;34(2-3):74-81.
- Footnote 5
-
Crain J, McFaull S, Thompson W, et al. The Canadian Hospitals Injury Reporting and Prevention Program: a dynamic and innovative injury surveillance system. 2016;36(6):112-7.
- Footnote 6
-
Butler M, Newton S, MacPhee S. The Canadian Hospital Injury Reporting and Prevention Program: captured versus uncaptured injuries for patients presenting at a paediatric tertiary care centre. Paediatr Child Health. 2017;22(3):134-8. doi: 10.1093/pch/pxx042.
- Footnote 7
-
Kang J, Hagel B, Emery CA, Senger T, Meeuwisse W. Assessing the representativeness of Canadian Hospitals Injury Reporting and Prevention Programme (CHIRPP) sport and recreational injury data in Calgary, Canada. Int J Inj Contr Saf Promot. 2013;20(1):19-26. doi: 10.1080/17457300.2012.656315.
- Footnote 8
-
Macpherson AK, White H, Mongeon S, et al. Examining the sensitivity of an injury surveillance program using population-based estimates. Inj Prev. 2008;14(4):262-5. doi: 10.1136/ip.2008.018374.
- Footnote 9
-
Keays G, Friedman D, Gagnon I. A 20-year comparison of football-related injuries in American and Canadian youth aged 6 to 17 years: a replication study. Clin pediatr (Phila). 2016;55(7):603-13. doi: 10.1177/0009922815602631.
- Footnote 10
-
Amanullah S, Schlichting LE, Linakis SW, Steele DW, Linakis JG. Emergency department visits owing to intentional and unintentional traumatic brain injury among infants in the United States: a population-based assessment. J Pediatr. 2018;203:259-65.e1. doi: 10.1016/j.jpeds.2018.08.023.
- Footnote 11
-
Avraham JB, Bhandari M, Frangos SG, Levine DA, Tunik MG, DiMaggio CJ. Epidemiology of paediatric trauma presenting to US emergency departments: 2006–2012. Inj Prev. 2019;25(2):136-43. doi: 10.1136/injuryprev-2017-042435.
- Footnote 12
-
Baker DR, Kulick ER, Boehme AK, Noble JM. Effects of the New York State Concussion Management and Awareness Act ("Lystedt Law") on concussion-related emergency health care utilization among adolescents, 2005–2015. Am J Sports Med. 2018;46(2):396-401. doi: 10.1177/0363546517738742.
- Footnote 13
-
Fridman L, Scolnik M, Macpherson A, et al. Annual trends in follow-up visits for pediatric concussion in emergency departments and physicians' offices. J Pediatr. 2018;192:184-8. doi: 10.1016/j.jpeds.2017.09.018.
- Footnote 14
-
Zemek RL, Grool AM, Rodriguez Duque D, et al. Annual and seasonal trends in ambulatory visits for pediatric concussion in Ontario between 2003 and 2013. J Pediatr. 2017;181:222-8.e2. doi: 10.1016/j.jpeds.2016.10.067.
- Footnote 15
-
Zogg CK, Haring RS, Xu L, et al. The epidemiology of pediatric head injury treated outside of hospital emergency departments. Epidemiology. 2018;29(2):269-79. doi: 10.1097/ede.0000000000000791.
- Footnote 16
-
Keays G, Friedman D, Gagnon I. Rates of concussions and minor head injuries in Quebec, 2003 and 2016, in children under 18 years old, and comparisons with Ontario's rates of mild traumatic brain injuries. Can J Public Health. 2018;109(1):52-60. doi: 10.17269/s41997-018-0037-6.
- Footnote 17
-
Statistics Canada. Census Program [Internet]. Ottawa (ON): Government of Canada; 2019 [cited 2018 Oct]. Available from: https://www12.statcan.gc.ca/census-recensement/index-eng.cfm
- Footnote 18
-
Zhang AL, Sing DC, Rugg CM, Feeley BT, Senter C. The rise of concussions in the adolescent population. Orthop J Sports Med [Internet]. 2016 [cited 2019 Mar 20];4(8):2325967116662458. doi: 10.1177/2325967116s00200.
- Footnote 19
-
Cancelliere C, Donovan J, Cassidy JD. Is sex an indicator of prognosis after mild traumatic brain injury: a systematic analysis of the findings of the World Health Organization Collaborating Centre Task Force on Mild Traumatic Brain Injury and the International Collaboration on Mild Traumatic Brain Injury Prognosis. Arch Phys Med Rehabil. 2016;97(2 Suppl):S5-S18. doi: 10.1016/j.apmr.2014.11.028.
- Footnote 20
-
Gaw CE, Zonfrillo MR. Emergency department visits for head trauma in the United States. BMC Emerg Med [Internet]. 2016 [cited 2019 Mar 20];16:5 doi: 10.1186/s12873-016-0071-8.
- Footnote 21
-
Gessel LM, Fields SK, Collins CL, Dick RW, Comstock RD. Concussions among United States high school and collegiate athletes. J Athl Train. 2007;42(4):495-503.
- Footnote 22
-
King NS. A systematic review of age and gender factors in prolonged post-concussion symptoms after mild head injury. Brain Inj. 2014;28(13-14):1639-45. doi: 10.3109/02699052.2014.954271.
- Footnote 23
-
Taylor AM, Nigrovic LE, Saillant ML, et al. Trends in ambulatory care for children with concussion and minor head injury from eastern Massachusetts between 2007 and 2013. J Pediatr. 2015;167(3):738-44. doi: 10.1016/j.jpeds.2015.05.036.
- Footnote 24
-
Brown DA, Elsass JA, Miller AJ, Reed LE, Reneker JC. Differences in symptom reporting between males and females at baseline and after a sports-related concussion: a systematic review and meta-analysis. Sports Med. 2015;45(7):1027-40. doi: 10.1007/s40279-015-0335-6.
- Footnote 25
-
Chen C, Shi J, Stanley RM, Sribnick EA, Groner JI, Xiang H. U.S. trends of ED visits for pediatric traumatic brain injuries: implications for clinical trials. Int J Environ Res Public Health [Internet]. 2017 [cited 2019 Mar 28];14(4):414. doi: 10.3390/ijerph14040414.
- Footnote 26
-
Blue Cross Blue Shield. The steep rise in concussion diagnoses in the U.S [Internet]. Chicago (IL): Blue Cross Blue Shield. The Health of America Report Series; 2016 Sep 27 [cited 2018 Oct]. Available from: https://www.bcbs.com/the-health-of-america/reports/the-steep-rise-concussion-diagnoses-the-us