Priority strategies to optimize testing and screening in long-term care homes
This is the second report of the COVID-19 Testing and Screening Expert Advisory Panel. It was released on February 26, 2021.
On this page
- Executive summary
- The Advisory Panel and reports
- Preamble
- Address equity issues
- Implement a robust testing and screening strategy
- Address shortages in health staffing
- Undertake further research to inform testing and screening strategies
- Conclusion and next steps
- Annex 1: Key terms
- Annex 2: National examples of testing and screening in long-term care
Executive summary
In November 2020, the Minister of Health established the COVID-19 Testing and Screening Expert Advisory Panel. The Panel provides evidence-informed advice to the federal government on science and policy related to innovative and existing approaches to testing and screening.
The Expert Advisory Panel issued its first report Priority strategies to optimize testing and screening for COVID-19 in Canada in January 2021.
This second report provides evidence-based recommendations and case studies to help inform the development of testing and screening strategies in long-term care homes. As the first wave of COVID-19 in Canada began to subside in June 2020, residents of long-term care homes accounted for about 80% of all COVID-19-related deaths. Just over 8 months later, as the country faced a second COVID-19 wave, SARS-CoV-2 has again caused many deaths in Canada's long-term care homes.
There is a broad agreement that we must protect long-term care residents, staff and essential caregivers. This must be a national priority in the months and years to come.
Prioritizing the vaccination of long-term care residents and staff is expected to substantially reduce the risk of morbidity and mortality in this at-risk population. Rates of serious infection are falling as vaccine deployment continues.
Nonetheless, there will continue to be a need for robust testing and screening strategies in long-term care homes. It's possible that the need for screening may decrease. However, any changes to these strategies must consider vaccination rates, levels of community transmission, outbreak status and emerging evidence.
The recommendations in this report build on available guidance and standard procedures to protect long-term care residents and staff, with a specific focus on testing and screening for SARS-CoV-2. An example is the Public Health Agency of Canada's evidence-informed infection prevention and control guidelines and recommendations for use in long-term care homes. The Panel also recognizes that some provinces and territories are addressing testing and screening in long-term care homes.
For this report, the Panel considered:
- epidemiological trends
- public health measures
- SARS-CoV-2 variants of concern
- the rollout of vaccines in long-term care homes
As highlighted in our first report, no single best approach to testing and screening is appropriate for every long-term care home in Canada. Every strategy and response must reflect the circumstances of a specific long-term care home, including the availability of resources to support the testing and screening strategy.
The Panel acknowledges that staffing and test delivery remain issues at many long-term care homes. The ability of long-term care homes to manage frequent screening varies widely. Provincial and territorial support will be essential to implementation in some jurisdictions.
The Panel's recommendations focus on 4 priority areas for action:
- Address equity issues
- consider equity issues and accessibility in testing and screening strategies
- Implement a robust testing and screening strategy
- implement asymptomatic test-based screening for staff, essential caregivers and residents
- test new residents and screen visitors
- prioritize processing of samples from potential or confirmed outbreaks
- test individuals who have symptoms
- manage COVID-19 cases and test individuals who don't have symptoms
- Address shortages in health staffing
- explore options for staffing support to help implement testing and screening strategies
- Undertake further research to inform testing and screening strategies
- wastewater surveillance
- testing hesitancy
- effectiveness of test methodologies at detecting variants of concern and SARS-CoV-2 in a vaccinated population
The Advisory Panel and reports
Mandate of the Panel
The COVID-19 Testing and Screening Expert Advisory Panel aims to provide timely and relevant guidance to the Minister of Health on testing and screening for COVID-19. This advice is based on the best available science and data.
The Panel's mandate is to complement, not replace, evolving regulatory and clinical guidance regarding testing and screening. The Panel's reports are intended to be responsive to federal, provincial and territorial needs, as all governments seek opportunities to integrate new technologies into their COVID-19 response plans. The Panel recognizes that jurisdictions may choose to adopt some testing and screening strategies and not others based on the unique circumstances of each jurisdiction and evolving evidence.
Plan for reports
The focus of the first Panel report included 4 immediate actions to optimize testing and screening:
- optimize diagnostic capacity with lab-based PCR testing
- accelerate the use of rapid tests, primarily for screening
- address equity considerations for testing and screening programs
- improve communications strategies to enhance testing and screening uptake
This second report provides a more in-depth perspective of how these preliminary recommendations are considered in the long-term care home setting. Although the Panel's advice focuses on long-term care homes, it may also be applied to other communal settings, such as retirement, assisted living and group homes for people with disabilities.
Future reports will continue to provide a more detailed perspective in areas that are key to managing the ongoing pandemic, including schools.
Consultation
The Panel consulted with more than 60 health experts, public policy experts, long-term care experts and other stakeholders who are contributing to the COVID-19 response. We will continue to consult with a variety of stakeholders as the Panel prepares further reports.
Guiding principles
Public health initiatives benefit from incorporating principles to prevent unintended harm, promote equity and increase accountability. Panel discussions and engagement with stakeholders highlighted a number of key principles to consider in its guidance. These principles align with the framework outlined in the Canadian National Advisory Committee on Immunization guidance and are based on ethics, equity, feasibility and acceptability. The Panel applied these principles in framing its guidance.
Terms
Some of the terms used in the report may not be familiar to all readers. A glossary of terms is included in an annex for reference. For the purpose of this report, the Panel describes testing and screening as follows:
- Diagnostic test/testing: used to identify current infection in an individual and is performed when a person has signs or symptoms consistent with COVID-19, or has no symptoms but has had recent known or suspected exposure to SARS-CoV-2
- Screening test/screening: used to identify infected individuals who have no symptoms and without known or suspected exposure to SARS-CoV-2
Acknowledgements
The Panel expresses its appreciation to the ex officio members of the Panel and to officials at Health Canada who have been working tirelessly to support the Panel. The Panel also acknowledges the contributions of the "shadow panel" on testing and screening, a group of students and young scientists who provided expert research and analytical assistance. Shadow panel members include Michael Liu, Matthew Downer, Tingting Yan, Sara Rotenberg, Netra Unni Rajesh, Jane Cooper and Rahul Arora.
Sue Paish, Co-Chair
Dr. Irfan Dhalla, Co-Chair
Panel members:
- Dr. Isaac Bogoch
- Dr. Mel Krajden
- Dr. Jean Longtin
- Dr. Kwame McKenzie
- Dr. Kieran Moore
- Dr. David Naylor
- Domenic Pilla
- Dr. Brenda Wilson
- Dr. Verna Yiu
- Dr. Jennifer Zelmer
Preamble
As of February 2021, close to 14,000 long-term care and retirement home residents have died from COVID-19. This accounts for approximately 70% of all deaths from COVID-19. There have also been more than 3,600 outbreaks in long-term care homes, with approximately 60,000 cases of COVID-19 reported.
As of February 2021, more than 24,000 long-term care staff have contracted SARS-CoV-2 and 26 deaths have been reported. Many staff who work at these homes, including personal care workers, are female and racialized. Along with the devastating impact of SARS-CoV-2 on residents, staff and their families, the disproportionate effects of COVID-19 in long-term care settings also reveal systemic issues that affect those who work in this essential service.
While designed to protect the health of Canadians, COVID-19 public health measures have also had unintended but significant impacts on residents, families and staff. For residents, isolation and restrictions on essential caregivers, visitors and activities have led to significant stress, reduced quality of life, and significant morbidity and mortality. For families and staff, these prolonged restrictions have also caused stress and anxiety. Visitors are defined as any family member or close friend who is not an essential caregiver.
Many factors will influence testing and screening strategies, including vaccine effectiveness as it is better understood in the long-term care setting and high versus low community prevalence of the virus. They must also consider vaccination rates, SARS-CoV-2 variants of concern and outbreak status.
Vaccine campaigns in all provinces and territories have made the residents of long-term care homes a priority. While the rollout of vaccines is promising, there remain unknowns to determine the impact of vaccine uptake among residents, staff and essential caregivers. It will be critical to understand this impact and that of other factors when it comes to protecting residents of long-term care homes against COVID-19 and informing testing and screening strategies.
The principles of "Find, Test, Trace, Isolate, Support" remain key pillars of outbreak prevention in long-term care homes, both during vaccine roll-out and for a period still to be determined after vaccine deployment. These strategies will need to evolve based on real-world findings. However, we know that nimble and responsive testing and screening in long-term care will remain a keystone until public health indicates otherwise.
Address equity issues
To manage the spread of the virus in long-term care homes, we must address the systemic issues that increase the risk of staff and essential caregivers becoming infected and unknowingly introducing and spreading SARS-CoV-2. Many factors influence the risk of infection in staff, including socio-demographic factors, rates of pay and access to sick leave.
Long-term care staff are more likely to be employed part-time and with low pay, resulting in them needing to pursue secondary employment. For example, British Columbia and Alberta issued an order preventing all staff from working in multiple long-term care homes. Secondary employment may be financially necessary, but it can also increase the risk of COVID-19 transmission from other job settings and between long-term care homes. Banning secondary work may result in staff choosing to work in higher-paid over lower-paid long-term care homes. This can result in staffing problems at lower-paid long-term care homes, negatively impacting lower income residents. Fair compensation for long-term care staff is the best overall solution to many of these issues.
Lack of paid sick leave for many frontline staff is also a key factor contributing to hesitancy of getting tested, although this is inconsistent across the country. For example, a person with symptoms who tests positive for COVID-19 is told to isolate for at least 10 days from the onset of the first symptom. Over each 5 days of isolation, an individual who is paid $15 an hour and working full-time will lose $560 of income.
In addition, long-term care staff are often living in situations that put them at a higher risk of contracting COVID-19. For example, many live in neighbourhoods with lower socioeconomic status, higher rates of COVID-19 infection and in multi-generational households. Some have reported being unable to afford permanent housing and are forced to use a local shelter.
The lack of paid sick leave programs combined with low pay leads to staff working at multiple long-term care homes. This is linked with ongoing transmission in long-term care homes, as some workers must continue to work despite being exposed to or having symptoms. This is contrary to public health guidelines, which require individuals waiting for results and confirmed COVID-19 cases to isolate and quarantine.
Case study
A recent study found that the average personal support worker would need to work 50 hours a week to afford the current cost of living and renting in Toronto.
Equity considerations for asymptomatic testing also apply to essential caregivers who are often family members. Testing requirements that include out-of-pocket costs (for example, for transportation to a testing centre or for the test itself) for essential caregivers will have a disproportionate, negative effect on lower-income residents and their families. This added cost may also limit care and social interaction, which are key to maintaining the physical and mental health of residents.
The Panel acknowledges the critical need for short- and longer-term strategies to protect long-term care staff. These strategies include higher overall compensation and work protections, including paid sick days, which would allow them to properly and equitably follow public health guidance.
Implement a robust testing and screening strategy
As vaccines are rolled out in long-term care homes and in the broader community, it will be critical to maintain and update robust testing and screening strategies in long-term care homes. Such a strategy should be ongoing based on local public health guidance.
Current evidence suggests that a period following a complete vaccination series is required to develop optimal protection from COVID-19. Concurrently, turnover of staff, residents, essential caregivers, visitors and others may contribute to the introduction of SARS-CoV-2 and gaps in vaccine coverage. Finally, much remains unknown as to the duration of vaccine effectiveness and the real-world potential risks of variants of concern particularly in the high-risk population.
Testing and screening strategies should ideally include a combination of lab-based PCR and rapid testing to prevent outbreaks and increase protection for staff, essential caregivers and residents (see Figure 1). Some long-term care homes may face resource limitations that impact their ability to implement new testing and screening strategies. As a result, a one-size-fits-all approach across a province, territory or region is unlikely to be optimal given the unique needs of individual long-term care homes.
Testing and screening strategies may also need to be modified once more Canadians are immunized. For example, random screening of some staff and residents may replace universal screening. Eventually, it may be necessary to test only people who have symptoms and close contacts.
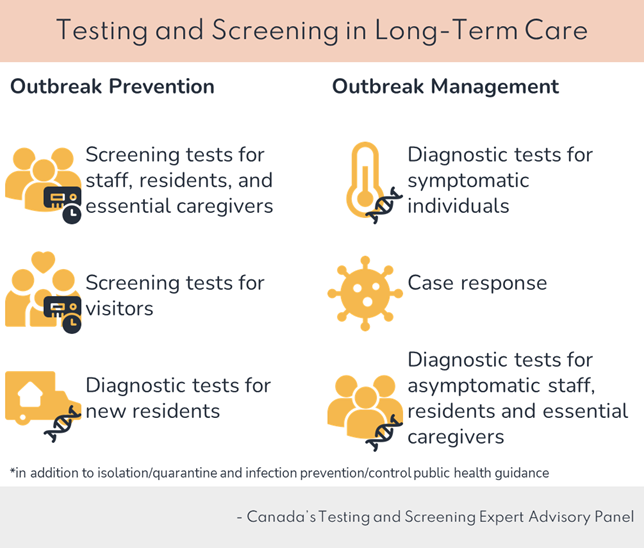
Long description:
Testing and screening strategies in long-term care have 2 portions: outbreak prevention and outbreak management. Under outbreak prevention, the strategy should include:
- screening tests for staff, residents and essential caregivers
- screening tests for visitors
- diagnostic tests for new residents
Under outbreak management, the strategy should include:
- diagnostic tests for symptomatic individuals
- case response
- diagnostic tests for asymptomatic staff, residents and essential caregivers
Diagnostic tests are lab-based PCR tests, while screening tests can also be point-of-care rapid tests. These strategies should be in addition to all public health guidance, including but not limited to isolation/quarantine and infection prevention/control recommendations. These recommendations are from Canada's Testing and Screening Expert Advisory Panel.
Implement asymptomatic test-based screening for staff, essential caregivers and residents
The risk of COVID-19 outbreaks in long-term care homes is linked to community transmission. Screening is therefore an important tool to prevent SARS-CoV-2 from being introduced into long-term care homes, especially in communities with high prevalence of COVID-19.
Screening involves regularly testing people who are unlikely to have COVID-19 (they do not have symptoms and no close contacts with someone who has COVID-19). It is important to screen, as people who are asymptomatic may be infectious for days before symptoms appear. They could also remain asymptomatic yet transmit the virus to others.
For screening strategies to be most effective, it is important to test people frequently, ensure rapid turnaround times for results and consider community prevalence.
Case study
An Ontario study found an association between the rate of infection in communities near long-term care homes and outbreaks in those homes. When daily active COVID-19 community cases are 2.3 per 100,000 people, there is a 75% greater chance of a long-term care home outbreak occurring 5 days later. This relationship can be used as an early warning indicator for establishing screening strategies.
Long-term care homes must be able to implement a COVID-19 screening strategy for staff, essential caregivers and residents that suits their environment and needs. Essential caregivers who are allowed entry under public health directives should undergo similar screening procedures as staff. This supports the ultimate goal of preventing the introduction of SARS-CoV-2 into the long-term care home.
Lab-based PCR tests are the 'gold standard' for testing due to their specificity and sensitivity at detecting SARS-CoV-2. Therefore, lab-based PCR with rapid turnaround could be considered the preferred approach for testing and screening this at-risk population. However, a successful screening program depends on rapid turnaround time, which is not always possible with lab-based PCR. Also, lab-based PCR tests are not readily available in some parts of the country. While there are reports of successful screening strategies using PCR with rapid turnaround times and limited impacts on long-term care staff, PCR-based screening strategies have not been effective in all long-term care settings. Examples of testing and screening strategies in long-term care homes from across the country are available in Annex 2.
As described in the Panel's first report, point-of-care (PoC) rapid tests, such as rapid antigen tests (RATs) and PoC PCR tests, allow for rapid turnaround times, many within 15 minutes to 1 hour. While not as sensitive as laboratory-based tests, when properly used most PoC tests may help to prevent the spread of COVID-19. Ontario recently announced that by mid-March 2021, everyone entering a "care home" must use a rapid test. However, some jurisdictions, such as Germany, have cited concerns about the high volume of rapid tests performed by already overburdened staff.
Each long-term care home should consider the pros and cons of various screening tools, as well as local testing and staff capacity, before implementing or changing a screening program. However, screening with either PoC PCR tests or RATs is strongly preferred over using solely symptom-based screening methods (for example a screening questionnaire), in the current pandemic context.
On-site sample collection in a designated area is preferred. Other options, for example mobile testing units, are also reasonable depending on the availability of staff, funding resources and current public health guidance.
The Panel recommends that testing and screening strategies for long-term care homes consider community prevalence, the vaccine status in residence and staff and evolving knowledge. A graded and responsive strategy with more frequent screening tests is recommended in high prevalence communities.
Until more evidence is available, the Panel also recommends that screening strategies continue to include vaccinated staff and residents (as well as people without symptoms). In part, this is because of uncertainties regarding SARS-CoV-2 variants of concern in the community. Integrating a robust screening strategy will likely require support to provide or build capacity in many long-term care homes. Where screening resources are limited, the Panel recommends screening unvaccinated staff, essential caregivers and residents first.
Different testing and screening strategies present different logistical considerations. Additionally, the long-term care sector is currently understaffed and over-extended. Long-term care homes that decide to proceed with a rapid test-based screening strategy will often benefit from support for development and implementation.
Finally, each long-term care home is unique. Thus, testing and screening strategies and responses must be specific to each. This requires periodic re-evaluation based on:
- vaccination rates, where screening could be:
- less frequent if rates are higher
- more frequent if rates are lower
- community prevalence, where screening strategies could:
- use PCR tests and be less frequent where prevalence is lower
- use PCR and rapid tests and be more frequent where prevalence is higher
- outbreak status, where:
- screening could be less frequent if no outbreak
- strategies could use PCR tests and more frequent screening if there's at least 1 positive case and then an outbreak
- variants of concern, with:
- more frequent screening if the variant is the common form of SARS-CoV-2 in the community
In First Nations, Inuit and Métis communities, the Panel emphasizes the need for consultation to develop Indigenous-led approaches, thus ensuring community needs are identified and met.
Case studies
Ontario: Maxville Manor piloted RATs to provide additional screening for essential caregivers beyond weekly PCR tests. This pilot successfully identified asymptomatic but infectious individuals who had not yet received an updated PCR test.
Manitoba: Manitoba launched a pilot project voluntarily screening asymptomatic staff in 3 retirement homes with the Abbott Panbio RAT. Staff members isolated while positive results were confirmed using PCR.
Test new residents and screen visitors
There's a risk that newly admitted residents may introduce SARS-CoV-2 into a long-term care home. Therefore, the Panel recommends that new residents receive a lab-based PCR test before and/or upon admission and be isolated in accordance with public health guidelines.
Many jurisdictions have restricted essential caregivers and other visitors in areas where community transmission is high. However, there's growing recognition that these restrictive policies negatively impact the mental and physical health of long-term care residents.
Essential caregivers and other visitors support the overall mental health and well-being of residents and often provide additional supportive care. Thus, it's important to develop an approach that balances the need to protect residents and staff from COVID-19 with the need for socialization and physical and emotional support from visitors. Requiring recent negative COVID-19 tests for visitors is standard practice in many long-term care homes. This practice should continue for now. Also, visitors should be screened by requiring either a negative result from a recent lab-based PCR test or using a rapid test on-site (for example, RAT or PoC PCR).
As more residents and staff are vaccinated and community transmission falls, it's reasonable that family members, particularly essential caregivers, will visit residents more frequently. Decisions to expand visitation policies must be made with consideration given to community prevalence, vaccine rates, outbreak status and variants of concern. The harms caused by isolation and reduced contact should also play into this. Expanding visits will require screening and testing of visitors until such time as public health guidance indicates otherwise.
At a minimum, visitors who do not come into close contact with residents or staff (for example, food delivery workers) should:
- be screened for symptoms
- follow all public health measures (for example, hand washing, personal protective equipment)
Prioritize processing of samples from potential or confirmed outbreaks
Our first report recommended creating higher- and lower-priority streams for specimen collection and testing when capacity is limited. In line with this recommendation, the Panel recommends that labs provide the results from long-term care homes as soon as possible, regardless of the home's vaccination status. Labs should also prioritize the processing of samples from homes that have potential or confirmed outbreaks.
Test symptomatic individuals
The Panel recommends that all symptomatic staff, residents, essential caregivers and close contacts (see the public health guidelines ) continue to be tested using lab-based PCR. They should follow public health guidance for isolation and quarantine requirements.
For a single confirmed case of COVID-19, regardless of the individual's vaccination status, the long-term care home should respond as if there's an outbreak. Working with its local public health team, the home should immediately limit the transmission of SARS-CoV-2. People who have been vaccinated fully should be assessed for loss of vaccine effectiveness, re-infection or potential infection with a variant of concern. Positive SARS-CoV-2 test results in vaccinated people suggest infection.
The Panel recommends that positive PCR tests in vaccinated individuals trigger genome sequencing to assess for variants of concern.
Manage COVID-19 cases and test asymptomatic individuals
Long-term care homes must have an outbreak management plan that outlines how to increase testing resources (tests, sample collection devices, human resources) in the event of an outbreak. The plan must clearly identify local expertise that can be made available in a timely and effective manner. When there's an outbreak, long-term care homes should continue to follow public health infection prevention and control guidance.
Until the outbreak ends, the Panel recommends that residents, staff, family, caregivers and non-essential visitors identified by contact tracing:
- be tested with PCR following exposure
- be re-tested regularly
- isolate according to public health guidelines
Regular screening tests can occur on-site or at a test centre, depending on resource availability.
These recommendations are in line with the Panel's first report and Canadian public health guidance.
In an outbreak situation, the Panel recommends testing asymptomatic staff and residents using lab-based PCR tests, including those in the home who are not close contacts. This is in accordance with public health guidance.
Case studies
Ontario: In a long-term care home in Ontario, almost all residents had COVID-19 within 3 weeks of a first case, with testing indicating the presence of the B.1.1.7 variant of concern. Other cases appeared shortly after in the community. The U.K. government estimates that variant B.1.1.7 has an attack rate of 10% to 55% higher than non-B.1.1.7 SARS-CoV-2.
Regardless of other contributing factors, this outbreak highlights the importance of ongoing frequent screening to detect even a single case of COVID-19. Frequent screening tests can help to prevent:
- outbreaks or minimize the size of an outbreak
- devastating impacts in the long-term care home and the community
Alberta: Alberta has been offering rapid testing at long-term care homes in Edmonton and other communities using mobile testing units. This is an expansion of the province's rapid COVID-19 testing program, which has tested over 1,000 Albertans. In a matter of hours, 76 people were notified of their positive results.
Address shortages in health staffing
Explore options for staffing support to assist with implementing testing and screening strategies
Due to the COVID-19 pandemic, many long-term care homes are facing significant staffing shortages and increased work demands. Where staffing capacity is impacting the implementation of robust testing and screening of residents and staff, long-term care homes and their community partners could consider:
- shifting testing, screening and contact tracing tasks to a wider variety of trained professionals
- accessing mobile teams to support testing and screening, where available and affordable
As recommended in our first report, shifting the screening and testing process to trained individuals presents an opportunity to reduce the strain on the health care workforce. This is especially important for long-term care homes that are already critically understaffed and overburdened during the pandemic.
U.K. field studies have found that RATs have higher sensitivity (73%; 95% confidence interval of 64% to 85%) when conducted by skilled research nurses compared to pharmacy test centre employees (58%; 95% confidence interval of 52% to 63%) following written instructions. It's therefore critical that staff who are conducting diagnostic and screening tests receive proper training.
The Panel understands that long-term care homes are experiencing challenges hiring additional staff. A national or regional approach is required to focus effort on developing innovative approaches to task-shifting. Such an approach may include:
- partnering with other trained professionals (for example, pharmacists, paramedics) to collect and/or process samples
- collaborating with the private sector to leverage employees who have been laid off temporarily or to address gaps (see the case studies below on the Nightingale Initiative and Creative Destruction Lab)
- establishing proactive partnerships between local health system partners and long-term care homes to ensure that health system staff can be available to help with testing in long-term care homes, where this is feasible
In addition, the Government of Canada has provided funding to the Canadian Red Cross for outbreak crisis management through COVID-19 Testing Assistance Response Teams.
The Panel acknowledges that addressing staffing challenges will require additional financial support, which may not be available to the long-term care sector. It's important that any efforts to address these challenges do not reduce existing care resources, which could negatively impact resident care. The Panel recommends developing a comprehensive strategy and allocating necessary financial and non-financial support to enable long-term care homes to deploy effective testing and screening strategies.
Case studies
United Kingdom: The U.K. Nightingale initiative involved hiring flight attendants who were laid off temporarily to work in health care settings. Those who participate in the program perform support roles (for example, changing beds and non-clinical tasks), under the supervision of nurses or clinicians. The initiative helped to address the strain in acute care settings.
CDL Rapid Screening Consortium: The Consortium is a private-led, not-for-profit initiative established in August 2020, in collaboration with the University of Toronto's Creative Destruction Laboratory (CDL). The Consortium developed protocols for rapid antigen screening in various workplaces and a platform that supports data collection, reporting and evaluation. CDL has spearheaded workplace screening pilots to support other employers.
Undertake further research to inform testing and screening strategies
To inform future diagnostic and screening test strategies, the Panel calls for additional research in the following 3 areas:
- investigating the utility of wastewater surveillance
- expanding toolkits looking at the behavioural aspects of testing and screening
- ensuring the effectiveness of test methodologies
These will be key to informing and adjusting testing and screening strategies.
Wastewater surveillance
Routine testing and screening could be complemented by wastewater surveillance at the community level or at the home. Wastewater surveillance involves collecting wastewater from sewage connections to measure levels of SARS-CoV-2 and the emergence of SARS-CoV-2 variants of concern.
Wastewater surveillance is being used as an emerging technique for testing and screening for viruses. In the case of long-term care, it's being used to indicate when outbreak response testing for COVID-19 is necessary.
The Panel recommends that long-term care homes and/or community partners consider working with researchers and public health authorities to explore whether wastewater testing can be undertaken as a surveillance approach. This may be an especially promising approach when levels of community transmission are low.
Case studies
Ottawa, Toronto and Edmonton: Wastewater surveillance is being used at long-term care homes to find early signals of COVID-19 outbreaks. This allows public health officials to be more alert and increase testing to minimize transmission.
McMaster has implemented a tracking system on campus to identify coronavirus in raw sewage. This could serve as an early warning sign for any outbreaks and inform future reopening plans.
Yellowknife is collecting and analyzing wastewater to determine whether COVID19 could be circulating in Yellowknife. For example, in December 2020, wastewater samples signalled undetected COVID cases in the community and triggered additional testing at a hotel for people isolating after travel. Data is reported publicly through an on-line dashboard.
Testing hesitancy
The Panel recognizes that frequent sampling using an invasive nasopharyngeal swab for testing in staff, essential caregivers and residents contributes to testing hesitancy. More tolerable sampling methods (for example, nasal swabs or swish-and-gargle) will likely reduce testing hesitancy in long-term care homes.
As technology continues to develop, less-invasive sampling methods will help make testing more acceptable. This will help to decrease testing hesitancy rates and reduce the load on health workers who administer the tests and confirm the results.
Case study
Quebec: The municipality of Laval implemented routine nasopharyngeal swab screening of health care staff in long-term care homes during the first wave. Participation rates fell to 15% because of testing hesitancy related to repeat swabbing. Once the saliva-based method was introduced in September 2020, compliance rates rose to 85%. As of February 2021, close to 4,000 asymptomatic health care staff are screened every week using a saliva-based PCR method.
Effectiveness of test methodologies in detecting variants of concern and SARS-COV-2 in vaccinated populations
The situation regarding vaccines and variants (such as the B.1.1.7 variant) is evolving and there is the potential for new variants of concern to emerge. Thus, there will be a need to continuously reassess the analytical and clinical performance of existing testing technologies and strategies to detect SARS-CoV-2 and variants of concern. This will be key to developing effective testing and screening strategies, such as using lower sensitivity point-of-care tests (for example, RATs) based on the potential impact of vaccination to reduce viral shedding.
Conclusion and next steps
In this report, the Panel presents 4 considerations to support testing and screening approaches in long-term care homes as vaccination efforts roll out in the broader community. Long-term care homes will need to re-evaluate their testing and screening strategies as new technologies become available, more Canadians are vaccinated and SARS-CoV-2 variants are better understood.
Our recommendations are grouped under the following 4 categories:
- Address equity issues
- Implement a robust testing and screening strategy
- Address shortages in health staffing
- Undertake further research to inform testing and screening strategies
The Panel anticipates providing additional guidance a subsequent report focusing on testing and screening for primary and secondary schools.
Annex 1: Key terms
- Antigen test
- A test that detects the presence of a specific protein that is part of the SARS-CoV-2 virus rather than the genetic material from the virus
- Asymptomatic person
- An individual without COVID-19 symptoms
- B.1.1.7
- SARS-CoV-2 variant of concern first detected in the United Kingdom
- B.1.351
- SARS-CoV-2 variant of concern first detected in South Africa
- COVID-19
- Coronavirus disease caused by SARS-CoV-2
- Essential caregiver
- A designate by the resident who provides direct care to the resident (may include a family member, private caregiver or paid companion
- Genome
- Complete set of genetic material
- Genome sequencing
- A process that determines the order of nucleotides in a genome
- Outbreak
- One or more positive cases of COVID-19 in a long-term care home
- PCR
- Polymerase chain reaction
- PoC
- Point-of-care
- Point of care
- Completed outside the clinical laboratory at or near where a patient is receiving care
- Prevalence
- The proportion of a population with COVID-19 at a given time
- RAT
- Rapid antigen test
- SARS-CoV-2
- Severe acute respiratory syndrome coronavirus 2, the coronavirus that causes COVID-19
- Screening/Screening test
-
Intended to identify infected persons who are asymptomatic and without known or suspected exposure to COVID-19
Usually performed to identify persons who may spread the virus so that measures can be taken to prevent further transmission
- Sensitivity
- The ability of a test to correctly identify those who have COVID-19 at the time the specimen was collected for laboratory analysis
- Surveillance
- Population-wide approaches undertaken to inform public health actions, such as wastewater monitoring
- Task shifting
- Re-distribution of tasks among different types of health workers (for example, nurses, pharmacists) to improve the use of resources and the provision of services
- Testing/diagnostic test
- Intended to identify current infection in an individual and is performed when a person signs or symptoms consistent with COVID-19 or had recent known or suspected exposure to COVID-19
- Turnaround time
- The time it takes from the time a sample is collected from an individual until the test results are available
- Variant of concern
- SARS-CoV-2 that have mutated to be more transmissible and/or cause more severe illness
| Location | Test | Frequency | Objective | Results |
|---|---|---|---|---|
| Vancouver, British Columbia | Abbott Panbio rapid antigen test | Staff tested 1 to 3 times per week | To enhance the health and safety in 5 long-term care homes, including those that have previously experienced outbreaks | Successfully identified multiple asymptomatic COVID-19 positive health care staff |
| Edmonton and Calgary, Alberta | Abbott IDNow and PanBio rapid antigen tests, confirmatory lab test of negative results | Using mobile centres, tested individuals exhibiting symptoms over the past 7 days | To manage and prevent spread to vulnerable Albertans at sites deemed at risk for an outbreak | Have been able to notify COVID-19 positive individuals of their results in a matter of hours |
| Saskatchewan | Abbott PanBio rapid antigen test, confirmatory lab test of positive results | On the spot | To screen asymptomatic staff and residents at 74 long-term care homes with another 22 facilities being trained | Results pending |
| Winnipeg and Neepawa, Manitoba | Panbio rapid antigen test | Once per week, while asymptomatic | To introduce asymptomatic testing for staff in 3 long-term care homes | Administered approximately 1,000 tests of which 3 asymptomatic staff members identified with COVID-19 |
| Ottawa, Ontario | Panbio rapid antigen test | On the spot | To provide the option of additional rapid testing for staff who are receiving weekly PCR tests | Identified 2 asymptomatic essential caregivers in between their weekly PCR tests |
| Toronto, Ontario | Lab-based PCR | One time | To prevent spread of COVID-19, Women's College Hospital undertook mobile testing at 3 long-term care homes | Administered more than 300 COVID-19 tests at 3 long-term care homes |
| Ontario | Lab-based PCR or Panbio rapid antigen test | PCR every 7 to 14 days or rapid test 1 to 3 times a week, depending on community prevalence | To ensure that long-term care staff, students and volunteers do not introduce COVID-19 | Confirmed positive cases in thousands of staff members at long-term care homes |
| New Brunswick | Lab-based PCR | Once every two weeks, while asymptomatic | To ensure that asymptomatic staff at long-term care homes do not introduce COVID-19 | This program will monitor, reduce and prevent the spread of COVID-19 in long-term care |
| Nova Scotia | Lab-based PCR | Once every two weeks, while asymptomatic | To ensure that asymptomatic staff, volunteers and essential caregivers at long-term care homes do not introduce COVID-19 | This program will monitor, reduce and prevent the spread of COVID-19 in long-term care |
British Columbia
- Jan. 25: Report released on impact of COVID-19 on the long-term care sector
Ontario
- Jan. 5: Additional $398 million for long-term care homes to reduce spread, including enhanced staff and visitor testing
