Modelling preventive effectiveness to estimate the equity tipping point: at what coverage can individual preventive interventions reduce socioeconomic disparities in diabetes risk? - CDIC: Vol 34, No 2-3, July 2014
Volume 34 · Number 2-3 · July 2014
Chronic Diseases and Injuries in Canada
Modelling preventive effectiveness to estimate the equity tipping point: at what coverage can individual preventive interventions reduce socioeconomic disparities in diabetes risk?
D. G. Manuel, MD (1, 2, 3, 4, 5); T. H. Ho, MSc (1); S. Harper, PhD (6); G. M. Anderson, MD, PhD (1, 7); J. Lynch, PhD (8, 9); L. C. Rosella, PhD (1, 2, 10)
https://doi.org/10.24095/hpcdp.34.2/3.04
This article has been peer reviewed.
Author references:
- Institute for Clinical Evaluative Sciences, Toronto, Ontario, Canada
- Dalla Lana School of Public Health, University of Toronto, Toronto, Ontario, Canada
- Ottawa Hospital Research Institute, Ottawa, Ontario, Canada
- Statistics Canada, Ottawa, Ontario, Canada
- Department of Family Medicine and Department of Epidemiology and Community Medicine, University of Ottawa, Ottawa, Ontario, Canada
- Department of Epidemiology, Biostatistics and Occupational Health, McGill University, Montréal, Quebec, Canada
- Department of Health Policy, Management, and Evaluation, University of Toronto, Toronto, Ontario, Canada
- School of Population Health and Clinical Sciences, University of Adelaide, Adelaide, Australia
- Department of Social and Community Medicine, University of Bristol, Bristol, United Kingdom
- Public Health Ontario, Toronto, Ontario, Canada
Correspondence: Douglas G. Manuel, Ottawa Health Research Institute, 1-008 Admin Services Building, 1053 Carling Avenue, Ottawa, ON K1Y 4E9; Tel.: 613-798-5555, ext. 19108; Fax: 613-761-5492; Email: dmanuel@ohri.ca
Abstract
Introduction: Most individual preventive therapies potentially narrow or widen health disparities depending on the difference in community effectiveness across socioeconomic position (SEP). The equity tipping point—defined as the point at which health disparities become larger—can be calculated by varying components of community effectiveness such as baseline risk of disease, intervention coverage and/ or intervention efficacy across SEP.
Methods: We used a simple modelling approach to estimate the community effectiveness of diabetes prevention across SEP in Canada under different scenarios of intervention coverage.
Results: Five-year baseline diabetes risk differed between the lowest and highest income groups by 1.76%. Assuming complete coverage across all income groups, the difference was reduced to 0.90% (144 000 cases prevented) with lifestyle interventions and 1.24% (88 100 cases prevented) with pharmacotherapy. The equity tipping point was estimated to be a coverage difference of 30% for preventive interventions (100% and 70% coverage among the highest and lowest income earners, respectively).
Conclusion: Disparities in diabetes risk could be measurably reduced if existing interventions were equally adopted across SEP. However, disparities in coverage could lead to increased inequity in risk. Simple modelling approaches can be used to examine the community effectiveness of individual preventive interventions and their potential to reduce (or increase) disparities. The equity tipping point can be used as a critical threshold for disparities analyses.
Keywords: inequalities, public health, health impact assessment, diabetes
Introduction
The role of individual preventive therapy in reducing health disparities is the subject of current debate. One the one hand, health disparities may be reduced when relative treatment effects are constant across the spectrum of underlying risk.Footnote 1, Footnote 2, Footnote 3 If this assumption held true, the absolute community effectiveness from health interventions would be greater for disadvantaged groups compared to others because disadvantaged groups tend to have a higher baseline risk. Greater gains in absolute benefit for those in the lowest socioeconomic position (SEP) compared to those in higher SEP would therefore lead to a decrease in disparities between them.Footnote 1
On the other hand, constant intervention efficacy should not be assumed and intervention coverage is often inequitable. Intervention coverage, defined as the proportion of the target population that is adherent to the intervention, encompasses the range of factors that affect the uptake of interventions, such as accuracy in identifying the target population, level of participation in the intervention and consumers' adherence.Footnote 4 Groups at a lower socioeconomic level tend to experience greater barriers in access to care, for example through income effects, or they may be less adherent to preventive therapies, for example, education effects.Footnote 5 Together, differences in efficacy and coverage undermine efforts to reduce disparities or else they can, perversely, increase disparities.Footnote 6
In this study, we show how a simple modelling approach can be used to estimate the potential effectiveness of prevention interventions at reducing disparities (see Formula 1). We demonstrate this using diabetes prevention in Canada.
FORMULA 1
Community effectiveness = target population X baseline risk X intervention efficacy X intervention coverageFootnote *
Community effectiveness: the benefit, or absolute risk reduction, of preventive interventions in the real-world community setting.
Target population: the proportion of the population, or each sociodemographic strata, that is eligible for the preventive intervention.
Baseline risk: the risk or probability of developing a disease prior to intervention implementation.
Intervention efficacy: the relative benefit of an intervention as determined from intervention trials or other studies, i.e. ideal or controlled settings.
Intervention coverage: the proportion of the target population that is adherent to the intervention.
The potential for interventions to reduce inequalities can be estimated when we calculate and compare community effectiveness for each socioeconomic stratum. Disease disparities will narrow if community effectiveness is larger for low socioeconomic groups compared to their higher SEP counterparts.
A common challenge when estimating community effectiveness for individual socioeconomic strata is the lack of information that is specific to the different strata, including variation in the target population size, baseline risk, intervention efficacy and coverage. For such situations, we introduce the concept of the ''equity tipping point,'' defined as the point at which the disparity between highest and lowest socioeconomic strata becomes larger as a result of differences in intervention efficacy, coverage or target population. The objective when calculating the equity tipping point is to gauge whether potential differences realistically exist. In the example of diabetes prevention, we sought to identify the point at which intervention coverage gaps resulted in a widened disparity in diabetes risk. To show this better, we did not vary intervention efficacy or target population criteria.
We examined 2 types of diabetes prevention interventions that have well-established efficacy: lifestyle interventions and pharmacotherapy.Footnote 7 Lifestyle interventions reduce obesity through diet and exercise programs. Pharmacotherapy uses medications such as metformin to reduce weight and insulin resistance so as to reduce new cases of diabetes among those at risk. While these therapies appear to be efficacious across socioeconomic groups,Footnote 7, Footnote 8 achieving high coverage for diabetes in particular and chronic diseases in general is a challengeFootnote 9, Footnote 10 and the level of coverage likely varies across socioeconomic groups. However, we are unaware of any data about intervention coverage by SEP for diabetes prevention.
We estimated the equity tipping point in 2 steps. First, we calculated community effectiveness of lifestyle interventions and pharmacotherapy under a scenario of 100% coverage for all socioeconomic groups. This estimated the maximum or optimal reduction in diabetes disparity. Next, we incrementally reduced coverage in the lowest SEP until we reached the equity tipping point, or the point where there was no reduction in diabetes disparities.
Methods
The study was approved by the Research Ethics Board of Sunnybrook Health Sciences Centre, Toronto, Ontario. Figure 1 shows the steps taken to select an eligible target population and evaluate the impact of health interventions on socioeconomic disparities in diabetes risk.
FIGURE 1
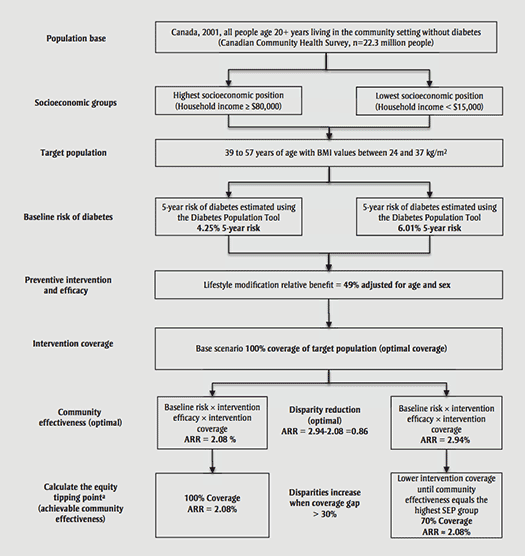
Process to estimate the community effectiveness and the equity tipping point of preventive interventions for diabetes (lifestyle modification or pharmacotherapy). Example of reducing disparities across income groups using lifestyle modification
[FIGURE 1, Text Equivalent]
Chronic Diseases and Injuries in Canada - Volume 34, Number 2-3, July 2014
FIGURE 1
Process to estimate the community effectiveness and the equity tipping point of preventive interventions for diabetes (lifestyle modification or pharmacotherapy). Example of reducing disparities across income groups using lifestyle modification
Figure 1 shows the steps taken to select an eligible target population and evaluate the impact of health interventions on socioeconomic disparities in diabetes risk, as explained in the text of the article.
Abbreviations: ARR, absolute risk reduction; BMI, body mass index.
a The reduction in coverage (and/or baseline risk, efficacy or target population) where there is equal effectiveness between groups.
Data sources and cohort selection
We used data from the 2005 Canadian Community Health Survey (CCHS) to obtain Canadians' self-reported diabetes status, SEP and other diabetes-related risk factors (n = 107 212, unweighted). The CCHS is a cross-sectional, population-based and nationally representative survey with self-reported information on health status and health determinants.Footnote 11 We identified all diabetes-free and non-pregnant Canadian adults from the CCHS.
Target population
We defined the target population for the preventive interventions using information from a meta-analysis of 17 efficacy studies that examined therapies that prevent or delay diabetes in adults.Footnote 7 Reflecting the range of participants' mean age and body mass index (BMI) from these 17 studies, we defined the target population as people aged 39 to 57 years with BMI values between 24 and 37 kg/m2.The studies included in the meta-analysis showed the same efficacy in a wide range of populations and socioeconomic settings.
Baseline risk of developing diabetes
The five-year (2005–2010) baseline risk of diabetes by level of SEP was calculated using the Diabetes Population Risk Tool (DPoRT), a validated risk prediction algorithm.Footnote 12 We further evaluated the predictive accuracy of DPoRT for this study and found that diabetes incidence can be predicted with discrimination and accuracy across socioeconomic groups (see supplementary online appendix).
Preventive intervention efficacy
The intervention meta-analysis reported a 5-year pooled hazard ratio (HR) of 0.51 (95% CI: 0.44–0.60) for lifestyle interventions and of 0.70 (95% CI: 0.62–0.79) for medication interventions, demonstrating relative treatment effects of 49% and 30%, respectively. The meta-analysis did not examine whether efficacy varied by SEP.
Community effectiveness analyses
Using household income and respondent education as indicators of SEP, we calculated diabetes risk (and absolute risk reduction [ARR]) across SEP groups for baseline and post-intervention scenarios assuming 100% coverage. ARR was defined as the absolute difference between baseline and post-intervention diabetes risk. We defined disparity as the absolute difference in diabetes risk between the lowest and highest SEP groups. We then compared the baseline disparity to the post-intervention disparity to determine the absolute reduction. Finally, we examined how disparity was affected by suboptimal intervention coverage. For ease of interpretation, we explored this scenario by maintaining widespread coverage among the highest SEP groups and varying the coverage among the lowest SEP groups. We calculated the equity tipping point by recalculating the ARR for the lowest SEP groups as we varied coverage, until we reached the same ARR as the highest SEP groups.
Results
Table 1 compares the baseline characteristics of adults in the target and non-target groups. The target population was predominantly male, and by definition, included mainly overweight or obese adults. The target population represented 32.8% of 22.3 million Canadians adults without diabetes.
TABLE 1
Baseline demographic, socioeconomic and anthropometric characteristics of diabetes-free adults, ≥ 20 years, Canadian Community Health Survey, 2005Table 1 - Footnote a
| Characteristic |
Target populationTable 1 - Footnote b |
Non-target population |
(N = 7 100 000)
% |
(N = 15 200 000)
% |
| Sex |
|
|
| Men |
60.1 |
43.4 |
| Women |
40.0 |
56.6 |
| Age, years |
| 20–34 |
— |
41.5 |
| 35–44 |
41.5 |
13.1 |
| 45–54 |
41.1 |
10.7 |
| 55–64 |
17.4 |
12.8 |
| ≥ 65 |
— |
21.9 |
| Household income, $ |
| < 15 000 |
3.5 |
6.4 |
| 15 000–29 999 |
7.1 |
15.1 |
| 30 000–49 999 |
16.8 |
21.6 |
| 50 000–79 999 |
29.1 |
26.3 |
| ≥ 80 000 |
43.4 |
30.6 |
| Education |
| < Secondary school |
12.2 |
17.1 |
| Secondary school graduate |
16.3 |
15.8 |
| Some post-secondary school |
6.8 |
9.2 |
| Post-secondary school graduate |
64.7 |
57.9 |
| Employment status |
| Yes |
88.1 |
74.8 |
| No |
11.9 |
25.2 |
| Ethnicity |
| Non-white |
13.8 |
17.3 |
| White |
86.2 |
82.7 |
| Immigrant |
| Yes |
20.8 |
22.8 |
| No |
79.2 |
77.2 |
| BMI, kg/m2 |
| Underweight (<18.50) |
— |
3.9 |
| Normal weight (18.50–24.99) |
20.6 |
61.1 |
| Overweight (25.00–29.99) |
57.2 |
23.6 |
| Obese (≥ 30) |
22.2 |
11.4 |
The 5-year baseline risk of diabetes for Canada, 2001, was 4.78%. The risk of diabetes declined with increase in SEP, from 6.01% among the lowest income earners to 4.25% among the highest, demonstrating a baseline disparity of 1.76% between the lowest SEP and highest SEP groups. Table 2 shows the predicted risk of developing diabetes across socioeconomic strata, BMI and other demographic factors.
TABLE 2
Five-year baseline risk and predicted number of new diabetes cases in the
target population,Table 2 - Footnote a 2005–2010
| Characteristic |
Target populationa |
| Number of cases,Table 2 - Footnote b n |
Mean risk, % |
|
|
| Overall |
323 000 |
4.78 |
| Sex |
| Men |
193 000 |
4.77 |
| Women |
130 000 |
4.80 |
| Age, years |
| 20–34 |
— |
— |
| 35–44 |
63 500 |
2.26 |
| 45–54 |
181 000 |
6.40 |
| 55–64 |
79 000 |
6.63 |
| ≥ 65 |
— |
— |
| Household income, $ |
| < 15 000 |
11 800 |
6.01 |
| 15 000–29 999 |
24 700 |
5.55 |
| 30 000–49 999 |
53 800 |
5.05 |
| 50 000–79 999 |
85 700 |
4.59 |
| ≥ 80 000 |
118 000 |
4.25 |
| Education |
| < Secondary school |
55 300 |
6.82 |
| Secondary school graduate |
62 300 |
5.60 |
| Some post-secondary school |
22 000 |
4.53 |
| Post-secondary school graduate |
184 000 |
4.10 |
| Employment status |
| Yes |
272 000 |
4.54 |
| No |
48 800 |
6.21 |
| Ethnicity |
| Non-white |
68 900 |
7.39 |
| White |
255 000 |
4.50 |
| Immigrant |
| Yes |
87 100 |
5.87 |
| No |
236 000 |
4.63 |
| BMI (kg/m2) |
| Underweight (< 18.50) |
— |
— |
| Normal weight (18.50–24.99) |
30 500 |
2.05 |
| Overweight (25.00–29.99) |
153 000 |
3.81 |
| Obese (≥ 30) |
140 000 |
9.19 |
Table 3 shows how complete coverage of lifestyle or pharmacological interventions affected socioeconomic disparities in diabetes risk. The ARR associated with a lifestyle intervention was 2.34%. This reduced the disparity between the lowest and highest income earners from 1.76% to 0.90%. With pharmacotherapy, the ARR was 1.43%, which narrowed the disparity from 1.76% to 1.24%. Benefit can also be reported in terms of total cases of diabetes prevented in Canada (144 000 cases prevented with lifestyle interventions vs. 88 100 cases prevented with pharmacotherapy). There were fewer cases of diabetes prevented in the lower SEP strata compared to the highest strata, reflecting a smaller number of people in the low SEP strata (see Tables 1 and 2).
TABLE 3
Impact of optimal (100%) coverage of lifestyle and pharmacological interventions on the disparity in diabetes risk
| Household income, $ |
< 15 000 |
15 000–29 999 |
30 000–49 999 |
50 000–79 999 |
≥ 80 000 |
Overall |
DisparityTable 3 - Footnote a |
Absolute disparity reductionTable 3 - Footnote b |
|
|
| Baseline risk of diabetes, % |
6.01 |
5.55 |
5.05 |
4.59 |
4.25 |
4.78 |
1.76 |
— |
| Lifestyle intervention |
| Absolute risk reduction,Table 3 - Footnote c % |
2.94 |
2.72 |
2.47 |
2.25 |
2.08 |
2.34 |
0.90 |
0.86 |
| Cases preventedTable 3 - Footnote d, n |
5760 |
12 100 |
26 400 |
42 000 |
57 600 |
144 000 |
|
|
| Pharmacological intervention |
| Absolute risk reductionTable 3 - Footnote c, % |
1.80 |
1.67 |
1.52 |
1.38 |
1.28 |
1.43 |
1.24 |
0.52 |
| Cases preventedTable 3 - Footnote d, n |
3530 |
7420 |
16 100 |
25 700 |
35 300 |
88 100 |
|
|
| Education |
< Secondary school |
Secondary school graduate |
Some postsecondary school |
Post-secondary graduate |
Overall |
DisparityTable 3 - Footnote a |
Absolute disparity reductionTable 3 - Footnote b |
| Baseline risk of diabetes, % |
6.82 |
5.60 |
4.53 |
4.10 |
4.78 |
2.72 |
— |
| Lifestyle intervention |
| Absolute risk reduction,Table 3 - Footnote c % |
3.34 |
2.74 |
2.22 |
2.01 |
2.34 |
1.39 |
1.33 |
| Cases preventedTable 3 - Footnote d, n |
27 100 |
30 500 |
10 800 |
90 100 |
159 000 |
|
|
| Pharmacological intervention |
| Absolute risk reduction,Table 3 - Footnote c % |
2.05 |
1.68 |
1.36 |
1.23 |
1.43 |
1.90 |
0.82 |
| Cases preventedTable 3 - Footnote d, n |
16 600 |
18 700 |
6610 |
55 200 |
97 000 |
|
|
Figure 2 shows how the complete coverage of health interventions affects diabetes risk disparities across different levels of income and education. As expected, the disparity widens when the intervention coverage drops in the lowest SEP groups, but is maintained at 100% for the highest SEP groups. The equity tipping point is reached at 70% coverage for lowest income earners and 60% for lowest education groups. Below these coverage levels, there is progressive widening of diabetes risk between SEP groups.
FIGURE 2
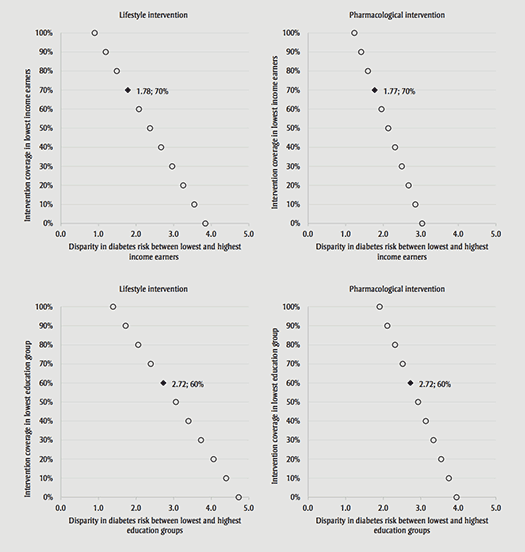
Estimating the impact of intervention coverage on the disparity in diabetes risk and identifying the equity tipping point for lifestyle and pharmacological interventions
[FIGURE 2, Text Equivalent]
Chronic Diseases and Injuries in Canada - Volume 34, Number 2-3, July 2014
FIGURE 2
Estimating the impact of intervention coverage on the disparity in diabetes risk and identifying the equity tipping point for lifestyle and pharmacological interventions
Figure 2 shows how the complete coverage of health interventions affects diabetes risk disparities across different levels of income and education. As expected, the disparity widens when the intervention coverage drops in the lowest SEP groups, but is maintained at 100% for the highest SEP groups. The equity tipping point is reached at 70% coverage for lowest income earners and 60% for lowest education groups. Below these coverage levels, there is progressive widening of diabetes risk between SEP groups.
Note: These scenarios assume 100% coverage in the highest socioeconomic group and varying coverage among the lowest socioeconomic group.
Discussion
Our study presents a straightforward modelling approach to estimate the potential reduction in socioeconomic disparities in disease risk using individual preventive interventions. In the considerable debate about whether individual interventions can or should have a role for reducing health disparities, the discussion is typically buttressed with either theoretical arguments or examples from specific studies or populations.Footnote 13, Footnote 14 In practice, most preventive interventions—whether they are individual-based or community-wide—have the potential to narrow or widen health disparities depending on the extent of disparities in baseline risk, intervention efficacy and intervention coverage. The ability to analytically examine the settings in which preventive interventions will likely narrow or widen health disparities is helpful for practical health planning and for more general discussions about disease prevention.
RoseFootnote 15 rightly indicated that an understanding of absolute measures of risk is a cornerstone of population health planning. However, the limitations of Rose's approach for evaluation of equity issues have been much debated.Footnote 6, Footnote 13, Footnote 16 Tugwell et al.Footnote 4 outlined a framework for considering equity issues when evaluating health policies. The modelling approach used here is similar to the ''effectiveness equity loop'' described by Tugwell et al.,Footnote 4 except that our calculations were specific to preventive interventions and used a multivariate risk tool to estimate baseline risk. As a measure the equity tipping point is also analogous to threshold or sensitivity analyses in economic studies where there is uncertainty or variation in costing of components and estimates of effectiveness.Footnote 17, Footnote 18
We varied only one component of community effectiveness—coverage—to examine its effect on the equity tipping point. We chose this variable because of concerns that coverage varies considerably across socioeconomic groups and because lower coverage of diabetes preventive therapies has been observed in low-income communities.Footnote 19 Intervention uptake is influenced by a complex array of individual, provider and health system factors—attitudes, language and cultural barriers, trust in the health care system, quality of the communication relationship and continuity of careFootnote 9, Footnote 10, Footnote 20, Footnote 21, Footnote 22—all of which can have varied effects on intervention coverage.
As expected, we found that when intervention coverage decreased among those in the lowest SEP group, so did the ARR. We further demonstrated the potential for poor coverage to exacerbate baseline disparity in diabetes risk when the intervention coverage surpasses the equity tipping point. At this threshold, the difference in intervention coverage voided any equity benefit of the health intervention and led to an increased disparity in diabetes risk. In an attempt to explain this predicted effect, others have theorized that health interventions may increase disparities if advantaged groups are more likely than their poorer, less educated and unemployed counterparts to have the financial and knowledge resources to capitalize on available opportunities to improve health.Footnote 13, Footnote 23 However, Anderson et al.Footnote 1 raised 2 relevant points:
- the steeper the initial gradient in baseline risk, the larger the effect that suboptimal coverage would have to exert in order to annul the potential for health interventions to reduce health disparities; and
- intervention coverage is responsive to policy action and, given the larger ARR associated with lower SEP, efforts can be productively focused on improving intervention coverage in this population group in order to reduce disparities.
Strengths and limitations
The use of a self-reported population health survey to define the study population provided both strengths and limitations in our community effectiveness calculations. One strength was the ability to calculate baseline risk of diabetes across key indicators of SEP using a population-based multivariate risk algorithm. These algorithms use individual data from population health surveys and are the most discriminating approach to estimate baseline risk.Footnote 6 The use of a population health survey also allowed flexibility in examining different SEP strata and target populations. Indeed, most components of community effectiveness could be varied for individual survey respondents, allowing a wide range of sensitivity analyses. We varied intervention efficacy based on age and BMI, but could have also varied it based on other attributes. Similarly, we varied coverage based on SEP strata, but it would have been straightforward to vary coverage on other respondent characteristics.
Our findings were based on the assumption that the relative benefit of lifestyle and pharmacological interventions for people at risk of diabetes was constant across SEP. Future applications of the modelling approach we have described would be strengthened by examining the effect of varying intervention effectiveness across SEP. However, there is some evidence to suggest diabetes prevention is equally efficacious—in relative terms—across SEP strata. For example, the Diabetes Prevention Program Research Group showed similar preventive benefit in all racial and ethnic groups in a study base of 27 centres across the United States.Footnote 8 The studies reviewed by Gillies et al.Footnote 7 were conducted in a wide range of community and ethnic settings worldwide with no heterogeneity identified. Second, lifestyle interventions have been shown to be comparatively effective, although with lower coverage, in low-income groups.Footnote 24 Finally, few studies and reviews have examined intervention efficacy differences across SEP strata. To address this important evidence gap, the Cochrane and Campbell Collaborations recently called for greater inclusion of equity in reviews and have provided a framework to facilitate the process.Footnote 25
Conclusion
The community effectiveness of a preventive intervention can be calculated using a simple model that considers target population size, baseline risk of disease, intervention efficacy and intervention coverage. The potential for interventions to reduce inequities can be estimated when community effectiveness is calculated for different socioeconomic strata. However, a current challenge is the lack of information on achievable levels of coverage and/or likely differences in target populations and intervention efficacy. Sensitivity analyses can be performed to estimate the equity tipping point, the setting where the intervention effect changes from reducing inequities to perversely increasing disparities in disease risk. Such sensitivity analyses can vary the expected coverage or other components of community effectiveness to examine their plausible influence and strengthen the evidence on the potential for reducing health inequities through individual-based prevention strategies.
Acknowledgments
We thank Dr. Michael J. Pencina, Boston University, for providing the SAS macro for calculating survival-based calibration and discrimination in order to conduct the validation analysis (found in the supplementary online appendix). Douglas G. Manuel holds a Chair in Applied Public Health from the Canadian Institute for Health Research and the Public Health Agency of Canada. John Lynch is supported by an Australian Fellowship from the National Health and Medical Research Council (NHMRC). The study was funded by the Canadian Institutes for Health Research and the Population Health Improvement Research Network of the Ontario Ministry of Health and Long-Term Care (MOHLTC). This study was supported by the Institute for Clinical Evaluative Sciences (ICES), which is funded by an annual grant from MOHLTC. The opinions, results and conclusions reported in this paper are those of the authors and are independent from the funding sources. No endorsement by ICES or the Ontario MOHLTC is intended or should be inferred.
References