Lyme disease in Canada, 2009 to 2019

 Download this article as a PDF
Download this article as a PDF Published by: The Public Health Agency of Canada
Issue: Volume 48-5, May 2022: Vector-Borne Infections–Part 1: Ticks & Mosquitoes
Date published: May 2022
ISSN: 1481-8531
Submit a manuscript
About CCDR
Browse
Volume 48-5, May 2022: Vector-Borne Infections–Part 1: Ticks & Mosquitoes
Surveillance
Surveillance for Lyme disease in Canada, 2009–2019
Salima Gasmi1, Jules K Koffi1, Mark P Nelder2, Curtis Russell2, Scott Graham-Derham3, Lisa Lachance4, Bijay Adhikari5, Jacqueline Badcock6, Shamara Baidoobonso7, Beverly A Billard8, Beth Halfyard9, Stéphanie Jodoin10, Mayank Singal11, Annie-Claude Bourgeois12
Affiliations
1 Centre for Food-borne, Environmental and Zoonotic Infectious Diseases, Public Health Agency of Canada, Saint-Hyacinthe, QC
2 Enteric, Zoonotic and Vector-Borne Diseases, Public Health Ontario, Toronto, ON
3 Communicable Disease Control Branch, Manitoba Health and Seniors Care, Winnipeg, MB
4 Health and Wellness Promotion Branch, Public Health and Compliance Division, Alberta Health, Edmonton, AB
5 Population Health Branch, Ministry of Health, Regina, SK
6 Office of the Chief Medical Officer of Health, New Brunswick Department of Health, Fredericton, NB
7 Prince Edward Island Department of Health and Wellness, Population Health Assessment & Surveillance Unit, Charlottetown, PE
8 Public Health Branch, Nova Scotia Department of Health and Wellness, Halifax, NS
9 Health and Community Services, Population Health Branch, St. John’s, NL
10 Direction générale adjointe de la protection de la santé publique, Ministère de la Santé et des Services sociaux, Québec, QC
11 Communicable Diseases and Immunization Service, BC Centre for Disease Control, Vancouver, BC
12 Centre for Food-borne, Environmental and Zoonotic Infectious Diseases, Public Health Agency of Canada, Ottawa, ON
Correspondence
Suggested citation
Gasmi S, Koffi JK, Nelder MP, Russell C, Graham-Derham S, Lachance L, Adhikari B, Badcock J, Baidoobonso S, Billard BA, Halfyard B, Jodoin S, Singal M, Bourgeois AC. Surveillance for Lyme disease in Canada, 2009–2019. Can Commun Dis Rep 2022;48(5):219–27. https://doi.org/10.14745/ccdr.v48i05a05
Keywords: surveillance, Ixodes scapularis, Ixodes pacificus, tick-borne disease, Lyme disease, Canada
Abstract
Background: Lyme disease (LD) is a multisystem infection that can affect the skin, heart, joints and nervous system. In Canada, the incidence of LD cases has increased over the past decade making this a disease of public health concern. The objective of this study is to summarize the epidemiology of LD cases reported in Canada from 2009 through 2019.
Methods: Incidence over time, case classification (confirmed and probable), seasonal and geographic distribution, demographic and clinical characteristics of reported LD cases were determined. Logistic regression was used to explore potential demographic risk factors for the occurrence of LD.
Results: During 2009–2019, a total of 10,150 LD cases were reported by the provinces to the Public Health Agency of Canada, of which 7,242 (71.3%) were confirmed and 2,908 (28.7%) were probable cases. The annual count increased from 144 in 2009 to 2,634 in 2019, mainly due to an increase in locally acquired infections, from 65.3% to 93.6%, respectively. The majority of cases (92.1%) were reported from three provinces: Ontario (46.0%); Nova Scotia (28.0%); and Québec (18.1%). Most of the locally acquired cases (74.0%) were reported in the summer months of June (20.0%), July (35.4%) and August (18.6%). The highest incidence rates (cases per 100,000 population) were in children aged 5–9 years (45.0) and in adults aged 65–69 years (74.3), with 57.3% of all reported cases occurring among males. The most common presenting symptoms were single erythema migrans rash (75.1%) and arthritis (34.1%). The frequency of reported clinical manifestations varied among age groups and seasons with erythema migrans and arthritis at presentation reported more frequently in children than older patients.
Conclusion: The results of this report highlight the continued emergence of LD in Canada and the need for further development and implementation of targeted awareness campaigns designed to minimize the burden of LD.
Introduction
Lyme disease (LD) is the most commonly reported tick-borne zoonosis in North America and Europe. In Canada, LD is caused by the spirochete Borrelia burgdorferi (B. burgdorferi) sensu stricto and transmitted by Ixodes pacificus (I. pacificus) ticks in British Columbia and Ixodes scapularis (I. scapularis) in central and eastern Canada. Over the last decade, the warming climate as well as anthropogenic factors such as landscape changes, have contributed to tick and tick-borne diseases expanding their geographic rangeFootnote 1Footnote 2. As a result, the incidence of LD cases increased over the past decadeFootnote 3 making this a disease of public health concern in Canada.
Lyme disease is a multisystem infection that can affect the skin, heart, joints and nervous system. Approximately 70% of people bitten by a B. burgdorferi-infected tick will develop a cutaneous rash, erythema migrans, which may be accompanied by flu-like symptomsFootnote 4. If left untreated, spirochetes disseminate throughout the body via the blood and may cause multiple secondary erythema migrans lesions, cardiac manifestations (carditis, atrioventricular heart block, arrhythmia and palpitations) and neurologic manifestations (facial paralysis—Bell’s palsy—and meningitis). Months to years post-infection, late LD can manifest with single or recurrent joint arthritis episode(s). It is noteworthy that one death attributed to complications of Lyme carditis has been recorded in Canada in 2018Footnote 5.
This report summarizes the epidemiology of LD cases reported in Canada from 2009 through 2019.
Methods
Case definition
Lyme disease became nationally notifiable in 2009. In 2016, the LD case definitionFootnote 6 was revised to propose five methods to identify LD risk to simplify reporting by jurisdictions (Table A1).
Data sources
Information on reported LD cases from 2009 through 2019 was obtained from the provincial and territorial public health authorities via the Canadian Notifiable Disease Surveillance System (CNDSS) and the Lyme Disease Enhanced Surveillance (LDES) system of the Public Health Agency of Canada (PHAC). The CNDSS only collects demographic data, episode date and case classification from the provinces and territories. The LDES system captures additional data, including possible geographic location of exposure for both locally acquired and travel-related cases, clinical manifestations and results of laboratory testing. Public health units in the provinces and territories are responsible for investigating the cases reported by clinicians using a case management toolFootnote 7. They collect among other information, the most likely location of LD acquisition, whether in Canada or abroad, regardless of the stage of diseaseFootnote 8.
Analysis
Incidence rates per 100,000 population for reported cases were calculated by year, province, age group and sex using the census population estimates for July 1st of Statistics Canada dataFootnote 9 for each year of the reporting period, 2009–2019. Seasonality was determined by the reported date of the symptom onset. Percentages of reported clinical manifestations of locally acquired infections were calculated for overall cases and by age group. The most likely geographic location for acquisition of LD infection was superimposed on a map of LD risk areasFootnote 6. Cases with a history of travel (within or outside of Canada) within 30 days of reporting were not included in the analysis of geographic distribution.
For locally acquired cases with no missing data, variations among age groups, sex, month of onset and reporting year were explored in multivariate logistic regression using Stata, version 15.1 (StataCorp, College Station, Texas, United States). In separate models, the binary outcome variable was the presence or absence of LD stage at presentation, for each of early localized (single erythema migrans), early disseminated (multiple erythema migrans, cardiac manifestations, Bell’s palsy and other neurological manifestations) and late disseminated stage (arthritis) as classified by the Infectious Disease Society of America guidelinesFootnote 10. For each model, explanatory variables were age group (10 and 15-year intervals), sex, month of symptom onset (in four categories for simplicity), year and province of reporting. The explanatory variable “province” was included in the analysis to account for possible variability in reporting between provinces. Explanatory variables were screened in bivariable logistic regression models, and those significant at the level of p<0.1 were included in multivariable models. The most parsimonious multivariate models were sought by backward elimination of non-significant variables until all factors in the model were significant (p<0.05).
Results
Incidence over time
From 2009 through 2019, 10,150 LD cases were reported in Canada. Of these 7,242 (71.3%) were confirmed and 2,908 (28.7%) were probable cases (Table 1). Overall, the annual number of reported cases increased from 144 in 2009 to 2,634 in 2019 (incidence rates per 100,000 population of 0.4 and 7.0, respectively); however, in 2014 and 2018 the number of cases decreased (Table A2). The number of cases acquired in Canada increased from 79 to 2,052 during the same period, representing 65.3% and 93.6%, respectively, of cases with known exposure location (Figure 1).
| Classification | Reported Lyme disease cases | |||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Year | ||||||||||||||||||||||||
| 2009 | 2010 | 2011 | 2012 | 2013 | 2014 | 2015 | 2016 | 2017 | 2018 | 2019 | Total | |||||||||||||
| N | % | N | % | N | % | N | % | N | % | N | % | N | % | N | % | N | % | N | % | N | % | N | % | |
| All cases (n=10,150) | ||||||||||||||||||||||||
| Confirmed | 115 | 79.9 | 109 | 76.2 | 109 | 76.2 | 232 | 68.6 | 485 | 71.1 | 334 | 64.0 | 651 | 71.0 | 672 | 67.7 | 1,496 | 73.9 | 1,053 | 70.8 | 1,900 | 72.2 | 7,242 | 71.3 |
| Probable | 29 | 20.1 | 34 | 23.8 | 34 | 23.8 | 106 | 31.4 | 197 | 28.9 | 188 | 36.0 | 266 | 29.0 | 320 | 32.3 | 529 | 26.1 | 434 | 29.2 | 734 | 27.8 | 2,908 | 28.7 |
| Total | 144 | 100 | 143 | 100 | 143 | 100 | 338 | 100 | 682 | 100 | 522 | 100 | 917 | 100 | 992 | 100 | 2,025 | 100 | 1,487 | 100 | 2,634 | 100 | 10,150 | 100 |
| Cases acquired in Canada (n=7,691) | ||||||||||||||||||||||||
| Confirmed | 56 | 70.9 | 56 | 65.1 | 56 | 65.1 | 129 | 58.1 | 286 | 61.1 | 198 | 59.5 | 467 | 70.0 | 542 | 64.8 | 1,204 | 72.0 | 751 | 67.2 | 1,410 | 68.7 | 5,195 | 67.5 |
| Probable | 23 | 29.1 | 30 | 34.9 | 30 | 34.9 | 93 | 41.9 | 182 | 38.9 | 135 | 40.5 | 200 | 30.0 | 294 | 35.2 | 467 | 28.0 | 366 | 32.8 | 642 | 31.3 | 2,496 | 32.5 |
| Total | 79 | 100 | 86 | 100 | 86 | 100 | 222 | 100 | 468 | 100 | 333 | 100 | 667 | 100 | 836 | 100 | 1,671 | 100 | 1,117 | 100 | 2,052 | 100 | 7,691 | 100 |
Figure 1: Number and proportion of Lyme disease cases, all reported and locally acquired (percentageFigure 1 Footnote a) in Canada, 2009−2019
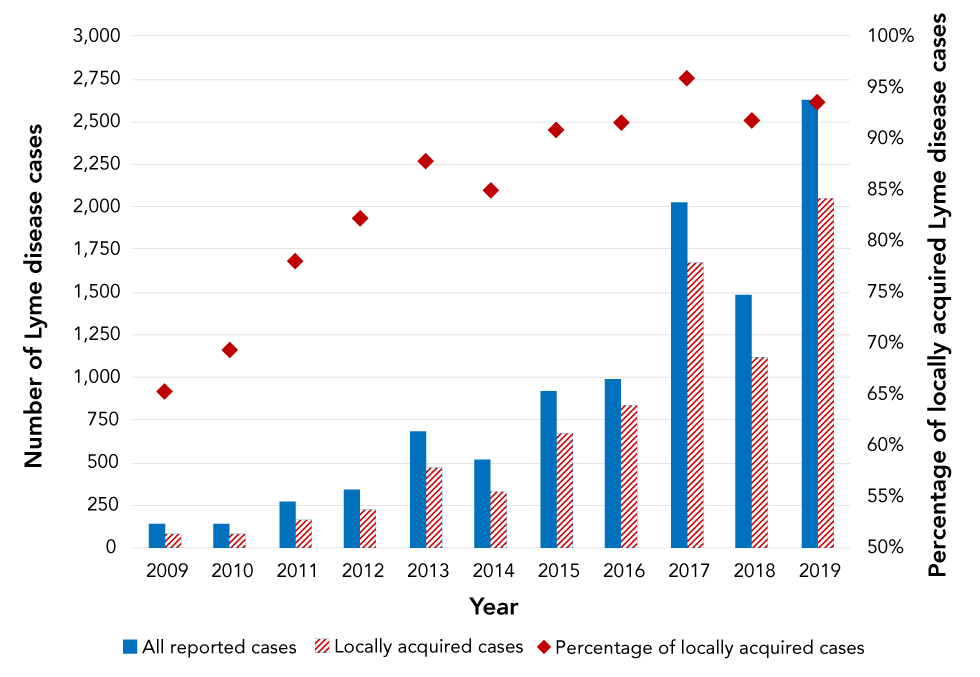
Text description: Figure 1
| Lyme disease cases | 2009 | 2010 | 2011 | 2012 | 2013 | 2014 | 2015 | 2016 | 2017 | 2018 | 2019 | Total |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| All reported cases | 144 | 143 | 266 | 338 | 682 | 522 | 917 | 992 | 2,025 | 1,487 | 2,634 | 10,150 |
| Locally acquired cases | 79 | 86 | 160 | 222 | 468 | 333 | 667 | 835 | 1,671 | 1,117 | 2,052 | 7,691 |
| Percentage of locally acquired cases | 65.3% | 69.4% | 78.0% | 82.2% | 87.8% | 84.9% | 90.9% | 91.6% | 95.9% | 91.8% | 93.6% | 91.1% |
Among all reported cases, the majority (92.1%) were reported from three provinces: Ontario (46.0%); Nova Scotia (28.0%); and Québec (18.1%). In 2019, Nova Scotia reported a LD incidence that was twelve-fold greater than the LD incidence for Canada overall (85.6 versus 7.0 per 100,000 population) (Table 2).
| Province | Incidence per 100,000 population | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 2009 | 2010 | 2011 | 2012 | 2013 | 2014 | 2015 | 2016 | 2017 | 2018 | 2019 | ||
| All cases (n=10,150) | ||||||||||||
| British Columbia | 0.2 | 0.2 | 0.4 | 0.4 | 0.1 | 0.1 | 0.4 | 0.8 | 0.3 | 0.2 | 0.3 | |
| Alberta | 0.0 | 0.0 | 0.2 | 0.2 | 0.5 | 0.2 | 0.3 | 0.2 | 0.3 | 0.3 | 0.3 | |
| Saskatchewan | 0.0 | 0.0 | 0.1 | 0.0 | 0.1 | 0.0 | 0.0 | 0.1 | 0.3 | 0.2 | 0.1 | |
| Manitoba | 0.4 | 1.0 | 1.0 | 1.5 | 2.3 | 2.7 | 2.4 | 3.9 | 3.2 | 4.0 | 4.7 | |
| Ontario | 0.8 | 0.7 | 1.0 | 1.4 | 2.4 | 1.7 | 3.1 | 2.7 | 7.1 | 4.4 | 8.0 | |
| Québec | 0.2 | 0.1 | 0.4 | 0.5 | 1.7 | 1.5 | 1.9 | 2.2 | 4.0 | 3.6 | 5.9 | |
| New Brunswick | 0.0 | 0.3 | 0.7 | 0.9 | 0.7 | 0.7 | 1.7 | 1.4 | 3.9 | 2.6 | 4.6 | |
| Nova Scotia | 1.7 | 1.8 | 5.7 | 5.4 | 16.2 | 12.1 | 26.1 | 34.6 | 61.2 | 47.0 | 85.6 | |
| Prince Edward Island | 0.0 | 0.0 | 0.7 | 1.4 | 0.0 | 0.0 | 2.7 | 2.7 | 2.0 | 0.7 | 3.8 | |
| Newfoundland & Labrador | 0.0 | 0.2 | 0.0 | 0.0 | 0.0 | 0.0 | 0.4 | 0.2 | 0.0 | 0.4 | 0.0 | |
| Canada | 0.4 | 0.4 | 0.8 | 1.0 | 1.9 | 1.5 | 2.6 | 2.7 | 5.5 | 4.0 | 7.0 | |
| Cases acquired in the province of residency (n=7,200) | ||||||||||||
| British Columbia | N/A | N/A | N/A | N/A | N/A | N/A | N/A | 0.1 | 0.1 | 0.0 | 0.0 | |
| Saskatchewan | N/A | N/A | N/A | N/A | N/A | N/A | N/A | 0.0 | 0.1 | 0.0 | 0.0 | |
| Manitoba | 0.3 | 0.6 | 0.6 | 1.0 | 2.0 | 2.4 | 2.3 | 2.4 | 2.9 | 3.5 | 4.1 | |
| Ontario | 0.5 | 0.5 | 0.8 | 0.8 | 2.1 | 1.3 | 2.7 | 2.0 | 5.5 | 2.5 | 5.0 | |
| Québec | N/A | N/A | N/A | N/A | N/A | N/A | N/A | 1.4 | 3.0 | 2.7 | 3.8 | |
| New Brunswick | 0.0 | 0.3 | 0.4 | 0.7 | 0.7 | 0.5 | 1.5 | 0.8 | 3.5 | 2.5 | 3.1 | |
| Nova Scotia | 1.5 | 1.5 | 5.2 | 5.3 | 16.1 | 12.1 | 26.1 | 25.4 | 55.2 | 34.8 | 79.2 | |
| Prince Edward Island | 0.0 | 0.0 | 0.0 | 0.7 | 0.0 | 0.0 | 0.0 | 0.0 | 0.0 | 0.0 | 0.0 | |
During 2009–2019, data on history of travel was available for 83.2% (n=8,444) of all reported cases (n=10,150). Of the cases acquired during travel outside Canada, 363 (57.4%) were exposed in the United States and 261 (41.3%) in Europe.
Seasonal distribution
Over the study period, the month of illness onset for locally acquired cases was available for 6,278 cases (81.6%). Most cases (95.8%) were reported from May through November, with the majority reported in the summer months of June (20.0%), July (35.4%) and August (18.6%) (Figure 2).
Figure 2: Month of illness onsetFigure 2 Footnote a of Lyme disease cases acquired in Canada, 2009−2019
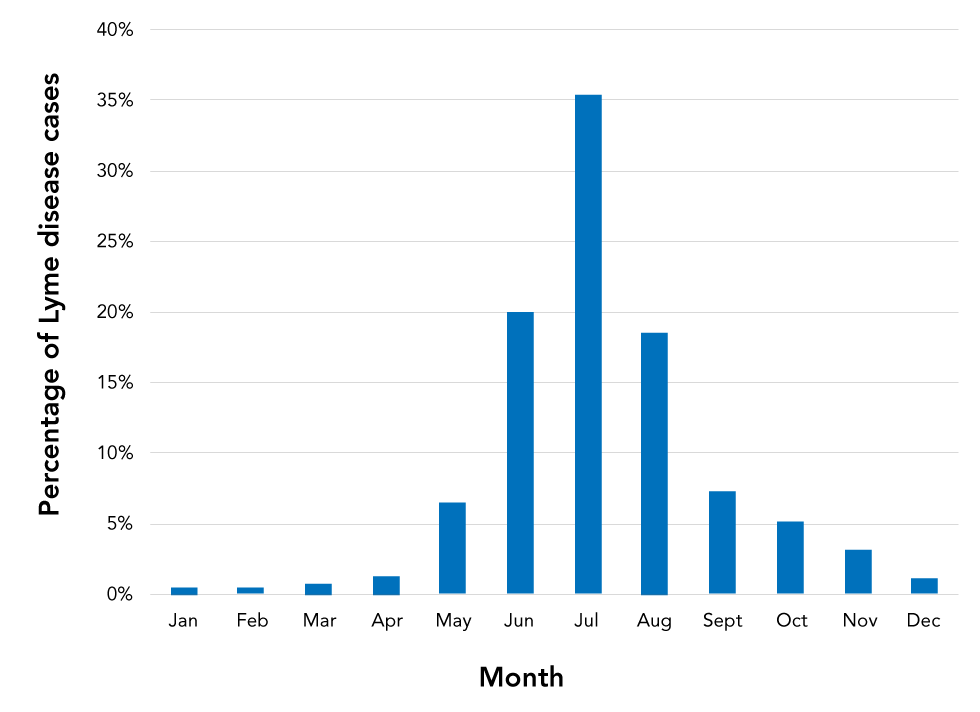
Text description: Figure 2
| Month | Percentage of Lyme disease cases |
|---|---|
| Jan | 1% |
| Feb | 0% |
| Mar | 1% |
| Apr | 1% |
| May | 6% |
| Jun | 20% |
| Jul | 35% |
| Aug | 19% |
| Sep | 7% |
| Oct | 5% |
| Nov | 3% |
| Dec | 1% |
Geographic distribution
Information on location of LD acquisition (at the sub-provincial level) was available for 93.5% (n=6,734) of the locally acquired cases. Most of the cases were concentrated in locations in southern Manitoba, south-central and south-eastern Ontario, southern Québec and New Brunswick and in Nova Scotia.
Some cases were likely acquired outside locations where populations of I. scapularis ticks are established (the hatched areas in the Figure 3).
Figure 3: Reported locations of Lyme disease acquisitionFigure 3 Footnote a, Canada, 2009–2019
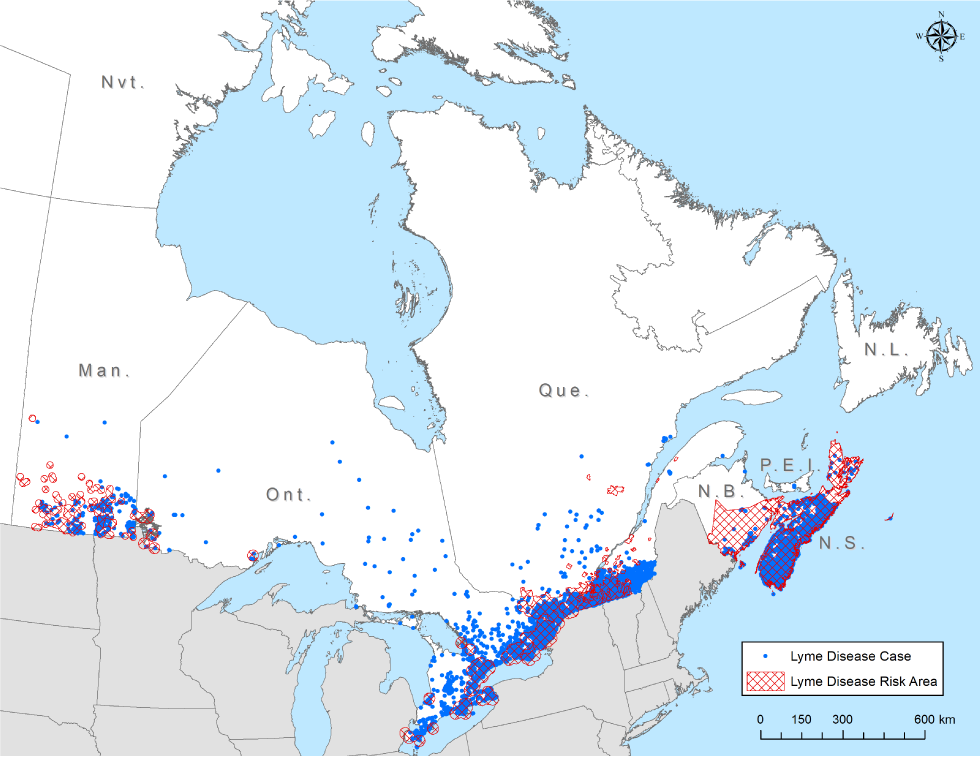
Text description: Figure 3
Each dot on the map represents the probable location of infection acquisition, randomly distributed at the census subdivision level for all provinces except: Québec (2016–2018) and Nova Scotia (2019) used the administrative region of probable acquisition and forward sortation area (FSA) of residency, respectively. In 2018, all of Nova Scotia was declared at-risk of Lyme disease, and since then, the probable location of acquisition was based on the FSA of residency for cases with no travel history outside the province. Data on location of acquisition was not available at sub-provincial level for British Columbia and Saskatchewan; Saskatchewan reported one locally acquired case in 2017. Cases reported by Alberta and Newfoundland & Labrador were travel-related only. Hatched areas indicate Lyme disease risk areas; these are locations where surveillance activities suggest that populations of the Lyme disease vector, Ixodes scapularis have been established and the likely transmission of B. burgdorferi is occurring.
Demographic and clinical characteristics
Demographic information was available for 7,667 (99.7%) of reported locally acquired LD cases. The overall average age was 47.4 years (95% confidence interval (CI): 46.9–47.9).
The cumulative incidence per 100,000 population shows a bimodal pattern with peaks in children aged 5–9 years (45.0) and adults aged 65–69 years (74.3). Incidence was higher in adults aged 50−84 years, representing 57.0% of all reported cases (Figure 4).
Figure 4: Cumulative incidenceFigure 4 Footnote a per 100,000 population of Lyme disease cases by age group and sex, Canada, 2009–2019 (n=7,667)
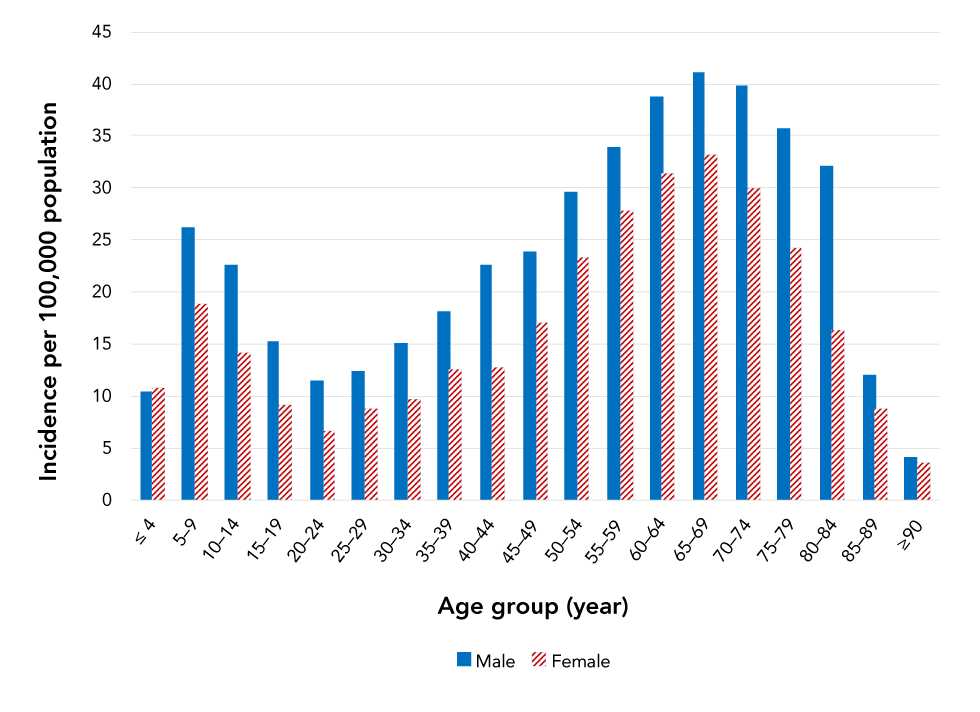
Text description: Figure 4
| Age group (year) | Incidence per 100,000 habitants | |
|---|---|---|
| Male | Female | |
| ≤4 | 10.4 | 10.8 |
| 5−9 | 26.2 | 18.8 |
| 10−14 | 22.6 | 14.1 |
| 15−19 | 15.2 | 9.1 |
| 20−24 | 11.4 | 6.6 |
| 25−29 | 12.3 | 8.7 |
| 30−34 | 15.1 | 9.7 |
| 35−39 | 18.1 | 12.6 |
| 40−44 | 22.5 | 12.7 |
| 45−49 | 23.9 | 17.1 |
| 50−54 | 29.6 | 23.4 |
| 55−59 | 33.9 | 27.8 |
| 60−64 | 38.7 | 31.4 |
| 65−69 | 41.1 | 33.2 |
| 70−74 | 39.8 | 30.0 |
| 75−79 | 35.7 | 24.2 |
| 80−84 | 32.0 | 16.3 |
| 85−89 | 12.0 | 8.9 |
| ≥90 | 4.2 | 3.6 |
Lyme disease cases were reported more often in males than females (57.3% versus 42.7%). In all age groups, incidence was higher among males than females, except for children under five years where the incidence was similar (Figure 4).
Information on clinical manifestations of LD cases was available for 4,961 (64.5%) of locally acquired infections. The most commonly reported manifestations were single erythema migrans rash (75.1%) and arthritis (34.1%). Cardiac manifestations, Bell’s palsy and other neurologic manifestations were reported in 3.7%, 7.6% and 19.0% of cases, respectively. Among the 4,961 cases, 33.7% reported a combination of LD stages; 28.2% had early localized stage and early disseminated or late disseminated stage, and 5.5% had early and late disseminated stages.
In a multivariate analysis of the LD stages at presentation (Table 3), the odds of age groups 10−19, 20−29, 30−39 and 50−59 years for being diagnosed in early localized stage were respectively 0.56 (95% CI: 0.42−0.75), 0.63 (95% CI: 0.47−0.85), 0.60 (95% CI: 0.46−0.79) and 0.77 (95% CI: 0.61−0.97) times lower than the reference age group 0−9 years.
| Outcome | Explanatory variables | Odds ratio | Wald (z value) |
p-value | |
|---|---|---|---|---|---|
| n | 95% CI | ||||
| Early localized | 10–19 years vs 0–9 years | 0.56 | 0.42–0.75 | -3.96 | 0.00 |
| 20–29 years vs 0–9 years | 0.63 | 0.47–0.85 | -3.05 | 0.00 | |
| 30–39 years vs 0–9 years | 0.60 | 0.46–0.79 | -3.65 | 0.00 | |
| 50–59 years vs 0–9 years | 0.77 | 0.61–0.97 | -2.21 | 0.03 | |
| Dec–Feb vs Jun–Aug | 0.46 | 0.30–0.69 | -3.77 | 0.00 | |
| Early disseminated | 10–19 years vs 0–9 years | 1.56 | 1.09–2.25 | 2.41 | 0.02 |
| 20–29 years vs 0–9 years | 1.76 | 1.21–2.55 | 2.98 | 0.00 | |
| 60–69 years vs 0–9 years | 1.42 | 1.04–1.94 | 2.19 | 0.03 | |
| Sep–Nov vs Jun–Aug | 0.81 | 0.66–0.99 | -2.08 | 0.04 | |
| Dec–Feb vs Jun–Aug | 0.51 | 0.29–0.90 | -2.32 | 0.02 | |
| Mar–May vs Jun–Aug | 0.62 | 0.46–0.82 | -3.32 | 0.00 | |
| Late disseminated | 60–74 years vs 0–14 years | 0.78 | 0.64–0.96 | -2.36 | 0.02 |
| 75 or more years vs 0–14 years | 0.52 | 0.38–0.72 | -4.04 | 0.00 | |
| Male vs female | 1.14 | 1.01–1.29 | 2.10 | 0.04 | |
| Sep–Nov vs Jun–Aug | 1.29 | 1.09–1.53 | 3.00 | 0.00 | |
| Dec–Feb vs Jun–Aug | 3.30 | 2.23–4.88 | 5.99 | 0.00 | |
| Mar–May vs Jun–Aug | 1.35 | 1.09–1.67 | 2.73 | 0.01 | |
When the outcome was in the early disseminated stage, the odds of age groups 10−19, 20−29 and 60−69 years were, respectively, 1.56 (95% CI: 1.09−2.25), 1.76 (95% CI: 1.21−2.55) and 1.42 (95% CI: 1.04−1.94) times higher compared with the 0–9 years age group. In contrast, when the outcome was in late disseminated stage, the odds of age groups 60−74 and 75 years and older were respectively 0.78 (95% CI: 0.64−0.96) and 0.52 (95% CI: 0.38−0.78) times lower when compared to the reference age group, 0–14 years.
The number of cases with early localized stage was less likely to be reported from December–February versus June–August (odds ratio [OR]: 0.46; 95% CI: 0.30−0.69). Cases with early disseminated stage were less likely to be reported September−November (OR: 0.81; 95% CI: 0.66−0.99), December−February (OR: 0.51; 95% CI: 0.29−0.90) and March−May (OR: 0.62; 95% CI: 0.46−0.82) than in the summer months of June–August. Cases diagnosed in late disseminated stage were reported more often during September–November (OR: 1.29; 95% CI: 1.09−1.53), December−February (OR: 3.30; 95% CI: 2.23−4.88) and March−May (OR: 1.35; 95% CI: 1.09−1.67) when compared with June–August.
Males were more likely to be reported with late disseminated stage than females (OR: 1.14; 95% CI: 1.01−1.29).
Discussion
This report provides an update on the epidemiology of LD cases reported in Canada from 2009 through 2019. Over the 11-year period, the incidence of reported LD cases has increased dramatically in Canada, mainly due to an increase in the number of locally acquired infections. The vast majority of cases continued to be concentrated in southern Manitoba, south-central and south-eastern Ontario, southern Québec and New Brunswick and in Nova Scotia, which likely coincide in most cases with the areas where I. scapularis ticks carrying B. burgdorferi are establishedFootnote 11.
In these parts of the country, the tick vector is spreading northward as a result of climate warming that drives, in part, the growing suitable habitat for tick survival and establishmentFootnote 12. Moreover, greater awareness among the public and healthcare providers and improvements to public health surveillance and notification may also have contributed to the increase in the number of reported cases.
It is important to note that the incidence in Nova Scotia during 2019 was twelve-fold higher than the national incidence. This is most likely a result of the increased number of established blacklegged tick populations; including the density, geographic range, B. burgdorferi infection prevalenceFootnote 13, and the maritime climate that permits, during some warm spells in winter, tick activity in the absence of snow coverFootnote 14Footnote 15.
In contrast, in western Canada, where the predominant vector I. pacificus is distributed along the coast and southern region of British Columbia, the LD risk has remained relatively low and stable because of the low prevalence of infected ticksFootnote 16.
Lyme disease symptom onset was more likely reported from May to November, a pattern that corresponds to nymphal tick activity in the summer monthsFootnote 17; these time periods also overlap with when people are most engaged in outdoor activities that expose them to the risk of tick bites and B. burgdorferi transmission. However, some cases reported illness onset in winter months, which may be explained by 1) the occurrence of the late disseminated stage that appears months to years post-infection in untreated patientsFootnote 18 or 2) advantageous weather that allows tick activity in British ColumbiaFootnote 19.
Consistent with previous studies, the age distribution of cases was bimodal in children and older adults. Among children, incidence peaked in those aged 5–9 years, which corroborates previous studies in Canada and the United StatesFootnote 20Footnote 21Footnote 22. However, we found that adults aged 50−84 years were at higher risk of LD compared with previous studies, which reported younger groups (range 50−64 years) to be the most at riskFootnote 20Footnote 21Footnote 22Footnote 23. The level of adoption of preventive behaviours toward LD or to the level of tick exposure could have contributed to the observed discrepancy in the most at-risk age group for LDFootnote 24. Targeted education and awareness of preventive measures are needed for older persons in order to decrease the risk of tick bites and LD.
Erythema migrans and arthritis were the most commonly reported clinical manifestations in this study; consistent with findings reported previously in Canada and the Unite StatesFootnote 20Footnote 21Footnote 22Footnote 23. Lyme arthritis is a manifestation of late-stage LD that usually appears in 51% of untreated patientsFootnote 25, highlighting the importance of early detection and treatment.
Males were more likely to have LD than females across almost all age groups, similar to previous reports from Canada and the United StatesFootnote 20Footnote 21Footnote 22. Additionally, late disseminated stage was more common in males than females, although no significant differences were found for earlier disease stages. This apparent sex-based difference might be a result of higher risk of tick bitesFootnote 26 and LD transmission; however, the reason why males are diagnosed more often than females with late Lyme arthritis may be due to a difference in immunologic response to B. burgdorferi infectionFootnote 27 or simply to a delay in presenting for medical care. Further research is needed to elucidate this finding.
Across age categories, the percentage of reported clinical manifestations varied widely in children younger than 15 years. The percentage of cases with single erythema migrans (early localized stage) was higher in younger children and the proportion of arthritis (late disseminated stage) was higher in older children (Figure A1) which is consistent with a study from the Canadian Paediatric Surveillance ProgramFootnote 14. Furthermore, children are at higher risk of both early localized LD and Lyme arthritis than older patients. Studies have found that children are at higher risk of tick bites from vector ticks such as I. scapularis and I. pacificusFootnote 26Footnote 28Footnote 29; hence, efforts to enhance awareness of ticks and LD should target this at-risk age group and their parents and caregivers.
The LD stage at presentation varied significantly between seasons. Cases with early localized stage were more frequently reported in summer months (June–August) than winter months (December–February); and cases with arthritis were less frequently reported in summer months compared with the rest of the year. This is expected given that untreated patients have manifestations of the early localized stage that appear within 30 days of infection, and the late disseminated stage can appear months to years post infectionFootnote 24. In contrast, cases with early disseminated stage were diagnosed more in the summer than other parts of the year. Given that early disseminated stage appears in untreated patients within three months post infection, this finding suggests it is likely that there is some underreporting of cases with cardiac and neurologic manifestations, which may go undetected or unreported outside of the summer months. This result underscores that prevention messages should not only be focused during the spring and summer months when nymphal and adult ticks are most active, but year-round.
Limitations
There are several limitations to the interpretation of the findings of this report. First, it is likely that the incidence rates over time are conservative estimates as some LD cases may be undiagnosed and probable cases may be underreported. Second, the 2016 LD case definition revision could have impacted the reporting of some cases. Third, clinical manifestations are reported voluntarily to the provincial public health organizations, which could have led to misclassification and underreporting. Fourth, information on whether the LD infection was locally acquired or travel-related is only an estimate because not all provinces provided these data. Finally, because of limited resources, field tick surveillance to detect the expansion of LD risk areas may not be up to date in many locations, which would affect the classification of cases.
Conclusion
The number of reported LD cases has continued to increase in Canada over the last decade, as did the geographic range of ticks that carry the LD bacterium. Continued surveillance, preventive strategies as well as early disease recognition and treatment will continue to minimize the impact of LD in Canada.
The key findings of this report highlight the need for further targeted awareness campaigns designed to minimize the burden of LD in Canada.
Authors’ statement
SG — Data collection and curation, conceptualization, methodology, formal analysis, writing–original draft, writing–review and editing
JKK, ACB — Conceptualization, methodology, writing–review and editing, management
MPN, CR, SGD, CS, BA, JB, SB, BAB, BH, SJ, MS — Writing–review and editing
Competing interests
None.
Acknowledgements
The authors thank all the provincial and regional public health workers who collect and report data through the Canadian Notifiable Disease Surveillance System (CNDSS), the Lyme Disease Enhanced Surveillance (LDES) system and the field tick surveillance system and Y Pelcat of the Public Health Agency of Canada for preparing Figure 3.
Funding
This study was supported by the Public Health Agency of Canada and all the provincial public health organizations that contributed to the data.
Annex
| Confirmed case | Probable case |
|---|---|
Clinical evidence of illness with laboratory confirmation by one of the following methods: Isolation of Borrelia burgdorferi (B. burgdorferi) from a clinical specimen as specified by current guidelinesFootnote 10Footnote 18Footnote 30 Detection of B. burgdorferi DNA by PCR testing on synovial fluid, cerebrospinal fluid, EM tissue biopsies or blood and by methods specified by current guidelinesFootnote 10Footnote 18Footnote 30 OR Clinical evidence of illness with a history of residence in, or visit to, a Lyme disease risk area; and with laboratory evidence of infection in the form of a positive serologic test using the two-tiered approach. The two-tiered testing approach consists of a screening ELISA followed by an immunoblot assay. Immunoblots include traditional Western blotsFootnote 30 or newer line blots, and both formats target an identical set of B. burgdorferi immunoreactive proteinsFootnote 31Table A1 Footnote a |
Clinical evidence of illness without a history of residence in, or visit to, a Lyme disease risk area; and with laboratory evidence of infection in the form of a positive serologic test as defined above under confirmed casesTable A1 Footnote a OR Clinician-observed erythema migrans without laboratory evidence but with history of residence in, or visit to, a Lyme disease risk area |
| Province | Lyme disease cases (n=10,150) | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 2009 | 2010 | 2011 | 2012 | 2013 | 2014 | 2015 | 2016 | 2017 | 2018 | 2019 | Total | |
| British Columbia | 9 | 7 | 20 | 18 | 6 | 5 | 21 | 40 | 17 | 9 | 14 | 166 |
| Alberta | 0 | 0 | 7 | 8 | 19 | 9 | 14 | 10 | 12 | 15 | 14 | 108 |
| Saskatchewan | 0 | 0 | 1 | 0 | 1 | 0 | 0 | 1 | 4 | 2 | 1 | 10 |
| Manitoba | 5 | 12 | 12 | 19 | 29 | 35 | 31 | 51 | 43 | 54 | 65 | 356 |
| Ontario | 100 | 93 | 134 | 191 | 327 | 229 | 426 | 371 | 1,005 | 628 | 1,168 | 4,672 |
| Québec | 14 | 11 | 32 | 42 | 142 | 125 | 160 | 177 | 329 | 305 | 500 | 1,837 |
| New Brunswick | 0 | 2 | 5 | 7 | 5 | 5 | 13 | 11 | 30 | 20 | 36 | 134 |
| Nova Scotia | 16 | 17 | 54 | 51 | 153 | 114 | 246 | 326 | 582 | 451 | 830 | 2,840 |
| Prince Edward Island | 0 | 0 | 1 | 2 | 0 | 0 | 4 | 4 | 3 | 1 | 6 | 21 |
| Newfoundland & Labrador | 0 | 1 | 0 | 0 | 0 | 0 | 2 | 1 | 0 | 2 | 0 | 6 |
| Canada | 144 | 143 | 266 | 338 | 682 | 522 | 917 | 992 | 2,025 | 1,487 | 2,634 | 10,150 |
Figure A1: Percentage of clinical manifestations by age group for locally acquired Lyme disease cases, in Canada, 2009−2019 (n=4,951)
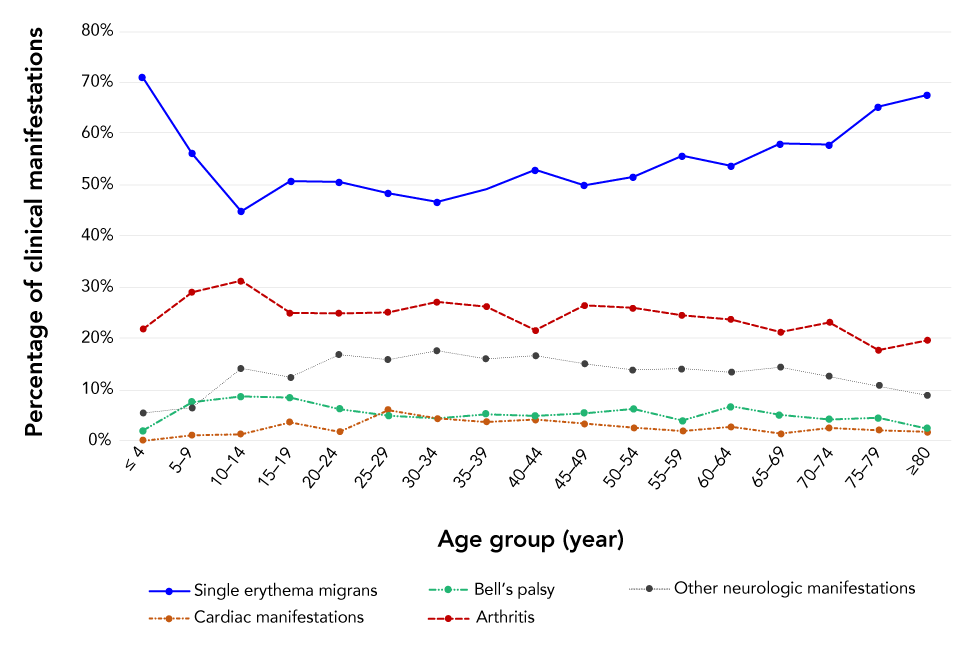
Text description: Figure A1
| Age group (year) | Single erythema migrans | Bell's palsy | Other neurologic manifestations | Cardiac manifestations | Arthritis |
|---|---|---|---|---|---|
| ≤4 | 71% | 2% | 5% | 0% | 22% |
| 5−9 | 56% | 8% | 6% | 1% | 29% |
| 10−14 | 45% | 9% | 14% | 1% | 31% |
| 15−19 | 51% | 8% | 12% | 4% | 25% |
| 20−24 | 50% | 6% | 17% | 2% | 25% |
| 25−29 | 48% | 5% | 16% | 6% | 25% |
| 30−34 | 47% | 4% | 18% | 4% | 27% |
| 35−39 | 49% | 5% | 16% | 4% | 26% |
| 40−44 | 53% | 5% | 17% | 4% | 22% |
| 45−49 | 50% | 5% | 15% | 3% | 26% |
| 50−54 | 51% | 6% | 14% | 3% | 26% |
| 55−59 | 56% | 4% | 14% | 2% | 24% |
| 60−64 | 54% | 7% | 13% | 3% | 24% |
| 65−69 | 58% | 5% | 14% | 1% | 21% |
| 70−74 | 58% | 4% | 13% | 3% | 23% |
| 75−79 | 65% | 5% | 11% | 2% | 18% |
| ≥80 | 67% | 2% | 9% | 2% | 20% |
| Total | 81% | 5% | 14% | 3% | 24% |
