Original quantitative research – Adolescents’ adoption of COVID-19 preventive measures during the first months of the pandemic: what led to early adoption?

HPCDP Journal Home
Published by: The Public Health Agency of Canada
Date published: August 2021
ISSN: 2368-738X
Submit a manuscript
About HPCDP
Browse
Previous | Table of Contents | Next
Claude Bacque Dion, MAAuthor reference footnote 1; Richard Bélanger, MDAuthor reference footnote 1Author reference footnote 2; Scott T. Leatherdale, PhDAuthor reference footnote 4; Slim Haddad, MD, PhDAuthor reference footnote 1Author reference footnote 3
https://doi.org/10.24095/hpcdp.41.12.03
(Published 25 August 2021)
This article has been peer reviewed.
Author references
Correspondence
Claude Bacque Dion, Projet COMPASS-Québec, Centre de recherche VITAM, CIUSSCN et Université Laval C.P. GMF-U Maizerets, 2480 chemin de la Canardière, Québec City, QC G1J 2G1; Tel: 418-663-5313 ext. 12202; Email: claude.bacque-dion.ciussscn@ssss.gouv.qc.ca
Suggested citation
Bacque Dion C, Bélanger R, Leatherdale ST, Haddad S. Adolescents' adoption of COVID-19 preventive measures during the first months of the pandemic: what led to early adoption? Health Promot Chronic Dis Prev Can. 2021; 41(12):423-30. https://doi.org/10.24095/hpcdp.41.12.03
Abstract
Introduction: The objectives of this study were to explore the extent to which adolescents adopted COVID-19 preventive measures in the first few months of the pandemic and to understand their adoption by looking at interconnected adoption-related factors and determining the strength of these factors, particularly among subgroups not expected to be early adopters.
Methods: Analyses focus on data collected during Spring 2020 from 29 eastern Quebec secondary schools that participated in the COMPASS study. Participants (n = 6052) self-reported their knowledge, perception of risk and preventive practices to do with the COVID-19 pandemic. Data were analyzed using structural equation models based on gender and anxiety level.
Results: The majority of respondents reported adopting the recommended COVID-19 preventive measures. The results showed three paths leading to adolescents' adoption of these measures: pandemic knowledge; perception of risk related to COVID-19; and, in particular, discussions with relatives about preventive measures and what to do in case of infection.
Conclusions: While most of the adolescent participants in this study appeared to comply with COVID-19 preventive measures, factors such as discussions with relatives emerge as elements to foster in order to improve adolescents' adoption of preventive measures.
Keywords: adolescents, youth, COVID-19, adoption of preventive measures, structural equation modelling, SEM
Highlights
- Adolescents' compliance of COVID-19 preventive measures is high, even in subgroups with lower adoption rates.
- In addition to accurate pandemic knowledge and proper risk perception, discussions with relatives should also be considered as a means of improving adoption of COVID-19 preventive measures by adolescents.
Introduction
Emerging evidence suggests that the health effects of COVID-19 infection tend to be less strong in children, including adolescents, than in adults.Footnote 1Footnote 2Footnote 3Footnote 4 Still, youth populations contribute to the spread of COVID-19 through school-based outbreaks and household transmission.Footnote 5Footnote 6 Because some studies identified youth as a population with potentially low compliance with COVID-19 infection preventive measures,Footnote 7Footnote 8 it is imperative to understand which youth were early adopters of the preventive measures, and what drove them to adopt the measures in order to design effective awareness campaigns that target this population.
Recent studies show that perception of risk contributes to adults' intention of adopting COVID-19 preventive measures.Footnote 9 Health-related stress also affects preventive behaviours.Footnote 10 The degree of knowledge about the epidemic also drives individual adoption of preventive measures, with knowledge about the transmission and gravity of the disease factors motivating adults' behaviours.Footnote 9
How these factors are associated with adolescents' adoption of preventive measures is currently unknown. Yet this information is critical when developing messages targeting youth, particularly in subpopulations known to be less likely to follow preventive measures, such as males and individuals reporting lower anxiety levels.Footnote 11Footnote 12
Using surveillance data collected from youth attending secondary schools in Quebec during the early stages of the COVID-19 pandemic (April–May 2020), our aim was to determine:
- the extent to which youth adopted COVID-19 preventive measures early on;
- how implementation of preventive measures can be explained via interconnected factors that are likely to predict their adoption; and
- if adoption of COVID-19 preventive measures and the relation to these interconnected adoption-related factors differ based on gender and anxiety level.
Methods
Survey design and study population
The present study is based on data collected in the province of Quebec as part of the COMPASS (Cannabis, Obesity, Mental health, Physical activity, Alcohol, Smoking, Sedentary behaviour) study (https://uwaterloo.ca/compass-system/).Footnote 13 COMPASS is a longitudinal multicentre study of adolescent life in Canada. School surveys have been conducted annually in three regions of the province of Quebec since the Spring of 2017, in partnership with the school communities and the regional public health departments. During the 2019/20 data collection cycle, the COVID-19 pandemic forced the closure of Quebec schools for in-person learning on 16 March 2020, and the COMPASS team transitioned its tools from paper-based within-school data collection protocols to online data collections using Qualtrics XM (Seattle, WA, USA).
Data collection occurred between March and May 2020.
The study population includes all students in the 5 years of the secondary level (equivalent to Grades 7 to 11 in the USA and the rest of Canada) of 29 Eastern Quebec secondary schools who had not already completed inputting their data for the 2019/20 data collection cycle before the pandemic-related school closures. Of the 16 748 solicited adolescents, 6052 (36.1%) answered the online questionnaire. Parents' refusal rate was less than 1% (108 participants).
Informed consent
The COMPASS protocol involves active-information passive-consent parental permission procedures. Students could decline to participate at any time.
Ethics approval
All procedures involving human participants were in accordance with the ethical standards of the institutional and/or provincial research committee and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards. All procedures in the COMPASS study received ethics approval from the University of Waterloo Research Ethics Board (ORE 30118), as well from the Research Ethics Review Board of the Centre intégré universitaire de santé et de services sociaux de la Capitale-Nationale (#MP-13-2017-1264) and participating school board review panels.
Ethics approval was obtained to include additional measures pertaining to youth respondents' knowledge, attitudes and behaviours to do with the COVID-19 pandemic.Footnote 14
Measures
One new component of the online questionnaire referred to adolescents' knowledge, perception of risk and practices in relation to the COVID-19 pandemic.Footnote 14 Most questions were adapted from a questionnaire developed by the World Health Organization (WHO) and information provided on the WHO website.Footnote 15Footnote 16Footnote 17 Items extracted from the WHO questionnaire were translated, adapted and pretested by the COMPASS research team.
Dependent variable: adoption of COVID-19 preventive measures
Adoption of COVID-19 preventive measures was determined based on responses to a set of five questions about the measures that were in place at the time of data collection. We asked study participants to report how frequently they had, since pandemic-related restrictions began (1) avoided gatherings and public places; (2) cancelled non-essential meetings; (3) washed their hands more often than previously; (4) disinfected often-touched objects; (5) and avoided coughing in public. Respondents could choose from three answers: "always," "sometimes" or "never." The "adoption score" is a continuous variable ranging from 0 to 10, with 10 representing the highest level of adoption of these five preventive measures (Cronbach α = 0.62).
Factors linked to the adoption of COVID-19 preventive measures
Four factors that could be related to the adoption of preventive measures were preselected based on the current (albeit limited) literature and some key elements of the Health Belief ModelFootnote 18: pandemic knowledge; perception of risk of COVID-19 for youths; worries about the COVID-19 pandemic; and discussions in relation to COVID-19 with relatives.
Pandemic knowledge was determined using a set of 17 questions that were based on health facts about COVID-19 disease transmission and symptoms as reported by WHOFootnote 17. Participants were asked if they believe each fact to be true, choosing yes/no responses. The "pandemic knowledge score" is a continuous variable ranging from 0 to 17, with 17 representing the highest level of knowledge (Cronbach α = 0.78).
Perception of risk of COVID-19 to youths was assessed based on agreement with a single statement: "I think that COVID-19 represents very little risk of complications to young people." Participants chose possible responses on a 5-point scale from true to false. The answers were subsequently recoded into three categories: (1) true; (2) mostly true; and (3) neutral, mostly false and false. The "perception of risk score" is a continuous variable ranging from 0 to 2, where 0 is equivalent to the perception that COVID-19 represents very little risk to youths (answer choices 1 and 2).
Worries about the COVID-19 pandemic were determined using a set of five questions of the worry battery. Participants were asked about their worries about the current circumstances; their personal health; their family members' health; and their stress level. Response options ranged from 0 (true) to 4 (false). The "worries score" is a continuous variable ranging from 0 to 20, with 20 representing the highest level of worry (Cronbach α = 0.77).
Discussions in relation to COVID-19 with relatives were determined based on agreement with two statements: (1) "I discussed measures to prevent infection with family, friends and/or health care professionals"; and (2) "I discussed what to do in case of infection with family, friends and/or health care providers." For both statements, respondents could choose one of three answers: "always," "sometimes" or "never." The "discussions score" is a continuous variable ranging from 0 to 4, with 4 equivalent to the highest level of discussions with relatives about COVID-19 preventive measures and what to do in case of infection (Cronbach α = 0.78).
Other variables
Participants were asked to report their gender, choosing from one of four options: "female"; "male"; "I describe my gender in a different way"; or "I prefer not to say." Based on the responses, we classified participants as "female" or "other."
Anxiety level was determined via the Generalized Anxiety Disorder 7-item scale (GAD-7)Footnote 19 questionnaire. The recommended cut point for further evaluation of generalized anxiety is a score of 10; those with a score of 9 or less are characterized as less anxious, and those with a score of 10 or higher as more anxious.
Each participant's age was determined through the question "How old are you today?", with response options 12 years or younger, 13 years, 14 years, 15 years, 16 years, 17 years, 18 years, or 19 years and older.
Statistical analyses
We used structural equation models to explore how adoption of preventive measures was linked to pandemic knowledge, perception, worries and discussions with relatives. The influences of these factors are known to be interconnected, and adoption is therefore conceptualized as the result of a complex non-linear causal process.Footnote 18 Structural equation modelling (SEM) is the standard approach to empirically address these kinds of issues.
Estimating was initiated using a preliminary statistical model derived from the literature and the Health Belief ModelFootnote 18 (see Figure 1). The fit of the initial model was not satisfactory and various iterations were completed to adjust the model and improve the goodness of fit, eventually leading to the final model (see Figure 2). Full information maximum likelihood method was used to control for missing data. Robust estimators accounted for the hierarchical structure of the data (respondents clustered in schools). Goodness of fit was assessed based on commonly accepted standards: (1) the model that minimizes the Bayesian Information Criterion (BIC) / Akaike Information Criterion (AIC) estimator; (2) root mean square error of approximation (RMSEA) below .05; (3) Tucker-Lewis index (TLI) and comparative fit index (CFI) as close to 1 as possible.Footnote 20 Statistical differences in group comparisons are shown by the confidence intervals of the mean differences.
Figure 1. Hypothesized model of the relationship between pandemic knowledge, perception of risk to youths, discussions with relatives, worries and adoption of COVID-19 preventive measuresFigure 1 Footnote a
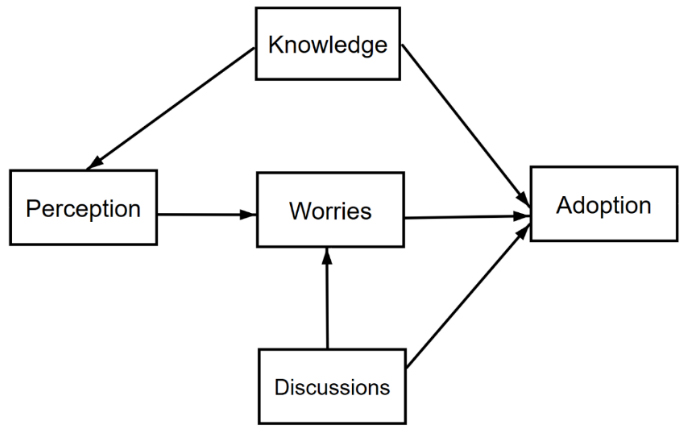
- Figure 1 Footnote a
-
Goodness of fit indices: χ2 = <.001; root mean square error of approximation (RMSEA) = .223; comparative fit index (CFI) = .416; Tucker-Lewis index (TLI) = −.314.
Text Description
This figure illustrates a complex, non-linear causal preliminary statistical model derived from the literature and the Health Belief Model18 used to estimate how adoption of preventive measures is linked to knowledge, perception, worries and discussions with relatives.
Based on the gender and anxiety level of the participants, we created four subgroups: more anxious females; less anxious females; more anxious others; and less anxious others. Socioeconomic status was considered to be a possible confounder in the preliminary analysis, but was found to have no influence on model estimators and was not retained in the final model.
All analyses were performed with STATA version 15.1 SEM routine (StataCorp, College Station, TX, US). The SEM group routine was used to allow model parameters to vary across the four subgroups.
Results
Of the 6052 participants, 60% (n = 3553) were female and 33% (n = 3413) had an anxiety score of 10 or higher. Mean age was 14.6 years. The majority reported having adopted preventive measures during the first months of the pandemic (Table 1). In fact, more than 9 out of 10 participants reported washing their hands more often and avoided coughing in public, while more than 8 out of 10 reported avoiding social gatherings and public places and cancelling non-essential meetings/gatherings. Over two-thirds of the respondents cleaned and disinfected frequently touched objects. Cronbach α was 0.62, suggesting a moderate level of covariation in the adoption of the measures.
| Sample | COVID-19 preventive measure, % (n) | ||||
|---|---|---|---|---|---|
| Wash hands more often | Avoid coughing in public | Avoid gatherings and public places | Cancel meetings | Disinfect frequently touched objects | |
| All (n = 6052) | 94 (4705) | 93 (4659) | 89 (4423) | 83 (4168) | 74 (3703) |
| Gender | |||||
| Female (n = 3553) | 95 (2915) | 95 (2891) | 91 (2761) | 87 (2654) | 78 (2392) |
| Other (n = 2408) | 92 (1780) | 91 (1758) | 86 (1654) | 78 (1504) | 68 (1306) |
| Anxiety level | |||||
| More anxious (n = 3413) | 93 (1491) | 92 (1475) | 87 (1397) | 81 (1304) | 75 (1211) |
| Less anxious (n = 1717) | 95 (3107) | 94 (3076) | 89 (2921) | 84 (2764) | 74 (2411) |
More female participants than other participants adopted all five preventive measures; the differences were statistically significant (p < 0.05). Effects of anxiety levels did not differ statistically significantly except for cancelling non-essential meetings/gatherings (p < 0.05).
Gender and anxiety level affected mean pandemic knowledge, worries and adoption scores (see Table 2). Female participants have higher mean worries scores than do other participants. In addition, compared with other adolescents, female participants have a higher mean pandemic knowledge score and mean adoption score. These same patterns are observed when comparing female participants and others based on anxiety level.
| Sample | Mean scores (95% confidence interval) | ||||
|---|---|---|---|---|---|
| Perception of riskTable 2 Footnote a | Pandemic knowledgeTable 2 Footnote b | WorriesTable 2 Footnote c | DiscussionsTable 2 Footnote d | AdoptionTable 2 Footnote e | |
| All | 0.79 (0.77 to 0.82) | 10.82 (10.75 to 10.90) | 6.44 (6.32 to 6.56) | 1.92 (1.89 to 1.96) | 7.05 (6.99 to 7.11) |
| Gender | |||||
| Female | 0.72 (0.69 to 0.75) | 11.21 (11.12 to 11.30) | 7.14 (6.98 to 7.29) | 2.01 (1.96 to 2.06) | 7.33 (7.26 to 7.39) |
| Other | 0.91 (0.87 to 0.95) | 10.21 (10.08 to 10.34) | 5.36 (5.18 to 5.54) | 1.79 (1.73 to 1.85) | 6.61 (6.51 to 6.71) |
| Differences | −0.19 (−0.24 to −0.14) | 1.00 (0.85 to 1.15) | 1.77 (1.53 to 2.01) | 0.22 (0.14 to 0.30) | 0.71 (0.59 to 0.83) |
| Anxiety level | |||||
| More anxious | 0.81 (0.77 to 0.85) | 10.67 (10.53 to 10.81) | 6.77 (6.53 to 7.00) | 1.93 (1.86 to 2.00) | 7.05 (6.94 to 7.16) |
| Less anxious | 0.79 (0.76 to 0.82) | 10.93 (10.85 to 11.02) | 6.26 (6.12 to 6.39) | 1.92 (1.87 to 1.97) | 7.05 (6.98 to 7.12) |
| Differences | 0.02 (−0.03 to 0.07) | −0.26 (−0.42 to −0.10) | 0.51 (0.25 to 0.77) | 0.01 (−0.07 to 0.09) | −0.01 (−0.13 to 0.12) |
| More anxious | |||||
| Female | 0.73 (0.67 to 0.79) | 11.19 (11.03 to 11.34) | 7.70 (7.39 to 8.00) | 2.00 (1.91 to 2.09) | 7.36 (7.23 to 7.48) |
| Other | 0.93 (0.86 to 1.00) | 9.90 (9.65 to 10.15) | 5.38 (5.04 to 5.73) | 1.83 (1.72 to 1.94) | 6.58 (6.38 to 6.78) |
| Differences | −0.20 (−0.29 to −0.11) | 1.29 (1.01 to 1.57) | 2.31 (1.85 to 2.78) | 0.17 (0.03 to 0.31) | 0.78 (0.55 to 1.00) |
| Less anxious | |||||
| Female | 0.72 (0.68 to 0.75) | 11.25 (11.14 to 11.35) | 6.85 (6.67 to 7.03) | 2.02 (1.96 to 2.08) | 7.31 (7.22 to 7.39) |
| Other | 0.91 (0.86 to 0.96) | 10.43 (10.28 to 10.58) | 5.31 (5.10 to 5.51) | 1.77 (1.69 to 1.84) | 6.65 (6.53 to 6.77) |
| Differences | −0.19 (−0.25 to −0.13) | 0.82 (0.64 to 1.00) | 1.55 (1.27 to 1.83) | 0.25 (0.15 to 0.35) | 0.65 (0.51 to 0.79) |
|
|||||
The results of the stratified SEM analyses showed three paths leading to adolescents' adoption of COVID-19 preventive measures (Figure 2). First, pandemic knowledge has a statistically significant direct effect on adoption except for more anxious females. Second, discussions with relatives have a statistically significant total effect, indirectly through worries, on all adoption, especially by more anxious others. Of all the factors, this one has the strongest effect on adoption by all groups. Third, perception of risk has a significant negative indirect effect on adoption through worries. We were able to confirm that more than 93% of participants worried about the health of their family members versus 44% for their own health (further information and data available on request from the authors).
Figure 2. Structural equation analyses of adoption and its related factors, by gender and anxiety level, showing standardized parameter coefficientsFigure 2 Footnote a
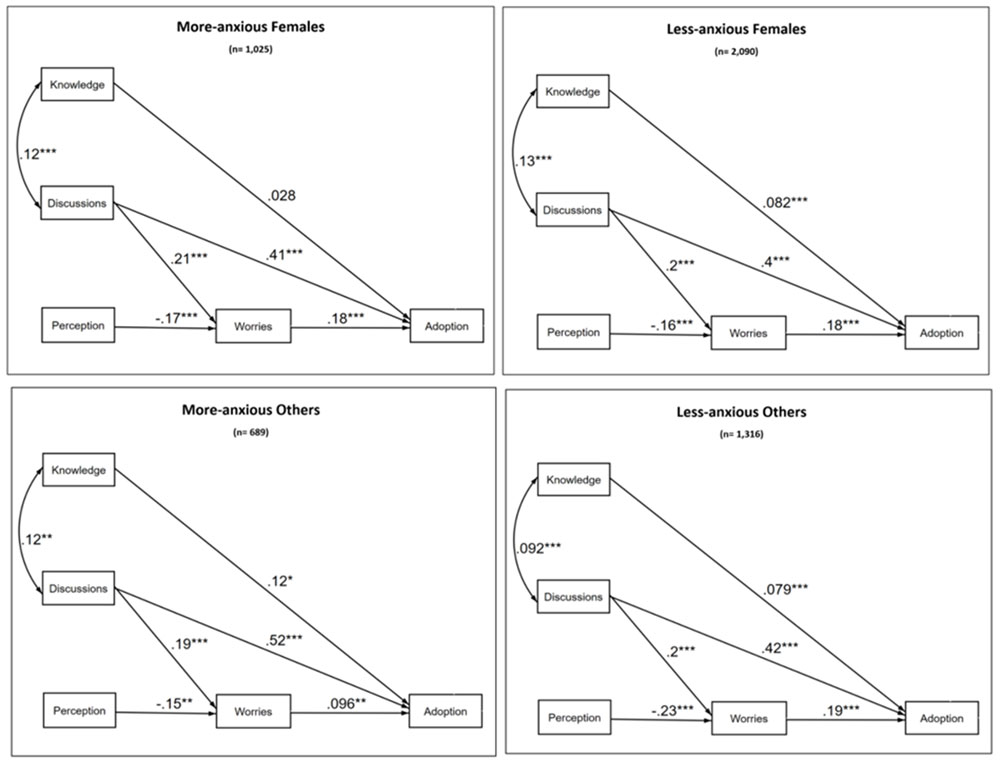
- Figure 2 Footnote a
-
Goodness of fit indices: χ2 = <.001; root mean square error of approximation (RMSEA) = .223; comparative fit index (CFI) = .416; Tucker-Lewis index (TLI) = −.314.
- * p < .05.
- ** p > .01.
- *** p ≤ .001.
- Note: Age variable has been omitted.
Text Description
This figure illustrates the final model used to estimate how adoption of preventive measures is linked to knowledge, perception, worries and discussions with relatives. There are 4 complex, non-linear causal models stratified by the following groups: More-anxious Females (n=1 025), Less-anxious Females (n=2 090), More-anxious Others (n=689) and Less-anxious Others (n=1 316). Standardized parameter coefficients are shown for 3 paths leading to adolescent's early adoption of COVID-19 preventive measures.
Knowledge and discussions are interrelated (More-anxious Females (0.12***), Less-anxious Females (0.13***), More-anxious Others (0.12**) and Less-anxious Others (0.092***)). Both directly lead to adoption. Pandemic knowledge has a statistically significant direct effect on adoption except for more anxious females (More-anxious Females (0.28), Less-anxious Females (0.082***), More-anxious Others (0.12*) and Less-anxious Others (0.079***)). Discussions also have a statistically significant direct effect on adoption for all groups (More-anxious Females (0.41***), Less-anxious Females (0.4***), More-anxious Others (0.52***) and Less-anxious Others (0.42***). Discussions also have a statistically significant direct influence on worries (More-anxious Females (0.21***), Less-anxious Females (0.2***), More-anxious Others (0.19***) and Less-anxious Others (0.2***)). Discussions with relatives have a statistically significant total effect, indirectly through worries, on all adoption, especially by more anxious others (More-anxious Females (0.18***), Less-anxious Females (0.18***), More-anxious Others (0.096**) and Less-anxious Others (0.19***)). Perception of risk has a significant negative indirect effect on adoption through worries (More-anxious Females (-0.17***), Less-anxious Females (-0.16***), More-anxious Others (-0.15***) and Less-anxious Others (-0.23***)).
These effects are stable in all four groups. The only group where age has a statistically significant negative effect is on less anxious others (data available on request from the authors). The model also suggests that some unmeasured factors statistically significantly influence the association between the knowledge of the pandemic and the discussions with relatives. SEM analysis of the entire sample show similar results in regard to the three observed paths (data available on request from the authors).
Discussion
Our study results show that the majority of adolescents were early adopters of the main protective measures against COVID-19 infection, that is, handwashing, disinfecting frequently touched objects, avoiding coughing in public, avoiding gatherings and public places and cancelling non-essential meetings. In contrast to young adults who report low compliance rates with adopting preventive measures,Footnote 7 studies addressing adolescents' adoption depict a more nuanced portrait. Dardas et al. (2020),Footnote 12 in their study of Jordanian high-school students' COVID-19 preventive practices, found that adolescents reported positive disinfecting behaviours and adequate social distancing and avoided crowded places and social gatherings; however, 40% of their sample did not practise correct hand washing and mask wearing. Similar results were also obtained in a study of Italian high-school students' practices.Footnote 21
At the time of data collection, health authorities had not yet recommended mask wearing as a COVID-19 preventive measure. The results from the next data collection (Spring 2021) will help verify whether adolescents continued to apply the various preventive measures including mask wearing.
Knowledge about the pandemic, perception of risk of COVID-19, worries about the pandemic and discussions with relatives were all significantly related to adoption of COVID-19 prevention measures. Our results highlighted three paths in the pattern of associations to adoption. First, adoption appears to be significantly if indirectly related to a higher perceived risk. Second, except for more anxious females, there is a significant direct link between knowledge and adoption.
The third path links discussions with relatives to adoption. Here too, a direct link coexists with an indirect link mediated by worries, especially on more anxious others. Adolescence is a time where friends are very important and their opinions matter.Footnote 5 Adolescents are much more socially influenced by friends than by adults in engaging in prosocial behaviours.Footnote 22 Nonetheless, the impact of discussions between parents and adolescents have been shown to have an effect on condom use.Footnote 23 Promoting discussions with relatives in order to improve adolescents' adoption of COVID-19 preventive measures, if effective and accurate, may benefit compliance via a snowball effect. In fact, research has found peer-led interventions to be a way to increase adoption of preventive measures.Footnote 5
Most promotion campaigns aimed at influencing adolescent behaviour are based on increasing adolescents' knowledge and awareness of the health risks. Unfortunately, these interventions are predominantly adult led and often unsuccessful with adolescents.Footnote 24
Worrying was expected to influence adoption of preventive measures because higher anxiety levels are associated with increased use of COVID-19 preventive measures among adults.Footnote 25 It was also anticipated that this association would be influenced by the perception of risk and discussions with relatives. Nonetheless, our results showed that adolescents with a perception of higher risk of COVID-19 complications for youths are less worried about COVID-19 than peers without this perception of risk. A potential explanation may be that most adolescents do not worry about their own health but do worry about that of family members, some of whom may be are at greater risk. Adolescents discussing COVID-19 preventive measures and what to do in case of infection with relatives worry more as well. This could be because such discussions lead to a better understanding of the gravity of the situation and potential consequences on human health.
Even if the three adoption paths discussed mostly apply to the four subgroups analyzed, based on gender and anxiety level, model comparisons demonstrate certain nuances. As seen in previous studies, female adolescents tend to adopt more preventive measures than do their peers.Footnote 12Footnote 26Footnote 27 A possible explanation is that some of the factors that lead to adoption, such as a higher level of knowledge and worry, are particularly associated with females.Footnote 4Footnote 20Footnote 21Footnote 22Footnote 23Footnote 24Footnote 25Footnote 26Footnote 27Footnote 28 In fact, our results show that female adolescents have a higher levels of pandemic knowledge and worries (which is emphasized by a higher level of anxiety) than do their non-female peers.
If a main objective is to increase the adoption of preventive measures, a noteworthy finding is that anxiety in non-female adolescents influences the effects of the different factors that lead to adoption. Indeed, discussions in relation to COVID-19 with relatives have an even greater influence on more anxious non-females than on less anxious non-females. Patterns are similar for perception of risk, worries and pandemic knowledge. These findings shed light on the importance of not looking for a unique model to apply to everyone because gender and anxiety levels influence the adoption of preventive measures and their factors.
Strengths and limitations
This study has some limitations. First, the cross-sectional study design hampers the ability to infer potential causal relations; however, we can expect adoption of preventive measures to be influenced by constructs other than those investigated.
Second, because of school closures, completing an online questionnaire at home was the only possible way to collect data on adolescents' behaviours and their perceptions of risk. Consequently, the usual participation rate (above 90% in class) was strongly affected in some schools. A review of the literature on adolescents' participation rates in online health surveys usually round up to between 30% and 40% and demonstrate self-selection bias.Footnote 29
Third, the population of participating schools was based on schools from the eastern part of the province of Quebec. Thus, the study's conclusions may not reflect the reality in other regions and countries because of differences in severity and duration of pandemic-related restrictions.
Fourth, these results are derived from an exploratory analysis where replication needs to be assessed. Still, the large number of participants in this study provide significant information about the adoption of preventive measures by the adolescent population.
Finally, the COMPASS platform offers a unique opportunity to follow and analyze changes over time in adolescents' perceptions of and attitudes towards the COVID-19 pandemic as well as their acceptance and adoption of preventive measures.
Conclusions
Most of the adolescents participating in this study appear to have complied with the COVID-19 preventive measures—even those from population subgroups with lower adoption rates. While accurate pandemic knowledge and proper risk perception should be promoted among youths, policy makers and health care providers should also consider ways of promoting discussions with relatives as a way of improving adolescents' adoption of COVID-19 preventive measures.
The longitudinal nature of the COMPASS study will allow researchers to follow, over the long run, the evolution of adherence to preventive measures, the influences of changes in interconnected adoption-related factors, and the impact of specific interventions intended to influence them. Most importantly, further studies are needed to better disentangle these relations and explore how contextual, personal and policy aspects are intertwined and how to develop comprehensive and appropriate approaches to reinforce and sustain preventive measures among youth.
Acknowledgements
The authors wish to thank the Quebec public health authorities, participating schools, school boards and students and the COMPASS team, especially Rabi Joel Gansaonre, for their continued confidence in our team.
Funding sources
The COMPASS study has been supported by a bridge grant from the Canadian Institutes of Health Research (CIHR) Institute of Nutrition, Metabolism and Diabetes (INMD) through the "Obesity – Interventions to Prevent or Treat" priority funding awards (OOP-110788; awarded to SL); an operating grant from the CIHR Institute of Population and Public Health (IPPH) (MOP-114875; awarded to SL); a CIHR project grant (PJT-148562; awarded to SL); a CIHR bridge grant (PJT-149092; awarded to KP/SL); a CIHR project grant (PJT-159693; awarded to KP); and a research funding arrangement with Health Canada (#1617-HQ-000012; contract awarded to SL).
The COMPASS- Québec project also benefits from funding from the Ministère de la Santé et des Services sociaux and the Direction régionale de santé publique du CIUSSS de la Capitale-Nationale.
Conflicts of interest
The authors declare that they have no conflicts of interest.
Authors' contributions and statement
- CBD and SH conceptualized and conducted the analysis.
- CBD conducted the literature review.
- CBD led the writing and wrote the first draft.
- STL conceptualized and leads the larger COMPASS study where SH and RB are the COMPASS-Québec provincial leads.
All authors provided feedback on drafts and reviewed and approved the final manuscript.
The content and views expressed in this article are those of the authors and do not necessarily reflect those of the Government of Canada.
References
- Footnote 1
-
Kamenidou IE, Stavrianea A, Mamalis S, Mylona I. Knowledge assessment of covid-19 symptoms: gender differences and communication routes for the generation z cohort. Int J Environ Res Public Health. 2020;17(19):1-16. https://doi.org/10.3390/ijerph17196964
- Footnote 2
-
Le Saux N. L'épidémiologie à jour sur la COVID-19 (causée par le virus SARS-CoV-2) chez les enfants et les conseils s'y rapportant : mars 2020 [Internet]. Ottawa (ON): Canadian Paediatric Society; 2020 [cited 2020 Nov 05]. Available from: https://www.cps.ca/fr/documents/position/lepidemiologie-a-jour-sur-la-covid-19-causee-par-le-virus-sars-cov-2-chez-les-enfants-et-les-conseils-sy-rapportant-mars-2020
- Footnote 3
-
Shen K, Yang Y, Wang T, et al. Diagnosis, treatment, and prevention of 2019 novel coronavirus infection in children: experts' consensus statement. World J Pediatr. 2020;16(3):223-31. https://doi.org/10.1007/s12519-020-00343-7
- Footnote 4
-
Zimmermann P, Curtis N. Coronavirus infections in children including COVID-19: an overview of the epidemiology, clinical features, diagnosis, treatment and prevention options in children. Pediatr Infect Dis J. 2020;39(5):355-68. https://doi.org/10.1097/INF.0000000000002660
- Footnote 5
-
Andrews JL, Foulkes L, Blakemore SJ. Peer influence in adolescence: public-health implications for COVID-19. Trends Cogn Sci. 2020;24(8):585-7. https://doi.org/10.1016/j.tics.2020.05.001
- Footnote 6
-
Bénéteau-Burnat B, Baudin B, Morgant G, Baumann FC, Giboudeau J. Serum angiotensin-converting enzyme in healthy and sarcoidotic children: comparison with the reference interval for adults. Clin Chem. 1990;36(2):344-6. https://doi:10.1093/clinchem/36.2.344
- Footnote 7
-
Nivette A, Ribeaud D, Murray A, et al. Non-compliance with COVID-19-related public health measures among young adults in Switzerland: insights from a longitudinal cohort study. Soc Sci Med. 2021;268:113370. https://doi.org/10.1016/j.socscimed.2020.113370
- Footnote 8
-
UNESCO. COVID-19 pandemic: youth engaged in the #NextNormal [Internet]. Paris (FR): UNESCO;2020 [cited 2020 Nov 5]. Available from: https://en.unesco.org/news/covid-19-pandemic-youth-engaged-nextnormal
- Footnote 9
-
Ahmad M, Iram K, Jabeen G. Perception-based influence factors of intention to adopt COVID-19 epidemic prevention in China. Environ Res. 2020;190:109995. https://doi.org/10.1016/j.envres.2020.109995
- Footnote 10
-
Luo Y, Yao L, Zhou L, Yuan F, Zhong X. Factors influencing health behaviours during the coronavirus disease 2019 outbreak in China: an extended information-motivation-behaviour skills model. Public Health. 2020;185:298-305. https://doi.org/10.1016/j.puhe.2020.06.057
- Footnote 11
-
Asmundson GJ, Taylor S. How health anxiety influences responses to viral outbreaks like COVID-19: what all decision-makers, health authorities, and health care professionals need to know. J Anxiety Disord. 2020;71:102211. https://doi.org/10.1016/j.janxdis.2020.102211
- Footnote 12
-
Dardas LA, Khalaf I, Nabolsi M, Nassar O, Halasa S. Developing an understanding of adolescents' knowledge, attitudes, and practices toward COVID-19. J Sch Nurs. 2020;36(6):430-41. https://doi.org/10.1177/1059840520957069
- Footnote 13
-
Leatherdale ST, Brown, KS, Carson V, et al. The COMPASS study: a longitudinal hierarchical research platform for evaluating natural experiments related to changes in school-level programs, policies and built environment resources. BMC Public Health. 2014;14(1):1. https://doi.org/10.1186/1471-2458-14-331
- Footnote 14
-
Reel B, Battista K, Leatherdale ST. COMPASS protocol changes and recruitment for online survey implementation during the Covid-19 pandemic [Internet]. COMPASS Technical Report Series. Waterloo (ON): University of Waterloo; 2020 [cited 2021 Jan 11]. Available from: https://uwaterloo.ca/compass-system/publications/compass-protocol-changes-and-recruitment-online-survey
- Footnote 15
-
World Health Organization. Survey tool and guidance: rapid, simple, flexible behavioural insights on COVID-19, 29 July 2020 [Internet]. Document number: WHO/EURO:2020-696-40431-54222. Copenhagen (DK): WHO; 2020. Available from: https://apps.who.int/iris/bitstream/handle/10665/333549/WHO-EURO-2020-696-40431-54222-eng.pdf
- Footnote 16
-
World Health Organization. Coronavirus [Internet]. Geneva (CH): WHO; 2020 [cited 2020 Nov 05]. Available from: https://www.who.int/health-topics/coronavirus#tab=tab_3
- Footnote 17
-
World Health Organization. Rational use of personal protective equipment (PPE) for coronavirus disease (COVID-19): interim guidance, 19 March 2020 [Internet]. Geneva: World Health Organization; 2020 [cited 2020 Nov 05]. Available from: https://apps.who.int/iris/bitstream/handle/10665/331498/WHO-2019-nCoV-IPCPPE_use-2020.2-eng.pdf
- Footnote 18
-
Becker MH. The Health Belief Model and Sick Role Behavior. Health Educ Monogr. 1974;2(4):409-19. https://doi.org/10.1177/109019817400200407
- Footnote 19
-
Spitzer RL, Kroenke K, Williams JB, Löwe B. A brief measure for assessing generalized anxiety disorder: the GAD-7. Arch Intern Med. 2006;166(10):1092-7. https://doi.org/10.1001/archinte.166.10.1092
- Footnote 20
-
Hooper D, Coughlan JP, Mullen MR. Structural equation modeling: guidelines for determining model fit. Electron J Bus Res Methods. 2008;6(1):53-60.
- Footnote 21
-
Souli D, Dilucca M. Knowledge, attitude and practice of secondary school students toward COVID-19 epidemic in Italy: a cross selectional study. bioRxiv [Preprint]. 2020:2020.05.08.084236. https://doi.org/10.1101/2020.05.08.084236
- Footnote 22
-
Foulkes L, Leung JT, Fuhrmann D, Knoll LJ, Blakemore SJ. Age differences in the prosocial influence effect. Dev Sci. 2018;21(6):e12666. https://doi.org/10.1111/desc.12666
- Footnote 23
-
Hadley W, Brown LK, Lescano CM, et al.; Project STYLE Study Group. Parent-adolescent sexual communication: associations of condom use with condom discussions. AIDS Behav. 2009;13(5):997-1004. https://doi.org/10.1007/s10461-008-9468-z
- Footnote 24
-
Yeager DS, Dahl RE, Dweck CS. Why interventions to influence adolescent behavior often fail but could succeed. Perspect Psychol Sci. 2018;13(1):101-22. https://doi.org/10.1177/1745691617722620
- Footnote 25
-
Wong LP, Hung C-C, Alias H, Lee TS-H. Anxiety symptoms and preventive measures during the COVID-19 outbreak in Taiwan. BMC Psychiatry. 2020;20(1):376. https://doi.org/10.1186/s12888-020-02786-8
- Footnote 26
-
Erfani A, Shahriarirad R, Ranjbar K, Mirahmadizadeh A, Moghadami M. Knowledge, attitude and practice toward the novel coronavirus (COVID-19) outbreak: a population-based survey in Iran. Bull World Health Organ. 2020; 1-23. https://doi.org/10.2471/BLT.20.256651
- Footnote 27
-
Mak KK, Lai CM. Knowledge, risk perceptions, and preventive precautions among Hong Kong students during the 2009 influenza A (H1N1) pandemic. Am J Infect Control. 2012;40(3):273-5. https://doi.org/10.1016/j.ajic.2011.10.023
- Footnote 28
-
Kolifarhood G, Aghaali M, Mozafar Saadati H, et al. Epidemiological and clinical aspects of COVID-19; a narrative review. Arch Acad Emerg Med. 2020;8(1):e41.
- Footnote 29
-
Bennett L, Nair CS. A recipe for effective participation rates for web‐based surveys. Assess Eval High Educ. 2010;35(4):357-65. https://doi.org/10.1080/02602930802687752
