Improving the vaccination experience with CARD

 Download this article as a PDF
Download this article as a PDFPublished by: The Public Health Agency of Canada
Issue: Volume 47-01: Foodborne and Animal Contact Disease Outbreaks
Date published: January 2021
ISSN: 1481-8531
Submit a manuscript
About CCDR
Browse
Volume 47-01, January 2021: Foodborne and Animal Contact Disease Outbreaks
Series
Managing pain and fear: Playing your CARDs to improve the vaccination experience
Anna Taddio1, Anthony Ilersich2, C Meghan McMurtry3, Lucie M Bucci4, Noni E MacDonald5
Affiliations
1 Leslie Dan Faculty of Pharmacy, University of Toronto, Toronto, ON
2 Faculty of Math, University of Waterloo, Waterloo, ON
3 Department of Psychology, University of Guelph, Guelph, ON
4 Immunize Canada, Canadian Public Health Association, Ottawa, ON
5 Faculty of Medicine, Dalhousie University, Halifax, NS
Correspondence
Suggested citation
Taddio A, Ilersich A, McMurtry CM, Bucci LM, MacDonald NE. Managing pain and fear: Playing your CARDs to improve the vaccination experience. Can Commun Dis Rep 2021;47(1):87–91. https://doi.org/10.14745/ccdr.v47i01a12
Keywords: vaccination, pain, fear, pain management, vaccine hesitancy, needlesticks
Abstract
Most vaccinations are administered with a needle, which can cause pain and pain-related symptoms such as fear and fainting. At present, interventions aimed at preventing pain and associated symptoms are not systematically integrated in the vaccination delivery process even though they contribute to negative experiences with vaccination and vaccination noncompliance. In this article, a novel framework for vaccination delivery called the CARD™ system was reviewed. CARD is an acronym for Comfort, Ask, Relax and Distract, whereby each letter category incorporates evidence-based interventions to reduce pain and fear and related symptoms. CARD can be integrated in usual vaccination planning and delivery activities in many settings to improve the vaccination experience and decrease pain and fear as barriers to vaccination. Immunizers in all settings and organizational leaders are invited to review their vaccination services against CARD to identify opportunities for enhancing the quality of care being provided.
Introduction
Vaccine injections are frequently associated with pain and pain-related adverse effects, such as fear, fainting, nausea and other stress-related responses Footnote 1 Footnote 2. Until recently, little attention has been paid to reducing pain and related symptoms during vaccination. However, accumulating evidence shows that negative experiences with vaccination can contribute to the development of needle fears, vaccine hesitancy and healthcare avoidance behaviours, including vaccination noncompliance Footnote 3 Footnote 4. This is particularly important during childhood, when concerns about pain and fear of needles are high and attitudes towards healthcare providers are being shapedFootnote 2 Footnote 5 .
Vaccination is the most common reason, by far, why people receive needles. The World Health Organization has identified overcoming barriers to immunizations as a priority for global health Footnote 6. Addressing barriers to vaccination is even more relevant now, during the pandemic, to help with acceptance of COVID-19 vaccine(s) when they become available.
There are numerous negative consequences of unmanaged pain when receiving needles. Individuals are often subjected to longer procedure times and increased use of restraint, and can experience potentially serious adverse events such as fainting, nausea and other stress-related responses Footnote 2 Footnote 7 Footnote 8 . Having to deal with long and complex patient interactions leads to additional stress for the healthcare providers administering vaccinations. Immunizers commonly report challenges with current vaccination delivery processes that may increase the risk of unwanted outcomes. These challenges include suboptimal physical spaces, lack of preparation and communication of important stakeholders, unclear roles, competing demands and excessive patient symptoms (fear, pain, dizziness), particularly in children Footnote 9 Footnote 10 Footnote 11. Recently, fear of acquiring COVID-19 infection while being immunized has only exacerbated these concerns.
There are numerous evidence-based and feasible interventions for improving the vaccination experience Footnote 1. Pain management needs to be recognized as a part of good vaccination practice and this knowledge needs to be systematically integrated into practice Footnote 12. Based on their clinical practice guideline Footnote 1, the national HELPinKids&Adults team recently developed a vaccine delivery framework called CARD™ that shows immunizers and program managers responsible for vaccination delivery how to integrate these interventions into vaccination planning and delivery processes. In addition, CARD teaches patients how to cope with their own vaccination experience Footnote 11. This article explains the framework and how to apply it in various settings.
What is CARD?
CARD stands for Comfort, Ask, Relax and Distract. Each of the four initial letters stands for an intervention category, and the four encompass activities that reduce pain, fear, fainting and related symptoms before, during and after vaccination. The CARD system can be used with children and adults, with participatory activities in all four intervention categories.
How was CARD developed?
CARD was originally designed to improve the vaccination experience at school, but it is a valuable tool for vaccination delivery in various settings, including healthcare providers' offices. In fact, one of its main strengths lies in its adaptability to many different settings. Most importantly, CARD was developed with input from different stakeholders involved in vaccinations at school. Immunizers, students, parents/guardians and school staff were involved in a stepwise approach that included identifying needs and preferences, developing tools and resources, and implementing and evaluating the impact of implementation Footnote 11.
CARD works
In a controlled cluster trial conducted in Niagara, Ontario, students in schools where CARD was implemented (versus control) reported less fear (odds ratio [OR] =0.47, 95% confidence interval [CI]: 0.27–0.82) and dizziness (OR=0.26, 95% CI: 0.07–0.91) during vaccination Footnote 13. Students educated about CARD had higher knowledge scores and more positive attitudes towards vaccination. Students wanted other students to learn about CARD as they had found it so helpfulFootnote 13. Immunizers, parents/guardians and school staff also reported more positive attitudes about the vaccination experience when CARD was in use Footnote 14.
Tailoring CARD to your setting
CARD can be tailored to work in a variety of settings, including private offices, hospitals, schools and pharmacies. Key elements of CARD include education of immunizers and patients, setting up the vaccination site to be supportive, and ensuring that immunizer and patient interactions embrace the patients' preferences (i.e. CARD choices). Patients can learn about CARD from online resources, for example, videos and pamphlets Footnote 11. While the majority of resources are primarily focused on adolescents, new resources are currently being developed for the adult vaccination context (https://immunize.ca/card-adults). Figure 1 shows sample interventions that patients can "play" to make the procedure a more positive experience.
Figure 1: Sample interventions from the CARD system
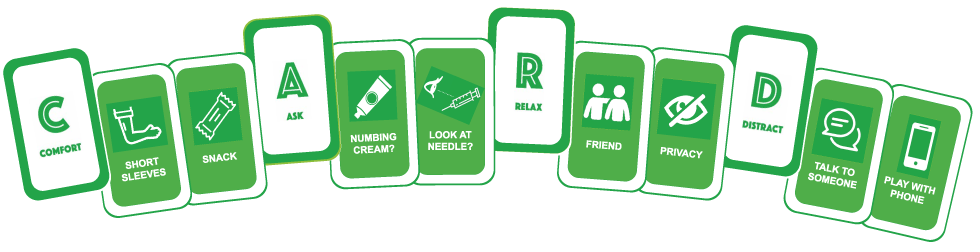
Text description: Figure 1
Figure 1: Sample interventions from the CARD system
Sample interventisons from each of the letter categories of CARD that people can play to reduce pain, fear and fainting.
Immunizers also receive simple training in the importance of the components of CARD and how to support the choices patients make. The immunizer and patient form a team to make the experience as positive as possible. From the planning stages to actual injection, and across different vaccination settings, the immunizer can review current vaccination procedures against the CARD framework, looking for opportunities to incorporate ways to optimize the vaccination experience.
Table 1 summarizes some of the activities normally associated with planning and delivery of vaccinations and how to incorporate CARD into those activities. All stakeholders involved in the vaccination process, including immunizers and patients, can "play their CARDs" to facilitate a more positive vaccination experience. For instance, immunizers can make sure there is comfortable seating for the patient (Comfort) and invite patients to ask questions before, during and after the procedure (Ask). Doing this helps patients feel comfortable, informed and involved, which helps them feel calm. It also builds trust in healthcare providers because they demonstrate that they are caring and attentive to patient needs. Immunizers can also ask patients questions (e.g. How afraid are you? Do you prefer to look away?) to help them assess the patient's status as well as to engage patients as active participants. Patients can bring a favourite item (Comfort) or an electronic device (Distract) for use during vaccination to help cope. While each stakeholder (needle givers and receivers) has their own CARDs to play, the full potential of the CARD framework is realized when all play their own CARDs with the shared goal of improving the vaccination experience.
| Phase of vaccination | Immunizer activity |
|---|---|
| Preparation/planning | |
| Ensure adequate clinic space |
|
| Educate patients and other stakeholders (e.g. parents/guardians, teachers) |
|
| Vaccination day reminders |
|
| Vaccination day | |
| Vaccination clinic set-up |
|
| Vaccination administration |
|
Playing CARD is teamwork
In many settings, vaccination delivery is complex, and immunizers are unable to make the necessary changes to adopt CARD on their own. It is crucial to involve organizational leaders who can facilitate adoption by making changes to relevant policies and procedures. These changes could include staff roles, training, ongoing communication and evaluation (e.g. staff meetings, summaries, audit and feedback) and ongoing support (e.g. educational resources) Footnote 11. This also includes promoting awareness and understanding of overarching models of healthcare delivery and professional standards that promote person-centred care and evidence-based practice, and actively practising continuous quality improvement and reflective practice.
Immunizers and their organizational leaders can also identify opportunities to leverage current activities to facilitate activities specific to CARD. For instance, immunizers typically notify teachers and parents/guardians of upcoming school-based vaccinations. These stakeholders can learn about CARD and reinforce teaching the CARD system to the children. Engaging stakeholders, including teachers and parents/guardians, has multiple benefits, including improving fidelity of implementation, creating a "social norm" that recognizes and respects individuals' participation in their healthcare, their preferences for information and coping, and it minimizes the need for additional resources. In turn, parents/guardians and teachers feel more at ease knowing that children are being cared for, and this creates a more welcoming environment for everyone.
Our experience with using CARD in a school-based vaccination program in Niagara, Ontario, was that, after training and support during initial implementation, the system could be incorporated into usual activities in a cost-neutral manner Footnote 12. Immunizers will need some additional time to prepare for vaccinations because of the planning steps, such as educating all stakeholders. However, the required time will lessen as everyone becomes familiar with CARD.
Conclusion
Addressing pain and associated stress-related reactions are proven to improve the vaccination experience for patients and immunizers alike. The long-term benefits of the CARD framework are numerous and include the potential for improved health outcomes due to improved acceptance of healthcare interventions, including vaccination. CARD allows immunizers to "play their best hand" with respect to setting up and running clinics or individual vaccination appointments. The CARD system is a valuable tool for optimizing the vaccination experience and addressing one of the long-recognized yet neglected harms of vaccination, the needle.
Authors' statement
- AT — Conceptualization, writing–original draft, review and editing
- AI — Conceptualization, writing–review and editing
- CMM — Conceptualization, writing–review and editing
- LMB — Writing–review and editing
- NEM — Writing–review and editing
All authors take responsibility for the content of this article.
Competing interests
AT reports a Section 9 Trademark No. 924835 for CARD. LMB reports that Immunize Canada received grants from Pfizer Canada, Merck Canada, GSK Canada, Seqirus Canada and Sanofi Pasteur outside the submitted work. There are no other disclosures.
Acknowledgements
The authors thank M Ho for creation of Figure 1.
Funding
This work is funded by the Canadian Institutes of Health Research (FRN 159905).
The content and view expressed in this article are those of the authors and do not necessarily reflect those of the Government of Canada.
