Developing injury indicators for First Nations and Inuit children and youth in Canada: a modified Delphi approach - CDIC: Vol 34, No 4, November 2014
Volume 34 · Number 4 · November 2014
Chronic Diseases and Injuries in Canada
Developing injury indicators for First Nations and Inuit children and youth in Canada: a modified Delphi approach
I. Pike, PhD (1, 2, 3); R. J. McDonald, PhD (3, 4); S. Piedt, BA (2, 3); A. K. Macpherson, PhD (3, 5)
https://doi.org/10.24095/hpcdp.34.4.03
This article has been peer reviewed.
Author references:
- Department of Pediatrics, Faculty of Medicine, University of British Columbia, Vancouver, British Columbia, Canada
- B.C. Injury Research and Prevention Unit, Child and Family Research Institute, B.C. Children's Hospital, Vancouver, British Columbia, Canada
- First Nations and Inuit Children and Youth Injury Indicators Working GroupEndnote *
- Katenies Research and Management Services, Akwesasne Mohawk Territory, Cornwall, Ontario, Canada
- School of Kinesiology and Health Science, Faculty of Health, York University, Toronto, Ontario, Canada
Correspondence: Shannon Piedt, B.C. Injury Research and Prevention Unit, F508-4480 Oak Street, Vancouver, BC V6H 3V4; Tel.: 604-875-2000 ext. 5478; Fax: 604-875-3569; Email: spiedt@cw.bc.ca
Abstract
Introduction: The purpose of this research was to take the initial step in developing valid indicators that reflect the injury issues facing First Nations and Inuit children and youth in Canada.
Methods: Using a modified-Delphi process, relevant expert and community stakeholders rated each indicator on its perceived usefulness and ability to prompt action to reduce injury among children and youth in indigenous communities. The Delphi process included 5 phases and resulted in a refined set of 27 indicators.
Results: Indicators related to motorized vehicle collisions, mortality and hospitalization rates were rated the most useful and most likely to prompt action. These were followed by indicators for community injury prevention training and response systems, violent and inflicted injury, burns and falls, and suicide.
Conclusion: The results suggest that a broad-based modified-Delphi process is a practical and appropriate method, within the OCAP™ (Ownership, Control, Access and Possession) principles, for developing a proposed set of indicators for injury prevention activity focused on First Nations and Inuit children and youth. Following additional work to validate and populate the indicators, it is anticipated that communities will utilize them to monitor injury and prompt decisions and action to reduce injuries among children and youth.
Keywords: First Nations, Inuit, indigenous populations, injury indicators, modified-Delphi technique, surveillance
Introduction
Injury has been recognized as an important health problem, one that strikes particularly hard at the most vulnerable people—children, youth, seniors and indigenous populations.Endnote 1 Injury is the leading cause of death among Canadian children, youth and young adults—a situation particularly important to indigenous First Nations and Inuit communities as more than 50% of their populations are under 25 years of age.
Injury is by far the greatest source of potential years of life lost (PYLL) among First NationsEndnote ** populations. At almost 3.5 times the national average, injury accounts for 26% of deaths among First Nations, compared with 6% of deaths overall in Canada.Endnote 2, Endnote 3 The injury rates among indigenous teens are almost 4 times greater than those of non-indigenous Canadians, and First Nations male and female youth are, respectively, 5 to 7 times more likely to die of suicide than their peers in other populations.Endnote 1, Endnote 4 Hospitalization rates due to injury are also significantly higher (twice the rate) for children and youth living in areas with a high percentage of indigenous residents compared to those living in areas with a low percentage of indigenous residents.Endnote 5
To begin to address these injury disparities, respectful approaches that are collaborative, sustainable and culturally sensitive and that reflect the unique identities of First Nations and Inuit peoples are recommended. Endnote 2, Endnote 6 In 2004, the Canadian Child and Youth Health Coalition listed injury prevention/trauma as one of the theme areas to establish Canadian infant, child and youth health indicators.Endnote 7 Despite this, Canada had fallen behind comparable countries in many of the key health indicators for children and youth.Endnote 8 A 5-year injury prevention strategic plan indicated the need to identify injury prevention programs and strategies within Inuit communities and establish an integrated surveillance system to measure injury trends.Endnote 9 And, while the First Nations Regional Longitudinal Health Survey gathers valuable individual and community information in Canada, some of which is focused on injury, no systematic gathering of comprehensive injury information currently takes place across the country for First Nations children and youth.
The purpose of this research was to take the initial step to develop valid indicators reflective of the injury issues facing First Nations and Inuit children and youth in Canada. The research builds upon the initial work of the Canadian Injury Indicators Development Team, a group of national injury prevention researchers, practitioners and policy makers who established national injury indicators for Canadian children and youth.Endnote 10 CryerEndnote 11,p.3-1 defined an injury indicator as "…a summary measure which denotes or reflects, directly or indirectly, variations and trends in injury, or injury-related or an injury control-related phenomenon." The specific aims of our present study were:
- to develop a strong collaborative working group of individuals and agencies representing indigenous peoples, and
- to develop and specify a suite of valid indicators that can provide a baseline for First Nations and Inuit communities to document, analyze and report child and youth injury data.
Once the indicators are populated with data, the resulting information can be used to support community injury prevention decision-making and action planning. Tracked over time, these indicators can show how a community or group's injury profile has changed.Endnote 12
An indicator is valid when itmeasures what it is presumed to measure.Endnote 13 The indicators in this study were developed based upon the work of the International Collaborative Effort on Injury Statistics (ICE)Endnote 11 in 2001 and subsequent work by Cryer et al.Endnote 14 that outlined criteria for indicator validity. These criteria suggest that an ideal indicator for injury cases should
- have a case definition based on diagnosis–on anatomical or physiological damage;
- focus on serious injury;
- have, as far as possible, unbiased case ascertainment;
- be derived from data that are representative of the target population;
- be based on existing data systems (or it should be practical to develop new data systems that would feed into it); and
- be fully specified in writing.
Methods
In early 2007, the First Nations and Inuit Health Branch, Health Canada invited the Canadian Injury Indicators Team to begin a 3-year project to develop injury indicators for First Nations and Inuit children and youth. In Canada, First Nations and Inuit peoples are represented by many local, regional and national indigenous agencies as well as the federal government departments whose responsibility it is to ensure the provision of health and social programs, including initiatives to reduce injury.
From the outset, the process and methods of this project sought to balance scientific rigour and a community-oriented approach consistent with the OCAP™ principles underlying the collection of indigenous peoples' data and information in Canada. That is, the data are Owned, Controlled, Accessed and Possessed by the indigenous community.Endnote 15 Briefly, the process attempted to ensure a practical approach to injury indicator development.
The First Nations and Inuit Health Branch, Health Canada identified relevant participants in this research and therefore included representatives from the Assembly of First Nations, Inuit Tapiriit Kanatami, Royal Canadian Mounted Police, Indian and Northern Affairs Canada, the SMARTRISK Foundation, Children's Hospital of Eastern Ontario, Plan-It-Safe Program, Katenies Research and Management Services, Statistics Canada, Nunatsiavut Department of Health and Social Development and Pauktuutit Inuit Women of Canada. Twenty-one participants from these agencies came together to plan the project and commence the process; together they formed the First Nations and Inuit Child and Youth Injury Indicators Project Working Group.
A multi-phase modified-Delphi research design was adapted from the methods described by Lindsay et al.Endnote 16 and applied to the development of injury indicators for First Nations and Inuit children and youth. The choice of each indicator was based on limited available data and information describing the burden of injury on First Nations and Inuit children and youth, previous prevention research and best practices and ongoing input from expert Working Group members and their respective networks.
Phase I: Literature review
Phase I included a review of the relevant literature, with the goal of identifying any previously established valid and evidence based First Nations and Inuit child and youth injury indicators. Research analysts at the First Nations and Inuit Health Branch, Health Canada conducted the literature review based upon the methodology used by Pike et al.Endnote 10 using the following databases for the period 1985 to 2007, inclusive: Medline, Ovid, Transport, Transportation Research Information Services, Sportdiscus, Cumulative Index to Nursing and Allied Health Literature, Embase, Psychinfo, Healthstar and Hispanic American Periodicals Index. The search also included indigenous agency and government websites and program report listings as a means of accessing relevant grey literature. The research analysts identified and summarized a total of 10 studies from the peer-reviewed and grey literature (list available from the authors upon request). The review of literature revealed an initial list of 48 injury indicators.
Phase II: Establishing important injury categories and ranking injury indicators
Of the 21-member Working Group, 19 were able to meet and agree on 4 areas in which to group child and youth injury indicators relevant to First Nations and Inuit communities: workplace, home and public safety; transport; sport and recreation; and inflicted injury / violence (including self-inflicted injury). Using their expertise, personal experience and knowledge of the research, the group discussed the most common injuries within each area and a way to potentially measure and monitor those injuries. As a result, 4 types of indicators were defined and described: outcome, risk and protective factors, program and policy.
The group then divided into small groups based on the 4 injury areas and reviewed the 48 indicators suggested by the literature review, adding additional indicators where deemed appropriate. Following full review and discussion, each small group presented their list of indicators to the large group. All in all, the list included 170 indicators.
With the goal of reducing the number of indicators while retaining those considered important and reflective of the community child and youth injury issues, the Working Group undertook another exercise to prioritize the indicators. In this exercise, the list of indicators was posted on flip charts. Participants were each given 55 paper adhesive dots (approximately one-third the number of the posted indicators) and instructed to position these beside those indicators they considered the most important. All indicators that were marked with 10 or more dots (representing an initial indication of importance) were retained and the remainder rejected. This N/3 technique of prioritizingEndnote 17 resulted in a list of 62 indicators that were regrouped by the participants from the original 4 into 7 broad injury categories: all injury areas; animal bites and hypothermia / frostbite; violent/inflicted injury; burns and falls; drowning; suicide; and motorized vehicle collisions.
The criteria used to inform priority setting included choosing injury indicators that
- reflected a significant burden to First Nations and Inuit peoples, their families and the health care system, and
- could be acted upon through prevention initiatives.
Further, the participants were provided the International Collaborative Effort Injury Indicators Group (ICEIInG) criteria for indicator validity to inform their decision-making.
The subsequent step was to review and further refine the list of 62 indicators. Working Group members were asked to consult with their constituent groups and, for each indicator, recommend whether to "keep" or "let go" of it or whether they were "unsure" based upon 3 criterion questions:
- Is this indicator important in your community?
- Would this indicator help you to track injuries in your community?
- Does this indicator give you sufficient information to take action to prevent injuries among children and youth in your community?
We reviewed the responses and retained those indicators that a majority of the Working Group had recommended keeping. Indicators that received a majority of "let go" responses were dropped. (No indicators received a majority vote of "unsure."') During this phase of the process and as a result of discussion among themselves, Working Group members proposed 2 additional indicators, which were circulated and judged to be important enough to keep: the percentage of children/ youth enrolled in "learn to swim" programs and percentage of violent offenders participating in restorative justice programs were included as additional potential indicators, resulting in a list of 36 injury indicators at this stage.
Phase III: Regional feedback
Further input was sought from potential users at the community level. Investigators attended regional meetings and engaged First Nations and Inuit injury prevention practitioners and decision makers. At each meeting, the project was explained and participants were asked for their feedback on the list of 36 child and youth injury indicators.
Feedback on each injury indicator was obtained from a number of regional organizations in Alberta, Manitoba, Ontario, Quebec and Nunatsiavuut: the Manitoba Community Wellness Working Group, the Assembly of First Nations Regional Injury Prevention Working Group, the First Nations Early Childhood Circle (representatives from Saskatchewan Aboriginal Head Start Initiative and Federation of Saskatchewan Indian Nations), Chiefs of Ontario and the National Inuit Council on Health.
In this phase of the process, regional agency representatives identified 7 additional indicators judged to be important in understanding and preventing child and youth injury in their communities. As a consequence, the list of potential injury indicators increased from 36 to 43.
Phase IV: Specification of indicators
We created a standard template for indicator specification (see Table 1) and developed draft specifications for the 43 indicators based upon the format for previous reports from Australia,Endnote 18 New Zealand,Endnote 19 EuropeEndnote 20 and Canada.Endnote 21
TABLE 1
Template for the specification of child and youth injury indicators
| Indicator |
| Definition |
| Definition of relevant terms |
| Justification for this indicator |
| Operational definition of a case |
| Method of calculation |
| Numerator |
| Denominator |
| Data sources, availability and quality/years represented |
| Units of measurement |
| Guide for use |
| Scope of indicator |
| Specification of data needed |
| Limitations |
| How to use this indicator |
The Working Group then met to discuss, revise and refine the indicators and their specifications, and an additional round of review and further feedback was accomplished via email. Nine members of the Working Group respondedEndnote † and recommended that several indicators be dropped due to the lack of available data and the difficulty and cost associated with generating new data collection systems to populate those indicators. Phase IV resulted in a further refined list of 33 candidate injury indicators (see Table 2).
TABLE 2
Ratings of usefulness and ability to prompt action of First Nations and Inuit child and youth injury indicators
Indicator
domain/area |
Indicator |
Usefulness mean
(SD) rating [1-9] |
Prompt action mean
(SD) rating [1-9] |
|
|
| Across all injury areas |
Mortality rate: number of deaths per 10 000 children and youth due to each type of injury |
9.00 (0.0) |
8.11 (1.5) |
| Hospitalization rate: number of hospitalizations per 10 000 children and youth due to each type of injury |
8.56 (0.9) |
7.67 (1.5) |
| Number and proportion of self-reported alcohol, solvent and substance use among First Nations children and youth (based on RHS data) |
6.63 (1.8) |
6.44 (2.1) |
| Number of communities that have culturally appropriate alcohol / drug programs available for community members |
4.88 (2.2) |
5.00 (2.4) |
| Number of self-governing features that exist in the community |
6.78 (2.7) |
6.11 (3.0) |
| Potential years of life lost (PYLL) due to injury among children and youthTable 2 - Footnote a |
n/a |
n/a |
| Community injury prevention training/response systems |
Proportion of community members who complete injury prevention training |
7.11 (1.3) |
6.33 (1.4) |
| Presence of a community emergency preparedness plan (i.e. flooding, fires, blizzards, earthquakes, etc.) |
7.78 (1.2) |
7.44 (1.1) |
| Availability of fire and ambulance services in a community within a defined response time |
7.56 (1.2) |
6.56 (1.9) |
| Animal bites |
Rate of injuries due to animal bites and maulings per 10 000 children and youth in a community |
8.44 (0.9) |
7.67 (1.9) |
| Number and proportion of communities with Animal Control Services |
7.25 (1.3) |
6.50 (2.2) |
| Hypothermia/Frostbite |
Rate of hypothermia or frostbite per 10 000 children and youth |
7.25 (1.4) |
5.63 (2.2) |
| Violent/inflicted injury |
Number and proportion of police calls and charges related to violent injury per 10 000 children and youth |
8.33 (0.9) |
7.56 (0.4) |
| Self-reported rate of inflicted injury (violence and abuse) per 10 000 children and youth (not including self-inflicted injuries) |
7.78 (1.1) |
7.00 (1.3) |
| Number and proportion of violent offenders participating in restorative justice programs |
5.00 (3.2) |
5.00 (3.0) |
| Burns and falls |
Number and proportion of homes in a community with working smoke detectors, tested fire extinguishers and carbon monoxide detectors |
8.33 (0.5) |
8.11 (0.8) |
| Number and proportion of self-reported burns among children and youth as well as the self-reported circumstantial details of each case |
7.13 (2.4) |
6.38 (2.4) |
| Place where falls among children and youth happen (this refers to self-reported falls to children and youth within the previous 12 months) |
8.44 (0.7) |
7.33 (1.4) |
| Drowning |
Number and proportion of communities with Emergency Response Teams |
7.11 (1.5) |
6.78 (1.5) |
| Number and proportion of communities with access to water safety education/programs |
7.89 (1.3) |
7.22 (0.8) |
| Enforcement of laws related to water |
5.13 (2.5) |
4.63 (2.2) |
| Number and proportion of children and youth who drown each year, including type of body of water and circumstances |
8.56 (0.7) |
7.33 (1.0) |
| Number and proportion of children and youth enrolled in "learn to swim" programs in a specific year |
7.67 (1.0) |
6.50 (1.2) |
| Suicide |
Number of communities with mental health and wellness promotion programs |
6.50 (2.8) |
6.86 (2.3) |
| Rate of self-reported poor mental health among children and youth |
7.89 (0.8) |
6.56 (1.9) |
| Rate of suicide attempts/self-harm and completed suicides per 10 000 children and youth |
8.78 (0.4) |
7.44 (1.0) |
| Rate of calls to suicide prevention crisis telephone services, by geographical region |
7.67 (1.0) |
7.22 (0.8) |
| Motorized vehicle collisions |
Rate of motorized vehicle collisions involving children and youth, by type of vehicle and crash circumstances |
8.78 (0.4) |
8.00 (1.0) |
| Number and proportion of seriously injured children and youth occupants who were unrestrained (not wearing a seatbelt) in a motor vehicle collision |
8.67 (0.5) |
8.22 (1.4) |
| Number and proportion of youth who enrolled in and completed driver education courses–skills for car, snowmobile, boat and ATV drivers |
8.22 (0.7) |
7.22 (1.0) |
| Proportion of motor vehicles demonstrating proper use of child vehicle restraints (car seats) and booster seats by community |
8.78 (0.4) |
8.33 (1.0) |
| Age and sex of drivers and occupants involved in motor vehicle crashes by vehicle type (car, van, truck, ATV, snowmobile) and road user (driver, passenger, pedestrian, cyclist) |
8.33 (0.9) |
7.67 (1.4) |
| Presence of legislation of minimum age to drive an ATV. Number of provinces and territories with legislation of minimum age to drive an ATV |
7.13 (2.2) |
6.00 (2.7) |
| Number and proportion of seriously injured or killed children and youth not wearing a helmet while riding ATVs, snowmobiles and/or bicycles by community |
8.67 (0.5) |
8.11 (0.9) |
Phase V: Finalizing injury indicators
Following the specification of all 33 indicators, the Working Group met for the last time in December 2008 with 13 members attending. Each indicator was rated for perceived usefulness and ability to prompt action to reduce injuries among First Nations and Inuit children and youth using a 9-point scale,with 1 being low (not useful, not actionable) and 9 being high (very useful, very actionable). This resulted in 7 indicators being judged as neither useful nor actionable (and therefore not meeting the criteria for validity), either because of lack of data and/or resources availability, and were dropped (see the shaded indicators in Table 2). The process concluded with the Working Group endorsing a final list of 27 injury indicators for First Nations and Inuit children and youth.
Immediately following the rating process, the group unanimously agreed to re-insert PYLL due to injury, which had been listed at the review of literature stage, although they did not rate it.
Results
The modified-Delphi method resulted in a proposed list of 27 injury indicators. Indicators related to motorized vehicle collisions, mortality rates and the number of children and youth hospitalized due to each injury type ranked highest in terms of usefulness and ability to prompt action. These were followed by community injury prevention training and response systems, violent and inflicted injury, burns and falls, and suicide although some were rated somewhat lower in terms of their ability to prompt action.
Discussion
This modified-Delphi approach represents the first step in the indicator development process that resulted in a final proposed set of 27 First Nations and Inuit child and youth injury-related indicators that can be used to inform injury prevention in Canada's indigenous peoples. While there was some variation in the degree to which experts rated the usefulness and likelihood to prompt action of each indicator, there was general consistency and agreement. The high scores given to the injury indicators suggest that they capture the needs of those working to prevent injuries among First Nations and Inuit children and youth.
While the indicators were developed to apply to First Nations and Inuit children and youth, some indicators are applicable to any children and youth living in rural or remote communities, and others apply to all children and youth.
Strengths and limitations
There are some limitations to this work, which are important to highlight here.
First, there is a paucity of published literature related to indigenous child and youth injury prevention to inform the decision-making around the indicator selection.
Second, the modified-Delphi process technique used is subjective and based upon participant expertise and experience. While efforts to be objective in generating and prioritizing indicators were made within the process, the results depend upon the opinions of the participating experts. Participants were advised of the criteria for indicator validity, but it is not known how much that influenced their choice of indicators. It is possible that the results would be different had a different group of experts participated. However, the experts chosen were those deemed most relevant to the process because they were knowledgeable about the field and the best representatives of their agencies and constituents.
A further limitation is the current and continuing lack of the data necessary to populate the indicators. Some indicators had no data available, and may not have in the foreseeable future. However, data for many of the indicators are available from the First Nations Regional Longitudinal Health Survey, and some communities (e.g. 10 bands of the Secwepemc Nation in British Columbia) collect health and injury data that can populate the indicators. In addition, we anticipate that, with time, more communities will gather their own data and information of local interest and relevance to child and youth injury prevention. This approach is consistent with the OCAP™ principles.Endnote 15
Conclusion
Using a systematic, interdisciplinary modified-Delphi method, which involved direct input and leadership from First Nations and Inuit experts, this study resulted in a proposed list of 27 useful and actionable injury indicators to guide First Nations and Inuit community injury prevention initiatives focused on children and youth.
While several of the indicators are in line with those developed for non-indigenous Canadian children and youth,Endnote 10 differences do exist. Most important, the current indicators are specific to injury among First Nations and Inuit children and youth, reflecting local circumstances and conditions important to injury risk and prevention in indigenous communities, some of which are small, rural and remote. For example, the First Nations and Inuit indicators included those that relate to community injury prevention training and response systems, animal bites, drowning, hypothermia and frostbite, which were considered less important for non-indigenous populations.
Further research and collaboration by the Working Group with indigenous communities will demonstrate the utility of the indicators in furthering injury prevention. Work will continue to identify the necessary appropriate data and information to populate the indicators. It is anticipated that the research team will work with communities to gather the necessary data and information to populate the indicators, including helping develop consistent definitions of causes of injury and injury severity. Ultimately, indigenous health authorities and communities can use the information to plan, implement and evaluate programs and initiatives to prevent injury among children and youth, consistent with the OCAP™ principles underlying research among Canadian indigenous communities.
Acknowledgments
Funding for this study was provided by the First Nations and Inuit Health Branch at Health Canada (FNIHB), the BC Child and Youth Health Research Network (CYHRNet) and the Canadian Institutes of Health Research (KTB-109190).
The authors wish to acknowledge all members of the First Nations and Inuit Child and Youth Injury Indicators Working Group for their contribution to this research. We would like to acknowledge the First Nations and Inuit Health Branch, Health Canada (FNIHB) and the BC Child and Youth Health Research Network (CYHRNet) for providing the funds to conduct this study and for their support in ensuring timely access to essential resources. In addition, we wish to thank the Assembly of First Nations (AFN), Inuit Tapiriit Kanatami (ITK), Pauktuutit Inuit Women of Canada and the Canadian Institutes of Health Research. We are most grateful to these organizations for the important resources provided and for their ongoing support to facilitate the process of refining our final list of indicators. We also wish to thank the Manitoba Community Wellness Working Group, the AFN First Nations Regional Injury Prevention Working Group, the First Nations Early Childhood Circle (representatives from the Saskatchewan Aboriginal Head Start Initiative and Federation of Saskatchewan Indian Nations), the Chiefs in Ontario, the AFN Health Officers Council, the representatives of the First Nations Regional Longitudinal Health Survey and the National Inuit Committee on Health for their input during the process of determining and refining the list of indicators.
References
Appendix
Injury Indicators for First Nations and Inuit Children and Youth Specification Details for Injury Indicators
Introduction
First Nations and Inuit children and youth experience a significantly higher rate of injury-related death and disability than other young people in Canada. An accurate determination of the factors related to injury as well as the ability to monitor trends and patterns among First Nations and Inuit children and youth is desirable to assist with prevention. Building upon previous work by the Canadian Injury Indicators Development Team to establish national injury indicators for Canadian children and youth, the purpose of this research was to take the initial step to develop valid indicators reflective of the injury issues facing First Nations and Inuit children and youth in Canada.
The specific aims of the present study were
- to develop a strong collaborative working group of individuals and agencies representing indigenous peoples, and
- to develop and specify a suite of valid indicators that can provide a baseline for First Nations and Inuit communities to document, analyze and report child and youth injury data.
The collaborators in this project committed to follow principles and ethics reflecting indigenous research in Canada. Specifically, the First Nations OCAP™ principles of Ownership, Control, Access, and Possession of Indigenous data, information and knowledge.
Once the indicators are populated with data, the resulting information can be used to support community injury prevention decision making and action planning; tracked over time, these indicators can tell a story of how a community or group's injury profile has changed. As such, this specification document represents a draft document that will be updated as indicators are populated and utilized.
The Process
In early 2007, the Canadian Injury Indicators Team was invited by the First Nations and Inuit Health Branch, Health Canada to begin a 3-year project to develop injury indicators for First Nations and Inuit children and youth. In Canada, First Nations and Inuit peoples are represented by many local, regional and national indigenous agencies as well as departments of the Federal Government whose responsibility it is to ensure health and social programs including initiatives to reduce injury are provided. Relevant participants in this research were identified by the First Nations and Inuit Health Branch (FNIHB), Health Canada, and included representatives from the Assembly of First Nations, Inuit Tapiriit Kanatami, Royal Canadian Mounted Police, Indian and Northern Affairs Canada, the SMARTRISK Foundation, Children's Hospital of Eastern Ontario, Plan-It-Safe Program, Katenies Research and Management Services, Statistics Canada, Nunatsiavut Department of Health and Social Development, and Pauktuutit Inuit Women of Canada. Twenty-one participants from these agencies came together to plan the project and commence the process. Together, they formed the First Nations and Inuit Child and Youth Injury Indicators Project Task Group.
Using a modified-Delphi process, this research first developed valid indicators reflective of the injury issues facing First Nations and Inuit children and youth in Canada. Relevant expert and community stakeholders rated each indicator on its importance to their community to:
- assist in monitoring injuries, and
- its usefulness and
- its ability to prompt action to reduce injury.
From an initial list of 48 indicators based upon a literature review, a refined set of 27 indicators was established. Indicators related to motorized vehicle collisions, mortality and hospitalization rates were rated the most useful and most likely to prompt action. These were followed by community injury prevention training and response systems, violent and inflicted injury, burns and falls, and suicide indicators. Following additional work to populate the indicators, it is anticipated that communities will utilize them to monitor injury and prompt decisions and action to reduce injuries among children and youth.
To ensure a standard approach to populating and utilizing the injury indicators, this document details how best to use the information as a community injury prevention resource and provides the detailed specification of each indicator.
How to Use This Document
It is intended that the indicators listed in this document will help to identify the burden of indigenous child and youth injuries on families, communities and regions so that decision and action to prevent injuries is prompted. The statistics in this document make it clear that more needs to be done to promote/improve injury prevention efforts for all children and youth.
Community leaders and community members can use the indictors to
- identify trends and patterns in injury in the community so that injury prevention resources can be targeted where most needed
- gather statistical data to support a request for further injury prevention resources
- evaluate the impact of injury prevention interventions
Regional leaders, researchers or policy makers can use the indicators to
- identify trends and patterns in injury for a whole region so that injury prevention resources can be targeted where most needed
- compare injury outcomes between communities with the goal to identify community-specific best practices in injury prevention
- evaluate the impact of injury prevention interventions
Commonly Used Terms in This Document
The First Nations Regional Longitudinal Health Survey (RHS) is a national survey that produces health and social data for on-reserve First Nations communities (on-reserve) across the country. It is conducted across the 10 regions in Canada, surveying participants in over 200 First Nation communities. The First Nations Information Governance Centre provides oversight to the RHS.
The RHS is a source of First Nations data for many of the indicators, using 4 survey components:
- Adult (≥18 years, self-reported)
- Youth (12–17 years, self-reported)
- Child (0–11 years, completed by primary care giver)
- Community Survey
The Aboriginal Peoples Survey (APS) is a National Survey of First Nations, Inuit and Métis people in Canada (Statistics Canada, 2007), conducted by Statistics Canada.
The Canadian Community Health Survey (CCHS) is conducted by Statistics Canada and collects information from over 130 000 respondents, aged 12 years or older, residing in households across all provinces and territories. The survey includes a section on injuries (Statistics Canada, 2005). Profiles are presented by a series of variables by different geographies, such as health regions, census metropolitan areas and rural/urban groups. CCHS has a profile for Aboriginals, but does not specify First Nations or Inuit.
International Classification of Disease Codes (ICD-10) is a coding system used to classify diseases and other health problems recorded on many types of health and vital records including death certificates and hospital records. In addition to enabling the storage and retrieval of diagnostic information for clinical and epidemiological purposes, these records also provide the basis for the compilation of national mortality and morbidity statistics by WHO Member States (World Health Organization, 2008). This document uses the term ICD-10-CA, which refers to version 10 in Canada.
Advocacy: For the purposes of this document, advocacy may include promoting and encouraging behaviour change, local interventions and seeking support at all levels of government and from non-government organizations (NGOs).
Injury Indicator Specifications Tables
The purpose of the Injury Indicator Specification Tables that follow is to clearly define and specify each of the 27 indigenous child and youth injury indicators. These tables are intended to provide community injury prevention leaders and practitioners, policy makers and non-governmental organizations with greater understanding of the indicators and their application in a consistent manner.
The detailed injury Indicator Specification Tables provide information on the key components of each indicator, including:
- A clear definition of the indicator itself, as well as definitions of important key terms
- Inclusion and/or exclusion criteria
- The underlying rationale for each indicator, including why it is important, what it means and how it should be interpreted.
It should be noted, however, that although each indicator is defined and specified, not all of the suggested or required data and/or information are available in Canada at this time. Utilization of the indicators and future research will serve to demonstrate the utility of these indicators to further injury prevention research, policy and practice.
In essence, it is hoped that these Indicator Specification Tables will encourage community practitioners, in particular, to think about the data and information they gather in their own communities, allow them to monitor their own local injury prevention systems and enable them to develop new local injury prevention initiatives based on what they learn.
FIGURE 1
Injury Indicator Specifications Table Attributes
[FIGURE 1, Text Equivalent]
Chronic Diseases and Injuries in Canada - Volume 34, Number 4, November 2014
Injury Indicator Specifications Table Attributes
The Indicator Specification Tables describe a number of attributes for each indicator. The diagram below numbers each individual attribute and is followed by corresponding definitions.
- Type of Indicator: Indicators are classified using 3 types of indicators.
- Community Training and Capacity – captures data regarding injury prevention training and capacity currently in place. Further work is needed to reflect the degree to which best practice is reflected within training and capacity-building programs.
- Risk / Protective Factor – captures data regarding the use or non-use of protective equipment. Child restraint use, seatbelt use, helmet use are all examples of risk indicators.
- Outcome – captures the sequelae of injuries. The number of children and youth who die or who are injured and the causes of those injuries give us a picture of the burden of injury in indigenous communities in Canada.
- Indicator Domain: Indicators are grouped in 9 domains, based upon the burden of injury and the collective expertise of the expert team. The Indicator Specification Tables are organized by domain, in the following order:
- Across All Injury Areas
- Community Injury Prevention Training / Response Systems
- Animal Bites
- Hypothermia/Frostbite
- Violent / Inflicted Injury
- Burns and Falls
- Drowning
- Suicide / Self-Harm
- Motorized Vehicle Collisions
- Indicator Number and Title: Each indicator is identified by a title and a number, assigned sequentially.
- Indicator Definition: Provides a concise definition of the specific aspects that the indicator addresses.
- Definition of Relevant Terms: Provides a definition for the relevant technical terms used within the indicator definition or description.
- Justification for this Indicator: Explains the importance and relevance of the indicator to indigenous community child and youth injury prevention.
- What are we Counting? Definition of a case.
- Where do we obtain data / information for this indicator? Identifies data sources that can be used to calculate the indicator.
- What data do we need? Specific description of the data required for the indicator.
- Method of Calculation: Provides a method of calculation and, for rate-based indicators, provides the description of the general specifications of any component that is the basis for inclusions and exclusions in the numerator and denominator needed to calculate it.
- Numerator: Used in calculation.
- Denominator: Used in calculation.
- Limitations: Identifies limitations specific to each indicator.
Injury Indicator Specifications Table Attributes
The Indicator Specification Tables describe a number of attributes for each indicator. The diagram below numbers each individual attribute and is followed by corresponding definitions.
- Type of Indicator: Indicators are classified using 3 types of indicators.
- Community Training and Capacity – captures data regarding injury prevention training and capacity currently in place. Further work is needed to reflect the degree to which best practice is reflected within training and capacity-building programs.
- Risk / Protective Factor – captures data regarding the use or non-use of protective equipment. Child restraint use, seatbelt use, helmet use are all examples of risk indicators.
- Outcome – captures the sequelae of injuries. The number of children and youth who die or who are injured and the causes of those injuries give us a picture of the burden of injury in indigenous communities in Canada.
- Indicator Domain: Indicators are grouped in 9 domains, based upon the burden of injury and the collective expertise of the expert team. The Indicator Specification Tables are organized by domain, in the following order:
- Across All Injury Areas
- Community Injury Prevention Training / Response Systems
- Animal Bites
- Hypothermia/Frostbite
- Violent / Inflicted Injury
- Burns and Falls
- Drowning
- Suicide / Self-Harm
- Motorized Vehicle Collisions
- Indicator Number and Title: Each indicator is identified by a title and a number, assigned sequentially.
- Indicator Definition: Provides a concise definition of the specific aspects that the indicator addresses.
- Definition of Relevant Terms: Provides a definition for the relevant technical terms used within the indicator definition or description.
- Justification for this Indicator: Explains the importance and relevance of the indicator to indigenous community child and youth injury prevention.
- What are we Counting? Definition of a case.
- Where do we obtain data / information for this indicator? Identifies data sources that can be used to calculate the indicator.
- What data do we need? Specific description of the data required for the indicator.
- Method of Calculation: Provides a method of calculation and, for rate-based indicators, provides the description of the general specifications of any component that is the basis for inclusions and exclusions in the numerator and denominator needed to calculate it.
- Numerator: Used in calculation.
- Denominator: Used in calculation.
- Limitations: Identifies limitations specific to each indicator.
Indicators
Indicator #1 - Injury Mortality Rate
| Across All Injury Areas |
Outcome |
| Indicator Definition |
The cause-specific indigenous child and youth (ages 0–19 years) injury mortality rate per 10 000 population for a particular year. Where data exist, rate can be stratified by injury cause (excluding patient safety/complications/ medical misadventures), sex, age, socioeconomic status and geographic location. |
| Definition of Relevant Terms |
Injury is the damage to the body resulting from acute exposure to thermal, mechanical, electrical or chemical energy or from the absence of such essentials as heat or oxygen.
Unintentional injuries are those injuries where there is no intent to do harm. They are typically classified according to the means of their occurrence (e.g. poisoning, burns and scalds, drowning, falls and transport-related).
Violent injuries (intentional injuries) resulting in child or youth death are also included in this definition of mortality and are classified according to intentional self-harm, maltreatment or assault.
Mortality data are based on children and youth killed immediately or dying within 30 days as a result of an unintentional or violent injury. |
| Justification for This Indicator |
Injury is a serious public health issue with a major impact on the lives of First Nations and Inuit as it is the number one cause of hospitalization and death among people aged 1–44 years (Health Canada, 1999). Injuries kill more indigenous children and young adults than all diseases combined and include both unintentional and intentional injuries. Injuries in children and youth are largely avoidable.
The mortality rate is perhaps the best indication of the burden of severe childhood injury. It is essential to track the mortality rate over time to assess trends in childhood injury. |
| What are we counting? (definition of a case) |
Cases will be identified by the nature of injury codes (ICD-10 S00–T98) and the external cause of injury codes (V01–Y98) recorded in mortality data files. |
| Where do we get this information / data? |
The central Vital Statistics Registry in each province and territory records data from death registrations. Regional offices of the First Nations and Inuit Health Branch (FNIHB), Health Canada have access to vital statistics with a First Nations or Inuit identifier. |
| What data do we need? |
Total number of deaths due to injury for all causes for children aged < 1, 1–4, 5–9, 10–14, 15–19 years and by male/female.
Population of children and youth broken down by age (< 1, 1–4, 5–9, 10–14, 15–19 years), male/female.
Mortality data broken down by external cause of death (ICD-10 Codes V01–Y98). |
| Method of Calculation |
(Numerator/Denominator) x 10 000 |
| Numerator |
Number of deaths stratified by: age, sex, each unintentional injury and each violent injury |
| Denominator |
Total resident population stratified by: age and sex. This can be obtained from FNIHB regional offices. |
| Limitations |
British Columbia
Data for Registered Indians in British Columbia were gathered through a data linkage with the British Columbia Vital Statistics Agency. These data include all Registered Indians, on- and off-reserve combined. Since the British Columbia Vital Statistics Agency use the Status Verification System (SVS) in their linkage, which includes both Registered Indian and Inuit clients, this data file will include some Inuit. The SVS file that the British Columbia Vital Status Agency uses, however, is for all of Canada. This means that Registered Indians (and Inuit) who have moved to British Columbia from elsewhere in Canada would also be captured, if they died or gave birth while living in the province.
Alberta
Data for all Registered Indians, on- and off-reserve combined, were obtained through a manual records match carried out by the Health Canada regional office in Alberta using the SVS and provincial vital statistics records. The Regional SVS file is used instead of the national list, so information is gathered only for Registered Indians who are members of Alberta bands. Data were classified using ICD-10 classification.
Saskatchewan
Data for Registered Indians were extracted from the provincial vital statistics database through an Aboriginal identifier in the dataset. These data were supplemented with a linkage with the SVS and provincial health records, to include individuals not flagged with an Aboriginal identifier. Saskatchewan Region uses the national version of the SVS, which includes Registered Indians and Inuit from across Canada. Data are broken down by the on- and off-reserve populations. Data are received in ICD-10 classification.
Manitoba
Data for First Nations are extracted from the provincial vital statistics database using an Aboriginal identifier. This identifier is voluntary, in that a person must identify themselves as a Registered Indian to the Manitoba Vital Statistics Agency. These individuals are double-checked through a manual records match with the SVS and the provincial dataset. This also identifies Registered Indians who were not flagged in the provincial records. These data are available for the on- and off-reserve populations. Data are reported in ICD-10 format.
Ontario
No vital statistics
Quebec
The Quebec Regional Office does not receive any information from the provincial Vital Statistics Registry. Reports on vital statistics are received from the communities that are covered under a health control transfer agreement and entered into a database. As the FNIHB regional office does not have full health information on each death, there is concern that determining the underlying cause of death is not possible. This reporting system covers only communities that have had their health care control transferred from Health Canada (29 of the 41 communities), and none of the off-reserve population is covered.
Atlantic
As with Quebec, theFNIHB Atlantic regional office does not receive any information from the vital statistics registries of any of the Atlantic provinces. Instead, they receive reports on births and deaths from the communities. Information is collected from community health nurses and submitted to the Atlantic regional office using Teleform, a fax-based database application. This system collects information from reserves and does not cover the off-reserve population. Although the Inuit communities in northern Labrador are not included in this reporting scheme, a small number of Inuit from other communities might be included in these data. The system of reporting deaths toFNIHB is voluntary and is often based on second-hand information received by the nurse from the family. The number of death reports received by the regional office is believed to be a severe underestimation of the actual number of deaths that occur in the region.
The Territories
The Territories do not identify First Nations or Inuit people separately in their vital statistics. |
Indicator #2 - Injury Hospitalization Rate
| Across All Injury Areas |
Outcome |
| Indicator Definition |
The number of child and youth (ages 0–19 years) hospital separations per 10 000 population for a particular year, for all injuries by male, female and total, stratified by age, socioeconomic status and geographic health region when available (excluding patient safety/complications/medical misadventures). |
| Definition of Relevant Terms |
The hospital separations rate indicates how many children/youth are discharged from hospital for each type of injury each year.
Hospital Separation is defined as the number of in-patient separations that leave hospital through discharge, transfer or death. Data for age group, ICD code and gender are available resulting in the number of separations each year. Hospital separations do not tell you if it is one person being discharged 3 times or 3 different people. |
| Justification for This Indicator |
The hospital separation rate is a key measure of the use of health services related to injury. It can give a sense of the burden of injury to the health care system, communities, children and their families. |
| What are we counting? (definition of a case) |
Cases will be identified by the nature of injury and the external cause of injury codes (V01–Y98) recorded in hospital separations data files. |
| Where do we get this information / data? |
British Columbia, Alberta, Saskatchewan and Manitoba are able to identify First Nations people from hospitalization data. The remaining provinces and territories do not have a “unique identifier.”
To obtain hospitalization data, a request needs to be made to the FNIHB regional offices.
In the case of communities that have their own First Nation–operated hospitals, contact the specific hospital for access to community-level data. |
| What data do we need? |
- Hospitalizations flagged by unique identifier
- External cause of injury
- Number of hospital separations due to injury for all causes for children < 1, 1–4, 5–9, 10–14, 15–19 years and by male and female
- Population of children and youth broken down by age (< 1, 1–4, 5–9, 10–14, 15–19 years), male and female
- Hospital Separations data broken down by external cause of death (injury codes V01–Y98)
- Number of child/youth hospital separations per 100 000 population for a particular year
|
| Method of Calculation |
Numerator divided by denominator times 10 000 |
| Numerator |
Total number of hospital separations per indigenous child/youth age group in Canada assigned to relevant ICD-10-CA codes for a particular year |
| Denominator |
Mid-year total for indigenous children and youth population for the same year as the numerator. This could be obtained from FNIHB regional offices. |
| Limitations |
- First Nation identifiers are only available for the 4 western regions
- 12 First Nations hospitals may not be included in hospitalization data and may not be reported in the same way
- Access to hospitals vary geographically influencing the rates (potential for under-representation)
- Potential for over-representation of high-users of hospital
- Statistics Canada and Indian and Northern Affairs Canada (INAC) have population counts, but they will not provide as accurate a rate as the FNIHB regional office population counts
Provincial and territorial governments have varying capacities to extract and analyze First Nations and Inuit data from their hospital databases. Two provinces, British Columbia and Alberta, identify First Nations clients in their databases through unique health card numbers or First Nations health premium lists. Using this method, Alberta estimates that their hospital registration files have 25%–35% greater numbers than INAC reports for the Alberta population. While Manitoba Health has a unique identifier, it cannot identify approximately 35% of the First Nations population of whom the majority are Bill C-31 reinstatements. Saskatchewan uses self-identification and address to determine status.
The remaining provinces and territories are unable to identify First Nations or Inuit at all. |
| How to use this indicator |
The hospital separations rate indicates how many children/youth are discharged from hospital for each type of injury each year. An increase in hospital separations for a specific injury would indicate the need for more effective injury prevention in that specific area. A decrease in hospital separations would indicate that the injury prevention strategies in place are working. For those causes of injury that tend to have a relatively lower mortality risk (e.g. skateboarding), but can still result in significant injury among children requiring hospitalization (e.g. fractures requiring operative reduction/management), this indicator highlights their impact to the overall injury burden.
Specific to First Nations and Inuit communities, this indicator could be used to:
- Advocate
- Identify priorities
- Plan and prioritize health services/rehab needs
|
Indicator #3 - Alcohol, Solvent and Substance use
| Across All Injury Areas |
Outcome |
| Indicator Definition |
Number and proportion of self-reported alcohol, solvent and substance use among First Nations children and youth (based on RHS data) |
| Definition of Relevant Terms |
Substance – something (as alcohol, methamphetamine or marijuana) deemed harmful and usually subject to legal restriction (Merriam–Webster Dictionary, 2007).
Solvent – a liquid substance that is used to dissolve another substance. There are many types of solvents that can be inhaled to produce a “high.” Gasoline, felt markers, nail polish remover, some types of glue and paint thinner are some examples. |
| Justification for This Indicator |
The problematic use of alcohol by Aboriginal peoples is 4 times the national average and is associated with low employment, family violence and suicide. Fetal Alcohol Spectrum Disorder (FASD) and solvent abuse are also particular challenges for Aboriginal children and youth. Like Canada's northern communities, some Aboriginal communities also face issues of isolation, both social and geographic. Barriers, such as language, geography and lack of culturally sensitive services, pose significant challenges to accessing health care and treatment (Supporting First Nations, 2006). |
| What are we counting? (definition of a case) |
The comparable burden using RHS data: proportion of children and youth who answered that they were “under the influence” when the injury happened – each individual survey is a case. |
| Where do we get this information / data? |
RHS data from question in injury section: "When the injury happened, were you under the influence of any of the following:
- alcohol
- marijuana
- other substances
- not under the influence
- don't know
- refusal
|
| What data do we need? |
Data from RHS: Proportion of children and youth who answered that they were “under the influence” when the injury happened (from injury section of RHS). |
| Method of Calculation |
Numerator divided by denominator for RHS |
| Numerator |
RHS: number of injured children and youth who self-report their use of substances when they were injured on the RHS survey |
| Denominator |
RHS: total number of injured children and youth who completed the RHS survey |
| Limitations |
Self-reported surveys may be subject to dishonesty |
Indicator #4 – Potential Years of Life Lost
| Across All Injury Areas |
Outcome |
| Indicator Definition |
Potential Years of Life Lost (PYLL) due to injury among children and youth (ages 0–19 years) |
| Definition of Relevant Terms |
PYLL is an indicator of premature mortality. It represents the total number of years NOT lived by an individual who died before age 75 years. It can help us understand what injuries leading to death result in the largest number of years not lived by children who died prematurely |
| Justification for This Indicator |
PYLL allows us to measure the loss of life due to “premature” death attributable to unintentional or violent injury. PYLL gives more importance to the causes of death that occurred at younger ages than those occurred at older ages and highlights the proportional impact of childhood deaths in a way that is more evident than mortality rates alone, particularly when comparing to other major causes of death (e.g. cardiovascular disease, cancer) |
| What are we counting? (definition of a case) |
|
| Where do we get this information / data? |
The central Vital Statistics Registry in each province and territory provides data from death registrations to Statistics Canada. Regional offices of the First Nations and Inuit Health Branch (FNIHB), Health Canada have access to vital statistics with a First Nations or Inuit identifier |
| What data do we need? |
- Total number of deaths due to injury for all causes for children aged < 1, 1–4, 5–9, 10–14, 15–19 years by cause of injury (ICD-10 Codes V01–Y98), sex, socioeconomic status and geographic location (if available)
- Population of children and youth broken down by age (< 1, 1–4, 5–9, 10–14, 15–19 years), cause of injury (ICD-10 Codes V01–Y98), sex, socioeconomic status and geographic location (if available)
- Mortality data broken down by cause of death (ICD-10 Codes V01–Y98)
|
| Method of Calculation |
PYLL can be calculated in 2 ways:
The first addresses PYLL at an individual level. PYLL due to death is calculated for each person who died before age 75 years. For example, a person who died at age 20 years would contribute 55 potential years of life lost. Potential years of life lost correspond to the sum of the PYLL contributed for each individual. The rate is obtained by dividing total potential years of life lost by the total population aged < 75 years
Numerator: Sum of differences between age at death and 75 for all deaths in a given year. Can be stratified by cause of injury (ICD-10 Codes V01–Y98), sex, socioeconomic status and geographic location (if available)
Denominator: Estimates of total resident population aged < 75 years stratified by cause of injury (ICD-10 Codes V01–Y98), sex, socioeconomic status and geographic location (if available)
Method of calculation: (Numerator/Denominator) x 100 000
The second method addresses PYLL by age group. PYLL due to death is calculated for each age group (< 1, 1–4, 5–9, … and 70–74 years) by multiplying the number of deaths by the difference between age 75 years and the mean age at death in each age group. PYLL correspond to the sum of the products obtained for each age group. The rate is obtained by dividing total potential years of life lost by the total population aged < 75 years old.
Numerator: Sum of the products obtained for each age group after multiplying the number of deaths by the difference between age 75 years and the mean age at death in each age group. Can be stratified by cause of injury (ICD-10 Codes V01–Y98), sex, socioeconomic status and geographic location (if available)
Denominator: Estimates of total resident population for the age group of age groups selected stratified by cause of injury (ICD-10 Codes V01–Y98), sex, socioeconomic status and geographic location (if available)
Method of calculation: (Numerator/Denominator) x 100 000 |
| Numerator |
See above |
| Denominator |
See above |
| Limitations |
PYLL is criticized for skewing the deaths of younger children as having more “weight” than deaths to older people |
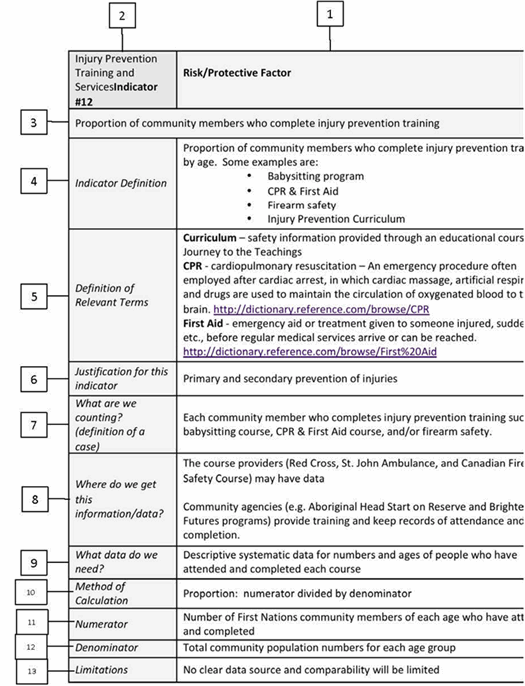
Indicator #5 – Injury Prevention Training
| Community Injury Prevention Training / Response Systems |
Risk / Protective Factor |
| Indicator Definition |
Proportion of community members who attend and complete injury prevention training, by age. Some examples are:
- Babysitting program
- CPR & First Aid
- Firearm safety
- Injury Prevention Curriculum
|
| Definition of Relevant Terms |
Curriculum – safety information provided through an educational course, e.g. Journey to the Teachings
CPR – cardiopulmonary resuscitation: An emergency procedure often employed after cardiac arrest, in which cardiac massage, artificial respiration and drugs are used to maintain the circulation of oxygenated blood to the brain.
First Aid – emergency aid or treatment given to someone injured, suddenly ill, etc., before regular medical services arrive or can be reached. |
| Justification for This Indicator |
Primary and secondary prevention of injuries |
| What are we counting? (definition of a case) |
Each community member who completes injury prevention training, e.g. babysitting course, CPR & First Aid course and/or firearm safety. |
| Where do we get this information / data? |
The course providers (Red Cross, St. John's Ambulance and Canadian Firearms Safety Course) may have data.
Aboriginal Head Start on Reserve and Brighter Futures programs provide some training to their staff. To find out what kind of training and how many staff are trained, contactFNIHB National Office and ask for the Regional AHSOR Coordinator or Brighter Futures Coordinator for the region of interest. |
| What data do we need? |
Need descriptive systematic data for numbers and ages of people who have completed each course. |
| Method of Calculation |
Proportion: numerator divided by denominator |
| Numerator |
Number of First Nations children and youth of each age who have completed
- Babysitting program
- CPR & First Aid
- Firearm safety
- Injury Prevention curriculum course
|
| Denominator |
Total population numbers for each age group |
| Limitations |
No clear data source and comparability will be limited |
Indicator #6 – Community Emergency Preparedness Plan
| Community Injury Prevention Training / Response Systems |
Risk / Protective Factor |
| Indicator Definition |
Presence of an emergency preparedness plan for community (i.e. flooding, fires, blizzards, etc.), including the proportion of community members trained in emergency preparedness.
- Updated
- Well understood
- Awareness
- Mock practice/drills
|
| Definition of Relevant Terms |
Emergency Plans: Through a management accountability framework, regional health offices of Indian and Northern Affairs Canada (INAC) provide funding to First Nations to develop emergency plans for preparedness in the event of fire, flooding or other potentially hazardous situations. (Community Factors Influencing First Nations Health - Survey, 2005). |
| Justification for This Indicator |
Communication is vital during a disaster. Accurate and consistent communication of information is very helpful in reducing the anxiety level of everyone involved and may lead to improved outcomes. |
| What are we counting? (definition of a case) |
The number of First Nations/Inuit communities/settlements that have an emergency plan as defined above. |
| Where do we get this information / data? |
RHS Survey of Community Factors Influencing First Nations Health, Section I, Question 1. |
| What data do we need? |
"Does the First Nation have an emergency plan? If yes, have community members and residents been made aware of the plan through newsletters or other communications from the First Nation?" (RHS, Question 1)
"Does the First Nation have an Emergency Coordinator? If yes, is the Emergency Coordinator trained for that position?" (RHS, Question 2) |
| Method of Calculation |
Proportion: numerator divided by denominator |
| Numerator |
Number of communities who answer “Yes” to both parts of RHS, Question 1 |
| Denominator |
Total number of communities responding to RHS community survey. |
| Limitations |
Community-specific data not available through RHS (includes a representative sample). |
Indicator #7 – Community Fire and Ambulance Services
| Community Injury Prevention Training / Response Systems |
Risk / Protective Factor |
| Indicator Definition |
Availability of fire & ambulance services in the community within a defined response time |
| Definition of Relevant Terms |
Availability: fire department and/or ambulance services with trained staff stationed in the community or access to local external fire-fighting or ambulance services within 50 km |
| Justification for This Indicator |
- Huge variability in response times
- Recognize the link between service & outcomes
|
| What are we counting? (definition of a case) |
Each community who completes the RHS community survey, Section VI, Question 5 & 6 |
| Where do we get this information / data? |
RHS community survey, Section VI, Question 5 & 6 |
| What data do we need? |
Number of communities that checked “Yes,” “No” and “Unknown” to questions about fire-fighting and ambulance services as well as average response times to reach the First Nation.
Distribution of response times reported by communities who do not have fire or ambulance services in the community. |
| Method of Calculation |
Proportion of communities that have fire and ambulance services in community: numerator divided by denominator |
| Numerator |
Number of communities that checked “yes” to Section VI, Question 5 or checked “yes” to Section VI, Question 6
Or Number of communities who checked “yes” to Section VI, Question 5a) or checked “yes” to Section VI, Question 6a) |
| Denominator |
Total number of communities who respond to RHS community questionnaire. |
| Limitations |
Community-specific data not available through RHS.
Inuit data not currently available. |
Indicator #8 – Animal Bites and Maulings
| Animal Bites |
Outcome |
| Indicator Definition |
The self-reported rate of injuries due to animal bites or maulings per 10 000 children and youth (ages 0–19 years) in a community |
| Definition of Relevant Terms |
Animal Bites: If an animal seizes something, or attempts to close or actually closes its jaws on something, and the teeth of the animal either enter, grip or wound that thing, a bite has occurred whether or not the skin is damaged.
Maulings: To beat, bruise, mangle or handle roughly (Merriam–Webster Dictionary, online, 2007) |
| Justification for This Indicator |
Animal bites are a serious problem in many First Nations and Inuit communities. The bites are frequently related to dogs and sometimes to wild animals
The RHS 2002/2003 found that dog bites account for 0.8% of injuries to children, just slightly lower than burns/scalds (0.9%) |
| What are we counting? (definition of a case) |
Number of people who answered the APS or RHS child or youth survey question "Have you been injured in the past 12 months?" with "Yes" and attributed the cause to "dog bite/mauling"
Note: Deaths and Hospital separations for dog bites (W54 of ICD-10-CA) are covered in Indicator #1 and #2 respectively |
| Where do we get this information / data? |
RHS Youth Questionnaire, Section J. Physical Injuries, Question 40.
RHS Child Questionnaire, Section H. Physical Injuries, Question 44.
APS Survey for 6–14 year olds, Section E. Physical Injuries, Question E4. |
| What data do we need? |
# bites/maulings |
| Method of Calculation |
Numerator divided by denominator |
| Numerator |
Number of children and youth who indicate dog bites and animal maulings as cause of injury on RHS
OR Number of children and youth who indicate dog bites and animal maulings as cause of injury on APS. |
| Denominator |
Total number of children and youth who indicate they were injured in the last 12 months on RHS
OR Total number of children and youth who indicate they were injured in the last 12 months on APS. |
| Limitations |
Community data may be suppressed due to low numbers.
APS does not have injury data for 15–19 year olds. |
Indicator #9 – Animal Control Services
| Animal Bites |
Risk / Protective Factor |
| Indicator Definition |
The number and proportion of communities that have Animal Control Services |
| Definition of Relevant Terms |
Animal Control Services
- Enforces all Animal Control Laws, responds to animal-related complaints and conducts investigations of cruelty and problem situations
- Investigates animal bite cases in conjunction with the Health Department ensuring that biting animals are properly vaccinated and quarantined and arranges for rabies tests when appropriate
- Provides weekly low cost Rabies Clinic to the public
- Provides and services humane traps for bite cases, aggressive animals and wildlife in homes ($25 deposit for traps, CHECKS only)
- Operates a Spay/Neuter Clinic where adopted animals are spayed/neutered, vaccinated against rabies as well as given initial vaccinations and worming at a minimum cost
|
| Justification for This Indicator |
Animal bites are a serious problem in many First Nations and Inuit communities. The bites are frequently related to stray dogs. Identifying communities with high numbers of stray dogs will prompt action to reduce these numbers. Animal control services are the ideal organization to deal with stray dogs
This indicator allows us to compare how many animal-related injuries take place among children and youth in communities with animal control services vs. communities without animal control services |
| What are we counting? (definition of a case) |
Identified animal control services in a community (yes or no) |
| Where do we get this information / data? |
Department of Indian and Northern Affairs now has access to this information
LINKS:
Data about Animal Bites
British Columbia
|
| What data do we need? |
INAC has access to the number of communities with animal control services. Community surveys could also be conducted to ask each participating community whether or not they have animal control services |
| Method of Calculation |
Presence or absence |
| Numerator |
Presence of animal control services |
| Denominator |
N/A |
| Limitations |
This information has only been collected very recently. There may be difficulty accessing it. |
Indicator #10 – Rate of Hypothermia / Frostbite
| Hypothermia / Frostbite |
Outcome |
| Indicator Definition |
The rate of hypothermia or frostbite per 10 000 children and youth (ages 0–19 years), by age |
| Definition of Relevant Terms |
Children and youth aged < 19 years. |
| Justification for This Indicator |
Identifying communities with a higher percentage of cases of hypothermia among children and youth may prompt action to prevent hypothermia in this population. |
| What are we counting? (definition of a case) |
This can be measured in 2 ways:
- Cases will be identified by the nature of injury and the external cause of injury codes (X31) recorded in hospital separation data files.
- The comparable burden using data from RHS and APS: proportion of children and youth who answered that hypothermia was the cause of their injury – each individual survey is a case.
|
| Where do we get this information / data? |
- British Columbia, Alberta, Saskatchewan and Manitoba are able to identify First Nations people from hospitalization data. The remaining provinces and territories do not have a “unique identifier.” To obtain hospitalization data, a request needs to be made to theFNIHB regional offices.
- The Regional Health Survey also provides information on where the injury occurred and what the child/youth was doing when hypothermia/frost bite occurred.
|
| What data do we need? |
- Number of hospital separations due to exposure to excessive natural cold (ICD-10 Code: X31) for children and youth aged < 1, 1–4, 5–9, 10–14 or 15–19 years, by male/ female and First Nations/Inuit if available.
- RHS Youth Questionnaire, Section J. Physical Injuries, Questions 39 and 40 (can link responses to birthdates to determine age of youth).
RHS Child Questionnaire, Section H. Physical Injuries, Questions 43 and 44 (can link responses to birthdates to determine age of youth).
APS Survey for 6–14 year olds, Section E. Physical Injuries, Question E4. |
| Method of Calculation |
- Rate for each age group of children and youth: numerator divided by denominator times 10 000
- Proportion of children and youth with hypothermia out of all children and youth who respond to RHS and APS surveys
|
| Numerator |
- Total number of hospital separations per First Nations and Inuit child/youth age group in Canada assigned to relevant ICD-10-CA X31 code (hypothermia) for a particular year
- Number of child/youth RHS or APS survey responses that list hypothermia as a cause of injury within the last 12 months
|
| Denominator |
- Mid-year total for First Nations and Inuit children and youth population for the same year as the numerator. This could be obtained from FNIHB regional offices (by age group).
- Total number of child/youth RHS or APS survey responses
|
| Limitations |
Provincial and territorial governments have varying capacities to extract and analyze First Nations and Inuit data from their hospital databases. Two provinces, British Columbia and Alberta, identify First Nations clients in their databases through unique health card numbers or First Nations health premium lists. Using this method, Alberta estimates that their hospital registration files have 25%–35% greater numbers than INAC reports for the Alberta population. While Manitoba Health has a unique identifier, it cannot identify approximately 35% of the First Nations population of whom the majority are Bill C-31 reinstatements. Saskatchewan uses self-identification and address to determine status.
There are no identifiers for Inuit hospitalization data. Data obtained for this indicator will be an under-estimate of the true number of cases of hypothermia as not all cases are treated in the health care system or reported. |
Indicator #11 – Police Response to Violent Injury Calls
| Violent / Inflicted Injury |
Risk / Protective Factor |
| Indicator Definition |
The number and proportion of police responses to calls and charges involving children and youth (ages 0–19 years) related to:
- domestic violence
- substance abuse related incidences
- gunshots fired
- assaults (basic, with weapon or causing bodily harm)
- child abuse
- sexual assault
- bullying
- gang violence
|
| Definition of Relevant Terms |
Police charges:
Domestic violence: Abuse between married or common-law partners. The abuse can be verbal, emotional, sexual or physical. It can also be a combination of a number of these forms. (Royal Canadian Mounted Police, 2007).
Substance abuse: Harmful or hazardous use of psychoactive substances, including alcohol and illicit drugs (WHO, 2007)
Assaults: A person commits an assault when
- without the consent of another person, he or she applies force intentionally to that other person, directly or indirectly
- he or she attempts or threatens, by an act or a gesture, to apply force to another person, if he or she has, or causes that other person to believe on reasonable grounds that he or she has, present ability to effect his or her purpose
Child abuse: Child abuse occurs when a parent, guardian or caregiver mistreats or neglects a child, resulting in
- injury or
- significant emotional or psychological harm or
- serious risk of harm to the child.
(Public Health Agency of Canada, 2005)
Sexual Assault/Exploitation: Every person who is in a position of trust or authority towards a young person or is a person with whom the young person is in a relationship of dependency and who
- for a sexual purpose, touches, directly or indirectly, with a part of the body or with an object, any part of the body of the young person, or
- for a sexual purpose, invites, counsels or incites, a young person to touch, directly or indirectly, with a part of the body or with an object, the body of any person, including the body of the person who so invites, counsels or incites and the body of the young person (Sexual Exploitation, 2005).
|
| Justification for This Indicator |
Violence and crime rates are important indicators of community dysfunction. These rates will be used to justify and evaluate positive programs that work to prevent injuries related to crime and violence.
Assaults represented the worst jump in crime in Iqaluit in 2003, with more than a 30% increase. Reports show the RCMP handled 727 assault cases in Iqaluit in 2003, up from 552 the year before (Nunatsiaq News, 2004). |
| What are we counting? (definition of a case) |
RCMP call centres code every call that comes in, though the provinces use different database software systems. Each type of call received by an RCMP call centre can be counted. Once the call has been responded to, the file is updated with information on whether or not charges have been laid and possible alcohol and drug use. It is unclear how consistently First Nations or Inuit are identified in the file; however, geographic location of the incident may have to serve as a proxy measure. Cases will be defined in 2 ways: first, any call to police that falls within any of the above categories; second, any charges laid by police related to any of the above categories. |
| Where do we get this information / data? |
Law enforcement (RCMP or tribal police)
RCMP (Royal Canadian Mounted Police) –
Other community-based law enforcement such as community-based police. |
| What data do we need? |
Number of calls of each type that are received by RCMP call centres or community-based police.
Number of files that indicate that a charge has been laid for each type of violence-related charge.
If possible, number of calls involving a child/youth. |
| Method of Calculation |
Proportion can be calculated based on the number of calls and number of charges due to violence in small, medium and large communities out of the total number of calls to police in small, medium and large communities. |
| Numerator |
Number of calls or charges due to violence in one year in small, medium and large communities. |
| Denominator |
Total number of calls or charges in one year in small, medium and large communities. |
| Limitations |
Community access to RCMP data or community-based police data may be difficult. Not all files will be identified as involving First Nations or Inuit. Not all files will be identified as involving children or youth. |
Indicator #12 – Rate of Inflicted Injury
| Violent / Inflicted Injury |
Outcome |
| Indicator Definition |
The self-reported rate of inflicted injury (violence and abuse) per 10 000 children and youth (ages 0–19) (not including self-inflicted injuries) |
| Definition of Relevant Terms |
Inflicted injury is an injury resulting from violence and includes the following:
Domestic violence: Abuse between married or common-law partners. The abuse can be verbal, emotional, sexual or physical. It can also be a combination of a number of these forms. (Royal Canadian Mounted Police, 2007).
Physical Assaults: A person commits an assault when
- without the consent of another person, he or she applies force intentionally to that other person, directly or indirectly;
- he or she attempts or threatens, by an act or a gesture, to apply force to another person, if he or she has, or causes that other person to believe on reasonable grounds that he or she has, present ability to effect his or her purpose
Bullying: Bullying is a type of personal harassment, and a form of aggression, that may include physical, verbal or emotional abuse.
[Retrieved on Nov. 15, 2007]
Gang violence: According to the Criminal Code, a gang is a group of at least 5 people engaging in criminal activities.
[Retrieved on Nov. 15, 2007] |
| Justification for This Indicator |
Violent injury rates for First Nations and Inuit are very high. We know that they are impacting children and youth in unacceptable ways. This indicator will assist in understanding the extent of the problem. |
| What are we counting? (definition of a case) |
We will measure the burden of violent injury using RHS data: proportion of children and youth who answered that their injury was caused by domestic/family violence or other physical assault – each individual survey is a case. |
| Where do we get this information / data? |
In the injury section of the RHS child and youth questionnaires, if respondents answer that they have been injured in the last 12 months, they are also asked, “What caused the injury?” and can choose
- domestic/family violence
- other physical assault
|
| What data do we need? |
Regional Health Survey results. |
| Method of Calculation |
Numerator divided by denominator × 100 000 |
| Numerator |
Number of injured children and youth who self-report their injury was caused by “domestic/family violence” or “other physical assault” on the RHS child and youth questionnaires. |
| Denominator |
Total number of children and youth who completed the RHS child and youth questionnaires. |
| Limitations |
This condition may be severely underestimated due to missed diagnosis and underreporting (particularly domestic violence). |
Indicator #13 – Restorative Justice Programs
| Violent / Inflicted Injury |
Community Injury Prevention Training / Response Systems |
| Indicator Definition |
The number and proportion of violent offenders participating in restorative justice (community justice forums, First Nations/Inuit justice programs or alternative justice programs). |
| Definition of Relevant Terms |
Community Justice Forum – A CJF is a safe, controlled environment in which an offender, the victim and their families or supporters are brought together under the guidance of a trained facilitator. Together they discuss the offence and how they have all been affected, and jointly develop a plan to correct what has occurred. Offenders must accept responsibility for their own actions (Royal Canadian Mounted Police, 2007). |
| Justification for This Indicator |
Programs that support offenders after they have been charged have the potential to reduce the number of repeat offenders. The use of such programs in a community is one possible indicator of wellness.
The philosophy of restorative justice is based on community healing. In other words, the community decides what is best for itself in terms of resolving certain criminal matters. The focus in restorative justice is on offender accountability, problem-solving and creating an equal voice for offenders and victims. The best results occur when the victim, offender and the community jointly resolve the affects of an offenders' behaviour. There are many options within restorative justice. The RCMP is championing one specific process: Community Justice Forums (Royal Canadian Mounted Police, 2007). |
| What are we counting? (definition of a case) |
Each violent offender participating in a community justice forum. |
| Where do we get this information / data? |
Sources: Law enforcement for number of offenders
Data from programs for number of offenders attending programs
Aboriginal Justice Strategy
Community-based Justice Programs Canadian Provinces
Community-based Justice Programs in…
Alberta:
- Metis Settlements General Council (MSGC) Justice Program
- Saddle Lake First Nations Restorative Justice Program
- Siksika Nation Aiskapimohkiiks Program
- Tsuu T'ina Nation Peacemaker Court
- Yellowhead Tribal Community Corrections Society First Nations Custom Advisory Panels
British Columbia:
- Esketemc Alternative Measures Program (Esketemc First Nation at Alkali Lake)
- Gitxsan Unlocking Aboriginal Justice Program (Gitxsan Treaty Office)
- Hida Gwaii Restorative Justice Program (Haida Tribal Society)
- Lower Post First Nation Community Justice Program (Daylu Dena Council)
- Nicola Valley Aboriginal Community Justice Program (Nicola Valley Family Justice Services)
- Nisga'a Yuuhlamk'askw Justice Program
- Nuxalk Restorative Justice Program
- Prince George Urban Aboriginal Justice Society
- Prince Rupert Urban Aboriginal Justice Program
- Qwi'qwelstom – Sto:lo Nation Justice Program
- Secwepemc Community Justice Program
- Ska'ls – Beliefs in Justice Program
- Sliammon Justice Program
- St'at'imc Restorative Justice Program
- Stikine Aboriginal Justice Program
- Tl'azt'en “Healing Circle” Justice Program
- Tsilhqot'in Community Justice Program
- Vancouver Aboriginal Transformative Justice Services
- Wet'suwet'en Unlocking Aboriginal Justice Program
Manitoba:
- Awasis Agency of Northern Manitoba Inc.
- Hollow Water Community Holistic Circle Healing Program
- Manitoba Keewatinowi Okimakanak Inc.
- Onashowewin Inc. – “Rekindling the Spirit Within”
- St. Theresa's Point First Nation Tribal Court System
Newfoundland and Labrador:
- Community Holistic Justice Program
- Community Justice Program
New Brunswick:
- Restorative Justice Initiative Program & Victims' Assistance Program
Northwest Territories:
- Community Justice Committees
Nova Scotia:
- Mi'Kmaq Legal Support Network Customary Law Program
Nunavut:
- Community-based Program
- Community Justice Committees
Ontario:
- Aboriginal Community Council Program
- Biidaaban – The Mnjikaning Community Healing Model
- Community Council Program
- Community Justice Programme
- Restorative Justice Progarm
- United Chiefs and Councils of Manitoulin Justice Program
Prince Edward Island:
- Aboriginal Community Justice Program
Quebec:
- Alternative Justice & Court Worker Programs
- Community-Based Justice Program
- Community Justice Panel & Youth Justice Program
- Community Justice Program
- Community Justice Program
|
| What data do we need? |
Number of violent offenders (ages 0–19) and the number of violent offenders attending programs. |
| Method of Calculation |
For each community, the following score could be applied:
0 – no program
1– existing, program, with low attendance (< 50%)
2 – existing program, high attendance (> 50%) |
| Numerator |
Number of offenders attending programs |
| Denominator |
Total number of offenders |
| Limitations |
This may make a better research question than indicator as this indicator is based on an assumption that restorative justice programs impact injuries. |
Indicator #14 – Working Smoke Detectors
| Burns and Falls |
Risk / Protective Factors |
| Indicator Definition |
The number and proportion of homes in a community with working smoke detectors, tested fire extinguishers and carbon monoxide detectors |
| Definition of Relevant Terms |
Smoke detectors: First line of defense device when there is fire in the home. It gives early warning that danger is present and could give enough time for family to reach safety. Fire Extinguisher: A portable fire extinguisher can save lives and property by putting out a small fire or containing it until the fire department arrives; but portable extinguishers have limitations. Because fire grows and spreads so rapidly, the number one priority for residents is to get out safely (U.S. National Fire Protection Association, 2007). Carbon monoxide detector: A device that detects the presence of the carbon monoxide (CO) in order to prevent carbon monoxide poisoning. CO is a colorless and odorless compound produced by incomplete combustion that is lethal at high concentrations. If a high concentration of CO is detected, the device sounds an alarm, giving people in the area a chance to ventilate the area or safely leave the building. |
| Justification for This Indicator |
The fire death rate in homes with working smoke alarms is 51% less than the rate for homes without this protection (U.S. National Fire Protection Association, 2007).
Many successful programs, such as smoke detector give-away programs, have been used to increase smoke detector use in Canada and the U.S. Examples of these evaluated programs can be found by searching “increase smoke detector use” on the internet. |
| What are we counting? (definition of a case) |
Percentage of residences with smoke detectors and fire extinguishers (each survey respondent is a case) |
| Where do we get this information / data? |
APS, Adult Questionnaire, Section H, Housing, Question H11, “Does your home have:
- A smoke detector
- A fire extinguisher”
First Nations Regional Health Survey Adult Questionnaire, Section F. Housing, Question 26, “Does your home have
- A working smoke detector
- A fire extinguisher
- A carbon monoxide detector”
|
| What data do we need? |
Survey response summary from the APS, Adult Questionnaire and the Regional Health Survey, Adult Questionnaire. |
| Method of Calculation |
(Numerator divided by denominator) × 100 |
| Numerator |
Number of survey respondents who answered that their home has a smoke detector and/or fire extinguisher. |
| Denominator |
Total number of respondents on the APS and RHS adult questionnaire. |
| Limitations |
The APS and RHS use self-reported data therefore may not be completely accurate.
The APS may include some Inuit survey respondents but is not designed as a representative sample of First Nations or Inuit. |
Indicator #15 – Burns and Scalds
| Burns and Falls |
Outcome |
| Indicator Definition |
Number and proportion of self-reported burns and scalds to children and youth (ages 0–19 years) as well as the self-reported circumstantial details of each case, such as:
- what happened?
- when?
- how?
- was it intentional or unintentional?
|
| Definition of Relevant Terms |
The Injury section in the RHS asks about injuries that were serious enough to affect normal day-to-day activities. Under “What type of injury did you have?”, respondents have the option of checking “burns or scalds.” |
| Justification for This Indicator |
Fire- and flame-related injuries are 4 to 8 times higher for First Nations people than in the Canadian population (Johnson as cited in McDonald, 2006, p. 9). Wood frame house construction, the lack of smoke detectors, and smoking habits can put Aboriginal people at increased risk of fire and flames. Almost one-third (31%) of all fire deaths in the Aboriginal population are in children (ages 1–14 years), compared to an average of 16% in the total Canadian population, a finding that may be partly explained by the higher proportion of children in the Aboriginal population (Assembly of First Nations, 2006, p. 10). |
| What are we counting? (definition of a case) |
The number of reported burns to children and youth by self-report in the RHS (each survey respondent who checked “burns or scalds” is a case). |
| Where do we get this information / data? |
RHS child and youth questionnaires ask many of these details in the Injury section:
- type of injury
- part of body that was injured
- where injury took place
- what the individual was doing when injury took place
- what caused the injury
- where the individual got treatment
- was individual under the influence of alcohol, marijuana or other substances
|
| What data do we need? |
The number of reported burns to children and youth by self-report in the RHS. |
| Method of Calculation |
Numerator divided by denominator gives the proportion of burns of each circumstance out of the total children and youth reporting having been injured in the last 12 months. |
| Numerator |
Number of children/youth reporting burns or scalds as cause of injury in RHS self-report, by each type of circumstance. |
| Denominator |
Total number of children/youth reporting having been injured in the last 12 months in the RHS questionnaire. |
| Limitations |
Community-specific data are not available.
Injuries from burns may be underreported in domestic settings. |
Indicator #16 – Falls
| Burns and Falls |
Risk / Protective Factors |
| Indicator Definition |
Place where falls among children and youth (ages 0–19) that result in injury happen (this refers to self-reported falls to children and youth within the last 12 months):
- Home
- School, college, university
- Sports fields/facilities of schools
- Street, highway, sidewalk
- Community buildings (community centre, band office)
- Industrial or construction area
- Office
- Countryside, forest, woodlot
- Lake, river, ocean
|
| Definition of Relevant Terms |
This indicator was originally written to find out about falls on playgrounds, through ice and in old abandoned houses; however, no data are currently gathered on those types of falls. |
| Justification for This Indicator |
Falls are very often a cause of death and hospitalization.
Death rates from falls among Status Indians was almost 3 times that of the provincial average for British Columbia in 1991–1998 (First Nations and Inuit Health, as cited in McDonald, 2006, p. 8). |
| What are we counting? (definition of a case) |
- The number and location of reported falls by self-report in the RHS (each survey is a case). This will include children and youth in First Nation, on-reserve communities.
- The number and location of reported falls by self-report in the CCHS (each survey is a case). This will include Aboriginal youth aged 12–19 years in every province/territory but NOT living on-reserve. This may be a good way to access some Inuit data.
- The number of falls at schools and childcare centres may be recorded in incident reports at schools and childcare centres. May provide a source for community-level data.
|
| Where do we get this information / data? |
- RHS child and youth questionnaires ask many details in the Injury section:
- type of injury
- part of body that was injured
- where injury took place
- what individual was doing when injury took place
- what caused the injury
- where did individual get treatment
- was individual under the influence of alcohol, marijuana or other substances.
- Data from Canadian Community Health Survey (CCHS), Injury Section, Question 10–15.
- Incident reports from schools and childcare centres.
|
| What data do we need? |
- The number and location details of falls for children/youth by self-report in the RHS.
- The number and cause of the fall to child/youth in CCHS data (Yukon, Northwest Territories, Nunavut and Labrador questionnaires will have many Inuit responses).
- The number and circumstantial details of falls for children/youth in schools, on school grounds, and in childcare centres.
|
| Method of Calculation |
Proportion of falls in each location: numerator divided by denominator |
| Numerator |
- Number of children and youth who report falling in each location (self-report on RHS)
- Number of youth who report falling in each location (self-report on CCHS)
- Number of children/youth listed as having fallen in incident reports of schools and childcare centres
|
| Denominator |
- Total number of children and youth who report injuries due to falling within the last 12 months.
- Total number of children and youth who report injuries due to falling within the last 12 months.
- Total number of children in the school or childcare centre.
|
| Limitations |
This indicator was originally written to find out about falls on playgrounds, through ice, and in old abandoned houses; however, no data is currently gathered on those types of falls. Injuries from falls may be underreported in domestic settings. It will be difficult to separate First Nation and Inuit responses on CCHS from mainstream responses. |
Indicator #17 – Community Emergency Response Teams
| Drowning |
Community Injury Prevention Training / Response Systems |
| Indicator Definition |
The number and proportion of communities with available Emergency Response Teams (e.g. Search and Rescue, Lifesaving Society or Armed Forces)
- open water or ice (lakes, oceans, rivers, etc.)
|
| Definition of Relevant Terms |
Search and rescue is the search for and provision of aid to people who are in distress or imminent danger. |
| Justification for This Indicator |
Aboriginal people are at a greater risk of injuries due to extreme weather due to the often rural, remote or northern location of many communities. They are at greater risk of drowning because of their proximity to water, especially in northern climates where the water temperature is low and can produce death from hypothermia. Risks associated with drowning in Aboriginal victims also include the low use of flotation devices, and alcohol use (Health Canada as cited in McDonald, 2006, p.8). Emergency response or search and rescue teams can find people in distress and assist with accessing medical attention. |
| What are we counting? (definition of a case) |
Presence of emergency response team services. |
| Where do we get this information / data? |
Not currently collected |
| What data do we need? |
|
| Method of Calculation |
|
| Numerator |
|
| Denominator |
|
| Limitations |
|
Indicator #18 – Water Safety Education Programs
| Drowning |
Community Injury Prevention Training / Response Systems |
| Indicator Definition |
The number and proportion of communities with access to water safety education / programs |
| Definition of Relevant Terms |
Water Safety Education includes the following types of programs:
- Use of Personal Floatation Device (PFD) training
- Use of the strategies in the Northern and Remote Water Safety Community Resource
- A PFD Loaner Program – a community-led project that loans personal floatation devices (sometimes called PFDs or lifejackets) to individuals and families at no cost. As of December 2007, 17 First Nations communities in Man. have received a supply of PFDs for a PFD loaner program
- Boating safety
- “Swim to Survive” teaches how to survive if you fall into water and how to swim 50 metres using any stroke to get to land
|
| Justification for This Indicator |
Northern or remote communities often live in proximity to water. They usually have little or no access to facilities where water safety education is offered such as recreation centres. If water safety education is offered in local bodies of water, there may only be 2 months of the year in which the weather is favourable enough to teach swimming and water safety programs.
The Lifesaving Society of Manitoba has developed a “Swim to Survive” program specifically targeted at children and youth in northern and remote communities. They began providing programs in 2005 and believe they have contributed to the decrease in drownings in Manitoba since that time. |
| What are we counting? (definition of a case) |
Each First Nation or Inuit community that has a drowning prevention program (of any kind). |
| Where do we get this information / data? |
Data on PFD Loaner Programs are provided by Manitoba Coalition for Safer Waters and IMPACT, Phone the Communications Coordinator for more information at : 204-787-1907 or email: WFRENCH@exchange.hsc.mb.ca
The Lifesaving Society programs teach self-rescue, rescue of others and basic first aid. Each provincial/territorial branch has statistics for programs offered. Contact information for the provincial/territorial Lifesaving Society Branch offices
Red Cross has developed a “Learn to Swim” program, but it is operated by community centres, therefore no statistics are kept by Red Cross. |
| What data do we need? |
Number of First Nation or Inuit communities that have water safety programs (see definition of relevant terms). |
| Method of Calculation |
Proportion: numerator divided by denominator |
| Numerator |
Number of communities who have reasonable access to drowning prevention education |
| Denominator |
Total number of communities |
| Limitations |
Data not currently available in one central location. Individual communities could collect this data through a community-level surveillance system as long as they could access it from the various program providers. It may be difficult to collect.
Not relevant to communities without pools or lakes (some are at higher risk) |
Indicator #19 – Number of Children and Youth who Drown
| Drowning |
Outcome |
| Indicator Definition |
The number and proportion of children and/or youth (ages 0–19) who drown each year by community and body of water type (i.e. pool, bath, lake, ocean, reservoir, pond, basin, canal, culverts, drainage ditches, etc.) |
| Definition of Relevant Terms |
Drowning is defined as deaths following submersion injury within 24 hours. Data are available for drowning.
Near drowning is survival beyond 24 hours following submersion incident. Less data are available for near drowning. |
| Justification for This Indicator |
Drowning is the second most important cause of injury death in many Aboriginal communities in Canada. In some locations, the number of drownings exceeds the number of road traffic deaths, especially when snowmobile drowning is included. According to the Canadian Surveillance System for Water-Related Fatalities, Aboriginal people had a drowning rate 6 times higher than other Canadians in 1996 (9.0 per 100 000 population versus 1.5).(The Red Cross Society and the Canadian Surveillance System for Water-Related Fatalities as cited by Health Canada, 2005.) The gap is even larger for toddlers (< 5 years): nationally, Aboriginal toddlers had a drowning rate 15 times higher than other Canadian toddlers (Health Canada, 2005). |
| What are we counting? (definition of a case) |
Cases will be identified by the nature of injury codes (ICD-10 S00–T98) and the external cause of injury codes (V01–Y98) recorded in mortality data files (Vital Statistics). |
| Where do we get this information / data? |
- The Canadian Surveillance System for Water-Related Fatalities collects data based on Coroner's Report data. It includes an identifier for Aboriginal, but does not specify First Nations or Inuit. It also includes details on type of body of water using the following categories:
- Ocean
- Lake or pond
- River/stream/creek/waterfall
- Bath Tub
- Private pool
- Public Pool
- Public Waterpark/Waterslide
- Hot tub/whirlpool
- Reservoir/artificial lake/dugout/retention pond
- Quarry
- Canal
- Dam, inlet or spillway
- Ditch/culvert
- Sewage lagoon
- Other body of water. Specified__________
- Vital Statistics keep mortality data include an “External Cause of Injury Code” that identifies drowning and submersion in bathtubs, swimming pools, natural water and unspecified. These codes are listed as ICD-10 W65–W74 or V90–V92. The place of the occurrence should be coded separately as 8 and specified as beach, canal, harbour, lake, marsh, pond or pool, river, sea, seashore, stream, swamp or water reservoir. The age of the child/youth could also be determined. However, each province identifies First Nations differently (see limitations).
- British Columbia has a Child Death Review Unit as part of the Office of the Chief Coroner that investigates the deaths of all children in British Columbia. Other provinces have unique ways of investigating child deaths. If access to this data was granted, you may also be able to determine:
- the age of the child/youth
- whether or not substance use was a factor
- the specific body of water where the drowning occurred
|
| What data do we need? |
- Canadian Surveillance System for Water-Related Fatalities
- Mortality and hospitalization data include an “External Cause of Injury Code” that identifies drowning and submersion in bathtubs, swimming pools, natural water, and unspecified. These codes are listed as ICD-10 W65–W74 or V90–V92. The place of the occurrence should be coded separately as 8 and specified as beach, canal, harbour, lake, marsh, pond or pool, river, sea, seashore, stream, swamp or water reservoir.
|
| Method of Calculation |
Proportion: numerator divided by denominator |
| Numerator |
Number of children and youth drowning in each body of water type, by age group |
| Denominator |
Total number of fatal drownings to children and youth, by age group. |
| Limitations |
- Access to data from the Canadian Surveillance System for Water-Related Fatalities may be a challenge. Also, data include an identifier for Aboriginal, but do not specify First Nations or Inuit.
The same limitation is true for this indicator as for mortality and hospitalization indicators.
- Provincial vital statistics identify First Nation deaths differently. In British Columbia, both on- and off-reserve First Nation people are identified the same way. In Alberta and Saskatchewan, only on-reserve First Nations are identified in vital statistics. In Ontario, vital statistics on First Nations come from nursing stations. In Quebec, only half of all communities provide data on vital statistics. In the Atlantic provinces, First Nation identifiers are provided through on-reserve Teleform.
The Territories do not identify First Nation people or Inuit separately in their vital statistics. |
Indicator #20 – Learn to Swim Programs
| Drowning |
Risk / Protective Factors |
| Indicator Definition |
The number and proportion of children/youth (ages 0–19) enrolled in “learn to swim” programs in a specific year by community. |
| Definition of Relevant Terms |
Learn to swim lessons: teach how to swim (swimming strokes) as well as safety, entries into water, boating knowledge and equipment. |
| Justification for This Indicator |
Northern or remote communities often live in proximity to water. They usually have little or no access to facilities where water safety education is offered, e.g. recreation centres. If water safety education is offered in local bodies of water, there may only be 2 months of the year in which the weather is favourable enough to teach swimming and water safety programs.
The Lifesaving Society of Manitoba has developed a “Swim to Survive” program (national program?) specifically targeted at children and youth in northern and remote communities. They began providing programs in 2005 and believe they have contributed to the decrease in drownings in Manitoba since that time.
In 1946, Red Cross launched its swimming program to address drowning deaths in Canada. When Red Cross took on water safety as a key program focus in the 1940s, an average of 1,200 Canadians died in the water annually, making drowning one of the leading causes of death among young Canadians. Today, thanks in part to the work of the Canadian Red Cross in those intervening 60 years, that number has fallen significantly to 472 deaths in 2000 (Canadian Red Cross, 2007). |
| What are we counting? (definition of a case) |
Each First Nations and Inuit child/youth enrolled in a “learn to swim” program in a specific year |
| Where do we get this information / data? |
The Lifesaving Society programs teach self-rescue, rescue of others and basic first aid. Each provincial/territorial branch has statistics for programs offered. They may have a list of programs offered in First Nation or Inuit communities. Contact information for the provincial/territorial Lifesaving Society Branch offices
Red Cross has developed a “learn to swim” program that is provided through various community centres and providers. The providers would have statistics on numbers of children/youth in their programs, but are not likely to have a First Nation or Inuit identifier. |
| What data do we need? |
Number of 0–19 year olds in “learn to swim” programs
Total number of 0–19 year old First Nations children and youth.
Total number of 0–19 year old Inuit children and youth. |
| Method of Calculation |
(Numerator divided by denominator) × 100 |
| Numerator |
Number of First Nation children and youth (0–19 year olds) in “learn to swim” programs
OR Number of Inuit children and youth (0–19 year olds) in “learn to swim” programs |
| Denominator |
Total number of 0–19 year old First Nations children and youth
OR Total number of 0–19 year old Inuit children and youth |
| Limitations |
Northern communities may be in close proximity to water, but may have water that is too cold to learn to swim in.
This indicator is most relevant to communities in close proximity to water. This indicator does not have a way of measuring informal swimming instruction such as lessons taught by parents to children.
Enrolment statistics from “learn to swim” programs may be difficult to obtain and may not have a First Nation or Inuit identifier. |
Indicator #21 – Rate of Suicide and Self-Harm
| Suicide / Self-Harm |
Outcome |
| Indicator Definition |
The rate of suicide attempts/self-harm and completed suicides per 10 000 among children and youth by community |
| Definition of Relevant Terms |
Suicide attempt refers to an attempt to purposely inflicted self-harm resulting in nonfatal injury.
Diminishing the risk of suicide attempts and intentional self-harm is a desirable outcome. It may not be possible to entirely eliminate the risk of suicide, but it is possible to reduce this risk. Suicide should not be viewed solely as a medical or mental health problem, since protective factors such as social support and connectedness appear to play significant roles in the prevention of suicide.
In research on factors of cultural continuity, Chandler and Lalonde (1998) found that measures intended to mark the degree to which individual Aboriginal communities had successfully taken steps to secure their cultural past in light of an imagined future proved to be strongly related to the presence or absence of youth suicide. The measures used in this study were land claims, self-government, education services, police and fire services, health services and cultural facilities. |
| Justification for This Indicator |
Suicide rates are known to be high among First Nations People and Inuit. Labrador and MB's RHS surveys asked people about this issue. The results were similar in both regions. About 25% of people had felt suicidal at some time in their lives and about 15% had actually attempted suicide at some point (RHS, 1999).
The Task Force on Suicide in Canada reported in 1994 that Aboriginal communities often have significantly higher suicide rates than those in the general Canadian population. High suicide rates tend to be associated with various community characteristics, including a higher number of occupants per household, more lone-parent families, fewer elders, lower average income and lower average education (Health Canada, 1994). While suicide rates in First Nation communities are known to be high, rates for Inuit may be even higher: data from the Northwest Territories suggest that while Dene people had suicide rates of 29 per 100 000 over the 1986–1996 period, rates among the Inuit were 79 per 100 000 population. (Northwest Territories Health and Social Services, 1998). |
| What are we counting? (definition of a case) |
Each child or youth who answered the cause of injury as "suicide attempt or other self-inflicted injury" in the injury section of the RHS (parent would complete the child questionnaire).
AND/OR Each child or youth who dies as a result of completed suicide listed in mortality databases (ICD-10 coding X60–X84). |
| Where do we get this information / data? |
Self-reported data from RHS (RHS self-report by youth aged 12–17 years / parent report for children aged < 12 years).
The injury section asks "If you have been injured in the last 12 months, what caused the injury?
- suicide attempt or other self-inflicted injury"
The mental health section, question #76 asks "Have you ever attempted suicide?
- Yes, when I was under 12 years of age
- Yes, when I was an adolescent (12–17 years of age)
- Yes, during the past year
- Never
- Don't know
- Refused
AND/OR The central Vital Statistics Registry in each province and territory records data from death registrations. Regional offices of theFNIHB have access to vital statistics with a First Nations or Inuit identifier (see Indicator #1 “Mortality”). |
| What data do we need? |
Number of children and youth identified as having an incident of self-harm or a suicide attempt
Total number of children and youth
Mortality data broken down by external cause of death (ICD-10 Codes X60–X84). |
| Method of Calculation |
(Numerator/Denominator) × 100 000 |
| Numerator |
Number of children and youth who report, or whose parents report, self-harm or suicide attempts on RHS.
AND/OR Number of children and youth who die from suicide and who are identified as First Nations or Inuit. |
| Denominator |
Total number of children and youth who respond to the RHS questionnaire |
| Limitations |
This indicator suffers from the limitation of all self-reported indicators. There is a risk of underestimating the true prevalence.
There is no self-reported Inuit data available.
See Indicator #1 “Mortality” for limitations of mortality data. |
Indicator #22 – Rate of Motorized Vehicle Collision Injuries and Deaths
| Motor Vehicle Collisions |
Outcome |
| Indicator Definition |
The rate of motorized vehicle collisions involving children and youth (ages 0–19), by type of vehicle (including cars, ATVs, boats, sea-doo, trains, and snowmobiles), and by crash circumstances (speed, bad weather, driver impairment) |
| Definition of Relevant Terms |
This definition includes any fatality due to a crash involving at least one moving motorized vehicle (car, truck, ATV, motorized boat, sea-doo, train or snowmobile)
Police collision reports use the following definitions:
Fatal collisions include all reportable motor vehicle crashes that resulted in at least 1 fatality where death occurred within 30 days of collision (8 days in Quebec).
Personal injury collisions include all reportable motor vehicle crashes that resulted in at least 1 injury but not death within the timeframes set out in "fatal collisions."
Fatalities include all those who died as a result of involvement in a reportable traffic collision within 30 days of its occurrence, except in Quebec (8 days).
Serious Injuries include persons admitted to hospital for treatment or observation.
Total Injuries include minimal, minor, moderate, serious and unspecified severities.
ATV: All-terrain vehicle. |
| Justification for This Indicator |
Incidents involving motor vehicles and pedestrians are more common among children, and some may involve school buses. A report prepared by IMPACT suggested that risk is attributable to traveling over water, icy conditions in winter, flooded roadways in spring, dusty and pot-holed roads in summer, bush areas and animals. Other risk factors include inconsistent safety procedures, overcrowding on school buses, problematic inspection and maintenance of vehicles, improper driver training and poor snow clearing on waiting areas (McDonald, 2006). |
| What are we counting? (definition of a case) |
Each motor vehicle crash (defined above) and the circumstances of the crash. |
| Where do we get this information / data? |
Crashes involving fatalities might be able to be identified from the Coroners Database. |
| What data do we need? |
Number of motor vehicle (MV) crashes involving First Nations or Inuit children and/or youth (stratified by contributing risk factors, e.g. speed, bad weather and driver impairment) |
| Method of Calculation |
Crash rates = (Number of MV crashes divided by population of relevant age group × 100 000)
Proportions (fatal/nonfatal, by road user type affected)
For example, fatal collisions/total collisions, road user type of interest/total road users |
| Numerator |
Number of MV crashes involving First Nations or Inuit children and/or youth (stratified by: age, sex, road user type – driver/passenger/pedestrian/cyclist) |
| Denominator |
First Nations population or Inuit population (for crash rates), collisions, road user type (for proportions) |
| Limitations |
Coroners' data may be difficult to access in some provinces. It is time-consuming to examine and the victim's ethnicity may not always be listed. |
Indicator #23 – Seat Belt / Restraint Use
| Motor Vehicle Collisions |
Risk / Protective Factor |
| Indicator Definition |
The number and proportion of seriously injured child and youth occupants (ages 0–19) who were unrestrained (not wearing a seatbelt) in a MV collision |
| Definition of Relevant Terms |
Unrestrained – not wearing a seat belt or using a child carseat restraint or booster seat
Serious injuries include persons admitted to hospital for treatment or observation |
| Justification for This Indicator |
In 1991, the APS reported that 50% of individuals aged 15 years and older in First Nations communities use seatbelts. This statistic diverges sharply from the general Canadian population where seatbelt use is at about 80% (Health Canada as cited in McDonald, 2006). |
| What are we counting? (definition of a case) |
The number and proportion of hospitalized involving unrestrained occupants will be identified from police reports. |
| Where do we get this information / data? |
|
| What data do we need? |
For each collision victim – age, sex, road user type, severity of injury, restraint use
Total number of serious injuries (ages 0–19 years) |
| Method of Calculation |
Unrestrained serious injuries divided by total serious injuries |
| Numerator |
Unrestrained First Nations or Inuit drivers and occupants (ages 0–19 years) with serious injuries |
| Denominator |
Total number of First Nations or Inuit serious injuries (ages 0–19 years) |
| Limitations |
Due to underreporting and missing data, it is difficult to capture accurate data on unrestrained injuries. |
Indicator #24 – Youth Driver Education
| Motor Vehicle Collisions |
Risk / Protective Factor |
| Indicator Definition |
The number and proportion of youth who enrol and successfully complete Driver Education Courses within 50 km of their community |
| Definition of Relevant Terms |
Driver Education Courses: Training that teaches how to safely operate a car, snowmobile, boat or ATV; skills for car, snowmobile, boat and ATV drivers Access: courses are located within the community or within 50 km of the community. Language may be a barrier to access if English is not the first language of the First Nation or Inuit person ATV: All-terrain vehicle. |
| Justification for This Indicator |
This indicator operates on the assumption that taking driver education and training improves the skills of the driver thereby preventing injuries due to crashes.
With regard to young drivers, 7 provinces and 1 territory in Canada have instituted graduated licensing programs that have proven effective in reducing collisions that cause injury to novice drivers (Simpson, 2003). |
| What are we counting? (definition of a case) |
Each community member who completed a driver education program for driving any type of MV (i.e. car, snowmobile, boat or ATV). |
| Where do we get this information / data? |
Course service providers, e.g. MV departments or insurance companies, may have data, but may not identify First Nation and Inuit participants. |
| What data do we need? |
Need descriptive systematic data for numbers and ages of people who have completed each course. |
| Method of Calculation |
Proportion: numerator divided by denominator |
| Numerator |
Number of First Nations children and youth of each age who have completed a safety education course to drive a:
- car/truck
- snowmobile
- boat
- ATV
|
| Denominator |
Total population numbers for each age group |
| Limitations |
No clear data source and comparability will be limited.
This indicator does not measure informal education provided by family or community members. |
Indicator #25 – Child Restraint Use
| Motor Vehicle Collisions |
Risk / Protective Factor |
| Indicator Definition |
The proportion of MVs demonstrating proper use of child vehicle restraints (carseats) and booster seats by community
Proper use is defined as correct selection and use as defined by Transport Canada (Keep Kids Safe: Car Time 1-2-3-4 and national child restraint survey design) and will be reported by age in years |
| Definition of Relevant Terms |
Type of restraint is defined by Transport Canada's national child restraint surveys as rear-facing child seat, forward-facing child seat, booster seat, seat belt. Appropriate use for age is defined as < 1 year, rear-facing child seat; 1–2 years, rear-facing or forward-facing child seat; 3–4 years, forward-facing child seat; 5–9 years, booster seat or seat belt; 10–15 years, seat belt. In Transport Canada's national child restraint surveys, proper use is determined according to the criteria for each of the restraint types: “A rear-facing child seat is considered to be properly used only if the harness is in use, the vehicle belt is used to restrain the child seat to the vehicle (only for rear-facing child seats) and the child seat is installed facing the rear of the vehicle. A forward-facing child seat is considered to be properly used only if the harness is in use, the child seat is secured with the vehicle seat belt and tether strap is used. A booster seat is considered to be properly used if the vehicle seat belt is used to secure the seat.” |
| Justification for This Indicator |
Road crashes are the leading cause of death and injury in children in Canada, despite mandatory use of vehicle restraints (Snowdon et al, 2006). The National Occupant Restraint Program (NORP) is an important element of Road Safety Vision 2010. The objective of NORP is to achieve a minimum rate of 95% in seat belt usage and in the proper use of child restraints by all MV occupants by 2010. |
| What are we counting? (definition of a case) |
Number of First Nations and Inuit children properly restrained in vehicles. |
| Where do we get this information / data? |
In Transport Canada's national child restraint surveys, children are observed in vehicles stopped at traffic lights, stop signs and parking lots during daylight hours to determine the type of restraints used for children aged < 16 years. Parking lot surveys require driver consent. |
| What data do we need? |
- Age of child observed
- Type of restraint used
- Proper use (as defined above)
- Location (specific community or province, rural/urban)
|
| Method of Calculation |
Child MV occupants properly restrained divided by total number of child MV occupants observed in that age group |
| Numerator |
Child MV occupants properly restrained in the specified age group (appropriate use for age and proper use can be calculated separately or combined) |
| Denominator |
Child MV occupants observed in the specified age group |
| Limitations |
The National survey listed above does not capture information specific to First Nations/Inuit populations on-reserve/in communities.
- May not be relevant for communities without roads or with primarily ATV/snowmobile use
|
Indicator #26 – Age and Sex of Motor Vehicle Crash Drivers and Occupants
| Motor Vehicle Collisions |
Outcome |
| Indicator Definition |
Age and sex of drivers and occupants (ages 0–19 years) involved in MV crashes by vehicle type (car, van, truck, ATV, snowmobile) and road user (driver, passenger, pedestrian, cyclist) |
| Definition of Relevant Terms |
A motor vehicle traffic crash is any crash on a public road involving at least one moving motorized vehicle. A crash is assumed to have occurred on a public road unless another place is specified, except in the case of crashes involving only off-road MVs (WHO, 1992). This definition excludes all cases where there is no MV involvement, e.g. pedal cycle only crashes; collisions between pedal cyclists and pedestrians (Cryer, 2004). ATV: All-terrain vehicle. |
| Justification for This Indicator |
Young drivers or riders, aged 16–19 years, are consistently overrepresented in victim statistics. They comprise approximately 5% of the licensed driver/rider population but 10% of fatally injured drivers and about 13% of those that are seriously injured. When comparisons are made on the basis of kilometres traveled, they are 7 times more likely to be killed in a crash than the general driving population (Transport Canada, 2005). |
| What are we counting? (definition of a case) |
The number and proportion of serious and fatal injuries involving First Nations or Inuit children and/or youth (ages 0–19) |
| Where do we get this information / data? |
- Mortality Data (see indicator #1)
- Coroner's Data
- Hospitalization data (see indicator #2)
|
| What data do we need? |
Number, age and sex of children and youth who were injured as drivers or passengers of a MV (car, van, truck, ATV, snowmobile) as well as road user type (driver/passenger/pedestrian/cyclist).
Hospitalization and mortality data coded with ICD-10-CA V01–V99. |
| Method of Calculation |
Number of each age of First Nations or Inuit drivers or passengers (age 0–4, 5–9, 10–14, and 15–19 years) with serious injuries/fatalities divided by all MV occupants with serious injuries/fatalities (0–19 years and all ages) |
| Numerator |
Number of deaths and/or number of hospital separations (ICD-10 V01–V99) of First Nation and Inuit drivers and passengers by age group, sex, road user type – driver/passenger/pedestrian/cyclist |
| Denominator |
All First Nations or Inuit MV deaths and serious injuries/fatalities (0–19 years and all ages) |
| Limitations |
Quality data are available; however, we need to have an effective statistical mechanism in place to capture underreported and missing serious injury crashes. |
Indicator #27 – Proportion of Non-Helmet Use
| Motor Vehicle Collisions |
Outcome |
| Indicator Definition |
The number and proportion of seriously injured or killed children and youth (ages 0–19) not wearing a helmet while riding ATVs, snowmobiles, and/or bicycles, by community |
| Definition of Relevant Terms |
ATV: All-terrain vehicle |
| Justification for This Indicator |
Helmet laws have been shown to be effective in increasing the use of bicycle helmets and reducing the incidence of bicycle-related head injuries (Macpherson et al, 2000). Helmet laws that require bicyclists of all ages to wear helmets, as well as those using in-line skates and scooters, are now considered to be the “best practice” laws.
About 50 Canadian children and adolescents die each year from bicycle-related injuries, and 75% of all bicycle-related deaths are due to head injuries. Although the use of helmets can reduce the risk of head injury by 85%, the rate of voluntary helmet use continues to be low (LeBlanc, 2002).
According to an article in Nunatsiaq News, young people from Nunavik accounted for almost 10% of patients treated for serious injuries at Montreal Children's Hospital last year - all-terrain vehicle crashes are mainly to blame (Nunatsiaq News, 2007). |
| What are we counting? (definition of a case) |
Each child/youth who was seriously injured or killed due to head injuries and who was not wearing a helmet while riding ATV, snowmobile or bicycle. |
| Where do we get this information / data? |
Coroner's provides details of helmet use for those children and youth who died. Need to find a data source for number of First Nations or Inuit children and youth who were injured due to not wearing a helmet while riding bicycle, ATV or snowmobile. CHIRRP provides information on the language spoken at home and has a checkbox for parents to check their language as Aboriginal; however, no distinction is made between First Nations and Inuit. |
| What data do we need? |
From Coroner's Data: Number of First Nations and Inuit children and youth killed in ATV, snowmobile or bicycle crash who were not wearing a helmet.
From CHIRRP Data:
- Number of First Nations and Inuit children and youth with head injuries in ATV, snowmobile or bicycle crash due to not wearing a helmet.
- Part of the body that was injured/ type of injury.
|
| Method of Calculation |
Number of children and youth killed from head injuries due to not wearing a helmet divided by number of children and youth killed from all bicycle, ATV or snowmobile incidents. |
| Numerator |
Number of First Nations and Inuit children and youth (0–19 years) killed from head injuries due to not wearing a helmet. |
| Denominator |
Number of First Nations children and youth killed from all bicycle, ATV or snowmobile incidents. |
| Limitations |
Coroner's database may not always identify First Nations and Inuit ethnicity or may not identify which deaths are due to lack of or improper use of helmets.
CHIRRP data is criticized for not being population-level data as it only counts injuries that are treated by the emergency department of 10 children's hospitals in Canada. |
Recommendations
After completing the work within this document, there are 3 recommendations that stand out:
- A survey similar to the First Nations Regional Longitudinal Health Survey needs to be created for/with Inuit communities. The lack of Inuit data makes it very difficult to populate these indicators with information that is relevant to Inuit communities. Inuit-specific data is needed in order to properly assess the injury problem for Inuit children and youth.
- Community-level surveillance to gather specific data points would do much to address the gaps in data identified in this document. It is recommended that communities facilitate community-level surveillance whenever possible.
- These indicators need to be populated with data. In order to ensure that the burden of injury decreases, work is needed to illuminate these indicators with data and make a plan for indicator uptake. The information gleaned through the use of these indicators will facilitate improved decision making and action to decrease injuries among indigenous children and youth in Canada.
References
Canadian Public Health Association. (2006). Pot and Driving in the North. Ottawa: Canadian Public Health Association.
Chandler, M.J., & Lalonde, C.E. (1998). Cultural continuity as a hedge against suicide in Canada's First Nations. Transcultural Psychiatry, 35(2), 191-219.
Cryer, C., Langley, J., and Stephenson, S. (2004). Developing Valid Injury Outcome Indicators. Dunedin: New Zealand Injury Prevention Strategy.
Cryer, C., Langley, J.D., Stephensen, S.C., Jarvis, S.N., & Edwards, P. (2002). Measure for measure: the quest for valid indicators of non-fatal injury incidence.
Public Health. Sep, 116(5), 257-62.
First Nations Centre (2005). First Nations Regional Longitudinal Health Survey (RHS) 2002/03. Ottawa: First Nations Centre.
Health Canada.(1997). Economic Burden of Illness in Canada, 1993. Ottawa: Minister of Public Works and Government Services Canada.
Leblanc, J.C., Beattie, T.L., Culligan, C. (2002). Effect of legislation on the use of bicycle helmets. CMAJ Canadian Medical Association Journal, 166, 592-5.
McDonald, Rose-Alma J. (2006). An AFN Handbook for Injury Prevention for First Nation Communities. Ottawa: Assembly of First Nations.
McDonald, Rose-Alma J. (2006). Injury Prevention Fact Sheets. Ottawa: Assembly of First Nations.
Plourde, C. et al. Use of alcohol and other drugs by Nunavik youths: key results of the survey. Recherche et intervention sur les substances psychoactives – Québec. 2007. (leaflet and presentation)
Public Health Agency of Canada. (2005). Inventory of Injury Data Sources and Surveillance Activities. Ottawa, Ontario: Minister of Health Canada and the Minister of State for Public Health.
Simpson, H. (2003). The Evolution and Effectiveness of Graduated Licensing. Journal of Safety Research 34(1), 25-34.
World Health Organization. (1992). International statistical classification of diseases and related health problems. 10th revision. Geneva: WHO.
Online References
Assembly of First Nations (2006). Fire. Injury Prevention Fact Sheet. Retrieved on September 3, 2014,
FEI Behavioral Health (2007). Crisis Management Disaster Communication Plan. Retrieved on August 27, 2007
Section 1.01 First Nations Information Governance Centre. Accessed on August 19, 2013.
Section 1.02 George, Jane. (2007, September 14). ATVs take toll on Nunavik youth. Nunatsiaq News. Retrieved on Dec. 6, 2007.
Health Canada (2006). It's your Health: Smoke Detectors. Retrieved on August 24, 2007
Health Canada (2005). Unintentional and Intentional Injury Profile for Aboriginal People in Canada. Retrieved on November 23, 2007
Indian and Northern Affairs Canada (2004). Backgrounder The Proposed Westbank First Nation Self-Government Act. Retrieved August 20, 2007.
Industrial Accident Prevention Association (2006). Fire Distinguishers. Retrieved on Aug 24, 2007.
McFarlane, P. (1997, Winter). New approaches to injury prevention. In Touch. 7 (3). Retrieved on September 3, 2014.
Merriam-Webster Dictionary (2007). Definition of substance. Retrieved on August 8, 2007.
Merriam-Webster Dictionary (2007). Definition of Drug. Retrieved on August 9, 2007.
Merriam-Webster Dictionary (2007). Definition of Mauling. Retrieved on November 30, 2007.
Medline Plus (2007). Definition of incidence. Retrieved on August 8, 2007
Supporting First Nations, Inuit and Métis People in Addressing Their Needs. (2006). Retrieved on August 10, 2007
National Indian & Inuit Community Health Representatives Organization (2007). In Touch Winter 7(3).
Public Health Agency of Canada (2005). Child Abuse and Neglect Overview Paper. Retrieved on November 15, 2007.
Royal Canadian Mounted Police (2007). Deal.org Domestic Abuse. Retrieved on Aug 8, 2007.
Royal Canadian Mounted Police (2007). Community, Contract, and Aboriginal Policing. Retrieved on Nov 27, 2007.
Sexual Exploitation (2005). Retrieved on November 15, 2007.
Statistics Canada (2007). Aboriginal Children's Survey. Retrieved on September 20, 2007.
Statistics Canada (2005). Canadian Community Health Centre Profiles. Retrieved on October 31, 2007.
The New York Times Company (2007). Survive the unthinkable through crisis planning. Retrieved on Aug 27, 2007.
Transport Canada (2005). Road Safety Vision 2010: Making Canada's Roads the Safest in the World. Retrieved on March 6, 2007.
U.S. National Fire Protection Association (2007). Smoke Alarms. Retrieved on November 28, 2007
U.S. National Fire Protection Association (2007). Fire Extinguishers. Retrieved on November 28, 2007.
Wikipedia (2008). Carbon Monoxide Detector. Retrieved on December 22, 2008
Wikipedia (2013). Search and Rescue. Retrieved on September 30, 2013
World Health Organization (2008). International Classification of Diseases. Retrieved on January 16, 2008.
World Health Organization (2007). Substance Abuse. Retrieved on Aug 8, 2007.
Younger-Lewis, Greg. (2004, January 23). Assault, property crime up in Iqaluit in 2003. Nunatsiaq News. Retrieved on Dec. 6, 2007.