Lyme disease: For health professionals
On this page
- Lyme and other tick-borne diseases
- Clinical manifestations
- Clinical diagnosis
- Treatment
- Laboratory testing
- Surveillance
- Subscribe to the email list
Lyme and other tick-borne diseases
Lyme disease is a vector-borne zoonotic disease caused by the bacterium Borrelia burgdorferi. The bacterium is a spirochete transmitted by infected nymphs and adult females of a small number of species of Ixodes ticks. The ticks mainly responsible for Lyme disease are the:
- blacklegged tick (Ixodes scapularis)

- western blacklegged tick (Ixodes pacificus)

These species of ticks feed on a variety of mammal and avian hosts, including:
- deer
- rodents
- ground foraging bird species
Some of these hosts serve as reservoirs in which the bacterium circulates.
Borrelia burgdorferi is the most common pathogen detected in these tick species. However, other pathogens that can cause disease in humans are also occasionally detected in these ticks, including:
- Anaplasma phagocytophilum, the agent of anaplasmosis
- Babesia microti, the agent of babesiosis
- a strain of Powassan virus
- Borrelia miyamotoi, the agent of tick-borne relapsing fever
- Borrelia mayonii (Lyme-like disease)
Most Borrelia burgdorferi infections occur during the warmer months, but Lyme disease cases have been reported throughout the year. Ticks can be active whenever the temperature is consistently above freezing and the ground is not covered by snow.
With an increase in the number of Lyme disease cases in Canada, health professionals are encouraged to learn more about this disease. Most cases of Lyme disease can be managed successfully with a timely diagnosis and appropriate treatment.
Clinical manifestations
The incubation period for early localized infection is 3 to 30 days.
It is important to note that some people with Lyme disease may have no or minimal symptoms. Others may experience more severe symptoms.
Individuals who do not develop symptoms until weeks after the tick bite may not remember being bitten nor associate symptoms with the bite. Furthermore, because nymphs are very small and tick bites are usually painless, most people may not know that they were bitten.
Clinical manifestations are not necessarily specific to the stage of infection. They can overlap and form a continuum in some untreated patients.
Early localized Lyme disease (3 to 30 days)
Early localized Lyme disease usually presents as an acute illness characterized by:
- flu-like symptoms, such as:
- fever
- malaise
- myalgia
- headache
- migratory arthralgia
- lymphadenopathy
- erythema migrans rash
Erythema migrans rash
An erythema migrans rash expands to greater than 5 cm in diameter at the site of the tick bite. It is usually painless and non-pruritic. In many cases, an erythema migrans rash will not present with a classic bull's-eye appearance.
Most patients will present with an erythema migrans rash within 7 days of the initial tick bite but this can range from 3 to 30 days. On dark skin, the rash may appear more as a bruise, making it difficult to diagnose.
An erythematous lesion is a hypersensitivity reaction to the tick bite itself, not an erythema migrans rash. An erythematous lesion occurs within 24 hours, is less than 5 cm in diameter and does not expand over time. Observe for 48 hours or longer to see if it expands into an erythema migrans rash.
Images of erythema migrans rash on light skin
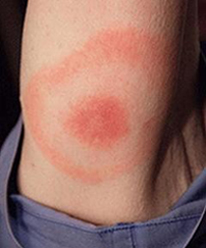
Image 1: A skin rash called erythema migrans can develop into a bull's eye at the site of a tick bite. It is shown here on the upper arm.
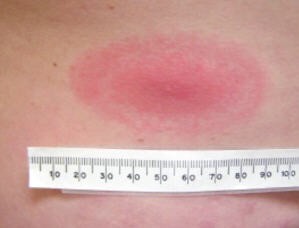
Image 2: An oval-shaped erythema migrans rash that can take on the appearance of a bull's eye.
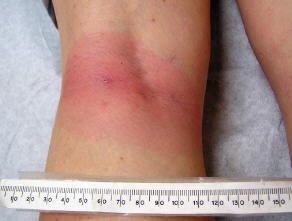
Image 3: An erythema migrans rashes that is uniformly red and does not appear with the classic bull's eye.
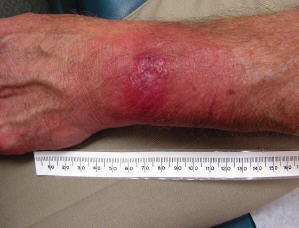
Image 4: An erythema migrans rash with a central blistering lesion, sometimes mistaken for a spider bite.
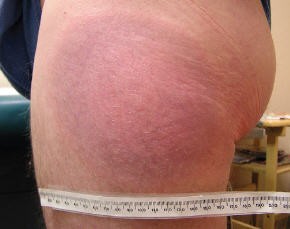
Image 5: An erythema migrans rash with a blue-purple colour, which is distinct from bruises because of its sharply defined border.
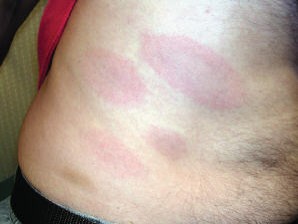
Image 6: Multiple erythema migrans lesions taking variable shapes.
Source: Dr. John Aucott, Johns Hopkins University
Images of erythema migrans rash on dark skin
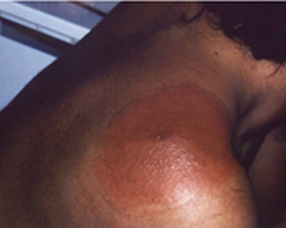
Image 7: An erythema migrans rash on right shoulder.
Source: U.S. Centers for Disease Control and Prevention, Public Health Image Library

Image 8: An erythema migrans rash on the back of the upper arm.
Source: Dr. John Aucott, Johns Hopkins University
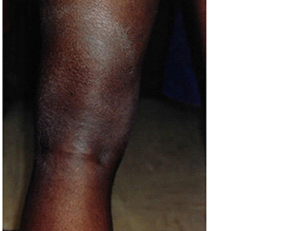
Image 9: An erythema migrans rash without bull's eye on the back of a knee.
Source: Professor Gary Wormser, New York Medical College
Early disseminated Lyme disease (less than 3 months)
If untreated, the bacterium causing Lyme disease can:
- disseminate via the bloodstream and lymphatic system to other body sites
- cause damage to body tissues at those sites, most commonly nervous and musculoskeletal systems
Signs and symptoms can include:
- fatigue and general weakness
- multiple erythema migrans lesions
- neurological manifestations
- aseptic meningitis
- cranial neuropathy, especially facial nerve palsy (Bell's palsy)
- encephalitis, encephalomyelitis, subtle encephalopathy or pseudotumor cerebri (all rare)
- motor and sensory radiculoneuropathy and mononeuritis multiplex
- subtle cognitive difficulties
It can also cause Lyme carditis, which may manifest in any of the following ways:
- high-degree atrioventricular block (the most common presentation)
- sinus node disease or dysfunction
- intra-atrial block
- atrial fibrillation
- supraventricular tachycardia
- bundle branch block
- ventricular tachycardia and fibrillation
Rare manifestations of early disseminated Lyme disease include:
- conjunctivitis
- keratitis
- mild hepatitis
- splenomegaly
- uveitis
Late disseminated Lyme disease (more than 3 months)
If Lyme disease remains untreated or diagnosed later, it can persist for months or years.
Possible musculoskeletal manifestations include:
- Baker's cyst
- intermittent episodes of pain and/or swelling in one or multiple joints, particularly the knees and other large joints leading to chronic arthritis
- if untreated, arthritis may recur in the same or different joints
Possible neurological and cognitive manifestations occur due to effects on the central and peripheral nervous systems. Presentation may include:
- meningitis
- meningoencephalitis
- subacute mild encephalopathy, affecting:
- memory
- concentration
- myelitis
- cranial neuropathy
- radiculopathy
- chronic mild axonal polyneuropathy, manifested as:
- distal paresthesia
- radicular pain (less common)
Rare forms of presentation include:
- encephalomyelitis
- leukoencephalopathy
- diaphragmatic paralysis caused by phrenic nerve palsy leading to tick-induced respiratory paralysis or respiratory distress
Clinical diagnosis
The diagnosis of early localized Lyme disease is primarily clinical with presence of an erythema migrans rash, supported by history of exposure to blacklegged ticks.
Blacklegged ticks and western blacklegged ticks can be found outside currently identified risk areas. While a known history of exposure to blacklegged and western blacklegged ticks helps with the diagnosis, absence of a history of exposure does not rule out Lyme disease.
Tick exposure with an erythema migrans rash
A patient presenting with an erythema migrans rash may be clinically diagnosed with Lyme disease if they have a history of tick exposure. A history of tick exposure includes a recent tick bite, or living in or having recently visited a Lyme disease endemic area.
In this scenario, treatment is recommended without laboratory confirmation, as serologic tests are not sensitive at this stage.
Tick exposure without an erythema migrans rash
If a patient has a history of tick exposure and presents with other non-specific symptoms, such as headache, fever, and muscle and joint pain, but does not present with an erythema migrans rash, the patient may still have Lyme disease.
In this scenario, serological testing is recommended, and an acute and convalescent sample (2 to 4 weeks after the acute one) may be required to obtain laboratory confirmation of Lyme disease.
However, some individuals who receive treatment during early localized Lyme disease may not seroconvert. That is, IgG antibodies may not be detected in serological tests performed on convalescent samples.
Treatment
Following tick exposure, a patient with an erythema migrans rash should be treated for Lyme disease promptly, without the need for serological testing.
Most cases of Lyme disease can be treated successfully with appropriate treatment.
Patients who are treated with an appropriate antibiotic early in the course of illness (early disease), tend to recover more quickly than those who are treated at later stages of disease (late disease).
Doxycycline, cefuroxime axetil and amoxicillin are the most commonly recommended oral antibiotics. Doxycycline is not recommended for pregnant people.
For more information:
- Centre for Effective Practice – Early Lyme Disease Management in Primary Care Toolkit
- Association of Medical Microbiology and Infectious Disease Canada
Lyme disease and pregnancy
Current evidence related to Lyme disease and pregnancy is limited.
While transmission of Lyme disease during pregnancy is possible, the risk of passing Lyme disease to a baby during pregnancy is considered very low.
If a pregnant person has Lyme disease, they can be safely and effectively treated with antibiotics. Early treatment reduces the risk of potential placenta infection and complications.
For more information:
Patients with persistent symptoms following treatment of Lyme disease
Most people with early Lyme disease who receive appropriate antibiotics recover completely. However, some patients may continue to have persistent symptoms following treatment.
Persistence of objective findings following treatment, especially high fever, may be due to co-infection with another pathogen transmitted by Ixodes ticks. This calls for investigation for co-infection if the initial antibiotic is not effective against these pathogens.
Other reasons that may explain a lack of response are as follows:
- The initial diagnosis of Lyme disease was incorrect.
- There is another condition that persists (for example, fibromyalgia, depression, patellofemoral joint disease).
- An autoimmune process may have been triggered (for example, in the case of knee synovitis of Lyme disease that persists for months after antibiotic therapy).
- Permanent tissue damage may have occurred (in patients with previous neurologic involvement).
Laboratory testing
The current laboratory test for Lyme disease is serology, where the presence of antibodies to Borrelia burgdorferi are detected using a two-tiered testing approach.
The results of laboratory testing should be considered in the context of the clinical presentation and duration of symptoms. It is important to understand the limitations of these tests.
Although the two-tiered serology test has a high degree of sensitivity in patients that present with late infection, false negative results can occur in early localized infections. This is because it takes time for a person to generate an antibody response that can be detected. This is a reflection of the bacteria's slow replication within the host.
Test may be negative in patients who are treated early with antibiotics.
Laboratory accreditation
Laboratory testing should be done through a licensed public health laboratory.
All diagnostic laboratories in Canada operate within quality assurance systems to ensure testing is done to the highest standard using best laboratory practices. They have systems in place that are recognized by accreditation bodies, such as:
- Accreditation Canada
- College of American Pathologists
- International Organization for Standardization
This applies to all procedures conducted in the laboratory, including those for Lyme disease serological testing.
Canadian laboratory diagnostic guidelines for Lyme disease meet current international standards. They are also consistent with those followed by public health authorities in the U.S. and Europe.
It is not recommended to:
- perform tests via non-licensed laboratories or private laboratories that do not use U.S. Food and Drug Administration or Health Canada approved tests, nor
- use alternative interpretive criteria
Two-tiered serological testing
The two-tiered or two-step serological testing approach is recommended when testing for antibodies to Borrelia burgdorferi.
In a two-step testing process, if the first step is negative, no further testing is recommended.
If the first step is positive or equivocal, the second step should be performed. The overall result is positive only when the first test is positive (or equivocal) and the second test is positive (or for some tests equivocal).
This approach is validated for use in Canada and currently includes:
- an enzyme immunoassay (EIA)
- a confirmatory immunoblots (e.g., western blots or line blots) which are performed on samples that are positive or equivocal on the EIA
To improve sensitivity in detecting early Lyme disease, substitution of the immunoblots with a second EIA is being considered as an alternative two-tiered approach.
Interpretative criteria for the EIA and immunoblot have been standardized and summaries of the diagnostic approaches for Lyme disease are available.
If testing is required, indicate the presumed exposure area (for example, North America or Europe) on the requisition. The location will determine which specific test kits will be used, as different immunoblot are used when exposure occurs in Europe versus North America. In suspected neuroborreliosis (or Lyme disease affecting the central or peripheral nervous system), testing for intrathecal IgG or IgM antibodies may be helpful. Consult your provincial public health laboratory.
Borrelia burgdorferi, sensu stricto, is the most common genospecies of Borrelia circulating in North America. A small number of other genospecies of the B. burgdorferi sensu lato group (e.g., B. garinii), known to occur in Europe, have been reported in Canada. They appear to be restricted to unique transmission cycles involving seabirds and seabird ticks.
Serological tests cannot be used to assess treatment response, as antibodies persist after treatment. Furthermore, because of antibody persistence, a positive serologic test cannot distinguish between recent and past infection.
Enzyme immunoassays
Most EIA have a high sensitivity if done at least 2 weeks after the possible exposure. A small percentage may cross-react with antibodies to:
- viruses (e.g., Epstein-Barr virus)
- certain autoimmune diseases (e.g., lupus)
- commensal or pathogenic spirochetes (e.g., syphilis)
Immunoblots
Immunoblots are performed only if the EIA is positive or equivocal. They are highly specific and can be used to rule out other infections or conditions. False negatives may occur if the test is performed before IgG antibodies develop, which typically occurs after 4 weeks post infection.
As IgM antibodies can persist for months to years (despite effective antibiotic treatment), a positive IgM immunoblot:
- may not indicate current infection
- is not sufficient evidence to diagnose current disease in patients with symptoms of longer duration
For this, a positive IgG immunoblot is required.
When testing patients with illness duration greater than 1 month, many diagnostic laboratories and some health care providers indicate that only IgG immunoblot should be performed (not IgM).
The U.S. Food and Drug Administration has approved Lyme disease testing that uses two EIA assays, substituting a second EIA for the traditional immunoblots. This new two EIA or modified two-tiered testing has been endorsed by the U.S. Centers for Disease Control and Prevention. It has been recommended specifically for patients with early localized Lyme disease because of improved sensitivity in this patient cohort.
Standard two-tiered testing can still be used for late disseminated Lyme disease. The Canadian Public Health Laboratories Network is considering implementing the two EIA approach for Lyme disease once sufficient data has been gathered on Canadian patients.
Figure 1. History of tick exposure
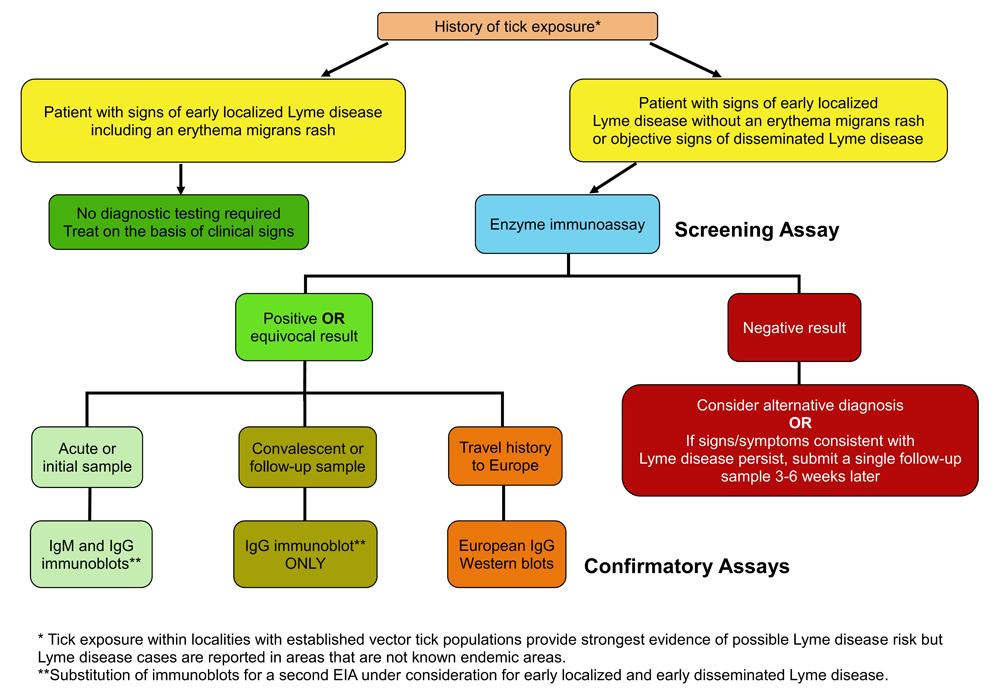
Figure 1: Text description
This flowchart shows actions that a health professional can take when their patient has a history of tick exposure.
If the patient has a history of tick exposure* and signs of early localized Lyme disease, including an erythema migrans rash, the patient does not require diagnostic testing. The patient should be treated based on the basis of clinical signs.
Patients should have an enzyme immunoassay if they have a history of tick exposure and:
- objective signs of disseminated Lyme disease or
- signs of early localized Lyme disease without an erythema migrans rash
If the immunoassay has a negative result:
- consider an alternative diagnosis or
- submit a single follow-up sample 3 to 6 weeks later if signs or symptoms of Lyme disease persist
If the immunoassay has a positive or equivocal result:
- perform IgM and IgG immunoblots** on acute or early samples
- perform only IgG immunoblots** on convalescent samples (>4 weeks)
- consider using European testing protocols and immunoblots for patients with history of travel outside of North America
* Tick exposure within localities with established vector tick populations provide strongest evidence of possible Lyme disease risk but Lyme disease cases are reported in areas that are not known endemic areas
** Substitution of immunoblots for a second enzyme immunoassay under consideration for early localized and early disseminated Lyme disease
Surveillance
The national case definition for Lyme disease is used to classify cases reported to the Public Health Agency of Canada. Reported cases from 2016 to 2019 use the updated Lyme disease case definition.
Lyme disease became nationally notifiable in 2009, when the first national case definition was developed. Nationally notifiable diseases are infectious diseases that have been identified by the federal, provincial and territorial governments as priorities for surveillance and control efforts. The national case definition was updated in 2016.
The national notification system is voluntary and receives cases reported through provincial and territorial public health authorities. Provinces and territories have their own legislation for the reporting of priority infectious diseases within their jurisdictions. If it meets the case definition, provinces and territories report newly diagnosed cases of Lyme disease to the Public Health Agency of Canada.
Subscribe to the email list
Subscribe to the zoonoses subscription list for regular updates about our work on zoonoses, including those that can be spread through the bite of a tick or mosquito. Subscribing to the email list will help keep you up to date and informed about our work on these diseases.
Related links
- Lyme and other tick-borne diseases: International resources for health professionals
- Lyme disease surveillance in Canada: Annual edition 2019
- Lyme disease surveillance in Canada: Annual edition 2018
- Lyme disease surveillance in Canada: Annual edition 2018 (infographic)
- Society of Obstetricians and Gynaecologists of Canada
- Centre for Effective Practice – Early Lyme Disease Management in Primary Care Toolkit
- Association of Medical Microbiology and Infectious Disease Canada
- Current Guidelines, Common Clinical Pitfalls, and Future Directions for Laboratory Diagnosis of Lyme Disease, U.S.
- Lyme disease: Lab diagnostics
- Surveillance for Lyme disease in Canada: 2009 to 2015
- National Lyme Disease Surveillance in Canada 2009 to 2012
Page details
- Date modified: