At-a-glance – What can paramedic data tell us about the opioid crisis in Canada?
Health Promotion and Chronic Disease Prevention in Canada
Minh T. Do, PhDFootnote 1Footnote 2Footnote 3; Greg Furlong, ACPFootnote 4; Micah Rietschlin, PCPFootnote 4; Matthew Leyenaar, MAFootnote 5; Michael NolanFootnote 6; Pierre Poirier, MBAFootnote 7; Brian Field, MBAFootnote 8; Wendy Thompson, MScFootnote 1
https://doi.org/10.24095/hpcdp.38.9.06
Author references:
- Author reference 1
-
Public Health Agency of Canada, Ottawa, ON, Canada
- Author reference 2
-
Dalla Lana School of Public Health, University of Toronto, Toronto, Ontario, Canada
- Author reference 3
-
Department of Health Science, Carleton University, Ottawa, Ontario, Canada
- Author reference 4
-
Ottawa Paramedic Service, Ottawa, Ontario, Canada
- Author reference 5
-
McMaster University, Hamilton, Ontario, Canada
- Author reference 6
-
Renfrew County Paramedic Service, Renfrew, Ontario, Canada
- Author reference 7
-
Paramedic Association of Canada, Ottawa, Ontario, Canada
- Author reference 8
-
Interdev Inc., Toronto, Ontario, Canada
Corresponding author: Minh T. Do, Surveillance and Epidemiology Division, Public Health Agency of Canada, 785 Carling Avenue, Ottawa, ON K1A 0K9; Tel: 613-797-7587; Fax: 613-941-2057; Email: minht.do@canada.ca
Abstract
The nature of Canada’s opioid crisis necessitates additional data sources that can provide a more comprehensive picture of the epidemic, in order to provide public health officials and decision-makers with a robust evidence base. Paramedic data provide a conduit into the community where overdoses occur.
Prehospital events and circumstances surrounding opioid-related overdoses provide unique opportunities to collect evidence that can contribute to prevention, harm reduction and health promotion efforts. Using data extracted from the Ottawa Paramedic Service (OPS), this proof-of-concept study demonstrated that paramedic response data were useful in providing near real-time epidemiological information (person, time and place) on the opioid epidemic and in assessing trends and opportunities to develop alert triggers.
Between January and June 2017, the OPS responded to an average of four opioid-related calls each week. On average, 0.5 mg of naloxone was administered each time. For the study period, linear trends show a small but insignificant increase in calls (p = 0.18). A higher volume of calls occurred between April 16 and 29, 2017. According to local media reports, this spike in paramedic responses was due to the arrival of high-grade fentanyl in Ottawa.
With further validation, paramedic data can potentially provide a novel data source to monitor opioid-related overdoses.
Keywords: opioids, paramedic, prehospital care, early warning system, Canada
Highlights
- Paramedic data can provide prehospital information that could be used in the systematic monitoring and detection of sudden changes in the number of opioid-related events community.
- As some of the people who overdose are not transported to hospitals, the paramedic record may offer the only medical record of their overdose event.
- In this proof-of-concept study, significant spikes in the number of paramedic responses to opioid-related events were detected in advance of media reports about the arrival of high-grade fentanyl arriving in Ottawa, Canada.
Introduction
Canada is in the midst of an opioid epidemic. In some parts of the country, the number of deaths has been increasing,Footnote 1 with little sign of the crisis abating. In 2016, a total of 2861 deaths were attributed to apparent opioid use.Footnote 1 This number is expected to increase to more than 4000 in 2017 if the current trend continues.Footnote 1
In response, resources have been mobilized to closely monitor the epidemic. For example, as a result of the collaboration between the provinces and territories, lag times for documenting opioid-related death data have been significantly reduced. Similarly, enhanced surveillance of emergency department visits has also been implemented. In Ontario, hospitals are required to report opioid-related emergency department visits on a weekly basis.Footnote 2 However, despite the coordinated public health response, there remains a data gap for the systematic monitoring of overdoses occurring in communities across the country.
In Canada, paramedics are usually the first health care professionals to arrive on the scene of an overdose event. It is routine practice for the paramedics to collect information about the circumstances of the overdose. In most jurisdictions, these “prehospital” data are entered into an electronic system within 24 hours of the event. Such information could be invaluable in providing context for understanding the opioid crisis. As such, the objective of this proof-of-concept study is to determine whether paramedic data can be routinely used for public health monitoring purposes.
Methods
The Ottawa Paramedic Service (OPS) collates data from dispatches to medical emergencies in the city of Ottawa (population approximately one million in an area of 2796 square kilometres). The OPS collects information on patient characteristics, the nature of the emergency response and the treatment, if provided, for example, the dose of naloxone administered.
For this proof-of-concept study, data collected between 1 January 2017 and 17 June 2017 were extracted from the OPS on 27 June 2017. Although geocoding information was available (i.e. location of overdose by address, full postal codes), these data were not shown for privacy reasons.
Statistical methods
We used anonymous and aggregate data in this analysis. An opioid-related event is defined as a response requiring administration of naloxone to counteract the effects of an opioid-related overdose. Due to small cell counts, events were reported on a weekly basis and aggregated into 5-year age groups. Descriptive statistics were conducted to examine distributions of events.
As part of a trend analysis, an alert threshold was computed. A 7-week moving average was used to compute stable expected values. Given the count nature of the data, a Poisson distribution was used to compute the 95% confidence interval (CI) around the expected value.Footnote 3 Statistical cutoffs (α = 0.05) were arbitrarily used to define alert thresholds. An Excel macro-enabled template produced by the European Centre for Disease Prevention and Control (ECDC) was used for the analyses.Footnote 3 The number of paramedic responses exceeding the upper bounds was considered a threshold event or a departure from the expected range, and required further investigation (i.e. alert level).
Results
Between 1 January 2017 and 17 June 2017, there were 86 paramedic responses to opioid-related overdoses that required administration of naloxone. An average dose of 0.5 mg of naloxone was administered each time. Two-thirds (66%) of the cases were males, and 57% of all cases were between 25 and 39 years of age (mode: 30–34 years).
Linear trends show a small but insignificant increase in the number of weekly paramedic responses (p = 0.18). During the study period, the OPS received an average of four calls per week. The numbers of responses exceeded threshold levels between April 16 and April 29 (Figure 1). The highest number of calls was received during week 17 (23–29 April, 2017), when nine calls resulted in naloxone administration by paramedics. The spike in the number of calls was reported by local print and broadcast/online mediaFootnote 4Footnote 5 and in social media one week later.Footnote 6
Figure 1. Distribution of observed and expected values and the 95% confidence interval threshold limits for number of paramedic responses by the Ottawa Paramedic Service to opioid-related overdoses requiring naloxone, 1 January 2017 to 17 June 2017, Ottawa, Canada
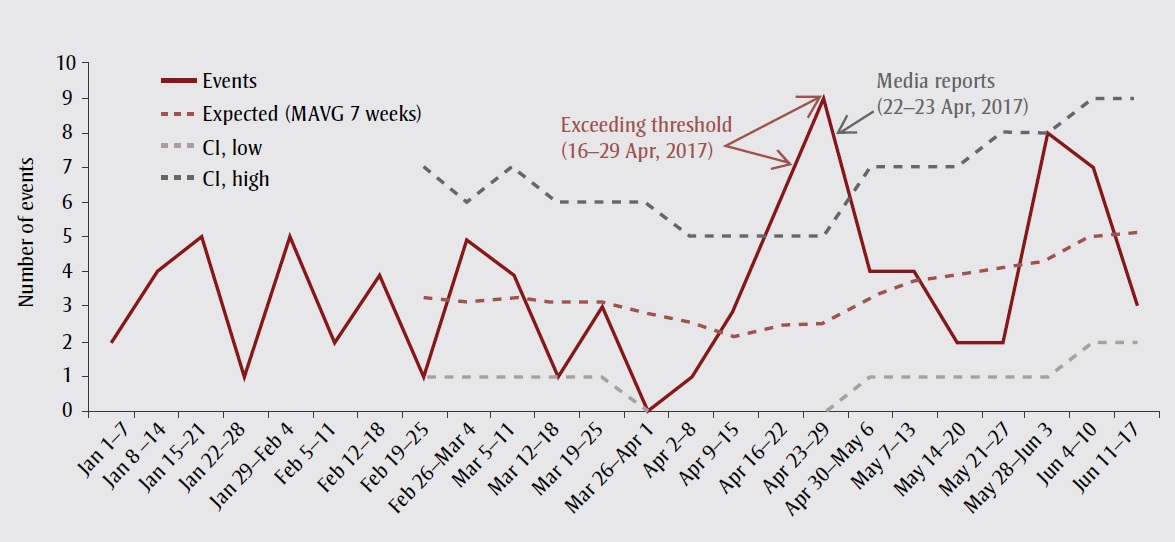
Abbreviations: CI, confidence interval; MAVG, moving average.
Text Description
| Date | Events | Expected (moving average 7 weeks) | Confidence interval, low | Confidence interval, high |
|---|---|---|---|---|
| Jan 1-7 | 2 | N/A | N/A | N/A |
| Jan 8 -14 | 4 | N/A | N/A | N/A |
| Jan 15-21 | 5 | N/A | N/A | N/A |
| Jan 22-28 | 1 | N/A | N/A | N/A |
| Jan 29- Feb 4 | 5 | N/A | N/A | N/A |
| Feb 5-11 | 2 | N/A | N/A | N/A |
| Feb 12 -18 | 4 | N/A | N/A | N/A |
| Feb 19 -25 | 1 | 3.29 | 1 | 7 |
| Feb 26 - Mar 4 | 5 | 3.14 | 1 | 6 |
| Mar 5 -11 | 4 | 3.29 | 1 | 7 |
| Mar 12 - 18 | 1 | 3.14 | 1 | 6 |
| Mar 19 -25 | 3 | 3.14 | 1 | 6 |
| Mar 26- Apr 1 | 0 | 2.86 | 0 | 6 |
| Apr 2 -8 | 1 | 2.57 | 0 | 5 |
| Apr 9 -15 | 3 | 2.14 | 0 | 5 |
| Apr 16 -22 | 6 | 2.43 | 0 | 5 |
| Apr 23 - 29 | 9 | 2.57 | 0 | 5 |
| Apr 30 - May 6 | 4 | 3.29 | 1 | 7 |
| May 7 - 14 | 4 | 3.71 | 1 | 7 |
| May 14-20 | 2 | 3.86 | 1 | 7 |
| May 21 - 27 | 2 | 4.14 | 1 | 8 |
| May 28 - Jun 3 | 8 | 4.29 | 1 | 8 |
| Jun 4-Jun 10 | 7 | 5 | 2 | 9 |
| Jun 11-Jun 17 | 3 | 5.14 | 2 | 9 |
Discussion
The purpose of this study was to evaluate whether paramedic response data can be used to monitor the opioid crisis. Public health surveillance is defined as the “systematic and continuous collection, analysis, and interpretation of data, closely integrated with the timely and coherent dissemination of the results and assessment to those who have the right to know so that action can be taken.”Footnote 7 In this context, the systematic collection of data by the OPS provided epidemiological information on person, place and time—information necessary for public health surveillance.
This information is consistent with what is known about the opioid crisis in Canada. Most of the paramedic responses (66%) involved opioid-related overdoses by males, which is similar to mortality data (74% of apparent opioid-related deaths occurred among menFootnote 1). Likewise, both prehospital (paramedic response data) and hospital data (emergency department visits and hospital admissions data) indicate that young adults are at high risk of opioid-related overdoses.Footnote 8 The ongoing collection of OPS data also provided opportunities to evaluate trends, with spikes exceeding statistical thresholds in advance of media reports. This lead-time health intelligence could prove to be invaluable for public health action.
In most parts of Canada, response data are entered into electronic databases within 24 hours of paramedics responding to an emergency event. This makes the data accessible for near real-time analysis and thus appropriate for contributing to an early warning systems.
Secondly, paramedic response data are geocoded (data not shown), as paramedics require an exact location in order to respond to an event. Accurate geographically indexed information would be available for public health surveillance to help identify hotspots and generate heat maps. Thirdly, as some individuals who overdose are not transported to hospitals, the paramedic record may be the only record of an overdose.
Finally, paramedic response data can be used to evaluate the impact of a particular public health policy or intervention. For example, the policy of making naloxone kits available to the general public without prescriptions may result in fewer individuals being transported to emergency departments because naloxone reverses the effects of the opioid-related overdose. Since the paramedic service has broad coverage and is active in most municipalities in Canada, there is the potential to provide a national picture of the opioid crisis.
Despite these advantages from the perspective of public health surveillance, there are limitations to using paramedic response data. These include the different infrastructure, prioritizing mechanisms and case definitions of opioid-related overdoses used by providers of paramedic services. In some jurisdictions, data on paramedic services are available at the provincial level, whereas in others such data are only available at the municipal level. Therefore, data quality needs to be evaluated for consistency, accuracy and precision.
From a national perspective, while pooling paramedic data in order to get a national picture would be desirable, comparing opioid-related overdoses in different jurisdictions with different case definitions is not possible. To this end, case definitions would need to be harmonized before comparisons across jurisdictions could be made. Alternatively, it would be valuable to be able to examine changes in trends as a way of monitoring the opioid crisis. There is also the potential to misclassify opioid-related events (for example, individuals who experience an opioid-related overdose may not be given naloxone and therefore would not meet the case definition).
Another consideration is that paramedics may not be called to attend all opioid-related overdoses in the community, so OPS data may fail to capture a proportion of overdoses.
In this study, we used a statistical cutoff (α = 0.05) to establish the alert threshold. It was an arbitrary decision to demonstrate a proof-of-concept. Depending on the context, a less conservative statistical threshold (e.g. α = 0.1) or a clinical cutoff could also be established.
Conclusion
Paramedic response data can provide prehospital information that has the potential to be used for systematic monitoring and detection of sudden changes in the number of opioid-related events in a community. In this proof-of-concept study, significant spikes in paramedic responses to opioid-related events in Ottawa were detected in advance of media reports. With further validation, paramedic response data can potentially provide a novel data source for monitoring public health events such as those related to opioid-related overdoses.
Authors’ contributions and statement
MD designed, analyzed and interpreted the data and drafted and revised the paper; GF and MR interpreted the data and drafted and revised the paper; ML analyzed and interpreted the data and revised the paper; MN, PP, BF and WT interpreted the data and revised the paper.
The content and views expressed in this article are those of the authors and do not necessarily reflect those of the Government of Canada.
References
- Footnote 1
-
Public Health Agency of Canada, Special Advisory Committee on the Epidemic of Opioid Overdoses. National report: Apparent opioid-related deaths in Canada (December 2017) [Internet]. Ottawa (ON): Government of Canada; 2017 [cited 2018 Feb 15]. https://www.canada.ca/en/public-health/services/publications/healthy-living/apparent-opioid-related-deaths-report-2016-2017-december.html
- Footnote 2
-
Canadian Institute for Health Information. NACRS ED reporting for opioid overdose. Bulletin. Ottawa (ON): CIHI; 2017 Feb 1 [cited 2018 Feb 15]. Available from: https://www.oha.com/Bulletins/NACRS%20ED%20Opioid%20Reporting%20Bulletin_Feb2017.pdf
- Footnote 3
-
European Centre for Disease Prevention and Control. Handbook on implementing syndromic surveillance in migrant reception/detention centres and other refugee settings. Stockholm (SE): ECDC; 2016.
- Footnote 4
-
CBC News. Spike in Ottawa drug overdoses continues through weekend [Internet]. Canadian Broadcasting Corporation. 2017 Apr 24 [cited 2018 Feb 15]. Available from: www.cbc.ca/news/canada/ottawa/drug-overdose-ottawa-hospital-1.4082752
- Footnote 5
-
Duffy A. Surge in overdoses feared as more fentanyl arrives in Ottawa [Internet]. Ottawa Citizen. 2017 Apr 23 [cited 2018 Feb 15]. Available from: http://ottawacitizen.com/news/local-news/six-more-opioid-overdose-victims-treated-at-the-ottawa-hospital
- Footnote 6
-
@DUAL Ottawa. High grade fentanyl influx in Ottawa people PLEASE be safe!!! And carry Nalozone!!! 2017 Apr 21. Available from: https://twitter.com/DUALOttawa?ref_src=twsrc%5Etfw&ref_url=http%3A%2F%2Fottawacitizen.com%2Fnews%2Flocal-news%2Fsix-more-opioid-overdose-victims-treated-at-the-ottawa-hospital
- Footnote 7
-
Porta M, editor. A dictionary of epidemiology, 6th edition. International Epidemiological Association, Inc. New York (NY): Oxford University Press; 2014.
- Footnote 8
-
Canadian Institute for Health Information. Opioid-related harms in Canada. Ottawa (ON): CIHI; 2017.