Wider impacts of COVID-19: A look at how substance-related harms across Canada have changed during the pandemic
Tell us what you think
Help us improve our products, answer our quick survey.
Download in PDF format
(213 KB, 2 pages)
Organization: Public Health Agency of Canada
Date published: 2021-05-05
ISBN: 978-0-660-38480-1
Cat.: HP35-144/2021E-PDF
Pub.: 210006
There is an increasing concern about a range of wider impacts of the pandemic response. Among these is the impact on problematic substance use.
Feelings of isolation, stress and anxiety, lack of a regular schedule, boredom and limited available or accessible services for people who use substances may impact harms.
Deaths, hospitalizations and visits to the emergency department are examples of harms.
Highlights
- Overall, substance-related hospital care and deaths have increased during the COVID-19 pandemic compared to the same period in 2019.
- Emergency department visits have increased for opioids, stimulants and cannabis.
- Some populations are affected more than others including males, lowest income quintile neighbourhoods and individuals aged 20 to 59 years.
- If you or a loved one is experiencing harmful substance use, there are available resources to help mitigate harms.
- For more detailed information and context surrounding these data, please view CIHI’s report.
Substance-related deaths
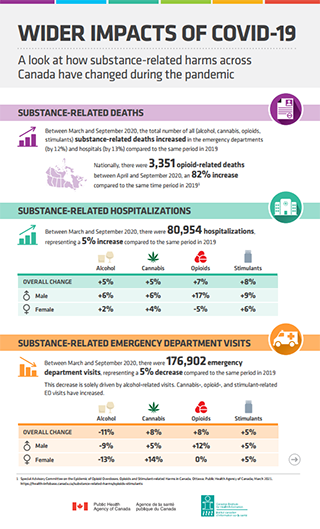
Between March and September 2020, the total number of all (alcohol, cannabis, opioids, stimulants) substance-related deaths increased in the emergency departments (by 12%) and hospitals (by 13%) compared to the same period in 2019.
- Nationally, there were 3,351 opioid-related deaths between April and September 2020, an 82% increase compared to the same time period in 2019Footnote 1.
Substance-related hospitalizations
Between March and September 2020, there were 80,954 hospitalizations, representing a 5% increase compared to the same period in 2019.
| % change (overall) | % change (males) | % change (females) | |
|---|---|---|---|
| Alcohol | +5% | +6% | +2% |
| Cannabis | +5% | +6% | +4% |
| Opioids | +7% | +17% | -5% |
| Stimulants | +8% | +9% | +6% |
Substance-related emergency department visits
Between March and September 2020, there were 176,902 emergency department visits, representing a 5% decrease compared to the same period in 2019.
This decrease is solely driven by alcohol-related visits. Cannabis-,opioid-,and stimulant-related ED visits have increased.
| % change (overall) | % change (males) | % change (females) | |
|---|---|---|---|
| Alcohol | -11% | -9% | -13% |
| Cannabis | +8% | +5% | +14% |
| Opioids | +8% | +12% | 0% |
| Stimulants | +5% | +5% | +5% |
Who was affected?
- People aged 20 to 59 years had increased hospitalizations for all substances from 2019Footnote * to 2020Footnote *
- Males
- 66% of all substance-related emergency department visits
- 64% of all substance-related hospitalizations
- 79% of all substance-related emergency department deaths
- 71% of all substance-related in-hospital deaths
- People among neighbourhoods where income is the lowestFootnote 2
- 1/3 of hospitalizations for substance-related harms
- 2/5 of emergency department visits for substance-related harms
Resources
How can you reduce substance-related harms
- Get informed, reach out to peers, family or health professionals for support.
- Wellness Together Canada (WTC): This online portal provides free and confidential, 24/7 access to mental health and substance use resources to help support the well-being of people across Canada during the COVID-19 pandemic.
- Learn more about alcohol and how to lower the risk of alcohol-related harms.
- Learn more about cannabis and how to lower the risks of cannabis-related harms.
- Learn more about fentanyl and other opioids, how reduce risks of an opioid overdose, the signs of an opioid overdose and what to do if you witness an opioid overdose.
- Learn more about stimulants, such as methamphetamines, cocaine and crack, and how to reduce the risks of stimulants-related harms.
Acknowledgements
The Public Health Agency of Canada released this infographic in collaboration with the Canadian Institute for Health Information (CIHI). PHAC would like to acknowledge CIHI for providing the data and analysis for this infographic, and for their assistance with reviewing the content. For additional information, please consult the CIHI’s full report and data tables. We would also like to acknowledge the Office of Drug Research and Surveillance, Controlled Substances Directorate, Controlled Substances and Cannabis Branch, Health Canada for reviewing the content of the infographic.
Notes and limitations
- The study population includes residents of Canada aged 10 years and older.
- Substances included in the total grouping (all substances) are: alcohol, opioids, cannabis, other central nervous system (CNS) depressants, cocaine, other CNS stimulants, other substances, and unknown and multiple substances. Substance categories for alcohol, opioids, stimulants and cannabis were examined individually. The most common substance noted in both substance-related emergency department visits and hospitalizations was alcohol, followed by opioids, then cannabis and stimulants.
- Emergency department data reported includes full coverage in Quebec, Ontario, Alberta and Yukon. It includes partial coverage in Prince Edward Island, Nova Scotia, Saskatchewan and British Columbia. Hospitalization data reported includes all provinces and territories, except Quebec. For additional information, please refer to CIHI’s full report.
- This analysis was based on provisional data and are not final; results presented should be interpreted with caution.
- This analysis only reveals the tip of the iceberg. Many people who use substances may not visit hospitals during the pandemic due to the fear of contracting COVID-19. Some may have died in the community because of acute toxicities of substances, and these individuals would not be captured in this analysis.
Footnotes
- Footnote *
-
Represents data from March to September
- Footnote 1
-
Special Advisory Committee on the Epidemic of Opioid Overdoses. Opioids and Stimulant-related Harms in Canada. Ottawa: Public Health Agency of Canada; March 2021. https://health-infobase.canada.ca/substance-related-harms/opioids-stimulants
- Footnote 2
-
Data for the lowest income quintile neighbourhoods
Production of this document has been made possible with the collaboration from the Public Health Agency of Canada and CIHI.